Professional Documents
Culture Documents
Microbio (Bacte)
Microbio (Bacte)
Uploaded by
Carl PinedaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Microbio (Bacte)
Microbio (Bacte)
Uploaded by
Carl PinedaCopyright:
Available Formats
TOPIC: (ENTER TOPIC HERE) STAPHYLOCOCCUS SPECIES
INSTRUCTOR: MATTHEW TUBOLA, RMT ● Two species are commonly associated with
staphylococcal diseases in humans:
1. Staphylococcus aureus
OUTLINE OF THE LESSON ➔ More virulent strain
➔ Some people are “carriers” in nose
I. INTRODUCTION and on skin.
A. (SUB TOPICS) 2. Staphylococcus epidermidis
- (SUPER SUB TOPIC) ➔ Normal microbiota of human skin
II. TITLE #2 ➔ Can cause opportunistic infections
HIGHLIGHTING BULLET PLACEMENT PATHOGENICITY
OF TOPICS ● ‘“Staph infections result when
staphylococci break through the body’s
Aaaaa - Main topic ● (Main definition) physical barriers
Aaaaa - Sub-topics ➔ (Sub-definition / ● Low “infectious dose”
AAAA - Title of Topic Enumerate) ➔ Entry of only a few hundred bacteria can
❖ Additional detail result in disease
● Pathogenicity results from the three
NOTE: (for additional
virulence factors
information during
discussions)
➔ Evades phagocytosis by capsule
production
➔ Produces enzymes
GRAM POSITIVE COCCI ➔ Produces exotoxins
STAPHYLOCOCCUS DEFENSE AGAINST PHAGOCYTOSIS
● Normal flora of every human ● Protein A coats the cell surface
● Gram-positive cocci in clusters ➔ Binds to class G antibodies
● Catalase positive Inhibits the complement cascade
● Facultative anaerobe ● Slime layer
● Tolerant of ➔ Inhibits chemotaxis of leukocytes
➔ Salt ➔ Helps Staphylococcus attach to artificial
➔ Desiccation surfaces
ENZYMES
COAGULASE
● Converts fibrinogen into fibrin to form blood
clots
● Fibrin clots hide the bacteria from
phagocytic cells
HYALURONIDASE
● Breaks down hyaluronic acid, enabling the
bacteria to spread between cells.
STAPHYLOKINASE
● Dissolves fibrin threads in blood clots,
allowing S. aureus to free itself from clots.
LIPASE
● Digest lipids, allowing staphylococcus to
grow on the skin’s surface and in oil glands
BETA-LACTAMASE
● Breakdown penicillin
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 1
● Allows the bacteria to survive treatment with
B-lactam antimicrobial drugs
➔ Methicillin - derivative of penicillin that
is resistant to beta-lactamase
➔ MRSA - Methicillin resistant
Staphylococcus aureus to grow on the
skin’s surface and in oil glands
TOXINS
CYTOLYTIC TOXINS SYSTEMIC DISEASE
● Disrupts host’s cell membrane ● Bacteremia
● Leukocidins lyse leukocytes ➔ Presence of bacteria in the blood from
wound infections
EXFOLIATIVE TOXINS ➔ 50% are nosocomial infections
● Causes skin cells to separate and slough off ● Endocarditis
➔ Occurs when bacteria attack the lining
TOXIC-SHOCK-SYNDROME TOXIN of the heart; 50% mortality rate
◆ Not that common
ENTEROTOXINS ● Pneumonia
● Stimulate intestinal muscle contractions, ➔ Inflammation of the lungs in which the
nausea, and intense vomiting associated alveoli and bronchioles become filled
with Staphylococcal food poisoning with fluid
● Toxin is heat-stable; resistant to boiling ● Osteomyelitis
NOTE: The bacteria may die but the spore is ➔ Inflammation of the bone marrow and
still present the surrounding bone; from wound or
bacteremia
COMPARISON OF VIRULENCE FACTORS
DIAGNOSIS, TREATMENT, & PREVENTION
DIAGNOSIS
● Detection of Gram-positive bacteria in
grape like arrangements isolated from pus,
blood or other fluids
TREATMENT
● Methicillin is the drug of choice
➔ Is a semisynthetic form of penicillin and
is not inactivated by B-lactamase
● MRSA - Methicillin-resistant Staph. Areus
➔ Vancomycin - drug of choice for
moderate to severe infections
TREATMENT FOR MRSA
STAPHYLOCOCCAL DISEASES ● Ceftaroline (Brand name Teflaro)
CUTANEOUS DISEASE ➔ The first commercially available
● Folliculitis cephalosporin with activity against:
➔ Hair follicle infection ❖ Methicillin-resistant Staphylococcus aureus
● Furuncle (MRSA)
➔ Boil ❖ Penicillin-resistant Staphylococcus
● Carbuncle pneumoniae
➔ Involves connective tissue ➔ In addition, ceftaroline is active against
● Impetigo most non-ESBL Enterobacteriaceae
➔ Red patches; pus-filled crust ➔ NOTE: a broad-spectrum antibiotic
PREVENTION OF MRSA SPREAD IN ICU
● All patients in ICU bathed daily with a 2%
chlorhexidine containing cloth, and had an
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 2
antibiotic ointment of mupirocin applied ● An illness with the following clinical
twice daily inside their nose (the body site manifestations:
most commonly colonized with S. aureus) 1. Fever :greater than or equal to 102.0°F
for 5 days 2. Rash: diffuse macular erythroderma
● 44% reduction in all septicemias including 3. Desquamation: 1-2 weeks after onset
those caused by MRSA. The incidence of of illness, particularly on the palms and
MRSA colonization on these patients was soles
reduced by 37%. 4. Hypotension: systolic blood pressure
● There are about 80,000 cases of invasive less than or equal to 90 mm Hg for
MRSA infections per year, resulting in adults
11,000 deaths annually. MRSA and 5. Multisystem involvement (3 or more):
Staphylococcus in general, account for examples -
approximately one quarter of the 80,000 ➔ Gastrointestinal: vomiting or
deaths from hospital-acquired infections in diarrhea at onset
the U.S. ➔ Muscular: severe myalgia (muscle
pain)
STAPHYLOCOCCUS TOXINS ➔ Hematologic: platelets less than
TOXIC SHOCK SYNDROME 100,000/mm3
● TSS toxin produced by Staphylococcus ➔ Renal, Hepatic, Central Nervous
aureus is absorbed into the blood and System
causes shock
● Linked to many initiating Staph infections STAPHYLOCOCCAL SCALDED
SKIN SYNDROME
● Caused by exfoliative toxins (ETA & ETB) of
Staph. aureus
● Acute exfoliation of the skin typically after an
erythematous cellulitis.
● Severity varies:
➔ Few blisters localized to the site of
infection
➔ Severe exfoliation affecting almost the
entire body
TOXIC SHOCK SYNDROME INFORMATION
● TSS was first described in children in
1978
● Later TSS was associated with menstruating Ritter von Ritterschein disease (in newborns)
women using highly absorbent tampons. Staphylococcus toxins
● Cases of menstrual TSS (1 case per FOOD POISONING
100,000) steadily declined after withdrawing ● From the ingestion of
these tampons from the market. enterotoxin-contaminated food
● 50% of cases of TSS are not associated ● Often this type of food poisoning occurs
with menstruation. when cooked food is allowed to cool slowly
● TSS usually are complications of surgical and/or sit at room temperature for some.
and postpartum wound infections, burns, ● Distinguish staphylococcal from other types
cutaneous lesions, osteomyelitis, and of food poisoning:
arthritis. ➔ short incubation period
● Although most cases of TSS occur in ➔ brevity of illness
women, about 25% of cases occur in men. ➔ usual lack of fever
TOXIC SHOCK SYNDROME - CDC CASE SEQUENCE OF EVENTS
IDENTIFICATION
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 3
saprophyticus either a bright yellow or white
pigment.
● S. aureus is usually beta-hemolytic, S.
epidermidis and S. saprophyticus are almost
always nonhemolytic.
STAPHYLOCOCCUS AUREUS
● Individual colonies on agar are round,
convex and 1-4 mm in diameter with a sharp
border.
● On blood agar plates, colonies of
DIAGNOSIS, TREATMENT, & PREVENTION
staphylococcus aureus are frequently
PREVENTION OF “STAPH” INFECTIONS
surrounded by zones of clear
● Prevention of “Staph” infections
beta-hemolysis.
➔ Hand antisepsis is the most important
● The golden appearance of some strains is
measure in preventing nosocomial
the etymological root of the bacteria’s name;
infections
aureus meaning “golden” in Latin.
➔ Proper cleansing of wounds and surgical
openings
➔ Aseptic use of catheters or indwelling
needles
➔ Refrigerate food
➔ Good hygiene
LABORATORY IDENTIFICATION
● Staphylococcus is a genus of bacteria that is
characterized by a round shape (coccus or NOTE:
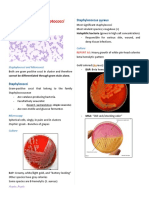
spheroid shaped), Gram-positive (purple), ● The left picture is of a MANNITOL SALT
and found as either single cells, in pairs, or AGAR showing the yellow colonies of S.
more frequently, in clusters that resemble a aureus. Originally, the MSA is colored
bunch of grapes. pink/red but in the case of S. aureus since it
● The genus name Staphylococcus is derived is a mannitol fermenter, its color becomes
from Greek terms (staphyle and kokkos) that yellow in that agar.
mean "a bunch of grapes"
STAPHYLOCOCCUS EPIDERMIDIS
● Showing y-hemolytic, porcelain-white
colonies as compared to S. aureus on BAP
● This clear distinction in colony color is seen
at all times.
STAPHYLOCOCCUS - BLOOD AGAR CULTURE
● Blood agar is both differential and enriched
medium.
● On blood agar, S. aureus usually displays a
light to golden yellow pigment, whereas S. CATALASE TEST
epidermidis has a white pigment and S.
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 4
● The Catalase test is primarily used to
distinguish among Gram-positive cocci
● Members of the genus Staphylococcus are
catalase positive, and members of the
genera Streptococcus and Enterococcus are
catalase-negative.
COAGULASE SLIDE TEST (CLUMPING FACTOR)
● Use BSL-2 precautions when performing
this test with an unknown organism or S.
NOTE: aureus
● Hydrogen peroxide (H2O2), the reagent, is ● Detects BOUND coagulase (difference from
dropped on a colony placed on a glass slide. Tube Coagulase test)
● If catalase is present, the enzyme will break
down H2O2 into oxygen and water. The
oxygen product can be seen physically or
macroscopically as BUBBLE FORMATION.
➔ BUBBLES (+) = Staphylococcus
➔ NO BUBBLES (-) = Streptococcus
or Enterococcus
COAGULASE TEST
● The only significant disease causing
bacteria of humans that produce Coagulase
enzyme are staphylococcus aureus. NOTE:
● The action of the coagulase enzyme ● The procedure for both the TUBE and
produces clotting of the plasma by SLIDE coagulase tests are the same.
converting fibrinogen to fibrin in the ➔ Plasma is added to a colony/growth
immediate vicinity of the bacteria as a of bacteria, and the occurrence of
means of protection by itself clotting is noted.
● Used to distinguish between pathogenic and ❖ CLOTTING: (+)
non pathogenic members of the genus ❖ NO clotting: (-)
Staphylococcus. All pathogenic strains of S.
aureus are coagulase positive whereas the MANNITOL SALT AGAR
nonpathogenic species (S. epidermidis) are ● Mannitol salt agar (MSA) is both a selective
coagulase negative and differential media used for the isolation
of staphylococci from mixed cultures
TUBE COAGULASE TEST ● On MSA, only pathogenic staphylococcus
● Free coagulase secreted by S.aureus but aureus produces small colonies surrounded
not CNS by yellow zones
● Clots rabbit plasma ● The reason for this color change is that
S.aureus have the ability to ferment
mannitol, producing an acid, which changes
the indicator color from red to yellow
● MSA components:
➔ 7.5% NaCl - selects for species of
Staphylococcus. This concentration
of salt is too high for most other
bacteria to withstand and, therefore,
inhibits their growth
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 5
❖ Other bacteria can only
withstand up to 6.5%.
➔ Mannitol - alcohol of the
carbohydrate mannose. Mannitol
fermentation produces acid end
products which turn the medium
yellow. Yellow indicates mannitol
positive and no color change
indicates mannitol negative
➔ Phenol red pH indicator - yellow in
acid pH (the same indicator that is
used in phenol red carbohydrate
fermentation broths)
❖ Phenol red is color red in
neutral pH.
GROUP A STREPTOCOCCUS =
STREPTOCOCCUS PYOGENES
● Beta-hemolytic
● Infects the pharynx or skin
● Often causes disease when normal
microbiota are depleted
● Spreads through respiratory droplets
.
STREPTOCOCCUS
● Gram-positive cocci, arranged in pairs or
chains
● Catalase negative
● Facultative anaerobes
➔ Aerobes that can grow without
oxygen (anaerobic condition) BETA HEMOLYSIS
● Categorized based on: ● Streptococcus pyogenes, or group A
➔ Hemolysis beta-hemolytic streptococci (GAS), and
❖ Brown’s classification Streptococcus agalactiae, or group B
(discovered by Brown) beta-hemolytic Streptococci (GBS) blood
❖ Ability to lyse RBCs agar cultures display beta hemolysis
❖ Beta, Alpha, Gamma ● Beta hemolysis, sometimes called
➔ Lancefield Grouping complete hemolysis, is a complete lysis of
❖ Divides the streptococci into red loom cells in the media around and
serotype groups based on under the colonies: the area appears
the bacteria’s cell wall lightened (yellow) and transparent
antigens
❖ Group A and B are
pathogens
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 6
● rash that begins on the chest and
spreads across the body
➔ The origin of the rash can
be used to differentiate from
other viral diseases (e.g.
mumps, measles).
3. Pyoderma/Impetigo
● confined, pus-producing lesion that
usually occurs on the face, arms, or
legs
4. Necrotizing fasciitis
● toxin production destroys tissues
and eventually muscle and fat tissue
➔ “Flesh-eating disease”
GROUP A STREP - VIRULENCE FACTORS
1. M protein of fimbriae STREPTOCOCCUS PYOGENES - STREP
● adheres to pharyngeal tissue THROAT
● resists phagocytosis ● Symptoms:
● 80 serotypes ➔ sore throat, cough
➔ high fever
➔ swollen lymph nodes
➔ “beefy” red throat
● Treatment:
➔ penicillin
● Autoimmune Complications:
➔ Rheumatic fever – inflammation
that leads to damage of heart valves
muscle
➔ Glomerulonephritis – inflammation
of the glomeruli and nephrons
obstruct blood flow through the
NOTE: kidneys
● The picture on the right shows the ❖ Can lead to renal failure
FIMBRIAE (color gray).
● The black dots on the picture on the
left are the M protein of the fimbriae.
2. Toxins
● Streptolysin O and S - hemolysis
➔ O: oxygen-LABILE NOTE:
➔ S: oxygen-STABLE ● The autoimmune complications are due to
● Erythrogenic toxin - rash immune complex deposition either in the
● Pyrogenic toxin - fever heart (rheumatic fever) or kidneys
3. Enzymes (glomerulonephritis) as a result of
● Deoxynuclease repeated/recurrent strep throat infections.
● Hyaluronidase
● Streptokinase – lyse platelets, WBC GROUP A STREPTOCOCCAL DISEASES
● Help spread bacteria through tissue SCARLET FEVER
● Accompanies strep throat if strain
GROUP A STREPTOCOCCAL DISEASES releases erythrogenic toxins
1. Pharyngitis (“strep throat”) ● Symptoms:
● inflammation of the pharynx ➔ strep throat
● Most common disease caused by S. ➔ “strawberry” tongue
pyogenes ➔ skin rash due to erythrogenic toxins
2. Scarlet fever ● Treatment:
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 7
➔ Penicillin
GROUP A STREPTOCOCCUS SKIN DISEASES NOTE: Letter A in the picture is GAS, as evidenced
● Erysipelas by the zone of inhibition.
GROUP B STREPTOCOCCUS =
STREPTOCOCCUS AGALACTIAE
● Normally colonizes the lower
gastrointestinal, genital, and urinary tracts
● Diseases
● Pyoderma (Impetigo) ➔ Most often associated with neonatal
bacteremia, meningitis, and
pneumonia
➔ Immunocompromised older patients
are at risk
● Pathogenicity
➔ Often infects newborns who have
● Necrotizing fasciitis “flesh-eating” bacteria not yet antibodies and whose
➔ Generalized as “bacteria” because mothers do not provide passive
S. pyogenes is not the only bacteria immunity
that can cause necrotizing fasciitis. ● Prevention
➔ Culture the vaginal tract (swab) at
37 weeks (of gestation) to check for
colonization of Group B
Streptococcus. If positive,
prophylactic administration of
penicillin
➔ Prophylactic administration of
BACITRACIN SENSITIVITY TEST (BETA penicillin at birth to children whose
HEMOLYTIC STREPTOCOCCI GROUP A, GAS) mothers’ urinary tracts are colonized
● In a clinical laboratory, bacitracin is useful in with group B streptococci
helping identify streptococci and other gram
positive bacteria CAMP TEST (B-HEMOLYTIC STREPTOCOCCI
● Principle: bacitracin test is used to GROUP B, GBS)
determine the effect of a small amount of ● S. agalactiae is the only species that has the
bacitracin (0.04 UL) on an organism. group B antigen
Streptococcus pyogenes (GAS) is inhibited ● CAMP - it is an acronym for “Christie, Atkins,
by the small amount of bacitracin in the disk Munch-Petersen” for the three researchers
(visible zone if inhibition of growth); other who discovered the phenomenon
beta-hemolytic streptococci usually are not. ● The CAMP test is a test to identify Group B
B-hemolytic streptococci based on their
formation of a substance called CAMP factor
that enlarges the area of hemolysis formed
by B-hemolysin from Staphylococcus aureus
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 8
● Alpha hemolysis is caused by hydrogen
peroxide produced by the bacterium,
oxidizing hemoglobin to green
methemoglobin.
➔ Does not destroy/lyse RBCs directly
(like in beta hemolysis)
➔ In alpha hemolysis, the destruction
of hemoglobin (which is responsible
NOTE: for the red color of blood) is the
● In the pictures, the line in the middle is the reason for the green color produced.
S. aureus colony. Perpendicular to that line, ● Alpha hemolytic colonies with depressions in
colonies of the test organism are streaked. their centers are characteristics of
➔ If the organism is S. agalactiae, pneumococci
there will be an ● Some strains produce high amounts of
ARROWHEAD/BOW TIE hemolysis capsular polysaccharide which gives a
pattern in the juncture or the point glistening appearance.
where the organism is in contact
with the S. aureus colony. VIRULENCE FACTORS
1. Phosphorylcholine – stimulates cells to
ALPHA-HEMOLYTIC STREPTOCOCCI: phagocytize the bacteria
STREPTOCOCCUS PNEUMONIAE 2. Polysaccharide capsule - protects the
● Gram-positive diplococcus bacteria from digestion after endocytosis
➔ Lancet-shaped appearance 3. Protein adhesin – binds the cells to pharynx
● Alpha-hemolytic epithelial cells
● Normally colonizes the mouth and pharynx 4. Secretory IgA protease – destroys IgA
● Can cause disease if travels to the lungs (antibody found in mucous membranes)
● Disease is highest in children and the elderly 5. Pneumolysin – lyses epithelial cells and
suppresses the digestion of the endocytized
bacteria
DISEASES CAUSED BY S. PNEUMONIAE
● Pneumococcal pneumonia
➔ Bacteria multiply in the lower lung;
cause damage to the alveolar lining;
produce an inflammatory response
ALPHA-HEMOLYSIS
➔ High fever; chest pain; SOB; sputum
● Streptococcus pneumoniae, Streptococcus
production
salivarius, viridans (including Streptococcus
➔ 85% occur after viral disease (i.e. flu)
mutans) are referred to collectively as
● Sinusitis and otitis media
viridans streptococci, a name derived from
➔ Bacteria invade the sinuses or middle
viridis (Latin for “green”), referring to the
ear, often following a viral infection
green pigment formed by the partial, alpha
(usually the immune system is
hemolysis of blood agar
weakened)
● Encapsulated, virulent strains of S.
● Bacteremia and endocarditis
pneumoniae often forming highly mucoid,
➔ Bacteria in the bloodstream or in the
glistening colonies (production of capsular
lining of the heart
polysaccharide) surrounded by a zone of
● Pneumococcal meningitis
alpha-hemolysis.
➔ Bacteria that have spread to the
● This is sometimes called green hemolysis
meninges
because of the color change in the agar.
● Other synonymous terms are incomplete
STREPTOCOCCUS PNEUMONIAE
hemolysis and partial hemolysis.
● S. pneumoniae accounts for 25-35% of
cases of community-acquired bacterial
ALPHA-HEMOLYTIC STREPTOCOCCI:
pneumonia leading to 40,000 deaths/year in
STREPTOCOCCUS PNEUMONIAE
the US (Merck)
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 9
● Treatment – Penicillin ● Sodium deoxycholate (2% in water) will lyse
➔ Up to 35% of strains are resistant to the pneumococcal cell wall.
penicillin (as well as erythromycin, ● A clearing of the turbidity in the bile tube
Bactrim, cephalosporins) indicates a positive test.
● Prevention - Pneumovax
➔ Vaccine from purified capsular
polysaccharides
➔ Provides long lasting immunity in normal
adults; (not as effective in children, the
elderly, or AIDS patients)
ALPHA-HEMOLYTIC STREPTOCOCCI: THE
VIRIDANS GROUP
● Alpha-hemolytic (“viridans = green”) ENTEROCOCCUS
➔ Greenish discoloration in blood agar ● E. faecalis and E. faecium
● No Lancefield group ➔ Previously classified as group D
➔ Lack group-specific carbohydrates streptococci but reclassified as a
● Normal microbiota separate genus (enteroccocus and
➔ mouth, pharynx, GI tract, GU tract non-enterococcus)
● Opportunistic Disease: ● Normal microbiota of the human colon
➔ One of the causes of dental caries and ● Opportunistic disease:
dental plaques; produces dextran; leads ➔ Urinary Tract Infection
to biofilm formation ➔ Endocarditis
➔ Can cause meningitis and endocarditis ● Common cause of nosocomial infections
● Treatment: Difficult to treat due to resistance
OPTOCHIN TEST ➔ Ampicillin and ceftriaxone
● Optochin (or ethylhydrocupreine) is a ➔ VRE - Vancomycin Resistant
chemical used in cell culture techniques for Enterococcus
the of Streptococcus pneumoniae, which is
optochin-sensitive (positive result), from
other alpha- hemolytic streptococci such as ENTEROCOCCUS FAECALIS- GAMMA
Streptococcus viridans which are resistant. HEMOLYSIS
● If an organism does not induce hemolysis,
the agar under and around the colony is
unchanged, and the organism is called
non-hemolytic or said to display gamma
hemolysis.
● Enterococcus faecalis (formerly called
Group D Streptococcus) displays gamma
hemolysis
● E. faecalis typically exhibits
gamma-hemolysis on blood agar, but some
strains are alpha hemolytic or even
beta-hemolytic (a plasmid-encoding
hemolysin called cytolysin).
BILE SOLUBILITY TEST EPIDEMIOLOGY OF VRE: RISK FACTORS FOR
● The bile (sodium deoxycholate) solubility ACQUISITION
test distinguishes Streptococcus ● Prior broad spectrum antibiotics (especially
pneumoniae from all other alpha-hemolytic cephalosporins and vancomycin)
(viridans) streptococci ● Prolonged hospitalization
● Streptococcus pneumoniae is bile soluble ● Immunocompromised host
whereas all other alpha-hemolytic ● Neutropenia
streptococci are bile resistant. ● Admission to an intensive care unit
● Renal failure requiring dialysis
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 10
BIOCHEMICAL CHARACTERISTICS OF S.
AUREUS
POSITIVE NEGATIVE OTHERS
DETERMINE WHAT ISOLATE IS THIS
● Catalase ● Oxidase ● OF test -
● Coagulase ● Indole fermentativ
Staphylococcu ● Coagulase and Catalase - presence ● Gas (-) e
s intermedius POSITIVE of free ● Hydrogen ● Beta
● Novobiocin SENSITIVE and/or sulphide hemolysis
● PYR-POSITIVE bound ● Motility on blood
coagulase ● PYR agar
Group B ● Creamy zones of Beta ● Methyl red (Pyrrolidon
Streptococcus hemolytic colonies ● VP yl
(Streptococcus ● Hippurate POSITIVE (Vogues-P Arylamidas
agalactiae) ● Bowtie type hemolysis in roskauer) e Rapid)
CAMP test ● Nitrate Test
● PYR-NEGATIVE reduction
● Gela
Staphylococcu ● Yellow Beta hemolytic ● Citrate
s aureus colonies in MSA ● Urease
● Catalase and Coagulase
POSITIVE
● Grows in 7.5% NaCl
Strep Viridans ● Alpha hemolytic
● Optochin RESISTANT
● Bile solubility test
NEGATIVE
● Bile esculin NEGATIVE
COAGULASE NEGATIVE STAPHYLOCOCCI
STAPHYLOCOCCUS
● Gram positive, non-motile cocci about 1 um
in diameter
● Form (grapelike) clusters of cells
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 11
● Common inhabitants of the skin and mucous ● Selective media:
membranes ➔ Thayer Martin
● As a group, Staphylococci do not have ➔ Modified Thayer martin
spores or flagella but may form as capsules ➔ Martin Lewis
● They grow well on routine laboratory media ➔ Modified New York City medium
and are facultative anaerobes
STAPHYLOCOCCUS STREPTOCOCCUS
Clusters (grapelike) Pairs/ chains
Catalase positive Catalase negative
Coagulase positive Coagulase positive
Growth in 7.5% NaCl Growth in 6.5% NaCl
GRAM NEGATIVE COCCI
NEISSERIAE
TAXONOMIC CLASSIFICATION
● KINGDOM: Bacteria
● PHYLUM: Protobacteria
● CLASS: Betaproteobacteria
● ORDER: Neisseriales
● CLASS: Neisseriaceae
● GENUS: Neisseriae
GENERAL FEATURES
Gram negative diplococci aerobes
oxidase positive
● Catalase positive
● Aerobes and facultativeanaerobes
● Non sporing
● Non motile
● Optimum temperature: 35-36 C
● Optimum pH: 7-7.4
● 5-10 % CO2 enhances growth
● Fastidious in growth requirements
● Oxidase positive
● Catalase positive
IMPORTANT HUMAN PATHOGENS
● Superoxol test:
● Neisseria gonorrhoeae
➔ Positive in N. gonorrhoeae
● Neisseria meningitidis
➔ Negative in N. meningitidis and N.
➔ Other species normally colonize mucosal
lactamica
surfaces of oropharynx, nasopharynx and
● Carbohydrates are oxidatively utilized.
anogenital mucosal membranes.
➔ Mainly differentiated on the basis of
carbohydrate utilization tests: Glucose,
maltose, lactose and sucrose. ORGANISMS DISEASES
● Transport Media:
➔ Stuart’s media N. gonorrhoeae Urethritis, cervicitis,
➔ Amies media salpingitis, PID,
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 12
proctitis, bacteremia,
arthritis, conjunctivitis,
skin lesions, pharyngitis
N. meningitidis Meningitis, bacteremia,
pneumonia, arthritis
Other neisseria Opportunistic infections
species
NEISSERIA MENINGITIDIS ● Blood Agar- weak hemolysis
● Diplococcus intrecellularis ● Liquid media- granular turbidity
● Meningitidis DIFFERENTIAL MEDIA
● Meningococcus ● Blood Agar, Chocolate Agar
● Weichselbaum first discovered and isolated ● Mueller-hinton starch, Casein hydrolysate
in 1887 from the spinal fluid. agar
MORPHOLOGY ● Modified Thayer-Martin (Vancomycin,
● Gram negative cocci Colistin, Nystatin)
● Oval/spherical
● Capsulated BIOCHEMICAL REACTIONS
● 0.6-0.8 um in size. OXIDASE TEST POSITIVE
● Arranged in pairs (adjacent sides are flat) ➔ Freshly prepared 1% oxidase reagent
● Non-motile
● Generally intracellularly or may be (Tetramethyl Para Phenylenediamine
extracellular. Dihydrochloride)
CELLULAR CHARACTERISTICS ↓
● Exacting growth requirements Culture Media
● Blood, serum, ascitic fluid ↓
● Optimal temperature: 35-36 C (25-42 C) Deep Purple Colonies
● Optimal pH: 7.0-7.4
● Growth facilitated by 5% to 10% CO2 KOVAC’S METHOD
COLONIES Growth in a loop
● Small, 1mm in diameter ↓
● Translucent
Rub on a strip of filter paper moistened with
● Round, convex
oxidase reagent
● Bluish gray
● Smooth glistening surface
↓
● Entire edges Deep purple color
● Lenticular shape
● Butyrous consistency OTHER BIOCHEMICAL REACTIONS
● Easily emulsifiable
● Smooth and rough forms
Catalase test POSITIVE
Indole and Hydrogen NOT PRODUCED
Sulphide
Nitrates NOT REDUCED
Glucose and Maltose UTILIZED with ACID
PRODUCTION only
Neisseria meningitidis in Thayer-Martin Agar (Peptone serum agar
slope, RCUT)
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 13
➔ 5 classes; class 5 protein (opa and
opc) is involved in attachment and
invasion epithelial cells
➔ Class 2 and 3 are major OMPs.
RESISTANCE ● LIPOOLIGOSACCHARIDES
➔ Lack repeating O-Ag (Rough LPS)
● Delicate freeze ➔ Lipid A moiety-portion that mediates
drying, induction of inflammatory cytokines
Microbanking, ● OTHER FACTORS
Liquid nitrogen ➔ IgAse
➔ Pili
HIGHLY SUSCEPTIBLE ➔ Iron is obtained from transferrin
● Heat
● Desiccation
● Disinfectants INFLAMMATORY MEDIATORS AND MOLECULES
● Penicillin INVOLVED IN MENINGOCOCCAL DISEASE
● Alterations in pH ● IL-1
CLASSIFICATION ● IL-6
● Based on capsular polysaccharide ● IL-8
● PAF
● Prostaglandins
● TNF
● H2O2
● Singlet Excited Oxygen
● Hydroxyl radical
● CD62, ELAM-1
● ICAM-1, CD 18
PATHOGENICITY
● Human pathogens- nasopharynx
● Cerebrospinal meningitis
● Meningococcal septicemia
● Rhinitis
● Pharyngitis
● Conjunctivitis
● Serotyping based on class 1 OMP and
subtyping based on class 2 and 3
● Group, type, and subtype are phenotypic
characteristics.
● Types 2, 15 and recently type 4 have been
associated with group B meningococcal
disease.
● The majority of group C meningococci
belong to type 2 (2a or 2b)
ANTIGENICITY AND VIRULENCE
● CAPSULE
➔ Antiphagocytic
➔ Opsonizing anticapsular antibodies
are protective
➔ Meningococcal vaccine
● OUTER MEMBRANE PROTEINS
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 14
➔ Paralysis of cranial nerves causing
facial drooping
● Cortical venous thrombophlebitis
● Cerebral edema
● Children develop subdural effusion
● Permanent sequelae (especially in children)
include mental retardation,
deafness,hemiparesis
CLINICAL FEATURES
● Chills
● Malaise
● Prostration
● Petechial rashes
● Metastatic involvement of joints, ears, eyes,
lungs, adrenals
● 10% pneumonia
WATERHOUSE FRIDERICHSEN SYNDROME
● Fulminant meningococcemia
➔ “Fulminant” - developing or progressing
rapidly/suddenly all over the body
FEATURES ● Fatal condition causing:
● Nausea ➔ Shock
● Vomiting ➔ DIC
● Headache ➔ Multisystem failure
● Neck ➔ Deficiency of C5-C9
stiffness ➔ Pathogenic component-LPS (endotoxin)
● Lethargy ➔ Adrenal hemorrhage and shock
● Confusion ● A type of meningococcemia named after
Friderichsen
OTHER MANIFESTATIONS
● Arthritis
● Primary meningococcal pneumonia
● Meningococcal pericarditis
● Endocarditis
● Conjunctivitis
EPIDEMIOLOGY
COMPLICATIONS ● Transmission
● Cranial Nerve Palsy ➔ Airborne-droplets
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 15
➔ Fomites ➔ Detection of antibodies (Chronic
● Common in children between 3 months to 5 meningococcemia)
years ● Molecular diagnosis
● Crowded conditions ➔ Detection of Meningococcal DNA-PCR.
➔ Jail ● Serological tests:
➔ Ships ➔ CFT, HA, ELISA.
➔ Army camp
CSF EXAMINATION
● MENINGITIS BELT OF AFRICA ● Sample of choice for meningitis
➔ Ethiopia- Senegal ● Obtained through spinal tap
● In 1996 there are: ● General appearance: Purulent
➔ 150,000 cases ● Biochemical parameters:
➔ 15,000 deaths ➔ Glucose <35mg/100ml
➔ Proteins 80-500mg/100ml
● Cytology: 400-20,000 PMNs/μl.
● Centrifuge the CSF sample
● Plate out the deposit on BA and CA and
incubate at 37oc in 5-10% CO2 for 24 hours.
● Add glucose broth to the remaining deposit,
incubate overnight and subculture in the
same way. Examine the colonies by Gram
stain and Oxidase test.
● Make 2 smears of the centrifuged deposit
and stain with Gram stain and methylene
blue respectively.
● FITC coupled antiserum may be examined
for the direct identification of the
INDIAN SCENARIO
meningococcal serogroup responsible for
● Meningococcal disease is endemic in Delhi
infection.
and sporadic cases of meningococcal
● Divide the supernatant into 2 aliquots
meningitis have been occurring in Delhi in
➔ One for biochemical reactions
the past.
➔ The other for meningococcal
● Isolated cases of meningococcal meningitis
polysaccharide antigen detection by
during 1985 were also reported from several
latex agglutination, CIEP or
states of India including Haryana, Uttar
coagglutination.
Pradesh, Rajasthan, Sikkim, Gujarat,
● Biochemical reactions
Jammu & Kashmir, West Bengal,
● Antibiotic sensitivity testing
Chandigarh, Kerala and Orissa.
● Serogrouping
● Serogroup A has been associated with all
the repeated outbreaks of meningitis,
although serogroup B and C have been
detected in a few sporadic cases.
LABORATORY DIAGNOSIS
●
● Blood culture
➔ Incubation for TREATMENT
4-7 days ● Penicillin G or Ceftriaxone (Confirmed
● Nasopharyngeal cases)
swab ● Empirical treatment:
● Petechial lesions ➔ Up to 3 months: ampicillin+cefotaxime
● Autopsy or ceftriaxone.
➔ Lateral ➔ 3 months to 7 years: cefotaxime or
ventricle/surface of brain & S.C. ceftriaxone.
● Retrospective evidence
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 16
➔ >7 years: ampicillin or penicillin G +
cefotaxime or ceftriaxone.
➔ Dexamethasone may be started 15
minutes before starting antibiotics.
PREVENTION
● Meningococcal polysaccharide vaccines
(univalent and polyvalent vaccines).
CULTURAL CHARACTERISTICS
ANTIMICROBIAL PROPHYLAXIS ● Aerobes/ facultative anaerobes
● Rifampicin ● pH: 7.2 - 7.6
● Ciprofloxacin ● Temperature: 35C - 36C
● 5-10% CO2
VACCINES ● Chocolate agar, Mueller-Hinton agar, Thayer
● Five serogroups, A, B, C, Y and W135 are martin media, Modified TM medium,
responsible for virtually all cases of the Modified NYCM
disease in humans.
● Vaccines are currently available against four COLONIES
of the five strains, and a vaccine against the ● Small
B strain is in development. ● Round
● Menactra, Menomune of Sanofi-Aventis, ● Translucent
Mencevax of GlaxoSmithKline and ● Convex/slightly umbonate
NmVac4-A/C/Y/W-135 (has not been ● Granular surface, lobulated margins
licensed in the US) of JN-International
Medical Corporation are the commonly
used vaccines.
● Vaccines offer significant protection from
three to five years (plain polysaccharide
vaccine Menomune, Mencevax and
NmVac-4) to more than eight years
(conjugate vaccine Menactra)
NEISSERIA GONORRHOEAE
● 1879 - Albert L.S.
Neisser
➔ First described in
gonorrhoeal pus.
● 1885 - Bumm
➔ Cultured & proved it’s
pathogenicity
● 1960 - Douglas Kellogg
➔ Discovered phase
variation in gonococci.
● Fred Sparling
➔ Showed that small colony gonococci
were piliate and virulent large colony
gonococci were non piliated and BIOCHEMICAL FEATURES
avirulent. ● Utilize only glucose
● Catalase positive
MORPHOLOGY ● Oxidase positive
● Gram negative ● Superoxol test positive
● Diplococcus Adjacent sides concave
● Kidney shaped RESISTANCE
● Exclusively intracellular Pili-adhesion to ● Delicate
mucosal surface ● Killed: heat, drying, antiseptics.
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 17
● Dies: 1-2 hours outside the body in
Designation Location Contribution
exudates.
● Culture dies: 3-4 days.
PilE Major fimbrial Initial binding to
● Survives: slant culture - 35 ̊c-sterile paraffin
protein epithelial cells
wax.
● Stored: (-70 ̊c) for years
P.II (Opa) Outer Contributes to
membrane invasion
ANTIBIOTIC RESISTANCE
protein
● Chromosomally resistant N. gonorrhoeae
(CMRNG)
P.I (Por) Outer May prevent
● PPNG (Penicillinase producing N.
membrane phagolysosome
gonorrhoeae)
porin formation in
➔ Mainly 3.2MDa and 4.4MDa plasmids
neutrophils
(TEM-1 β lactamase).
and/or reduce
● Tetracycline resistant N. gonorrhoeae
oxidative burst
(TTNG): 25.2MDa plasmid- tetM gene.
LOS Outer Elicits
ANTIGENIC PROPERTIES
membrane inflammatory
● Pili
lipooligosacch response,
● Hair-like structure
aride triggers release
● Composed of repeating peptides subunits
of TNF
(pilins)
➔ Pilins contain 159 amino acids. P.III (Rmp) Outer Elicits formation
● Cyanogen bromide digestion has recognized membrane of ineffective
3 regions. Region 2 is receptor binding protein antibodies that
region and 3 is type specific region. block bactericidal
antibodies
against P.I and
LOS
Tbp1 and Outer Iron acquisition
Tbp2 membrane for growth
receptors for
transferrin
Lbp Outer Iron acquisition
membrane for growth
● P1: Principal outer membrane protein. receptor for
● P2: OPA lactoferrin
● P3: Binds with P1 to form porin channels
● LOS: Damage to cilia sloughing of epithelial
cells.
NOTE: Responsible for the dead cells and for the
pus when infected with the bacteria.
● Lacks somatic O antigen. Sialation protects
from antibody mediated defense processes.
● Peptidoglycan: C6 hydroxyl group is o-
acetylated. Induces fever, ciliary damage,
epithelial damage, arthritogenic and
activates complement. Also prevents lytic
action of lysozymes.
● IgAse: Cleaves Fc portion of sIgA.
● Alpha protein or factor.
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 18
IN WOMEN
Note: First, there is sexual contact then the bacteria ● Urethra & cervix
will enter, it will attach to the microvilli of our mucus ➔ Affected
membrane cells (anal, vaginal, pharyngeal). It will ● Vaginal mucosa
then be endocytosed, it will either multiply inside the ➔ Not affected
host cell or it will penetrate the basement membrane ➔ Stratified squamous epithelium
and spread. It will still survive even inside the ◆ If destroyed, it can be changed to a
neutrophils and macrophages. It can go out the new set of cells.
PMNs together with the pus. ➔ Acidic pH
● Vulvo-vaginitis
➔ Prepubertal girls
● Urethra, cervix, bartholin’s glands, F.T
● P.I.D & Salpingitis-sterility
● Peritonitis
● Perihepatic inflammation (Fitz-Hugh-Curtis
Syndrome)
Note: After incubation period it will now cause
symptoms.
IN MAN
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 19
IN BOTH THE SEXES
● Proctitis
● Conjunctivitis
● Arthritis
● Ulcerative endocarditis
● Rarely meningitis
● Pyemia
● Non-Venereal-Gonococcal Ophthalmia
○ Occurs during normal vaginal
delivery, when it will pass in the LABORATORY DIAGNOSIS
vaginal wall containing bacteria, it SAMPLES TO BE COLLECTED
can affect the eyes. Sometimes ● MEN:
babies are given prophylaxis to the ➔ Urethral discharge(acute cases),
eyes. ‘morning drop’ of secretion in chronic
● Gonococcal bacteremia cases.
● Hemorrhagic papules - hands,forearm; ➔ Exudate may be obtained after prostatic
arthritis - knee,ankles massage.
➔ Centrifuged deposits of urine may be
used.
● WOMEN:
➔ Urethral discharge, cervical swabs.
Although repeated sampling of multiple
sites is ideal, a single well taken
endocervical swab will detect
ANORECTAL GONORRHOEA approximately 90% of gonococcal
● Anorectal pain/pruritus infections in women.
● Tenesmus ➔ High vaginal swabs not to be collected
● Purulent rectal discharge (1 in 3 infected women likely to be
● Rectal bleeding missed).
● Pharyngeal Gonorrhoea ● Other samples include rectal swabs, throat
● Ocular Gonorrhea swabs, blood, swabs from skin lesions, pus
○ Can also be transmitted if you aspirated from joints, conjunctival swab in
haven’t disinfected your hand when neonatal ophthalmia.
handling a positive specimen and ● Purulent material should be collected using
you scratch your eyes. dacron or rayon swabs because calcium
● Autoinoculation from infected site alginate and cotton swabs may contain
materials toxic for Gonococci.
EPIDEMIOLOGY ● Microscopy:
● Source: human carrier ➔ Gram stained smear reveals Gram
● Mode of infection: venereal negative kidney shaped diplococci.
○ Venereal-meaning through sexual ➔ If mostly intracellular then positive, if
contact extracellular then equivocal and if not
● Non-venereal: Ophthalmia Neonatorum found then negative
● 1% Silver nitrate - CREDE’S METHOD ◆ If extracellular, investigate further
● 1970 Global incidence: 16million ● CULTURE:
● Higher in B-blood group people. ➔ Direct plating of the sample followed by
● Most common in the age group of 15-29 immediate incubation at 36-37C in a
years. moist atmosphere containing 5-10%
● Risk factors include unprotected intercourse CO2.
and multiple sexual partners. ● If direct plating and immediate incubation is
● Proctitis , throat infections , arthritis and impracticable several transport and culture
disseminated infections can also be seen. systems are available.
● Amies transport media and Stuart’s media.
● Biochemical tests
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 20
● Serology ● Some strains grow on selective media for
● Molecular methods pathogenic Neisseriae.
● Colonies on Blood agar or Chocolate agar
TREATMENT AND PROPHYLAXIS are 1-2 mm in size, non-haemolytic,
● Ceftriaxone + doxycycline or tetracycline friable, white or grayish, convex with an
or azithromycin. entire margin later becoming irregular. After
○ Either of the 3 drugs 48 hours colonies are larger, more elevated
● If penicillin sensitive (NON PPNG) then with a raised opaque center.
amoxicillin + probenecid and doxycycline. ● Oxidase positive
● No effective vaccine. ● Catalase positive
● Health education, contact tracing, ● Do not utilize carbohydrates.
monogamy and use of condoms are the only ● Reduce nitrates to nitrites.
preventive measures. ● Produce DNase.
● More resistant than meningococcus and
OTHER NEISSERIA SPECIES gonococcus.
● N. elongata ssp. nitroreducens ● Cultures may remain viable for several
● N. weaveri ssp nov months at 20C if prevented from drying.
● N.gonorrhoeae ssp kochii May survive in sputum for 3-4 weeks.
● N. flavescens ○ Culture is easy to store
● N.mucosa ● Susceptible to a wide range of antibiotics but
Note: many strains produce β-lactamase and are
● The following are considered as resistant to penicillin and ampicillin.
commensals ● It is found in the respiratory tracts of
MORAXELLA 1.5-5.4% of healthy young and middle-aged
● Moraxella species were formerly called adults, 26.5% of healthy elderly people and
Neisseria and later Branhamella species 50.8% of healthy children.
● Separated from Neisseriae based on DNA ● It is therefore recognized as a significant
base composition, fatty acid composition potential pathogen of the respiratory
and inability to produce acid from tract, including the sinuses, bronchi and
carbohydrates. larynx.
● Moraxellas may be involved in opportunistic ● 20% of the cases of sinusitis are due to M.
infections in compromised patients. catarrhalis.
● These occur as components of the normal ● Chronic bronchitis among smokers is often
flora of the upper respiratory tract, the caused by M. catarrhalis.
conjunctiva, the skin and genital tract. ● Although laryngitis is often caused by this
organism, about 90% of cases are due to
MORAXELLA CATARRHALIS viruses.
● Oval Gram negative cocci about 0.8 μm in Note:
size ● The only specie that is pathogenic to man
● May occur singly, but majority of these are
diplococci with adjacent sides flattened. LABORATORY DIAGNOSIS
● Sometimes these may occur in groups of 4.- ● Specimens collected are sputum and
tetrads transtracheal aspirates.
● May be found within polymorphonuclear ● Microscopy
leukocytes. ● Culture (some strains on selective media
○ Can be intracellular used for pathogenic Neisseriae).]
● Aerobes ● Oxidase test, RCUT test, test for
● Non-sporing, non-capsulated, and β-lactamase production.
non-motile.
● Optimum temperature is 36C but many OTHER MORAXELLA SPECIES
strains may grow at 22C . ● Moraxella lacunata
● CO2 is not an absolute requirement. ➔ Causes purulent conjunctivitis (angular
○ Difference between Neisseria and blepharoconjunctivitis)
Moraxella ● Moraxella lacunata and M. atlantae require
● Most strains grow on Nutrient agar. serum for growth
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 21
● Loeffler's medium supports the growth of
M. lacunata and M. liquifaciens
● Moraxella lacunata produces gelatinase.
OLIGELLA
● Recently delineated from Moraxella on the
basis of DNA:Rrna hybridization and
serological tests.
● O. urethralis is a rare cause of septic
arthritis.
● Can be misidentified as N. gonorrhoeae
as it is non-motile, Gram negative
diplococcus, both oxidase and catalase
positive which will grow on Thayer-Martin
medium. However, Oligella will grow on
MacConkey's agar,
Note:
● Oligella can grow to MacConkey agar, while
Neisseria can not
END OF TRANS
MICROBIOLOGY: BACTERIOLOGY | MLS 24 / MT 12 ASSESSMENT | DINO | PAGE 22
You might also like
- ClassificationDocument83 pagesClassificationDisha SharmaNo ratings yet
- Endocrine Glands PDFDocument99 pagesEndocrine Glands PDFXochitl ZambranoNo ratings yet
- Improving Interpersonal Communication Between Healthcare Providers and Clients Reference ManualDocument43 pagesImproving Interpersonal Communication Between Healthcare Providers and Clients Reference ManualSalwani SobriNo ratings yet
- Micro Microbial Mechanisms of Pathogenicity NOTESDocument6 pagesMicro Microbial Mechanisms of Pathogenicity NOTESAriane NobleNo ratings yet
- William Boericke - Pocket Manual of Homeopathic Materia MedicaDocument702 pagesWilliam Boericke - Pocket Manual of Homeopathic Materia Medicaadityaupasani100% (4)
- Blueprints in Cardiology - USMLE PDFDocument269 pagesBlueprints in Cardiology - USMLE PDFLazar VelickiNo ratings yet
- (PEDIA) 2.04 Pediatric Neurologic Exam - Dr. Rivera PDFDocument15 pages(PEDIA) 2.04 Pediatric Neurologic Exam - Dr. Rivera PDFJudith Dianne IgnacioNo ratings yet
- Gram Positive Cocci TransDocument5 pagesGram Positive Cocci Transkerynne dyNo ratings yet
- Mtap - BacteriologyDocument11 pagesMtap - BacteriologyMoira Pauline LibroraniaNo ratings yet
- MTAP BACTE MIDTERMS MergedDocument26 pagesMTAP BACTE MIDTERMS MergedLea Juan100% (1)
- Mtap2 Bacte 1Document27 pagesMtap2 Bacte 1DENISE MARA�ANo ratings yet
- (Microbio) Staphyloccocus and Streptococcus-Dr. Salandanan (BHND)Document16 pages(Microbio) Staphyloccocus and Streptococcus-Dr. Salandanan (BHND)Lee Delos Santos100% (1)
- EDITED ENDO50items 1Document12 pagesEDITED ENDO50items 1Darren Vargas100% (1)
- StaphylococciDocument7 pagesStaphylococciAlexander PanodNo ratings yet
- StaphylococcusDocument4 pagesStaphylococcusipad backupNo ratings yet
- Is Lec PrefinalsDocument57 pagesIs Lec Prefinalskent de guzmanNo ratings yet
- Chapter 7 CATALASE POSITIVE GRAM POSITIVE COCCIDocument12 pagesChapter 7 CATALASE POSITIVE GRAM POSITIVE COCCIDianne Xia Andreen LedesmaNo ratings yet
- Questions To ReviewDocument3 pagesQuestions To ReviewReign ChristyneNo ratings yet
- Chapter 14Document8 pagesChapter 14SamanthaNo ratings yet
- Streptococcus-Midterm - 2ND SemDocument6 pagesStreptococcus-Midterm - 2ND Semrhenzyl ganoNo ratings yet
- 2) BacteriologyDocument94 pages2) BacteriologyMadhulikaNo ratings yet
- 7 Family Micrococcaceae PDFDocument5 pages7 Family Micrococcaceae PDFAnne MorenoNo ratings yet
- Family Micrococcaceae PDFDocument73 pagesFamily Micrococcaceae PDFJean Tsuna KalawNo ratings yet
- SCTL Anti MicrobeDocument45 pagesSCTL Anti Microbenur qistina humaira zulkarshamsiNo ratings yet
- Chapter 15: Streptococci, Enterococcus, and Other Catalase-Negative, Gram-Positive CocciDocument9 pagesChapter 15: Streptococci, Enterococcus, and Other Catalase-Negative, Gram-Positive CocciJezzah Mae CañeteNo ratings yet
- PRELIMSby MRDHDocument23 pagesPRELIMSby MRDHPatchNo ratings yet
- Lecture 4 - SCI 8007SEF Medical Microbiology & Virology-Introduction To Medical Microbiology I - 24 Sep 2023Document62 pagesLecture 4 - SCI 8007SEF Medical Microbiology & Virology-Introduction To Medical Microbiology I - 24 Sep 2023Ada ChanNo ratings yet
- MP Week 2 Part 2 NotesDocument5 pagesMP Week 2 Part 2 NotesDara BilocuraNo ratings yet
- MT 6314 - Lesson 12 - Introduction To Antimicrobials Beta Lactam and Other Cell Wall InhibitorsDocument12 pagesMT 6314 - Lesson 12 - Introduction To Antimicrobials Beta Lactam and Other Cell Wall InhibitorsCARL ANGELA SISONNo ratings yet
- Reviewer - Bacteriology FINALS - ANGELES, ANGELICDocument38 pagesReviewer - Bacteriology FINALS - ANGELES, ANGELICAngelic AngelesNo ratings yet
- Gram Positive CocciDocument140 pagesGram Positive CocciBles Cy LagrimasNo ratings yet
- Microbiology - FA (2017)Document83 pagesMicrobiology - FA (2017)asdasdasdasdasdNo ratings yet
- para Lec - Flagellates-Giardia LambliaDocument2 pagespara Lec - Flagellates-Giardia Lambliafoxgod183No ratings yet
- Formulation and Evaluation of Fast Dissolving Oral Films of Cetirizine HydrochlorideDocument25 pagesFormulation and Evaluation of Fast Dissolving Oral Films of Cetirizine HydrochlorideGaurav AdhikariNo ratings yet
- C16-Aerobic Gram BacilliDocument9 pagesC16-Aerobic Gram BacilliJezzah Mae CañeteNo ratings yet
- Micro TestDocument8 pagesMicro TestMark Frederick100% (1)
- Cutaneous Bacterial Infections 3549Document17 pagesCutaneous Bacterial Infections 3549MasithaNo ratings yet
- Gram-Positive BacteriaDocument54 pagesGram-Positive BacteriaNurul AnisshaNo ratings yet
- W8 - Normal Human Microbiota and Nosocomial InfectionDocument3 pagesW8 - Normal Human Microbiota and Nosocomial InfectionZelle Da ReyesNo ratings yet
- Micro GramNegCocci MD2021Document5 pagesMicro GramNegCocci MD2021Patricia Mae de JesusNo ratings yet
- Staphylococcus Aureus: Presented byDocument29 pagesStaphylococcus Aureus: Presented byAyesha ArshadNo ratings yet
- Paralec M1Document8 pagesParalec M1VE NI CENo ratings yet
- MC3 NotesDocument23 pagesMC3 NotesJustineNo ratings yet
- Staphylococc I: Ni Nyoman Desi Bintari, S.Si.,M.SiDocument36 pagesStaphylococc I: Ni Nyoman Desi Bintari, S.Si.,M.SiDesi BintariNo ratings yet
- Bacte Midterm Di TaposDocument9 pagesBacte Midterm Di TaposAL-HUSSEIN NAWABNo ratings yet
- 1) StaphylococciDocument13 pages1) StaphylococciOmar K. FahmyNo ratings yet
- Lecture 5 MicrobiologyDocument89 pagesLecture 5 Microbiologyjessenia.tutor2010No ratings yet
- L1 - StaphylococciDocument35 pagesL1 - Staphylococciyouservezeropurpose113No ratings yet
- USMLE Step 1 First Aid 2020 30th - MICROBIOLOGYDocument82 pagesUSMLE Step 1 First Aid 2020 30th - MICROBIOLOGYArt PuffNo ratings yet
- Staphylococcus and MicrococcusDocument4 pagesStaphylococcus and MicrococcusAive BelistaNo ratings yet
- Bacte Reviewer MidtermDocument30 pagesBacte Reviewer MidtermShiella Mae SalamanesNo ratings yet
- Staphylococci: MaheshyadavDocument36 pagesStaphylococci: MaheshyadavMuhammad IlhamNo ratings yet
- Cocci DONEDocument11 pagesCocci DONEJo Marchianne PigarNo ratings yet
- Gram Positve Cocci: Module No.11Document6 pagesGram Positve Cocci: Module No.11Francis ValdezNo ratings yet
- Week-6.1 GramPositiveCocci 1stpartDocument6 pagesWeek-6.1 GramPositiveCocci 1stpartRegine Delos SantosNo ratings yet
- (DR - Fritz) Tetanus - Animal BiteDocument46 pages(DR - Fritz) Tetanus - Animal BiteAfiq IzzuddinNo ratings yet
- ECHINOCOCCUSDocument5 pagesECHINOCOCCUSGhina RizwanNo ratings yet
- Tubular Diseases: Immune-Mediated Toxic SubstancesDocument4 pagesTubular Diseases: Immune-Mediated Toxic SubstancesMoira Pauline LibroraniaNo ratings yet
- Cell Adaptation - DefenceDocument8 pagesCell Adaptation - DefenceClaraNo ratings yet
- Microbiology Casi Lec 2Document3 pagesMicrobiology Casi Lec 2Stevens MacabidangNo ratings yet
- DM Lec 28-10Document46 pagesDM Lec 28-10s.zainabtanweerNo ratings yet
- MICROCOCCEAEDocument28 pagesMICROCOCCEAEMarl EstradaNo ratings yet
- Acute InflammationDocument51 pagesAcute InflammationNayela AkramNo ratings yet
- Bacte Compilation PDFDocument83 pagesBacte Compilation PDFAnne MorenoNo ratings yet
- Immunology 3Document10 pagesImmunology 3Qusay QatawnehNo ratings yet
- Bacteriology (Heba)Document176 pagesBacteriology (Heba)irs531997No ratings yet
- Asthma Management and Prevention in ChildrenDocument57 pagesAsthma Management and Prevention in ChildrenSundararajaperumal AnandhakrishnanNo ratings yet
- 2001 Self-Assessment Examination For Residents (Sae-R) Multiple-Choice Questions Booklet Abridged VersionDocument23 pages2001 Self-Assessment Examination For Residents (Sae-R) Multiple-Choice Questions Booklet Abridged VersionSoumabho DasNo ratings yet
- A59. Brain Stem LESIONSDocument8 pagesA59. Brain Stem LESIONSMariana AmbossNo ratings yet
- Clinicas de Norteamerica, 2004, Vol.88, Issues 4, Type II Diabetes Mellitus PDFDocument324 pagesClinicas de Norteamerica, 2004, Vol.88, Issues 4, Type II Diabetes Mellitus PDFJesus Eduardo Cruz-BurgoinNo ratings yet
- DR Dhiman BanikCariogenic Shock Final 2022 DDDocument59 pagesDR Dhiman BanikCariogenic Shock Final 2022 DDCloudySkyNo ratings yet
- Pulmonology: Dr. Amjad K. Al-Afeef Tel: 0798843824 E-MailDocument279 pagesPulmonology: Dr. Amjad K. Al-Afeef Tel: 0798843824 E-MailZaid ZayedNo ratings yet
- KARYOTYPEDocument23 pagesKARYOTYPELucia AndreeaNo ratings yet
- Liver Function Test: Presented By: Vikas Kumar JR-1Document19 pagesLiver Function Test: Presented By: Vikas Kumar JR-1vikasNo ratings yet
- Neuroanatomy, Upper Motor Neuron LesionDocument14 pagesNeuroanatomy, Upper Motor Neuron LesionAnonymous 6MGui8dqNo ratings yet
- 05-Adrenergic Agonists DR Hala 2020Document30 pages05-Adrenergic Agonists DR Hala 2020مشاعرمبعثرةNo ratings yet
- Verruca Vulgaris of The Buccal Mucosa: A Case Report: CorrespondenceDocument3 pagesVerruca Vulgaris of The Buccal Mucosa: A Case Report: CorrespondenceChyntiananda Prabu HeningNo ratings yet
- NRCM0112 - Handout - Chronic IllnessDocument2 pagesNRCM0112 - Handout - Chronic IllnessYuuki Chitose (tai-kun)No ratings yet
- Review Article: Diagnostic Features of Common Oral Ulcerative Lesions: An Updated Decision TreeDocument15 pagesReview Article: Diagnostic Features of Common Oral Ulcerative Lesions: An Updated Decision TreemutiaNo ratings yet
- Revue Neurobehcet Lancet Neuro 2009Document13 pagesRevue Neurobehcet Lancet Neuro 2009Pompilia Lazureanu GhermanNo ratings yet
- MY MAXICARE (Brochure) PDFDocument16 pagesMY MAXICARE (Brochure) PDFFeedLab CARNo ratings yet
- AIOC Scientific ProgramDocument26 pagesAIOC Scientific Programprashant oberoiNo ratings yet
- G.R. No.146891. July 30, 2002 Ruben T. Limbo, Petitioner, V. Employees Compensation Commission and Social SecurityDocument3 pagesG.R. No.146891. July 30, 2002 Ruben T. Limbo, Petitioner, V. Employees Compensation Commission and Social Securityfritzie abellaNo ratings yet
- Drug StudyDocument9 pagesDrug Studykuro hanabusaNo ratings yet
- Hand Foot and Mouth DiseaseDocument3 pagesHand Foot and Mouth DiseaseAisah AisahNo ratings yet
- IM - Pericardial DiseaseDocument6 pagesIM - Pericardial DiseaseElisha BernabeNo ratings yet
- Normocytic Normochromic AnemiaDocument18 pagesNormocytic Normochromic AnemiaElaizha PagulayanNo ratings yet
- Cleft Lip PDFDocument47 pagesCleft Lip PDFFaisal BalochNo ratings yet
- Epistaxi S: Dr. Assaddullah Hamza Department of Ent SZMC Rahim Yar KhanDocument21 pagesEpistaxi S: Dr. Assaddullah Hamza Department of Ent SZMC Rahim Yar KhanasssadulllahNo ratings yet