Professional Documents
Culture Documents
Respiratory System Anatomy
Uploaded by
ALEXANDRA SAN PEDROOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Respiratory System Anatomy
Uploaded by
ALEXANDRA SAN PEDROCopyright:
Available Formats
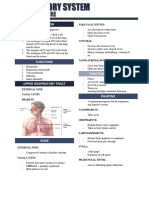
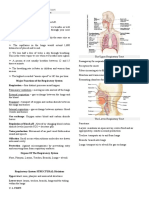
RESPIRATORY SYSTEM
Functions:
• Gas exchange
• Regulation of blood pH
• Voice production
• Olfaction
• Protection against some microorganisms
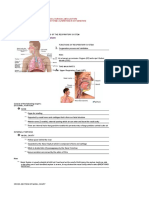
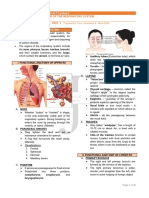
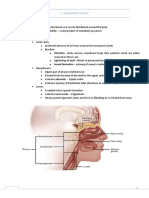
NOSE
- External nose and the nasal cavity
o External nose
- Mainly composed of hyaline cartilage plates
- The bridge of the nose consists of the nasal bones
o Nasal cavity
- A passageway for air
- Cleans the air
- Humidifies and warms the air
- Contains the sensory organ for smell
- With the paranasal sinuses, it is a resonating chamber for
speech
Openings:
▪ Nares or nostrils: external openings
▪ Choanae: openings into the pharynx
❖ Vestibule
- Anterior part
❖ Hard palate
- Bony plate that forms the floor of the nasal cavity
- Separates the nasal cavity from the oral cavity
❖ Nasal septum
- Divides the nasal cavity into right and left parts
❖ Olfactory epithelium
- Most superior part of the nasal cavity
- Sensory organ for smell
❖ Conchae
- Bony ridges at the lateral walls of the nasal cavity
❖ Meatus
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 1 of 26
- Passageway beneath concha
- Superior & middle: paranasal sinuses
- Inferior: nasolacrimal duct
PHARYNX
- Common opening of both the digestive and respiratory
systems
- It receives air from the nasal cavity and receives air, food,
and drink from the oral cavity
o Nasopharynx
- Located posterior to the choanae and superior to the soft
palate
*An incomplete muscle and connective tissue partition
separating the nasopharynx from the oropharynx
*Prevents swallowed materials from entering the nasopharynx
and nasal cavity
*Two auditory tubes from the middle ears open into the
nasopharynx
*The posterior surface contains the pharyngeal tonsil, or
adenoid which helps defend the body against infection
o Oropharynx
- From the soft palate to the epiglottis
- Air, food, and drink all pass through the oropharynx
o Laryngopharynx
- Extends from the tip of the epiglottis to the esophagus and
passes posterior to the larynx
- Food and drink pass through the laryngopharynx to the
esophagus
LARYNX
- Located in the anterior part of the throat and extends from
the base of the tongue to the trachea
- Prevents the entry of swallowed materials into the lower
respiratory tract
- Regulates the passage of air into and out of the lower
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 2 of 26
respiratory tract
- 9 cartilages (6 paired; 3 unpaired)
Unpaired cartilages:
❖ Thyroid cartilage (Adam’s apple)
- The largest of the cartilages
❖ Cricoid cartilage
- Forms the base of the larynx on which the other cartilages
rest
❖ Epiglottis
- Attached to the thyroid cartilage and projects superiorly as a
free flap toward the tongue
Paired cartilages:
❖ Arytenoid
❖ Corniculate
❖ Cuneiform
- The superior ligaments are covered by a mucous membrane
called vestibular folds, or false vocal cords
- The inferior ligaments are covered by a mucous membrane
called the vocal folds, or true vocal cords
TRACHEA
- Windpipe
- A membranous tube attached to the larynx
- Consists of:
➢ 15 – 20 C-shaped pieces of hyaline cartilage which support
the anterior and lateral sides of the trachea
➢ Trachea muscle which support the posterior side of the
trachea
Tracheobronchial Tree:
1. Trachea
2. Primary (Main) Bronchi
3. Secondary (Lobar) Bronchi
4. Tertiary (Segmental) Bronchi
5. Bronchioles
6. Terminal bronchioles
7. Respiratory bronchioles
BRONCHI
o Carina
- The point where the trachea divides into right and left
primary bronchi
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 3 of 26
- Superior border of the fifth thoracic vertebra
o Right primary bronchus
- More vertical, shorter, and wider than the left
- Divides into 3 secondary bronchi
o Left primary bronchus
- Divides into 2 secondary bronchi
ALVEOLI
- Small, air-filled chambers where gas exchange between the
air and blood takes place
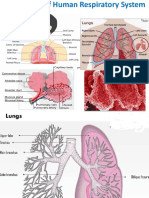
LUNGS
- The principal organs of respiration
- Each lung is conical in shape
- Base – rests on the diaphragm
- Apex – extends approximately 2.5 cm superior to the
clavicle
- The right lung is larger (620 g) than the left (560 g)
HILUM
- Where structures, such as the main bronchus, blood vessels,
nerves, and lymphatic vessels, enter or exit the lung
PLEURA
- Surround the lungs and provide protection against friction
RIGHT LUNG (10) LEFT LUNG (9)
SUPERIOR LOBE SUPERIOR LOBE
Apical Apicoposterior
Anterior Anterior
Posterior Superior lingula
Inferior lingula
MIDDLE LOBE
Lateral -
Medial
LOWER LOBE LOWER LOBE
Superior Superior
Anterior & Posterior Anterior & Posterior
Basal Basal
Medial & Lateral Medial & Lateral
Basal Basal
MUSCLES OF RESPIRATION
o Muscles of Inspiration
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 4 of 26
- Primary: Diaphragm
- Accessory: External intercostals, pectoralis minor, SCM,
and scalenes
o Muscles of Expiration
- Primary: None
- Accessory: Abdominal muscles and internal intercostals
BLOOD SUPPLY
- The deoxygenated blood flows through pulmonary arteries
to pulmonary capillaries, becomes oxygenated, and returns
to the heart through pulmonary veins
PULMONARY VOLUMES
o Tidal volume – the volume of air inspired or expired with
each breath (500 mL)
o Inspiratory reserve volume – the amount of air that can be
inspired forcefully after inspiration of the tidal volume
(3000 mL)
o Expiratory reserve volume – the amount of air that can be
forcefully expired after expiration of the tidal volume (1100
mL)
o Residual volume – the volume of air still remaining in the
respiratory passages and lungs after the most forceful
expiration (1200 mL)
PULMONARY CAPACITIES
o Inspiratory capacity – the amount of air that a person can
inspire maximally after a normal expiration
(TV + IRV = 3500 mL)
o Functional residual capacity – the amount of air
remaining in the lungs at the end of a normal expiration
(ERV + RV = 2300 mL)
o Vital capacity – the maximum level of air that a person can
expel from the respiratory tract after a maximum
inspiration
(IRV + ERV + TV = 4600 mL)
o Total lung capacity – the sum of the inspiratory and
expiratory reserve volumes plus the tidal volume and the
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 5 of 26
residual volume (5800 mL)
URINARY SYSTEM
Consists of:
• Two kidneys
• Two ureters
• Urinary bladder
• Urethra
Functions:
• Excretion
• Regulation of blood volume and pressure
• Regulation of concentration of solutes in the blood
• Regulation of the pH of the extracellular fluid
• Regulation of red blood cell synthesis
• Vitamin D synthesis
KIDNEYS
- Bean-shaped
- Each is about the size of a tightly clenched fist
- Extend from the level of the last thoracic (T12) to the third
lumbar (L3) vertebrae
- Liver is superior to the right kidney, causing the right kidney
to be slightly lower than the left
- Each kidney measures about 11 cm long, 5 cm wide, and 3
cm thick and weighs about 130 g
o Renal capsule – fibrous connective tissue surrounding
each kidney
o Perirenal fat – adipose tissue covering the capsule; acts as
a shock absorber, cushioning the kidneys are against
mechanical shock
o Renal fascia – anchors the kidneys and surrounding
adipose tissue to the abdominal wall
o Hilum – found on the medial side of each kidney, where
blood vessels and nerve enter and exit the kidney
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 6 of 26
o Renal sinus – where structures that enter and leave the
kidney pass through
➢ Outer cortex and inner medulla
o Renal pyramids – cone-shaped structures that make up the
medulla
o Bases of the pyramids – form the boundary between the
cortex and the medulla
o Renal papillae – tips of the pyramids that point toward the
renal sinus
o Renal columns – projects between the renal pyramids
o Minor calyces – funnel-shaped chambers into which the
renal papillae extend
o Major calyces – larger funnels formed by minor calyces of
several pyramids
➢ The major calyces converge to form the renal pelvis
➢ The renal pelvis narrows into the ureter
NEPHRON
- Functional unit of the kidney
- ~1.3 million in each kidney
- Parts:
▪ Renal corpuscle
▪ Proximal convoluted tubule
▪ Loop of Henle
▪ Distal convoluted tubule
▪ Collecting duct
▪ Papillary duct
o Renal corpuscle
- Bowman’s capsule
- Glomerulus
o Juxtamedullary nephrons
- Nephrons whose Bowman’s capsules lie near the medulla
- They have long loops of Henle which extend deep into the
medulla
- Only about 15%
o Cortical nephrons
- Their loops of Henle do not extend deep into the medulla
o Juxtaglomerular apparatus
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 7 of 26
- Juxtaglomerular cells of the afferent arteriole and the macula
densa
- Secretes the enzyme renin and plays an important role in the
autoregulation of filtrate formation and blood pressure
regulation
PART OF URINE DRAINAGE
GLOMERULUS
BOWMAN’S CAPSULE
PROXIMAL CONVOLUTED TUBULE
THICK DESCENDING LOOP OF HENLE
THIN DESCENDING LOOP OF HENLE
THIN ASCENDING LOOP OF HENLE
THICK ASCENDING LOOP OF HENLE
DISTAL CONVOLUTED TUBULE
COLLECTING DUCT
PAPILLARY DUCT
MINOR CALYX
MAJOR CALYX
RENAL PELVIS
URETER
URINARY BLADDER
URETHRA
URINE PRODUCTION
o Filtration – the movement of water and small solute across
the filtration membrane as a result of a pressure difference
*Filtrate: fluid entering the nephron
o Glomerular filtration rate (GFR) – the amount of filtrate
produced each minute; ~125 mL/minute or 180 L/day
o Tubular reabsorption – the movement of water and solutes
from the filtrate back into the blood
o Tubular secretion – the active transport of solutes across
the walls of the nephron into the filtrate
URETERS & URINARY BLADDER
o Ureters – tubes through which urine flows from the
kidneys to the urinary bladder
o Urinary bladder – a hollow, muscular container that lies in
the pelvic cavity
o Urethra – transports urine to the outside of the body
*WALLS (I-O)
- Transitional epithelium, lamina propria, muscular coat, and
fibrous adventitia
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 8 of 26
*WALL OF THE URINARY BLADDER IS THICKER
- Detrusor muscle
Urinary bladder
- Acts as a reservoir for urine until it can be eliminated
relatively quickly at an appropriate time and place
- Can distend to accommodate a large volume of fluid
*Maximum volume: 1 liter of urine
*Discomfort becomes noticeable when urine volume excess
approximately 500 mL
Urethra
o Internal urinary sphincter
- Elastic connective tissue and smooth muscle that keeps urine
from flowing out of the urinary bladder until the pressure in
the urinary bladder is great enough to force urine to flow
from it
o External urinary sphincter
- Skeletal muscle that surrounds the urethra as the urethra
extends through the pelvic floor
- Acts as a valve that controls the flow of urine through the
urethra
*Males – extends to the end of the penis, where it opens to the
outside
*Females – much shorter and opens into the vestibule anterior
to the vaginal opening
ENDOCRINE SYSTEM
- Composed of glands that typically secrete chemical signals
into the circulatory system
• Hormones
- Produced in minute amounts by a collection of cells
- Secreted into the interstitial spaces
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 9 of 26
- Enters the circulatory system, where it is transported some
distance
- Acts on target tissues, at another site un the body to
influence the activity of those tissues in a specific fashion
Functions:
• Metabolism and tissue maturation
• Ion regulation
• Water balance
• Immune system regulation
• Heart rate and blood pressure regulation
• Control of blood glucose and other nutrients
• Control of reproductive functions
• Uterine contractions and milk release
PITUITARY GLAND
- Hypophysis
- Secretes nine (9) major hormones that regulate numerous
body functions and the secretory activity of several other
endocrine glands
- Hypothalamus and pituitary gland are major sites where
the nervous and endocrine systems interact
- Hypothalamus regulates the secretory activity of the
pituitary gland
*The posterior pituitary is an extension of the
hypothalamus
- Roughly 1 cm in diameter, weighs 0.5-1.0 g, and rests in the
sella turcica of the sphenoid bone
- Connected to the hypothalamus by a
stalk of tissue
called the infundibulum
*Divided functionally into two parts:
➢ Posterior pituitary (neurohypophysis)
➢ Anterior pituitary (adenohypophysis)
o Posterior pituitary
- Neurohypophysis
- Extension of the hypothalamus
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 10 of 26
- Secretes neurohormones
o Anterior pituitary
- Three areas:
➢ Pars tuberalis
➢ Pars intermedia
➢ Pars distalis
HYPOTHALAMIC FUNCTIONS
HORMONES
Growth hormone- Increased growth
releasing hormone hormone secretion
(GHRH)
Growth hormone- Decreased growth
inhibiting hormone hormone secretion
(GHIH) or
somatostatin
Thyrotropin-releasing Increased thyroid-
hormone (TRH) stimulating hormone
secretion
Corticotropin- Increased
releasing hormone adrenocorticotropic
(CRH) hormone secretion
Gonadotropin- Increased secretion
releasing hormone LH and FSH
(GnRH)
Prolactin-releasing Increased or
hormone (PRH) and decreased prolactin
prolactin-inhibiting secretion
hormone (PIH)
POSTERIOR PITUITARY (NEUROHYPOPHYSIS)
HORMONES OF RESPONSE
THE PITUITARY
GLAND
Antidiuretic Hormone Increased water
(ADH) reabsorption
Oxytocin Increased uterine
contractions;
increased milk
expulsion from
mammary glands;
unclear function in
males
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 11 of 26
ANTERIOR PITUITARY (ADENOHYPOPHYSIS)
HORMONES OF RESPONSE
THE PITUITARY
GLAND
Growth hormone Increased growth in
(GH) tissues; increased
amino acid uptake &
protein synthesis
Thyroid-stimulating Increased thyroid
hormone (TSH) hormone secretion
Adrenocorticotropic Increased
hormone (ACTH) glucocorticoid
hormone secretion
Lipotropins Increased fat
breakdown
Endorphins Analgesia in the
brain; Inhibition of
gonadotropin-
releasing hormone
secretion
Melanocyte- Increased melanin
stimulating hormone production in
(MSH) melanocytes to make
the skin darker in
color
Luteinizing hormone Ovulation and
(LH) progesterone
production in ovaries,
testosterone synthesis
Follicle-stimulating Follicle maturation
hormone (FSH) and estrogen
secretion in ovaries;
sperm cell production
in testes
Prolactin Milk production in
lactating women;
Increased response of
follicle to LH and
FSH; unclear function
in males
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 12 of 26
THYROID GLAND
- Composed of two lobes connected by a narrow band of
thyroid tissue called the isthmus
- Weighs approximately 20 g
- Highly vascular and appears more red than its surrounding
tissues
o Thyroid follicles
- Triiodothyronine; T3 (10%)
- Tetraiodothyronine or Thyroxine; T4 (90%)
o Parafollicular cells
- Calcitonin
HORMONES FUNCTIONS
Thyroid hormones Increased metabolic
- Triiodothyronine T3 rate, essential for
- Tetraiodothyronine T4 normal process of
growth and
maturation
Calcitonin Decreased rate of
breakdown of bone
by osteoclasts;
prevention of a
large increase in
blood Ca levels
PARATHYROID GLAND
- Embedded in the posterior part of each lobe of thyroid gland
- Two cell types:
➢ Chief cells – secrete parathyroid hormone
➢ Oxyphils – unknown function
HORMONES FUNCTIONS
Parathyroid hormone Increased rate of
breakdown of bone
by osteoclasts;
increased
reabsorption of Ca in
kidneys; Increased
absorption of Ca from
the small intestine,
increased vitamin D
synthesis; increased
blood Ca levels
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 13 of 26
ADRENAL GLANDS
o Suprarenal glands – near the superior poles of the kidneys
o Retroperitoneal
o Adrenal cortex (O-I)
➢ Zona glomerulosa
➢ Zona fasciculata
➢ Zona reticularis
o Adrenal medulla
Hormones (Medulla)
- Flight or flight response
➢ Epinephrine & Norepinephrine
- Increased cardiac output, increased blood flow to skeletal
muscles, and increased blood flow to the heart;
Vasoconstriction of blood vessels, especially visceral and
skin blood vessels; Increased release of glucose and fatty
acids into blood; In general, preparation of physical activity
Hormones (Cortex)
➢ Androgens
- Zona reticularis
- Minor importance in males; In females, development of
some secondary sexual characteristics, such as axillary and
pubic hair
PANCREAS
- Lies behind the peritoneum between the greater curvature of
the stomach and the duodenum
- Elongated structure approximately 15 cm long; weighing
approximately 85 – 100 g
- Both an exocrine gland and an endocrine gland
*Exocrine portion consists of acini which produce pancreatic
juice
*Endocrine part consists of pancreatic islets (islets of
Langerhans) which secrete hormones
➢ Alpha cells (20%) – secrete glucagon
➢ Beta cells (75%) – secrete insulin
➢ Delta cells (5%) – secrete somatostatin
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 14 of 26
o Glucagon – increased uptake and use of glucose and
amino acids
o Insulin – increased breakdown of glycogen; release of
glucose into the circulatory system
o Somatostatin – inhibition of insulin and glucagon
secretion
TESTIS
Testosterone Aids in
spermatogenesis,
development of
genitalia;
maintenance of
functional
reproductive organs;
secondary sex
characteristics; sexual
behavior
Inhibin Inhibits FSH
secretion
OVARY
Estrogens Uterine and
mammary gland
development and
function;
menstruation
Progesterone Uterine and
mammary gland
development and
function;
menstruation
Inhibin Inhibits FSH
secretion
Relaxin Increases flexibility
of connective tissue
in the pelvic area;
especially in the
symphysis pubis
PINEAL BODY
- In the epithalamus
o Melatonin
- Inhibition of gonadotropin-releasing hormone-secretion,
thereby inhibiting reproduction; significance is not clear in
humans; may help regulate sleep-wake cycles
o Arginine
- Possible inhibition of gonadotropin-releasing hormone
secretion
THYMUS
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 15 of 26
- In the neck and superior to the heart in the thorax
o Thymosin
- Play an important role in the development and maturation of
the immune system
PANCREAS
o Glucagon – serves to keep blood glucose levels high
o Insulin – responsible for allowing glucose in the blood to
enter cells; breaks down fats or proteins for energy
o Somatostatin – inhibition of insulin and glucagon
secretion
REPRODUCTIVE SYSTEM
MALE REPRODUCTIVE SYSTEM
• Testes
• Series of ducts: epididymides, ductus deferentia, and
urethra
• Accessory glands: seminal vesicles, prostate gland, and
bulbourethral glands
• Supporting structure: scrotum and penis
Functions of MS:
• Production of sperm cells
• Sustaining and transfer of the sperm cells to the female
• Production of male sex hormones
SCROTUM
- Contains the testes and is divided into two internal
compartments by an incomplete connective tissue septum
- Raphe – an irregular ridge at the midline of the scrotum
- Dartos and cremaster muscles – help regulate testicular
temperature
PERINEUM
- The area between the thighs
- Boundaries:
➢ Anterior: symphysis pubis
➢ Posterior: coccyx
➢ Lateral: ischial tuberosities
- Two triangles
- Divided by the superficial transverse & deep transverse
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 16 of 26
perineal muscles
o Urogenital triangle
- Base of the penis and the scrotum
o Anal triangle
- Anal opening
TESTES
- Small, ovoid organs, each about 4-5 cm long, within the
scrotum
- Both an exocrine & endocrine gland
➢ Exocrine: sperm (seminiferous tubules)
➢ Endocrine: testosterone (interstitial or Leydig cells)
o Tunica albuginea – the outer connective tissue capsule of
the testes
- The seminiferous tubules empty into a set of short, straight
tubules, the tubuli recti, which in turn empty into a tubular
network called the rete testis
- The rete testis empties into 15-20 tubules called efferent
ductules
DUCTS
o Efferent ductules – extend from the testes to the head of
the epididymis
o Epididymis – a comma-shaped structure on the posterior
side of the testis that is the site of final sperm cell
maturation
- Head, body, and tail
- 12-16 days to travel through the epididymis and appear
in the ejaculate
o Ductus or Vas deferens – passes from the epididymis into
the abdominal cavity
➢ Spermatic cord: ductus deferens, testicular artery and
venous plexus, lymphatic vessels, and nerves
➢ Coverings of the spermatic cord (O-I): external
spermatic fascia, cremaster muscle, and internal
spermatic fascia
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 17 of 26
o Ejaculatory duct – formed by the end of the ductus
deferens, called the ampulla, and the seminal vesicle
- Approximately 2.5 cm long
- Project into the prostate gland and end by opening into
the urethra
URETHRA
- 20 cm long and extends from the urinary bladder to the
distal end of the penis
- Passageway for both urine and male reproductive fluids
o Prostatic urethra
- Connected to the bladder and passes through the
prostate gland
- Fifteen to 30 small ducts from the prostate gland and
the two ejaculatory ducts empty into the prostatic
urethra
o Membranous urethra
- Shortest part of the urethra
- Extending from the prostate gland through the
perineum
o Spongy or penile urethra
- Longest part of the urethra
- Extends from the membranous urethra through the
length of the penis
PENIS
- Contains three columns of erectile tissue
- Engorgement of this erectile tissue with blood causes
the penis to enlarge and become firm, a process called
erection
- Organ of copulation, through which sperm cells are
transferred from male to the female
o Two corpora cavernosa - form the dorsum and the sides
of the penis and expands at the base to form crus of the
penis
o Corpus spongiosum – forms the ventral portion of the
penis
- Expands at the base to form the bulb of the penis
- Expands to form a cap, the glans penis, over the distal
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 18 of 26
end of the penis
- Where the spongy urethra passes through, penetrates
the glans penis, and opens as the external urethral
orifice
o Root of the penis – bulb and crus of the penis
o Prepuce – a loose fold of skin that covers the glans penis
ACCESSORY GLANDS
o Seminal vesicles
- Sac-shaped glands located next to the ampulla of the
ductus deferentia; Empty into the ejaculatory ducts
o Prostate gland
- At the base of the urinary bladder, where it surrounds
the prostatic urethra and the two ejaculatory ducts
o Bulbourethral glands
- A pair of compound mucous glands that empty into the
spongy urethra
SEMEN - A composite of sperm cells and secretions from the
male reproductive glands
❖ Testes – 5%
❖ Seminal vesicle – 60%
❖ Prostate gland – 30%
❖ Bulbourethral glands – 5%
• Emission – the discharge of the secretions of the seminal
vesicles, prostate gland, and bulbourethral glands with
sperm cells from the epididymides into the urethra to
form semen
• Ejaculation – the forceful expulsion of semen from the
urethra caused by the contraction of the urethra, the
skeletal muscles in the floor of the pelvis, and the
muscles at the base of the penis
o Bulbourethral glands and urethral mucous glands
- Produce a mucous secretion just before ejaculation
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 19 of 26
• Lubricates the urethra, neutralizes the contents of
the normally acidic spongy urethra, provides a
small amount of lubrication during intercourse,
and helps reduce vaginal acidity
o Testis – sperm cells, a small amount of fluid, and
metabolic by products
o Seminal vesicles
- Large amounts of fructose, citric acid, and other
nutrients that that nourish the sperm cells
- Fibrinogen which is involved in a weak coagulation
reaction of the semen immediately after ejaculation
- Prostagalandins which can cause uterine contractions
MALE SEXUAL ACT
o Parasympathetic centers
➢ Erection
- First major component of the male sexual act
- The penis becomes enlarged and rigid
- The glands of the urethra and the bulbourethral glands
produce mucus
o Sympathetic centers
- Erection, emission, and ejaculation
FEMALE REPRODUCTIVE SYSTEM
• Ovaries
• Uterine tubes
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 20 of 26
• Uterus
• Vagina
• External genital organs
• Mammary glands
BROAD LIGAMENT
- An extension of the peritoneum that spreads out on
both sides of the uterus and to which the ovaries and
uterine tubes are attached
- Holds the internal reproductive organs in place
PARTS:
- Mesosalpinx
- Mesovarium
- Mesometrium
OVARIES
- Small organs about 2-3.5 cm long and 1-1.5 cm wide
o Mesovarium – peritoneal fold that attaches each ovary to
the posterior surface of the broad ligament
o Suspensory ligament – extends from the mesovarium to
the body wall
o Ovarian ligament – attaches the ovary to the superior
margin of the uterus
OVULATION
- Release of a secondary oocyte from an ovary
FERTILIZATION
- Begins when a sperm cell binds to the plasma membrane
and penetrates into the cytoplasm of a secondary oocyte
- Forms a zygote
*23 pairs (46) of chromosomes
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 21 of 26
*Divides by mitosis to form two cells, which divide to form
four cells, and so on
*The mass of cells formed, after about 7 days after
ovulation, may implant or attach to, the wall of the uterus
*The implanted mass of cells continues to develop to form,
after approximately 9 months, a new individual
UTERINE TUBES
- Fallopian tubes or oviducts
- Located along the superior margin of the broad ligament
o Mesosalpinx – part of the broad ligament most directly
associated with the uterine tube
- Opens directly into the peritoneal cavity to receive the
oocyte from the ovary
- It expands to form the infundibulum and long, thin
processes called fimbriae surround the opening of the
infundibulum
o Ampulla – nearest the infundibulum; widest and longest
part of the tube
o Isthmus – nearest the uterus; much narrower and has
thicker walls than does the ampulla
o Uterine or intramural part of the tube – passes through
the uterine wall and ends in a very small uterine opening
Layers of the uterine wall (O-I):
➢ Serosa
➢ Muscular
➢ Mucosa
- Provides nutrients for the oocyte or, if fertilization has
occurred, for the developing embryonic mass as it passes
through the uterine tube
- The ciliated epithelium helps move the small amount of
fluid and the oocyte, or the developing embryonic mass,
through the uterine tubes
UTERUS
- Fundus, body, and cervix
- Uterine cavity and the cervical canal are the spaces formed
by the uterus
- Uterus is held in place by the broad, round, and uterosacral
ligaments
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 22 of 26
Wall of the uterus (O-I):
➢ Perimetrium (Serous membrane)
➢ Myometrium (Smooth muscle)
➢ Endometrium (Mucous membrane)
VAGINA
- A tube about 10 cm long that extends from the uterus to the
outside of the body
- The female organ of copulation, functioning to receive the
penis during intercourse
- It allows menstrual flow and childbirth
- Hymen – thin mucous membrane that covers the vaginal
opening, or orifice
- Wall consists of an outer muscular layer and inner mucous
membrane
➢ Muscular layer – smooth muscle that allows the
vagina to increase in size to accommodate the penis
during intercourse and to stretch greatly during
childbirth
➢ Mucous membrane – moist stratified squamous
epithelium that forms a protective surface layer;
releases most of the lubricating secretions produced by
the female during intercourse
EXTERNAL GENITALIA
- Vulva or pudendum
- Consists of the vestibule and its surrounding structures
o Vestibule – the space into which the vagina opens
posteriorly and the urethra opens anteriorly
o Labia minora – a pair of thin, longitudinal skin folds
which forms the border on each side of the vestibule
o Clitoris – a small erectile structure located in the anterior
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 23 of 26
margin of the vestibule
o Prepuce – a fold of skin anteriorly where the two labia
minora unite over the clitoris
o Labia majora – two prominent, rounded folds of skin
lateral to the labia minora
o Mons pubis – an elevation over the symphysis pubis where
the two labia majora unite anteriorly
PERINEUM
o Clinical perineum
- Region between the vagina and the anus
- The skin and muscle of this region can tear during childbirth
MAMMARY GLANDS
- Organs of milk production
- Modified sweat glands located in the breasts
- Have a raised nipple surrounded by a circular, pigmented
areola
- The areola normally have a slightly bumpy surface caused
by the presence of rudimentary mammary glands, called
areolar glands
- Cooper’s ligaments support & hold the breasts in place
FEMALE SEXUAL ACT
o Parasympathetic stimulation
- Erectile tissue within clitoris around the vaginal opening
becomes engorged with blood
- The nipples of the breast often become erect as well
- The mucous glands within the vestibule secrete small
amounts of mucus
MENSTRUAL CYCLE
- Females experience their first episode of menstrual bleeding
or menarche between the ages of 11 and 16
- Elevated rates of estrogen and progesterone secretion
- Refers to the cyclic changes that occur in sex
- Refers to the cyclic changes that occur in sexually mature,
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 24 of 26
nonpregnant females and culminate in menses
- ~28 days long
*Can be as short as 18 days in some women and as long as
40 days in others
- A period of mild hemorrhage which occurs approximately
once each month
o Menstruation
- The discharge of the blood and elements of the uterine tube
mucous membrane
o First day of menses
- Day 1 of the menstrual cycle, and menses typically lasts 4-5
days
o Follicular or proliferative phase
- Time between the ending of menses and ovulation
- Rapid development of ovarian follicles
- Rapid proliferation of the uterine mucosa
o Ovulation
- Occurs on about 14 of a 28-day menstrual cycle
*Variable
- The time between ovulation, on day 14, and the next menses
is typically 14 days
o Luteal or secretory phase
- Period after ovulation and before the next menses
- Existence of the corpus luteum
- Maturation of and secretion by uterine glands
MENOPAUSE
- Cessation of menstrual cycles
- 40-50 years old
o Female climacteric or perimenopause
- the time from the onset of irregular cycles to their complete
cessation, which is often 3 to 5 years
- “hot flashes”, irritability, fatigue, anxiety, and occasionally
severe emotional disturbances
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 25 of 26
https://cdn.fbsbx.com/v/t59.2708-21/74897417_54347733309…oh=cc0890abf93bd1eb73a3b70b1b46a1b1&oe=5DD49F74&dl=1 18/11/2019, 8G54 PM
Page 26 of 26
You might also like
- Breathe In, Breathe Out: Learning About Your LungsFrom EverandBreathe In, Breathe Out: Learning About Your LungsRating: 3.5 out of 5 stars3.5/5 (3)
- Respiratory System: LarynxDocument4 pagesRespiratory System: LarynxLouise GermaineNo ratings yet
- Respiratory SystemDocument54 pagesRespiratory SystemEndin Nokik StujannaNo ratings yet
- Medical Surgical Nursing Lecture 234 Pages Pg. 333 566Document189 pagesMedical Surgical Nursing Lecture 234 Pages Pg. 333 566Crystal Ann TadiamonNo ratings yet
- Medical Surgical Nursing Lecture 234 Pages Pg. 333 566Document242 pagesMedical Surgical Nursing Lecture 234 Pages Pg. 333 566ShiraishiNo ratings yet
- RESPIRATORY DISTURBANCES - HandoutsDocument35 pagesRESPIRATORY DISTURBANCES - Handoutsfebie pachecoNo ratings yet
- TH E RE SP IRA TO RY SY ST EM: Learning ObjectivesDocument36 pagesTH E RE SP IRA TO RY SY ST EM: Learning Objectivesmaria tafaNo ratings yet
- Respiratory System s2 2019Document56 pagesRespiratory System s2 2019noviantyramadhani12No ratings yet
- Respiratory SystemDocument55 pagesRespiratory SystemSitotaye DinkuNo ratings yet
- 01 Respiratory SystemDocument15 pages01 Respiratory Systemnaseer alfahdNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemCharlie CharlesNo ratings yet
- Functions of Respiratory SystemDocument2 pagesFunctions of Respiratory SystemcjNo ratings yet
- The Respiratory SystemDocument6 pagesThe Respiratory SystemIftikharNo ratings yet
- Respiratory System Functions, Anatomy and Gas ExchangeDocument7 pagesRespiratory System Functions, Anatomy and Gas ExchangeChristiane with an ENo ratings yet
- Respiratory System Anatomy and PhysiologyDocument11 pagesRespiratory System Anatomy and PhysiologyLabinnah MoresNo ratings yet
- The Respiratory System: ASTIKA NUR ROHMAH, S.Kep., NS., M.BiomedDocument43 pagesThe Respiratory System: ASTIKA NUR ROHMAH, S.Kep., NS., M.BiomedAdek KhazeliaNo ratings yet
- The Respiratory System: Structure & FunctionDocument72 pagesThe Respiratory System: Structure & FunctionShanique ReidNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory Systemshane.surigaoNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemChelsie NicoleNo ratings yet
- Medical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationDocument44 pagesMedical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationYman Gio BumanglagNo ratings yet
- Respiratory system overviewDocument8 pagesRespiratory system overviewGladys Mae S. BañesNo ratings yet
- Respiratory SystemDocument21 pagesRespiratory SystemSalah ElwakilNo ratings yet
- Respiratory SystemDocument61 pagesRespiratory SystemDenise Nicole PinedaNo ratings yet
- Respiratory SystemDocument2 pagesRespiratory SystemFiona MarfaNo ratings yet
- Anatomy of The Respiratory SystemDocument37 pagesAnatomy of The Respiratory SystemPal SedNo ratings yet
- A &P Overview Respiratory SystemDocument16 pagesA &P Overview Respiratory SystemOpeyemi OmolabakeNo ratings yet
- Lab Module Activity Respiratory SystemDocument8 pagesLab Module Activity Respiratory SystemJecel LazarraNo ratings yet
- CVS and RSDocument132 pagesCVS and RSclareawambuiNo ratings yet
- Medical-Surgical 1 Lecture Overview Respiratory SystemDocument3 pagesMedical-Surgical 1 Lecture Overview Respiratory SystemJacqueline S. PunoNo ratings yet
- Anatomy and Physiology Handout # 15 Respiratory System-1Document8 pagesAnatomy and Physiology Handout # 15 Respiratory System-1Jounri Arsted Dimabuyu (Kaiz)No ratings yet
- Anatomy of Respiratory System: Moderator: Dr. Aruna Speaker:Dr - Vipin KR - SinghDocument69 pagesAnatomy of Respiratory System: Moderator: Dr. Aruna Speaker:Dr - Vipin KR - SinghAnshul JainNo ratings yet
- NCM 112 LEC Topic 1 Respiratory System Anatomy PhysiologyDocument7 pagesNCM 112 LEC Topic 1 Respiratory System Anatomy PhysiologyViviene Faye FombuenaNo ratings yet
- Zoo 1 PPT 10 Respiratory (2015)Document17 pagesZoo 1 PPT 10 Respiratory (2015)Zucc mahnutNo ratings yet
- Week 3 Respiratory SystemDocument10 pagesWeek 3 Respiratory SystemangeliaNo ratings yet
- ANATOMYDocument53 pagesANATOMYJocel Mae OrtegaNo ratings yet
- Respiratory SystemDocument5 pagesRespiratory SystemrianaNo ratings yet
- Respiratory System - NotesDocument4 pagesRespiratory System - NotessNo ratings yet
- The Respiratory System Lec TransesDocument10 pagesThe Respiratory System Lec TransesVENUS LIRIA PANTINo ratings yet
- Respiratory SystemDocument3 pagesRespiratory SystemElaine Eloisa CapilloNo ratings yet
- Respiratory SystemDocument9 pagesRespiratory Systemmariel.angeles29No ratings yet
- Respiratory System GuideDocument49 pagesRespiratory System GuideHiraya WNo ratings yet
- Anatomy of AirwayDocument50 pagesAnatomy of AirwayHari Om ChaurasiyaNo ratings yet
- RespiratorysystemDocument35 pagesRespiratorysystemLevy GerpacioNo ratings yet
- Respiratory SystemDocument5 pagesRespiratory SystemPreeti ChouhanNo ratings yet
- CHAPTER 10-Respiratory SystemDocument3 pagesCHAPTER 10-Respiratory SystempraiseginelcNo ratings yet
- Part 5 - Human Respiratory SystemDocument19 pagesPart 5 - Human Respiratory SystemAmal Naeem JHNo ratings yet
- Airway BSC AnesthesiaDocument72 pagesAirway BSC AnesthesiaTerefe AlemayehuNo ratings yet
- Respiratory GDocument58 pagesRespiratory GHirpâsà MămoNo ratings yet
- AP - Respiratory SystemDocument3 pagesAP - Respiratory SystemKatalina Estelle LaurierNo ratings yet
- Respiratory SystemDocument36 pagesRespiratory SystemLovejoy TiñaNo ratings yet
- Respiratory System-2cgf2Document42 pagesRespiratory System-2cgf2Nzenwa Jedidiah KimizuNo ratings yet
- Anatomy and Physiology of Respiratory SystemDocument110 pagesAnatomy and Physiology of Respiratory SystemFarhin FarjenaNo ratings yet
- 1.anatomy of Respiratory SystemDocument73 pages1.anatomy of Respiratory Systemokoti.omutanyi22No ratings yet
- ANAPHY Respiratory SystemDocument30 pagesANAPHY Respiratory SystemAshley Franceska CansanayNo ratings yet
- Anatomy and Physiology: The Respiratory SystemDocument82 pagesAnatomy and Physiology: The Respiratory SystemMaria Angelique Ofciar100% (2)
- Respiratory SystemhjhuDocument23 pagesRespiratory SystemhjhuSara ANo ratings yet
- Functions of The Respiratory SystemDocument10 pagesFunctions of The Respiratory SystemKrisha AvorqueNo ratings yet
- Respiratory SystemDocument12 pagesRespiratory SystemTricia CabiliNo ratings yet
- Upper Respiratory Tract AnatomyDocument61 pagesUpper Respiratory Tract Anatomyيحيى اسماعيل الجميليNo ratings yet
- Anatomy and Physiology of The Respiratory SystemDocument31 pagesAnatomy and Physiology of The Respiratory Systemgoluraviranjan84No ratings yet
- Long-Term Memory - ProcessDocument30 pagesLong-Term Memory - ProcessALEXANDRA SAN PEDRONo ratings yet
- Long-Term MemoryStructureDocument30 pagesLong-Term MemoryStructureALEXANDRA SAN PEDRONo ratings yet
- Understanding Brain Anatomy and Function Through Cognitive Neuroscience ResearchDocument34 pagesUnderstanding Brain Anatomy and Function Through Cognitive Neuroscience ResearchALEXANDRA SAN PEDRONo ratings yet
- Cog Psych - MemoryDocument31 pagesCog Psych - MemoryALEXANDRA SAN PEDRONo ratings yet
- AttentionDocument56 pagesAttentionALEXANDRA SAN PEDRONo ratings yet
- MLTP Week 1-6Document20 pagesMLTP Week 1-6ALEXANDRA SAN PEDRONo ratings yet
- Activity 2 Slogan - Communication For The Common GoodDocument1 pageActivity 2 Slogan - Communication For The Common GoodALEXANDRA SAN PEDRONo ratings yet
- Dev Psych - Intro ReviewerDocument14 pagesDev Psych - Intro ReviewerALEXANDRA SAN PEDRONo ratings yet
- Gen PhysioDocument8 pagesGen PhysioALEXANDRA SAN PEDRONo ratings yet
- Flap Design For Minor Oral SurgeryDocument22 pagesFlap Design For Minor Oral SurgerysevattapillaiNo ratings yet
- Assessing the Male Genitourinary SystemDocument46 pagesAssessing the Male Genitourinary SystemJonah nyachae100% (1)
- Tooth DevelopmentDocument20 pagesTooth DevelopmentArslan Jokhio0% (1)
- Menstrual CycleDocument8 pagesMenstrual Cyclejeni antonyNo ratings yet
- Alveolar bone grafting treatment goals and timingDocument13 pagesAlveolar bone grafting treatment goals and timingDayal SharanNo ratings yet
- 2 1 E28093 Structure and Function of The Ventilation SystemDocument10 pages2 1 E28093 Structure and Function of The Ventilation Systemapi-343368893No ratings yet
- DigestionpracticetestDocument41 pagesDigestionpracticetestRennik McCaigNo ratings yet
- Division of Human AnatomyDocument3 pagesDivision of Human Anatomyriffyjean0% (1)
- Repro. - NursingDocument79 pagesRepro. - NursingARAK Aldarwish100% (1)
- Reproductive Processes: Chapter-34-Lesson-2 Page-961-966Document26 pagesReproductive Processes: Chapter-34-Lesson-2 Page-961-966JanaNo ratings yet
- Normal Menstrual CycleDocument28 pagesNormal Menstrual CycleCristóbal ConchaNo ratings yet
- Orca Share Media1571800842460Document27 pagesOrca Share Media1571800842460Reniel De MesaNo ratings yet
- Chapter 62: General Principles of GI Function-Motility, Nervous Control, and Blood CirculationDocument36 pagesChapter 62: General Principles of GI Function-Motility, Nervous Control, and Blood Circulationjackie funtanillaNo ratings yet
- Excretory System - Print - QuizizzDocument4 pagesExcretory System - Print - Quizizzosama0% (1)
- Stomach and Spleen Gross LectureDocument27 pagesStomach and Spleen Gross LectureChigozie GeraldNo ratings yet
- Surat Dental 181Document15 pagesSurat Dental 181deva nesanNo ratings yet
- Detailed Lesson Plan Digestive SystemDocument5 pagesDetailed Lesson Plan Digestive SystemMaripres SalvaNo ratings yet
- Diagestive, Urinary and Reproductive SystemDocument39 pagesDiagestive, Urinary and Reproductive SystemCarolina Calle HerreraNo ratings yet
- Summary Highlights of Yoga Secrets For Extraordinary Health and Long Life by Frank Rudolph YoungDocument62 pagesSummary Highlights of Yoga Secrets For Extraordinary Health and Long Life by Frank Rudolph Youngfmntime100% (7)
- Greenfield - The Human Brain - A Guided TourDocument97 pagesGreenfield - The Human Brain - A Guided TourAlexandru Pop50% (2)
- Gomerged Document 7Document576 pagesGomerged Document 7bizzarobmNo ratings yet
- Autonomic Nervous System Bio FactsheetDocument4 pagesAutonomic Nervous System Bio FactsheetEleanor WilliamsNo ratings yet
- Orientación Postural y Equilibrio. Lo Que Se Necesita Saber Acerca Del Control Neural Del Balance para Prevenir Caídas.Document5 pagesOrientación Postural y Equilibrio. Lo Que Se Necesita Saber Acerca Del Control Neural Del Balance para Prevenir Caídas.Mauro Esban Obreque QuianNo ratings yet
- Anatomy and Physiology For PudDocument6 pagesAnatomy and Physiology For PudBj Renquijo100% (1)
- 3ES-2 Thyroid and Antithyroid Drugs 1436Document46 pages3ES-2 Thyroid and Antithyroid Drugs 1436Muath AlqarniNo ratings yet
- The Cardiovascular System: The Heart: Human Anatomy & Physiology, Sixth EditionDocument37 pagesThe Cardiovascular System: The Heart: Human Anatomy & Physiology, Sixth EditionJeramie DeanNo ratings yet
- Man Becomes Math Genius After Head InjuryDocument11 pagesMan Becomes Math Genius After Head InjuryvishalankitNo ratings yet
- Group 4 GCS Type II Diabetes Mellitus With Stage 1 Renal Failure NCM 116 RLEDocument67 pagesGroup 4 GCS Type II Diabetes Mellitus With Stage 1 Renal Failure NCM 116 RLEAriane Gay DuranNo ratings yet
- Embryology of The KidneysDocument18 pagesEmbryology of The KidneysPrincewill SmithNo ratings yet
- Cardiovascular MCQsDocument17 pagesCardiovascular MCQsRamadan PhysiologyNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (17)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 5 out of 5 stars5/5 (4)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Summary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedRating: 4 out of 5 stars4/5 (11)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisFrom EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisRating: 5 out of 5 stars5/5 (8)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosFrom Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosRating: 4.5 out of 5 stars4.5/5 (207)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)