Professional Documents
Culture Documents
Module 13 Thorax and Lungs
Uploaded by
Kristine Angie RamosOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Module 13 Thorax and Lungs
Uploaded by
Kristine Angie RamosCopyright:
Available Formats
St.
Paul College of Ilocos Sur
(Member, St. Paul University System)
St. Paul Avenue, 2727 Bantay, Ilocos Sur
NCM 101: Health Assessment
Module 13.1
Assessing Thorax
and Lungs
Melanio P. Rojas Jr, MAN
Clinical Instructor
2022
THORAX AND LUNGS 1
Module No. 13.1
Assessing Thorax and Lungs
Learning Objectives:
After completing this module, the students will be able to:
1. Describe the function and structure of the thorax and lungs.
2. Perform a physical assessment of the thorax and lung using the correct techniques of
inspection, auscultation, palpation and percussion.
THORAX AND LUNGS 2
OVERVIEW OF ANATOMY AND PHYSIOLOGY OF RESPIRATORY SYSTEM
• Respiration. The process of gaseous exchange between the individual and the
environment.
• The process of respiration
1. Ventilation. Refers to the movement of gases in and out of the lungs.
- Inhalation (inspiration) is voluntary phase
- Exhalation (expiration) is involuntary phase
2. Diffusion. The exchange of gases from an area of higher pressure to an area of lower
pressure.
3. Perfusion. The availability and movement of blood for transport of gases, nutrients and
metabolic waste product.
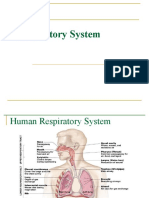
• The respiratory system is composed of the following structures:
1. The Airways
a. Upper Airways
✓ Nasal cavity or nares
✓ Pharynx
✓ Larynx or voice box
b. Lower airways (Tracheobrochial tree)
✓ Trachea
✓ Right and left mainstem bronchi
✓ Segmental bronchi
✓ Subsegmental bronchi
✓ Terminal bronchi
c. Functions of the Upper Airways:
✓ Transport of gases to the lower airways
✓ Protection of the lower airways from foreign matter
✓ Warming, filtration and humidification of inspired air.
d. Function of the Lower Airways
✓ Clearance Mechanism
Cough
Mucociliary system
Macrophages
Lymphatics
✓ Immunologic responses
Cell-mediated immunity in the alveoli
✓ Pulmonary protection in injury
Respiratory epithelium
Mucociliary system
• The opening of the nose on the face area are called nostril or nares.
• Each nostril leads to a cavity called vestibule.
• The hair that lines the vestibule are called vibrissae. The vibrissae filter foreign objects.
• The paranasal sinuses are open areas within the skull, lined with mucous membrane. They help
in phonation. The different sinuses are as follows: frontal, maxillary, ethmoid and sphenoid.
• The pharynx is a funnel shaped tube that extends from the nose to the pharynx. It is a common
opening between the digestive and respiratory system.
• The three sections of the pharynx are as follows: nasopharynx, oropharynx, and larnygopharynx.
• From the middle ear, the euschatian tubes open into the nasopharynx
• The larynx is the voice box
• The epiglottis covers closes when speaking it opens.
THORAX AND LUNGS 3
• The trachea (windpipe) is 12 cm (4 to 5 inches) long. The point at which divides is called carina.
• The trachea and bronchi are lined with cilia and goblet cells.
• The cilia are microscopic hair-like projection which have rapid, coordinated, unidirectional
upward motion.
• The cilia sweep out debris and excessive mucous from the lungs.
• The goblet cells secrete 120 ml of mucous per day. The mucous secretions entrap debris in the
respiratory tract.
• The right mainstem bronchus is shorter, broader, and more vertical than the left.
2. The pleura
• The pleura are serous membranes that enclose the lungs.
• The visceral pleura directly covers the lungs.
• The parietal pleura lines the cavity of each hemothorax.
• The pleural space is a potential space between the two pleurae. Only few ml of
serous fluid is found in the pleural space, to serve as lubricant.
3. The lungs
• The right lung has three lobes while the left lung has two lobes.
• The two lungs are separated by a space called mediastinum
• There are approximately three hundred million alveoli in the lungs.
• The right lung is broader, but shorter due to the presence of the liver on the right
side of the abdomen.
• A. Divisions (structure)
a. Root: consist of the primary bronchus and pulmonary artery and veins bound
together by connective tissue.
b. Hilum. Vertical slit on medial surface of the lung, through which root structure
enter the lung.
c. Lobes; three in the right and two in the left.
d. Apex: pointed upper part of the lung.
e. Base: broad, inferior surface of the lung.
4. Bronchial tree consists of the following:
A. Bronchial: right and left formed by branching of the trachea; right bronchus slightly larger
and more vertical than left each primary bronchus branches into segmental bronchi in
each lung: primary and segmental bronchi all contain C-shaped cartilage
B. Bronchioles: small branches off the secondary bronchi, distinguished by lack of C-
shaped cartilage and a duct diameter about 1 mm, which further branch into terminal
bronchioles, respiratory bronchioles and then alveolar ducts.
C. Alveoli: microscopic sacs composed of a single layer extremely thin squamous epithelial
cells enveloped by a network of capillaries.
4. Covering of the lung: visceral and layer pleura.
B. Function:
A. Bronchi, bronchioles, alveoli ducts: passage to move air into and out of
alveoli.
B. Alveoli: provide a surface area large enough and thin enough to allow rapid
gas exchange:
✓ Type I cells from walls
✓ Type II cells produce surfactant to prevent alveolar collapse
THORAX AND LUNGS 4
PHYSIOLOGY OF RESPIRATION
A. Mechanism of breathing
1. Following phrenic nerve stimulation, the diaphragm and other respiratory muscles
contract.
2. Thorax increases in size
3. Intrathoracic and intrapulmonic pressures decrease
4. Air rushes from positive pressure in the atmosphere to negative pressure in the alveoli
5. Expiration reverse procedure and inspiration
B. Control of respiration
1. Alveolar stretch receptors respond to inspiration by sending inhibitory impulses to
inspiratory neurons in brainstem to prevent lung distention (Hering- Breuer reflex)
2. Central and peripheral chemoreceptors stimulate respirations in respond to lowered ph,
increased PCO2 or decreased PO2
C. Amount of air exchanged in breathing:
1. Directly related to gas pressure gradient between atmosphere and alveoli and inversely
related to resistance that opposes air flow; pulmonary function can be evaluated with a
spirometer
2. Expiratory reserve volume: largest additional volume of air that can be forcibly expired
after a normal respiration and expiration. Normal ERV is 1000 to 2000 ml.
3. Inspiratory reserve volume: is the amount of extra air that can be inhaled, beyond the
tidal volume. Normal IRS is 3000 ml
4. Residual volume is the amount of air that remains in the lungs after forceful expiration. It
prevents collapse of the lungs during expiration. Normal RV is 1200 ml.
5. Tidal volume is the amount of air that moves in and out of the lungs with each normal
breath. Normal TV is 500 ml
6. Total lung capacity is the total of all four volumes (residual, tidal, inspiratory reserve and
expiratory reserve volume).
7. Forced expiratory volume: volume of air that can be forcibly exhaled within a specific
time usually 1 to 3 seconds.
8. Functional residual capacity is the amount of air that remains in the lung after normal
exhalation.
9. Positions such as orthopnea and fowler’s position can lower abdominal organs and
reduce pressure against diaphragm.
D. Diffusion of gases between air and blood
1. Occurs across alveolar-capillary membranes (in lungs between air in alveoli and venous
lung capillaries: adequate diffusion depends on a balanced ventilation-perfusion (V/Q)
ratio.
2. Direct of diffusion
a) Oxygen: net diffusion toward lower oxygen pressure gradient (from alveolar air to
blood).
b) Carbon dioxide: net diffusion toward lower carbon dioxide pressure gradient (from
blood to alveolar air)
E. The thorax and the diaphragm
• The thorax provides protection for the lungs, heart and great vessels.
• The thorax is made up of 12 pairs of ribs, bounded anteriorly by the sternum and
posteriorly by the thoracic vertebrae.
• The diaphragm is the main respiratory muscle for inspiration. It is supplied by the phrenic
nerve.
THORAX AND LUNGS 5
• The following are the accessory muscles for inspiration: sternocleidomastoid, scalene,
parasternal, trapezius, and pectoralis muscles. They are used during increased work of
breathing.
F. Respiratory Centers
• Medulla oblongata is the primary center
• Pons contains the following:
Pneumotaxic center. Responsible to the rhythmic quality of breathing
Apneustic center. Responsible for deep, prolonged inspiration
• Carotid and aortic bodies
Peripheral chemoreceptors. Take up the work of breathing when the central
chemoreceptors in the medulla oblongata are damaged. It responds to low
oxygen concentration in the blood. Respond to pressures. If the BP is elevated
the respiratory rate becomes slow. (HPN leads to respiratory acidosis). If the BP
is decreased, the respiratory rate becomes rapid (hypotension leads to respiratory
alkalosis). The primary chemical stimulation for breathing is high carbon dioxide
level in the blood.
• Muscles and Joints
Prioreceptors. Exercise increases respiratory rate.
THORAX AND LUNGS 6
ASSESSMENT NORMAL FINDINGS ABNORMAL FINDINGS
PROCEDURE
General
INSPECTON
Inspect for nasal Nasal flaring is not observed. Nasal flaring is seen with labored
flaring and pursed lip Normally the diaphragm and the respirations ( especially in small
breathing. internal costal muscles do most of children) and is indicative of
the work of breathing. This is hypoxia.
evidenced by outward expansion of
the abdomen and lower ribs on Pursed lip breathing may been in
inspiration as well as return to asthma, emphysema, or CHF as a
resting position one expiration. physiologic response to help slow
down expiration and keep alveoli
open longer.
Observe color or face, The client has evenly colored skin Ruddy to purple complexion may
lips and chest. tone, without unsual or prominent be seen in clients with COPD or
discoloration. CHF as a result of polycythemia.
Cyanosis may be seen if client is
cold or hypoxic.
Inspect color and Pink tones should be seen in the Pale or cyanotic may indicate
shape of nails. nailbeds. There is normally a 160- hypoxia. Early clubbing ( 180
degree angle between the nail base degree angle) and late clubbing (
and the skin. greater than a 180 degree) can
occur from hypoxia.
Posterior thorax
INSPECTION
Inspect for Scapulae are symmetric and Spinous processes that deviate
configuration. While nonprotruding. Shoulders and laterally in the thorax are may
the client sits with arms scapulae are at equal horizontal indicate scoliosis.
at the sides, stand positions.
behind the client and Spinous configuration may have
observe position of The ratio of anteroposterior to respiratory implications. Ribs
scapulae and the shape transverse diameter is 1:2. appearing horizontal at an angle
configuration of the greater than 45- degree with the
chest wall. Spinous process appera straight, spinal column are frequently the
and thorax appears symmetric, with result of an increased ( 1 to 1) ratio
ribs slopping downward at between the anterioposterior and
approximately a 45- degree angle in transverse diameter ( barrel chest.
relation to the spine. This condition is commly the result
of emphysema due to
Older Adult Considerations hyperinflation of the lungs.
Kyphosis ( an increased curve of
the thoracic spine) is common in
older clients. It results from a
loss of lung resiliency and a loss
of skeletal muscles.
THORAX AND LUNGS 7
Spinous configuration may have
respiratory implications. Ribs
appearing horizontal at an angle
greater than 45 degree with the
spinal column are frequently the
result of an increased ( 1 to 1)
ratio between the
anterioposterior and transverse
diameter ( barrel chest. This
condition is commly the result of
emphysema due to
hyperinflation of the lungs.
Abnormal findings:
1. Barrel chest
2. Pectus excavatum- funnel
chest
3. Pectum carinatum- pigeon
chest.
4. Scoliosis- curvature of the
spine
5. Kyphosis- is an
exaggerated increased
rounding of the thorcic spine,
often seen with osteoporosis
in older women.
Trapezius or shoulder, muscles
are used to facilitate inspiration
in cases of acute and chronic
airway obstruction or atelectasis.
Observe use of The client does not use Client leans forward and uses
accessory muscles. accessory ( trapezius/shoulder) arms to support weight and lift
Watch as the client muscle to assist breathing. The chest to increase breathing
breathes and note use of diaphragm is the major muscle capacity, referred as the tripod
muscles. at work. This is evidenced by position. This is often seen in
expansion of the lower chest COPD.
during inspiration.
Inspect the client’s Client should be sitting up and Tender or painful areas may
positioning. Note the relaxed breathing easily with indicate inflamed fibrous
client’s posture and arms at sides or in lap. connective tissue. Pain over the
ability to support weight intercostal spaces may be from
while breathing infammed pleurae. Pain over the
comfortably. ribs, especially at the costal
chondral junctions, is a symptom
of fractured ribs.
THORAX AND LUNGS 8
ASSESSMENT PROCEDURE NORMAL FINDINGS ABNORMAL FINDINGS
PALPATION
Palpate for tenderness and Client reports no Muscle soreness from
sensation. Palpation may be tenderness, pain or unusual exercise or the excessive
performed with one or both hands, sensations. Temperature work of breathing ( as in
but the sequence of palpation is should be equal bilateral. COPD) may be palpated
established. Use your fingers to as tenderness.
palpate for tenderness, warmth, pain,
or sensations. Start toward the Increased warmth may
midline at the level of the left scapula be related to local
( over the apex of the left lung) and infection.
move your hand left to the right,
comparing findings bilaterally. Move
systematically downward and out to
cover the lateral portions of the lungs
at the bases.
Palapte for crepitus. Crepitus, also The examiner finds no Crepitus can be palpated
called subcutenous emphysema is a palpable crepitus. if air escapes from the
crackling sensation ( like bones or lung or other airways into
hairs rubbing against each other) that the subcutenous tissue,
occurs when air passes through fluid as occurs after an open
or exudate. Use of fingers when thoracic injury, around a
palpating. chest tube, or
tracheostomy. It also may
be palpated in areas of
extreme congestion or
consolidation. In such
situations, mark margins
and monitor to note any
decrease or increase in
the crepitant area.
Palpate surface characteristics. Skin and subcutenous tissue A physician or other
Put on gloves and use your fingers to are free of lesions and appropriate professional
palpate any lesions that you noticed masses. should evaluate any
during inspection. Feel for any unusual palpable mass.
unusual masses.
Palpate for fremitus. Following the Fremitus is symmetric and Unequal fremitus is
sequence described previously, use easily identified in the upper usually the result of
the ball or ulnar endge of the hand to regions of the lungs. If consolidation (which
assess for fremitus ( vibrations of air fremitus is not palpable on increases fremitus) or
in the bronchial tubes transmitted to either side, the client may bronchial obstruction, air
the chest wall). As you move your need to speak louder. A tapping in emphysema,
hand to each area, ask the client to decrease in the intensity of pleural effusion, or
say “ninety-nine.” Assess all areas for fremitus is normal as the pneumothorax ( which all
symmetry and intensity of vibration. examiner moves toward the decrease fremitus).
base of the lungs. However, Diminished fremitus even
fremitus should remain with a loud spoken voice
symmetric for bilateral indicate an obstruction of
positions. the tracheobronchial tree.
THORAX AND LUNGS 9
Assess chest expansion. When the client takes a deep Unequal chest expansion can
Place your hands on the breath, the examiner’s occur with severe atelectasis (
posterior chest wall with your thumbs should move 5 to 10 collapse or incomplete
thumbs at the level of T9 or T10 cm apart symmetrically and expansion), pneumonia, chest
and pressing together a small pressing together a small skin trauma, pneumothorax ( air in the
skin fold. As the clients takes a fold. As the client takes a pleural space).
deep breath, observe the deep breath, observe the
movement of your thumbs. movement of your thumbs.
Older Adult Considerations Decreased chest excursion at
Because of calcification of the the base of the lungs is
costal cartilages and loss of characteristic of COPD. This is
the accessory musculature, due to decreased diaphragmatic
the older client’s thoracic
function.
expansion may be decreased,
although it should still be
symmetric
PERCUSSION NORMAL FINDINGS ABNORMAL FINDINGS
Percuss for tone. Start at the Resonance is the percussion Hyperresonce is elicted in cases
apices of the scapulae and tone elicited over normal lung of trapped air such as in
percuss across the tops of both tissue. Percussion elicits flat emphysema or pneumothorax.
shoulder. Then percuss the tones over the scapula.
interscostal spacess across
and down comparing sides.
Percuss to the lateral aspects
at the bases of the lungs,
comparing sides.
Percuss for diapgramatic Exursion should be equal be Dullness is present when fluid or
excursion. Ask the client to bilaterally and measure 3-5 solid tissue replaces air in the lung
exhale forcefully and hold the cm in adults. or occupies the pleural space, such
breath. Beginning at the as in lobular pneumonia, pleural
effusion, or tumor.
scapular line ( T7), percuss the
intercostal spaces of the right
posterior chest wall.
Diaphragmatic descent may be
Percusses downward until the The level of the diaphragm limited by atelectasis of the lower
tone changes from resonance may be higher on the right lobes or by emphysema, in which
to dullness. Mark the level and because of the position of the diaphragmatic movement and air
allow the client to breathe. Next liver. trapping are mininal. The diaphragm
ask the client to inhale deeply remains in a low position on
and hold it. Percuss the In well-conditioned clients, inspiration and expiration.
intercostal spaces from the excursion can up to 7 to 8 cm.
Other possible causes for limited
mark downward until descent can be pain or abdominal
resonance changes to changes such as extreme ascites,
dullness. Measure the distance tumors or pregnancy.
between 2 marks. Perform this
assessment technique on both Uneven excursion may be seen with
sides of the posterior thorax inflammation from unilateral
pneumonia, damage to the phrenic
nerve or splenomegaly.
THORAX AND LUNGS 10
AUSCULTATION NORMAL FINDINGS ABNORMAL FINDINGS
Auscultate for breath sounds. Three types nof normal Diminshed or absent sounds
To best assess lung sounds, you breath, sounds may be often indicate that little or no
will needed to hear the sounds as auscultated- bronchial, air is moving in or out of the
directly as possible. Do not bronchovesicular and lung area being auscultated.
attempt to listen through clothing vesicular. See table 1. This may indicate obstruction
or a drape, which may produce within the lungs as a result of
additional sound or muffle lung secretions, mucus plug, or a
sounds that exist. To begin, place foreign object. It may also
the diagphragm of the indicate abormalities of the
stethoscope firmy and directly on pleural space such as pleural
the posterior chest wall at the apex thickening, pleural effusion or
of the lung at C7. Ask the client to Sometimes breath pneumothorax. In cases of
breathe deeply through the mouth sounds may be hard to emphysema the hyperinflated
for each of auscultation ( each hear with obese or nature of the lungs, together
placement of the stethoscope) in heavily muscled clients with a loss of elasticity of lung
the auscultation sequence so that due to increased tissue, may result in
you can best hear inspiratory and distance to undelying diminished inspiratory breath
expiratory sounds. Be alert to the lung tissue. sounds. Increased ( louder)
client’s comfort and offer times for breath sounds often occurs
rest and normal breathing if when consolidation or
fatigue is becoming a problem. compression results in a
denser lung area that
ehnhaces the trasmission of
sounds.
Auscultate from the apices of the
lungs at C7 to the bases of the
lungs at T10 and laterally from the
axilla down to the 7 or 8 rib. Listen
at each site for at least one
complete respiratory cycle.
Auscultate for adventitious No adventitious sounds, Adventitious lung sounds,
sounds. Adventitious sounds are such as crackles such as crackles or rales and
sounds added or superimposed (discrete and discontious wheezes or rhonchi are
over normal breath sounds and sounds) or wheezes evident. See table 2
heard during auscultation. Be (musical and continous
careful to note the location on the sounds) are auscultated. Clinical Tip: If you hear an
chest wall where adventitious abnormal sounds during
sounds are heard as well as the auscultation, always have
location of such sounds within the the client cough, then listen
respiratory cycle. again and note any change.
Coughing may clear the
lungs.
THORAX AND LUNGS 11
ASSESSMENT PROCEDURE NORMAL FINDINGS ABNORMAL FINDINGS
AUSCULTATE VOICE SOUNDS
Bronchopony: Ask the client to Voice transmission is The words are easily understood
repeat the phase “ ninety-nine” soft, muffled, and and louder over of increased
while you auscultate the chest indistict. The sound of the density. This may indicate
wall. voice may be heard but consolidation from pneumonia,
the actual phrase cannot atelectasis or tumor.
be distinguished.
Egophony: Ask the client to Voice transmission will be Over areas of consolidation or
repeat the letter “ E” while you soft and muffled but the compression the sound is louder
listen over the chestwall. letter “E” should be and sound like “ A.”
distinguishable.
Whisphered pectoriloquy: Ask Transmission of sound is Over areas of consolidation or
the client to whisper the phrase very faint and muffled. It compression, the sound is
“one-two-three” while you may be inaudible. transmitted clearly and distinctly.
auscultate the chest wall. In such areas, it sounds as if the
client is whispering directly into the
stethoscope.
ANTERIOR THORAX NORMAL FINDINGS ABNORMAL FINDINGS
INSPECTION
Inspect for shape and The anteroposterior Anteroposterior equals transverse
configuration. Have the client sit
diameter is less than the diameter, resulting barrel chest.
with arms at the sides. Stand in transverse diameter. The This is often seen in emphysema
front of the client and assess ratio of anteroposterior because of hyperinflation of the
shape and configuration. diameter to the lungs.
transverse diameter is
1:2
Inspect position of the sternum. Sternum is positioned at Pectus excavatum is a markedly
Observe the sternum from an midline and straight. sunken sternum and adjacent
anterior and lateral viewpoint. cartilages ( often referred to as
funnel chest). It is a congenital
malformation the seldom causes
symptoms other than self-
conciousness. Pectus carinatum
is a forward protrusion of the
sternum causing the adjacent ribs
to slope backward. Both
conditions may restrict expansion
of the lungs and decrease lung
capacity.
Watch for sternal retractions. Retractions not observed. Sternal retractions are noted, with
severely labored breathing.
Inpsect slope of the ribs. Rib slope downward with Barrel-chest configuration results
Assess the ribs from an anterior symmetric intercostal in a more horizontal position of the
and lateral viewpoint. spaces. Costal angle is ribs and costal angle of more than
within 90 degrees. 90 degrees. This often results from
long-standing emphysema.
THORAX AND LUNGS 12
Observe quality and pattern of Respiration are relaxed, Labored and noisy breathing is
respiration. Note breathing effortless, and quiet. often seen with severe asthma or
characteristics as well as rate, They are of a regular chronic bronchitis. Abnormal
rhythm, and depth. See table 3. rhythm and normal depth breathing patterns include
at a rate of 10-20 per tachypnea, bradypnea,
minute in adults. hyperventilation and
Tachypnea and hypoventilation, Cheyne-Stokes
bradypnea may be respiration, and Biot respiration.
normal in some clients.
ASSESSMENT PROCEDURE NORMAL FINDINGS ABNORMAL FINDINGS
Inspect intercostal spaces. Ask No retractions or bulging Retraction of the intercostal
the client to breathe normally and of intercostal spaces are spaces indicates an increased
observe the intercostal spaces. noted. inspiratory effort. This may be the
result of an obstruction of the
respiratory tract or atelectasis.
Bulging of the intercostal spaces
indicates trapped air such as in
emphysema or asthma.
Observe for use of accessory Use of accessory Neck muscles ( sternomastoid,
muscles. Ask the client to breathe muscles ( sternomastoid scalene, and trapezius ) are used
normally and observe for use of and rectus abdominis) is to facilitate inspiration in cases of
accessory muscles. not seen with normally acute or chronic airway
respiratory effort. After obstruction or atelectasis. The
strenous exercise or abdominal muscles and the
activity, clients with internal intercostal muscles are
normal respiratory status used to facilitate expiration in
may use neck muscles COPD.
for a short time to
enhance breathing.
PALPATION NORMAL FINDINGS ABNORMAL FINDINGS
Palpate for tenderness, No tenderness or pain is Tenderness over thoracic muscles
sensation, and surface masses. palpated over the lung can result from exerising ( e.g,
Use your fingers to palpate for area with respirations. pushups) especially in a
tenderness and sensation. Start previously sedentary client.
with your hand positioned over the
left clavicle ( over the apex of the
left lung) and move your hand to
left to right, comparing findings
bilaterally. Move your hand
systematically downward toward
the midline at the level of the
breasts and outward at the base to
include the lateral aspect of the
lung. The established sequence
for palpating the anterior thorax
serves as a guide for positioning
your hands.
THORAX AND LUNGS 13
Palpate for tenderness at Palpation does not elicit Tenderness or pain at the
costochondral junctions of ribs. tenderness. constochondral junction of the ribs
is seen with fractures especially in
older clients with osteoporosis.
Palpate for crepitus as you No crepitus is palpated. In areas of extreme congestion or
would on the posterior thorax consolidation, crepitus may be
( described previously). palpated, particularly in clients
with lung disease.
Palpate for any surface masses No unusual surface Surface masses or lesions may
or lesions. massess or lesions are indicare cysts or tumors.
palpated.
Palpate fremitus. Using the Fremitus is symmetric Diminished vibrations even with a
sequence for the anterior chest and easily identified in the loud spoken voice, may indicate
described previously, palpate for upper regions of the an obstruction of the
fremitus using the same technique lungs. A decreased tracheobronchial tree. Clients with
same as for the posterior thorax. intensity of fremitus is emphysema may have
expected toward the base considerably decreased fremitus
of the lungs. However, as a result of air trapping.
fremitus should be
symmetric bilaterally.
Palpate anterior chest Thumbs move outward in Unequal chest expansion can
expansion. Place your hands on a symmetric fashion from occur with severe atelectasis,
the client’s antero-lateral wall with the midline. pneumonia, chest trauma, pleural
your thumbs along the costl effusion, or pneumothorax.
margins and pointing toward the Decreased chest excursion at the
xiphoid process. As the client base of the lungs is seen with
takes a deep breath, observe the COPD.
movement of your thumbs.
PERCUSSION
Percuss for tone
Percuss the apices above the Resonance is the Hyperresonance is elicited in
clavicles. Then percuss the percussion tone elicited cases of trapped air such as in
intercostal spaces across and over normal lung tissue. emphysema or pneumothorax.
down, comparing sides. Depicts normal tones and Dullness may characterize areas if
their locations. increased density such as
consolidation, pleural, effusion or
Percussion elicits tumor.
dullness over breast
tissue, the heart, and the
liver. Tympany is
detected over the
stomach and flatness is
detected over the
muscles and bones.
THORAX AND LUNGS 14
AUSCULTATION NORMAL ABNORMAL FINDINGS
Auscultation for anterior breath Voice transmission is Refer to adventitious breath
sounds, adventitious sounds soft, muffled, and sounds.
and voice sounds. Place the indistict. The sound of theDiscontinuous sounds:
diaphragm of the stethoscope voice may be heard but 1. Crackles (fine)
firmly and directly on the anterior the actual phrase cannot 2. Crackles (coarse)
chest wall. be distinguished. Continuous sounds:
1. Pleural friction rub
Voice transmission will be 2. Wheeze (sibilant)
soft and muffled but the 3. Wheeze (sonorous)
letter “E” should be
distinguishable.
Transmission of sound is
very faint and muffled. It
may be inaudible.
Auscultate from the apices of The words are easily understood
the lungs slightly above the and louder over of increased
clavicles to the bases of the density. This may indicate
lungs at the sixth rib. Ask the consolidation from pneumonia,
client to breathe deeply through atelectasis or tumor.
the mouth in an effort to avoid
transmission of sounds that may Over areas of consolidation or
occur with nasal breathing. Be compression the sound is louder
alert to the client’s comfort and and sound like “ A.”
offer times for rest and normal
breathing if fatigue is becoming a Over areas of consolidation or
problem, particularly for the older compression, the sound is
client. transmitted clearly and distinctly.
In such areas, it sounds as if the
Listen at each site for at least one client is whispering directly into the
complete respiratory cycle. Follow stethoscope.
the sequence for anterior
auscultation.
THORAX AND LUNGS 15
Table 1
NORMAL BREATH SOUNDS
Type Pitch Quality Amplitude Duration Location
Bronchial High Harsh or Loud Short during Trachea and
hollow inspiration long thorax
in expiration.
Bronchovesicular Moderate Mixed Moderate Same during Over the
inspiration and major bronchi-
expiration. posterior
between
scapulae;
anterior
around the
upper sternum
in the first and
second
intercostal
spaces
Vesicular Low Breezy Soft Long in Peripheral
inspiration lung fields.
short in
expiration.
Table 2
ADVENTITIOUS BREATH SOUNDS
Abnormal sounds Characteristics Source Associated
Conditions
Discontinuous
sounds
Crackles (fine)
High-pitched, short, Inhaled air suddenly
popping sounds opens the small, Crackles occurring
heard during deflated air passages late in inspiration are
inspiration and not that are coated and associated with
cleared with sticky with exudate. restrictive diseases
coughing; sounds are such as pneumonia
discontinuous and and congestive heart
can be stimulated by failure. Crackles
rolling a strand of hair occurring early in
between your fingers inspiration are
near your ear. associated with
obstructive disorder
such as bronchitis,
asthma or
emphysema.
THORAX AND LUNGS 16
Crackles Low-pitched, Inhaled air comes May indicate pneumonia,
(coarse) bubbling, moist into contact with pulmonary edema, and
sounds that may secretions in the pulmonary fibrosis. Velcro
persist from early large bronchi and rales of pulmonary fibrosis
inspiration to early trachea. are heard louder, and closer
expiration; also to stethoscope, usually do not
described as softly change location, and are
separating Velcro. more common in clients with
long-term COPD.
Continuous
Sounds
Pleural friction Low-pitched, dry, Sound is the result Pleuritus
rub grating sound; sound of rubbing of two
like crackles, only inflamed pleural
more superficial and surfaces.
occurring during both
inspiration and
expiration.
Wheeze High-pitched, Air passes through Sibilant wheezes are often
(Sibilant) musical sounds constricted heard in cases of acute
heard primarily passages (caused asthma or chronic
during expiration but by swelling, emphysema.
may also be heard secretions or
on inspiration. tumor.
Wheeze Low-pitched snoring Same as sibilant Sonorous wheezes are often
(Sonorous) or moaning sounds wheeze. The pitch heard in cases of bronchitis
heard primarily of the wheeze or single obstruction and
during expiration but cannot be snoring before an episode of
may be heard correlated to the sleep apnea. Stridor is a
throughout the size of the harsh, honking, wheeze with
respiratory cycle. passageway that severe
These wheezes may generates it. broncholaryngospasm such
clear with coughing. as occurs with croup.
THORAX AND LUNGS 17
Table 3
RESPIRATORY PATTERNS
Type Description Clinical indication
Normal 12-20 bpm Normal breathing pattern
Tachypnea More than 24 breaths Maybe be normal response to fever,
per/min and shallow anxiety or exercise can occur with
respiratory insufficiency, alkalosis,
pneumonia or pleurisy.
Bradypnea Less than 10 BPM and May be normal in well-continued
regular athletes. Can occur with medication-
induced depression of the respiratory
center, diabetic coma, neurologic
damage.
Hyperventilation Increased rate and Usually occurs with extreme
increased depth. exercise, fear or anxiety. Cause of
hyperventilation include disorders of
the CNS, an overdose of the drug
salicylate or severe anxiety.
Kussmaul Rapid, deep, labored A type of hyperventilation associated
with diabetic ketoacidosis.
Hypoventilation Decreased rate, Usually associated with overdose of
decreased depth, narcotics or anesthetics.
irregular pattern.
Cheyne-Stokes Regular pattern May result from severe congestive
respiration characterized by heart failure, drug overdose,
alternating periods of increased intracranial pressure or
deep, rapid breathing renal failure. May be noted in elderly
followed by periods of persons during sleep, not related to
apnea. any disease process.
Biot respiration Irregular pattern Meningitis or severe brain damage.
characterized by varying
depth and rate of
respirations followed by
periods of apnea.
Ataxic Significant A more extreme expression of Biot
disorganization with respirations indicating respiratory
irregular and varying compromise.
depths of respiration.
Air trapping Increasing difficulty in In chronic obstructive pulmonary
getting breath out. disease, air is trapped in the lungs
during forced expiration.
THORAX AND LUNGS 18
You might also like
- Lesson Exemplar-Circulatory SystemDocument10 pagesLesson Exemplar-Circulatory SystemRica Manansala IbeNo ratings yet
- Lung Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandLung Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Problems With OxygenationDocument92 pagesProblems With OxygenationEbiNo ratings yet
- NursingBulletin Respiratory SystemDocument35 pagesNursingBulletin Respiratory Systemseigelystic100% (3)
- Blood Tranfusion11Document60 pagesBlood Tranfusion11Marites Angeles Bautista100% (2)
- Care of Clients with Respiratory ProblemsDocument115 pagesCare of Clients with Respiratory ProblemsarielleortuosteNo ratings yet
- Section-I Mcqs and SeqsDocument3 pagesSection-I Mcqs and SeqsSadia NasirNo ratings yet
- Rabbit RespirationDocument5 pagesRabbit RespirationshajehanNo ratings yet
- Anatomy and Physiology of Respiratory SystemDocument21 pagesAnatomy and Physiology of Respiratory Systemsameeha semiNo ratings yet
- Anatomy and Physiology: The Respiratory SystemDocument82 pagesAnatomy and Physiology: The Respiratory SystemMaria Angelique Ofciar100% (2)
- Anatomy and Physiology of the Respiratory SystemDocument43 pagesAnatomy and Physiology of the Respiratory Systemflex gyNo ratings yet
- Respiratory System Practice TestDocument25 pagesRespiratory System Practice TestEstevan MartinezNo ratings yet
- Bronchial AsthmaDocument21 pagesBronchial AsthmaMoonNo ratings yet
- Human Respiratory System ExperimentDocument6 pagesHuman Respiratory System ExperimentRohan Saste100% (1)
- Reticulo Endothelial SystemDocument15 pagesReticulo Endothelial Systemssdb14No ratings yet
- Respiratory System (Anatomy)Document54 pagesRespiratory System (Anatomy)Juliet Ileto Villaruel - AlmonacidNo ratings yet
- Digestive System in 40 CharactersDocument2 pagesDigestive System in 40 CharactersZinya Robinson100% (1)
- Anatomy and Physiology of Respiratory SystemDocument6 pagesAnatomy and Physiology of Respiratory SystemMonica VelascoNo ratings yet
- Respiratory System NotesDocument5 pagesRespiratory System NotesBrandice BradleyNo ratings yet
- Respiratory System: Ventilation Cellular RespirationDocument4 pagesRespiratory System: Ventilation Cellular RespirationSoleil MaxwellNo ratings yet
- Supplementary Material 3.1 Basic Concepts and Assessment (N) - 2Document13 pagesSupplementary Material 3.1 Basic Concepts and Assessment (N) - 2Kent Borro CantomayorNo ratings yet
- Resp 2023 Arsi-1Document118 pagesResp 2023 Arsi-1abenezer isayasNo ratings yet
- 2020 Respiratory SystemDocument146 pages2020 Respiratory Systemsyafi zulNo ratings yet
- Unit 7: Respiratory System (2 Hours Lecture/3 Hours Lab) : at The End of This Unit, Students Will Be Able ToDocument4 pagesUnit 7: Respiratory System (2 Hours Lecture/3 Hours Lab) : at The End of This Unit, Students Will Be Able ToRUSSEL AQUINONo ratings yet
- X Respiratory SystemDocument31 pagesX Respiratory SystemHannah DiñosoNo ratings yet
- Respiratory SystemDocument21 pagesRespiratory SystemSalah ElwakilNo ratings yet
- Arbaminch College Respiratory SystemDocument6 pagesArbaminch College Respiratory SystemWorkinesh Kaynabo KambaloNo ratings yet
- Anatomy & PhysiologyDocument42 pagesAnatomy & PhysiologyArah Lyn ApiagNo ratings yet
- Respiratory SystemDocument53 pagesRespiratory SystemRotan CirebonNo ratings yet
- 2- الجاهزة20.02.2022 lower Respiratory system physiologyDocument32 pages2- الجاهزة20.02.2022 lower Respiratory system physiologybessan alfqeatNo ratings yet
- Respiiiraatatoory SystemDocument78 pagesRespiiiraatatoory Systempriyanshuraj717No ratings yet
- Respiratory System ExplainedDocument42 pagesRespiratory System ExplainedSohailriazNo ratings yet
- General Introduction: Respiration Takes Place in Four StagesDocument4 pagesGeneral Introduction: Respiration Takes Place in Four Stagesriskyy1No ratings yet
- Zoo 1 PPT 10 Respiratory (2015)Document17 pagesZoo 1 PPT 10 Respiratory (2015)Zucc mahnutNo ratings yet
- 1a - Gonzalez, Jamaica Caryl N. (Respiratory)Document13 pages1a - Gonzalez, Jamaica Caryl N. (Respiratory)Jhamm GonzalezNo ratings yet
- ANATOMY OF THE RESPIRATORY SYSTEMzDocument12 pagesANATOMY OF THE RESPIRATORY SYSTEMzalthea jade villadongaNo ratings yet
- Respi SystemDocument33 pagesRespi SystemJohn Harzel NagaNo ratings yet
- TH E RE SP IRA TO RY SY ST EM: Learning ObjectivesDocument36 pagesTH E RE SP IRA TO RY SY ST EM: Learning Objectivesmaria tafaNo ratings yet
- BMED 66 Chapter 17 REspiratory SystemDocument7 pagesBMED 66 Chapter 17 REspiratory SystemBSMT 1-1, TAN, NICOLE SELINA L.No ratings yet
- d77be476 c1ec 4034 a6e7 305113d3044dPhysiology of RespirationDocument9 pagesd77be476 c1ec 4034 a6e7 305113d3044dPhysiology of RespirationMalti SharmaNo ratings yet
- Respiratory SystemDocument29 pagesRespiratory SystemCHARMAINE ORUGANo ratings yet
- Breathing and Exchange of Gases-HumansDocument14 pagesBreathing and Exchange of Gases-Humansnihalbolla2023No ratings yet
- Anatomy of The Respiratory SystemDocument37 pagesAnatomy of The Respiratory SystemPal SedNo ratings yet
- Anatomy and Physiology 2nd Semester BSN Notes, Educational PlatformDocument367 pagesAnatomy and Physiology 2nd Semester BSN Notes, Educational PlatformMuhammad KashifNo ratings yet
- 172 Anatomy Resp SystemDocument29 pages172 Anatomy Resp SystemJerry ZahidNo ratings yet
- Respiratory System Functions and AnatomyDocument40 pagesRespiratory System Functions and AnatomychromaNo ratings yet
- Kuliah 3 Respirasi + CardiovasculerDocument73 pagesKuliah 3 Respirasi + CardiovasculerNindya Alfa DichaNo ratings yet
- Lecture - 5 PDFDocument5 pagesLecture - 5 PDFDavid JokerNo ratings yet
- M7 RespiratoryDocument6 pagesM7 RespiratoryNel joy PaurilloNo ratings yet
- Exercise IxDocument27 pagesExercise IxShengrace GavinoNo ratings yet
- RESPIRATORY DISTURBANCES - HandoutsDocument35 pagesRESPIRATORY DISTURBANCES - Handoutsfebie pachecoNo ratings yet
- Respiratory System OverviewDocument17 pagesRespiratory System Overviewsaad SaadNo ratings yet
- The Respiratory System: ASTIKA NUR ROHMAH, S.Kep., NS., M.BiomedDocument43 pagesThe Respiratory System: ASTIKA NUR ROHMAH, S.Kep., NS., M.BiomedAdek KhazeliaNo ratings yet
- Dulutalias - Chapter23-THE RESPIRATORY SYSTEMDocument15 pagesDulutalias - Chapter23-THE RESPIRATORY SYSTEMKie MusstisqueNo ratings yet
- 1-Respiratory MechanicsDocument56 pages1-Respiratory MechanicsDoha JKNo ratings yet
- Respiratory System PreDocument11 pagesRespiratory System PrecontehamosaNo ratings yet
- XII Notes (SHRT QS) .Document65 pagesXII Notes (SHRT QS) .AmnaNo ratings yet
- Respiratory System s2 2019Document56 pagesRespiratory System s2 2019noviantyramadhani12No ratings yet
- Anatomy and Physiology of The Respiratory System (Vizconde, Ehreiz Raiden C. BSN2A)Document4 pagesAnatomy and Physiology of The Respiratory System (Vizconde, Ehreiz Raiden C. BSN2A)Raiden VizcondeNo ratings yet
- Respiratory SystemDocument5 pagesRespiratory SystemPreeti ChouhanNo ratings yet
- 17 - The Functional Structure of The Respiratory System - Ass. Prof. Mona Gamal - 2020Document7 pages17 - The Functional Structure of The Respiratory System - Ass. Prof. Mona Gamal - 2020Hossam BaniisNo ratings yet
- Assessing Respiratory Function and Common InterventionsDocument15 pagesAssessing Respiratory Function and Common InterventionsJhosita Flora LarocoNo ratings yet
- Chapter 15Document6 pagesChapter 15Holy HaeinNo ratings yet
- Lect 3Document8 pagesLect 3علي الاسديNo ratings yet
- How Do Humans Breathe? Science Book Age 8 | Children's Biology BooksFrom EverandHow Do Humans Breathe? Science Book Age 8 | Children's Biology BooksNo ratings yet
- Theories and Principles of Health EthicsDocument47 pagesTheories and Principles of Health EthicsKristine Angie RamosNo ratings yet
- NCP Breast CADocument3 pagesNCP Breast CAHannah Lacambra100% (1)
- 2nd-Sem-Micro-Lab 2Document3 pages2nd-Sem-Micro-Lab 2Kristine Angie RamosNo ratings yet
- Microbial Diseases of The Respiratory SystemDocument37 pagesMicrobial Diseases of The Respiratory SystemKristine Angie RamosNo ratings yet
- Skin Checklist ProcedureDocument6 pagesSkin Checklist ProcedureKristine Angie RamosNo ratings yet
- Funda Lab Report 1 1Document11 pagesFunda Lab Report 1 1Kristine Angie RamosNo ratings yet
- Ged 102 ActivityDocument8 pagesGed 102 ActivityKristine Angie RamosNo ratings yet
- Micro para LecDocument3 pagesMicro para LecKristine Angie RamosNo ratings yet
- Kristine Angie Ramos Bsn1-A STSDocument7 pagesKristine Angie Ramos Bsn1-A STSKristine Angie RamosNo ratings yet
- My Civic Welfare Activity: St. Paul College of Ilocos SurDocument2 pagesMy Civic Welfare Activity: St. Paul College of Ilocos SurKristine Angie RamosNo ratings yet
- HYGIENE AND COMFORT Assignment or ActivityDocument2 pagesHYGIENE AND COMFORT Assignment or ActivityKristine Angie RamosNo ratings yet
- Untitled DocumentDocument8 pagesUntitled DocumentKristine Angie RamosNo ratings yet
- Practical Exercise 1: Answer ThisDocument1 pagePractical Exercise 1: Answer ThisKristine Angie RamosNo ratings yet
- Module 3 - Setting Goal Activity Answer SheetDocument1 pageModule 3 - Setting Goal Activity Answer SheetKristine Angie RamosNo ratings yet
- Kristine Angie Ramos - Module 3 - Act 3Document3 pagesKristine Angie Ramos - Module 3 - Act 3Kristine Angie RamosNo ratings yet
- Kristine Angie Ramos - Module 3 - Act 2Document2 pagesKristine Angie Ramos - Module 3 - Act 2Kristine Angie RamosNo ratings yet
- Part 2 Final Exam Ged 102Document10 pagesPart 2 Final Exam Ged 102Kristine Angie Ramos0% (1)
- CHECKLIST FOR Proper Hand WashingDocument5 pagesCHECKLIST FOR Proper Hand WashingKristine Angie RamosNo ratings yet
- COVID-19's Psychological Impact on Healthcare WorkersDocument8 pagesCOVID-19's Psychological Impact on Healthcare WorkersKristine Angie RamosNo ratings yet
- 1.4 The Lymphatic SystemDocument11 pages1.4 The Lymphatic SystemCikdar Yunus100% (1)
- Organs and Organ Systems P1Document8 pagesOrgans and Organ Systems P1Arniel CatubigNo ratings yet
- Lesson Plan: ObjectivesDocument4 pagesLesson Plan: ObjectivesChaden Al TawilNo ratings yet
- Pharmacodynamic Study of Polyethylene Glycol Conjugated Bovine Hemoglobin (Peg-Bhb) in RatsDocument16 pagesPharmacodynamic Study of Polyethylene Glycol Conjugated Bovine Hemoglobin (Peg-Bhb) in RatsIstván PortörőNo ratings yet
- Circulatory SystemDocument22 pagesCirculatory SystemEzequiel ManluluNo ratings yet
- Just Go with the FlowDocument2 pagesJust Go with the FlowIRIS50% (2)
- Foss - Living Systems Content QuestionsDocument2 pagesFoss - Living Systems Content Questionsapi-242986395No ratings yet
- To Study The Effect of Buteyko Breathing Technique in Patients With Obstructive Airway DiseaseDocument15 pagesTo Study The Effect of Buteyko Breathing Technique in Patients With Obstructive Airway DiseaseGerry KrikhoffNo ratings yet
- Lymphatic System SummaryDocument2 pagesLymphatic System SummaryLizbeth Quinn BatangosoNo ratings yet
- Informative Speech DhafaDocument9 pagesInformative Speech Dhafadhafah sajaNo ratings yet
- Patient's Name: Jannah U. Rakim Age: 22 Sex: Female Room: APDocument7 pagesPatient's Name: Jannah U. Rakim Age: 22 Sex: Female Room: APtflorenz100% (1)
- Mod 8 ZooDocument10 pagesMod 8 ZooLM Tricia T. DE LA CRUZNo ratings yet
- Experiment of Human PhysiologyDocument6 pagesExperiment of Human Physiologyapi-383624767No ratings yet
- REFERAT II - 2ndDocument40 pagesREFERAT II - 2ndagung anugrahNo ratings yet
- Circulatory System AssessmentDocument4 pagesCirculatory System Assessmentapi-98991203No ratings yet
- Biological Rhythms: Dr. Zahiruddin OthmanDocument40 pagesBiological Rhythms: Dr. Zahiruddin OthmanZubair Ul IslamNo ratings yet
- Science Year 4Document6 pagesScience Year 4Masnizan Binti HamdanNo ratings yet
- Energy Producing & Distributing SystemsDocument40 pagesEnergy Producing & Distributing SystemsZerille Anne InsonNo ratings yet
- Blood TransfusionDocument17 pagesBlood TransfusionRayne BonifacioNo ratings yet
- Hazards of Blood TransfusionDocument2 pagesHazards of Blood TransfusionSakshi ShuklaNo ratings yet
- Advance Nursing 1 End of SemDocument17 pagesAdvance Nursing 1 End of SemGraham Wilfred Addah GilbertNo ratings yet
- Pcap Pathophysiology PDFDocument3 pagesPcap Pathophysiology PDFMikaela RamosNo ratings yet
- Sleeping Twice British English TeacherDocument12 pagesSleeping Twice British English TeacherIgorNo ratings yet
- Lymphatic and Immune SystemDocument2 pagesLymphatic and Immune SystemmkpovakNo ratings yet