Professional Documents
Culture Documents
Peds UTI
Uploaded by
Meles0 ratings0% found this document useful (0 votes)
16 views1 pageThis document provides guidelines for testing and treating pediatric urinary tract infections (UTIs) in children over 2 months old. It outlines signs and symptoms as well as risk factors for UTIs. Recommended testing includes urinalysis, urine culture, and imaging studies like ultrasound or VCUG based on factors like age and infection recurrence. Common causative organisms and appropriate antibiotic choices are presented, with preference for oral cephalexin or sulfamethoxazole/trimethoprim. Treatment duration is typically 7-10 days once culture sensitivities are known. Referral to urology is advised for recurrent or atypical UTIs.
Original Description:
Original Title
PedsUTI
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document provides guidelines for testing and treating pediatric urinary tract infections (UTIs) in children over 2 months old. It outlines signs and symptoms as well as risk factors for UTIs. Recommended testing includes urinalysis, urine culture, and imaging studies like ultrasound or VCUG based on factors like age and infection recurrence. Common causative organisms and appropriate antibiotic choices are presented, with preference for oral cephalexin or sulfamethoxazole/trimethoprim. Treatment duration is typically 7-10 days once culture sensitivities are known. Referral to urology is advised for recurrent or atypical UTIs.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
16 views1 pagePeds UTI
Uploaded by
MelesThis document provides guidelines for testing and treating pediatric urinary tract infections (UTIs) in children over 2 months old. It outlines signs and symptoms as well as risk factors for UTIs. Recommended testing includes urinalysis, urine culture, and imaging studies like ultrasound or VCUG based on factors like age and infection recurrence. Common causative organisms and appropriate antibiotic choices are presented, with preference for oral cephalexin or sulfamethoxazole/trimethoprim. Treatment duration is typically 7-10 days once culture sensitivities are known. Referral to urology is advised for recurrent or atypical UTIs.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 1
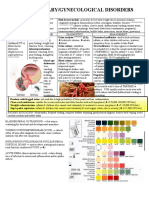
Pediatric Urinary Tract Infection Testing and Treatment Guideline (>2 months old)
Signs and Symptoms Risk Factors Testing
Pre-Verbal Verbal Not Toilet Trained Toilet Trained Not Toilet Trained Toilet Trained
Fever Dysuria <12 months old Female sex Catheterization Midstream clean catch
Increased risk of Frequency Female sex Constipation SPA Consider “dirty” urine
UTI with: Urgency/hesitancy Uncircumcised CAKUT Clean catch using Quick-Wee method*3 for STI screening in
- Fever >2 days Abdominal infant male High grade VUR Bag specimen for screening urinalysis in
adolescents
- Temp >102.2F & pain/flank pain Constipation Sexual activity infants >6mo (ONLY use to rule out UTI)
no source New onset CAKUT Diabetes Mellitus If positive nitrite, LE, or >0-2 WBC obtain
Poor feeding incontinence High grade VUR Kidney stones urine for urinalysis and culture by catheter or
Vomiting Prior history of UTI: clean catch/Quick-Wee method
Irritability Review prior
organisms and Order: “Urinalysis with Microscopic”
For 2-23mo UTI Risk
susceptibilities Obtain urine culture PRIOR to starting antibiotics
Calculator available at:
Note: urine culture is reflex in children <2yo,
https://uticalc.pitt.edu/
for older children a urine culture needs to be ordered separately
Urinalysis and Culture Interpretation Imaging Refer to urology:
Likely UTI Likely Contamination Renal/bladder ultrasound for Recurrent febrile UTI’s
Leukocyte esterase OR >10 per high-powered field - 1st febrile UTI in 2-24 mo Abnormal imaging on RUS or
Positive nitrite (not sensitive for children due squamous epithelial cells - Recurrent UTI in >24 mo VCUG
to frequent urination) OR Non-uropathogen growth Complete after treatment unless Need for DMSA scan
≥5 WBC/hpf (Lactobacillus, Corynebacterium, concern for acute complication/
AND viridans streptococci, coag-neg no improvement in 48-72 hours
A positive urine culture growing a Staph) VCUG for
uropathogen: >2 pathogens growing - recurrent febrile UTI
- >50,000 CFUs/mL for catheterization - abnormalities seen on RUS
- >100,000 CFUs/mL for clean catch - atypical pathogen
- complex clinical course
- known renal scarring
Antibiotic Selection
Most Common Organisms: Escherichia coli (85-90% of UTIs), Klebsiella, Proteus, Enterococcus, and Enterobacter species
Ambulatory Empiric Treatment Inpatient Empiric Treatment Duration of Therapy
Cephalexin can be divided TID or QID:
Ceftriaxone 50mg/kg IV Q24H
Preferred Treatment 17mg/kg PO TID (max 4gm/day) OR Narrow or adjust
(max 2gm/day)
12.5mg/kg PO QID (max 4gm/day) antibiotic coverage as
soon as culture
Gentamicin sensitivities and
7-10 days
Sulfamethoxazole/trimethoprim
Beta-lactam allergy 2mo-<5yo: 7.5mg/kg IV Q24H susceptibilities
4-5mg/kg PO BID (trimethoprim component
(severe) 5-10yo: 6mg/kg IV Q24H available
for dosing; max 160mg trimethoprim/dose)
≥10yo: 4.5mg/kg IV Q24H
Considerations
Exclusion criteria: chronic kidney disease, known urinary tract abnormality, neurogenic bladder, immune deficiency.
*Quick-Wee method: clean perineum, stimulate suprapubic area with cold fluid soaked gauze, collect urine midstream
Antimicrobial Stewardship Program Approved 2016; Updated January 2022
1. Roberts KB. Urinary tract infection: clinical practice guideline for the diagnosis and management of the initial UTI in febrile infants and children 2 to 24 months. Pediatrics. 2011;128(3):595-610.
2. Shaw K, et al. Clinical Pathway for the Evaluation and Treatment of Children with Febrile UTI. Children’s Hospital of Philadelphia. August 2020. https://www.chop.edu/clinical-pathway/urinary-tract-infection-uti-febrile-clinical-
pathway. Accessed 27 December 2021.
3. Kaufman H, et al. Faster clean catch urine collection (Quick-Wee method) from infants: randomized controlled trial. BMJ. 2017; 357:j1341. Available at: https://www.bmj.com/content/357/bmj.j1341
4. Mattoo, T. K., Shaikh, N., & Nelson, C. P. Contemporary management of Urinary Tract Infection in children. Pediatrics. 2021;147(2): e2020012138
You might also like
- Mayo Clinic - Images in Internal MedicineDocument385 pagesMayo Clinic - Images in Internal Medicinemohammed97% (35)
- Urinary Tract InfectionDocument9 pagesUrinary Tract InfectionTom Mallinson100% (1)
- Gi Gu Pregnancy - BoardsDocument12 pagesGi Gu Pregnancy - BoardsSoojung NamNo ratings yet
- Impaired Urinary EliminationDocument2 pagesImpaired Urinary EliminationSiafei RabeNo ratings yet
- Urinary Tract InfectionDocument10 pagesUrinary Tract InfectionMira Mariana UlfahNo ratings yet
- Hematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesFrom EverandHematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesRating: 5 out of 5 stars5/5 (2)
- Differential Diagnosis in Neurology Biomedical and Health ResearchDocument1,500 pagesDifferential Diagnosis in Neurology Biomedical and Health ResearchMelesNo ratings yet
- To Promote Good Hygiene and Physical Comfort.: Coli (E. Coli), NormallyDocument2 pagesTo Promote Good Hygiene and Physical Comfort.: Coli (E. Coli), NormallyFran LanNo ratings yet
- CPG Uti PDFDocument7 pagesCPG Uti PDFhellokathyyyyyyNo ratings yet
- Preterm LabourDocument3 pagesPreterm Labourcgao30No ratings yet
- Interstitial CystitisDocument9 pagesInterstitial CystitisKousik Amancharla100% (3)
- NCP-impaired Urinary Elimination-TAHBSODocument3 pagesNCP-impaired Urinary Elimination-TAHBSOtinatin9890% (1)
- MycosisDocument5 pagesMycosisMaiWahidGaberNo ratings yet
- UTIDocument57 pagesUTIGireesh NagaruruNo ratings yet
- CPG Uti PDFDocument7 pagesCPG Uti PDFhellokathyyyyyyNo ratings yet
- CPG Uti PDFDocument7 pagesCPG Uti PDFhellokathyyyyyy100% (1)
- Urinary Tract Infection (UTI) : Omega Mellyana Sub Bag. Nefrologi Anak FK UNDIP-RSUP Dr. KariadiDocument24 pagesUrinary Tract Infection (UTI) : Omega Mellyana Sub Bag. Nefrologi Anak FK UNDIP-RSUP Dr. KariadiRastia AlimmattabrinaNo ratings yet
- L22. Urinary Tract Infections. UndergradDocument27 pagesL22. Urinary Tract Infections. UndergradPhilemon ChizororoNo ratings yet
- Cultivation and Isolation of Bacteria: by Pamela NabhanDocument16 pagesCultivation and Isolation of Bacteria: by Pamela NabhanChristine KamaleddineNo ratings yet
- UTIs Practical 2023Document11 pagesUTIs Practical 2023abodeissaalssabagNo ratings yet
- Urinary Tract Infections in ChildrenDocument6 pagesUrinary Tract Infections in ChildrenMarianNo ratings yet
- Urinary Tract Infection in ChildrenDocument45 pagesUrinary Tract Infection in ChildrenMuhammad HaziqNo ratings yet
- Butler Uti or Pyelo 1 1Document34 pagesButler Uti or Pyelo 1 1api-611517539No ratings yet
- Grand Case StudyDocument13 pagesGrand Case StudyLaica A. LunetaNo ratings yet
- Urinary Tract Infection CMEDocument43 pagesUrinary Tract Infection CMEDarwithaNo ratings yet
- (Concept Map) Urinary Tract InfectionsDocument1 page(Concept Map) Urinary Tract InfectionsRica Alyssa PepitoNo ratings yet
- Urinary Tract Infection in ChildrenDocument17 pagesUrinary Tract Infection in Childrendeladestianiaji2490No ratings yet
- 04 NephrologyDocument25 pages04 Nephrologyliu ren weiNo ratings yet
- Referat - Syifa Firza UtiDocument28 pagesReferat - Syifa Firza Utimiir ikbalNo ratings yet
- Biochemistry Laboratory Manual Group 2: 2. Enumerate The Different Methods of Preserving A Urine SampleDocument18 pagesBiochemistry Laboratory Manual Group 2: 2. Enumerate The Different Methods of Preserving A Urine SampleMonique BorresNo ratings yet
- Urinary Tract Infection in PregnancyDocument49 pagesUrinary Tract Infection in PregnancyBALMERA, DANIELLA B.No ratings yet
- Urinary Tract Infection in Children: DR Nada Qawasmi Alquds Faculty of MedicineDocument25 pagesUrinary Tract Infection in Children: DR Nada Qawasmi Alquds Faculty of Medicineولاء إبراهيمNo ratings yet
- GenitoDocument12 pagesGenitofatima_antonioNo ratings yet
- UTI, HSC With QuestionsDocument43 pagesUTI, HSC With QuestionsAlex MatthewNo ratings yet
- Notes On UtiDocument15 pagesNotes On UtiSaleh Mohammad ShoaibNo ratings yet
- Urinary Tract Infection in Children: Dr. Alia Al-Ibrahim Consultant Pediatric Nephrology Clinical Assistant ProfessorDocument11 pagesUrinary Tract Infection in Children: Dr. Alia Al-Ibrahim Consultant Pediatric Nephrology Clinical Assistant ProfessorJim Jose AntonyNo ratings yet
- Uti Asbu Guidance FinalDocument14 pagesUti Asbu Guidance FinalJohn Vincent Dy OcampoNo ratings yet
- NCM 109 Reviewer 2Document13 pagesNCM 109 Reviewer 2Jerick PapoloniasNo ratings yet
- 1110 UtiDocument12 pages1110 Utizobi2020No ratings yet
- Urinary Tract Infection in ChildrenDocument38 pagesUrinary Tract Infection in ChildrensivaNo ratings yet
- Health Education On UTIDocument5 pagesHealth Education On UTIJyoti SidhuNo ratings yet
- 4 - Gyne Orders, or Tech, MaterialsDocument10 pages4 - Gyne Orders, or Tech, MaterialsJC GoodLifeNo ratings yet
- UTI FinalDocument29 pagesUTI FinalVijay ArumugamNo ratings yet
- PDFDocument1 pagePDFGina GiammalvoNo ratings yet
- Urinary Tract InfectionDocument10 pagesUrinary Tract InfectionditaNo ratings yet
- CPG UtiDocument4 pagesCPG UtiNomar NonatoNo ratings yet
- Standard Treatment: Guidelines 2022Document6 pagesStandard Treatment: Guidelines 2022Swathi KrishnaNo ratings yet
- 2106 UtiDocument2 pages2106 UtishimiNo ratings yet
- Taralan Tambunan: Department of Child Health Faculty of Medicine University of Indonesia JakartaDocument30 pagesTaralan Tambunan: Department of Child Health Faculty of Medicine University of Indonesia JakartaNicholasNo ratings yet
- UTI in ChildrenDocument94 pagesUTI in ChildrenSarfraz AnsariNo ratings yet
- University of The Assumption: College of Nursing Level Ii Related Nursing Experience Nursing Care PlanDocument3 pagesUniversity of The Assumption: College of Nursing Level Ii Related Nursing Experience Nursing Care PlanEugene MananganNo ratings yet
- Infeksi Saluran Kemih: Oleh Hendra Santoso Pembimbing Dr. Hasnawaty SP - OGDocument22 pagesInfeksi Saluran Kemih: Oleh Hendra Santoso Pembimbing Dr. Hasnawaty SP - OGHendra SantosoNo ratings yet
- Paeds Bilious VomitingDocument2 pagesPaeds Bilious Vomitingsinghurvashi365No ratings yet
- UTI GuidelinesDocument7 pagesUTI GuidelinesstarkNo ratings yet
- Aquino NCP UtiDocument3 pagesAquino NCP UtiGianne ObaldoNo ratings yet
- Laporan Tutorial Case 6 Kelompok 18Document97 pagesLaporan Tutorial Case 6 Kelompok 18Jason Maxwell mcguireNo ratings yet
- Case Pres NCP ProperDocument3 pagesCase Pres NCP ProperMyraNo ratings yet
- UTI Childhood Tadulako2015Document38 pagesUTI Childhood Tadulako2015ani bandasoNo ratings yet
- UTI - SarahDocument5 pagesUTI - SarahkhaledNo ratings yet
- Assessment and Diagnostic ExamsDocument10 pagesAssessment and Diagnostic ExamsJan Mark SotoNo ratings yet
- Ped VIDocument10 pagesPed VIVictor UrquizaNo ratings yet
- Subjective: Nephrolithiasis Is STO: After 8 Diagnostics: STO: Fully MetDocument3 pagesSubjective: Nephrolithiasis Is STO: After 8 Diagnostics: STO: Fully MetSebastianNo ratings yet
- UrinalysisDocument35 pagesUrinalysisAbdulelah MurshidNo ratings yet
- ASRHDocument68 pagesASRHMelesNo ratings yet
- Completion StatementDocument1 pageCompletion StatementMelesNo ratings yet
- Chapter 12 - Nervous SystemDocument34 pagesChapter 12 - Nervous SystemMelesNo ratings yet
- Assessing The Role of Community PolicingDocument108 pagesAssessing The Role of Community PolicingMelesNo ratings yet
- UTIs in Children 508Document8 pagesUTIs in Children 508MelesNo ratings yet
- Hiv Aids FNLDocument68 pagesHiv Aids FNLMelesNo ratings yet
- Completion Statement: Course Name: Childhood Blindness: Retinopathy of PrematurityDocument1 pageCompletion Statement: Course Name: Childhood Blindness: Retinopathy of PrematurityMelesNo ratings yet
- 12 D Marvel TutorialsDocument4 pages12 D Marvel TutorialsMelesNo ratings yet
- Completion StatementDocument1 pageCompletion StatementMelesNo ratings yet
- Ethiopia Nurses Association: Course Summary Report Zenebech Kasahun 4347238 Total: 30.5 HoursDocument2 pagesEthiopia Nurses Association: Course Summary Report Zenebech Kasahun 4347238 Total: 30.5 HoursMelesNo ratings yet
- Diseases of Public Health SignificanceDocument34 pagesDiseases of Public Health SignificanceMelesNo ratings yet
- Completion StatementDocument1 pageCompletion StatementMelesNo ratings yet
- Disorders of Coagulation FactorsDocument35 pagesDisorders of Coagulation FactorsMelesNo ratings yet
- Ethiopian Medical Association: Course Summary Report Dinku Dadi 4090410Document1 pageEthiopian Medical Association: Course Summary Report Dinku Dadi 4090410MelesNo ratings yet
- CVS Pharmacology For Health ScienceDocument54 pagesCVS Pharmacology For Health ScienceMelesNo ratings yet
- Tsegaye Thesis Full FinalDocument86 pagesTsegaye Thesis Full FinalMelesNo ratings yet
- Yoseph. Thesis Final PaperDocument70 pagesYoseph. Thesis Final PaperMelesNo ratings yet
- Abiy MogesDocument67 pagesAbiy MogesMelesNo ratings yet
- Thesis 3Document113 pagesThesis 3MelesNo ratings yet
- Diabetes Mellitus PresentationDocument178 pagesDiabetes Mellitus PresentationMelesNo ratings yet
- Dr. Joanri T, Riveral, SR., FPLS Schistosomiasis Control and Elimination Program Manager Department of Health Regional Office VIIDocument66 pagesDr. Joanri T, Riveral, SR., FPLS Schistosomiasis Control and Elimination Program Manager Department of Health Regional Office VIIPatNo ratings yet
- CHNN312 FinalDocument26 pagesCHNN312 FinalVALERIANO TRISHANo ratings yet
- Farm Animal Diseases Epidemiology and Control GuidelinesDocument71 pagesFarm Animal Diseases Epidemiology and Control GuidelinesHikmat UllahNo ratings yet
- Tuberculosis in Children (1) - PIR 2019Document13 pagesTuberculosis in Children (1) - PIR 2019Jose Fernando Díez ConchaNo ratings yet
- MMR Vaccine: Review of Benefits and RisksDocument6 pagesMMR Vaccine: Review of Benefits and RisksAldo Pravando JulianNo ratings yet
- Topic 4 - MAJOR DISEASES IN DEVELOPED AND DEVELOPING COUNTRIESDocument10 pagesTopic 4 - MAJOR DISEASES IN DEVELOPED AND DEVELOPING COUNTRIESAYO NELSONNo ratings yet
- German Measles (Rubella) : Romena Salazar Monderondo Bs BiologyDocument10 pagesGerman Measles (Rubella) : Romena Salazar Monderondo Bs Biologycasandra moranteNo ratings yet
- J of Cosmetic Dermatology - 2023 - Aryanian - Various Aspects of The Relationship Between Vitiligo and The COVID 19Document5 pagesJ of Cosmetic Dermatology - 2023 - Aryanian - Various Aspects of The Relationship Between Vitiligo and The COVID 19AinaaqorryNo ratings yet
- I Know That My Redeemer LivethDocument3 pagesI Know That My Redeemer LivethMichelle KwokNo ratings yet
- Certification: Office of The Municipal Health OfficerDocument15 pagesCertification: Office of The Municipal Health OfficerSample BakeshopNo ratings yet
- Hepatitis B Cases StudiesDocument53 pagesHepatitis B Cases Studiesrieza_huseinNo ratings yet
- Autism Medical ComorbiditiesDocument15 pagesAutism Medical ComorbiditiesMartha Patricia López PimentelNo ratings yet
- SPM MeaslesDocument30 pagesSPM MeaslesAri YudiNo ratings yet
- Dr. Ugi Sugiri, SpEm - PPT OBMED PDFDocument56 pagesDr. Ugi Sugiri, SpEm - PPT OBMED PDFDaniel Aprianto SihotangNo ratings yet
- A Reading On: Kawasaki DiseaseDocument6 pagesA Reading On: Kawasaki DiseaseRaijenne VersolaNo ratings yet
- Melanoma of Anal CanalDocument3 pagesMelanoma of Anal CanalAjay GujarNo ratings yet
- Serologicchartv8 PDFDocument1 pageSerologicchartv8 PDFOlga CîrsteaNo ratings yet
- Berries in DermatologyDocument2 pagesBerries in DermatologyIjsrnet EditorialNo ratings yet
- Cervical ErosionDocument8 pagesCervical ErosionPipaticoNo ratings yet
- MS Soapie #1Document2 pagesMS Soapie #1Fatima KateNo ratings yet
- Journal of Internal Medicine - 2019 - Shaw - The Face of Postural Tachycardia Syndrome Insights From A Large 2Document11 pagesJournal of Internal Medicine - 2019 - Shaw - The Face of Postural Tachycardia Syndrome Insights From A Large 2Liza HavengaNo ratings yet
- Zoonotic DiseasesDocument27 pagesZoonotic DiseasesGift Summer DinoNo ratings yet
- Marcia Texler Segal, Vasilikie Demos, Jennie Jacobs Kronenfeld - Gender Perspectives On Health and Medicine, Volume 7 - Key Themes (Advances in Gender Research Series) (2003)Document328 pagesMarcia Texler Segal, Vasilikie Demos, Jennie Jacobs Kronenfeld - Gender Perspectives On Health and Medicine, Volume 7 - Key Themes (Advances in Gender Research Series) (2003)Federico AnticapitalistaNo ratings yet
- Case Presentation LeptoDocument16 pagesCase Presentation LeptoMalaka AtapattuNo ratings yet
- Diagnosis MalariaDocument18 pagesDiagnosis MalariaCiciNo ratings yet
- Toronto IMR - Toronto Internal Medicine Review 2024 (2024, Toronto Internal Medicine Review) - Libgen - LiDocument2,188 pagesToronto IMR - Toronto Internal Medicine Review 2024 (2024, Toronto Internal Medicine Review) - Libgen - LiHenrique Augusto LinoNo ratings yet
- Signs and Symptoms of Chest InfectionsDocument10 pagesSigns and Symptoms of Chest InfectionsHussain MirzaNo ratings yet
- Post Covid Effects of Black Fungus Mucormycosis: A ReviewDocument7 pagesPost Covid Effects of Black Fungus Mucormycosis: A ReviewIJAR JOURNALNo ratings yet