Professional Documents
Culture Documents
Regulare Gastrică
Uploaded by
Aurelia AlexandraOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Regulare Gastrică
Uploaded by
Aurelia AlexandraCopyright:
Available Formats
01 PHYSIOLOGY
23. Gastric regulation
Describe what happens in the GI There are three main phases of gastric regulation:
tract when a meal is anticipated.
> Cephalic phase
> Gastric phase
> Intestinal phase.
Cephalic phase
These reflexes are decreased by stimulation of the sympathetic nervous
system with, for example, pain, fear and anxiety.
Thought, sight and smell of food
Stimulates
Cerebral cortex and hypothalamus
Stimulates
Medulla oblongata
Impulses from medulla travel via vagus
Vagus nerve
Submucosal plexus
Stomach – ↑ Gastric Juices Blood – ↑ Gastrin
Fig. 23.1 Cephalic phase
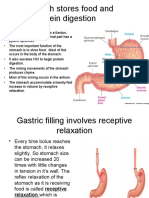
Gastric phase
> As food and fluid enter the stomach, stretch and chemoreceptors are
activated.
> This leads to a further increase in gastric secretions and increases
peristalsis.
> The tone of the lower oesophageal sphincter is increased to prevent
reflux of acid.
> Once the pH has reached 2, gastrin begins to exert a negative feedback
to inhibit further acid secretion.
Intestinal phase
This begins when chyme (food mixed with gastric juices) enters the
duodenum, causing the secretion of three main gut hormones:
> Gastric inhibitory peptide (GIP), which inhibits further gastric secretions
and motility
> Secretin, which inhibits further gastric secretions
> Cholecystokinin (CCK), which inhibits stomach emptying.
72
9781785230981_text.indb 72 24/02/16 9:36 pm
GASTRIC REGULATION
Describe the function of these There are four main hormones involved: gastrin, GIP, secretin and CCK.
gut hormones.
Table 23.1 Functions of gut hormones
Hormone Release stimulated by: Actions
Gastrin Cephalic phase ↑ Secretion of gastric juices
Stomach distension ↑ Motility
Proteins in stomach Encourages growth of mucosa
↑ pH of chyme in stomach Constricts LOS
Relaxes pyloric and ileocaecal sphincters
GIP Fatty acids in small intestine ↑ Insulin release
Inhibits secretion of gastric juices
Slows gastric emptying
Secretin Acidic chyme in small Stimulates contraction of gallbladder to release bile
intestine Stimulates release of pancreatic enzymes
Augments effect of CCK
CCK Amino acids in small intestine Stimulates contraction of gallbladder to release
Fatty acids in small intestine bile
Stimulates release of pancreatic enzymes
Induces feeling of satiety
Inhibits gastric emptying
Enhances actions of secretin
Describe the sphincters present A sphincter is a structure, usually made up of circular muscle, that surrounds
in the gastrointestinal tract. the opening of a hollow organ or body and constricts to close it. Sphincters
can be anatomical, where they are clearly different from the surrounding
tissue, e.g. the anus, or functional where the histological distinction is not so
clear, e.g. lower oesophageal sphincter. Sphincters can be under voluntary
or involuntary control. There are many sphincters in the gastrointestinal tract:
> Upper oesophageal
> Lower oesophageal
> Pyloric
> Ileocaecal
> Sphincter of Oddi
> Anus
Upper oesophageal sphincter: This is at the level of the C5–6 vertebrae
and is made up of the cricopharyngeal part of the inferior pharyngeal
constrictor muscle. It is under conscious control and in its resting state it is
usually constricted to avoid air being drawn into the stomach during breathing.
Lower oesophageal sphincter (also called the ‘cardiac’ sphincter): This
is a functional sphincter, found at the junction between the non-keratinised
squamous epithelium of the oesophagus and the simple columnar epithelium
of the stomach. Its function is to prevent reflux of the acidic stomach
contents into the oesophagus and so it is constricted at rest and has a
pressure of 15–20 mmHg. The sphincter opens ahead of peristalsis during
the process of swallowing to allow food and fluid to enter the stomach. It is
supplied by the vagus nerve.
‘Barrier pressure’ describes the difference between LOS pressure
and intragastric pressure. The closer the barrier pressure is to zero, the
more likely it is that reflux will occur. So, reducing LOS tone or increasing
intragastric pressure (e.g. pregnancy, full stomach, abdominal distension)
makes reflux more likely.
Pyloric sphincter: This is an anatomical sphincter found at the junction of
the stomach and duodenum. Its ring of muscle relaxes to allow chyme to
pass out of the stomach. It is supplied by the coeliac ganglion.
73
9781785230981_text.indb 73 24/02/16 9:36 pm
01 PHYSIOLOGY
Ileocaecal sphincter: An anatomical sphincter found at the junction of the
small and large bowels. It prevents reflux of colonic material into the ileum.
Sphincter of Oddi: This is a ring of muscle that surrounds the bile and
pancreatic ducts as they emerge into the lumen of the duodenum about
halfway down its length. The sphincter controls the release of bile and
pancreatic enzymes into the duodenum.
Anus: The gastrointestinal tract ends in a pouch called the rectum,
where faeces are stored prior to defecation. At the exit of the rectum is the
anorectal junction, a voluntary sphincter that is made up of an internal and
an external ring of muscle. The internal anal sphincter is supplied by the
hypogastric plexus. It is involuntary and will relax in response to stretching.
The external anal sphincter is voluntary and supplied by the inferior
rectal nerves.
LOS Tone
by: by:
C5-6 UOS -
Cholinergic stimulation Cholinergic inhibition CRICOPHARYNGEUS
Histamine Dopamine
Gastrin Oestrogen SNS T5 - L3
Motilin CCK
Secretin
PNS S2, 3, 4 LOS 15-25 mmHg
Pyloric G cells
Gastrin
Acid secretion
by: by:
Food/brain/mouth/stomach FA/Glucose/AA in small intestine
Stress H2 receptor antagonists/PPI
Gastrin Vagotomy
Alcohol/Caffeine CCK, GIP/Secretin
Secretin
Oxyntic Glands
Chief cells Pepsinogen
Mucus cell Mucus
Gastrin, ACh, Histamine
stimulates Parietal cells H+
Gastric Emptying
by: by:
Cholinergic stimulation Food
Metoclopramide Stress, Pain etc.
Neostigmine Old age
Diabetes
Obstruction
Pregnancy
Opiods
Anticholinergics
Sympathomimetics
Alcohol
PNS Parasympathetic nervous system
SNS Sympathetic nervous system
UOS Upper oesophageal sphincter
LOS Lower oesophageal sphincter
FA Fatty acids
AA Amino acids
PPI Proton pump inhibitors
Fig. 23.2 Overview of gastric regulation
74
9781785230981_text.indb 74 24/02/16 9:36 pm
You might also like
- Physiology, Lecture 8, GIT 2 (Stomach) (Slides)Document24 pagesPhysiology, Lecture 8, GIT 2 (Stomach) (Slides)Ali Al-Qudsi100% (2)
- HungerDocument2 pagesHungermeeraNo ratings yet
- Digestive SystemDocument8 pagesDigestive SystemAnamta AkhtarNo ratings yet
- GastricDocument21 pagesGastricParas TripathiNo ratings yet
- GI NeurotransmittersDocument1 pageGI NeurotransmittersMaryam FadahNo ratings yet
- Control of DigestionDocument5 pagesControl of DigestionMichael NyaongoNo ratings yet
- GI PHYSIOLDocument8 pagesGI PHYSIOL유예진No ratings yet
- GI HormonesDocument1 pageGI HormonesCarla CentenoNo ratings yet
- DIGESTIONDocument6 pagesDIGESTIONRane MandapatNo ratings yet
- Chapter 62: General Principles of GI Function-Motility, Nervous Control, and Blood CirculationDocument36 pagesChapter 62: General Principles of GI Function-Motility, Nervous Control, and Blood Circulationjackie funtanillaNo ratings yet
- GitDocument4 pagesGitSabbir AhmedNo ratings yet
- Digestive Physiology ExplainedDocument14 pagesDigestive Physiology ExplainedJãçk SparrowNo ratings yet
- Digestive System and Bioenergetics NotesDocument9 pagesDigestive System and Bioenergetics NotesDestinee LegendsNo ratings yet
- Physiology of Digestion in the StomachDocument187 pagesPhysiology of Digestion in the StomachJane Andrea Christiano Djianzonie100% (1)
- ProductsDocument4 pagesProductsstudy mailNo ratings yet
- 3 Gi Motility (Parts I-Iv) Swallowing & Esophageal MotilityDocument11 pages3 Gi Motility (Parts I-Iv) Swallowing & Esophageal MotilityLinh PhanNo ratings yet
- Gastrointestinal System Hormones and MediatorsDocument72 pagesGastrointestinal System Hormones and MediatorsAdvin BurkeNo ratings yet
- CPH 1902 Group PresentationDocument15 pagesCPH 1902 Group PresentationNicole MicallefNo ratings yet
- 2.6 Kontrol Saraf Hormon DigestivusDocument19 pages2.6 Kontrol Saraf Hormon DigestivusDewi Kartika SariNo ratings yet
- Hormone of Gi TractsDocument2 pagesHormone of Gi TractsMehedi hasan aponNo ratings yet
- Lecture-5 Hormonal Regulation of Intestinal MotilityDocument4 pagesLecture-5 Hormonal Regulation of Intestinal Motilityمرتضى حسين عبدNo ratings yet
- Feedback Circuites Regulate: Campbell 41.5Document26 pagesFeedback Circuites Regulate: Campbell 41.5Toka TariqNo ratings yet
- FISIOLOGIA GASTROINTESTINAL_43fde26492f2d4fd14857a5783846cfeDocument59 pagesFISIOLOGIA GASTROINTESTINAL_43fde26492f2d4fd14857a5783846cfecarlosNo ratings yet
- Gastrontestinal System: 2 Types of ContractionsDocument10 pagesGastrontestinal System: 2 Types of ContractionsReyjan Lozano ApolonioNo ratings yet
- Gastric Juice AnalysisDocument6 pagesGastric Juice Analysismaynard pascualNo ratings yet
- Pages From Physio Term 2Document453 pagesPages From Physio Term 2Deshi SportsNo ratings yet
- GI hormones, their origin, function and responseDocument1 pageGI hormones, their origin, function and responseMaryam FadahNo ratings yet
- Top Ten Topics Program Powered by ATPDocument53 pagesTop Ten Topics Program Powered by ATPNashir MahmudNo ratings yet
- Gastrointestinal HormonesDocument5 pagesGastrointestinal Hormonesanjali.jha1909No ratings yet
- Digestive System: Freshmen Year Program Medical School Universitas Islam Bandung 2011-2012Document125 pagesDigestive System: Freshmen Year Program Medical School Universitas Islam Bandung 2011-2012deasyahNo ratings yet
- 1.physiologe Emrcs2016Document117 pages1.physiologe Emrcs2016Farah FarahNo ratings yet
- Ondansetron: Gastric EmptyingDocument4,170 pagesOndansetron: Gastric EmptyingdrsaidumerNo ratings yet
- Git SecretionDocument3 pagesGit Secretionstudy mailNo ratings yet
- Gastric Juice (Autosaved)Document15 pagesGastric Juice (Autosaved)ZahidKhanNo ratings yet
- Physio 6. Digestive System 6Document21 pagesPhysio 6. Digestive System 6Xena XenaNo ratings yet
- Digestive System Processes and Regulation FunctionsDocument7 pagesDigestive System Processes and Regulation FunctionsMahadi Hasan KhanNo ratings yet
- Kontrol Sistem PencernaanDocument12 pagesKontrol Sistem PencernaanFatimah Azahra ZettaNo ratings yet
- Pancreatic JuiceDocument26 pagesPancreatic JuiceachalsinghbdnNo ratings yet
- Anatomy and Physiology of the Gastrointestinal TractDocument6 pagesAnatomy and Physiology of the Gastrointestinal TractjollypadillaNo ratings yet
- Hormone Secreted by Stimuli For Release Major ActivitiesDocument4 pagesHormone Secreted by Stimuli For Release Major ActivitiesYule RoxasNo ratings yet
- Unit 3. Digestive SystemDocument46 pagesUnit 3. Digestive SystemNURIA VAZQUEZNo ratings yet
- 5 Small IntestineDocument16 pages5 Small IntestineRayssa OliveiraNo ratings yet
- Physio Gastrointestinal Motility PDFDocument11 pagesPhysio Gastrointestinal Motility PDFKim RamosNo ratings yet
- Oleh: Dr. Herdiantri Sufriyana: @herdiantsDocument25 pagesOleh: Dr. Herdiantri Sufriyana: @herdiantsSheillaMerlyanaNo ratings yet
- Medical School Notes On Stomach IssuesDocument31 pagesMedical School Notes On Stomach IssuesDeji KajiNo ratings yet
- L 9. Physiology & Disorders of StomachDocument52 pagesL 9. Physiology & Disorders of Stomachsjfk1416No ratings yet
- The University of Lahore BDNS: Submitted To: Ma'Am Tara Khursheed Submitted by Group 5 & 10Document3 pagesThe University of Lahore BDNS: Submitted To: Ma'Am Tara Khursheed Submitted by Group 5 & 10Khazina MoazzamNo ratings yet
- Physiology Lecture 2 - Functions of the Stomach and Control of Gastric SecretionDocument32 pagesPhysiology Lecture 2 - Functions of the Stomach and Control of Gastric SecretionGracen33No ratings yet
- Stomach Anatomy, Functions and SecretionsDocument29 pagesStomach Anatomy, Functions and SecretionsSaad Zafar AwanNo ratings yet
- Gastrointestinal Physiology: Dr. Bipin Shrestha MBBS, MD 1Document50 pagesGastrointestinal Physiology: Dr. Bipin Shrestha MBBS, MD 1Prepladder ChyNo ratings yet
- GI Review BulletsDocument19 pagesGI Review Bulletsjanet_alexisNo ratings yet
- The Digestive System: SphinctersDocument33 pagesThe Digestive System: SphinctersJerome EkohNo ratings yet
- Cheat Sheet ExamsDocument5 pagesCheat Sheet ExamsSwe LayNo ratings yet
- Physiology: Stomach by DR Anam IsrarDocument20 pagesPhysiology: Stomach by DR Anam IsrarSaher Yasin100% (1)
- Regulation of GIT by gastrointestinal hormonesDocument13 pagesRegulation of GIT by gastrointestinal hormonesRaja Rashid IqbalNo ratings yet
- Movements of GITDocument69 pagesMovements of GITDisha SuvarnaNo ratings yet
- Digestive System: Anatomy and Functions of the StomachDocument28 pagesDigestive System: Anatomy and Functions of the StomachNaveelaNo ratings yet
- ControlDocument12 pagesControlSirVietaNo ratings yet
- Gastric SecretionDocument45 pagesGastric SecretionAzeeza Elya100% (1)
- Anti Fribrinolitic DrugsDocument15 pagesAnti Fribrinolitic DrugsAurelia AlexandraNo ratings yet
- 22 The Application of Farmacodynamics in The Optimization of Antibiotic Therapy PDFDocument2 pages22 The Application of Farmacodynamics in The Optimization of Antibiotic Therapy PDFAurelia AlexandraNo ratings yet
- Ultrasound Și DopplerDocument3 pagesUltrasound Și DopplerAurelia AlexandraNo ratings yet
- Hypotermia and HipertermiaDocument9 pagesHypotermia and HipertermiaAurelia AlexandraNo ratings yet
- Airway Management - Supraglottic Airway PDFDocument4 pagesAirway Management - Supraglottic Airway PDFPiet Pogen PoelNo ratings yet
- The Primary FRCA Structured Oral Examination: Study Guide 1Document13 pagesThe Primary FRCA Structured Oral Examination: Study Guide 1Aurelia Alexandra0% (1)
- Cursuri de Revisitare Și ValveDocument4 pagesCursuri de Revisitare Și ValveAurelia AlexandraNo ratings yet
- Sisteme de BreathingDocument5 pagesSisteme de BreathingAurelia AlexandraNo ratings yet
- Pulse OximetryDocument3 pagesPulse OximetryAurelia AlexandraNo ratings yet
- Lasers: What Do You Understand by The Term Laser'?Document3 pagesLasers: What Do You Understand by The Term Laser'?Aurelia AlexandraNo ratings yet
- ADâncimea de Anestezie MOnITORINGDocument3 pagesADâncimea de Anestezie MOnITORINGAurelia AlexandraNo ratings yet
- CT Și RMNDocument3 pagesCT Și RMNAurelia AlexandraNo ratings yet
- Presiune de Sânge MeasurementDocument3 pagesPresiune de Sânge MeasurementAurelia AlexandraNo ratings yet
- Vaporisers: Classify The Types of Vaporiser in UseDocument7 pagesVaporisers: Classify The Types of Vaporiser in UseAurelia AlexandraNo ratings yet
- Neuromuscular Blockade MonitoringDocument7 pagesNeuromuscular Blockade MonitoringAurelia AlexandraNo ratings yet
- venTILATORIDocument3 pagesvenTILATORIAurelia AlexandraNo ratings yet
- Monitori de DiscnecțieDocument2 pagesMonitori de DiscnecțieAurelia AlexandraNo ratings yet
- Temperature MeasurementDocument4 pagesTemperature MeasurementAurelia AlexandraNo ratings yet
- Featuri de Siguranță A Machinelor AnesteziceDocument3 pagesFeaturi de Siguranță A Machinelor AnesteziceAurelia AlexandraNo ratings yet
- PH MeasurementDocument2 pagesPH MeasurementAurelia AlexandraNo ratings yet
- Poluare Și ScavengingDocument3 pagesPoluare Și ScavengingAurelia AlexandraNo ratings yet
- Oxygen MeasurementDocument4 pagesOxygen MeasurementAurelia AlexandraNo ratings yet
- Presiune Arterială WaveformDocument3 pagesPresiune Arterială WaveformAurelia AlexandraNo ratings yet
- COMPONENTE eLeCTRICEDocument3 pagesCOMPONENTE eLeCTRICEAurelia AlexandraNo ratings yet
- Cardiac Utput MonitoringDocument7 pagesCardiac Utput MonitoringAurelia AlexandraNo ratings yet
- Carbon Dioxide MeasurementDocument2 pagesCarbon Dioxide MeasurementAurelia AlexandraNo ratings yet
- Adaptarea Gazelor MediceDocument4 pagesAdaptarea Gazelor MediceAurelia AlexandraNo ratings yet
- SIGURANȚĂ eLeCTRICĂDocument3 pagesSIGURANȚĂ eLeCTRICĂAurelia AlexandraNo ratings yet
- States of Matter, Heat Capacity and Latent Heat: PhysicsDocument7 pagesStates of Matter, Heat Capacity and Latent Heat: PhysicsAurelia AlexandraNo ratings yet
- ReFLexeSDocument2 pagesReFLexeSAurelia AlexandraNo ratings yet
- Cervicogenic HeadacheDocument8 pagesCervicogenic HeadacheEmma KopcikasNo ratings yet
- Group 3 and 4 MCN UpdatesDocument11 pagesGroup 3 and 4 MCN UpdatesDance TagleNo ratings yet
- 2316 Clia 900 EngDocument4 pages2316 Clia 900 EngOsama Ben DawNo ratings yet
- NCP4Document4 pagesNCP4Noreen GyleNo ratings yet
- Doctors Missed Call ReportDocument18 pagesDoctors Missed Call ReportVijaykumar MankaniNo ratings yet
- Near DrowningDocument53 pagesNear DrowningDr. Anish GolchhaNo ratings yet
- Hydatidiform MoleDocument2 pagesHydatidiform MolePaola AgustinNo ratings yet
- Venturi Mask RevealedDocument1 pageVenturi Mask RevealedTommy JNo ratings yet
- Unit 3 Part 2 Rheumatoid ArthritisDocument10 pagesUnit 3 Part 2 Rheumatoid ArthritisReman AlingasaNo ratings yet
- H2T Assessment RubricDocument3 pagesH2T Assessment Rubricalicia KNo ratings yet
- Hematology Review Section on Blood Cells and DevelopmentDocument79 pagesHematology Review Section on Blood Cells and DevelopmentLUZVIMINDA GORDONo ratings yet
- 2011.Three-Dimensional - Esthetic Analysis in Treatment PlanningDocument18 pages2011.Three-Dimensional - Esthetic Analysis in Treatment PlanningCarolina Rodríguez RamírezNo ratings yet
- TORCH in PregnancyDocument122 pagesTORCH in PregnancyroserosannaNo ratings yet
- Ear Disorder Multiple Choice Questions-RationaleDocument5 pagesEar Disorder Multiple Choice Questions-Rationalemydewyboy83% (6)
- Bronchial AsthmaDocument3 pagesBronchial AsthmaSabrina Reyes0% (1)
- BLS MCQDocument22 pagesBLS MCQGeraldine Augusta100% (1)
- SouvenirDocument86 pagesSouvenirMohak AroraNo ratings yet
- FHPL Network Hopsitals List - 7dec2017Document819 pagesFHPL Network Hopsitals List - 7dec2017Badhra Rao100% (2)
- Anesthesia MCQ 425Document4 pagesAnesthesia MCQ 425dungulu50% (2)
- UH Neurosurgery Tips: Presenting on RoundsDocument2 pagesUH Neurosurgery Tips: Presenting on RoundsAndré PérezNo ratings yet
- 19 Prenatal and Antepartum ManagementDocument34 pages19 Prenatal and Antepartum ManagementMichelle Joy M. VicenteNo ratings yet
- Wound Healing, Tissue Repair, and FibrosisDocument28 pagesWound Healing, Tissue Repair, and FibrosisRibka Theodora100% (1)
- Apache ScoreDocument36 pagesApache ScoreSugianto Parulian SimanjuntakNo ratings yet
- DIPHENHYDRAMINE HYDROCHLORIDE-diphenhydramine Hydrochloride Injection, S Olution Mylan Ins Titutional LLCDocument7 pagesDIPHENHYDRAMINE HYDROCHLORIDE-diphenhydramine Hydrochloride Injection, S Olution Mylan Ins Titutional LLCNur As-Syifa AzzahraNo ratings yet
- Case History Surgery Chole CystitisDocument23 pagesCase History Surgery Chole CystitisMardiana KamalNo ratings yet
- FCCS - VentilatorDocument18 pagesFCCS - VentilatorEga Jaya100% (2)
- Cardio SLE Mcqs With AnswersDocument37 pagesCardio SLE Mcqs With AnswersAsif Newaz100% (4)
- PT Joint Mobilization TechniquesDocument5 pagesPT Joint Mobilization TechniquesHari PrasadNo ratings yet
- First Aid For Gunshot Wounds and FracturesDocument42 pagesFirst Aid For Gunshot Wounds and FracturesIfedigbo-Ejidike NwamakaNo ratings yet
- Sign 108Document108 pagesSign 108Fibrianti Ratna SariNo ratings yet