Professional Documents
Culture Documents
DRY EYE SYNDROME ANATOMY AND PHYSIOLOGY
Uploaded by
Princess Cate MercadoOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
DRY EYE SYNDROME ANATOMY AND PHYSIOLOGY
Uploaded by
Princess Cate MercadoCopyright:
Available Formats
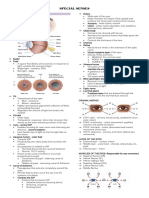
DRY EYE SYNDROME o The mucus layer helps spread the watery layer over
the eye’s surface, keeping it moist. Without mucous,
Vic Santos, MD tears would not stick to the eye. Mucus is made in
the conjunctival goblet cells.
ANATOMY OF THE EYE Doc (record): The tears are not just composed of water. It is a
trilaminar fluid layer. We have the closest to the cornea which is the
mucinous layer produced by the conjunctival goblet cells. The middle
layer, the watery portion is produced by the lacrimal glands and
accessory glands. The most superficial is the oily layer produced by the
meibomian glands.
Doc (record): The lacrimal gland located at the lateral, temporal portion
of orbit. The conjunctival goblet cells which line the whole palpebral
conjunctiva. When we say palpebral and bulbar conjunctiva, the bulbar
conjunctiva aligns with the eyeball, and the palpebral conjunctiva lines
up the eyelids. The blinking mechanism causes about a suction
mechanism which drains the tears into the punctum.
DRY EYE SYNDROME
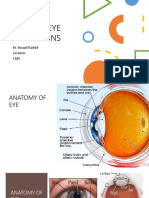
Doc (record): This is the basic anatomy of the eye. We have here
the eyelid, the eyelashes, and the glands. Our topic today is Dry Eye
Disease. However, you will note that the tears also has a drainage. Part of
the discussion is tearing. Know the physiology. It is produced by different
glands in the eye and it has a drainage which goes into the hole into the
lid margin known as the punctum, then goes into the lacrimal duct and Doc (record): We blink to about 10-15 times per minute.
then exits into the nose.
If there is a blockade from inflammation, fibrosis, or infection,
the blockade will cause a back flow causing the eyes to tear up. That is DRY EYE SYNDROME
called EPIPHORA.
• Group of disorders of the tear film that are due to reduced tear
NORMAL PHYSIOLOGY OF TEARS production or excessive tear evaporation, associated with
ocular discomfort and/or visual symptoms and possible disease
• When you blink, a film of tears spreads over the eye. This keeps of the ocular surface.
the eye’s surface smooth and clear.
• The tear film is made of three layers • Dry eye is a frequent cause of ocular irritation that leads
o The oily layer makes the tear surface smooth and patients to seek ophthalmologic care, while these symptoms
keeps tears from drying up too quickly. This layer is often improve with treatment, the disease usually is not
made in the eye’s Meibomian glands. curable, which may be a source of patient and physician
o The watery layer makes up most of what we see as frustration.
tears. This layer cleans the eye, washing away
particles that do not belong in the eye. This layer
comes from the lacrimal glands in the eyelids.
WHISKY, SWIRLY DRY EYE SYNDROME OPHTHA ROTATION 1 | 7
Impact of Dry Eyes • Decreased tear secretion and clearance initiates an
• Difficulty with activities of daily living inflammatory response on the ocular surface that involves both
- reading soluble and cellular mediators
- driving
• Loss of work productivity
• Quality of life decrease SYMPTOMS OF DRY EYES
- chronic debilitating symptoms
- anxiety and depression • Burning
• Management cost • Stinging
• Itching
Doc: The impact of dry eyes will always have blurring of vision like a • Tearing
windshield in the rain that doesn't get wiped or a dried-up with full of • Sandy or gritty feeling
dust instead of being cleaned. You'll have trouble reading and driving. You • Scratchy or foreign-body sensation
have loss of work productivity and overall, it is a major cause of • Discharge
discomfort. • Frequent blinking
• Mattering of the eyelashes (usually worse upon waking)
RISK FACTORS FOR DRY EYE DISEASES • Redness
• Blurry or fluctuating vision (made worse when reading,
computer, watching television, driving or playing video games)
• Light sensitivity
• Eye pain and/or headache
• Heavy eyelids
• Eye fatigue
Doc: Majority will be discomfort, blurring of vision, itchiness and dry eye
sensation.
VICIOUS CYCLE OF DRY EYE SYNDROME
Doc: More at risk is the female gender because of the lack of testosterone
which is associated with tear production. The older the person, tear
production will be less. Hormonal deficiency which is also associated with
the female sex and menopause. We also have systemic diseases Such as
sjogren, rheumatoid and grave’s disease. Diabetes mellitus and infection
and a lot of medication use. Any of ophthalmic surgery can cause about
dry eyes also such as cataract and glaucoma surgery. We also have
nutritional deficiency cause about by lack of vitamin A and lack of omega-
3 fatty acid.
PATHOGENESIS
The ocular surface and tear-secreting glands function as an integrated
unit. Damage or dysfunction leads to an unstable and poorly maintained
film that causes ocular irritation symptoms and possible damage to the
ocular surface epithelium. MAIN SUBTYPES OF DRY EYE DISEASE /
DYSFUNCTIONAL TEAR SYNDROME
Doc: The basic symptom is deficiency in tear production which causes
dryness, which causes inflammation, and the inflammation causes Aqueous Tear Deficiency
decreased production in tears. It is essentially a vicious cycle. • Lacrimal gland dysfunction
• Neurotrophic corneas
• Sjogren syndrome
DYSFUNCTION MAY DEVELOP FROM
• Aging Blepharitis/ Meibomian Gland dysfunction
• Decrease in supportive factors (such as androgen hormones) • Anterior/ Posterior Blepharitis
• Systemic inflammatory disease (such as Sjogren syndrome or
rheumatoid arthritis)
• Ocular surface disease (herpes simplex virus [HSV] keratitis) Goblet Cell/ Mucin Deficiency
• Surgeries that disrupt the trigeminal afferent sensory nerves • Steven-Johnson syndrome
(e.g., LASIK) • Vitamin A deficiency
• Systemic diseases or medications that disrupt the efferent • Contact lens wear
cholinergic nerves that stimulate tear secretion • Thermal and chemical injuries
WHISKY, SWIRLY DRY EYE SYNDROME OPHTHA ROTATION 2 | 7
Exposure related
• Bell’s Palsy
• Parkinson’s disease
• Ectropion
• Lagophthalmos
• “Focus” activities
Co-conspirators
• Medicamentosa
• Ocular allergy
• Mucus fishing syndrome
• Conjunctivitochalasis
• Floppy eyelid syndrome
QUESTIONNAIRES
OCULAR SURFACE DISEASE INDEX (OSDI)
• Used to assess the symptoms of ocular irritation in dry eye
disease and how they affect functioning related to vision
• 12-item questionnaire assesses dry eye symptoms and effects it
has on vision-related function in the past week of the patient’s
life
• The questionnaire has 3 subscales:
• Ocular symptoms
• Vision-related function, and
• Environmental triggers
• The OSDI limits itself by assessing a small variety of dry eye
symptoms including sensitivity to light, grittiness, and pain. The
questionnaire lacks different symptoms such as tearing and
foreign body sensation. The lack of these fields makes the
questionnaire less accurate in assessing specific symptoms that
the patient may describe
DIAGNOSTIC TEST
• The OSDI has demonstrated good specificity (0.83) and a
moderate sensitivity (0.60) when distinguishing between
• Evaluation of the face and eyelids, blinking patterns, eyelid
patients with dry eye disease and normal subjects.
margins, eyelashes, conjunctiva, cornea and tear film
o Tear Break Up Time (TBUT)
▪ Function of dry spots caused by
IT IS A SUBJECTIVE MEASUREMENT
withholding the blink
o Ocular surface staining (Fluorescein sodium, Rose
Bengal, Lissamine green)
▪ Dry spots by certain dyes in cornea
o Schirmer test
▪ Amount of tears in mm by the spread of
OTHER QUESTIONNAIRES FOR DRY EYE DISEASE
wetness in the litmus paper
o Tear Osmolarity (TearLab Osmolarity System)
• 5-item Dry Eye Questionnaire (DEQ-5)
▪ More advanced, amount of solutes in the
• McMonnies questionnaire (MQ)
tears
• Impact of Dry Eye Institute Visual Function Questionnaire-25
o Tear Film Interferometry
(NEi-VFQ-25)
o Keratograph
• Standardized Patient Evaluation of Eye Dryness (SPEED)
▪ Measurement of tear spread in cornea
Questionnaire
o HD Analyzer
• Symptom Assessment in Dry Eye (SANDE)
▪ Effect of dry eyes into the vision
WHISKY, SWIRLY DRY EYE SYNDROME OPHTHA ROTATION 3 | 7
TEAR BREAK UP TIME (TBUT) OCULAR SURFACE STAINING
• It checks tear film instability FLUORESCEIN SODIUM
• The proper method of TBUT testing is using a fluorescein- • Fluorescein dye is the most commonly used stain in
impregnated strip wet with non-preserved saline solution ophthalmology. Areas in which the corneal or conjunctival
• The dye is distributed by blinking, and the patient is then asked surface epithelial cells are loos or desquamated will stain with
to stare straight ahead without blinking fluorescein
• The tear film is observed under the cobalt blue light of a slit
lamp, and the time between the last blink and the appearance
of the first dry spot or hole in the tear film is measure and
equal to the TBUT
• Normal subjects show variability in TBUT, although 10 seconds
is the typical cutoff between normal and abnormal results and
has been found to be relatively specific in screening patients for
tear film instability. LISSAMINE GREEN
• Lissamine green has similar staining characteristics but is much
better tolerated than Rose Bengal. Lissamine green is also
available in dye-impregnated paper strips
Staining is devitalized areas
ROSE BENGAL
• Rose Bengal is more sensitive for conjunctival staining, but also
more difficult to visualize and less well tolerated compared to
fluorescein. Rose Bengal stains devitalized epithelial cells that
lack a healthy mucin coating. It is applied using a dye-
impregnated paper strip.
SCHIRMER TEST • In aqueous tear deficiency, the interpalpebral conjunctiva is
the most common location for Rose Bengal staining
• It is performed by placing a paper test strip in the lateral third • The severity of staining has been shown to correlate with the
of the lower eyelid after drying the inferior fornix and then degree of aqueous deficiency, tear film instability, and reduced
measuring the length of the moistened portion of the strip mucin production by conjunctival goblet and epithelial cells
after 5 minutes
• The Schirmer I test is performed without anesthesia and thus
measures reflex tearing
• The Schirmer II test also lacks anesthesia but is done following
nasal stimulation
• “Schirmer with anesthesia” is also commonly performed and
measures basal tear secretion
• The Schirmer test is often criticized for its variability and poor
Devitalized epithelial cells will stain red.
reproducibility
• It is most useful in the diagnosis of patients with severe
aqueous deficiency, but is relatively insensitive for patients
VAN BIJSTERVELD OCULAR DYE SCORE
with mild dry eye
Anything above 10mm is considered normal
Measure of dry eye disease based on the dryness pattern.
WHISKY, SWIRLY DRY EYE SYNDROME OPHTHA ROTATION 4 | 7
TEAR OSMOLALRITY (TEARLAB OSMOLARITY SYSTEM) KERATOGRAPH 5M
Will show the different areas of dryness.
Right lower frame: meibomiography
Similar to schirmer’s test, only this one measures the amount of solutes. A • Keratography 5M combines corneal topography and dry eye
HYPEROSMOLAR tear will connote dry eyes, whereas a low analysis in one machine. The machine uses Placido disc
osmolarity/HYPOOSMOLAR will show a normal tear production. illumination to make measurements of the ocular surface, and
More reliable than the tear film, which can be altered by humidity and different colors of light emitting diodes (LEDS) are used
reaction of eye to the irritation of the paper. depending on the application
• The Keratograph 5M offers Meibo-Scan for meibography of the
TEAR OSMOLARITY upper and lower eyelid to check for Meibomian Gland
• Patients with dry eye disease have been found to have elevated Dysfunction (MGD), TF-Scan for evaluation of the tear film
tear film osmolarity (TFO). Tear hyperosmolarity can induce break-up time, and R-Scan for automatic bulbar redness
tear film instability by modifying the interaction between tear classification.
film lipids and proteins, damaging the epithelial cell
membranes, triggering inflammation and stimulating corneal
nerves ASSESSMENT RESULTS
• Tear osmolarity can be determined easily in the office using the
point of care TearLab Osmolarity System (TearLab, San Diego,
CA), which measures the osmolarity of a 50-nL tear sample.
Normal values are considered to be 296±9.8 mOsm/L.
• Greater than 308 mOsm/L is considered to indicate at least
mild dry eye and has been demonstrated to serve as an early
indicator of ocular surface instability.
• The test is performed by placing the tip of the handheld device
at the lateral tear meniscus and then docking the sampler into
the reader
• The device contains a gold-plated microchip that measures
electrical impedance in the sample and displays the osmolarity
measurement within seconds
TEAR FILM INFEROMETRY
Corneal mapping of the non-invasive TBUT. Non-invasive because nothing
is put to the eye, which can alter the results.
That’s what we do in different types of dyes, we put in anesthetic and
there’s no reaction, but then we put in a paper, and that will cause
alteration in the actual surface of the cornea.
Measures the blockade in the meibomian gland. The gray spots, is the
meibomian gland drop-out or the blockade.
• This technique permits determination of the thickness of the
superficial lipid layer that floats upon the normal tear film and
of the fluid layer that covers the anterior surface of contact This is the tear meniscus level. There is a fluid level: if too low, it is an
lenses. indicator of dry eyes.
• In general, these thickness estimates have been based upon
the general hue (color) of the reflected interference patterns
WHISKY, SWIRLY DRY EYE SYNDROME OPHTHA ROTATION 5 | 7
MANAGEMENT
MANAGEMENT BASED ON PATHOPHYSIOLOGY
Doc: How do we manage dry eyes? The simplest answer is replacement –
artificial tears. Though there are subtleties in the prescription of
lubricants. Most are OTC, believed not to cause serious side effects.
However, because of the way they are prescribed – liberally, in other
words, if it’s a good enough lubricant, you don’t have to worry about
Showing different degrees of blockade overdose. You can put it as often as you want based on the symptoms you
LEFT MOST: normal are feeling. However, if you are a bit obsessive compulsive, it can form
RIGHTMOST: most abnormal into a habit of dry eye, blinking, and putting drops – which is
counterproductive. They are OTC because they are relatively cheaper,
laden with preservatives to keep bottles in stock. However, the
HD ANALYZER preservatives can cause irritation and dry eyes as well. Now, you’re
hooked in the vicious cycle of buying lubricants because there is
something in the lubricant causing dry eyes as well. So, when you buy,
A measurement of a high
make sure it is preservative free and appropriate to your condition. Also,
order aberration. It will
there is a degree of severity where you give the appropriate type of
show the effect of dry
lubricant.
eyes on the vision based
on the concept of ocular
• Adding Tears
scatter index. The ocular
o Using artificial tears
scatter index is a
o Use preservative-free tears if patient is allergic
measurement that shows
the quality of vision. This
is more accurate than
the traditional Snellen’s
test.
• Conserving Tears
o Blocking the tear ducts
o Tiny silicone or gel plugs (punctal plug) may be
inserted in the tear ducts
Blocking the punctum
to have an intentional
epiphora to dry eyes.
It shows stability of the vision after the patient holds the blink or holds • Increasing your tears
the stare. If the vision or quality of vision doesn’t change, we can deduct o by using a special eyedrop medication
that the patient has no problem with dry eyes. However, if the vision
changes, there is the effect of dry eyes.
• Treating dry eye culprits
o prescription eye drops or ointments
▪ ointment if a very severe meibomian gland
dysfunction
▪ gel-like so that it stays longer in the eye
o warm compresses on the eyes
o massaging your eyelids
o certain eyelid cleaners
▪ can release the blockade
WHISKY, SWIRLY DRY EYE SYNDROME OPHTHA ROTATION 6 | 7
• Dry Eye Prevention CATEGORIES OF DRY EYE TREATMENTS
o try not to use a hair dryer, if possible
o stay away from very warm rooms Type of Therapy Treatment
o in the winter, add moisture to the air with the Environmental/ • Education and Environment modifications* (eg
humidifier. Or put a pan of water near your heater or Exogenous humidifier)
radiator • Elimination of offending topical and/or systemic
o protect your eyes from drying wind by wearing wrap- medications
around glasses outside Medication
o talk to your ophthalmologist about adding omega-3 Topical • Artificial tear substitutes; gels/ointments*
fatty acids for dry eye relief. They are found naturally • Anti-inflammatory agents (topical cyclosporine
in oily fish (such as tuna, salmon, sardines, tuna, and corticosteroids)
trout, and anchovies), and in flaxseeds. Omega-3 • Mucolytic agents
fatty acids can be added as a dietary supplement (pill • Autologous serum tears
or tablet). Systemic • Omega 3 fatty acids*
o Use artificial tear ointment or thick eye drops just • Tetracyclines* (for meibomianitis, rosacea)
before you go to bed to prevent waking up with dry • Systemic anti-inflammatory agents
and scratchy eyes.
Surgical • Punctal plugs
• Permanent punctal occlusion
* If you are fond of devices, especially in the pandemic, you tend to look
• Tarsorrhaphy*
at the devices from much longer time, and the blink rate diminishes. You • Repair of eyelid (malpositions or exposure)*
are staring at the screen for a long time – you will have symptoms of dry
• Mucus membrane, amniotic membrane
eyes. Rest and put on some lubricant. transplantation
Other • Eyelid therapy (warm compress and eyelid
hygiene)*
• INTENSED PULSED LIGHT
• Contact lenses
o The light is absorbed by the blood vessels, it
• Moisture chamber spectacles*
generates heat in the dermal layer that melts the
* Particularly helpful for increased evaporative loss
secretions and opens the glands
o The absorption of light and thermal action inside the
Data from Pflugfelder SC (Chair). Management and Therapy
blood vessels result in vasoconstriction to the vessel
Subcommittee of the International Dry Eye Workshop. Management and
endothelial lining, hence it decreases the
Therapy of dry eye disease: report of the Management and Therapy
inflammatory cytokines that contribute to
Subcommittee of the International Dry Eye Workshop (2007). Ocul Surf
Meibomian gland dysfunction
2007;5:163-78.
First one is topical medications.
Secretagogue – which not only replaces but pumps up the tears. One
brand – Diquas by Santen.
Anti-inflammatory agents like steroids with the provision that you
monitor the patient for adverse effect.
Topical interferon which aids in inflammation. Surgical – punctal plug.
Tarsorrhaphy – in cases of patient who cannot blink their eyes.
Gel-like usually reserved for severe dry eyes
*********END OF LECTURE*********
Heat and massaging function of meibomian gland, which helps in the Reference: PPT and lecture video
production of the oily layer of tear film.
If you notice the meibomian graph, if you see a lot of drop out, we
recommend this. The results are quite dramatic – you have subjective
feelings of relief and there is an objective measurement in the meibomian
graph, that some meibomian glands are liberated.
Lower left pic: The white is the patch of the eye. Because we do not want
any retinal toxicity. The arrow is where the light pulse is applied. About 5
applications in the lower eyelid is done. It causes liberation of the
gland/block.
WHISKY, SWIRLY DRY EYE SYNDROME OPHTHA ROTATION 7 | 7
You might also like
- CorneaDocument465 pagesCorneawisinasa100% (2)
- CPG 19Document78 pagesCPG 19anon-24970100% (1)
- Dry EyeDocument2 pagesDry EyeDaya PNo ratings yet
- Ophthalmology: Almendrala-Molina, Jorja Post Graduate InternDocument65 pagesOphthalmology: Almendrala-Molina, Jorja Post Graduate InternJajaAlmendralaNo ratings yet
- The Lacrimal System: Lynn E. Lawrence, CPOT, ABOC, COA, OSCDocument31 pagesThe Lacrimal System: Lynn E. Lawrence, CPOT, ABOC, COA, OSCUlayya Ghina NabillaNo ratings yet
- Topic 12-Special Senses: Eyes: Name: Jewel Eve Balida Competency Appraisal Date: 10/17/16Document9 pagesTopic 12-Special Senses: Eyes: Name: Jewel Eve Balida Competency Appraisal Date: 10/17/16Lewej Eve Laurente AdilabNo ratings yet
- Corneal Dystrophies: Retinal DetachmentDocument5 pagesCorneal Dystrophies: Retinal DetachmentCake ManNo ratings yet
- DRY EYE AgungDocument23 pagesDRY EYE AgungGustiAngriAngalanNo ratings yet
- The Tearing Patient: Diagnosis and Management: Ophthalmic PearlsDocument3 pagesThe Tearing Patient: Diagnosis and Management: Ophthalmic PearlsAnonymous otk8ohj9No ratings yet
- Dry Eye Syndrome OverviewDocument7 pagesDry Eye Syndrome OverviewhaninamaulianiNo ratings yet
- Dry Eye SyndromeDocument39 pagesDry Eye Syndromeمحمد عمر الجركNo ratings yet
- Eye and Vision Problems GuideDocument11 pagesEye and Vision Problems GuideDarius CrisostomoNo ratings yet
- Perceptual DisturbancesDocument7 pagesPerceptual DisturbancesVin SageNo ratings yet
- The EyeDocument8 pagesThe Eyezyrine jhen100% (1)
- The CorneaDocument60 pagesThe CorneaSarahNo ratings yet
- Marco-Equinox-Patient Hand OutDocument2 pagesMarco-Equinox-Patient Hand OutDr. Richard JohnsonNo ratings yet
- Unit 3Document14 pagesUnit 3Krunal ParmarNo ratings yet
- Corneal Dystrophies, Contact Lenses, and Retinal Detachment GuideDocument6 pagesCorneal Dystrophies, Contact Lenses, and Retinal Detachment GuideMarissa AsimNo ratings yet
- General Eye Care: Prepared By: Ma. Elena Fe G. Acosta, SN4, HTUDocument26 pagesGeneral Eye Care: Prepared By: Ma. Elena Fe G. Acosta, SN4, HTUmefacostaNo ratings yet
- The Healthy Eye: Structure, Function and Common Eye DiseasesDocument38 pagesThe Healthy Eye: Structure, Function and Common Eye DiseasesHasnain Ahmad KhanNo ratings yet
- Secondary Glaucoma IGADocument28 pagesSecondary Glaucoma IGANur JannahNo ratings yet
- M040GB014A00A-DOC00 - Smart ScreeningDocument11 pagesM040GB014A00A-DOC00 - Smart Screeningrocol.aplicaciones2No ratings yet
- Eyes, Ears, Nose, Throat and Mouth AssessmentDocument86 pagesEyes, Ears, Nose, Throat and Mouth AssessmentD A M N E R ANo ratings yet
- Special Senses (1)Document8 pagesSpecial Senses (1)Giane Qeirr Osias TimmalogNo ratings yet
- Red Eye - Conjunctivitis I Dr. Nuke Erlina Mayasari, SPMDocument23 pagesRed Eye - Conjunctivitis I Dr. Nuke Erlina Mayasari, SPMismkipendprowil2No ratings yet
- NCM 114 Finals LectureDocument11 pagesNCM 114 Finals LectureClea Amber FullanteNo ratings yet
- Secondary Glaucomas: Printed July 2014 Review Date July 2017Document28 pagesSecondary Glaucomas: Printed July 2014 Review Date July 2017Anonymous YYWsfmocYNo ratings yet
- Chp6 Ocular Surface DiseasesDocument31 pagesChp6 Ocular Surface DiseasesarifdikmanNo ratings yet
- BLEPHAROKERATOCONJUNCTIVITIS: EYE INFLAMMATIONDocument15 pagesBLEPHAROKERATOCONJUNCTIVITIS: EYE INFLAMMATIONWaiwit KritayakiranaNo ratings yet
- Computer Vision Syndrome and Dry Eye: Causes, Symptoms, and TreatmentsDocument37 pagesComputer Vision Syndrome and Dry Eye: Causes, Symptoms, and TreatmentsIntan Winta PratiwiNo ratings yet
- Anatomyphysiology ReviewerDocument116 pagesAnatomyphysiology Reviewerrosekatekate929No ratings yet
- Assessing The EyesDocument61 pagesAssessing The EyessrslytrdNo ratings yet
- ATENGCO - Activity11 The Sense OrgansDocument8 pagesATENGCO - Activity11 The Sense OrgansJoann Mae PudaderaNo ratings yet
- Chapter 8 AnaPhyDocument15 pagesChapter 8 AnaPhyCorinne VizcondeNo ratings yet
- 4 23Document8 pages4 23Camila Díaz QuinterosNo ratings yet
- DISORDERS of The EYE and EARDocument8 pagesDISORDERS of The EYE and EARAnna Carmela P. MelendezNo ratings yet
- Dry EyeDocument36 pagesDry EyeJ NATASHA MARIANo ratings yet
- DARE's Eye PDFDocument33 pagesDARE's Eye PDFvirag.patilNo ratings yet
- Dry Eye Investigation Management 2003Document18 pagesDry Eye Investigation Management 2003Harminul Isya100% (1)
- 8 Lacrimal Drainage System Diseases by James PMDocument63 pages8 Lacrimal Drainage System Diseases by James PMCharles AntonyNo ratings yet
- Eye PDFDocument16 pagesEye PDFhasbshahNo ratings yet
- The EyeDocument48 pagesThe Eyezyrine jhen100% (1)
- Special SensesDocument10 pagesSpecial SensesEthel May AlabastroNo ratings yet
- Eyelid Orbit and ConjunctivaDocument123 pagesEyelid Orbit and ConjunctivaRgdNo ratings yet
- Eye PPT 01Document21 pagesEye PPT 01zzzNo ratings yet
- NursingDocument4 pagesNursingAndrea Jewel BaladjayNo ratings yet
- Danni All'occhio Dopo Intervento Da Neurinoma AcusticoDocument20 pagesDanni All'occhio Dopo Intervento Da Neurinoma Acusticoctenzo56No ratings yet
- Human Eye Sec4 BioDocument10 pagesHuman Eye Sec4 BioFrancine TheophilaNo ratings yet
- U2 OphthalmicTerminologyDocument6 pagesU2 OphthalmicTerminologyAlberto Ybañez CastañedaNo ratings yet
- The Human EyeDocument33 pagesThe Human Eyegrace liwantoNo ratings yet
- DRY EYE AgungDocument23 pagesDRY EYE AgungGustiAngriAngalanNo ratings yet
- Dry Eye AgungDocument23 pagesDry Eye AgungAgung TriatmojoNo ratings yet
- Mata Merah 2Document26 pagesMata Merah 2Miftahuljnh01No ratings yet
- Eye ExaminationDocument34 pagesEye ExaminationSashwini DheviNo ratings yet
- Visual SystemDocument6 pagesVisual SystemJobelle Acena100% (1)
- Anatomy of Human EyeDocument41 pagesAnatomy of Human EyeCarly MelachioNo ratings yet
- BlepDocument1 pageBlepSweet CandyNo ratings yet
- Assessment of The EyesDocument9 pagesAssessment of The Eyesmarkkkkkkkheeess100% (3)
- Journal Article 27 487 PDFDocument4 pagesJournal Article 27 487 PDFrifkidwianugrahNo ratings yet
- The Lacrimal System: Anatomy and FunctionDocument6 pagesThe Lacrimal System: Anatomy and FunctionIon NagomirNo ratings yet
- Dry Eye SyndromeDocument69 pagesDry Eye Syndromeendalew mulugetaNo ratings yet
- Low Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsFrom EverandLow Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsNo ratings yet
- Wound ManagementDocument53 pagesWound ManagementJay DeeNo ratings yet
- Foreign Body Airway Obstruction First AidDocument87 pagesForeign Body Airway Obstruction First AidPrincess Cate MercadoNo ratings yet
- Types of Wounds 2Document30 pagesTypes of Wounds 2Jay Dee100% (1)
- EMED4Document59 pagesEMED4Princess Cate MercadoNo ratings yet
- EMED2Document23 pagesEMED2Princess Cate MercadoNo ratings yet
- Types of Wounds 2Document30 pagesTypes of Wounds 2Jay Dee100% (1)
- FB Airway Obstruction in Adults & ChildrenDocument28 pagesFB Airway Obstruction in Adults & ChildrenPrincess Cate MercadoNo ratings yet
- Emed - BLS - FBAO - First Aid Part 1Document85 pagesEmed - BLS - FBAO - First Aid Part 1Princess Cate MercadoNo ratings yet
- Emed - BLS - FBAO - First Aid Part 1Document85 pagesEmed - BLS - FBAO - First Aid Part 1Princess Cate MercadoNo ratings yet
- Wound ManagementDocument53 pagesWound ManagementJay DeeNo ratings yet
- Special Resuscitation Situations: Stroke, Hypothermia, Anaphylaxis, Drowning, Trauma, PregnancyDocument55 pagesSpecial Resuscitation Situations: Stroke, Hypothermia, Anaphylaxis, Drowning, Trauma, PregnancyPrincess Cate MercadoNo ratings yet
- Emed - TriageDocument54 pagesEmed - TriagePrincess Cate MercadoNo ratings yet
- Emed - Pedia2 GiNeuroDocument7 pagesEmed - Pedia2 GiNeuroPrincess Cate MercadoNo ratings yet
- Shock: Types, Causes, Signs and TreatmentDocument34 pagesShock: Types, Causes, Signs and TreatmentPrincess Cate MercadoNo ratings yet
- Emed - Advance Cardiac Life Support (Doc Vito)Document38 pagesEmed - Advance Cardiac Life Support (Doc Vito)Princess Cate MercadoNo ratings yet
- RV Ollero MD's Guide to Advanced Trauma Life SupportDocument18 pagesRV Ollero MD's Guide to Advanced Trauma Life SupportPrincess Cate MercadoNo ratings yet
- Emed - Trauma Life Support (Doc Ollero)Document51 pagesEmed - Trauma Life Support (Doc Ollero)Princess Cate MercadoNo ratings yet
- Wound Closure TechniqueDocument73 pagesWound Closure TechniqueJay DeeNo ratings yet
- Emed - Principles of Poison ManagementDocument40 pagesEmed - Principles of Poison ManagementPrincess Cate MercadoNo ratings yet
- Emed - Pedia 1Document7 pagesEmed - Pedia 1Princess Cate MercadoNo ratings yet
- Emed - Pulmonary EmergenciesDocument13 pagesEmed - Pulmonary EmergenciesPrincess Cate MercadoNo ratings yet
- Emed - Airway Management of The Trauma VictimDocument49 pagesEmed - Airway Management of The Trauma VictimPrincess Cate MercadoNo ratings yet
- Emed - Pulmonary Emergencies (Doc Vito) .PDFXDocument13 pagesEmed - Pulmonary Emergencies (Doc Vito) .PDFXPrincess Cate MercadoNo ratings yet
- Emed - OB Part 1Document6 pagesEmed - OB Part 1Princess Cate MercadoNo ratings yet
- Emed - Advance Cardiac Life SupportDocument45 pagesEmed - Advance Cardiac Life SupportPrincess Cate MercadoNo ratings yet
- Suture MaterialsDocument39 pagesSuture MaterialsJay DeeNo ratings yet
- Emed - Head Injuries (Doc Ollero)Document49 pagesEmed - Head Injuries (Doc Ollero)Princess Cate MercadoNo ratings yet
- Emed DR de Guzman SamplexDocument2 pagesEmed DR de Guzman SamplexMarco TolentinoNo ratings yet
- Emed - OB Part 2Document4 pagesEmed - OB Part 2Princess Cate MercadoNo ratings yet
- ACLSDocument37 pagesACLSWendy LucasNo ratings yet
- Shadrack Muma ThesisDocument74 pagesShadrack Muma ThesisJune BellNo ratings yet
- Vernal Keratoconjunctivitis: Moderator-Dr. Seema Meena Presenter - Dr. Sulabh SahuDocument58 pagesVernal Keratoconjunctivitis: Moderator-Dr. Seema Meena Presenter - Dr. Sulabh SahuSulabh SahuNo ratings yet
- Eyelid & Lacrimal DisordersDocument35 pagesEyelid & Lacrimal Disordersputri wid100% (1)
- Dry Eye ManagementDocument8 pagesDry Eye ManagementMul YaniNo ratings yet
- Wang 2005Document10 pagesWang 2005Anggia BungaNo ratings yet
- Computer Vision Syndrome (Digital Eye Strain) - EyeWikiDocument12 pagesComputer Vision Syndrome (Digital Eye Strain) - EyeWikiYeremia JerryNo ratings yet
- Contact Lenses and Associated AnteriorDocument13 pagesContact Lenses and Associated AnteriorJose Antonio Fuentes VegaNo ratings yet
- Lipofilm Microemulsion Effectiveness in Dry EyeDocument5 pagesLipofilm Microemulsion Effectiveness in Dry Eyedr.cintaNo ratings yet
- KeratitisDocument70 pagesKeratitisHoopmen Silaen100% (1)
- Eyes Condition Associated With Exposure To HazeDocument15 pagesEyes Condition Associated With Exposure To HazeTria PahanNo ratings yet
- Frequency and Risk Factors of Symptomatic Dry Eye Disease at Tertiary Care Eye Hospital, KarachiDocument4 pagesFrequency and Risk Factors of Symptomatic Dry Eye Disease at Tertiary Care Eye Hospital, KarachiekalapaleloNo ratings yet
- Anatomi Dan Fisiologi KorneaDocument133 pagesAnatomi Dan Fisiologi KorneaAriyanie NurtaniaNo ratings yet
- Cornea and External DiseaseDocument26 pagesCornea and External Diseaserajeshwari saravananNo ratings yet
- EYE DISORDERS: GLAUCOMA AND CATARACTSDocument127 pagesEYE DISORDERS: GLAUCOMA AND CATARACTSjoan olanteNo ratings yet
- Rev G - TearLab Osmolarity System User Manual - EnglishDocument20 pagesRev G - TearLab Osmolarity System User Manual - EnglishRommel ValladaresNo ratings yet
- Dry EyeDocument36 pagesDry EyeJ NATASHA MARIANo ratings yet
- How Does Radiation Therapy Work?Document5 pagesHow Does Radiation Therapy Work?mikeadrianNo ratings yet
- BLEPHAROKERATOCONJUNCTIVITIS: EYE INFLAMMATIONDocument15 pagesBLEPHAROKERATOCONJUNCTIVITIS: EYE INFLAMMATIONWaiwit KritayakiranaNo ratings yet
- Drug Rewetting Drops, Artificial TearsDocument1 pageDrug Rewetting Drops, Artificial TearsSrkocherNo ratings yet
- Oamjms 10b 668Document6 pagesOamjms 10b 668Faris Mufid MadyaputraNo ratings yet
- An Insight Into Meibomian Gland DysfunctionDocument22 pagesAn Insight Into Meibomian Gland DysfunctionvalbayerosNo ratings yet
- Hom M, Demodex - Clinical Cases & Diagnostic Protocol. OVS 2013Document8 pagesHom M, Demodex - Clinical Cases & Diagnostic Protocol. OVS 2013cassie_kuldaNo ratings yet
- Ocular Pharmacology - Dr. Fermin (2023)Document6 pagesOcular Pharmacology - Dr. Fermin (2023)Patricia Manalili100% (1)
- Senior Citizen's Day - 27 August 2019Document8 pagesSenior Citizen's Day - 27 August 2019Times MediaNo ratings yet
- A Review On Netra Tarpana - An Ayurveda Method of Eye Care: January 2021Document10 pagesA Review On Netra Tarpana - An Ayurveda Method of Eye Care: January 2021Lepaksha GowdaNo ratings yet
- Ophthalmology NotesDocument82 pagesOphthalmology NotesDr-Fadi AlkayyaliNo ratings yet
- Vision and Values: Teacher ManualDocument133 pagesVision and Values: Teacher ManualWim SupergansNo ratings yet
- MCQ in OphthalmologyDocument107 pagesMCQ in OphthalmologyDr-Arsalan Zahid100% (2)