Professional Documents
Culture Documents
Ncma217 Prelim Reviewer
Uploaded by
roldanmarygrace023Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ncma217 Prelim Reviewer
Uploaded by
roldanmarygrace023Copyright:
Available Formats
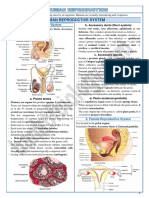
NCMA 217 PRELIM REVIEWER
REPRODUCTIVE DEVELOPMENT paramesonephric duct will turn to male or female
- discussed by Sir Francis A. Vasquez reproductive organ.
• Obstetric Nursing – came from the word
“obstetric” means “midwife”. - How? – If between 7th or 8th of pregnancy if the
• Midwife – took care of the client during the under level of testosterone being produce by primitive
prandial period, inter prandial period, post-prandial testes will became high the mesonephric duct will
period. turn into the male reproductive organs, whereas
GONADS paramesonephric duct will regress. (kase ang
paramesonephric duct will be the one to turn into the
female reproductive system)
• High testosterone level - Mesonephric duct male
reproductive organs
- Paramesonephric duct regression
• If testosterone level is not present by 10th week -
Gonadal tissues will become – ovaries – therefore,
paramesonephric duct will turn to – female
reproductive organs.
- The male & female reproductive organ - So, it is all about the testosterone but we can say
- Male gonad: Testis that this is already pre-determined.
- Female gonad: Ovaries
a) Sperm – produce by the testes carry the x and y
chromosomes
b) Ovaries – egg coming from the ovary they carry
xx chromosomes
(That determine of the gender/sex of the individual)
Testis – XY chromosome
Ovaries – XX chromosome
How does gender of individual develop?
When the woman gets pregnant of the 5th week of
intrauterine life, there is a presence of primitive
Gonadal Tissue that has two ducts:
TWO DUCTS:
1. Mesonephric Duct
2. Paramesonephric Duct
- These two ducts will be the one that will change so
that the baby will become male or female
What happened to the developing baby?
- The 7th and 8th week of pregnancy the baby/fetus
will producing or developing a primitive testis.
- Primitive Testes – capable of producing a small
amount of testosterone.
- The level of testosterone will be the one to
determine if mesonephric duct and
NERIZA BA-AR BSN 2-YA-6 1
NCMA 217 PRELIM REVIEWER
• Range: 9-17 years old
• Average:
9-12 (girls)
12-14 (boys)
• Growth spurt (A sudden increase) – is earlier in
girl and later in boys.
ROLE OF ANDROGEN HORMONE
- FEMALE: adrenal cortex and Ovaries
• Master clock is the hypothalamus
- Hypothalamus – will trigger the adrenal cortex to
start producing the hormones
- Ovaries – will produce estrogen and progesterone
REMEMBER: - MALE: Adrenal Cortex and Testis
- OVARIES – produce egg cells, Ovum produced by • Adrenal cortex – will start producing androgen and
the ovaries are carrying XX chromosomes. will stimulate the testes to produce testosterone
- TESTES – produce sperm cells. Carry X or Y (that’s why there will be an appearance of
chromosome. characteristics of male and female secondary
characteristics
• Therefore, if the xx chromosomes of the sperm TANNER’S SEXUAL DEVELOPMENT
fertilize or if the sperm that is carrying an xx - FEMALE SECONDARY SEX
chromosome fertilize the egg that always carrying the CHARACTERISTICS (IN ORDER)
xx chromosomes (pre-determined), so the paring and 1. Acceleration in linear growth (growth spurt)
the combination will be xx, therefore the gender of (Could have Broadening of the hips)
the baby will be female 2. Increase transverse diameter of the pelvis
3. Breast development (Thelarche)
• But the sperm cell carrying a y chromosome and it 4. Growth of pubic hair (Adrenarche)
fertilized the egg cell that always carrying xx 5. Onset of menstruation (Menarche)
chromosomes the combination will be xy, therefore 6. Growth of axillary hair (Adrenarche) *not
the gender baby will become boy. frequently asked so our code will be ABTAMOI
7. Ovulation
• Therefore, if the combination of the chromosomes 8. Increase in vaginal secretions
will be x and y the primitive testes is expected to
increase in production testosterone. So, the ABTAMOI
mesonephric duct will turn into male reproductive CBQ:
organ whereas, the paramesonephric duct progresses. • Thelarche
• Adrenarche
RECAP: • Menarche
- If the sperm that is carrying an xx chromosome • Ovulation
fertilize the egg that always carrying the xx
chromosomes (pre-determined). What will happen?
The level of the testosterone by the 10th week of
intrauterine life will not increase so therefore the What is the earliest sign of female secondary sex
mesonephric duct will be the one that will regress, characteristics? Increase in height or Breast
and the paramesonephric duct will develop into the development?
female reproductive organs - Increase in height (accelerated in linear growth)
PUBERTAL DEVELOPMENT
- Puberty will start at the age of 9 and end the age of Among the following which is the female
17, called pubertal period. secondary sign of sex characteristics? Adrenarche,
Thelarche, Menarche, Ovulation.
- Secondary sex changes begin: - Thelarche (breast development)
NERIZA BA-AR BSN 2-YA-6 2
NCMA 217 PRELIM REVIEWER
Which one comes out first? pubic hair or axillary - Size of penis matters in terms of survival of the
hair? sperm
- Pubic hair. Pubic hair before axillary hair. - Small penis has a compensatory mechanism which
is forceful expulsion
MALE SECONDARY SEX - Semen must reach the uterus via the cervix in 9
CHARACTERISTICS (IN ORDER) seconds and reach the fallopian tube in 5 minutes
1. Increase in weight.
2. Broadening of shoulders How will the penis erect?
3. Growth of testes. • Sexual stimulation – have blood rush, when the
4. Growth of face, axillary and pubic hair. male person sexually stimulated the penile arteries
5. Voice changes- because of androgens dilate more blood rush towards the penis and penile
6. Penile growth veins will constrict, the blood inside corpora
7. Increase in height (second to the last) spongiosum will trapped and it will absorb by it that’s
8. Spermatogenesis why the penis will erect. (pinkish color)
• If sexual stimulation subside the penile vein will
NOTE: - If a 10-year-old masturbate there is no dilate and blood goes out of corpus spongiosum so
sperm cell, seminal fluid pa lang kase ang production mawawala ang erection.
ng sperm sa male last pa nangyayari 12–14-year-old. • Parasympathetic stimulation
MALE REPRODUCTIVE ANATOMY GLANS PENIS
EXTERNAL STRUCTURES – highly sensitive area in males
- Female counterpart: Clitoris
PREPUCE (FORESKIN)
– covers the glans penis
- majority of Christian world are circumcised
- benefits of circumcision: hygiene
CORONA
– sit of sexual excitement
SCROTUM
- sperm cells are heat sensitive
- responsible for protecting the testes
- scrotal sac is 1F lower than the body temp (vice
versa)
- scrotal sac is not equally elevated (left sac is lower)
POINTS TO REMEMBER
Why is it the testes are found inside the scrotal
sac? And scrotal sac is found outside the body?
• Because there are sperms inside the testes
• Sperm cells are heat sensitive (pag masyadong
PENIS mainit
– organ of copulation/coitus namamatay sila)
- Female counterpart: Vagina
- Penis is not highly muscular but rather high in What’s temperature diff. bet. the body temp. and
ligaments (Corpora cavernosa & Corpus scrotal temp?
spongiosum) • 1 degree Fahrenheit
- covered by glands skin known as prepuce • The body temp is 1 degree Fahrenheit higher than
the scrotal temperature. (vice versa)
NERIZA BA-AR BSN 2-YA-6 3
NCMA 217 PRELIM REVIEWER
How long is the average length of the penis fully TESTES
erect? - Spermatogenesis
• Around 4 to 5 inches - Leydig’s cell nourishes the sperm with
• There is lesser than 4 in. or longer than 5 in. glucose/fructose
• Urethra – tip portion of the penis - produce male hormone testosterone
Function: dual, passageway of urine and semen - Spermatogenesis occurs specifically at
Therefore, reproduction and elimination seminiferous tubules
How long is the male urethra? VAS DEFERENS/DUCTUS DEFERENS
• 5 to 9 in an average of 7 - the site of the male surgical sterilization
• dual function (elimination and reproduction) (vasectomy- ligate ligate then cut)
• Scrotal sac – does not equally level. (isa mababa, • sperm cells after maturation will die
left side) • they provide nurishment
• made up of protein
What are the structures connected to male • Vasectomy is permanent contraception
urethra? • After vasectomy still possible to make the wife
1. Urinary bladder pregnant because may natira sa vas deferens
2. Ejaculatory duct
3. Prostate gland Nursing Teaching Plan (After vasectomize)
4. Cowper’s gland - Do not forget that after vasectomy that you need to
wear condom if you are going to engage sexual
AVERAGE SIZE/LENGTH OF FULLY ERECT intercourse for at least 2 months
PENIS: - Sperm cells that located on your vas deferens are
- 4-5 inches capable of 64 days maturing causing pregnancy
- To quickly emptying the part needed to ejaculate
MALE URETHRA LENGTH: (35 to 45 ejaculation, there is no guarantee)
- 5-9 inches (average of 7 inches) - Surest method is you need to test your sperm count
- Male urethra has dual function (for urination and - 1st result – not sure even the sperm count is zero
ejaculation) - 2nd result – still zero
- 2 consecutive zero sperm count results
- Blood rush causes the penis to erect during sexual - Vasectomy cannot stop the erection and not
stimulation preventing spermatogenesis and can still ejaculate
(but seminal fluid only no sperm)
MALE INTERNAL REPRODUCTIVE ORGANS - Vasectomy cannot protect the husband from STD
1. Testes 4 STRUCTURES PRODUCING SEMINAL
2. Epididymis – on top of testes FLUID
3. Vas difference 1. Epididymis
4. Ampulla 2. Seminal vesicle
5. Seminal vesicle 3. Prostate gland
6. Ejaculatory duct – where the ampulla and seminal 4. Cowper’s gland
vesicle meet
connected to the urethra How many percent of the seminal fluid will
7. Urethra – structure connected to this is ejaculatory epididymis produce?
duct, • Epididymis – 5%
prostate gland, & bulbourethral gland (cowper’s • Cowper’s gland – 5%
gland) • Prostate gland – 60%
8. Corpora spongiosum – came from the word sponge • Seminal vesicle – 30%
EPIDIDYMIS * Prostate gland is the main producer of seminal
– storage of testes for growth and maturation of fluid
sperms (takes 64-75 days to mature)
NERIZA BA-AR BSN 2-YA-6 4
NCMA 217 PRELIM REVIEWER
During anal intercourse why is it some males - woman can also take clomid (stimulates ovulation)
ejaculate even without masturbating?
- Because of the vibration of the prostate gland 2 TYPES OF SPERM (NORMAL)
during anal sex MORPHOLOGY
• Maturation of cells in epididymis – 64 to 70 days 1. Gynosperm – big head, small tail (contains more
(common answer 64 days more than 2 months) alkaline; acid-resistant)
• Sperm Cells travels from vas deferens to ampulla – 2. Androsperm – small head, long tail (fast moving;
because of the 5% of the seminal fluid produce by the mas madaling mamatay)
epididymis
• Sperm route: Testes (produce) → epididymis FEMALE REPRODUCTIVE EXTERNAL
(mature/storage, 5% fluid) → vas deferens STRUCTURES
(connecting struct.) → ampulla (dito naka pila mga
sperm) → seminal vesicle (already prod. 30%
seminal fluid kaya super lubricated na ung ejac. duct)
→ prostate 60% and cowpers 5% at the same time
produce total of 65% seminal fluid
• Sperm Cells are alkaline in nature because of the
fluids (able to survive the acidity of vaginal canal
bec. of alkaline)
• Vaginal canal is acidic
2 STRUCTURES THAT GIVES THE SPERM
ALKALINITY: • Mons pubis/ Mon veneris - protects the symphysis
1) Cowper’s gland pubis
2) Prostate gland • Labia Majora and labia minora
• Clitoris - sit of sexual excitement for female.
• During contraction of ejaculatory duct there is Homologous part of glans penis of the male.
forceful • Vestibule – pear/boat-shaped space. 2 obvious
ejaculation so that the sperm will not stay in the opening found in here: urethral meatus and vaginal
acidic vaginal canal. orifice (for vaginal opening)
• Sperm cells will reach the cervix in 90 seconds and
reach fallopian tube in 5 minutes • Female urethra – 2-3 inches;
• Testes- male sex gland Male- 5-9 average of 7.
• Testosterone- male sex hormones That is why female is prone to UTI. Have single
SPERM ANALYSIS RESULT function for elimination only passage of urine
- mL of semen/ejaculation: 3-5 mL • For correct catheterization we can see the clitoris
- sperm count/mL – 20-150 million
- sperm count/ejaculation: 400 million • Fourchette – where labia minora and majora meet
- Life span of sperm: 3-5 days/72 hours • Perineum- fourchette to anus
- pH: 7-8 • Paraurethral gland (skene’s) – lubricates the
- Morphology: 30% urethra
- Motility: 50% • Bartholin’s gland – lubricates the vagina
- Viability: 50%
• Down the fourchette and perineum this is the site of
Oligospermia – less than 20 million sperms episiotomy.
Aspermia – 0 sperm count • Episiotomy – the cutting of the perineum of the
woman to provide wider space to delivery and
Low sperm count – less than 20 million sperm prevent laceration.
number one cause of infertility
HAS 2 TYPES: midline and mediolateral
CLOMID – increases sperm production episiotomy.
- with doctor’s order • Mediolateral episiotomy- is better than midline.
NERIZA BA-AR BSN 2-YA-6 5
NCMA 217 PRELIM REVIEWER
• If you have laceration and there is total
communication bet. The vaginal canal and the
rectum that can lead to infection because of fecal
contamination
• When will the doctor perform the cut? During
contraction or between contraction? Is there an
anesthesia?
- No, because it has a natural anesthesia, the doctor
will cut during the peak of the uterine contraction,
because when there is strong uterine contraction
during the acme, because one contraction is
composed of three parts: relaxation, contraction,
relaxation
- There is a natural anesthesia during Acme
- Head of baby is putting pressure so nerve endings
will not be able to transmit pulses so patient is numb
A - Ovaries
B – Fallopian tube
C - Uterus
D – Vaginal canal
I-ncrement (start), A-cme (peak), D-ecrement (end)
UTERUS
• The doctor will not do the cut during the increment
and decrement. The doctor will do the cut during
acme because during this time the peak of the
uterine contraction, the head of the baby is already
pressuring the perineum of the woman. If the head of
the baby is pressuring the perinium of the woman the
nerve ending will not be able to transmit pain
SIZE:
3”x2”x1”
3 inch long
2 inch wide
1 inch thick
Weight: 50 grams
Shape: pear-shaped
Location: Suspended between urinary bladder and
rectum
INTERNAL STRUCTURES 4 POSITION:
NERIZA BA-AR BSN 2-YA-6 6
NCMA 217 PRELIM REVIEWER
3. Aids in labor and delivery
4. Organ of menstruation
3 LAYERS OF UTERUS:
1. Perimetrium- outermost layer
2. Myometrium- middle, thickest layer, source of
origin of uterine contraction; thickest layer is found
in the fundus
3. Endometrium- inner most layer and the site of
implantation.
.
UTERUS IS COMPOSED OF 4 PARTS:
1. Fundus – upper most triangular portion
2. Corpus – the working you find the uterine cavity.
Body of uterus
3. Isthmus – lower segment/part
4. Cervix (collar) – mouth/opening of uterus.
• Anteflexion - fundus of uterus is leaning sharply
forward and it is abnormal because it can compress
to much of urinary bladder and other organs in front
of it.; cystocele; protrudes to bladder wall
• Anteverted/ anteversion (non-pregnant)- normal
position, fundus of uterus is leaning forward.
- This position is also assumed in 1st trimester of
pregnancy, as the baby grows, the mother will
experience urinary frequency as the uterus is
pushing the bladder
The woman is 2 ½ mos pregnant is the uterus already
enlarging?
• Yes, and its position is anteverted and can compress
the bladder so discomfort of pregnancy experienced
by pregnant woman is urinary frequency and this will
disappear in 2nd trimester beginning 4th month
because the uterus assume the retroverted position
• Retroverted/ retroversion – normal position in
pregnant women, assumes position in 2nd trimester (4- • The thickest layer of the myometrium located in
6 months) the fundus.
• Retroflexion- protrudes to rectal wall; rectocele; - Because that is the site of uterine contraction.
can experience pain in defecation - The strongest uterine contraction.
- When the fundus contracts it gives the baby a
* Flexion - means abnormal downward push.
In the 3rd mos. of trimester, she experiences urinary - Uterine contraction in upper segment is the
frequency why? strongest because it pushes the baby out
• Because the baby is so big
• The uterine contraction in lower uterine segment
FUNCTIONS OF THE UTERUS are not that strong.
1. Site of implantation
2. Houses and nourishes the products of conception
NERIZA BA-AR BSN 2-YA-6 7
NCMA 217 PRELIM REVIEWER
- If the uterine contraction here is strong, the baby 2. Intensity
cannot go out the baby will have a hard time going 3. Duration
out. 4. Frequency
SPECIFIC SITE OF IMPLANTAION:
- Endometrium ONLY DRUGS
- The ideal site of implantation is Upper uterine OXYTOCIC DRUGS – stimulates contraction
segment – posterior. Oxytocic drug increases BP
- Posterior because uterine arteries are located at the Constricts blood vessel/vasoconstriction and
posterior. Rich in nourishment, nutrient supply may lead to water intoxication which is
and oxygen supply. harmful
- REMEMBER: The site of implantation is the site of More than 140/90 mmHg means you need
placental development to hold the drug and notify the doctor
- Not in the lower because the site of implantation is 1. Syntocinon
the site of placental development. Ibig sabihin kung 2. Pitocin
saan nag plant dun din mag grow ang placenta. 3. Oxytocin – given via IM; given 1 minute after
– If the implantation happened in lower, called baby is out; it stimulates rhythmic uterine
Placenta Previa. The placenta obstructs the birth contraction
canal and lead to bleeding 4. Methergine – not given nowadays; sustained
uterine contraction stimulates cervix to close,
o The implantation should only happen in give after the placenta is out
endometrium. Given if there is postpartum uterine atony
- It should not reach in myometrium.
- If the implantation invaded the myometrium, in the * Syntocinon and Pitocin is given via IV
future the placenta is attach up to myometrium. incorporation
- After the baby goes out, the placenta goes out next.
The placenta separate itself from endometrium.
Meaning, the placenta is superficially implanted on
the endometrium. TOCOLYTIC DRUGS – relieve contraction
- smooth muscle relaxant; also bronchodilator
- If implantation goes deeper/ invasive, the - uterus is composed of smooth muscle
placenta is attached permanently on the (myometrium)
myometrium (because during delivery the baby goes
out and after that the placenta goes out next and it 1. Duvadilan
separates itself from endometrium meaning placenta 2. Dactil OB
is superficially implanted in the endometrium but if 3. Yuotpar
the implantation goes deeper invasive implantation 4. Bricanyl (brand name)
the placenta is attached permanently and it is called 5. Terbutaline (generic name)
Placenta Accreta 6. MgSO4
- If there’s Placenta Accreta, the placenta will not
go out, because the placenta becomes part of the ABRUPTIO PLACENTA
uterus. - premature and sudden separation of placenta from
- When the baby went out, but the placenta cannot uterus
detach itself from the uterus, the women bleed to - sudden and abrupt
death. - abdomen is board-like
MANAGEMENT: removal of uterus called - use Tocolytic drug (MgSO4)
hysterectomy
If a pre-term labor is cannot be stopped, used
UTERINE CONTRACTION Oxytocic drug
- Monitored by:
1. Interval
NERIZA BA-AR BSN 2-YA-6 8
NCMA 217 PRELIM REVIEWER
- Drug contraindicated in Fetal distress Oxytocic - During delivery we measure internal os by
(because it vasoconstricts) percentage. What is the full cervical effacement?
3 STAGES OF UTERINE CONTRACTION 100%, how about dilatation? Centimeters, what is the
full dilatation? 10 cm.
- During pregnancy, the level of estrogen is high. -
When the level of estrogen is high, it makes the
cervix soft. And softening of cervix is known as
GOODELL’S SIGN
Increment
Acme Three probable signs of pregnancy can be found
Decrement in the vagina, cervix and isthmus:
Frequency Increment to Increment
Duration Increment to Decrement
Interval Decrement to Increment
1. Chadwick sign – purplish or bluish discoloration
of vaginal mucosa
2. Goodell’s sign – softening of cervix
3. Hegar’s sign – softening of cervix
- GS and HS are the same thanks to estrogen because
during pregnancy the level of estrogen increases
causes to increase vascularity (means temporary
capillaries are building up that increases fluid supply
CERVIX that’s why it becomes soft) on the isthmus and cervix.
PARTS:
How soft is non pregnant cervix?
- as soft as tip of the noses
How soft is Early pregnancy cervix?
- Earlobe
How soft is late pregnancy cervix?
- lips
Why is there a need to cervix soften?
- To be able to allow the cervix to efface and dilates.
Kailangan lumambot para numipis ang internal os at
mag open ang external os
• Internal OS – during pregnancy it effaces PAPANICOLAU SMEAR (PAP SMEAR)
(thinning); thinning is measured by percentage - Females also produce smegma in vestibule that
(100%) builds up to the vaginal canal and smegma is prone to
• Cervical canal – during pregnancy turns into cervical cancer in females during coitus
operculum (thickened) - Smegma is a combination of residual urine and
• External OS – during pregnancy it dilates sweat
(widening/opening) Location: above vaginal canal;
dilation is measured by centimeters (10 cm) When should you check for a pap smear?
AGE: 21 years old (mandatory)
Or 1 YEAR after becoming sexually active
NERIZA BA-AR BSN 2-YA-6 9
NCMA 217 PRELIM REVIEWER
• Uterosacral ligament/pelvic floor ligament –
PURPOSE: lower support
- To identify abnormal cervical cells
What ligament allows the uterus to assume the
- Doctor will smear in endocervical canal using retroverted position during pregnancy?
sterile cotton applicator • Round ligament. During 2nd trimester the round
ligament is contracting so fundus is going up
RESULTS (CLASS 5): retroverted position.
1. Absence of atypical cells • Cardinal ligament. It will not be called cardinal if
2. Presence of atypical cells but not suggestive of it is not important. Fundus and isthmus is not stable.
malignancy Middle part is usually stable and not becoming soft
3. Presence of atypical cells suggestive of so what is the ligament attached? Cardinal.
malignancy
4. Strongly suggestive of malignancy
5. Conclusive of malignancy
RESULTS (CLASS 4):
1. Absence of atypical cells
2. Presence of atypical cells but not suggestive of
malignancy
3. Presence of atypical cells suggestive of
malignancy
4. Conclusive of malignancy UTERINE BLOOD SUPPLY
PREPARATIONS:
- No sexual intercourse 3-5 days before pap smear
- No mechanical method of contraception (cervical
cap/diaphragm) wearing will result in false
positive result
- No chemical method of contraception
- No vaginal deodorant/perfume
Vaginal perfume acts as pheromones which
stimulates arousal
OPERCULUM
- Thickened cervical mucus
- When the cervical mucus thickened it acts as a seal
that protects the mother and the baby against the
ascending infection.
- Protection against microorganisms are acidity of
vaginal canal and operculum
- Dislodge during through labor (bloody show) UTERINE NERVE SUPPLY
SUPPORTING LIGAMENT STRUCTURE OF
UTERUS
• Broad Ligament – it keeps the fallopian tube and
uterus in place.
• Round ligament – upper support, pair of ligament
attached to the fundus.; assumes ante/retroverted
position
• Cardinal ligament – middle support (important, it
is vital), provides stabiltiy
NERIZA BA-AR BSN 2-YA-6 10
NCMA 217 PRELIM REVIEWER
Uterus nerves 2. Isthmus – site of tubal ligation. The doc. Will fold
a) Afferent sensory – from thoracic #11 to #12 fallopian tube.
b) Efferent motor – from t5 to t10 CBQ: - 3. Ampulla – fertilization happens and common
site of ectopic pregnancy (pregnancy outside the
Epidural Anesthesia – stops pain of uterine uterus) and meeting place/mating place, widest part.
contraction at t11 and t12 without stopping uterine 4. Infundibulum
contraction. For painless delivery.
• Because the motor nerves that will allow the motor
nerves to contract is t5 to t10, sensory from t11 to
t12.
• Kaya if woman receives epidural anesthesia the
woman will continue uterine contraction because
epidural anesthesia affects at t11 and t12 but not
affecting the nerves t5- t10 so she will continue
uterine contraction but not feeling the pain.
VAGINA - If fallopian tubes is divided into 3 equal parts (4 if
- Length – 3 to 4 inches including infundibulum) it is called:
- Rugaeted – skin folds, stretching ampulla- outer most third
- Function – organ of intercourse; passageway of isthmus- middle third
menstrual discharge; birth canal interstitial - inner most third (narrowest and goes to
- Environment - Acidic – douderlein bacillus this 3 layers of uterus)
produces lactic acid
- pH – 4 to 5 - Fimbrae- farthest part of the infundibullum, to
- During IE the fingers are inserted to vaginal canal catch the egg cell. When the follicle of the ovary
- Vagina can accommodate a bigger and longer size releases an egg cell the fimbrae catch the egg cell.
of penis, because it has rugae The egg cell will then go to ampulla to wait for the
- During sexual intercourse the cervix moves little arrival of the sperm.
upward and the rugae is stretched
FALLOPIAN TUBE * Most common site of fertilization for tubal
pregnancy: Ampulla
- Dangerous site: Interstitial
Lifespan of egg cell: 1 day (maximum of 2 days/48
hours)
- When woman is pregnant, estrogen increases but
progesterone increases more
ESTROGEN:
- enlarges uterus
- encourages contraction
- Pair of tubular organs
- Also called oviduct, because it is the passage way PROGESTERONE:
of ovum once it is fertilized - hormone of pregnancy
- Length 3-4 inches - prevents contraction
- Ciliated - provides nourishment
PARTS:
1. Interstitial – dangerous because of ectopic
pregnancy bec. it is narrowest and connected to the Braxton-Hicks contraction – contracting, painless,
uterus so bleeding is profuse irregular
NERIZA BA-AR BSN 2-YA-6 11
NCMA 217 PRELIM REVIEWER
- Once fertilization occurred, fertilized egg stays in egg cell ika-catch sya ng fimbrae → it will enter
fallopian tube for 3-4 days estrogen is increasing ampulla → there will be fertilization.
- Cilia will move inward and will take another 3-4
days of travelling to reach uterine cavity and implant - Once its fertilized the egg it stays on the fallopian
on endometrium tube for 3-4 days, during w/c the level of estrogen is
- So implantation will happen 7-10 days increasing and progesterone is increasing more
because the woman is already pregnant.
QUESTIONS:
- Site of fertilization? Fallopian tube, - When level of estrogen is increasing it encourages
specific part? Ampulla contraction in the fallopian tube nag kakaroon ng
- Functions: site of sterilization and transports ovum wave like motion.
to the uterus. - Inner portion of the fallopian tube is ciliated so as
- Pomeroy Procedure – cutting of fallopian tube the fallopian tube is contracting the cilia are moving
- Modified Pomeroy – no cutting the fallopian tube so the fertilized egg is also moving inward for
- The doctor will do the tubal lateral ligation during another 3-4 days if it moves outward, it will cause
menstruation because it is a sign that the woman is high risk of ectopic pregnancy.
not pregnant.
- After fertilization the implantation will happen 6 to
8 days or average of 7 days (1 week) and maximum
of 10 days
- 7 to 10 days implantation will occur in upper
segment in posterior uterus in the endometrium
- Pro (for) gesterone (gestation)- hormone of
preganancy, provides nourishment for the baby and
hormone that prevents contraction
- Estrogen- hormone that encourages contraction
and hormone that enlarges the uterus.
OVARIES
- Female gonad that produce estrogen and
progesterone
3 DIVISIONS:
1) Surface epithelium
2) Cortex – maturation of oocytes
3) Medulla
- During the pregnancy ovaries are not active because
- When is the best time will the woman undergo placenta will be the one will provide the estrogen
tubal ligation? and progesterone
– 1st day after the last menstrual period or during
BREAST MAMMARY GLANDS
mens. Choose the day closest to the day that the
- The breast lies in the pectoralis muscle
woman is menstruating.
- For example, the woman had sex the sperms enter
vaginal canal → uterine cavity → 2 fallopian tubes
→ tapos wala pa ung egg cell dahil hindi pa siya nag
ovulate, eh ung life span ng sperm ay 72 hrs/3 days
maximum of 5 days so tatambay muna siya sa
ampulla → nag ovulate na ung egg cell → mature
NERIZA BA-AR BSN 2-YA-6 12
NCMA 217 PRELIM REVIEWER
- Cells responsible for producing the milk are the
acini cells that is found in the lobe that contains 15-
20 each breast.
How milk ejection happens?
- When the newborn baby sucks the nipple of mother,
it sends signal to the posterior pituitary gland to
release oxytocin.
- Lobes of the breast- are connected to the
- Once oxytocin release, it will cause the
lactiferous ducts; contains 15-20 lobes each breast
contraction of milk gland cells and acini cells will
- Lactiferous sinuses/Ampulla of the breast- dulo ng
release milk.
lactiferous duct, storage room for the milk
- Then, the milk flows into lactiferous ducts, it will be
- From: Lobes → lactiferous ducts → Lactiferous
stored in the lactiferous sinus.
sinuses/Ampulla → opening of lactiferous
- Because sucking action of the baby, the milk is
expressed in the nipple.
What hormone stimulates the breast to produce milk?
- Prolactin – it produces by the pituitary gland.
- Is there any advantage when posterior pituitary
(Anterior and posterior)
gland during breast feeding releases oxytocin
– the advantage will be contraction of the uterus
- Prolactin – from anterior pituitary gland; Oxytocin
during the post-partum period. Then, the uterus
– from Posterior pituitary gland.
remains firm and contracted, it stops or prevents
- Oxytocin causes uterine contraction.
post-partum bleeding.
- Prolactin stimulates acinar cells (found inside lobes
- The normal consistency of the uterus after delivery
that can produce milk)
must be firm and contracted. Because if the uterus is
relaxing, the woman bleeds.
SELF BREAST EXAM
How will the mother breast feed the baby after
- Done 5-7 days after menstruation
delivery?
PELVIS
- Because of the action of the prolactin and oxytocin.
- Supports and protects the reproductive and other
- Prolactin stimulates the production of milk by
pelvic organ
acini cells inside the lobes
- Bony ring structure
- Milk ejection reflex or let down reflex of the milk
- Inside the pelvic cavity there is female internal
we need oxytocin, coming from the posterior
reproductive system including the part of the renal
pituitary gland.
system, the bladder, and the digestive system, the
MAMMARY GLANDS & MILK EJECTION
rectum and the anus.
REFLEX
2 DIVISIONS:
NERIZA BA-AR BSN 2-YA-6 13
NCMA 217 PRELIM REVIEWER
1. False pelvis – from symphysis pubis and up - Cannot support pregnancy and delivery
- supports the growing uterus (acts as funnel) 3 PARTS OF TRUE PELVIS
- Ilium
2. True Pelvis: from symphysis pubis and below
- serves as the birth canal
1. Inlet
2. Cavity
3. Outlet
4 TYPES OF PELVIS
- Ischial tuberosity- called sitting bones, the ones
carrying our body weight when we are sitting
- Ischial spine/ sipit-sipitan- katapat ng coccyx;
where station zero is located
1. GYNECOID
- True female pelvis because this is the most Anterior Posterior Lateral
rounded type of pelvis. Inlet Superior Sacral Ilium
- It can easily support pregnancy and delivery. Pubis prominence
- Rounded Cavity - - -
2. ANTHROPOID
Outlet Inferior Coccyx Ischial
- Can also support pregnancy and delivery.
pubis spines
3. ANDROID
- Male pelvis
– heart or triangular shape - If you get the distance from superior pubis to
sacral prominence it is anterior-posterior diameter
4. PLATYPELLOID of the inlet
- The anterior and posterior diameter is short.
- Flat pelvis
NERIZA BA-AR BSN 2-YA-6 14
NCMA 217 PRELIM REVIEWER
- If you get the distance from inferior pubis to
coccyx it is anterior-posterior diameter of the • Ischial spines – landmark for the station zero.
outlet (Station zero is landmark of engagement – means
the head is already between the ischial spines naka
- If you get the distance between the 2 iliums, then sipit ang head kaya tinawag na sipit-sipitan)
transverse diameter
• If the fetus still inside of the uterus of mother, there
- If you get the measurement between the 2 ischial is amniotic fluid. The fetus bouncing in the amniotic
spines then, transverse diameter of outlet and inlet fluid.
kase may diameters ang pelvis
• Ballottement – the bouncing of the baby in the
DIAMETER OF PELVIS amniotic fluid.
Anterior- Transverse Oblique
Posterior
Inlet 11 cm 13 cm 12 cm
Cavity 12 cm 12 cm 12 cm
Outlet 13 cm 11 cm 12 cm
- All oblique and cavity are 12 cm
- Inlet- transverse is bigger and AP dia. is smaller
- Outlet- transverse is smaller and AP dia. is bigger
THE 6 MECHANISM OF LABOR & DELIVERY
The baby needs to rotate while passing the birth
canal. – 6 mechanism labor.
D-FIRE-ER-E
1) Decent
2) Flexion • Engagement is when the head of the baby reaches
3) Internal Rotation at least minimum of station zero or if the head of
4) Extension the baby is already reaching the two ischial spine.
5) External Rotation • Station zero- is the level of the ischial spine
6) Expulsion • Above station zero is negative 1, negative 2 etc.
NERIZA BA-AR BSN 2-YA-6 15
NCMA 217 PRELIM REVIEWER
• Below station zero is positive 1, positive 2 etc.
• 1 station = 1 cm.
EXAMPLE:
1. The head is located at the negative 2 station, so
the baby is located 2 cm above ischial spine.
2. If the head is located at the positive 3 station the
baby is located 3 cm below ischial spine.
3. The head is located 2 cm above the ischial spine, FETAL SKULL
is the head already engage? Not yet but there is 3 MAIN BONES:
ballottement since the Station zero (-) Not Engaged 1) Frontal bones
(+) Engaged, head is not yet engage the baby can 2) Parietal bones
still bounce and the baby is floating 3) Occipital bones
4. When the head is already engaged in station zero it SUTURES:
is no longer floating w/out ballottement. - Cranial joints, like space
1) Frontal suture - between 2 frontal bones
5. When the head goes down to positive 5 the head is 2) Coronal suture - between 2 parietal and 2 frontal
always engaged. 3) Sagittal suture - between 2 parietal bones
4) Lambdoidal suture - between 2 parietal and 1
6. You performed IE upon inserting your finger you occipital
are able to feel/palpate the ischial spine, but the head
is not yet there the head is located at the negative FONTANELLES
station. 1) Anterior fontanelle – diamond space (closes
within 12-18 mos.)
7. Upon inserting your finger, you feel the head 2) Posterior fontanelle – triangular space (closes
w/out feeling/ palpating ischial spine the head is within 2-3 mos.) the one that closes first
located at the positive station
8. Upon inserting your finger, you feel the head
along the ischial spine then that is station zero.
• Crowning – when the head reaches positive 4 and
5. The head of the baby is being encircle already by
the vaginal opening
FETAL SKULL-PELVIS RELATIONSHIP
- The fetal skull is the most important part of the
fetal body during the labor and delivery because:
• The most frequent presenting part. (Because the
most common fetal presentation is cephalic
presentation)
• Largest part of the fetal body. (Since it is the
largest that’s the part of the body that can have a
problem of not passing through the birth canal kase
malaki)
ATTITUDES:
• Least compressible. (When head passed birth canal
1) Flexion
the head is compressed and that is called molding)
NERIZA BA-AR BSN 2-YA-6 16
NCMA 217 PRELIM REVIEWER
2) Extension • All babies that are in cephalic presentation will be
delivered normally? No, it depends.
4 REGIONS OF THE FETAL SKULL: • If the presenting part in the vagina is the face of the
1) Face - biggest baby, it is dangerous because as the uterus is
2) Brow/ sinciput - big contracting the uterus is pushing the baby down and
3) Vertex - small the head further extend is face that can cause
4) Occiput – smallest fracture of the cervical bone
FETAL LIE
EXAMPLE:
- If the head is:
• fully flexed the presenting part is occiput
• Partially flexed the presenting part is vertex
• Partially extended the presenting part is brow
• Fully extended the presenting part is face
Occiput and vertex - 2 ideal presenting part, kase
maliit sila
• Longitudinal lie - if the axis of uterus and baby is
parallel to each other.
Two types: Cephalic and breech
• Transverse lie
• In actual area presentation is the commonly used
term because it is direct.
MENSTRUATION
- periodic, cyclic discharge of blood from the uterus
- Uterus – organ of menstruation
- blood loss 30-80 cc (average of 60 cc)
- 60 cc ¼ cup
- iron loss 12-29 mg
- If the woman is heavily having menstrual period,
pwede siya mamutla/ pallor.
FETAL PRESENTATION
MENSTRUAL PERIOD VS. MENSTRUAL
CYCLE
MENSTRUAL PERIOD:
- are the days that the woman is menstruating
- Average length of menstrual period: 3-5 days,
maximum of 7 days
MENSTRUAL CYCLE:
- Average of 28 days per cycle
- ranges from 23-35 days; maximum of 40 days
- starts from the first day of period to the next period
1) Cephalic – headfirst of regla (period to period)
2) Breech – buttocks first - occurs during puberty; 9-17 years old, average of
3) Transverse- shoulder first 12 years old
NERIZA BA-AR BSN 2-YA-6 17
NCMA 217 PRELIM REVIEWER
- First onset of menstrual cycle is called menarche - or add 14 days from beginning of the cycle ONLY if
* Menarche is not the first sign of female secondary the cycle is 28 DAYS, it its not, then this method can
sex development, its thelarche (breast development) no longer be used if the person is irregular
1) Growth spurt
2) Broadening of Hips - Ovulation starts 2 weeks before the menstruation
3) Thelarche (kasi if after the mens, nagvavariable ang days)
4) Andrenarche - The first half of cycle is where the days are variable
5) Menarche - 2nd half is 14 days fixed
6) Ovulation
7) Increased vaginal secretions - To know if the cycle of woman is regular or
irregular. The length of cycle is constant for 6
- Menstrual cycle can be regular or irregular months of 28 days
- Irregular cycle cannot use calendar method as a
method of contraception because day of ovulation is
changing every month (we will have to deduct
longest cycle to shortest cycle and that’s how we will
get ovulation days)
FERTILE WINDOW
• Ovulation - the day that the one of the 2 ovaries of - These are the days the woman is considered fertile.
the woman is releasing a mature egg cell. - If you want to get pregnant have sex during the
• The woman is fertile when the one of her 2 ovaries fertile window.
is releasing egg cell. - If you don’t want to get pregnant have sex outside
• If the woman is fertile and she had sex there is a the window
possibility that the egg will be fertilized by the sperm - Subtract 5 days from the day of ovulation (5 days
and get pregnant. is the lifespan of sperm)
- Add 3 days from the day of ovulation (3 days –
• How are we going to compute for the day of lifespan of an egg cell, it is actually 1-2 days but they
ovulation? - From the end of the cycle, minus 14. make it 3 days)
- 28 – 14 = 14
- minus 14 is a constant value as this is the lifespan
of the corpus luteum
- she will be ovulating on day 14. - This is only done
by regular 5 days lifespan of sperm cell
• Hormone estrogen is high on the first half of the 3 days lifespan of egg cell
cycle.
• Hormone progesterone is high on the second half Example: 5 days of menstruation
of the cycle. - Days 1-5 = menstrual period is safe
• The length of the cycle affects the day of the cycle? - Deduct 5 days from the day of ovulation 14-5 = 9
Yes - Add 3 days from the day of ovulation 14+3 =17
• The day of ovulation is based on the length of the - Day 9-17 fertile window, the woman is considered
cycle fertile
• If the length of the cycle is changing every month, - The woman is considered safe to have sex if she
then the day of your ovulation every month is also doesn’t want to get pregnant beyond the window so
changing, then you are not regular. less than 9 and above 17
- Specifically, the woman is safe to have sex from
- For the nurse to accurately determine the day of day 1 to day 8 but days 1 to 5 have menstrual period.
ovulation, she must deduct 2 weeks from end of Therefore, day 6- 8 and during menstrual period is
cycle (best answer) safe.
NERIZA BA-AR BSN 2-YA-6 18
NCMA 217 PRELIM REVIEWER
- Day 18 – 28 is also safe 4) If you don’t want to get pregnant have sex more
- Day 9 – 17 fertile days, not safe than 5 days before ovulation: day 8 paatras.
RECAP:
5 days explanation:
28 Days Cycle Legend:
• Red - menstruation (safe) - It is considered safe to have sex during menstrual
• Green – safe days period but not all menstrual period are safe
• Orange - fertile window (not safe) depending if you are regular or irregular
• Violet- ovulation day - The shorter the menstrual cycle (shorter than 28
• Blue- sex days days), mas di nagiging safe
1) If the woman is a 28-day cycle, she will ovulate - So having sex during period is not always safe
on day 14, granted that the menstrual period of the - It is possible to ovulate while menstruating or pasok
woman is 1-5 days. sa fertile window
2) From the day of ovulation minus 5 (14-5 =9) &
from the day of ovulation plus 3 (14+3 =17) so days 21 DAY CYCLE
9-17 she is fertile. Menstruation ----- Ovulation ------- Menstruation
1-5 7 21
3) Therefore days 1-8 she is safe but if she wants to -5 +3
engage in sex beyond menstrual period, she is safe 1 day safe FW: 2-10 days 11-21 = safe
from days 6-8 and from day 18-28.
- Q: Is she ovulating at day 9? A: No, because day 14
is the ovulation day
1) Day 9 is 5 days before ovulation, means that if you
have sex on day 9 sperm enters the vagina → Another Example: 4 days of menstruation
cervix (w/in 90 sec) → uterine cavity → fallopian - Fertile window: 19-27
tube (reached w/in 5 min) and; - Safe days: 1-18 and 28-38
- Ovulation day: 24
2) Starting from day 9 the sperm is waiting in the
ampulla of the fallopian tube for the arrival of the 38 Days Cycle Legend:
egg for 5 days (kase diba ang life span ng sperm is 3- • Red - menstruation (safe)
5 days so 5 days siyang mag hihintay sa ampulla) and • Green – safe days
the egg will arrive on the 5th day at exactly day 14 • Orange - fertile window (not safe)
(ovulation day) in the ampulla of the fallopian tube • Violet- ovulation day
therefore she will get pregnant even if the sex was 5
days ago. • For irregular there is computation but it is not
highly recommended because from the very
3) Note the sperm lives for 3-5 days that is why you beginning the woman is irregular.
have to subtract 5 and add 3 is derived from the life
span of the ovum/egg cell. It is only 1-2 days or • To know if you are regular or not you have to:
actually average of 24 hrs or 1 day, maximum of - Monitor your menstrual cycle for at least 6 mos.
48 hrs. or 2 days. Plus 3 kase they added 1 day. - For regulars your menstrual cycle should be fixed to
specific no. of days.
NERIZA BA-AR BSN 2-YA-6 19
NCMA 217 PRELIM REVIEWER
- Producing:
• Ex. Your cycle is 30-day cycle so dapat every - GnRH or Gonadotropic Releasing Hormone
following month 30 days pa din siya.
- Although naiba nung April ng 28 hindi pa din siya 2 TYPES OF GNRH:
considered as irregular, ask ur self if you are stressed 1) FSHRF or Follicle Stimulating Hormone
that time because it can alter mens. cycle. Releasing Factor
2) LHRF or Luteinizing Hormone Releasing Factor
2. Anterior pituitary gland
- Producing:
- FSH or Follicle Stimulating Hormone
- LH or Luteinizing Hormone
• For irregular, you must also monitor your menstrual
3. Ovaries
cycle at least 6 months.
Producing:
- You have to identify the month that has longest
- Estrogen- dominant on the 1st half of cycle
cycle and the shortest cycle.
- Progesterone- dominant on the 2nd half of cycle
- You have to deduct 11 days from the longest cycle
then,
4. Uterus
- Deduct 18 days from the shortest cycle.
- We cannot identify exactly the ovulation day but we
will know the fertile window.
Example for irregular:
a) (May) Longest cycle – 38 – 11 = 27 days ↑
4 DATES IN MENSTRUAL CYCLE
Considered as the cycle because it is the longest
1. ↓ 3rd day - the level of estrogen in the blood of
b) (Aug.) Shortest cycle – 21 – 18 = 3 days
the woman is very low.
- Days 1-5, she is menstruating at the beginning
menstrual cycle.
2. ↑ 13th day - the level of estrogen in the blood of
the woman is very high
- Day 5 still menstruating and day 3 ovulation day-
they are overlapping 3. ↓ 13th day - the level of progesterone in the blood
of the woman is very low.
4. ↑ 14th day - the level of progesterone in the blood
of the woman is very high.
38 Days Cycle for Irregular Legend:
• Red - menstruation (safe)
• Green – safe days
• Orange - fertile window (not safe)
• NO ovulation day
4 IMPORTANT STRUCTURES
- In menstrual cycle, there are different glands that
control/regulate menstrual cycle
- Hypothalamus gland starts the menstrual cycle and
the hypothalamus stimulates Anterior Pituitary
Gland and APG stimulates Ovaries and ovaries
affects Uterus
1. Hypothalamus
NERIZA BA-AR BSN 2-YA-6 20
NCMA 217 PRELIM REVIEWER
How ovaries produce progesterone?
- Estro is low on 3rd day and high on 13th day so on
the 13th day the level of estro is high and pro is low.
Since the 13th day the level of estrogen is already
very high, there will be a feedback effect.
- That high level of the estrogen will send signal to
the APG to temporarily stop producing FSH.
- Effect: If the FSH stop producing, then ovary will
no longer produce estrogen. (may stock na
sya ng estrogen sa graafian follicle)
SECOND HALF OF THE CYCLE –
FIRST HALF OF THE CYCLE – ESTROGEN PROGESTERONE
1) Particularly days 1-5, on the 3rd day of 1) That’s why on the 13th day of the menstrual cycle
menstrual period the level of estrogen in the blood the level of progesterone is very low stimulating the
of the woman is already very low because she is hypothalamus to release LHRF.
menstruating.
2) LFRH stimulates the APG to release LH.
2) That low level of the estrogen of woman
stimulates the hypothalamus to start a new cycle. 3) LH stimulates the ovary to release progesterone.
Then,
3) Estrogen stimulate hypothalamus to release
FSHRF 4) Progesterone will affect the uterus.
- When the level of LH is high, LH triggers
4) FSHRF stimulates the APG to release FSH. ovulation.
- The high level of progesterone will convert graafian
5) FSH stimulates the ovary to release estrogen. follicle into corpus luteum. (Corpus luteum -
Then, yellowish)
- Progesterone will stimulate uterus, there will be
6) Estrogen will affect the uterus. increased vascularity on endometrium
- Once APG release, FSH – will develop egg cells. It - Increase vascularity – building up of temporary
will cause the maturation of oocytes (1st effect). capillary.
(Oocyte – immature egg cells) - Progesterone builds up temporary capillaries on
- (2nd effect of FSH) FSH stimulates ovaries to endometrium.
release estrogen so once estrogens is released, it - The blood supply will be high when there’s a build-
converts the follicle of the ovary into graafian up of temporary capillary.
follicle. - If the blood supply in endometrium will become
- Follicle is the compartment in the ovary where you high, it increased supply of O2, H2O, Glucose,
can find the egg cells and becomes graafian follicle. Amino Acid.
Estrogen is the hormone that is very high in the - Progesterone made the endometrium highly
graafian follicle. nourished.
- The effect of the estrogen on the uterus is
thickening of myometrium and endometrium.
- Myometrium is also thickening – the uterus will
slightly enlarge during menstrual cycle because of the PATHWAY OF WOMAN GETTING
hormone estrogen. PREGNANT
- If the woman gets pregnant the level of estrogen is
high that is why estrogen enlarges the uterus.
- Hindi sabay pinoproduce ng ovary ang estrogen and
progesterone. Isa isa lang.
- Estrogen partner niya si FSH. Progesterone is LH
NERIZA BA-AR BSN 2-YA-6 21
NCMA 217 PRELIM REVIEWER
1) Placental Aging/Degeneration Theory – the
placenta will start to degenerate as it reached 9
months and then it will cause progesterone levels to
decrease 2) Progesterone Deprivation Theory
- Therefore, the Braxton-Hicks contraction (painless
and irregular) starts to be painful and regular it
will increase uterine contractionn.
- The reason why it is minus 14 is because the - Then the woman enters the labor.
lifespan of Corpus Luteum is 14 days
- Corpus luteum came from graafian follicle, GF PATHWAY OF MENSTRUATION
produce estrogen. CL combines estrogen with
progesterone. But progesterone is higher during
pregnancy.
- 2 hormones produced by CL is estrogen and
progesterone.
- Mat. oocyctes 13th ↑ Triggers ovulation Graafian
follicle Graafian follicle Corpus luteum Thickening
of myo and endo ↑vascularity on endo Corpus luteum
(2 weeks life span)
- Estrogen is high (encourage contraction) but
progesterone is higher (prevent contraction) and we
need these 2 hormones in pregnancy. - If she did not engage in sexual intercourse, or she
engaged in sexual intercourse but protected. There is
- The reason why the woman will not menstruate no fertilization.
when she gets pregnant because lifespan of CL after - If there is no fertilization, there is no pregnancy to
fertilization, extends from 2 weeks to 2 months. support. So, CL will not extend life span from 2
Since nag extend menstruation missed. weeks to 2months. So, within 2 weeks the corpus
- On the 2nd month, corpus luteum is luteum is degenerating.
aging/degenerating. - If the corpus luteum is degenerating, the level of
estrogen and progesterone will begin to decrease.
- On the 2nd month of pregnancy, the placenta will - If the estrogen and progesterone decrease, the
develop. And the placenta produces estrogen and uterine contraction will increase.
progesterone, but the progesterone is higher than - The temporary capillaries will begin to
estrogen. rupture/slough off – giving you menstrual
discharge.
- The lifespan of placenta (inunan) is 9 months.
- When the placenta reaches the 9th month of
pregnancy, placenta is considered aging (Placental
Aging/Degeneration Theory) TO SIMPLIFY:
- Progesterone – preventing contraction then, the
ability of the placenta to produce progesterone, will
begin to decrease (Progesterone Deprivation
Theory) Mnemonic: FEG – HAOU – LPC
Legend:
* Aging will decrease progesterone level that is •Yellow – hormones
preventing contraction and that decrease of • Green – structures
progesterone has a theory called Progesterone - If hormones contain “RF” releasing factor it came
Deprivation Theory from hypothalamus, if theres no “RF” from APG
- If the questions are about structures look at the
2 theories used: middle
NERIZA BA-AR BSN 2-YA-6 22
NCMA 217 PRELIM REVIEWER
- If the question is about the hormones look at the
outside.
QUESTIONS:
1. What gland that starts menstrual cycle?
Hypothalamus
2. Hypothalamus stimulates? APG
3. APG stimulates? Ovary
4. Ovary affects? Uterus
5. Hormone high in the graafian follicle? Estrogen
6. Hormone high in the CL? Progesterone
7. What gland stimulate ovary to produce estrogen
and progesterone? APG
8. What hormone will stimulate the ovary to
produce estrogen? FSH
9. What hormone will stimulate the ovary to
produce progesterone coming from what gland? LEARNING OBJECTIVES
APG, under the regulation of hypothalamus gland After the discussion, learners should be able to:
10. What hormone will stimulate APG to produce 1. Assess the readiness for parenthood and the health
LH? LHRF coming from hypothalamus status of a pregnant woman and her family.
11. What day the level of estrogen is highest? 13th 2. Relate ovulation and ejaculation to the process of
12. What day the level of progesterone is lowest? human conception.
13th 3. Explain implantation and nourishment of the
13. What day the level of progesterone is highest? embryo before development of the placenta.
14th 4. Describe normal prenatal development from
14. What day the level of estrogen is lowest in the conception through birth.
blood of the woman? 3rd day because she is CONCEPTION
menstruating Ovum
15. What hormones trigger ovulation? LH - Female sex cell
16. Hormone that decreases GI motility - mature gamete
Progesterone - released during ovulation
17. Hormone that leads to pyrosis (heartburn) - Lifespan: 24 hours (maximum of 48 hours)
Progesterone
18. Hormone that causes epistaxis Estrogen
19. What mineral if depleted during pregnancy causes
leg cramps Calcium
Four parameters/tools to know accurately when a
woman is ovulating:
1) CYCLE REGULARITY – regular menstrual
cycle (21-35 days; maximum of 40 days; average of
28 days)
- Woman cannot use calendar method if she is
irregular
- Mitelschmerz
- Can feel slightest of pain
NERIZA BA-AR BSN 2-YA-6 23
NCMA 217 PRELIM REVIEWER
- Slight discomfort associated with the - Interstitial – most dangerous site for ectopic
stretching of follicle pregnancy
- One-sided, kung saan nagrerelease si ova
- Situated in lower abdomen • This gamete once released is ready for fertilization
- German for middle pain – it occurs already and normally occur in the ampulla of the
midway through a menstrual cycle about 14 fallopian tube, whether the ova is fertilized or not
fays before your next menstrual period tuloy pa din ang journey niya.
- Doesn’t require medical attention
• The ovum proceeds to the uterus in approximately 4
2) CHANGES IN CERVICAL MUCUS – days after it is released by the ovary.
There are changes every month. TWO IMPORTANT LAYERS OF OVA
- It starts from white, dry, pasty cervical mucus to egg 1) CORONA RADIATA - outer layer, granulosa or
white consistency and stretchy follicular cells that formed around developing oocyte
• Usually start with dry wala tayong mga secretions in the ovary and remain until ovulation.
and eventually mag kakaroon ng konti-konti until the
secretions is stretchy and clear you can actually 2) ZONA PELLUCIDA - transparent but thick,
compare to egg white. composed of glycoprotein that surround the cell
plasma membrane.
• Spinnbarkeit - 6 cm before it breaks
- Needs to be stretchy, so that it can go farther or it Other parts of ova:
can transport the sperm to ova that is targeting to
- Plasma membrane
meet. (makiki-ride sya).
- Cytoplasm
3) HORMONAL CHANGES – - Nucleus
Estrogen and progesterone.
• There is slight increase because of the presence of Kapag nag karoon ng conception in a natural
corpus luteum. interaction of many factors including the correct
timing in between the release of the mature ovum
4) BODY TEMPERATURE CHANGES during ovulation and ejaculation of enough healthy
- prior to ovulation there will be a temp. drop to a motile sperm in woman vagina.
low normal and then the following day it shoots up to
SPERM CELLS
a very high normal and this will tell us that the
Parts: Head, neck, and tail
woman is actually ovulating. Lifespan: 48-72 hours (3 days maximum of 5 days)
• We have to use basal body thermometer when we
use this technique.
• The woman should check her temperature daily
upon arising (kapag bagong gising sya)
Ovulating - 14 days before the next cycle.
• Every good fertilization, start from a good
ovulation. And every good conception, starts from the
good fertilization.
• The ovum released by the ovary is then transported - Male is the one who determine the sex of the baby.
through the tube by the muscular movement. - Ave. male produce: 525B sperm cells over a
• Cilia- used to move the ova. lifetime.
- Healthy adult men: 20M-150M with the max of
• Fallopian tube 1.2B in a single ejaculation.
- Infundibulum - Typically, volume of climax: 3-5ml/ejaculate. (3
- Ampulla – outer; meeting place; common site of quarters of the teaspoon – ¾)
ectopic pregnancy
- Isthmus – inner - If it lowers down to 1.5 ml or 1/3 teaspoon – check
for a doctor
NERIZA BA-AR BSN 2-YA-6 24
NCMA 217 PRELIM REVIEWER
- Pre ejaculation cannot be measured
- Pre ejaculation is usual among teens
TYPES:
a. Gynosperm
- large head – slow swimmer
- alkaline – low survival on vagina’s acidic environment
- carries Y chromosome – male
b. Androsperm
- small head
- acidic – can survive longer in vagina’s acidic environment
because it is already acidic
- Carries X chromosome – girl
-------
- First to reach ova doesn’t mean winning, it depends
REPRODUCTION on the penetration called capacitation
- First to release hyalase/hyaluronidase
- Intercourse more than a day after ovulation will
usually not result to fertilization
- After fertilization, we create 23 chromosomes of
ova and 23 chromosomes of sperm joined
together diploid of 46 chromosomes
- Sexual activity involves the insertion of erected
penis into the vagina, both for sexual pleasure and
reproduction purposes.
- Both of which will be culminating in an orgasm and
ejaculation.
- Irregardless of the position of the couple as long as
the penis enters the vagina during sexual intercourse.
- Ejaculation – ejecting semen into the body.
- When a couple executed sexual activity millions of
candidates sit off a long peroneus journey with a
single target is to reach the ova.
- Many sperm are loss in the vaginal introitus,
because of the ejaculation drips kase may nababawas
ng mga sperm.
NERIZA BA-AR BSN 2-YA-6 25
NCMA 217 PRELIM REVIEWER
- Survivors continue their journey to the cervix going - Cell will split to have – zygote; which happens from
to the uterus and the fallopian tube through the help day 0 to 14. Then, the cell continues to divide, 2
of the whip like movement of tails to swim upward. cells, 4 cells, 6 cells, this is what we called cleavage.
- Only the viable sperms enter the cervix. Tapos ung - By the time they reach the endometrium they
seminal fluid naiiwan na nag seseparate na sila. become morula or mulberry → hallow spear of cell
- They meet in the ampulla of the fallopian tube. blastocyst. This is the preliminary stages in the
embryo beginning form
- Remember that there is only one ova waiting to be
fertilized for every menstrual cycle. - Rapid cell division Cleavage divides into two
Monozygotic identical twins
- The first one to reach the finish line is not
guaranteed to win, the sperm has to undergo - Accidentally two ova matures and both of them has
capacitation – glycoprotein and seminal proteins that been fertilized Dizygotic fraternal twins
are being removed from the acrosome of the sperm
head. And after that, same pa rin ung itsura ng sperm. - Trophoblast – outer layer of blastocyst
Pero pag Nawala na yon, this particular sperm have a cells that formed the outer layer of blastocyst. They
better fight or possibility of getting into or are present 4 days post fertilization.
penetrating the corona radiata (also release hyalase) They provide nutrients to the embryo and develop
and zona pellucida covering the ovum. into large part of placenta. Located next to the
maternal endometrium and must exhibit invasive
- Body of sperm release Acrosin – it allows the properties that forms an effective maternal fetal
penetration of zona pellucida. vascular relationship. Nag kakaroon ng vascular
relationship yung mother and fetus and this is what
- Once the sperm is able to penetrate mag kakaroon we call chorionic villi.
na ng fertilization
- CHORIONIC VILLI – finger like projections by
- Fertilization – this is when a sperm and egg cell 10th to 11th day of pregnancy; for vascular relationship
combine. (nagsasama sila) and their nuclei is fused for fetus, will be connected to umbilical cord and this
together at this time is the beginning of pregnancy. is the passage way of nutrients from the mother
- From the start of cell division up to the time it
- Fertilization is a number game we started millions reaches endometrium and the fetus is formed, the
up to 1 sperm will survive. Usually, it takes 30 process usually takes 2-8 weeks
minutes to 2 hours and if the sperm did not encounter
an oocyte immediately, they can survive in the - kumakapit sya doon sa endometrium and has same
uterine tubes for 3-5 days. genetic material as the fetus.
- While in the blastocyst cavity there is a formation of
- Thus, fertilization can still occur if intercourse takes the fetus
place a few days before ovulation. - Early blastocyst
- Late blastocyst – buries itself in the endometrium
- Intercourse more than a day after ovulation will and eventually become fetus.
therefore not usually result in fertilization. - From the start of cell division up to the time that
- After fertilization occurs the 23 chromosomes of reaches the endometrium, and the fetus is formed, the
sperm and 23 chromosomes of ova together restoring process usually takes 2-8 weeks.
the diploid 46. - During implantation it happens approximately
around the 10th day after fertilization.
- Fertilization is complete when cell division starts
from the entry of the sperm to the ova, we call it
fertilization then;
NERIZA BA-AR BSN 2-YA-6 26
NCMA 217 PRELIM REVIEWER
- And that benefits the fetus because it increase the
availability of maternal glucose for fetal
consumption.
- It also antagonaist the cellular action of insulin
decreasing the use of insulin which predisposes
pregnant woman into developing glucose
intolerance. That can lead to gestational diabetes.
HUMAN CHORIONIC GONADOTROPIN ORAL GLUCOSE TOLERANCE TEST (OGTT)
(HCG) Oral Glucose Tolerance Test – papainumin ng liquid
- available at 8-10 days after conception. sobrang tamis.
- Primary role is to keep the corpus luteum - Ordered by the doctor between 24th- 28th weeks of
functioning so that corpus luteum continues to pregnancy.
produce estrogen and progesterone until placenta is - If levels is low, it may result to abortion or
fully developed tapos siya na ung mag poproduce ng intrauterine growth
estrogen and progesterone. DECIDUA
- This is the stage of pregnancy where the embryo - serves as maternal bed embracing the embryo
adheres to the wall of the uterus. And stages of - has 3 layers
prenatal development the conceptus is still called 1) Decidua basalis/ serotina – the area of
blastocyst. endometrium between the implanted chorionic
- It is by adhesion of the embryo in the uterus on vesicles and myometrium. Which becomes later the
the upper or lower uterine segment that embryo maternal part of placenta.
receives oxygen and nutrients from the mother in
order to be able to grow. 2) Decidua Capsularis – surrounds the chorionic
- Embryo receives oxygen and nutrients from the sack.
mother.
3) Decidua Vera – makes the operculum of the
* HCG is the earliest basis for pregnancy to be mucus plug. To prevent ascending infections.
tested on pregnancy test kit (urine) Mucus plug released once there is already bloody
- Corpus luteum deteriorates after 2 months and show. Synonymous to decidua parietalis which will
placenta will replace fused with the decidua capsularis by the 4th month
gestation.
HUMAN PLACENTAL LACTOGEN/ HUMAN
CHORIONIC SOMATOMAMMOTROPIN
(HPL)
– produced by syncytiotrophoblast.
From about when the production HCG begins nag
dediminished siya which promotes fetal growth by
stimulating amino acid uptake and DNA synthesis.
- HPL both growths promoting hormone and
lactogenic hormone.
Lacto – milk producing. It is produced by the
placenta beginning as early as 6 weeks of pregnancy.
Increases to a peak level by the time fetus reaches CHORIONIC VILLI
term. Promotes mammary gland growth in - Finger like projections develop by 10th to 11th
preparation for lactation of the mother. day of pregnancy.
– serves important role of regulating maternal - Sprout from the chorion to provide maximal contact
glucose, protein, and fat level. area with maternal blood. They are an essential
- So that adequete amount of nutrients will be given element in pregnancy from a histomorphologic
to the growing fetus; diabetogenic effect or insulin perspective, and by definition, a product of
antagonist. conception. Branches of the umbilical arteries carry
embryonic blood to the villi.
NERIZA BA-AR BSN 2-YA-6 27
NCMA 217 PRELIM REVIEWER
- Used for testing
CHORIONIC VILLI SAMPLING (CVS)
• Removal of tissue sample from the fetal portion of
the developing placenta
FAMILY PLANNING
- is the use of a range of methods of fertility
regulation in order to:
1. Avoid unwanted births/pregnancy
- Used for genetic screening as it is done earlier in 2. Bring about wanted births/pregnancy
pregnancy usually 9 – 12 weeks 3. Regulate the number of children born
- Prenatal test to detect birth defects 4. Regulate intervals between pregnancies/ birth
- During test small sample of the chorionic villi will spacing
be aspirated from the placenta where it attaches the 5. Control time at which birth occurs
wall of uterus.
- Most common complications: fetal limb defects - Recommended number of children per couple:
such as missing digits and toes. 2-3 children
- Interval between 2 pregnancies: 3-5 years
2 COMPONENTS
1. Planning pregnancy
2. Preventing pregnancy
SEXUAL REPRODUCTIVE HEALTH
- Good sexual and reproductive health is a state of
complete physical, mental and social well-being in
all matters relating to the reproductive system.
THE BLASTOCYST - It implies that people are able to have a satisfying
- Adhesion to uterus either to upper or lower uterine and safe sex life, the capability to reproduce, and
segment the freedom to decide if, when, and how often to
- Ideal: upper posterior do so. – United Nations Population Fund
- Placenta (high in progesterone; low in estrogen)
- Blastocele (embryonic disc) - To maintain one’s sexual and reproductive health,
people need access to accurate information and the
3 PRIMARY GERM LAYERS safe, effective, affordable and acceptable
1) Ectoderm – outermost layer of cell; embryo CNS contraception method of their choice.
2) Mesoderm – middle layer; majority of major - They must be informed and empowered to protect
organs themselves from sexually transmitted infections. And
3) Entoderm – inner layer when they decide to have children, women must have
access to services that can help them have a fit
pregnancy, safe delivery and healthy baby.
REPRODUCTIVE LIFE PLAN
A plan for whether, when and how to have children.
It includes personal goals, and states how to achieve
them. The plan is based on a person's priorities and
goals with regards to life and children
IF YOU DO NOT WANT TO HAVE CHILDREN,
YOU MIGHT ASK YOURSELF:
NERIZA BA-AR BSN 2-YA-6 28
NCMA 217 PRELIM REVIEWER
• How do I plan to prevent pregnancy? Am I sure that women to recover their health improves women's
I or my partner will be able to use the method chosen potential to be more productive and to realize their
without any problems? personal aspirations and allows more time to care for
• What will I do if I or my partner becomes pregnant children and spouse/husband, and;
by accident? • Informed Choice that is upholding and ensuring
• What steps can I take to be as healthy as possible? the rights of couples to determine the number and
• What medical conditions (such as diabetes, obesity, spacing of their children according to their life's
and high blood pressure) or other concerns (such as aspirations and reminding couples that planning size
smoking, drinking alcohol, and using drugs) do I of their families have a direct bearing on the quality
need to talk about with my doctor? of their children's and their own lives.
• Is it possible I could ever change my mind and want
to have children one day? NATURAL FAMILY PLANNING METHOD
- Abstinence
IF YOU DO WANT TO HAVE CHILDREN ONE - Lactational Amenorrhea Method (LAM)
DAY: - Fertility Awareness Method (FAM)
• Am I ready to have a baby? Calendar or Standard days method
• How old do I want to be when I start and when I Two days method
stop having children? Cervical mucus test/Billing’s test
• How many children do I want to have? Basal Body temp
• How many years do I want between my children? Symptothermal method
• What method do I plan to use to prevent pregnancy - Coitus interruptus not included in natural family
until I’m ready to have children? Am I sure that I or planning as it has a high failure rate according to
my partner will be able to use this method without DOH
any problems? ARTIFICIAL CONTRACEPTIONS
• What, if anything, do I want to change about my Hormonal - Oral, Injectable, Implant, Patch
health, relationships, home, school, work, finances, Chemical - Spermicide
or other parts of my life to get ready to have Mechanical - Cervical Cap, Diaphragm, IUD
children? Surgical - Bilateral Tubal Ligation and Vasectomy
• What steps can I take to be as healthy as possible,
even if I’m not ready to have children yet? PLANNING THE PREGNANCY
• What medical conditions (such as diabetes, obesity, • Proper nutrition and exercise
and high blood pressure) or other concerns (such as • Lifestyle changes:
smoking, drinking alcohol, and using drugs) do I Remember:
need to talk about with my doctor? • Smoking can cause SGA baby (Small for
Gestational Age)
FAMILY PLANNING – DOH • Alcohol can cause cognitive impaired- baby
The program is anchored on the following basic • Medical History Taking and Check up is important
principles. • Genetic counselling
• Responsible Parenthood which means that each
family has the right and duty to determine the desired PREVENTING PREGNANCY
number of children they might have and when they - Contraceptive methods are used
might have them. And beyond responsible - Always remember that there is always a possibility
parenthood is Responsible Parenting which is the for the method of contraception to fail thus
proper upbringing and education of children so that pregnancy may occur.
they grow up to be upright, productive and civic-
minded citizens.
NATURAL METHODS
• Respect for Life. The 1987 Constitution states that CONCEPT: No use of any chemical and mechanical
the government protects the sanctity of life. Abortion means of preventing pregnancy.
is NOT a FP method: 1. ABSTINENCE
• Birth Spacing refers to interval between
pregnancies (which is ideally 3 years). It enables
NERIZA BA-AR BSN 2-YA-6 29
NCMA 217 PRELIM REVIEWER
- refraining from vaginal sexual intercourse -
different from STRICT ABSTINENCE Advantages:
- acceptable, 100% effective, no cost
Disadvantages: - loss of self control- difficult to
maintain
LACTATION AMENORRHEA METHOD (LAM)
- Use of this method requires regular and fulltime 4. FAM-CMT
breast feeding (Exclusive) - aka Billing’s Test, Spinnbarkheit, Creighton’s
- Effective during the first 6 months post partum - Estrogen
- No ovulation and no menstruation - clear, elastic, watery, slippery, thin, abundant
- Not effective after 6 months If can be stretched by 5-10 cm without breaking,
- After 6 months, woman may ovulate but without woman is fertile.
menstruation (because she still continue 2-day method
breastfeeding the baby after the first 6 months) If
woman is breastfeeding the baby in the first 6 months
of post partum, the level of estrogen remains high,
thus, hypothalamus will not release FSHRF APG
will not produce FSH no egg cells will mature
thus no ovulation
So how does the woman know if she is pregnant?
- Breastmilk production is decreasing
5. FAM-BBT
- Since she still breastfeeds after 6 months, she will - Progesterone
not menstruate but ovulation occurs - sudden rise in BBT during ovulation because of
- You cannot compute for fertile window sudden rise in progesterone (3 days elevated BBT) -
- Its ok for a breastfeeding mother in first 6 months to consistency is the key (same time, same route: oral)
take pills to prevent pregnancy (POP progesterone After Ovulation – temperature slightly rises by 0.20C
pills) to 0.50C (thermal shift)
2. COITUS INTERRUPTUS
- Withdrawal of penis before ejaculation inside the
vagina
- Sperm may leak from the penis even before
ejaculation – pre-cum
- Effectiveness is only 84%
- No protection to STD/STI
- Self-control is the key
6. FAM – SYMPTOTHERMAL
- Use of BBT and CMT
3. FERTILITY AWARENESS METHOD (FAM) ARTIFICIAL METHOD (BARRIER)
- The identification of the woman’s fertile and - Refers to chemical, mechanical or the
unfertile phases during her menstrual cycle. combination of the two in preventing the sperm
- Requires cooperation between the Female And cells from entering certain points/ parts of the female
Male (FAM) reproductive canal.
Advantages: Inexpensive, no side effects, no harmful 1 SPERMICIDE
chemicals and gadgets - Provides both physical and chemical barrier
FAM CALENDAR - Ex. Nonoxyno 9 (N9)
CALENDAR METHOD: Fertile Window - kill spermatozoa before reaching
? = Regular or Irregular - cervix
? = Day of Ovulation - make vaginal pH strongly acidic
- No.1 contraindication: allergy
NERIZA BA-AR BSN 2-YA-6 30
NCMA 217 PRELIM REVIEWER
- No.1 side effect: allergy, ↑ incidence of birth defect, - makes noise
unpleasant taste - can cause vaginal or penile irritation
- inserted into the vagina 10 minutes before - it may slip during vigorous intercourse
intercourse not more than 30 minutes 4. DIAPHRAGM AND CERVICAL CAP
- wait 6-8 hours after coitus before douching
2. MALE CONDOM
– is a shallow dome-shaped latex rubber device
with flexible, circular wire rim that fits over the
cervix.
- this is only available upon prescription in wide
- Collects semen during and after intercourse range of diameters between 50 and 90 mm and
- Protects the couple from some STIs, low cost, requires fitting by a trained practitioner
- May break, cause allergy from latex, and may B. It must be inserted before intercourse and
decrease sensation during intercourse should remain for 6 hours after. A diaphragm
3. FEMALE CONDOM should not be left in place for 24 hours
– or vaginal sheath is a thin tube that is made up of
polyurethane with flexible rings at both ends
4. ORAL PILLS
Action: inhibits ovulation by suppressing FSH and
LH
Types: combined (COC; Estrogen and Progesterone)
A. it collects the sperm before, during and after and mini (POP; Progesterone) Contraindications:
intercourse like the male condom - pregnancy and lactation
- smoking - over 35 y/o
B. Advantages - hx of thromboembolic disease, DM
- erection is not necessary to keep the condom in - hypertension, cardiac disease, liver problem
place - cancer of the breast and reproductive tract
- external ring can provide extra clitoral stimulation
- available without prescription
C. Disadvantages
- difficult to apply
NERIZA BA-AR BSN 2-YA-6 31
NCMA 217 PRELIM REVIEWER
Pills – inhibits ovulation because estrogen and
progesterone levels are high
Danger signs:
A – abdominal pain
C – chest pain and dyspnea
H – headache
E – eye problems
S – severe leg pain
Danger SIGNS Side effects:
J-Jaundice (Liver problem) W – weight gain
A – abdominal pain- (liver problem) I - increased cervical discharge
C – chest pain and dyspnea (heart problem) S – spotting
H – headache (severe)- HPN H – headache
E – eye problems - HPN
S – severe leg pain – (Thromboembolic disease) Rule before taking CP:
PPP PE, Pelvic exam and Pap smear
DMPA
DMPA – Depot medroxy progesterone acetate
(150mg) - Depo provera
ACTION – INHIBITS OVULATION; THICKENS
CERVICAL MUCUS
Duration of Protection: 3 mos
Rule: Do not massage injection site.
EFFECT: NO MENSTRUATION
FERTILE WINDOW LUNELLE: with menstruation
Let’s relate menstrual cycle to contraception
MENSTRUATION:
HORMONAL IMPLANTS
– a small, flexible, plastic rod about the size of the
matchstick and is inserted under the skin under
local anesthesia.
CONTRACEPTIVE PILLS - insertion takes approximately 4 minutes
Effect: Suppressing ovulation A. Advantages:
Action: by keeping the levels of estrogen and - extremely effective birth control
progesterone in the blood of the woman high - no daily pills to remember and no interference to
Will the woman still menstruate? Yes sexual activity
When: Ater the 21st pill
B. Disadvantages:
Estrogen – 3rd, 13th - weight gain
Progesterone – 13th, 14th - irregular bleeding patterns to some women
Hypothalamus – initiator - no protection against STIs
NERIZA BA-AR BSN 2-YA-6 32
NCMA 217 PRELIM REVIEWER
- may cause increase vaginal discharge
TRANSDERMAL PATCH INTRAUTERINE DEVICE (IUD)
– available upon prescription and provides – a small T-shaped device that is inserted into the
continuous supply of estrogen and progestin. uterine cavity (copper or progestin-bearing)
- the patch is placed on the skin continuously for 3 - copper bearing device is effective for 4 to 10
weeks and remove for a week to allow menses to years and acts as a contraceptive by damaging the
occur sperm in transit to the uterus
- progestin-bearing device is effective for 5 to 7
A. advantage: years and affects mucus and endometrial
- with high rates on compliance development
- side effects include cramping and bleeding upon
insertion of the device and offers no protection for
B. Disadvantages: STIs
- decrease effectiveness on women over 198 pounds
- with side effects such as headache and application
site reactions
- Ortho Evra
-
prevents pregnancy by causing sterile inflammatory
reaction
VAGINAL RING
- blocks the access of sperm cells to fallopian tube
– soft flexible ring, approximately 2 inches in
- pap smear and pelvic exam must be done before
diameter that contains estrogen and progestin.
insertion
- it is placed in the vagina once a month and
- contraindicated in: PID, pregnancy, multiple sex
removed after 21 days to allow menstruation
partners, severe dysmenorrhea, cervical/ uterine
malignancy/ abnormalities
A. advantages:
- inserted during menstruation
- with high effectiveness
- low incidence of hormone-related symptoms
CBQ – most common problem: spontaneous
- easy to insert and discreet to use
expulsion of the device (signs s/x spotting and uterine
cramping)
B. disadvantages:
- woman may feel un comfortable with the ring
NERIZA BA-AR BSN 2-YA-6 33
NCMA 217 PRELIM REVIEWER
CBQ – most common complaint: ↑ excessive
vaginal discharge and dysparenunia (painful sexual
intercourse)
- Use condom for the first 3 months after insertion -
Wait 3 months after removal before attempting
pregnancy
- Check every month then after 6 months and yearly
DANGER SIGNS:
P - -period is late/missed period
A – abdominal pain (severe)
I – increase temperature
N – noticeable vaginal discharge (foul smelling)
S – spotting, bleeding, heavy periods
STERILIZATION
– permanent method of birth control obtained via MALE STERILIZATION
surgical procedure. – or vasectomy is the permanent sterilization in
- Passages of the ova and sperm cells are occluded to male.
render the person infertile. - it takes one month until ejaculations are free
WHO: from sperm
- with genetic abnormalities - vasectomy has no effect on the man’s ability to
- with medical conditions achieve or maintain erection and there is no
- couple who reached the desired no. of children interference in the production of testosterone
- have no wish to have children
-CBQ – BTL (Bilateral Tubal Ligation): sterility is
immediate
-CBQ – Vasectomy – sterility is achieved after 2
negative sperm count results
FEMALE STERILIZATION
– by tubal ligation or tubal occlusion involves
blocking or ligating (tying) the fallopian tubes
- it may be done immediately after giving birth and
is effective until 3 months until scars are fully
healed
NERIZA BA-AR BSN 2-YA-6 34
NCMA 217 PRELIM REVIEWER
VOLUME – 500-1200 ml (average of 1L)
Abnormalities in Amniotic fluid volume
- Oligohydramnios – less than 500 cc possible
malformation of fetal kidney or PROM (premature
rupture of membrane)
- Polyhydramnios – more than 1500cc indicate
GIT problem, trachea esophageal atresia/fistula
- Majority is water
- 99% water
- 1% solid particles – albumin, urea, uric acid,
lecithin, sphingomyelin, bilirubin, vernix caseosa
- Odor: mousy
- Appearance: clear and colorless or straw colored
- pH: 7-7.25 (alkaline)
- If amniotic fluid is green meconium; meconium
or the first bowel movement should be 24 hours after
birth
- can also be sign of fetal distress (cephalic)
- breech position (magkcocontract si mommy maiipit
abdominal ni baby leading to pooping) sign of
impending labor
- - If amniotic fluid is gold/yellow hemolytic
disease/Rh or Abo incompatibilities
- gray amniotic fluid infection
PURPOSE:
• Protects the baby from moving
• Controls the temperature
• Supports symmetrical growth
FETAL MEMBRANES • Prevents adherence to the amnion
1) Chorion – outermost membrane of the fetus • Allows to move
where later on going to be placenta • Source of oral fluid- kase iniinom ito ni baby dahil
2) Amnion – innermost layer, divided into parts sterile naman ito
where bag of water, amniotic fluid, and umbilical • Acts as excretion- collection repository
cord develops DIAGNOSTIC TEST FOR AMNIOTIC FLUID
- connected to umbilical cord 1) Amniocentesis
AMNIOTIC FLUID - Obtaining a sample of amniotic fluid by inserting
a needle through the abdomen.
NERIZA BA-AR BSN 2-YA-6 35
NCMA 217 PRELIM REVIEWER
UMBILICAL CORD
Aka funis
FUNCTION:
• Transport oxygen and nutrients to fetus,
unoxygenated blood and water to placenta
• Returns waste products from the fetus to the
placenta
Blood vessels: 2 arteries1 vein (AVA)
Length: 50-55 cm
Insertion: center of the placenta
- Membrane (velamentous)
- Edge of the placenta (Battledore)
2) Amnioscopy ABNORMALITIES
- “oscopy” means visualization. 1) KNOTS
- Direct visualization through an invasive intact - lead to perinatal loss because this is the lifeline of
fetal membrane. the baby
- An exam employed to visualize the forebag of the - cause brain injury or HIE (Hypoxic-ischemic
amnionic sac and to look out for meconium staining. encephalopathy)
- kulang sa oxygen supply ang brain
- brain does not have oxygen stores kase meron syang
blood brain barrier.
3) Fern test
- Determines if bag of water ruptured or not
- refers to detection of a characteristic 'fern like'
pattern of vaginal secretions when a specimen is
allowed to dry on a glass slide and is viewed under a 2) CORD COIL
low-power microscope.
- Positive – has amniotic fluid (will show fern
pattern)
- can be single or double
- usually, we insert 2 fingers to the neck of the baby
4) Nitrazine paper test to cut it and clump it hindi na pwedeng hinataying
- yellow – acidic/urine tuluyan makalabas kase masasakal si baby.
- blue green/ blue gray – alkaline; amniotic fluid - Happens 15-35% of pregnancy (common
abnormality)
3) TENSION OF THE CORD
- means that the cord is short
NERIZA BA-AR BSN 2-YA-6 36
NCMA 217 PRELIM REVIEWER
- there is low amount of Wharton’s jelly resulting to
still birth
- short cord means hindi galaw ng galaw si baby
- cause birth injuries or complication because it will
pull the placenta that will lead to Abruptio placenta
early detachment
- The doctor will do emergency cesarian birth
- Baby will experience dangerous oxygen deprivation
and sustaining brain damage worst uterine inversion
TYPES OF INSERTION:
1) Battledore insertion of umbilical cord is at the
THE PLACENTA edge
- Came from the Greek word pancake or after birth - kita maternal side
- Inunan in tagalog - there is cut blood vessel from chorionic villi
- From the combination of chorionic villi and decidua there is bleeding
basalis
Weight: 500 to 1000 grams at term 2) Velamentous Center insertion
- has 15-20 cotyledons (maximum of 28) - Cotyledons are trapped inside
(maghahanap ka kung may butas; pag may butas ibig
sabihin may naiwan foreign material si baby) - Placenta has high amounts of collagen
- Produces hormones: estrogen, progesterone, HPL, - Actual placenta is -not allowed for manufacturing of
HCG products risk for HIV
HAS 2 SIDES: FUNCTIONS
1. Maternal called Duncan; dirty looking • Protective barrier against microorganisms
- at the periphery • Has respiratory functions means there is gas
exchange of O2 and CO2
• Serves as gastrointestinal system because it
transports nutrients
• Facilitated diffusion for glucose transport and
Active transport of amino acid
• Functions as excretory. It passes through arteries
and the mother’s liver will be the one to detoxify the
waste of the baby
2. Fetal called Schultz; shiny • Circulatory system, arteries that carries the
- center--- oxygenated blood and arteries carries unoxygenated
blood.
Fetoplacental circulation through selective osmosis.
• Endocrine system. It has hormone production
called HCG. Primary purpose is to maintain corpus
luteum at first trimester of pregnancy. Secondary
function basis as pregnancy test.
• Stimulates testosterone production in the fetal
male testis and excessive levels indicate twin
pregnancy or complication such as hydatidiform
mole or chorionic carcinoma. Low HCG indicates
ectopic pregnancy and may lead to threatened or
missed abortion.
NERIZA BA-AR BSN 2-YA-6 37
NCMA 217 PRELIM REVIEWER
• Relaxin is also produced to soften the bones kay
nakaka bend si baby.
• Produces estrogen formed in the ovary possibly in
adrenal cortes, testis, fetal placenta unit and has
various functions in both sexes acts female genitalia
to produce environment suitable for fertilization and
implantation as well as nutrition for an early embryo.
• Exclusively by the corpus luteum up to 6-7 weeks
and is produced by placenta as well between 7-9
weeks. And after 9 weeks corpus luteum - Ovum – from ovulation until fertilization
degenerates and the production of progesterone is - Zygote – from fertilization until implantation
now the main responsibility of placenta. It prepares - Embryo – from implantation until 5-8 weeks of life
the lining of the uterus to receive and sustain the – Fetus – from 5-8 weeks until term.
fertilized egg and permits pregnancy kaya tinawag na - Organogenesis – formation of organ, begins 1st 2
female hormone months of pregnancy. Self-medication is not allowed
during 1st trimester of pregnancy because possible
effect of organ development.
- Placenta appears 2nd month of pregnancy (8weeks)
PLACENTA EXCHANGE ORGAN
1. Diffusion – CO2, O2, Na, Cl, fat-soluble vitamins - Ovulation age – life of fetus from ovulation →
2. Facilitated Diffusion – glucose Fertilization
3. Active Transport – amino acid, water-soluble - Gestational age (AOG) – Length of pregnancy (1st
vitamins, iron, calcium, iodine day of LMP until birth)
4. Pinocytosis – antibodies & movement of minute - Both ovulation age and gestational age are reported
particles in lunar months (4 weeks) or measured by trimesters,
we have 3 mos. in a trimester
FETAL DEVELOPMENTAL MILESTONES - Fetus grows in uterus in 9 ½ lunar months or 3 full
- From 8 to 40 weeks trimesters 38 weeks/ 266 days
- Lunar months – consist of 4 weeks - 10 months of
- 3 STAGES: pregnancy = total of 40 weeks, 280 days
1) Pre-embryonic development stage – 1st 2 weeks - Intrauterine life – in uterus
after fertilization. (1-14 days)
1ST TRIMESTER
The period of organogenesis.
2) Embryonic development stage – 2 weeks to 2
- Most critical period for fetal groth and development
months/ week 3-8 (15th day – 2 mos.)
(kasi ito ung time na nag mamature, nag gogrow, nag
dedevelop ang organs, pag nagkaproblema sa time na
3) Fetal development stage – 2 months to birth
to, the baby will have congenital deformities)
(week 8- birth)
- Organogenesis – formation of organ begins 1st 2
months of pregnancy.
- Self-medication is not allowed during 1st trimester
of pregnancy because possible effect of organ
development.
1ST MONTH (1-4 WEEKS)
NERIZA BA-AR BSN 2-YA-6 38
NCMA 217 PRELIM REVIEWER
Length: 0.75-1 cm - Sucking reflex is present. (which is tamang tama
Weight: 400 mg dahil the fetus swallows the amniotic fluid, therefore
kapag nilunok nya yung amniotic fluid the fluid will
- Heart functions as early as 16th day go to the gastrointestinal system. And thru absorption
- Development – nervous system; maternal some of the fluid will be absorb could mix with the
hypoglycemia blood and go to the kidney)
- First sign in the development of NS is - Placenta is fully developed and functional
hypoglycemia because glucose is essential to the - Sex is distinguishable
development of nervous system. - By the end of month, the fetal heart tone is already
- Rudimentary heart appears as a prominent bulge audible, by doppler
on the anterior surface that is towards end of 1st - 9-12 weeks na ang baby so may buds na siya for
month (1-4 weeks) milk teeth, teeth starts to form, nail beds also forms
- Arms and legs are buds like structure - Spontaneous movement ang galaw ni baby pero
- Spinal cord, nafoform na at fused in the midline - faint
Rudimentary eyes, nose, ears are already
discernible
2ND MONTH (5-8 WEEKS)
Length: 1 inch
Weight: 20 grams
- Sex differentiation starts
- External genitalia forming but sex is still not yet
distinguishable (ultrasound is not recommended this
early just to confirm pregnancy)
- if the sex differentiation starts in 2 months of
pregnancy, sex differentiation is completed in 4th - IMPORTANT TO REMEMBER:
month of pregnancy. • Heart functions as early in 16th day
- But the 4th month is not the best time that the • Nervous development which is manifested by
woman will undergo ultrasound to be able to identify hypoglycemia in the part of the mother because
the gender of the baby, kase ang genetalia are still glucose is unnecessary ingredient for the
small. So, pwede sya ma pagkalaman na yung development of the nervous system
scrotum can be the labia then vice versa. • Sex differentiation starts in 2nd month of pregnancy
- The fetus assumes human form • Fetal heart rate determination in second month
- Presence of amniotic fluid • 3rd month renal system is functional
- FHR determination by Doppler.
- Vital organs are formed and developing. 2ND TRIMESTER
- By the end of month, almost complete - Second trimester focuses on the length of the fetus
organogenesis. 4TH MONTH (13-16 WEEKS)
- The heart is now with septum and valves. Starting Length: 10-17 cm
to beat rhythmically. Weight: 55-120 g
- Genitals – already forming but it cannot distinguish
the gender yet. - FHT by fetoscope
- Abdomen – starting to bulge. Medyo lumalaki na - Sex differentiation is complete (pwede na makita
sya kasi nag gogrow na ung intestine sa loob. ung gender)
- Ultrasound – presence of gestational sac. - Quickening for multipara (quickening – fetal
Considered as diagnostic of pregnancy. (Positive sign movement felt by the mother 16th weeks – multi
of pregnancy) gravid mother; 5th month of pregnancy for
primigravida)
3RD MONTH (9-12 WEEKS) - IgG transport from mother to fetus
Renal system is functional - Lanugo is well formed. (Lanugo start to disappear
in 8th month)
NERIZA BA-AR BSN 2-YA-6 39
NCMA 217 PRELIM REVIEWER
- The liver and pancreas are functioning.
- Fetus actively swallows amniotic fluid. 3RD TRIMESTER
Period of rapid growth and development.
- Focus of growth is weight gain and adipose
tissues. (kailangan ng adipose tissue para maging
- Urine is also present in amniotic fluid. cute sya HAHAHA JOKE, to regulate body
- Appearance of the buds for the permanent teeth in temperature once he is born)
the gums.
7TH MONTH (25-28 WEEKS)
5TH MONTH (17-20 WEEKS) Length: 35-38 cm
- Age of viability on 20th week (generally accepted Weight: 1200 g
20-24 weeks) AOV is the earliest stage at which
fetus will be able to survive if they are born - Continued growth and development
- Weight: 500-600 g - Bone ossification
- Survival depends on the maturity of fetal nervous - Surfactant develops
system. Maturity of lungs/ presence of lungs - Male testes start to descend in the scrotal sac,
surfactant. (dapat naka suspend sa scrotum ang testis)
- Vernix appears (disappear in 9 months) - Female clitoris is prominent. (mas pansin na)
- FHT by stethoscope - Blood vessels and retina of the eyes are formed but
- Lanugo covers the body extremely thin. If retina of the eyes is extremely thin,
- Swallow amniotic the fetus also extremely susceptible to damage kapag
- Spontaneous fetal movement (mafifeel na rin kahit nag administer ng high oxygen concentration.
first time pregnant) quickening for primigravida - This is the good time for 3D ultrasound to
- Fetal stool, already present in upper intestine determine the gender of the fetus.
6TH MONTH (21-24 WEEKS) 8TH MONTH (29-32 WEEKS)
Length: 28-36 cm Length: 38-43 cm
Weight: 550 g Weight: 1600 g
- Surfactant production begins (Hearing can be - Subcutaneous fat is present
demonstrated by the fetus as he/she response to - Iron transfer from mother to fetus (going to
sudden sound.) provide iron in immediate extrauterine life)
- Hears external sound – good time to talk and play - Lanugo starts to disappear – fine downy hairs.
to the baby Full term: no lanugo
- Vernix caseosa - Nails extend to fingers.
- Eyelids start to open - Still considered as premature when delivered. -
- Skin is red and wrinkled Response to movements by sounds inside the
- Focus on continues growth and development of mother’s body.
fetus. - Moro reflex/ startle reflex is present
- Pwede ng mapanganak, preterm, high risk.
- Lung surfactant – used to sweating agents to 9TH MONTH (33-36 WEEKS)
prevent alveolar walls from sticking and allowing the Length: 42-48 cm
lungs to expand during extrauterine life. Weight: 1.8-2.7 kg
Corticosteroid (Dexamethasone, - Testes descends in scrotum
Betamethasone) - Lanugo and vernix caseosa disappear (vernix
caseosa – cheese like substance, nakabalot sa buong
- Fetal stool, already in rectum. Kaya kapag fetal katawan, cold protection)
distress sya, pwede na magkaroon ng meconium - Amniotic fluid somewhat decreases
staining - Body stores of glycogen, sugar, iron,
carbohydrate, and calcium are already deposited in
the body.
- Additional subcutaneous fats are also deposited.
NERIZA BA-AR BSN 2-YA-6 40
NCMA 217 PRELIM REVIEWER
- Most fetus starts to position in cephalic. - Fetal circulation differs from uterine circulation
(pumupwesto na siya) because fetus derives oxygen and excretes carbon
- Still considered as preterm when it delivered dioxide, not from gas exchange, but from the
exchange in the placenta.
10TH MONTH (37-40 WEEKS) - Fetal circulation differs from extra uterine
Length: 48-52 cm circulation because the fetus derives oxygen and
Weight: 3kg / 7-7.5 lbs excretes carbon dioxide not from gas exchange in the
lungs but from the exchange in the placenta.
- Bone ossification of fetal skull begins - Fetal circulation in the utero depends on the use of
- Full term; ready to be born shunts to pull blood away from the lungs. While
- Fetus kicks actively which causes discomfort of the laboring the fetus expel the fluids in its body as well
mother. as fluids in the lungs. That’s why we use surfactants
GENETICS
FETAL CIRCULATION Inherited or Genetic Disorders – disorders that can
- The heart is the first system that is functional as be passed from one generation to the next
early as the 4th week of AOG. Genetics – study of the way such disorders occur
Cytogenetics – is the study of chromosomes by light
- Normal at birth: 120-160 per minute, microscopy and the method by which chromosomal
- Heard at Doppler 10-12 weeks aberrations are identified
- Heard by stethoscope/fetoscope 18-20 weeks GENES
- Deoxyribonucleic acid (DNA)
- May difference sa heart ng baby at adult kasi may - Chromosomes
temporary structures ang baby, at a certain time mag - Human beings are composed of 46 chromosomes
ko-closed or mawawala yan (22 pairs of autosomes; homologous autosomes)
TEMPORARY STRUCTURES - 1 pair or sex chromosomes (No. 23)
• PLACENTA – source of nutrients and gas
exchange. Connected to the mother Egg cells always carry XX chromosome
Sperm cells carry either XX or XY chromosome
• FORAMEN OVALE – opening between the XX – girl
right atrium and left atrium. In adult circulation XY – boy
there is no opening between the two chambers HUMAN KARYOTYPE
• DUCTUS VENOSUS – connection between the Karyotype = appearance of chromosomes; an
umbilical veins and inferior vena cava to bypass individual’s complete set of chromosomes
the immature fetal liver. (temporary bypass; vein to X chromosome is bigger than Y chromosome
vein connection)
• DUCTUS ARTERIOSUS – connection between
the pulmonary artery and aorta in order the blood
to bypass the lungs. (artery to artery) So that the
majority of the blood won’t go to the lungs because
the fetal lungs are still immature. Some of the blood
will still go to the liver and to the lungs in order to
provide nourishment. But the majority of the blood
will bypass them because those structures are still
immature.
• UMBILICAL CORD – AVA (in fetus, 2 arteries – -
carries deoxygenated blood and 1 vein – carries
oxygenated blood) by this the baby will breathe.
NERIZA BA-AR BSN 2-YA-6 41
NCMA 217 PRELIM REVIEWER
Parent 2 (Mother) – inherited 1 non dominant gene
(blue eyed) and another dominant gene (brown eyes)
Homozygous – same trait/pattern (both non
dominant/dominant)
Heterozygous – different trait/pattern (1 dominant; 1
non dominant)
Phenotype - outward appearance of a person (face,
eyes, looks, etc)
Genotype - a person’s actual gene composition
Genome - complete set of genes.
Example 46XX or 46XY
P - short arm defect;
q - long arm defect
Example:
46XX5p- Cri-Du-Shat syndrome
46 pieces
Girl
Short arm defect
------
47XX21+ or 47XY21+ - Down’s syndrome
46 Chromosome
Homozygous – healthy gene + healthy gene
21st chromosome has additional 1 chromosome
Heterozygous – healthy gene + unhealthy gene
- Trisomy 21
46X-7q – Cystic fibrosis
MANDELIAN INHERITANCE: DOMINANT
AND RECESSIVE PATTERNS
BY GREGOR MENDEL
- discusses the dominant and recessive pattern
- dominant and non-dominant gene B = dominant
b = recessive
Bb = heterozygous
For example:
Parent 1 (Father) – inherited both non dominant
gene from his parents and his parents has blue eyes
NERIZA BA-AR BSN 2-YA-6 42
NCMA 217 PRELIM REVIEWER
Interpretation
25% chances only that their child will be normal
50% chances whether its Dh or hD that their child
will have the disease
25% incompatible for life; the baby can die during
labor and delivery
Interpretation:
AUTOSOMAL RECESSIVE INHERITANCE
25% Homozygous dominant
- Non dominant gene naman may problem
50% Heterozygous dominant
- is a pattern of inheritance characteristic of some
25% Homozygous non dominant
genetic disorder
AUTOSOMAL DOMINANT INHERITANCE
- Autosomal means that the gene in question is
“Dominant” means that a single copy of the mutated
located on one of the numbered, or non sex
gene (from one parent) is enough to cause the
chromosomes
disorder.
- Recessive means that two copies of the mutated
gene (one from each parent) are required to cause the
disorder.
Legend:
h = healthy gene
D = disease gene, dominant Legend:
hD = disease H= healthy gene
d= disease gene, recessive
Interpretation: dd= disease (not incompatible since non dominant
50% chance that their child will be normal and 50% lang pareho)
Hd or dH- carrier (since the dominant hormone is
chance that will inherit dominant disease gene
healthy but non dominant is a disease the child
will not experience the signs and symptoms of the
disease; he has the trait but not experience the
problem itself)
Interpretation
25% - healthy
50% - carrier
25% - disease
Legend:
h= healthy gene
D= disease gene, dominant
hD or Dh= disease
DD= incompatible with life
NERIZA BA-AR BSN 2-YA-6 43
NCMA 217 PRELIM REVIEWER
dd= disease
Hd or dH- carrier
Interpretation:
50% disease
50% carrier
--
Legend-:
H= healthy gene
d= disease gene, recessive
dd= disease
Hd or dH- carrier
Interpretation: Legend:
50% - healthy H= healthy gene
50% - carrier (will not experience full blown disease; d= disease gene, recessive
will only pass to next generation) dd= disease
Hd or dH- carrier
Interpretation:
All of their children will experience disease
100% disease
X-LINKED DOMINANT INHERITANCE
1. All individuals are affected.
2. All female children of affected men are affected;
all male children of affected men are unaffected
(because sex chromosome of the sperm that is
affected is the only one that is carrying the X not the
Legend: Y, and male will be coming from the Y chromosome)
H= healthy gene 3. It appears in every generation.
d= disease gene, recessive 4. All children of homozygous affected women are
dd= disease affected (XX). Fifty percent of the children of
Hd or dH – carrier heterozygous affected women are affected.
Interpretation: X-linked dominant inheritance occurs when a gene
100% carrier responsible for a trait or disorder is located on the X
chromosome.
Legend:
Xx – disease state
H= healthy gene
Xy – disease state
d= disease gene, recessive
Dominant X of the mother has the disease
NERIZA BA-AR BSN 2-YA-6 44
NCMA 217 PRELIM REVIEWER
Baby girl will have the disease
Baby boy of the father will also have the disease
because the dominant problem is from the dominant
X of the mother.
- Father has both heterozygous non dominant gene
but they are both healthy
- Mother has one x chromosome non dominant is
disease and other x chromosome is dominant but
Father have the disease healthy
All male child will not be affected
Legend:
Legend: xx- carrier
xX- disease state xy- disease state
xy- normal
How come xx is a carrier and xy is a disease state?
- because the female has another x, the normal x gene
coming from the father is balancing the disease state
of the gene x from the mother
- Since its x-linked and there is no other x that will
try to balance the problem, the male child will have
the disease
Interpretation:
- If both gene of the father are normal and one
recessive gene of the mother has abnormality
- 50% children will be normal
- 25% will be a carrier
- 25% the male child has the disease
X-LINKED RECESSIVE INHERITANCE - If we are talking about 4 children
1. Only males in the family will have the disorder.
2. A history of girls dying at birth for unknown - if 2 children:
reason often exists (females who had the affected 50% of males will have the disease
genes on both X chromosomes) 50% of girls will be carrier
3. Sons of an affected man are unaffected.
4. The parents of the affected children do not have the
disorder
NERIZA BA-AR BSN 2-YA-6 45
NCMA 217 PRELIM REVIEWER
Legend:
xy- normal
Xx- carrier
Xy- disease
Genes that are healthy are overpowering the recessive
disease gene The child will only be carrier
--
CHROMOSOMAL ABNORMALITIES --- Individual with Trisomy 21 (Down syndrome)
Cytogenic Disorders - happens when there is
abnormality in the number or structure of
chromosomes -missing, additional or distorted
chromosomes
Meiosis - type of cell division which the number of
chromosomes in the cell is reduced to haploid (half)
number for reproduction.
1. NONDISJUNCTION
- division is uneven
- failure to separate; failure to disjunction during
meiosis
EXAMPLE:
Trisomy 21: 47XX21+ or 47XY21+
Klinefelter Syndrome: 47XXY excess of one (it
boy but there is an extra X chromosome; excess
female trait)---
Turner Syndrome: 45X0 (it is a girl because there is
an X but it is lacking another X chromosome)
a) Karyotype (G banding)
Additional X chromosome leading to mal
hypogonadism
NERIZA BA-AR BSN 2-YA-6 46
NCMA 217 PRELIM REVIEWER
GENETIC COUNSELLING
1. Provide concrete, accurate information about the
process of inheritance and inherited disorders.
2. Allow people who are affected by the inherited
disorders to make informed choices about future
reproduction.
3. Offer support to people who are affected by
genetic disorders.
Timing: before the first pregnancy
Consideration: Confidentiality of information Who:
1. A couple who has a child with congenital disorder
or an inborn error of metabolism.
2. DELETION ABNORMALITIES 2. A couple whose close relatives have a child with a
part of a chromosome breaks during cell division genetic disorder.
resulting to normal number of chromosomes plus or 3. A consanguineous couple. very related couple-
minus an extra portion of a chromosome. 4. Any woman older than 35 or man older than 55
Example: Cri-du-chat syndrome: 46XY5q- when got married.
(has a long arm problem on 5th chromosome)
• History taking
• Genogram
• Physical Assessment
• Diagnostic Testing
• Karyotyping – picture of chromosome
• Choronic Villi Sampling – will get sample f-
rom placenta
NERIZA BA-AR BSN 2-YA-6 47
NCMA 217 PRELIM REVIEWER
• Maternal Serum Alpha Feto Protein – - 2 visits for the 3rd trimester
special protein coming from the liver of the - Total of 4 visits
baby (normal alpha feto protein in the blood
of the mother is 38-45 ng/dl (<38 ng is SCREENING ON THE FIRST PRENATAL
chromosomal disorder) VISIT
• Fetal Imaging 1.Health history
• Fetoscopy 2.Complete physical examination (Pelvic
PERINATAL CARE examination)
- aka pre-pregnancy care or antenatal care 3.Blood and urine specimen for laboratory analysis
- Medical care that you do during pregnancy 4.Manual pelvic measurement to determine pelvic
- Develop a plan for their reproductive life adequacy
- Health care you get while you are pregnant
- Essential for ensuring the overall health of
newborns and their mothers and a major strategy or
helping mothers to reduce complications of
pregnancy
- The early part of pregnancy is organogenesis kaya
dapat alagaan at ingatan maigi si nanay and baby.
- Nurses develop a plan for are productive life.
PURPOSE OF PRENATAL CARE
• Identify women at risk & minimize possible
complications. (iba-iba ang situation ng mga nanay
kaya gusto natin malaman ito ng maaga at kung risk
sila sa work)
• Educate women about important steps they can take
INITIAL INTERVIEW
to protect their infant and ensure a healthy pregnancy.
- Includes both present and past history. (we have to
(ano ba yung mga dapat i-participate ng nanay to
develop baseline data for future use)
ensure that she is physically healthy)
- Interviewing is best accomplished in a private, quiet
• Establish a baseline of present health.
setting.
(kasalukuyang kalusugan niya, may maintenance ba
- Caution woman that a first visit may be lengthy
siya para maiba ng doc. ung gamot na hindi pwede sa
because of all the things that need to be
buntis etc)
accomplished.
• Determine the gestational age of the fetus.
- Be certain to ask how a woman wants the nurse to
• Monitor fetal development and maternal well-being
address her and make certain she also knows the
• Provide education about pregnancy, lactation, and
name and the role of the nurse.
newborn care (ituturo natin ung mga dapat nilang
- First time that the client visits the doctor’s office.
malaman para maging aware sila na common lang un
(to gain the trust and confidence of the client)
kapag nagbubuntis, breastfeeding, paano alagaan si
COMPONENTS OF HEALTH HISTORY
baby)
a) Demographic data
HEALTH ASSESSMENT DURING THE FIRST
- This are the common information’s (name, age,
PRENATAL VISIT
address, religion)
First visit happens as soon as they suspect they are
- Age is important. (Teenage pregnancy)
pregnant
- Address – we wanted to know if the client is living
FREQUENCY OF CONSULTATION:
in congested place.
- Once a month/every 4 weeks From 1-7th month
- Religion – Jehovah does not want blood transfusion
(4-28th week)
do recommend iron sucrose
- Place of employment – baka may hazardous sa
- Every 2 weeks 36th week and then every week
work place niya or mabigat work niya
until birth
- Ethnicity – baka may cultural beliefs siya
* DOH recommends (specially this pandemic):
- 1 visit each for the first and second trimester
NERIZA BA-AR BSN 2-YA-6 48
NCMA 217 PRELIM REVIEWER
- We have to know from the very start so that we can • Multiple pregnancy – twins are counted as one
prepare. (para alam natin kung ano dapat ang action PHYSICAL EXAMINATION
natin at manners natin kay mommy) - Baseline height/ weight and vital sign measurement
- Assessment of body systems (general appearance,
b) Chief Concern mental status)
- Document the date of LMP (first day of last mens - Assessment of the heart, lungs, back, rectum,
period) extremities, and skin.
- Signs of early pregnancy (nausea and vomiting, DETERMINATION OF ESTIMATED DATE OF
breast changes, easy fatiguability, at ano mga DELIVERY (EDD)
ginagawa niya to relieve this) - Estimated Date of Delivery (EDD)
- Discomfort of pregnancy (constipation) - Estimated Date of Birth (EDB)
- Danger signs (red alert, any sign of bleeding even it - Estimated Date of Confinement (EDC)
is small amount she needs to report it; abdominal 1. NAEGELE’S RULE
pain needs to be specified; continues headache also) Formula: 1. For the first three months of the year,
add 12 to the numerical value then subtract 3 months
c) Family profile (anong meron sa family, past and add 7 days to the first day of the LMP January: 1
medical history genetic conditions) + 12 = 13
d) History of past illnesses (ano ung mga naging February: 2 + 12 = 14
sakit niya dati) March: 3 + 12 = 15
e) History of family illnesses (may mga sakit kase
na genetic)
f) Day history/ social profile (lifestyle, alcoholic,
smoker)
g) Gynecologic history – menstrual history,
perennial and breast self-examination. (ask menarche,
cycle, regular or irregular, interval, duration, amount
of menstrual flow, discomforts)
h) Past surgery (past caesarian section, surgical
procedure sa ovary, previous abdominal surgery and
etc) Formula 2. For the month of April to December,
i) Reproductive planning – is this wanted pregnancy subtract 3 months and add 7 days of the last
or unplanned menstrual period (LMP)and add 1 year.
j) Sexual history – when exactly she got sexually
active? Isa lang ba partner niya or marami?
k) Stress incontinence – naiihi ba siya kapag nauubo
etc
l) Obstetric history
– GPTPALM
• Gravida – number of pregnancies regardless of
outcome
• Parity – number of pregnancies that reach the age
of Viability (20 weeks) live or still birth?
• Term – the fetus already reaches 37 weeks and 2, MC DONALD’S RULE
above. -helps in estimating fetal gestational age using
• Preterm – the fetus delivered before 37 weeks and fundic height.
after viability. (Between 20-36 weeks)
• Abortion – miscarriages, therapeutic and non-
therapeutic, spontaneous miscarriages should be lost
before age of viability. Less than 500gms.
• Living – living children, nag kaka difference lang
sa mga may twins
NERIZA BA-AR BSN 2-YA-6 49
NCMA 217 PRELIM REVIEWER
a) Obesity
b) Polyhydramnios – increase amount of amniotic
fluid.
c) Anterior placental location
Formula 1 (Computing in lunar months):
multiply the fundic height by 2, then divide by 7.
= FH (in cm.) x 2 /7 = Gestational age in lunar
months
Formula 2 (Computing in weeks)
multiply the fundic height by 8, then divide by 7.
= FH (in cm.) x 8 / 7 = Gestational age in weeks
1) Fundal grip – palpate upper portion of abdomen
(buttocks – globular but soft and ballotable; head –
globular but hard and mass); to know if its cephalic
or breech
BARTHOLOMEW’S RULE 2) Umbilical grip – side to side (looking for fetal
- Measures the AOG by determining the position of back to auscultate – flat; toes and fingers – if other
the uterus in the abdominal cavity. side is irregular shape); fetal back is the best position
- 12 weeks – palpable just above the symphysis for fetal heart tone auscultation
pubis.
- 20th or 22nd weeks – palpable at the level of the 3) Pawlik’s grip – at symphysis pubis (which part
umbilicus. of the fetal body occupies the pelvic inlet; engage or
- 36th week – touches the xiphoid process. not engage; ballottement); if buttocks ang na fefeel sa
- 38th week – 2 weeks before term for primigravida fundal grip, it should be head that we feel on Pawlik’s
the fetal head settles into the pelvis and the uterus grip
returns to the height it was at 36 weeks. 4) Pelvic grip – determine the fetal attitude and
degree of fetal extension/ flexion (we maneuver the
baby to be in cephalic presentation)
ROLE OF THE NURSE IN PRENATAL CARE
1.Established baseline data relevant to a woman’s
health and identify health promotion strategies.
2. Teaching women and their families about safe
pregnancy lifestyle.
3. Obtained a detailed health and sexual history
including screening for the risk of teratogen exposure
as well as any concern about the woman pregnancy
4. Urging the client to continue prenatal care is
LEOPOLD’S MANEUVER important because lack of prenatal care is associated
- Are systematic abdominal palpation to determine with pregnancy complications.
the position and presentation of the fetus. 5. Be certain to reserve sufficient time during
- They are done at about 32 weeks and over. prenatal visit, so care can be thorough and there is
enough time to set realistic goals and expected
-Factors that affect reliability of findings: outcomes with both a woman and her partner
NERIZA BA-AR BSN 2-YA-6 50
NCMA 217 PRELIM REVIEWER
FETAL GROWTH & DEVELOPMENT
TERATOGENS – any drug, virus, irradiation, or any
harmful substances the exposure to which may cause
damage to the fetus.
• Streptomycin/Quinine – damage to the 8th cranial
nerve
• Tetracycline – staining the tooth enamel and inhibit
the growth of long bones.
• Vitamin K – leads to hemolysis or destruction of
RBC and hyperbilirubinemia.
• Iodines – enlargement of thyroid gland or goiter
• Thalidomides – Amelia (absence of extremities) or
Phocomelia
• Steroids – cleft lip, cleft palate, and abortion
• Lithium – congenital malformation, Epstein’s
anomaly
• Dilantin – fetal hydantoin syndrome, IUGR
(Intrauterine Growth Restriction), craniofacial
dysmorphism, microcephaly, nail hypoplasia, heart
defects
• Isotretinoin (Accutane) - congenital deafness,
microtia, CNS defects, CHO
• Alcohol – low birth weight, Fetal Alcohol
Withdrawal Syndrome characterized by microcephaly
• Smoking - low birth weight
• Caffeine – low birth weight
• Cocaine – low birth weight and abruption placenta
NERIZA BA-AR BSN 2-YA-6 51
You might also like
- Week 1 217 LecDocument15 pagesWeek 1 217 Leckristelaaa guevarraNo ratings yet
- Ncma217 Lec PrelimDocument38 pagesNcma217 Lec PrelimIVY SUPNETNo ratings yet
- Reproductive & Sexual Health: Pp. 83-116 PiliteriDocument9 pagesReproductive & Sexual Health: Pp. 83-116 PiliteriGwyneth ManioNo ratings yet
- Undescended TesticleDocument50 pagesUndescended TesticleAlvin GfNo ratings yet
- MATERNAL NleDocument8 pagesMATERNAL NleMary Danielle SaludarioNo ratings yet
- Reviewer Unit 5 by Adelle PilliteriDocument3 pagesReviewer Unit 5 by Adelle PilliteriMaria Luisa VillalunaNo ratings yet
- Module 1.1 Reproductive SystemDocument12 pagesModule 1.1 Reproductive SystemPrincess Dela CruzNo ratings yet
- Chapter 5 - MCN ReviewerDocument12 pagesChapter 5 - MCN ReviewerPrincess Queenie OlarteNo ratings yet
- Obstetric NursingDocument12 pagesObstetric NursingQueenNo ratings yet
- Science ReviewerDocument7 pagesScience ReviewerGilvert PanganibanNo ratings yet
- TH THDocument12 pagesTH THchn pastranaNo ratings yet
- 1a ReproductiveAndSexualHealthDocument2 pages1a ReproductiveAndSexualHealthKenjie Palaganas CentenoNo ratings yet
- Lesson 2 NCM 107: Review of The Anatomy and Physiology of The Male and Female Reproductive System Prof. Dymphna CasquejoDocument3 pagesLesson 2 NCM 107: Review of The Anatomy and Physiology of The Male and Female Reproductive System Prof. Dymphna CasquejoLynnelljhyen MALUBAYNo ratings yet
- F3L Int Sci Session 3-5Document30 pagesF3L Int Sci Session 3-5Danny DanNo ratings yet
- Reproduction (Dr. B. Vanderhyden) Course OutllookDocument63 pagesReproduction (Dr. B. Vanderhyden) Course OutllookJeff ParkNo ratings yet
- MCN ReviewerDocument10 pagesMCN ReviewergreinabelNo ratings yet
- Male Reproductive System PDFDocument2 pagesMale Reproductive System PDFTandingco, Olivia Mari H.No ratings yet
- Reproductive PharmaDocument106 pagesReproductive PharmaDessalegn LemmaNo ratings yet
- Male Gametes: OvariesDocument5 pagesMale Gametes: OvariesJasper OrilNo ratings yet
- Chapter 1 - SEX and Determinants of GenderDocument40 pagesChapter 1 - SEX and Determinants of GenderMA. CARLA CACHUELANo ratings yet
- 3 Human Reproduction-Sample Notes 2021Document2 pages3 Human Reproduction-Sample Notes 2021shahd elmaghraby (user206)No ratings yet
- Understanding The Self - THE SEXUAL SELFDocument5 pagesUnderstanding The Self - THE SEXUAL SELFGabrielle Anne OBOSNo ratings yet
- SCIENCE ReviewerDocument18 pagesSCIENCE Reviewermarealyn.hermida.camachoNo ratings yet
- Chapter 1 GENSO PDFDocument2 pagesChapter 1 GENSO PDFElian Kristoffer PacresNo ratings yet
- Module 3 Sexual Anatomy and Physiology of MaleDocument18 pagesModule 3 Sexual Anatomy and Physiology of MaleJazmine MoratallaNo ratings yet
- The Reproductive SystemDocument42 pagesThe Reproductive SystemAries BautistaNo ratings yet
- Simple Anatomy and PhysiologyDocument9 pagesSimple Anatomy and PhysiologyPatrick ValerioNo ratings yet
- Maternal and ChildDocument20 pagesMaternal and ChildpaderamosNo ratings yet
- Human Reproduction UPDATEDDocument16 pagesHuman Reproduction UPDATEDCandy OpsadNo ratings yet
- Term I - Chapter 15 CoreDocument37 pagesTerm I - Chapter 15 Core1005754antonioNo ratings yet
- Reviewer (HumanRep) : PRELIMDocument10 pagesReviewer (HumanRep) : PRELIMHazel GeronimoNo ratings yet
- Male & Female Reproductive SystemDocument211 pagesMale & Female Reproductive SystemDanica Marie SibayNo ratings yet
- Science 10 - Sexual Reproduction in HumansDocument4 pagesScience 10 - Sexual Reproduction in Humansj4nelle.zNo ratings yet
- CHAPTER 3 - Reproduction (Science Form 1)Document13 pagesCHAPTER 3 - Reproduction (Science Form 1)w pNo ratings yet
- Class 10 Biology 8.9.20Document11 pagesClass 10 Biology 8.9.20Shruti MahtoNo ratings yet
- The Menstrual Cycle Dra GoDocument94 pagesThe Menstrual Cycle Dra GoMichael Erick Valera VirtucioNo ratings yet
- Week 1 - Male & Female Reproductive SystemsDocument7 pagesWeek 1 - Male & Female Reproductive SystemsTEDDY BEAR PRODUCTIONNo ratings yet
- 217 Lec - Reproductive SystemDocument3 pages217 Lec - Reproductive SystemJessielyn FranciscoNo ratings yet
- 19 Reproductive SystemDocument6 pages19 Reproductive SystemEugene HerreraNo ratings yet
- Reproductive System TransesDocument5 pagesReproductive System Transesadrielvamos28No ratings yet
- Uts FinalsDocument14 pagesUts Finalsocoyjanrino274No ratings yet
- Developmental Biology XL 138: Week 10Document61 pagesDevelopmental Biology XL 138: Week 10Soji AdimulaNo ratings yet
- Sexual Reproduction in HumanDocument15 pagesSexual Reproduction in Humanganu89No ratings yet
- Presentation StudentDocument61 pagesPresentation Studentvsvm2009No ratings yet
- Maternal NewDocument30 pagesMaternal NewKhristine Rose Sanchez CaloNo ratings yet
- Thahseena Abdul Aziz S4 PsychologyDocument7 pagesThahseena Abdul Aziz S4 Psychologyunknown nnNo ratings yet
- Obstetric Nursing Review NLEDocument48 pagesObstetric Nursing Review NLEDylan Angelo AndresNo ratings yet
- Notes in ScienceDocument4 pagesNotes in ScienceKate NicoleNo ratings yet
- 107 Lec Prelim TopicsDocument22 pages107 Lec Prelim TopicsMary Ann SacramentoNo ratings yet
- Report in Sexual Self-A&bDocument34 pagesReport in Sexual Self-A&bJulie LusuegroNo ratings yet
- Enhanced Notes 3 Reproductive SystemDocument5 pagesEnhanced Notes 3 Reproductive SystemLyle CasulNo ratings yet
- Maternal & Child Care Nursing ReviewDocument37 pagesMaternal & Child Care Nursing Reviewɹǝʍdןnos98% (130)
- Evaluation and Management of Elevated Intracranial Pressure in Adults - UpToDate PDFDocument32 pagesEvaluation and Management of Elevated Intracranial Pressure in Adults - UpToDate PDFSebastianNo ratings yet
- In Partial Fulfillment of The Final Requirements in Advanced Health Assessment MSN 205Document13 pagesIn Partial Fulfillment of The Final Requirements in Advanced Health Assessment MSN 205Gummie Akalal SugalaNo ratings yet
- Goodnight Beautiful-Dorothy KoomsonDocument13 pagesGoodnight Beautiful-Dorothy KoomsondarijarasetaNo ratings yet
- Steps To Prepare The Divine Golden BookDocument2 pagesSteps To Prepare The Divine Golden Bookdesign12No ratings yet
- Jurnal 5 CDocument9 pagesJurnal 5 CCintya RambuNo ratings yet
- Desribe Facial ExpressionDocument3 pagesDesribe Facial ExpressionAsmidar HashimNo ratings yet
- Mark Scheme (Results) Summer 2016: Pearson Edexcel International GCSE in Biology (4BI0) Paper 2BRDocument12 pagesMark Scheme (Results) Summer 2016: Pearson Edexcel International GCSE in Biology (4BI0) Paper 2BRMostofa ZarifNo ratings yet
- Ucsc TranscriptDocument8 pagesUcsc Transcriptapi-463075447No ratings yet
- Abnormal Progress in Labor (Precipitous Labor and Birth & Retraction Rings)Document34 pagesAbnormal Progress in Labor (Precipitous Labor and Birth & Retraction Rings)Ana100% (3)
- A Textbook of Clinical Pharmacology and Therapeutics PDFDocument6 pagesA Textbook of Clinical Pharmacology and Therapeutics PDFMovie Box MoviesNo ratings yet
- Acoelomate Bilateral AnimalsDocument31 pagesAcoelomate Bilateral AnimalsHirendra GurnaniNo ratings yet
- Surgical SkillsDocument47 pagesSurgical SkillsSamah SuhailNo ratings yet
- MM TemperamentsDocument27 pagesMM TemperamentsKalpesh Jain100% (2)
- Genetics Notes Bio 2C03Document29 pagesGenetics Notes Bio 2C03Wayne FangNo ratings yet
- Iron-Refractory Iron Deficiency Anemia May Not Lead To Neurocognitive Dysfunction: A Case ReportDocument6 pagesIron-Refractory Iron Deficiency Anemia May Not Lead To Neurocognitive Dysfunction: A Case ReportwitwiiwNo ratings yet
- IS.5216 1982part2Document27 pagesIS.5216 1982part2Mahendra SuryavanshiNo ratings yet
- Carbohydrate and Lipid Metabolism in Farm AnimalsDocument4 pagesCarbohydrate and Lipid Metabolism in Farm AnimalsPinaNo ratings yet
- Ammonium Persulfate (A3678) - Product Information SheetDocument1 pageAmmonium Persulfate (A3678) - Product Information SheetPatricio Javier Alfaro CerdaNo ratings yet
- Post-Herpetic Neuralgia: A Review: Current Pain and Headache Reports March 2016Document6 pagesPost-Herpetic Neuralgia: A Review: Current Pain and Headache Reports March 2016headseNo ratings yet
- RH Incompatibility: Go ToDocument4 pagesRH Incompatibility: Go ToFadhila AnasNo ratings yet
- Anatomy of The Psoas MuscleDocument2 pagesAnatomy of The Psoas MuscleMilos KovacevicNo ratings yet
- Felixcharlie Electrolyte Homeostasis Part 3Document3 pagesFelixcharlie Electrolyte Homeostasis Part 3Nur Fatima SanaaniNo ratings yet
- Breathing For Singing-The Anatomy of RespirationDocument11 pagesBreathing For Singing-The Anatomy of RespirationAnurrag Kumar100% (3)
- Human FactorDocument210 pagesHuman FactorJames MwamuyeNo ratings yet
- Bahasa Inggris XI K13Document12 pagesBahasa Inggris XI K13Shazea R AtayasakhiNo ratings yet
- Anatomy ProstateDocument2 pagesAnatomy ProstateCarl Julienne MasangcayNo ratings yet
- Ujian Bio Tingkatan 4Document4 pagesUjian Bio Tingkatan 4amanNo ratings yet
- Biopsychology NotesDocument5 pagesBiopsychology NotesPatricia100% (1)
- Anabolic Priming Posture RestoreDocument21 pagesAnabolic Priming Posture RestoreSamir KapetanovicNo ratings yet
- Types of Necrosis and InfarctDocument4 pagesTypes of Necrosis and InfarctTowhidulIslam75% (4)