Professional Documents
Culture Documents
CMS RN
Uploaded by
day alcoberOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CMS RN
Uploaded by
day alcoberCopyright:
Available Formats
Cardiovascular System
Anatomy
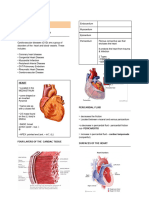
● The heart is a muscular organ located in the chest
● Four chambers of the heart
○ Right atrium (RA): receives blood from the body
○ Right ventricle (RV): pumps blood to the lungs
○ Left atrium (LA): receives oxygenated blood from the lungs
○ Left ventricle (LV): pumps oxygenated blood out of the heart to the aorta
● Valves of the heart
○ Atrioventricular valves (AV)
■ Tricuspid valve: b/w the RA and RV
■ Mitral valve: b/w the LA and LV; the only valve with two cusps
○ Semilunar valves
■ Pulmonary valve: separates the RV from the pulmonary artery
■ Aortic valve: separates the LV from the aorta
○ Stenosis: a valve that does not open properly
○ Regurgitation: a valve that does not close properly and lead to leaking
● Heart sounds “lub dub”
○ S1: “lub” sound during systole by the closure of the mitral and tricuspid valves
○ S2: “dub” sound during diastole by the closure of the pulmonic and aortic valves
○ S3: abnormal heart sound created by ventricular straining with increased volume
(due to CHF or pulmonary edema)
○ S4: abnormal heart sound due to worsening HF
○ Murmur: a muffled “whoosh” sound due to heart valves not opening or closing
properly (stenotic valves)
○ Friction rub
■ Creaking or scratching sound caused by rubbing of the pericardial sac
■ More pronounced when patient leans forward
■ How to differentiate pericardial v.s. pleural friction rub
● Ask patient to hold their breath
○ If the sound continues, it’s pericardial
○ If the sound stops, it’s pleural
● Pericardium: a sac that surrounds and lubricates the heart
● Vessels of the heart
○ Superior vena cava (SVC): returns blood from the head, neck, arms, and chest to
the right atrium
○ Inferior vena cava (IVC): returns blood from the legs and organs in the abdomen
and pelvis to the right atrium
○ Pulmonary arteries: carries deoxygenated blood from the heart to the lungs (the
only arteries that carry deoxygenated blood in the body)
○ Pulmonary veins: carries oxygenated blood from the lungs to the heart
○ Aorta: main artery that pumps oxygenated blood from the heart to the rest of the
body
○ Coronary arteries
Disclaimer: This study guide is intended for educational purposes only.
■ Arteries that branch off the aorta and supply blood to the heart
■ Coronary blood flow occurs mostly during diastole
■ Left coronary artery (LCA)
● Left main coronary artery (LMCA)
○ Left anterior descending (LAD) artery
■ Supplies blood to the anterior LV, interventricular
septum, right bundle branch, small portion of left
bundle branch
○ Circumflex artery
■ Supplies blood to the lateral walls of LA, LV
● Right coronary artery (RCA)
○ Supplies blood to RA, RV, inferior wall of LV
○ Branches off into
■ Posterior descending artery (PDA)
■ Right marginal artery
● Conduction system
○ The heart’s ability to generate and spread electrical activity that causes cardiac
muscle contraction
○ Sinoatrial node (SA node) ➜ Atrioventricular node (AV node) ➜ Bundle of His ➜
Right & Left bundle branch (LAF & LPF) ➜ Ventricular purkinje fibers
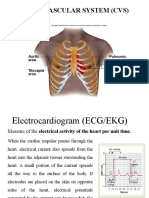
○ P-wave
■ Occurs in the SA node (pacemaker)
■ Contraction of the atria
○ P-R interval
■ Occurs in the AV node
■ Traveling of impulses across the AV node to the His-Purkinje system
■ Normal = <0.20 sec
○ QRS interval
■ Impulses traveling down to the His-Purkinje system
■ Systole: depolarization (or contraction) of both ventricles
○ T wave
■ Diastole: repolarization (or resting) period of the heart
○ ST interval
■ Interval between depolarization and repolarization
■ Vulnerable phase as it can be easily stimulated by other impulses and
cause life-threatening rhythm
Disclaimer: This study guide is intended for educational purposes only.
○ Life threatening arrhythmias
Symptomatic Bradycardia Ventricular Tachycardia Ventricular Fibrillation
● <40 bpm ● Rapid ● fatal rhythm
● 3rd degree heart ventricular rate and does not
block (150-250 bpm) self resolve
● Low cardiac output ● HR >300
Risk ● Ischemia/MI ● Electrolyte ● MI
factors ● Drugs imbalance
● Sick sinus ● MI
● Electrolyte ● Cardiomyopath
imbalance y
S/S ● hypotension/low ● Chest pain ● Hypotension
MAP ● Fainting ● Loss of
● Decreased LOC ● Dizziness conscious
● Confusion ● SOB ● death
● Fatigue
Treatment Call a code, start CPR if Call a code, start Call a code, start CPR
indicated CPR if indicated and AED
● Atropine (to ● Medication to ● Implantable
increase HR) slow the heart defibrillators
● Transcutaneous rate (for long term
pacing ● AED or management)
synchronized
cardioversion
● Implantable
defibrillator (for
long term
management)
● Hemodynamics
○ Cardiac output (CO)
■ Total volume of blood ejected by the heart per minute
■ Normal output = 5 L/min
■ CO=heart rate (HR) x stroke volume(SV)
● HR affected by ANS and demand of oxygen
● SV affected by preload, afterload, and contractility (see below)
■ Changes in either HR or SV can alter CO
○ Cardiac index (CI): 2.5 to 4 L/min
■ Takes body surface area (BSA) into account
■ More accurate
○ Stroke volume
■ Volume of blood ejected from the ventricles with each contraction
Disclaimer: This study guide is intended for educational purposes only.
■ Preload
● The measurement of stretching of the ventricles at the end of
diastole (ventricular filling)
● Depends on whether patient is hypovolemic (reduces preload) or
overloaded (increases preload)
■ Afterload
● The amount of force ventricles must overcome to pump blood into
arterial circulation
● Factors that affect afterload: vasoconstriction, vasodilation,
hypertension, atherosclerosis (narrowing of arteries)
■ Contractility
● The strength of the heart muscle to contract
● Starling’s Law states greater stretch leads to greater
contraction to a point of overstretch or overfill, leading to
muscle weakness
○ Ejection fraction
■ Percentage of blood ejected from the left ventricle with each heartbeat
■ Normal = 55%-65%
○ Blood pressure
■ Measure of pressure exerted by blood against the arterial walls
■ Systolic BP: the pressure of blood that is exerting against the artery walls
during contraction
■ Diastolic BP: the pressure of blood that is exerting against the artery walls
during the resting phase
○ Mean arterial pressure (MAP)
■ Measures the average perfusion pressure to a patient’s organs through a
single cardiac cycle
■ = SBP + (2 X diastolic blood pressure) / 3
■ MAP has to be 65-70 for vital organ perfusion
● Vascular system
○ Arteries
■ Carry oxygenated blood away from the heart and towards the body
■ Aorta: the largest artery
■ Arterioles: the smallest branches of arteries
○ Capillaries
■ Smallest blood vessels that connect arteries and veins
○ Veins
■ Carry deoxygenated blood back to the heart and have one-way valves to
prevent blood from flowing backwards
■ SVC and IVC are the largest veins in the body
■ Venules: small veins that receive blood from capillaries and merge into
larger veins
Labs
● Troponin
Disclaimer: This study guide is intended for educational purposes only.
○ Proteins found in the cardiac myocytes
○ First line test for evaluating acute MI
○ Starts to elevate 3-4 h after myocardial injury, and peaks in 12-16 h, then
begins to fall over in the next 1-2 wk
○ Useful for diabetics with subtle symptoms due to decreased sensation of pain
(SOB, nausea, fatigue)
○ Trend troponin to rule out other causes; only MI will lead to rise and fall of
troponin levels
○ Other causes: CKD (has a constant elevated troponin), myocardial strain, CVA
● CPK-MB
○ 6-8 h after injury
○ Peaks in 12-24h
○ Lasts 48 h
○ Less sensitive and specific than troponin to indicate acute MI
○ However they are useful in evaluating second infarct
○ Since CPK-MB normalizes 48 to 72 hours after myocardial ischemia (vs.
troponins, which can persist for days), it can be useful in detecting
re-infarction if levels rise again after declining
○ Can be elevated in non-cardiac conditions such as skeletal muscle injury,
hypothyroidism, chronic renal failure, and severe exercise
● B-type Natriuretic Peptide (BNP)
○ A chemical released by the ventricles when there is a strain on the heart
○ BNP helps to get rid of Na and water; hence the name “natriuretic”
○ Indicator for CHF and used to trend the effectiveness of CHF treatment
● Myoglobin
○ Not cardio-specific; also found in skeletal muscles
○ Can be released after injury by any muscle in the body
○ Can cause AKI: aggressive fluid
○ Present within 1 hour of injury (aids in fast diagnosis of possible MI but less
specific)
○ Peaks in 8-12 h
○ Lasts 24 h
● Homocysteine
○ An amino acid
○ Elevation can indicate heart disease
○ If high, take 1 mg of folic acid daily to lower it
● C-reactive protein and procalcitonin
○ Chemical released during an inflammatory response in the body
Acute Coronary Syndrome (ACS)
● A group of conditions where the blood flow to the heart is decreased
● Examples include unstable angina, NSTEMI, STEMI
● Causes
○ Atherosclerosis with rupture of plaque (most common)
Disclaimer: This study guide is intended for educational purposes only.
○ Thrombus
○ Vasospasm
● Chest pain
○ (different population has different presentation of chest pain)
○ Males
■ Typical symptoms: crushing pain or pressure (“elephant sitting on chest”),
radiates to the neck, jaw, left or both arms, lightheadedness, nausea,
SOB
■ More likely to have STEMI
○ Females
■ Atypical symptoms: burning in the throat, neck, jaw, back, palpitation,
fatigue, anxiety, SOB, nausea
■ Occur later
○ Diabetics
■ SOB, fatigue
■ Altered sensation of pain due to neuropathy
○ Elderly
■ Inability to describe due to aging, dementia
■ Don't want to complain or bother staff
● Stable angina
○ Chest pain caused by transient ischemia
○ Worsened with activities but relieved by rest and nitroglycerin
○ Usually due to spasm (instead of occlusion in NSTEMI and STEMI)
○ Predictable and manageable
● NSTEMI
○ MI with no ST elevation
■ If positive troponin = NSTEMI
■ If negative troponin = unstable angina
○ Partial occlusion of vessels leading to ischemia without myocardial injury
○ Not relieved by rest or nitroglycerine
○ A precursor to MI
○ EKG: T wave inversion, ST depression
● STEMI
○ MI with ST elevation
○ Total occlusion of vessels resulting in ischemia with myocardial injury and/or
infarct
○ The full thickness of the wall of the heart has been damaged
○ EKG: ST elevation (tissue injury), pathological Q wave (infarction)
● Treatment
○ (goal is to provide oxygen, decrease the workload of the heart, dissolve or
prevent blood clots)
○ STEMI
■ Once confirmed, obtain cath lab for PCI within 90 minutes or thrombolytic
therapy within 30 minutes
Disclaimer: This study guide is intended for educational purposes only.
○ NSTEMI & STEMI interventions
■ Morphine, Oxygen, Nitroglycerin, Aspirin
■ Beta blockers (lowering the HR helps to reduce myocardial demand)
■ ACEI/ARB (to reduce preload)
■ Heparin infusion
■ Antiplatelets: ticagrelor (Brilinta) or clopidogrel (Plavix)
■ Statin
■ Cardiac monitor (dysrhythmia and HF are common complications after
MI)
○ Core measure
■ Aspirin on arrival and at discharge
■ beta-blockers and statins at discharge
■ ACEI or ARB at discharge for all patients with left ventricular systolic
dysfunction
■ fibrinolytic therapy within 30 minutes of arrival
■ timely initiation of PCI within 90 minutes of arrival
○ Patient education
■ Smoking cessation
■ Cardiac diet: low salt, low fat
■ Lower cholesterol level: diet, statins
■ Exercise
■ Prevent or control hypertension, diabetes, obesity
■ If pain occurs at rest: take aspirin, call 911
■ Cardiac rehab
Heart Failure (HF)
● Pathophysiology
○ Inability of the heart to pump blood forward, resulting in backup of fluid
○ Starling’s Law: greater stretch leads to greater contraction to a point of
overstretch or overfill, leading to muscle weakness
○ Complications:
■ Inability to pump blood forward will lead to
● Reduced EF/cardiac output, AKI, cardiogenic shock, multisystem
organ failure (MODS)
■ Backup of fluid will lead to
● Pulmonary edema, hepatic congestion
● Causes
○ MI, CAD, arrhythmias (all weakens the cardiac muscles)
○ Cardiomyopathies
○ Uncontrolled HTN, valvular disease (increases the pressure that heart has to
pump against leading to enlargement of heart muscle)
○ COPD (pulmonary HTN increases the pressure on the right heart causing right
HF or Cor Pulmonale)
● Renin-Angiotensin-Aldosterone System (RAAS)
Disclaimer: This study guide is intended for educational purposes only.
○ A compensatory mechanism
○ Decreased blood flow to the kidneys→ kidneys release renin→ liver converts
angiotensinogen to angiotensin I→ ACE converts angiotensin I to II in the lungs
○ Angiotensin II causes vasoconstriction and stimulates the adrenal gland to
release aldosterone
○ Aldosterone causes reabsorption of Na and retains fluid
○ (Remember: kidneys→ renin, liver→ angiotensin I, lungs→ ACE & angiotensin II)
● S/S
○ Left: fluid backup to the lungs → respiratory s/s
○ Right: fluid backup to the systemic circulation → generalized swelling
○ Left sided HF can lead to right sided HF and lead to combination of s/s
Right sided HF Left sided HF
● (backflow to the body) ● (backflow to the lungs)
● JVD (assess with HOB at 30 ● DOE
degrees) ● Orthopnea
● Abdominal distention ● Crackles in the lungs
(anorexia, bloating, nausea) ● S3 & S4 heart sounds
● Engorged liver/spleen ● Systolic murmur
● Dependent edema ● Anxiety
● Activity intolerance ● Activity intolerance
● Treatment
○ Goal is to increase cardiac output and reduced workload of the heart
○ Medications
■ Beta blockers: lowers HR and oxygen demand of the heart muscles; also
prevents cardiac remodeling (especially after MI)
■ ACEI/ARBs/Diuretics/Nitrates: all decrease preload and afterload
■ Digoxin: positive inotropy (increases the contraction force of the heart and
improves the cardiac output)
○ HF core measures
■ Echo to evaluate EF & LVF before discharge
■ ACEI/ARB on discharge for pt with LVEF <40% or moderate to severe
systolic dysfunction
■ Patient education
● Low Na, low cholesterol, fluid restriction
● Activity level (balance between rest and exercise)
● Weight monitoring
○ Weight in the morning
○ Notify provider if >2-3 lb weight gain in a day or >5 lb in a
week
● S/S of increasing failure
○ Weight gain, SOB, worsening edema, decreased urine
output
● Follow up appt
Disclaimer: This study guide is intended for educational purposes only.
Hyperlipidemia
● Total cholesterol <200 mg/dL
● HDL: 40-60 mg/dL (“good” cholesterol as it can pull fatty deposits away from vessel
walls)
● LDL: <130 mg/dL (“bad” cholesterol as it can form plaques that can rupture and lead to
blood clots)
● Triglyceride: <150 mg/dL
● Treatment
○ Dietary modification can lower LDL and triglyceride level while exercise can
improve HDL level
○ Statins: Atorvastatin (Lipitor), simvastatin (Zocor)
■ Monitor liver functions
■ Monitor for rhabdomyolysis (breakdown of muscle cells causing severe
muscle pain)
Peripheral Vascular Diseases
Arterial Venous
Definitions ● Decreased blood flow in the ● Pooling of blood and waste
arteries often due to products in the veins of the
atherosclerosis lower extremities
● Caused by DVT obstructing
venous return or venous
insufficiency in which the
valves in the veins don’t shut
properly and blood flows
backward and pools in the
veins
Risk factors ● Smoking ● Age
● High cholesterol ● Obesity
● Diabetes ● Prolonged sitting or standing
S/S ● Loss of hair (specific to ● Edema
arterial disease) ● Dark discoloration (due to
● Cool extremities breakdown of hgb)
● Pain with activity ● Non-healing wounds (due to
inability to remove waste
product from tissues)
Treatment ● Exercise ● Exercise (as veins rely on
● Statins to lower cholesterol muscle movement to force
● Thrombolytic for clots the blood flow back up to the
● Bypass surgery heart)
● Compression stocks;
elevation of extremities
● Diuretics
● Avoid high salt diet
Disclaimer: This study guide is intended for educational purposes only.
● Antiplatelet drugs
Hypertension
● #1 risk factor for strokes
● Definitions
○ Normal: SBP <120 & DBP <80
○ Elevated: SBP 120-129 & DBP <80
○ Hypertension stage I: SBP 130-139 & DBP 80-89
○ Hypertension stage II: SBP >140 & DBP >90
○ Hypertensive urgency: SBP >180 and/or DBP >120
○ Hypertensive emergency: SBP >220 & DBP >140
● Risk factors
○ Family history, age >60, African American
○ Pregnancy, diabetes, thyroid disorders
○ Lifestyles: high salt diet, smoking, alcohol use, illegal drug use
○ Medications: NSAIDs, decongestants, oral contraceptives, steroids
● Treatment
○ Dietary modification: restrict Na, increase K+ intake
■ DASH diet to prevent hypertension
● Low fat, low sodium
○ Smoking cessation, minimize alcohol intake, stress management
○ Exercise
○ Educate elderly patients on possible S/E of dizziness and falls
○ Medications
■ ACE inhibitors
● blocks formation of angiotensin II & aldosterone and lead
vasodilation
● “-pril”
● S/E: hyperkalemia, dry cough, hypotension
■ Angiotensin II receptor blockers (ARBs)
● Similar to SCRI
● “-sartan”
● Contraindicated in pregnancy
■ Calcium channel blockers
● Blocks calcium influx into smooth muscles and cause vasodilation
■ Diuretics
● Promote Na excretion in the kidneys and increased urine output
● Hypertensive emergency
○ Severely elevated BP (>220/140) with evidence of end-organ damage
○ S/S: severe headache, dizziness, vision changes, epistaxis, chest pain, oliguria
○ Treatment
■ Treatment within 1 hour to prevent end-organ damage and death
■ Reduce arterial pressure carefully
Disclaimer: This study guide is intended for educational purposes only.
● No more than >10% decrease in MAP in the first hour
● Dropping too quickly can lead to organ damage
Aortic Aneurysm
● Weakening of the vessel walls resulting in bulging of the aorta
● Locations
○ Thoracic: by the aortic arch; more common for dissecting aneurysm
○ Abdominal: most common
● Risk factors
○ HTN is #1 risk factor in elderly
○ HLD, atherosclerosis (plaque can erode the vessel wall)
○ Marfan syndrome
● S/S
○ Aortic/thoracic: pain, dysphagia, dyspnea
○ Abdominal: dull lower back pain, pulsation in the abdomen, abdominal bruit
● Ruptured aneurysm
○ A medical emergency
○ S/S
■ Sudden, severe low back pain or sharp tearing pain in the mid-chest
■ Bruising along the abdomen, flank
Cardiac Tamponade
● Fluid or blood filled in the pericardium and lead to inefficient pumping of the heart
● S/S: chest pain, hypotension, muffled heart sounds
● Pulsus paradoxus: drop of 10 mmHg in blood pressure during inspiration
● Treatment
○ Oxygen, IVF, positive inotropes, pericardiocentesis
Cardiovascular Medications
● Familiar with drug classifications instead of individual drugs, know their side effects,
precautions, and patient education
Classifica Examples Action Side effects & precautions
tions
Beta Ends in “lol” ● Block beta receptors ● S/E: bradycardia,
blockers Beta 1 blockers and slow down the fatigue, depression,
● Metoprolol conduction signals erectile dysfunction
(Lopressor) ● Lower HR ● Dose reduction in
● Atenolol ● Reduce workload renal dysfunction
(Tenormin) ● Prevent arrhythmia ● Caution in COPD or
Beta 2 blockers ● Beta 1 blockers asthma; may cause
● Propranolol (cardioselective; mainly bronchospasm
(Inderal) affects the heart) ● Caution in diabetic pt
Mixed blockers ● Beta 2 blockers as BB can mask s/s
Disclaimer: This study guide is intended for educational purposes only.
● Labetalol (non-cardioselective; of hypoglycemia
(Normodyn affects both the heart (tachycardia,
e) and lungs) sweating)
● Carvedilol ● Mixed alpha & beta
(Coreg) blockers (have both
beta and alpha blockers
effects)
Calcium End in “-pine” ● Block entry of calcium ● Reflective
channel ● Amlodipine into muscle cells and tachycardia (due to
blockers (Norvasc) cause vasodilation and lowered BP)
● Nifedipine decreased contractility ● Constipation
● (Procardia) (negative inotropy) ● Could worsen CHF
● Nicardipine ● Lower BP, less vascular
(Cardene) resistance
● However, the negative
inotropy can worsen
CHF
ACE Ends in “-pril” ● Inhibit actions of ● Dry cough
inhibitors ● Lisinopril ACE/RAAS and lead to ● Hyperkalemia (ACEI
(ACEI) (Prinivil) vasodilation and promotes Na
● Enalapril decreased afterload excretion and K+
(Vasotec) ● Cardioprotective retention)
● Captopril (prevent ventricular ● Pt should avoid
(Capoten) remodeling after MI) taking K+
● Most beneficial with LV supplements, or
dysfunction diet rich in K+ (salt
substitute)
● Angioedema (rare;
life-threatening
airway swelling &
obstruction)
Angioten Ends in “-sartan” ● Blocks the activation of ● Frequently used with
sin ● Losartan the RAAS leading to CCB as first line
Receptor (Cozar) vasodilation treatment for BP
Blockers ● Valsartan ● S/E: orthostatic
(ARBs) (Diovan) hypotension,
● Candesarta hyperkalemia
n (Atacand)
Nitrates ● Nitroglyceri ● A vasodilator ● S/E: headache,
n ● Reduces preload and syncope,
● Isosorbide afterload hypotension
(Isordil) ● Mostly used for acute ● Continuous nitrate tx
treatment can lead to tolerance
within 24 to 48 h
making it less
effective
Disclaimer: This study guide is intended for educational purposes only.
● Nitrate free period is
a 8-12 h break in
between doses
Positive ● Digoxin ● block Na+/K+ pumps ● Caution with use in
inotropes and increase cardiac kidney impairment
contractility ● hypokalemia can
● For HF, rate control in A lead to dig toxicity
fib (but not first line) while dig toxicity
● Narrow therapeutic itself can lead to
index (1-2 ng/ml) and hyperkalemia
requires close ● Dig toxicity
monitoring ○ arrhythmias,
● Reversed with DigFab anorexia,
nausea,
confusion,
hyperkalemia
○ halos,
green-yellow
vision
● Amiodarone and
NSAID can increase
dig toxicity
Diuretics ● Most diuretics work by ● Caution with kidney
inhibiting sodium impairment
reabsorption in kidneys ● S/E: hypotension,
● Loop diuretics dehydration,
○ Furosemide hypokalemia
(Lasix)
○ Bumetanide
(Bumex)
● Thiazide
○ Hydrochlorothia
zide (Microzide)
○ Chlorothiazide
(Diuril)
● Potassium sparing
○ Spironolactone
Anti-plate ● Aspirin ● Make platelets less
let ● Clopidogrel sticky to prevent
aggregat (Plavix) aggregation
es ● Ticagrelor ● Do not dissolve existing
(Brilanta) clots
● No regular blood tests
needed
Anticoag ● Warfarin ● Warfarin is a vitamin K ● Warfarin & diet:
Disclaimer: This study guide is intended for educational purposes only.
ulants (Coumadin) antagonist Vitamin K intake
○ Takes 3 days to should be consistent;
be therapeutic no need to increase
and can last for or decrease; warfarin
3-5 days after dosing will match
discontinuation patient’s dietary
○ Requires INR intake of Vit K as
monitoring (goal long as it does not
2-3) fluctuate significantly
○ Can be
reversed with vit
K, FFP
Indirect Both injectable ● Inhibit part of the ● Lovenox dose
thrombin ● Heparin (IV, clotting cascade adjustment for
inhibitor subq) ● Used as a bridge kidney insufficiency
● Enoxaparin before Warfarin is (should not be used
(Lovenox) therapeutic in dialysis dependent
(subq) ● Heparin patients)
○ Prevents ● Rotate injection sites
formation of and do not rub
clots or growth
of existing clots
○ Does not
dissolve existing
clots
○ Reversed by
Protamine
Sulfate
○ Can lead to
heparin-induced
thrombocytopen
ia (HIT);
platelets fall
>30% baseline
Novel Ends in “-an” ● Factor Xa inhibitors ● Monitor for excessive
oral ● Apixaban ● Short half-life bleeding
anticoagu (Eliquis) ● No lab monitoring ● Short half life makes
lants ● Dabigatran ● However, no reversal holding or missing a
(NOACs) (Pradaxa) agents (and most are dose important
● Rivaroxaba not dialyzable) ● Take a dose at the
n (Xarelto) same time
everyday. If a dose
is missed, take it
as soon as
remembered but
Disclaimer: This study guide is intended for educational purposes only.
do NOT double up
on doses
Disclaimer: This study guide is intended for educational purposes only.
Respiratory System
Definitions
● Ventilation: movement of air in and out of the lungs
● Perfusion: gas exchange in the alveoli where oxygen is absorbed and carbon dioxide is
released
● V/Q mismatch
○ V=ventilation, Q=perfusion
○ The amount of air and blood that reaches the alveoli should be a 1:1 ratio
○ V/Q mismatch happens when the amount of ventilation in the alveoli does not
match the amount of perfusion
● Vital capacity: the maximum amount of air a patient can expel from the lungs after a
maximum inhalation
● Residual volume: the amount of air remaining in the lungs after a forced exhalation
● Tidal volume: the normal amount of air that moves in and out when extra effort is not
applied; normal is 500 ml
● Peak flow: a measure of the patient’s maximum speed of expiration; peak flow meter is
recommended daily to predict narrowing of the airways in asthma patients
Anatomy
● Upper airway
○ Nose, sinuses, pharynx, oropharynx, laryngopharynx, trachea
○ Warm, filter and humidify air
● Lower airway
○ Left and right lungs (left two lobes, right three lobes), bronchus, bronchioles
○ Alveoli: where gas exchange takes place; type II alveoli = surfactant
● Respiratory muscles
○ Intercostal muscles, sternocleidomastoid, trapezius, diaphragm
○ Muscles contract during inhalation to create negative pressure and draw air into
airways
○ Muscles relax during exhalation to create positive pressure and force air out of
airways
Abnormal lung sounds
● Crackles: heard on inspiration; caused by fluid in the lungs from CHF, pulmonary
edema
● Rhonchi: heard on expiration; caused by mucus in the airways
● Wheezes: heard on inspiration and/or expiration; caused by narrowing of airway due to
inflammation
● Pleural friction rub: heard on inspiration; caused by inflammation and rubbing of the
visceral pleura and parietal pleura
● Increased fremitus: increased vibration felt by palpation due to consolidation in the
lungs; press against the chest with the palms of the hands and ask the patient to say
“99”
Disclaimer: This study guide is intended for educational purposes only.
Oxygen
● FiO2:
○ Fraction of inspired oxygen (%)
○ Whenever you take a breath, you are breathing in a mix of oxygen and other
gasses and only 21% of the gasses you breath in is oxygen
○ When you give patients oxygen, you are increasing their FiO2 level
● Nasal cannula: 24-45% FiO2; flow rate 1-6 L/min
● Simple mask/oxymask: 35-50% FiO2; flow rate 6-8L; low flow rate can cause rebreathing
of CO2
● Non-rebreathing mask: 70-100%; flow rate 10-15L; for acutely desatting patient
● High flow: humidify inspired air delivered through device
Arterial Blood Gas (ABG)
● Tips to remember
○ Ask yourself if the CO2 and HCO3 are normal; whichever is furthest away from
normal will indicate the primary issue as respiratory or metabolic.
○ CO2 is acidic
○ Upper GI is acidic and lower GI is alkalotic
○ Metabolic compensation can take days to complete while respiratory
compensation is immediate
○ Uncompensated: abnormal pH + abnormal CO2 or HCO3
○ Compensated: normal pH (usually borderline) + abnormal CO2 or HCO3
pH pCO2 HCO3 Common
Causes
Normal values 7.35 -7.45 35-45 22-26
Respiratory Normal Hypoventilation
acidosis ⇩ ⇧ such as
respiratory
depression
(drugs, CNS
trauma), COPD,
pneumonia
Respiratory Normal Hyperventilation:
alkalosis ⇧ ⇩ anxiety, pain,
PE, mechanical
ventilation
Metabolic Normal DKA, shock,
acidosis ⇩ ⇩ renal failure,
excessive
diarrhea
Disclaimer: This study guide is intended for educational purposes only.
Metabolic Normal Prolonged
alkalosis ⇧ ⇧ vomiting, NGT
suction, Na
bicarb overdose,
Cushing’s
disease
Anion gap
● The difference between positively charged ions (cations) and negatively charged ions
(anions) in the blood
● Indirect measure of acidosis severity (but it does not help in determining the causes)
● Normal: 8-16
● The larger the gap, the more severe the acidosis
COPD
● A group of diseases that obstruct airflow including chronic bronchitis, emphysema, and
asthma and result in airway remodeling
● The most common respiratory disorder in adults
● Non-curable and progressive; goal is to prevent exacerbation and slow progression
● High flow oxygen can knock out the respiratory drive in COPD and the CO2
retention can lead to hypercapnic respiratory failure
● Risk factors
○ Smoking, air pollution, occupational chemicals, infection
○ Alpha-1 antitrypsin deficiency: genetic disorder with a lack of protein produced by
the liver
Chronic bronchitis Emphysema
● Chronic inflammation of the ● Alveoli damages
bronchi ● Little sputum, thick gray/white
● Chronic productive “wet” cough ● Air trapping, retains CO2
with pus or blood streaked ● Barrel chest (enlarged alveoli)
● Increased infection risk ● Use of accessory muscles
● Drive for breath is rise in CO2 ● Drive for breath is low O2
● “Blue bloater” ● “Pink puffer” (due to CO2)
● Tends to develop Cor Pulmonale ● Tends to lead to hypercapnic
(right sided heart failure due respiratory failure
chronic hypoxemia)
● Treatment
○ Bronchodilator
■ Short acting (rescue): Albuterol
■ Long acting: salmeterol, formoterol
■ S/E: tremor, hypokalemia, headache, dizziness, tachycardia
○ Anticholinergics
Disclaimer: This study guide is intended for educational purposes only.
■ Smooth muscle relaxant of airways to prevent tightness; longer acting
■ Ipratropium (Atrovent)
■ S/E: urinary obstruction, headaches, restlessness, bronchospasm
○ Corticosteroids
■ Inhaled or oral
■ Treat and prevent inflammation
■ Fluticasone/Salmeterol
■ Rinse mouth after to prevent thrush
○ Methylxanthines (theophylline)
■ Bronchodilator effects
■ Used during exacerbation
■ Narrow therapeutic range with potential for toxicity (esp in elderly)
● Nausea, irritability, tachycardia, seizures
■ Decrease effects of lithium and dilantin
● Patient education
○ Pursed lip breathing (helps with getting rid of CO2)
○ Monitor for changes in mucus color (sign of infection)
○ Proper use of inhaled medications
○ Smoking cessation
○ Energy conservation and exercise
○ Recognize symptoms for exacerbation
○ High protein, high calorie diet (burns calories rapidly and the flattened diaphragm
can cause early satiety)
Asthma
● A receive airway disease with narrowing of the bronchioles due to inflammation triggered
by allergens
● Long term effect: narrowed airway, increased resistance, increased mucous, decreased
oxygen saturation
● Status asthmaticus: life threatening asthma attack that is refractory to standard therapies
● S/S: wheezing (esp expiratory), non-productive coughing (esp at night), dyspnea and
chest tightness, use of accessory muscles
● Treatment
○ Requires daily maintenance for prevention of emergencies
○ Avoids triggers, stay hydrated and use humidifier (helps to thin and clear mucus)
○ Maintenance medications
■ Long acting bronchodilators
■ Beta agonists
■ Leukotriene receptor antagonist (Singulair)
● Not for acute attacks
● S/E: liver injury, headache, dizziness, GI distress
● Rescue medications
○ Short acting bronchodilators
○ Theophyllines
● Patient educations
Disclaimer: This study guide is intended for educational purposes only.
○ Smoking cessation, preventing and avoiding asthmatic attacks, flu and
pneumonia vaccine
○ Peak flow meter
■ Measures maximum speed of air expelled from the lungs
■ Do it two times in the morning
■ Helps to identify exacerbations early
● Green indicator: good
● Yellow indicator: some inflammation; more medication or call the
doctor
● Red indicator: airway closing; go to ED
Pneumonia
● Lung infection that impairs gas exchange due to consolidation
● Can be caused by
○ Bacteria: streptococcus is the most common; meningococcal is most dangerous
and requires isolation
○ Viral: flu
○ Fungus: difficult to treat
● Can be categorized by
○ Community acquired (CAP)
○ Hospital acquired (HCP)
○ Ventilator associated (VAP)
○ Aspiration pneumonia
● S/S
○ Fever, chills
○ Dry or productive cough
○ SOB
○ Fatigue
○ Elderly: confusion, weakness, anorexia
● Treatment
○ Antibiotics, oxygen, humidification, fluids, moderate activity
Tuberculosis
● Highly contagious airborne transmitted disease; needs to be reported to the public health
● High risk population: immunocompromised, HIV, homeless, group homes (with poor
ventilation)
● Can be active (transmissible) or latent (exposed but not transmissible)
● Diagnosis
○ Skin or blood test
■ PPD, quantiferon
■ A positive PPD or quantiferon indicates exposure to TB but does not
tell you whether it is active TB or not
○ Active TB
■ CXR with infiltrates
■ Positive AFB (acid fast bacilli) sputum
Disclaimer: This study guide is intended for educational purposes only.
● S/S
○ Hemoptysis or blood streaked (but not all active TB have productive cough)
○ Fever, chills
○ Night sweats
○ Anorexia, weight loss
● Treatment
○ Combination of Isoniazid, Rifampin, Pyrazinamde
○ S/E: nausea, anorexia, fatigue, orange urine from rifampin
Pneumothorax
● Accumulation of air in the pleural space that causes positive pressure and pushes on the
lung making it collapse
● Types of pneumothorax
○ Open: from gunshot, stab wounds
○ Closed: from medical procedures (bronchoscopy, mechanical ventilation), rib
fracture
○ Spontaneous: common in those with Marfan syndrome
● S/S
○ Sudden SOB
○ Pleuritic chest pain
○ Tachycardia, hypotension, tachypnea, hypoxemia
○ Diminished to absent breath sounds on affected lung
○ Pallor, cyanosis
○ Anxiety
● Tension pneumothorax
○ Occurs when injured tissue forms a one-way valve or flap, enabling air to enter
the pleural space and preventing it from escaping naturally
○ Can cause a mediastinal shift pushing the heart, great vessels, trachea, and
lungs toward the unaffected side of the thoracic cavity (tracheal deviation)
■ S/S: severe respiratory distress, cyanosis, muffled heart sounds, cardiac
arrest
● Treatment
○ High flow oxygen
○ Thoracentesis
○ Chest tube
● Chest tube
○ A plastic tube that is inserted to drain fluid or air in the pleural space so that the
collapsed lung(s) can re-expand.
○ Collection chamber: collects air or fluid from the pleural space
○ Water seal chamber
■ Acts as a one way valve that allows air to exit the chest but prevents air
from returning to the pleural space
Disclaimer: This study guide is intended for educational purposes only.
■ fluid level must be at 2 cm at all times (acts as a water manometer for
measuring intrathoracic pressure) --> therefore, water level rises & falls
with respiration
■ intermittent bubbling in water seal is expected for pt with pneumothorax
and will be resolved once the lung is re-expanded.
■ however, if there is a continuous air bubbling, it indicates an air leak
● Ask the patient to take a deep breath in and out, or cough to
assess for bubbling
○ Suction chamber
■ chest tube can be drained by gravity or by wall suction
■ The amount of suction is controlled by the chest drainage system, not the
suction source
■ -20 cm water is the standard suction level (the lower the water
measurement, the lower the imposed suction and vice versa)
■ How to tell if suction is on
● Dry system: dial set on “-20 cm” and the “orange float” is visible
● Wet system: gentle bubbles in the suction chamber (need to make
sure to keep water filled)
○ Nursing considerations
■ Secure all connections, check for kinks, dependent loops
■ Assess insertion site for any redness
■ Assess respiratory status, medicate for pain to prevent splinted breathing
and/or atelectasis
■ Check for subq emphysema
■ Always keep the unit below chest level
■ Unit must be in upright position at all times
■ Call for assistance with ambulation
■ Notify MD if output changes from serous to bloody or there is more than
70ml of blood output per hour
■ Only clamp a chest tube when
● It is ordered by MD to mimic the absence of chest tube before
removal
● Replacing the collection system
● Trying to determine the source of an air leak
○ Chest tube dislodgement
■ Ensure patient is stable
■ Cover the site with dressing tape on 3 sides to allow air to escape with
expiration
■ Placed on oxygen as needed
■ Notify MD
Pulmonary embolism
● Obstruction of the pulmonary vascular bed
Disclaimer: This study guide is intended for educational purposes only.
● VTE is the most common cause; others include plaque from fracture (esp long bone,
pelvic) or trauma, IV air injection
● Virchow’s Triad (risk factors)
○ Hypercoagulability
■ History of PE/DVT
■ Malignancy
■ Oral contraceptives
■ Sickle cell anemia, thrombophilia
○ Venous stasis
■ Age > 40
■ Prolonged immobility
■ Obesity, diabetes, stroke, CHF, MI, A fib
○ Vessel wall damage
■ Central lines
■ Chemotherapy
■ Infections, rheumatic disease
■ Surgery, trauma
■ Atherosclerosis
● S/S
○ Pleuritic chest pain, dyspnea, hemoptysis, hypotension
○ Impending sense of doom (unique to PE)
● Treatment
○ Give oxygen (high flow)
○ Anticoagulant (Heparin bolus and drip, Lovenox, or oral Coumadin or DOAC)
■ Heparin drip is the gold standard treatment
○ tPA or surgical intervention (IVC filter, embolectomy) may be indicated for large
clots
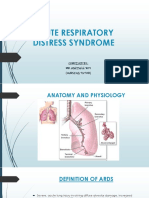
Acute respiratory distress syndrome (ARDS)
● Non-cardiogenic pulmonary edema causing accumulation of fluid in the alveoli/interstitial
space leading to impaired gas exchange
● Risk factors
○ Sepsis (common cause)
○ Pneumonia (esp aspiration)
○ Lung trauma
○ Severe pancreatitis
● S/S
○ Tachypnea, labored breathing (remember change in RR is usually the first sign of
distress; upper limit of normal RR is 16)
○ Acute dyspnea, hypoxemia
○ Tachycardia, hypotension
○ Diffuse crackles/rhonchi
○ Anxiety, restlessness
● Treatment
Disclaimer: This study guide is intended for educational purposes only.
○ Follow ABC’s
○ Support with oxygen (high flow, BiPAP, ventilator)
○ Bronchodilators, diuretics, corticosteroids
○ Call RRT and transfer to ICU for higher level of care
Disclaimer: This study guide is intended for educational purposes only.
Neurological System
Anatomy
● Central nervous system (CNS)
○ Includes the spinal cord, brain (cerebrum, cerebellum, brainstem)
○ Cerebellum
■ Frontal lobe: intellectual functions, speech production
■ Temporal lobe: hearing, speech perception, memory
■ Parietal lobe: sensory integration
■ Occipital lobe: vision, vision perception
○ Cerebellum
■ Coordination, equilibrium
○ Brainstem
■ Cranial nerves
■ Pain, temperature, touch, pressure
■ Pons: motor & sensory, regulates breathing pattern
■ Medulla oblongata: control of ventilation and heart rate
○ Spinal cord
■ Extension of the CNS
■ Neural transmission between periphery and brain
○ Meninges
■ Dura mater: outer layer; fibrous and tough
■ Arachnoid mater: middle layer
■ Pia mater: inner layer that covers the brain surface; thin and delicate
● Peripheral nervous system (PNS)
○ Cranial nerves
■ 12 pairs
■ Communication between the brain and head, neck, and senses
○ Peripheral nerves
Definitions
● Aphasia: loss of ability to understand (receptive) or express speech (expressive)
● Babinski reflex: stroke the heel to great toe, then continue under the the remaining toes;
when positive, the great toe will dorsiflex (bends backwards) and the other toes fan open
● Choreoathetosis: irregular involuntary movements that may involve the face, neck, trunk,
extremities or respiratory muscles
● Hemiparesis: muscle weakness on one side of the body
● Hemiplegia: paralysis of one side of the body
● Todd’s paralysis: a temporary paralysis or weakness that can occur after seizures
Diagnostic tests
● Skull and spine X-rays
● CT & MRI of brain, spine
● MRA: an angiogram that looks at the blood flow in the heart and other soft tissues;
needs contrast and NPO for 4-8 h prior
Disclaimer: This study guide is intended for educational purposes only.
● Cerebral angiography: a serial X-rays that use contrast to look at intracranial and
extracranial blood vessels
● Electroencephalogram (EEG): to diagnose areas of the brain that causes seizures
● Electromyography (EMG): to diagnose peripheral nerve disease and myopathic
conditions by inserting tiny needles into a muscle and record via electrodes
● Myelography: to detect lesions in the spine via X ray with contrast dye injected into the
subarachnoid space
● Lumbar puncture:
○ to obtain CSF to rule out infection or to diagnose neurological conditions
○ Invasive procedure requiring informed consent
○ Position: sits with the back arched or in the recumbent position with the knees
flexed
○ A spinal needle is inserted into the subarachnoid space at L3-4 or L4-5 to collect
CSF (which should be clear in color)
○ Post-procedure
■ Lay flat for 6-8 h
■ Monitor for headaches (especially headaches that increases when
standing up and decreases when laying down; a classic sign of CSF
leaking from LP site)
■ Monitor vitals, monitor neuro status
■ Increase fluid intake
Increased intracranial pressure (ICP)
● Normal ICP 0-15 mmHg
○ Must be treated if sustained pressure of 20-25 mmHg
● Factors that affect pressure
○ Brain (fills 80% of cavity)
■ A change in brain tissue (brain tumor for example)
○ Blood (fills 10%)
■ Excess of blood volume
○ CSF (fills 10%)
■ Excess fluid volume
● S/S
○ Early signs: restlessness, confusion, change in LOC, headaches
○ Late signs: pupil changes, posturing, hemiparesis, Cushing’s Triad
■ Cushing’s Triad (late sign)
● Hypertension (with an increase only in the SBP)
● Widening pulse pressure (the difference between SBP & DBP and
is greater than 100)
● Bradycardia
■ Posturing
● Abnormal posturing can indicate CNS damage
● Decerebrate (extensor posturing)
○ Extends upper extremities from the body
Disclaimer: This study guide is intended for educational purposes only.
○ Adduction and extension of arms
○ Pronation and flexion of feet
● Decorticate (flexor posturing)
○ Brings upper extremities to the middle of the body
○ Adduction and flexion of arms
○ Rotation of legs internally
○ Flexion of feet
● Brain herniation
○ Increased ICP can displace brain tissues through openings in rigid intracranial
barriers
○ Respiratory changes is a sign of impending brain herniation
○ Fixed, dilated pupils indicates temporal lobe herniation into the brain stem
● Treatment
○ Lower BP: BP meds, diuretics (usually mannitol)
○ Lower temperature (to conserve energy and oxygen)
○ Elevated HOB
○ Give oxygen
○ Sedation, pain relief (decrease stimuli that can increase ICP)
○ Steroids (reduce swelling)
○ Surgical intervention
Traumatic brain injury (TBI)
● Could be injury to scalp, skull, or brain
● Scalp injury
○ Can lead to lots of bleeding
● Skull injury
○ Linear skull fracture
■ No worrisome unless vessels compromised
○ Basilar skull fracture
■ Frontal and temporal lobes
■ Raccoon eyes (periorbital ecchymosis) & Battle’s sign (mastoid area or
behind the ears bruising)
■ Meningeal tears, cerebrospinal fluid leak increases risk of brain infection
○ Depressed skull fracture
■ Medical emergency
■ Brain bruising and possible bone fragments in brain
○ LeForte fractures
■ Severe facial bone trauma
■ Drainage from nasal cavity or ears can be cerebrospinal fluid
■ Hemotympanum (blood behind eardrum)
● Injury to cranial nerves for vision, hearing, smell, facial movement
● Brain injury
○ Concussion
■ High forced blow to the body where the brain impacts the skull
Disclaimer: This study guide is intended for educational purposes only.
■ May have LOC <5 min, amnesia, clear CT/MRI
○ Contusion
■ Bleeding under skin
■ May have brief to permanent LOC, permanent neurological damage with
extent dependent on location and severity of injury
○ Contusion-laceration
■ May have brief to permanent LOC with bruising and damage to brian
tissue
■ Can result in vegetative state, brain swelling, Hematomas, ICP
● Treatment
○ Extent of injury is measured with the Glasgow Coma Scale
■ The lower the score, the more extensive the injury
○ Frequent neurological assessments
○ Pain and agitation management
○ Nutrition (enteral feeding)
Meningitis
● Infection or inflammation of the meninges that cover the brain and spinal cord
● Caused by bacterial or viral infection (following surgery, head injuries, or ear infections)
● Bacterial meningitis
○ A medical emergency
○ Can progress quickly and requires prompt treatment
○ Caused by streptococcus pneumoniae or meningococcal B in 18-50 yr
○ S/S
■ Headache, elevated ICP, AMS, facial paralysis, deafness
■ Positive Brudzinski sign: hips and knees flex when head is flexed
■ Positive Kernig’s signs: cannot extend leg when lying flat and hip at 90
degree angle
■ Nuchal rigidity (neck stiffness)
■ Opisthotonos: severe hyperextension and arching of the back due muscle
spasm
○ CSF from LP: cloudy, milky white, presence of neutrophils, decreased glucose
level, marked elevation in opening pressure, positive cultures
○ Treatment
■ Droplet precaution required for 24 hours until the causative
pathogen is identified
■ Monitor neuro status, seizure precaution
■ Analgesics, antipyretics, antibiotics
● Viral meningitis
○ Less serious
○ 90% of cases caused by enteroviruses
○ S/S
■ Headache, rash, weakness, fever, myalgia, nausea, photophobia, neck
stiffness
Disclaimer: This study guide is intended for educational purposes only.
○ CSF from LP: clear, <500 WBC, normal glucose, normal/slight elevation in
opening pressure, negative culture
○ Treatment
■ Provide a quiet, dark environment
■ Analgetisc, antipyretics, antivirals
Seizures
● Abnormal, sudden and excessive uncontrolled discharge of cerebral neurons in the brain
● Epilepsy: defined as two or more unprovoked seizures greater than 24 hours apart
● Seizure types
○ Partial seizures
■ Also called "Focal Seizures"
■ Seizures involving one area of the brain
■ Two subtypes:
● Simple partial = partial seizure without impaired awareness
○ Patient is aware of what's happening during the seizure
● Complex partial =partial seizure with impaired awareness
○ Loss of consciousness (LOC) during seizures
○ Often associated with aura and postictal symptoms
○ Can become generalized seizures
○ Generalized seizures
■ Involves bilateral brains so symptoms are present on both sides of the
body
■ Types
● Absence (petit mal): brief unconsciousness
● Myoclonic: isolated jerking movements
● Clonic: repetitive jerking movements
● Grand Mal (generalized tonic-clonic): unconsciousness,
convulsion, rigidity
● Atonic seizure: “drop attacks”, sudden loss of muscle control;
common in children
○ Status epilepticus
■ A seizure that lasts more than 30 mins without a seizure free/recovery
period
■ Is a neurological emergency
■ Due to fever, infection, medication withdrawal
● Management
○ Airway and safety are the priority
■ Side-lying position, protect the head, loosen tight clothing, no restraints,
do not put anything in the mouth
■ Place on oxygen, monitor O2 sat
■ Observe and assess patient before, during, and after seizure
■ Medications
● For active seizures: Lorazepam (Ativan), diazepam (Valium)
Disclaimer: This study guide is intended for educational purposes only.
● For prevention: phenytoin (Dilantin), carbamazepine (Tegretol),
valproate (Depakote), levetiracetam (Keppra). Lamotrigine
(Lamictal)
○ Should not take antacid within 2 hours of some
anti-epileptic meds (phenytoin)
Stroke
● Infarction or death of a portion of brain tissue
● Blood flow interference for > 4-6 min can cause tissue death
● Types
○ Ischemic (87%)
■ Blockage of blood flow
○ Hemorrhagic (13%)
■ Bleeding due to ruptured vessel
○ Transient Ischemic Attack (TIA)
■ Temporary with mild symptoms (usually gone in 24 h)
■ May not shown on scans but is a warning sign of impmending stroke
● Risk factors
○ Atrial fibrillation and uncontrolled HTN are the two main risk factors
○ HLD, Diabetes, use of blood thinners, hormone replacement therapy, birht control
pills
○ Obesity, smoking, use of alcohol and illicit drugs
● BE FAST
○ Balance loss
○ Eyesight changes
○ Face drooping
○ Arm weakness
○ Speech difficulty
○ Time to call 911
● Assessment
○ Time is brain: immediate recognition of changes is critical and therefore, a
baseline assessment must be done at every shift for comparison
○ NIH stroke scale
■ A measurable set of data on the severity of neurological deficits
■ The higher the score, the greater the severity
● Intervention
○ Time is brain: call a code stroke or alert
○ Last known normal
○ Quick assessment: airway, breathing, circulation, vital signs
○ Neuro exam: LOC, pupils, motor strength, NIH
○ Rule out hypoglycemia that might mimic stroke
○ Stroke education JACHO core measures
■ IV thrombolytic therapy
■ DVT prophylaxis
Disclaimer: This study guide is intended for educational purposes only.
■ Antithrombotic medication
■ Discharge on statin, anticoagulant
■ Stroke education (recognize stroke symptoms, smoking cessation,
modifiable lifestyle risk factors)
■ Rehab assessment
Disorders of motor function
● Multiple Sclerosis (MS)
○ Common in young female Caucasians
○ Progressive deterioration of myelin sheath leading to scarring and plaque
formation causing debilitating neuro-sensory symptoms
○ Remissions and relapse are common
● Parkinson’s Disease
○ Degeneration of dopamine (a neurotransmitter that transmits impulses)
○ Signs
■ Tremor: “pill-rolling” of fingers, starts in upper extremities
■ Muscle rigidity: bent posture
■ Dyskinesia: shuffling gait, bradykinesia, hypokinesia, mask-like, reduced
blinking and swallowing
■ Postural instability: late in disease; unbalanced, dementia
● Amyotrophic Lateral Sclerosis (ALS)
○ Progressive and degenerative disease affecting motor neurons in the brainstem
and spinal cord
○ Lead to atrophy and eventually immobile, dysphagia with drooling, dysphonia,
and total care
○ But cognition, bladder/bowel sphincter muscles, sensation, extraocular eye
movements are unaffected
○ Typical cause of death: pneumonia or respiratory failure
● Myasthenia Gravis (MG)
○ An acquired autoimmune disease that spreads through the musculature from the
brainstem, through the truncal area, and into extremities
○ Muscle weakness and increased fatigue with activity, lessons with rest
○ Ocular and facial involvement: ptosis (drooping of eyelids), diplopia (double
vision), ocular palsy, mask-like features
○ Respiratory failure can occur when the respiratory muscles are affected leading
to dyspnea and hypoventilation; intubation and ventilator can be expected
○ Plasmapheresis may be performed to filter the autoantibodies
Disclaimer: This study guide is intended for educational purposes only.
Musculoskeletal System
Osteoarthritis (OA)
● Progressive, non-inflammatory degenerative joint disease
● Joint cartilage breaks down from “wear and tear” and is asymmetrical that it affects the
“most used” joints (knees and hips)
● The most common form of joint disease and leading cause of progressive
disability
● Pain increases with movement and relieved with rest
○ Often more stiff in the morning
● Common in women in the 40s-50s
● Pain management
○ Acetaminophen is the first line
○ Followed by Aspirin, NSAID, Duloxetine/Cymbalta
○ Steroid injections
Rheumatoid Arthritis (RA)
● Autoimmune, inflammatory response and affects the body systemically and bilaterally
● Targets the small joints of hands and feet first (does not affect the spine)
● Pain increases with rest and relieved with movement
○ Stiffness may last from 1 hour to all day; more intense in the morning
● Extreme pain, exacerbations and remissions
● Can progress to deformed joints: spindle-shaped fingers, swan-neck deformity
● Common in women >20 yr
● Treatment
○ Disease-modifying antirheumatic drugs (DMARDs)
■ Methotrexate,
■ Start early to slow progression
○ Biologic response modifiers
■ To target molecules and cells involved with chronic inflammation
○ NSAIDs, Aspirin
■ Decreases inflammation but does not slow down progression
○ Steroids
■ Reduces inflammation but cannot be used constantly
Osteoporosis
● A reduction in bone density, when bone mass loss exceeds formation
○ At high risk of falling from bone breakdown
● Bone mass peaks at 30 yrs and decline after that
● Risk factors
○ Women at higher risk due to menopause
■ Loss up to 15% due to decreased estrogen
○ Malabsorption of calcium and vit D due to
■ Alcoholism, bariatric surgery, anorexia, Cushing’s syndrome,
hyperparathyroidism
Disclaimer: This study guide is intended for educational purposes only.
○ Smoking
○ Medications: thyroid meds, anticonvulsants, lasix, chemo, steroids, PPI (>1 yr
use)
● DEXA scan: gold standard for diagnosing
● S/S
○ Hip fracture can be the first sign with high mortality
○ Spinal compression fractures lead to “widow's hump”
● Treatment
○ Calcium rich diet (soy products), vit D supplements, hormonal replacement
therapy
○ Weight bearing exercise
○ Compression fracture surgeries
Fractures
● A break or disruption in the continuity of the bone
● Open fractures
○ More emergent
○ Culture before cleansing
○ Irrigate
○ Apply sterile dressing
● S/S
○ Pain, edema, deformity, spasm, ecchymosis at fracture site
● Treatment
○ Immobilize with splint, bandage
○ Pain control
○ Apply ice
○ Neurovascular assessment: circulation, sensation, motion
○ Surgical repair if indicated
● Traction
○ Used to restore bone alignment and length and reduce pain and spasm
○ When traction is applied, ensure patient’s body and the fracture bone is
aligned
○ Pain management (a priority), neurovascular assessment, prevent pressure
injuries
○ Always maintain the prescribed line of pull
○ Always maintain continuous pull unless ordered as intermittent (except for Buck’s
traction)
○ Prevent friction that will interfere with line of pull
○ Identify and maintain counter traction
Compartment Syndrome
● Is a medical emergency
● High pressure building up inside an enclosed muscle space in the body
● Dangerously high pressure (>30 mmHg) in the compartment can impede blood flow and
Disclaimer: This study guide is intended for educational purposes only.
result in tissue death/nerve injury
○ Permanent muscle/nerve damage can occur within 6 hours if pressure is not
relieved
○ Immediately remove whatever is restricting the blood flow when compartment
syndrome is suspected
● Causes
○ Usually results from bleeding or swelling after an injury
○ Crush injuries, burns, tight bandaging, prolonged compression of a limb, blood
clot in the arm/leg
● S/S (6 P’s)
○ Pain distal and disproportionate to the injury is the first sign
○ Paresthesia, pallor, pressure, paralysis, pulselessness
○ Calf is most commonly affected body part
● Management
○ Remove whatever is restricting the blood flow
○ Keep in neutral position (elevation can decrease arterial blood flow)
○ Do not perform passive range of motion (as it can increase pressure)
○ Fasciotomy: cutting into the affected area to relieve pressure
○ Neurovascular assessment
Rhabdomyolysis
● Excessive breakdown of muscle tissues leading to renal failure with myoglobinuria
● Due to muscle trauma, excessive muscle activity (status epilepticus), strenuous exertion
(marathon running)
● S/S: muscle weakness, tenderness, swelling, dark, reddish brown urine
● Treatment
○ Treat underlying cause
○ IVF, diuretics
○ Dialysis
Bone cancers
● Can be from metastasis from other cancers (common in older adults) or from primary
bone cancers (common in age 10-30)
● Monitor closely for severe hypercalcemia and pathologic fractures
● Primary bone cancers
○ Osteosarcoma
■ Most common, most fatal
■ Common in teens and young adults
■ Usually in fast growing long bones
■ Painful and edematous
○ Ewing’s sarcoma
■ Least common
■ Common in children and young adults of male sex
■ Can be in any bone or soft tissue
Disclaimer: This study guide is intended for educational purposes only.
■ Painful and edematous
Disclaimer: This study guide is intended for educational purposes only.
Pain Management
● Pain is subjective; “pain is what patients says it is”
● Self-reporting by patient is gold standard
○ Non-verbal signs of pain when self-reporting is not achievable
■ Moaning, grimacing, guarding
■ Hyperactive or hypoactive
● Types of pain
○ Acute pain
■ < 6 month
■ Result of injury, disease, surgery
■ Curative
○ Chronic pain
■ > 6 month
■ Result of chronic/terminal illness
■ Not curative
○ Nociceptive pain
■ Mechanical or chemical stimulation of PNS
■ Visceral pain: deep internal organ pain
■ Somatic pain: superficial or cutaneous tissue pain
○ Neuropathic pain
■ Nerve pain
■ From Diabetic neuropathy, phantom limb pain, neuralgia
● Assessment
○ Initial assessment
○ Re-evaluation after pain meds
■ Reassess 1 h after oral meds
■ Reassess within 15-30 min after IV meds
● Route of administration
○ Oral
○ Intravenous
○ Intramuscular: least preferred due to shorter duration, and poor absorption
○ Subcutaneous: slower to absorb, peak effect is not as strong; subcutaneous PCA
pump can be used via this route
○ Epidural and subarachnoid
■ Used to administer pain med via the spine by bolus or an implantable
pump
■ Epidural lasts 5-16 hours whereas subarachnoid lasts up to 36 h
● Transdermal: fentanyl patch; takes 12- 24 h to be fully effective so patient may
require additional analgesic during this period
● Medications
○ Non-opioids
■ Acetaminophen
● Max dose is 4g/day or 2.4g/day for those with liver disease
● Norco, Tylox, and Vicodine also have Tylenol in them
Disclaimer: This study guide is intended for educational purposes only.
■ Acetylsalicylic acid (Aspirin)
● For inflammatory pain
● Affects platelet function and increased risk of bleeding especially
GI bleed
● Take with food or antacid
■ Non-steroidal anti-inflammatories (NSAID)
● Reduce pain by inhibiting prostaglandin synthesis
● Monitor for GI bleed and renal insufficiency
● Take with food or milk
● Celecoxib: a COX-2 inhibitor and affects the GI system less but
has cardiac risk
■ Opioids
● Bind to opioid receptors in the CNS
● Treat nociceptive pain
● Morphine is the gold standard
● Others include: codeine, hydrocodone, oxycodone, meperidine,
hydromorphone
● S/E: respiratory depression, nausea, constipation (an expected
side effect)
● Naloxone (Narcan): antidote for opioids
○ Via IV push (0.1-0.4 mg over 2-3 min)
Disclaimer: This study guide is intended for educational purposes only.
Gastrointestinal System
Assessment
● Abdomen
○ Orders: inspection → auscultation → percussion → palpation
○ Inspection
■ First step
■ Any distention or convex?
■ Check for any discoloration or bruising
● Cullen’s sign: bruise around the umbilical area
● Grey Turner’s sign: bruise in the lower abdomen
● These bruising can indicate a massive GI bleed
○ Auscultation
■ Second step
■ Standard of practice is 5 minutes in each quadrant
■ Abnormal bowel sounds: absence, hyperactive, high pitched sounds (can
indicate an obstruction)
■ Right lower quadrant is best location to listen if bowel sounds are distant
or absent
○ Percussion
■ Third step
■ Helps to identify borders of the liver and spleen
■ Tympany sounds are heard over stomach and intestines
○ Palpation
■ Last step
■ Abnormal: tenderness, firm, mass
■ Rebound tenderness
● Typical with peritonitis
● deeply palpate the abdomen and hold it down for 5 seconds, then
rapidly release the pressure. Ask the patient if pressing down or
releasing caused more pain. Rebound tenderness means pain is
higher when pressure is released.
● S/S
○ Pain:
■ referred pain is common in GI system
■ Any pain between the navel to the nose should be investigated
further to rule out GI vs cardiac causes
○ Anorexia, weight loss
○ Nausea, vomiting
○ Constipation, diarrhea
○ Hematemesis: vomiting up blood
○ Hematochezia: passing fresh blood per rectum (from lower GI)
○ Melena: tarry, black stool (from upper GI)
● Diagnostic tests
Disclaimer: This study guide is intended for educational purposes only.
○ Upper GI series: X ray with use of contrast to examine the GI tract and can
identify SBO
○ CT: infection or ductal dilation
○ Upper endoscopy: same as gastroscopy; examines upper GI (esophagus,
stomach, and upper duodenum)
○ ERCP: assess and treat biliary and pancreatic ducts for stones and strictures
○ All GI procedures require
■ NPO, consent, preparation, verification of allergies
GERD
● Backflow of acid and stomach contents into the esophagus causing heartburn due to an
incompetent sphincter
● Causes: obesity, hiatal hernia, gastroparesis, smoking, pregnancy
● S/S: heartburn, indigestion, hoarse voice (HCL acid can damage vocal cords), upper
respiratory symptoms (some may develop asthma due to possible damage to the
bronchus and trachea)
● Barrett’s Esophagus
○ A condition in which the lining of the esophagus changes, becoming more like the
lining of the small intestine rather than the esophagus.
○ Due to chronic reflux and can become precancerous
● Treatment: H2 blockers, PPI, Nissen fundoplication (the top portion of the stomach is
wrapped around the esophagus to prevent reflux of acid)
Peptic ulcers
● Erosion of mucosa in any part of the upper GI: esophagus, stomach, duodenum
● Causes
○ H. pylori (gram negative bacteria in the stomach wall)
○ Use of NSAIDS
○ Stress ulcers (develop with long term hospital stays, trauma, extensive surgeries)
● Type of ulcers
Gastric ulcer Duodenal ulcer
● More common in women ● Most common type (80%)
● Associated with an incompetent ● More common in young men
pyloric sphincter ● Higher chance of perforation as
● Commonly seen with COPD symptoms not as apparent
● Pain 1-2 h after eating ● Pain at night or 2-4 h after
● In epigastric area or the back eating
● Pain with an empty stomach if ● Pain comes and goes
erosion through the mucosa
● Perforated ulcer
○ A perforated ulcer causes 90% of GI bleeds
Disclaimer: This study guide is intended for educational purposes only.
○ Is an emergency due to hemodynamic instability
○ S/S
■ Changes in vitals
■ A loss of 25% of circulating volume (about 1500 ml) of the I&Os
○ Treatment includes surgical repair, antibiotics, IV fluids, NGT, pain meds
● Treatment
○ 95% heal in 3 months with treatment but 70% re-occur within one year
○ Diet: avoid milk, caffeine, carbonated beverages
○ Lifestyle: avoid NSAIDS, aspirin based medications, smoking
○ Medications
■ Antibiotics (metronidazole) for H pylori
■ Antacids
● Neutralizes acid and provide pain relief but does not treat the ulcer
■ PPI
● Reduce production of HCL
● Short term use with 2 weeks on, 2 weeks off
○ PPI can dramatically reduce HCL which is the GI main
defense mechanism against bacteria
○ Long term use can alter absorption of calcium leading to
osteoporosis
○ May also increase the risk of C diff
● Ends with “-prazole”: Pantoprazole (Protonix), Lansoprazole
(Prevacid), Omeprazole (Prilosec)
■ H2 blockers
● Used as “in between” treatment to take a break from a PPI
● Ends in “-dine”: Famotidine (Pepcid), Ranitidine (Zantac)
GI bleed
Upper GI Lower GI
● Esophagus to duodenum ● Cecum to rectum
● More common ● Less common
● Due to ulcers, lesions, varices ● Due to hemorrhoids, diverticulitis,
● Higher risk of bleeds polyps, cancer
● Coffee ground or bright red emesis ● Emesis with strong odor due to mix of
● Melena (slow bleed) blood with bacteria and digestive
enzyme
● Frank blood in stool (hematochezia)
● Treatment
○ Support with IVF and blood transfusion to prevent shock
■ Monitor I & Os
■ Monitor for acute tubular necrosis
Disclaimer: This study guide is intended for educational purposes only.
○ Stop the bleed via endoscopy or surgery if indicated
■ Catuery, sclerotherapy, variceal ligation, balloon tamponade, embolization
○ NPO, NGT, oxygen
○ Monitor and replete electrolytes
○ Medications
■ H2 blockers, PPI, sandostatin (vasoconstriction in the gut)
Irritable bowel diseases (IBD)
● Chronic inflammation of the GI tract
● Increases risk for colon cancer; regular screening recommended
Crohn’s Disease Ulcerative Colitis
● Affects the entire bowel ● Left colon
● Cobblestone bowel ● Starts at rectum and ascends
● Lesions separated by normal tissue ● Continuous segments affected
● Involves all layers of the bowel ● Involves the mucosa layer
● No rectal bleed ● Shallow ulcerations
● Bloody diarrhea
● Immunosuppressants, steroids, ● Aminosalicylates (ASA, mesalamine,
antimicrobials, Remicade (biotherapy) sulfasalazine), steroids
● Colectomy or ileostomy is only ● Colectomy or ileostomy can be a cure
palliative
● Treatment
○ Bowel rest and/or TPN during exacerbation
○ Diet: high protein, high calorie, low fat, low residual
○ Pain control
Bowel obstruction
● Partial or complete blockage in the small or large intestines
● Complete blockage is an emergency
● Causes
○ Mechanical
■ Tumors, adhesions, abscesses
○ Functional
■ Ineffective peristalsis, ileus
■ Pancreatitis, lymphoma
○ Vascular: atherosclerotic narrowing
● S/S
○ Partial obstruction: diarrhea (liquid stool leaking around the blockage)
○ Complete obstruction: not passing gas or stool
Disclaimer: This study guide is intended for educational purposes only.
Small Bowel Large Bowel
Onset Rapid Gradual
Pain Cramp-like, intermittent Low grade
Vomiting Frequent & copious Rare
Stool Feces for a short time Constipation
Abdomen Minimally increased Greatly increased
distention
● Diagnosis
○ CBC, BUN, Cr, electrolytes
○ WBC > 20,000 suggests bowel infarction or gangrene
○ Abd X ray/CT scan: dilated bowel loops
● Treatment
○ (always consider treatment choices that are least invasive and less
expensive first for the test purpose)
○ Conservative: bowel rest, IVF, TPN if prolonged bowel rest, NGT for
decompression
○ Pain control, antiemetics, monitor and replete electrolytes
○ Hemodynamic monitoring
○ Large bowel obstructions are likely to need surgery
● Perforation
○ Bowel obstructions can cause increased capillary permeability and fluid shift into
the third space (peritoneum)
○ Infection of the ascitic fluid can lead to peritonitis
○ S/S: rebound tenderness, hypotension, tachycardia, low potassium, elevated
BUN, elevated Cr
Acute Pancreatitis
● Inflammation of the pancreas which triggers release of pancreatic enzymes and cause
auto-digestion of the pancreas
● Causes
○ Alcohol use (#1 reason)
○ Biliary disease, gallstones
● S/S
○ Severe abdominal pain
○ Rigid and distended abdomen, nausea, hypoactive bowel sounds, steatorrhea
(increased fat in stool due to malabsorption)
○ Low grade fever, hypotension, respiratory impairment
○ Labs
■ elevated lipase and decreased calcium
Disclaimer: This study guide is intended for educational purposes only.
● Lipase breaks down fat and release free fatty acids that bind to
Ca++ → decreased calcium
■ elevated LFTs, decreased total protein
● S/S of pancreatic hemorrhage
○ Cullen’s sign: bruising around the umbilical cord; indicates intra-abdominal bleed
○ Turner’s sign: discoloration of the lower abdomen or left flank; indicates
retroperitoneal bleed
● Treatment
○ Pain control, NPO, bowel rest, NGT if indicated
○ IVF, TPN for nutrition support, replace electrolytes, monitor glucose
○ Low fat, low protein diet upon refeeding
○ For patients with alcohol use, monitor for withdrawal
■ CIWA assessment: score >10 requires intervention based on severity
■ Ask the when the last drink was
■ Symptoms can develop within 24-72 h after the last drink
■ May need to be on seizure precaution
Liver diseases
Liver circulation
● Hepatic artery: carries oxygenated blood from heart to the liver (only 25% of blood
supply)
● Hepatic portal vein: carries blood from GI tract to liver that is full of nutrient but poor in
oxygen
● Hepatic vein: carries blood that has been processed by liver back to heart
Functions of the liver
● Detox and excretion of waste products/medications
● Makes and stores bile in gallbladder
● Converts ammonia (byproduct of protein breakdown) to urea and excreted by kidney
● Stores glucose as glycogen and converts glycogen back to glucose as needed
● Converts hemoglobin to bilirubin→ bilirubin gets metabolized in liver & mixed with bile in
CBD→ gets excreted in stool & gives stool its brown color (result of mixing with bacteria
in intestines); when bilirubin is not metabolized in liver damage, bilirubin leaks into blood
vessels & causes jaundice & clay-colored stools (as there is no bilirubin to mix with
bacteria to give stool its brown color)
● makes albumin to maintain oncotic pressure
● Production of antibodies, clotting factors (PT, fibrinogen, vit K)
● Storage and release of vitamins, iron, copper
Hepatitis
● Inflammation of the liver
● Can be caused by virus (most common), bacteria, alcohol, drugs, nonalcoholic
steatohepatitis (NASH/ fatty liver)
● Can lead to
○ Decreased liver function
Disclaimer: This study guide is intended for educational purposes only.
○ Impaired bilirubin conversion & excretion → jaundice
○ Portal hypertension
● Types
Hep A Hep B Hep C Hep D Hep E
fecal/oral Blood and body fluids, IV Blood and body fluids, Must have Water
route drug abuse transfusion Hep B in borne
order to
replicate
Positive Hep B vaccine made Positive hep C antibody = Positive n/a
antibody (HA from the surface of the current or past infection Delta
Ab) = current virus that is not harmful; Antigen
or past so when a person is
infection vaccinated against Hep
B, body produces
antibodies & should have
“SURFACE antigen
positive & CORE antigen
negative” in blood test
Hep B infection will have
“CORE antigen positive &
SURFACE antigen
positive” in blood test
Acute only ● Chronic ● Chronic
(immunity ● Once infected, ● #1 cause of liver
after infection treatment is cancer &
is usually supportive transplant
lifelong) ● Can lead to
cirrhosis, liver
cancer
Vaccines available Direct acting antivirals
(DAAs)
● 90-100% cure
● 8-24 week course
● Monitor for
reactivation of
HVB when HVC is
cured
● Four stages of hepatitis
○ Prodromal
■ Last 7-10 days
■ Malaise, fever, anorexia, NO jaundice
○ Icteric
Disclaimer: This study guide is intended for educational purposes only.
■ Last 4-6 weeks
■ Jaundice (unable to convert bilirubin to bile), liver enlargement and
tenderness
■ Avoid acetaminophen or ibuprofen during this period
○ Post-icteric
■ Last 2-4 months
■ Bilirubin and enzymes return to normal
■ Energy level increases and GI symptoms subside
○ Recovery
■ Lasts 6-12 month
■ Liver needs to rest for another year
● Treatment
○ Refrain from alcohol use
○ Rest
○ Diet: high calorie, high protein, low fat
○ Monitor LFTs
○ Standard precaution (do not share items)
Acute Liver Failure
● Loss of liver function that occurs quickly (in days or weeks); prevents liver regeneration
and cellular necrosis can occur if not reversed quickly
● Causes
○ Acetaminophen overdose
○ Toxin exposure (mushroom toxicity)
○ Viral hepatitis (B or C)
● S/S
○ Jaundice, ascites, pruritus, dark urine color, pale stool color
○ Labs: elevated LFTs, elevated bilirubin, elevated PT/INR (bleeding risk),
metabolic acidosis (elevated lactate), elevated ammonia
○ Hepatic encephalopathy
■ Due to massive hepatocellular necrosis and rapid buildup of ammonia
■ Develops within 8 weeks of onset of liver failure or within 2 weeks of
onset of jaundice
■ Rapid deterioration into a comatose state
● Treatment
○ Acetylcysteine
■ Antidote for acetaminophen-induced liver failure
■ Administered within 8 hours of the ingestion
○ Critical care or transplant may be needed
● Complications
○ Metabolic alkalosis
○ Hypokalemia (to compensate for metabolic alkalosis)
○ Hypoglycemia
○ Coagulation disorders leading to DIC
Disclaimer: This study guide is intended for educational purposes only.
○ Sepsis (due to deficiency in WBC)
○ Renal failure (hepatorenal syndrome), respiratory problems (pulmonary edema)
Chronic liver failure
● A progressive destruction of liver cells leading to atrophy of the liver
● Causes
○ ETOH use (#1 reason)
○ Chronic hepatitis, infection, cirrhosis, liver cancer
● S/S
○ Early stages
■ Fatigue, weight loss, nausea, anorexia (similar to hepatitis)
○ Late stages
■ Jaundice, ascites, skin lesions (spider angiomas), peripheral neuropathy,
hepatic encephalopathy
○ Labs: decrease in albumin and protein, increase in liver enzymes
○ Portal hypertension
■ Increased pressure in the portal vein due to blockage from damaged or
scarred tissues and lead to backflow of blood into GI organs
■ Splenomegaly, ascites
■ Esophageal varices (variceal hemorrhage is a medical emergency;
protect airway, prevent aspiration, support with IVF and transfusion,
endoscopic variceal ligation)
■ Diagnosed on an ultrasound or Doppler when the hepatic venous
pressure gradient is >10-12 mmHg
■ TIPS (transjugular intrahepatic portosystemic shunt) may be placed
● Treatment
○ Supportive measures
■ Ascites: paracentesis, albumin and diuretics
■ Encephalopathy: lactulose (removes ammonia buildup in the gut; goal 2-4
BM a day), rifaximin (kills urea producing bacteria in the gut and reducing
ammonia), neomycin (binds with bacteria in the gut and neutralizes
ammonia)
■ Diet: high calorie, low fat, low sodium, low protein (due to formation of
ammonia), fluid restriction
○ Monitor for bleeding
○ Caution with sedative and narcotics (harder to detoxify)
○ Liver transplant
● Cirrhosis
○ End-stage liver disease
○ Fibrosis of liver and irreversible
Diet and nutrition
Portions (for healthy individuals)
● Complex carbohydrates: 45-65% of daily calories
Disclaimer: This study guide is intended for educational purposes only.
● Fat calories: no more than 35% daily
● Proteins: no more than 0.8 kg/kg daily
● Liquid: at least 2L/day unless restricted
Different diets
● Carb controlled diet
● Low sodium diet
● Renal diet
● Hepatic diet
● Vegetarian diet
● Ovo/Lacto vegan diet
● Clear liquid
● Full liquid
● Low residual
GI disorder and diets
● Chronic pancreatitis: small frequent meals, high carb, high protein, low fat
Alternative nutrition
Enteral nutrition Parenteral nutrition
● NGT, NJT, G tube, J tube ● For those with GI tract disorders
● Preferred route for those with a ● For those who need support for longer
functional GI tract as it maintains GI than 10 days
function and has less complications ● Requires central line (PICC line,
● For those who cannot tolerate po tunneled, implanted)
intake or not getting enough nutrition
● Contraindications: obstruction, ileus,
GI bleed, fistula, diarrhea, vomiting
Complications Complications
● Tube obstruction (flush before and ● Infection (“CLABSI”; scrub hubs with
after for prevention; flush with warm alcohol wipes before each use;
water and pancreatic enzyme to change tubes Q24H)
declot) ● Pneumothorax, PE, arrhythmias (from
● Tube displacement (X ray verification central line complications)
before use) ● Phlebitis, occlusion
● Aspiration pneumonia
● Nausea, vomiting, diarrhea,
constipation
Disclaimer: This study guide is intended for educational purposes only.
Kidneys And The Urological System
Anatomy
● Nephron: functional unit of the kidneys; 1 million nephrons per kidney
● Glomerular filtration: the filtering of blood that flows through the kidneys; about 20-25%
of cardiac output; filtration ceases if MAP <40-60 mmHg
● Ureters: move urine to the bladder via peristalsis and clog easily
● Urethra: a tube connecting the neck of the bladder to the urethral opening
Kidney functions (“A WET BED”)
● Acid-base balance
● Water-removal/regulation
● Erythropoietin production to increase RBC and Hg
● Toxin removal of protein waste products such as BUN, Cr, uric acid
● Blood pressure control: Renin
● Electrolyte balance
● D-Vit D activation
Risk factors
● Cardiac diseases can cause inadequate perfusion to kidneys or overwhelms the kidneys
with fluid retention
● Diabetes: kidney damage and bladder dysfunction due to blood vessels
● Drug abuse: damages nephrons and glomeruli
● Smoking: leading cause for bladder cancer
S/S
● Pain: from kidney and bladder infections, kidney stones
● Urination frequency, urgency, hesitation: BPH, bladder infection
● Nocturia: BPH, heart failure
● Hematuria: normal and transient after urologic procedures; if no trauma, consider
bladder cancer (painless hematuria is a common first symptom of bladder cancer)
● Cloudy urine: infection
● Minimum urine output is 0.5ml/kg/h
Diagnostic
● Creatinine: 0.5-1.2 mg/dL
○ byproduct of skeletal muscle breakdown & filtered by glomerulus and excreted in
kidneys
○ renal dysfunction reduced the ability to filter Cr & Cr level rises
● BUN 10-20 mg/dL
○ Blood uirrigationrea nitrogen is a waste product of protein breakdown & is
synthesized by liver & excreted in kidneys
○ BUN is a less sensitive test for kidney compared to Cr
● Glomerular filtration rate: 60ml/min/1.73 m2 (African American x 1.2)
Disclaimer: This study guide is intended for educational purposes only.
● Electrolyte imbalance (Na, K, Mg)
● Urinalysis
○ Should be yellow (amber indicates dehydration)
○ Slightly acidic
○ Specific gravity used to assess fluid volume status
○ Trace amount of glucose, protein, WBC and RBC (large amount indicates
glomerular damage
● Noninvasive: X rays (Kidney, ureter, and bladder study), ultrasound, CT scan
● Kidney biopsy
Benign Prostatic Hyperplasia
● A benign enlargement of the prostate gland that puts pressure on the urethra and
pushing up into the bottom of the bladder
● Can lead to bladder outlet obstruction, urinary retention, infection
● Digital rectal exam is done to examine the prostate
● S/S
○ Obstruction: weak flow of urine, hesitancy, dribbling, retention
○ Irritation: frequency, urgency, dysuria, nocturia
○ Elevated PSA
● Treatment
○ Limit fluid intake at bedtime; limit/avoid caffeine, alcohol
○ Frequent voiding, double voiding
○ Medications
■ Alpha-blockers
● Relax urethra muscle and relieve symptoms but do not stop the
enlargement
● End in “-zosin”: Doxazosin (Cardura), Terazosin (Hytrin),
Tamsulosin (Flomax)
● May cause hypotension, making patient more prone to falls
■ 5-alpha reductase inhibitors
● Reduce prostate size
● Take 6+ months to show effect
● End in “-asteride”: Dutasteride (Avodart), Finasteride (Proscar)
● Dutasteride is teratogenic so do not donate blood while on this
med
■ Oxybutynin: to relief urinary spasm, for overactive bladder
○ Transurethral resection of prostate (TURP)
■ Resection of the prostate with a resectoscope via the urethra
■ Needs to three-way foley to irrigate bladder to prevent clots
● Actual urine output = total amount drained from foley -
amount of irrigation
■ Urine should be pink to clear
■ Temporary incontinence may occur post-procedure
■ Does not affect erectile function
Disclaimer: This study guide is intended for educational purposes only.
■ Frequent voiding to prevent edema
Kidney calculi
● Kidney stone are about sizes of a sharpened pencil lead or a speck of dust (that’s why a
filter is required to strain the stones)
● Flank pain is the hallmark symptoms
○ comes in waves due to peristalsis
○ Narcotics use are often needed to relieve pain
● Types of kidney stones
○ Calcium phosphate stones: caused by hyperparathyroidism, or too much
calcium or dairy intake,
○ Calcium oxalate stones: caused by too much dark green leafy foods, coffee,
tea, coke, chocolate
○ Struvite stones: caused by WBC sticking together usually after a kidney infection
○ Uric acid stones: caused by gout
● Treatments
○ Strain the urine to see if the stone passes
○ Neutralize urine with allopurinol, thiazides
○ Lithotripsy: procedure of breaking the stone into tiny particles to pass naturally
Kidney v.s. Bladder Infection
Kidney (pyelonephritis) Bladder infection
Causes ● E.coli through urethra and ● Foley catheters
travels up to kidneys ● E.coli through urethra
● Any bacteria filtered through the
glomeruli
S/S ● Pain in the flank area of the ● Pain during urination
affected kidney
Treatment ● Increase fluid intake, IVF ● Increase fluid intake (to flush
● Antibiotics out the bacteria)
● Phenazopyridine (Pyridium):
helps with dysuria; turns urine
bright orange
Acute Kidney Injury
● Acute kidney dysfunction with elevation of Cr and BUN that occur in hours to days
● Reversible but can progress to CKD or kidney failure if not treated promptly
● Causes
○ Pre-renal
■ Problems occur before the kidneys resulting in reduced perfusion
■ Caused by hypovolemia, shock, heart failure
Disclaimer: This study guide is intended for educational purposes only.
○ Intrinsic
■ Problems occur within the kidneys
■ Acute tubular necrosis: most common; caused by injury to the renal
tubular epithelial cells resulting in tubular dysfunction and decreased GFR
■ Caused by nephrotoxic medications such as NSAIDs, aminoglycosides (a
class of antibiotics that ends with “-mycin”; gentamicin, streptomycin)
○ Post-renal
■ Caused by obstruction to urine drainage after the level of the kidneys
■ BPH, kidney stones, obstructed catheter
● Three stages of AKI
○ Oliguric stage
■ Decreased urine output (<400 mL/day)
■ Last 2-5 days
■ Increase in Cr & BUN
■ Electrolyte imbalance, fluid overload, acidosis
■ Short term dialysis may be needed
○ Diuretic stage
■ Occurs when cause of AKI is corrected
■ Renal tubule scarring and edema
■ Increased glomerular filtration rate and less reabsorption of water
resulting in increased urine output
■ Last 1-3 weeks
■ Manage fluid and electrolytes to prevent hypovolemia (which can happen
quickly)
○ Recovery stage
■ Decreased edema, normalizing fluid and electrolyte balance, labs
dropping
■ Can take several months to a year
■ Patient education to avoid nephrotoxic medications
● S/S
○ Oliguria: <400 mL/day (anuria: <100 mL/day)
○ Fluid retention: edema, JVD, rales
○ Anorexia, n/v, diarrhea/constipation
○ Proteinuria
Chronic Kidney Disease (CKD)
● A progressive decline in renal function that occurs over months to years
● Causes
○ Diabetes and hypertension are the main causes
■ Once diagnosed with diabetes, considered to be in stage I CKD
■ Increased glucose sticks to vessel walls and cause damage
○ Others: chronic pyelonephritis (leads to sclerosing of the nephrons), Polycystic
Kidney Disease (a genetic disease with increased risk in minority and with
advanced age)
Disclaimer: This study guide is intended for educational purposes only.
● Five stages of CKD
○ Normal GFR = 90-120 mL/min/1.72 m2
○ Stage I
■ GFR > 90
■ Kidney damage with normal GFR and kidney function
■ Treat and prevent progression (control diabetes, reduce risk of CVD)
○ Stage II
■ GFR 60-89
■ Kidney damage with normal function
○ Stage III
■ GFR 30-59
■ Decrease in kidney function (elevated Cr & BUN) with presence of
hypertension and anemia
○ Stage IV
■ GFR 15-29
■ Kidney insufficiency with severe loss of kidney functions and symptomatic
■ Prepare for initiation of dialysis, evaluate for transplant list
○ Stage V
■ GFR <15
■ Kidney failure or end stage renal disease (ESRD)
■ Dialysis dependent, s/s of uremia
● S/S
○ Metabolic acidosis, electrolyte imbalance (⇧ K, ⇧ Mg, ⇧ Phos)
○ Decreased erythropoietin production, anemia
○ Uremic pruritus, change in mental status
○ Anorexia, n/v, metallic taste
○ Hypertension, pulmonary edema
● No lifting or B/P on the fistula arm
● IV, lab sticks only below fistula site but should be avoided due to risk of infection
● Feel “thrill” & hear “bruit” for assessment
AKI & CKD Treatments
● Non-pharmacologic
○ Renal diet: low Na, low potassium, low phosphorus, low protein (to prevent
uremia), high carbohydrate, moderate fats
○ Fluid restriction
○ Avoid nephrotoxic meds: NSAIDs, contrast, aminoglycosides
○ Smoking cessation
● Pharmacologic
○ Adjust medications based on renal function as needed
○ ACEI (“-pril”) & ARBs (“-sartan”): slow progression in CKD
○ Phosphate binder (to prevent hyperphosphatemia)
○ Erythropoietin and calcitriol (to replace renal hormones)
■ For erythropoietin/epogen, keep Hg between 11-12 g/dL
Disclaimer: This study guide is intended for educational purposes only.
● Hemodialysis (focus on fistula care)
○ Fistula selection usually starts distally in the arms
○ Takes 2-6 weeks to mature (a dialysis catheter is placed for temporary use)
● Peritoneal dialysis
○ Less expensive than HD
○ Higher risk of contamination and infection
○ Sterile procedure
○ Assess for tightness and pain
○ Monitor for cloudy output
○ Daily weight in between dialysis
● Transplant
○ Cheaper than both forms of dialysis
○ New kidneys are placed in the iliac fossa in front of the hip
○ Needs to be on life-long immunosuppression and need to protect from infection
Fluid and Electrolytes
“Anatomy”
● Approx 40 L of body fluid (about 45-75% of body weight); 75% is intracellular and 25% is
extracellular
● Third-spacing: fluid is in an abnormal space such as peritoneum (ascites), pleural space
(pleural effusion)
● Average daily intake of fluid is 1.5L -2L and output is 1.5L
● Regulated by kidneys and affected by sodium level and ADH hormone
Hypervolemia
● From too much IVF, heart failure
● s/s: bounding pulses, hypertension, may lead to heart and lung failure
Hypovolemia
● From bleeding, third-spacing, dehydration, hyperemesis gravidarum
● s/s: weak, thready pulses, hypovolemia
Third-spacing
● Leaking of fluid into interstitial space due to trauma, infection, low albumin level
● s/s: tissue edema (but pt is intravascularly dry), tachycardia, hypotension
Serum osmolality
● The “thickness” of the solution; how many Na, BUN, & glucose versus how much fluid in
a liter of serum
● The higher the osmolality, the drier the patient
● The lower the osmolality, the more fluid that is present
● Fluid will be pulled from the one with lower osmolality into the one with higher
osmolality
● Normal osmolality = sodium level x 2 (140x2=280)
● Isotonic solution
○ NS, LR 275-295mOsm/L; same as serum osmolality
○ Stay in the vascular space and expand volume to increase perfusion to vital
organs
Disclaimer: This study guide is intended for educational purposes only.
○ Given first to treat hypovolemia
● Hypertonic solution
○ D5LR, D5NS >295 mOsm/L; thicker than serum osmolality
○ Pulls fluid out of the tissue into vascular space
○ Usually given to postop patients to pull fluid from third spacing
○ Not given to dehydrated patients as they will pull even more fluid from tissues
● Hypotonic solution
○ Half NS (0.45%), ¼ NS (0.2%): <275 mOsm/L; less thickness than serum
○ They are pulled from the vascular space into interstitial tissue
○ Given for dehydration
○ But be caution that it may lead to edema esp cerebral edema
Disclaimer: This study guide is intended for educational purposes only.
Endocrine System
● Comprised of glands that secrete hormones to maintains homeostasis
● Hormones are chemical substances that either stimulate or inhibit body processes
Endocrine glands
● Pituitary gland
○ Anterior & posterior pituitary glands
■ Regulated by the hypothalamus
■ The anterior pituitary gland must first receive signals from the
hypothalamus before releasing the hormones to stimulate other
endocrine glands
■ The posterior pituitary gland stores the hormones produced by
hypothalamus and can release them on its own when needed
○ Anterior pituitary hormones
■ “Master gland”; serves as a “bridge” between the hypothalamus and the
other glands
■ Adrenocorticotropic hormone (ACTH): stimulates the anterior pituitary
gland to secrete cortisol in response to stress
■ Thyroid stimulating hormone (TSH): stimulates the thyroid glands
■ Follicle stimulating hormone (FSH) & Luteinizing hormone (LH):
stimulates ovaries & testis
■ Growth hormone (GH): stimulates growth of tissues and bones
■ Procalcitonin: stimulates milk production
○ Posterior pituitary hormones
■ Oxytocin: stimulates milk production & contraction of uterus during labor
■ Antidiuretic hormone (ADH): prevent water loss in the kidneys
● Thyroid gland
○ Located in between larynx and the anterior trachea
○ The only endocrine gland that can be palpated
○ Thyroid hormones
■ T3 & T4
● Secreted by thyroid gland when stimulated by TSH
● Maintains metabolism
■ Calcitonin
● Reduces serum calcium and phosphorus level
● Negative feedback
● Parathyroid gland
○ Four small glands located behind the thyroid glands
○ Regulates calcium level via parathyroid hormones (PTH)
■ When calcium is low, PTH secreted and increases bone resorption to
return calcium into the blood
■ When calcium is high, PTH secretion is decreased (but calcitonin
secretion is increased)
● Pancreas
Disclaimer: This study guide is intended for educational purposes only.
○ Produces pancreatic cells (or islet cells) that secrete insulin and glucagon
○ Insulin
■ Secreted by beta cells
■ Lowers glucose level by allowing glucose to enter the cells
○ Glucagon
■ Secreted by alpha cells
■ Increases glucose level by stimulating the liver to release the glucose
storage (glycogen)
● Adrenal glands
○ Lies on top of each kidney
○ Cortex releases steroids
■ Mineralocorticoids: aldosterone (reserves Na and excretes K+; increase
BP)
■ Glucocorticoids: cortisol (depresses inflammatory and immune response)
■ Androgens: testosterone
○ Medulla releases stress hormones
■ For acute stress response; “Fight or flight” stress response
■ Catecholamines, epinephrine, norepinephrine
■ Increased HR, BP, increased blood flow to muscles and brain, stimulates
release of glucose from the liver
● Reproductive organs
○ Testis: secretes testosterone and androgens
○ Ovaries: secretes estrogens and progesterones
Glands and diagnostic labs
(know each gland and the corresponding hormones)
Pituitary gland Growth hormone, antidiuretic hormone, ACTH
Thyroid gland T3, T4, TSH (thyroid stimulating hormone)
Parathyroid gland PTH, calcium, phosphorus
Pancreas Fasting serum glucose, ketones, glycosylated hemoglobin
Adrenal glands Aldosterone, cortisol, 24 h urine test
Reproductive glands Testosterone, androgen, estrogens, progesterones
Hyperthyroidism
● Overproduction of T3 & T4 resulting in a hypermetabolic state
● Causes
○ Primary hyperthyroidism: overproduction of thyroid hormones due to dysfunction
in the thyroid gland itself (such as thyroid tumor/nodules)
■ ⇧T3, T4, ⇩TSH
Disclaimer: This study guide is intended for educational purposes only.
○ Secondary hyperthyroidism: overstimulation from the hypothalamus or pituitary
gland resulting in overproduction of the thyroid hormones; the thyroid gland itself
is functioning normally
■ ⇧T3, T4, ⇧TSH
● Grave’s disease: an autoimmune disorder in which the immune system produces
“TSH receptor antibodies” that can mimic TSH & stimulate release of thyroid
hormones
● Plummer’s disease (toxic multinodular goiter): nodules growing around the
thyroid gland and produces excessive thyroid hormone; can feel firm nodules
during thyroid palpation
● S/S
○(due to increased metabolism)
○Atrial fibrillation (possible first sign), HTN, tachycardia, fever,
○Restlessness, diarrhea, weight loss, heat intolerance
○Exophthalmos: bulging of the eyeballs due to inflammation & swelling of the
tissue behind the eyeballs
○ Pretibial myxoedema: deposits of mucin under the skin in the front of the legs;
skin becomes waxy & discolored; edematous; caused by skin reaction to the
antibodies
● Treatment
○ Carbimazole: first line; regain normal thyroid function after 4-8 weeks & complete
remission in 18 months
○ Propylthiouracil: second line; risk of liver injury; ok to use in the first trimester
○ Radioactive Iodine (I131): an oral dose of radioactive iodine that is swallowed,
absorbed in bloodstream, and then taken up by the thyroid gland → the radiation
in the iodine releases & destroys the thyroid cells → ⇓⇓ thyroid hormones; no
contact with anyones for a few days after the I131 since the iodine emits radiation
and is harmful to others
○ Beta blockers: blocks adrenalin related s/s such as tachycardia, anxiety,
sweating, tremor
○ Thyroidectomy: surgical removal of all or part of the thyroid; post-op
complications include hemorrhage, hypocalcemia, and tetany (due to possible
damage to the parathyroid gland)
● Thyroid storm
○ Life threatening complication with rapid release of T3/T4 from untreated or
under-treated hyperthyroidism or from thyroidectomy
○ Presentation is the same as hyperthyroidism but much more severe→ everything
is working at an accelerated rate but the body can only do that for so long before
it no longer can → can lead to death
○ S/S: severe HTN, heart attack, dysrhythmia, delirium, fever, increased respiration
○ Nursing intervention: maintain airway, monitor BP & HR, tylenol, beta blockers,
keep quiet & cool, anti-anxiety meds
○ Aspirin in contraindicated due to it interfering with binding of T3/T4
Disclaimer: This study guide is intended for educational purposes only.
Hypothyroidism
● Not enough thyroid hormones leading to a decrease in metabolic rate
● Causes
○ Hashimoto’s thyroiditis: autoimmune disorder in which the immune system
attacks the thyroid gland
○ Primary hypothyroidism
■ Complication from hyperthyroidism treatment such as medications and
surgery
■ ⇩ T3, T4, ⇧ TSH
○ Secondary hypothyroidism include hypopituitarism: decreased TSH & ACTH from
pituitary due to tumors, infection
■ ⇩ T3, T4, ⇩ TSH
● S/S
○ (due to decreased metabolic rate)
○ Bradycardia, hypotension, cold intolerance
○ Coarse hair/hair loss, dry skin
○ Weight gain (no T3 or T4 to help burn calories)
○ Constipation, fatigue, amenorrhea, fluid retention (edema, pleural effusion,
ascites)
● Treatment
○ Levothyroxine/synthroid
■ Lifelong treatment
■ Dose titration & monitor TSH level at the beginning (if TSH high→ dose is
too low; if TSH low→ dose is too high)
■ Half life is 2 weeks so it takes a while to start working
■ Take on empty stomach one hour before breakfast in the morning or 2
hours after meals
■ Do not take within 4 hours of GI med like keflex, simethicone, aluminum
hydroxide because they decrease the effect
■ Do not stop abruptly
○ Iodine rich diet: seafood, seaweed, dairy, table salt with iodine
● Myxedema Coma
○ Life-threatening condition caused by uncontrolled hypothyroidism where
metabolism is slowed down to the point of death
○ Stuporous state, altered LOC, coma, hypothermia, respiratory depression
○ Precipitated by infection, trauma, drugs, exposure to extreme cold
Cushing’s Disease
● Oversecretion of cortisol from adrenal cortex
● Causes
○ Primary
■ Long term use of steroids
■ Adrenal tumor
○ Secondary
Disclaimer: This study guide is intended for educational purposes only.
■ Oversecretion of ACTH from pituitary gland
■ Pituitary tumor, small cell lung cancer causing increased ACTH
● S/S
○
“STRESSED”
○
Skin fragile
○
Truncal obesity with small arms
○
Round face (“moon face”); Reproductive issues (menstruation, erectile
dysfunction)
○ Ecchymosis (bruises); Elevated BP
○ Striae in extremities (purplish stretch marks like on arms & esp. abdomen)
○ Sugar very high (hyperglycemia)
○ Excessive body hair (esp. female with excessive facial hair, body hair)
○ Dorsocervical fat pad (“buffalo hump on the back); Depression (due to the
appearance)
○ Key points: appearance of “moon face”, “buffalo hump”, “striae”; HTN,
hyperglycemia,& increased hair production
● Treatment
○ Discontinue steroid therapy (slow taper to prevent adrenal insufficiency)
○ Mitotane: inhibits adrenal function (but does require steroid replacement as the
adrenal is being suppressed and not able to produce cortisol on its own)
○ Supportive care/symptom management
■ Prevent infection
■ Treat hyperglycemia
■ Fluid restriction
■ Monitor electrolytes, BP, edema
Addison’s Disease
● Adrenal insufficiency with low level of cortisol in blood
● Causes
○ Autoimmune disease causing the body to attack adrenal gland resulting in
decreased production of cortisol & aldosterone
○ Tumor or infection of the adrenal gland or pituitary gland
○ Sudden discontinuation of high-dose steroid, history of recent steroid use
● S/S
○ ( low “STEROID” hormone)
○ Sodium & sugar very low; salt craving
○ Tired & weak (low cortisol)
○ Electrolyte imbalance (due to low aldosterone)
○ Reproductive changes (low androgen levels→ irregular periods, ED in males)
○ lOw BP (due to low steroid; risk for vascular collapse/shock) & tachycardia as
result of low BP
○ Increased pigmentation of skin (generalized hyperpigmentation or bronze
appearance → hallmark sign)
○ Diarrhea, nausea, Depression
Disclaimer: This study guide is intended for educational purposes only.
● Cortisol-Stimulation Test
○ A diagnostic test with administration of artificial ACTH
○ Obtain a baseline cortisol blood level→ administration of artificial ACTH→ check
cortisol level after administration at 30 min & 60 min (cortisol level should be
doubled the baseline if normal adrenal function)
○ Result
■ If elevated cortisol→ normal adrenal function (adrenal responded
appropriately to ACTH)
■ If no change→ confirms primary adrenal insufficiency
● Treatment
○ Hydrocortisone/prednisone replacement:
■ Lifelong medications
■ Important for patient to recognize & report when there is extra stress in
life in which they may need higher dose of steroid as their bodies are not
able to compensate
■ Do not stop medication abruptly
■ Monitor for hyperglycemia
○ Fludrocortisone (Florinef): replaces aldosterone; may cause HTN (as aldosterone
retains sodium & water)
○ Support care: IVF for hypotension, monitor electrolytes, EKG changes,
tachycardia
Diabetes Insipidus
● A result of low level of antidiuretic hormone (ADH)
● has nothing to do with blood glucose or insulin but is a problem of fluid imbalance due to
low ADH → which causes increased urine output & loss of water → “polyuria &
polydipsia”
● Causes
○ Lack of ADH production by the brain
■ head trauma, craniotomy, brain tumors, infections
○ Normal production of ADH but kidneys failed to respond
■ Familial, pregnancy (esp 3rd trimester)
■ Anything that causes kidney injury (infection, electrolyte imbalance,
tumor)
■ Drugs that inhibit ADH (lithium, phenytoin)
● S/S
○ Sudden onset of excessive polyuria and polydipsia
○ Dehydration (hypernatremia, low urine osmolality, high plasma osmolality)
○ (glucose level is not affected)
● Treatment
○ Medications: desmopressin (to replace ADH), chlorpropamide (increased renal
sensitivity to ADH)
○ Aggressive fluid replacement (hypotonic fluid 0.45% NS)
○ Monitor electrolytes especially Na level (monitor neuro status)
Disclaimer: This study guide is intended for educational purposes only.
○ Safety precaution: due to hypotension & frequent urination
○ Avoid foods that promote diuresis: caffeine, watermelon, grapes)
Syndrome of Inappropriate ADH Secretion (SIADH)
● Excessive release of ADH causing fluid retention and hyponatremia due to dilution
● Causes
○ Pituitary dysfunction, tumor, or infection
○ Lung cancer (causes excessive secretion of ADH)
● S/S
○ Neuro changes (due to low Na): confusion, seizures, headache
○ Respiratory: pulmonary edema, crackle lung sounds
○ Cardiovascular: HTN (due to fluid overload & ADH is a vasopressin), tachycardia,
generalized edema, weight gain
○ GI: anorexia (too much pressure on GI), nausea, abdominal cramps
○ GU: low urine output, concentrated urine, elevated urine osmolality
● Treatment
○ Treat the underlying cause
○ Diuretics, demeclocycline (decrease renal sensitivity to ADH)
○ Monitor Na level: do not increase Na > 10 mEq/L per day due to risk for central
pontine demyelination (destruction of myelin sheath of nerve cells when Na
corrected too fast which can lead to paralysis, speech & swallowing difficulty)
○ Monitor neuro status
○ Fluid restriction, strict I&O, monitor weight
Diabetes Mellitus
● Cells are unable to take in glucose due to either no insulins present (type I) or resistance
to insulin (type II)
Type I Type II
● Pancreatic islet cells are destroyed ● Inadequate insulin production or cells
resulting in low or total lack of insulin are being insulin resistant
production ● Caused by sedentary lifestyle,
● Caused by genetic, autoimmune medications (such as steroid), more
disorder in children, but can present in common in adults
adults due to trauma ● Can be controlled with diet, exercise;
● Rapid onset oral insulin and/or insulin injection
● Classic “3 Ps”: polyuria, polydipsia, ● At high risk for hyperosmolar
polyphagia Hyperglycemic Nonketotic Syndrome
● Lifetime dependence on insulin (HHNS)
injection
● At higher risk for diabetic ketoacidosis
(DKA)
Type I symptoms Type II symptoms
Disclaimer: This study guide is intended for educational purposes only.
● Weight loss, thin ● Overweight, obese
● Younger age ● Occurs over longer period of time
● Abrupt onset ● Polyuria
● Polyuria ● Polydipsia
● Polydipsia (increased thirst) ● Polyphagia
● Polyphagia (increased appetite)
● Dry skin/mucous membrane
● Glucose level and HbA1c level
○ (know the normal and abnormal values)
Normal level Pre-diabetes Diabetes
Fasting (NPO after 70-99 mg/dL 100-125 mg/dL >126 mg/dL
midnight; at least 8
hours)
Random <125 mg/dL >100 mg/dL >200 mg/dL
(depends on last
intake
2 hour postprandial 56-139 mg/dL 140-199 md/dL >200 mg/dL
HbA1c 4-5.5% 5.7-6.4% >6.5%
● Management
○ Diet
■ Balance carbohydrate intake with insulin and exercise
■ Small amount of protein, higher fats, high fiber
■ Pt education on how to read food labels
■ Same amount of food consumed at the same time to maintain
consistency of glucose level
■ Avoid alcohol to reduce the risk of nocturnal hypoglycemia in those using
insulin or oral meds; if had to, consume alcohol with food
○ Exercise
■ Improves insulin sensitivity by enhancing glucose transport into exercising
muscles
■ Effects of glucose-lowering can last for hours after exercise
■ Type II benefits the most but might be limited in type I as they have to be
aware of hypoglycemia during exercise
■ Aerobic moderate to high intensity exercise, muscle/joint strengthening
■ When to avoid exercising: when glucose level is low or s/s of
hypoglycemia; when glucose is >250 with positive ketonuria (as body is
already burning proteins for metabolism)
○ Patient education
■ Lose weight if indicated
Disclaimer: This study guide is intended for educational purposes only.
■ Decreased or no ETOH intake
■ Sick day management
■ Foot care (wear shoes that fit without rubbing; check for skin breakdown
with a mirror)
■ Understanding and use of the glucometer
■ Annual eye exam
■ Follow up with provider
○ Insulin
■ Mimic normal body response to glucose
■ Basal: slow releasing insulin to keep glucose level consistent during
fasting (in between meals, during sleep)
● Lantus, Levemir, NPH
● Usually given daily at bedtime
■ Bolus: to be given with meals to supply insulin for glucose consuming
from meals; do not give if patient is NPO
● Regular, Humalog, Novolog
● Must be taking with food
■ Correction (sliding scale): based on glucose measurement; should NOT
be held if patient is NPO (as this is given based on the high glucose level
which needs to be “corrected”)
● Humalog, Novolog, Apidra
Insulin Name Onset Peak Duration
Rapid-acting Lispro (Humalog, 5-20 min 0.5-1.5 h 2-5 h
Admelog)
Aspart (Novolog,
Fiasp)
Short-acting Regular (Humulin 0.5-1 h 2-5 h 5-8 h
R, Novolin R)
Intermediate- Insulin NPH 1-2 h 6-12 h 10-24 h
acting (Humulin N,
Novolin N, ReliOn)
Long-acting Detemir (Levemir), 1-2 h Steady level 24 h
glargine
(Basaglar, Lantus)
● Patient education on insulin administration
○ Rotate sites for injection; do not rub or use heat after injection as that
increases absorption
○ Monitor for s/s of possible hypoglycemia when insulin reaches its “peak”
time
○ NEVER mix long-acting insulin with any other insulin
Disclaimer: This study guide is intended for educational purposes only.
○ Ok to mix short-acting with intermediate acting in the same syringe
■ Always draw Regular (the clear) insulin first to prevent
contaminating the clear-vialed insulin with NPH (the cloudy) insulin
■ Administer immediately after mixing
● Oral agents
Classification Drug Actions
Sulfonylureas Glipizide (Glucotrol) ● Stimulate pancreatic cells to secrete
Glyburide (Diabeta) more insulin & increase sensitivity of
peripheral tissues to insulin
● Can trigger severe hypoglycemia
● Can last for 36 h
Biguanides Metformin (Glucophage) ● Decrease overproduction of glucose
by liver & increases binding of insulin
to tissues
● Be caution in pt with kidney problems
as metformin can build up & lead to
lactic acidosis
● Hold for 48 h after contrast dye
Thiazoldinedio Rosiglitazone (Actos) ● Reduces gluconeogenesis and
nes Pioglitazone (Avandia) cellular insulin resistance
● Can cause weight gain and fluid
retention
● Diabetic complications
○ Hypoglycemia
■ Glucose level <70
■ Causes: reduced oral intake, too much insulin, exercise
■ S/S: shakiness, nausea, palpitation, diaphoresis, altered LOC, irritability,
seizures, coma (due to lack of glucose for brain cells), death
■ Treatment
● 10-15 g of fast acting carbohydrates: apple juice, glucose
gel/tablets, glucagon, D50 IVP for NPO pt
● Once blood glucose is stabilized, choose food that is complex
carbohydrate and high in protein to prevent rebound
hyperglycemia
○ Milk, cheese, crackers, peanut butter
■ Tips to prevent hypoglycemia
● Choose foods that are high in protein, complex carbohydrates;
and avoid simple carbohydrates
○ Simple carbs can cause glucose to rise quickly and lead to
increased insulin production and that can cause
hypoglycemia
● Avoid fasting
Disclaimer: This study guide is intended for educational purposes only.
● Balance eating and exercise (esp in Type I diabetes)
● Keep a glucometer available
○ Diabetic Ketoacidosis
■ A serious complication of uncontrolled diabetes and no insulin available→
body turns to fat for metabolism & produces ketone as a byproduct→
accumulated ketones causes the blood pH level to drop & lead to acidosis
■ Occurs in type I diabetes, usually younger patients
■ Cause of death: metabolic acidosis with hyperkalemia
■ S/S
● Hyperglycemia: >300 g/dL
● UA with + glucose & ketones
● Polyuria, polydipsia, polyphagia
● Abdominal pain, nausea (due to acidosis)
● Electrolyte imbalance: especially hyperkalemia
● Kussmaul breathing: rapid respiration due to body trying to blow
off carbon dioxide (which is acidic)
● Acetone odor in breath: fruity, sweet breath from excess ketones
■ Treatment
● Insulin drip to lower BG (only regular insulin can be given IV) &
hourly blood glucose monitoring to prevent hypoglycemia
● IV fluid to correct hypovolemia/dehydration
● Cardiac monitoring
● Monitor K+: when glucose level is high in blood, K+ leaves the
cells & follow glucose to the blood vessels→ resulting in both
HIGH glucose & potassium with DKA → when insulin is given &
drives glucose back into cells → K+ also follows & goes back to
intracellular → Need to monitor for hypokalemia with IV insulin
treatment
○ Hyperosmolar Hyperglycemic Syndrome (HHS)
■ A serious complication of diabetes with super high BG level (>600;
higher than DKA) which makes blood concentrated
(“hyperosmolar”=high osmolarity)
■ But NO production of ketoacidosis (some of the insulin is still working to
prevent breakdown of fats)
■ Occurs in type II, older patients
■ Happens gradually
■ Cause of death: hypovolemia
■ S/S
● Similar to DKA: polyuria, polydipsia, polyphagia, electrolyte
imbalance, dehydration
● But NO ketoacidosis involved → so no Kussmaul breathing,
acetone odor in breath
● Neuro changes: confusion, seizures
■ Treatment
Disclaimer: This study guide is intended for educational purposes only.
● Similar to DKA
Difference between DKA & HHS
DKA HHS
● Type I (more common) ● Type II (more common)
● Absence of insulin ● Not enough insulin
● Ketoacidosis (hyperkalemia, fruity ● No ketoacidosis
breath, Kussmaul respiration) ● BS >600
● BS >300 ● Super high BS & dehydration
● Rapid onset ● Slow onset
● Neurological changes
Disclaimer: This study guide is intended for educational purposes only.
Hematological System
Physiology
● Hematopoiesis
○ Process of a stem cell differentiating itself into types of blood cells
○ Types of blood cells include:
■ Myeloid which differentiate to RBC, platelets, WBC
● WBC further differentiate into
○ Granulocytes: basophils, eosinophils, neutrophils
○ Agranulocytes: T cells, B cells, monocytes
■ Lymphoid which differentiate to lymphocytes: T cells, B cells, NK cells
● T cells:
○ Mature in the thymus gland
○ Helper T cells: stimulate B cells to produce antibodies
○ Killer T cells: attack abnormal molecules on cell surfaces,
esp viruses
● B cells:
○ Originate in both bone marrow and lymphatic tissues
○ Produce antibodies in response to antigens
○ Each B cell is programmed to make one specific type of
antibody
○ Can develop into plasma cells which make more
antibodies
● Natural Killer Cells
○ Attack any type of foreign body without needing to assess
the antigen
● Whole blood component
○ Red blood cells (RBC)
■ Erythrocytes
■ Life span 120 days
■ Hemoglobin (Hgb): 12-16 g/dL female, 13-18 g/dL male
■ Hematocrit (Hct): 38-47% female, 40-54% male
■ Reticulocyte count: measure of immature RBCs, indicates effectiveness
of BM production of RBCs
○ Platelet
■ Thrombocytes; stop bleeding by clumping together
■ Life span 10 days
■ Normal: 150 K-350 K /mm3
○ White blood cells (WBC)
○ Leukocytes; activated in response to infection
○ Normal: 5 K -10 K /mm3
○ Neutrophils
■ Most abundant (50-70%)
■ First line of defense against bacteria
■ Bands: matured neutrophils
Disclaimer: This study guide is intended for educational purposes only.
○ Monocytes
■ Macrophages and kill bacteria after neutrophils
○ Eosinophils
■ Activated during hypersensitivity reaction
○ Basophils
■ Keep blood flowing through micro-vessels (microvasculature
circulation)
○ Plasma
■ Light yellow liquid portion of the blood
■ 90% of water and 10% of clotting factors (mainly fibrinogens), plasma
proteins (albumin, globulin), electrolytes, immunoglobulins
Anemia
● Is a decrease in Hgb concentration and can lead to hypoxia-induced impairment of body
organ systems
● Grade 1=10g/dl or lower, grade 2=8-10 g/dl, grade 3=6.5-8 g/dl, grade 4-5=life
threatening and death
● Causes
○ Bleeding (chronic or acute)
○ Iron deficiency anemia
■ insufficient iron for RBCs due to malnutrition or malabsorption
■ S/S: spooning nail plates, smooth tongue, cheilosis (cracks at the corner
of the mouth), cheilitis (inflammation of the lips), glossitis (inflammation of
the tongue), pica (craving of dirt, clay, ice)
● S/S
○ Decreased activity tolerance
○ Mild SOB, increasing during exertion
○ Increase in fatigue
● Treatment
○ Fluid resuscitation, transfusion, oxygen
○ For iron deficiency
■ Ferrous sulfate and vitamin C to enhance absorption
■ IV iron
Sickle cell anemia
● Hereditary disorder in which the abnormal Hgb changes the shapes of the RBCs due to
lack of oxygen and results in congestion and vaso-occlusion of microcirculation
● Increased risk for thrombosis, stroke, heart failure
● Can be diagnosed via amniocentesis in an unborn baby
● Sickle cell crisis
○ Painful condition in which small blood vessels are occluded leading to distal
ischemia and infarction
○ Precipitating factors
■ Hypoxia, dehydration, fever, bleeding
Disclaimer: This study guide is intended for educational purposes only.
■ Infection, stress
■ Strenuous exercise, elevated altitude, cold weather
■ Pregnancy
○ S/S
■ Hypoxia, dyspnea, fatigue
■ Severe pain
■ Joint swelling, peripheral edema
■ Decreased/dark urine output
■ Jaundice
○ Treatment
■ IV/PO hydration, oxygen, blood transfusion
● Normal oxygenation can return RBCs back to a normal shape
■ Pain management (use of opioids, NSAID)
■ Stem cell transplant
○ Patient education
■ Adequate hydration (4-6 L/day)
■ Avoid strenuous exercises, high altitude, stress
■ Infection prevention
■ Smoking cessation
Disseminated Intravascular Coagulation (DIC)
● Activation of coagulation pathways, leading to a situation of simultaneous hemorrhage
and clot formation, which can result in congestion and blockage of the microvasculature
● Risk factors
○ Sepsis (most common)
○ Some solid and hematologic cancers
○ Severe transfusion reaction
○ Organ destruction/toxic reactions
○ Some obstetric complications
● Diagnosis (hallmark)
○ Low platelet
○ Decreased fibrinogen
○ Fibrin degradation products elevated (indicates breakdown of fibrin and
fibrinogen)
● S/S
○ Bleeding that occurs simultaneously from at least three unrelated sites is a
hallmark sign of DIC
○ Common sites are from intravenous lines or catheters, wound sites, mucous
membranes, or surgical sites
○ Bruising, petechiae
● Treatment
○ Treatment of underlying causes
○ Supportive care with monitoring bleeding, giving blood products including cryo,
platelets, plasma, PRBC
Disclaimer: This study guide is intended for educational purposes only.
○ Fall and bleeding precautions
Leukemia
● Malignant immature white blood cells proliferate and crowd out normal cells in the bone
marrow and inhibit normal hematopoietic cell functioning
● Types
○ Acute: cells are immature, undifferentiated
○ Chronic: cells are mature, well-differentiated but of abnormal appearance
○ Lymphocytic: immature lymphocytes
○ Myelogenous: myeloid stem cells fail to mature and result in decreased RBC,
WBC, platelets
○ AML & CLL: most common in adults
○ ALL: most common in children and teens
● Signs and symptoms
○ Elevated WBCs (>5% blast cells)
○ Fatigue, weight loss, pale skin
○ Frequent infections
○ Bruising, nose bleeds, petechiae
○ Bone or joint pain
○ Swelling in lymph nodes or abdomen
○ CLL is typically asymptomatic
● Treatment
○ Chemo is the treatment of choice
○ Biotherapy, radiation, bone marrow/stem cell transplant
○ Bleeding and neutropenic precaution
○ CLL: often a watchful waiting cancer for many years until symptoms become
significant
Neutropenia
● Inadequate production of or excessive destruction of neutrophils
● Absolute neutrophils count (ANC)
○ Measurement of number of mature WBCs in the circulation
○ Defined as ANC < 1500
○ Severe when ANC <500
● Causes: Leukemia, immunosuppression therapy, chemotherapy
● S/S
○ Maybe absent or diminished
○ Low grade fever, chills, fatigue, weakness
○ Ulceration in mouth and oral cavity
● Treatment
○ Monitor for s/s of infection
○ Prophylactic antibiotics may be used
○ Neutropenic precaution/patient education
■ Meticulous hygiene
Disclaimer: This study guide is intended for educational purposes only.
■ Avoid crowds, limit exposure, wear masks
■ Private room when in hospital
■ Visitors must perform hand hygiene and wear masks when in patient’s
room
■ No raw vegetables, fruits (unless peeled), avoid directly handling
plants/flowers
■ Educate patient that neutropenic fever is a medical emergency and
should be intervened immediately
Hodgkin’s and Non-Hodgkin’s lymphoma
● Hodgkin’s Lymphoma (HL)
○ Lymph tissue malignancy that originates in the WBCs of the lymph nodes
○ Presences of Reed Sternberg cells (from lymph node biopsy)
○ Localized involvement
○ Better prognosis
● Non-Hodgkin’s Lymphoma (NHL)
○ Lymph malignancy that originates in B cells (90%) or T cells
○ No Reed Sternberg cells
○ Widespread involvement
○ Poorer prognosis
● Risk factors
○ HL peaks in young adults and again in older adults; NHL increases with age
○ Family history
○ Immunosuppression
○ Viral exposure: Epstein Barr, Hep C
○ Bacterial exposure: H. pylori
● S/S
○ Lymphadenopathy
■ Usually painless
■ HL: typically involving cervical, supraclavicular, and mediastinal nodes;
some has splenic involvement
■ NHL: 50% present with symptoms associated with liver or spleen
○ “B” symptoms
■ Fever
■ Drenching night sweats
■ Anorexia and unexplained weight loss
● Treatment
○ Chemotherapy, radiation, immunotherapy, stem cell transplant
○ Provide information on family planning, sexual dysfunction, sperm or egg
banking
Multiple Myeloma
● Cancer of the plasma cells that are responsible for producing immunoglobulins
Disclaimer: This study guide is intended for educational purposes only.
● Causes elevated levels of monoclonal immunoglobulins and stimulates activity of
osteoclasts cells which causes destruction of bone tissues
● Incidence is twice in African Americans than that of Caucasians
● Has a poor diagnosis with 75% becoming fatal
● Classic Symptoms (“CRAB”)
○ C=calcium elevation (>11.5 g/dL)
○ R=renal insufficiency
○ A=anemia
○ B=bone disease: lytic lesions causing swiss cheese presentation on bone scan
with bone pain in the back and chest; caused by production of osteoclastic
factors by the malignant plasma cells
● Classic Diagnostic Triad
○ Elevated “M” protein
○ Bone marrow with abnormal plasma cell
○ Lytic lesion of the bone
● Treatment
○ Chemotherapy is the treatment of choice
○ Followed by stem cell/bone marrow transplant
Stem cell transplant
● Autologous
○ From self
○ Risks/benefits:
■ No development of graft versus host disease
■ Potential for contamination of graft with cancer cells
● Allogenic
○ From a human leukocyte antigen (HLA) matched donor
■ HLA: proteins found on the surface of WBCs and they can differentiate
self from non-self
■ When two individuals share the same HLA, their WBCs are
immunologically and histologically compatible
■ Could be siblings, non-related donors
○ Risks/benefits
■ Complications of infection or long-term organ damage
■ Graft versus host disease risk
■ No malignant cells in the graft
Disclaimer: This study guide is intended for educational purposes only.
Cancers
● Results from cell mutations due to genetic, chemical, radiation, virus, environment
● Treatment
○ Chemotherapy: inhibit rapidly growing cell; affects both cancerous and normal
cells
■ PPEs required to handle chemotherapy
○ Biotherapy: enhances the immune system to fight cancer
○ Radiation: affects both normal and cancerous cells; fatigue and skin reactions are
the most common symptoms
● Nursing care for patients undergoing treatment
○ Fatigue, anorexia, nausea, flu like symptoms
○ Blood counts drop to the lowest at 7-10 days after chemotherapy
■ Neutropenia (absolute neutrophil count <1.5); high risk of infection
● No consumption of raw food, wash fruits and vegetables
thoroughly, avoid gardening (exposure to fungal infection)
● Neutropenic fever is a medical emergency and is defined as a
single oral temperature greater than or equal to 101 F (38.3 C) or
a temperature greater than or equal to 100.4 F (38 C) for at least
an hour, with an absolute ANC < 1.5
● High risk for sepsis
● Colony stimulating factors can be given to increase white cell
production
○ Filgrastim (Neupogen), pegfilgrastim (Neulasta)
■ Thrombocytopenia, anemia
● Increased risk of bleeding
○ Provide education and emotional support
Oncological emergencies
● Sepsis: pan-culture should be done and antibiotics should be started within an hour of
neutropenic fever
● Tumor lysis syndrome
○ Rapid release of intracellular contents (K+, phosphate, uric acid) into the
intravascular space and can lead to kidney failure
○ Occurs due to cancer and normal cells killed by chemotherapy
● Syndrome of inappropriate antidiuretic hormone (SIADH)
○ Inappropriate activation of ADH resulting in fluid overload and low Na
○ Commonly seen in lung cancers
● Hypercalcemia
○ Elevated calcium level due to bone mets
○ Commonly seen in multiple myeloma
○ s/s: weakness, polyuria, polydipsia, nausea, bradycardia
● Disseminated intravascular coagulation (DIC)
○ A consumption coagulation disorder leading to simultaneous clotting and
bleeding problems
Disclaimer: This study guide is intended for educational purposes only.
● Superior vena cava syndrome
○ Tumor compressing on the SVC causing backflow of blood resulting in swelling of
face, neck, arms, and respiration distress
● Spinal cord compression
○ Tumor compressing on spinal cord causing loss of function below the level of the
tumor
Disclaimer: This study guide is intended for educational purposes only.
Types of Shock
Cardiogenic shock
● Heart is unable to pump effectively resulting in decreased cardiac output followed by
collapse of the vascular system
● Causes: MI, severe cardiomyopathy, cardiac tamponade (filling of fluid or blood in the
pericardial sac)
● Change in RR is often the first subtle sign
● ICU for intra-aortic balloon pump, intravenous blood pressure support
Hypovolemic shock
● Most common type
● Inadequate circulating volume due massive blood loss and lead to deprived oxygen in
organs
● Causes: post-op bleeding, GI bleed
● S/S: increased RR, tachycardia, hypotension (drops quickly)
Septic shock
● An overactive immune response to an infection causing systemic inflammation and
hypoperfusion to organs
● Can occur with or without presence of bacteremia
● Septic shock can be prevented with early intervention with fluids and antibiotics
● Risk factors
○ Elderly (esp women with repeated UTIs)
○ Patients with central line and/or foley
○ Patients with wounds
● Stages of sepsis
○ Stage 1: inflammatory response
■ RR>20, temp <36 or > 38, HR >90, WBC <4000 or >12,000 or >10%
bands
○ Stage 2: sepsis
■ Infection suspected or an inflammatory response is identified
○ Stage 3: severe sepsis
■ Overwhelmed response to sepsis with signs of organ dysfunction
■ Changes in oxygen requirement, SBP<90, urine output <0.5 ml/kg/h,
changes in mental status, lactate >2
■ Requires rapid fluid resuscitation (with isotonic fluids) and possible
transfer to ICU
○ Stage 4: septic shock
■ Severe sepsis with refractory hypotension
■ High mortality rate
■ Refractory hypotension after 30ml/kg/fluid
■ ICU needed for vasopressors
Disclaimer: This study guide is intended for educational purposes only.
Neurogenic shock
● Rare; occurs in those with severe damage to the CNS and spinal cord
● Results from sudden loss of sympathetic tone causing massive vasodilation which leads
to the autonomic instability
● S/S: marked hypotension, bradyarrhythmia, temperature dysregulation
● Fluids and pressors
Anaphylactic shock
● Severe systemic allergic response after exposure to an allergen (food, medications, bee
stings)
● Constriction of airways, severe hypotension, tachycardia, swelling
● Airway management (priority), epinephrine (to stop vasoconstriction of the airway),
anti-histamines (H1 & H2 blockers), steroids
Disclaimer: This study guide is intended for educational purposes only.
Immunological System
Immune surveillance
● Ability of the immune system to recognize and destroy foreign cells, functioning as the
primary defense
● Two types of immune response
○ Innate response
■ Generic immune response to antigens and non-specific
■ No memory
■ Consists of the following
● Physical barriers, skin, mucous membranes, lining of respiratory
tract
● Inflammatory response: monocytes, macrophages,
polymorphonuclear cells (neutrophils)
○ Acquired or adaptive response
■ Involves B and T lymphocytes in response to specific antigens
■ Has memory on the same antigens
■ Two types
● Humoral or antibody-mediated immunity
○ B cells
○ Production of antibodies and immunoglobulins
○ Separates into plasma and memory cells
○ Secretes immunoglobulins that label the foreign antigens
for destruction
● Cell-mediated immunity
○ T cells
○ Changes into cytotoxic T cells and helper T cells
○ Recognizes foreign antigens from exposure and activates
the immune response
○ No antibody production
Types of immunity
● Immunity to a disease is achieved through the presence of antibodies to that disease
● Active immunity
○ From exposure to a disease triggering the immune system to produce antibodies
■ Naturally acquired: acquired through infection with the actual disease;
long duration, perhaps lifelong
■ Vaccine-induced immunity: acquired through vaccination with weakened
form of the disease; shorter duration and may require “boosters”
● Passive immunity
○ Occurs when a person is given antibodies to a disease rather than producing
them through his or her own immune system
■ Naturally acquired: antibodies passed from placenta or breastfeeding
Disclaimer: This study guide is intended for educational purposes only.
■ Artificially acquired: through antibody-containing blood products such as
immune globulin, which may be given when immediate protection from a
specific disease is needed.
● Antigens
○ On the surfaces of cells
○ Body uses antigens to differentiate “self” cells from foreign cells
● Antibodies
○ Proteins formed in response to antigen exposure
○ Recognize self
Hypersensitivity
● An exaggerated antibody response to a previously exposed antigen
● Types of hypersensitivity
○ Classified by the function of the immunoglobulins (Ig)
○ Type I (IgE mediated)
■ IgE bounds to mast cells and trigger release of histamine
■ Initial exposure producing no symptoms
■ Common allergens: latex, insect stings, medications, foods (shellfish,
peanuts, eggs)
■ S/S depends on local vs widespread release of histamine
■ Allergic reaction
● Hives, urticaria, eczema, rhinitis, asthma, headache, diplopia,
dizziness, diarrhea, flatulence, distention, GI/GU pain, urinary
frequency
■ Anaphylaxis reaction
● Occurs rapidly, producing severe respiratory and cardiac
signs and symptoms and causing a feeling of “impending
doom”
● Increased eosinophil count
● Sudden rhinitis, itching eyes and skin, flushing, weakness
● Stridor, wheezing, dyspnea, chest tightness, coughing
● Hypotension, tachycardia, pallor, syncope, confusion
■ Treatment
● Airway management is the priority
○ Elevated HOB, bronchodilators, intubation
● Medications
○ Epinephrine, antihistamine (Benadryl), steroids
● Education: avoid trigger, have EpiPen available, obtain a
medic-alert bracelet
○ Types II (IgG-mediated)
■ Destruction of the cells with the antigens attached by activating the
complement cascade or cytotoxic T cells
■ Examples include: hemolytic anemia, immune thrombocytopenia
■ Hemolytic anemia
Disclaimer: This study guide is intended for educational purposes only.
● Premature destruction of RBCs and the remaining fragments lead
to vessel occlusion and circulatory compromise
● Caused by mismatched blood transfusion, Rh incompatibility
during pregnancy (Rh + mother builds antibodies to the infant’s Rh
+ blood)
■ Thrombocytopenia
● Increased destruction of platelets due to medications
(Heparin-induced thrombocytopenia) or immune thrombocytopenia
purpura (ITP)
● Platelet transfusion usually NOT preferred and only indicated if
count is less than 20,000 or patient is actively bleeding
○ Type III (immune complex-mediated hypersensitivity)
■ Antigen-antibody forms “immune complexes” with invasion of leukocytes
and accumulates in vasculature causing skin, joint, and glomerular
inflammation
■ Examples include glomerulonephritis, rheumatoid arthritis, SLE (lupus)
■ Systemic S/S usually occur over 1-2 weeks after allergen exposure
● Fever, systemic rash, joint/skin inflammation and pain, pruritus,
lymphadenopathy, proteinuria
○ Type IV (cell-mediated hypersensitivity)
■ Activation and accumulation of macrophages and cytotoxic T cells at the
site
■ Delayed reaction; antibodies not involved
■ Examples include contact dermatitis, tuberculin reaction, transplant
rejection
Pernicious Anemia
● An autoimmune disorder that can cause malabsorption of Vitamin B12 and permanent
damage to nerves and other organs
● Deficiency of Vitamin B12 affects RBCs production and the nervous system
● Treatment: requires life-long injection of Vitamin B12
Systemic Lupus Erythematosus (SLE)
● An autoimmune disorder in which the T cells attack the body’s own cells, serum proteins,
and tissues
● Joints, skin, kidneys, blood cells, brain, heart, and lungs can be affected
● Risk factors: female gender, genetic predisposition, certain ethnicities (African
Americans, Asian Americans, and Native Americans), sun burns, infections, sulfa drugs
● S/S: usually vague: fever, fatigue
● Treatments
○ There is no cure; supportive treatment with the following
○ NSAID (contraindicated with kidney involvement)
○ Corticosteroids, immunosuppressants, IVIG
○ Targeted therapy (Belimumab)
Disclaimer: This study guide is intended for educational purposes only.
○ Antimalarial medications: hydroxychloroquine (effective for cutaneous lesions)
○ Sodium restriction and good skin care and sun protection
Acquired Immunodeficiency Syndrome (AIDS)
● HIV is a blood borne virus that attacks the T cells resulting in immune system
suppression
● AIDS is third stage of HIV infection and defined as
○ HIV infection + CD4 count <200
○ Or one or more of AIDS defining conditions such as opportunistic infections,
kaposi sarcoma, Non-Hodgkin’s lymphoma, Wasting syndrome
● HIV can be transmitted in blood, semen, vaginal fluid, and breast milk
○ Standard precaution
● Diagnostic testing for HIV i
○ Initially involves highly sensitive antibody screenings (such as enzyme
immunoassay and rapid HIV antibody tests)
■ A positive screening result does not confirm HIV and a negative screening
does not rule out HIV
■ A window period exist during which antibodies and the HIV antigen are
absent or too low to be detected
○ Followed by confirmatory tests (such as Western blot or indirect
immunofluorescence assay tests)
● Treatment
○ Highly active antiretroviral therapy (HAART)
○ Pre and post exposure prophylaxis
○ Education on safe sexual practice, nutritional needs, routine medical care and
immunization, safety measures, psychosocial support, close monitoring for early
symptoms of opportunistic infections
Disclaimer: This study guide is intended for educational purposes only.
Integumentary System
● Three layers
○ Epidermis: avascular, secretes keratin, produces melanin, absorbs vitamin D,
differs in thickness
○ Dermis: vascular, contains nerve endings, hair follicles, oil glands, connective
tissue
○ Subcutaneous: vascular, contains connective tissue, fat
● Diagnostics
○ Skin, wound cultures
○ Skin biopsy
○ Patch test or scratch test for allergens
○ Wood’s light exam: illuminate areas of blue-green or red fluorescence in the
presence of certain skin infections
○ Diascopy exam: lens pressed against skin to evaluate the size and shape
underlying lesions
Pressure injury
● Tissue damage resulting from skin and soft tissue compression, shear and/or friction for
extended periods of time
● Risk factors
○ Sensation and mobility deficits
○ Bed and chair bound
○ Excessive skin moisture (incontinence)
○ Fragile skin, friction, skinny (decreased subcutaneous fats)
○ Nutritional deficiency
○ Altered mental status, older age
● Assessment
○ Braden scale: pressure ulcer risk assessment
○ Assessment and documentation are required on admission and every shift
(or daily at a minimum)
● Stages
○ Stage I: non-blanchable redness, intact skin
■ May appear differently in darkly pigmented skin
■ Color change does not include purple or maroon discoloration (which may
indicate DTI)
○ Stage II: partial thickness skin loss with exposed dermis
■ The wound bed is pink or red, moist
■ Non-stick dressings that retain moisture in the wound bed are needed
○ Stage III: full-thickness skin loss
■ Adipose tissue is exposed (but not tendon, muscle, or bone)
■ Can have undermining and tunneling
■ Can require debridement
○ Stage IV: full thickness skin loss exposing tendon, muscle, or bone
■ Frequent undermining and tunneling
Disclaimer: This study guide is intended for educational purposes only.
○ Unstageable
■ Full thickness but base covered with slough and/or eschar so the extend
of tissue damage cannot be confirmed
○ Deep tissue injury (DTI)
■ Purple or maroon discolored skin area resulting from pressure or shearing
■ Can present as firm or boggy, warm or cool, and with or without pain
● Interventions
○ Frequent skin assessment (especially on bony prominences)
○ Keep skin clean and dry
○ Minimize shearing or drying of skin
○ Protect skin from medical devices
○ Bed bound patients must be turned Q2H and every hour when chair bound
○ Placed on pressure-relieving mattresses (waffle mattress, air bed)
○ HOB not >30 degree for prolonged period of time
○ Avoid massaging over ulcers
● Wound healing
○ Primary intention
■ Healing with clean, non-infected wounds
■ Well approximated edges and minimal scar formation (surgical wound
closure with sutures, small cuts)
○ Secondary intention
■ Infected wounds or wounds with edges that are not approximated
■ Healing by granulation (the primary type of tissue that will fill in a wound
that is healing)
■ Needs to keep wound bed moist: wet to dry dressings
■ Wide scare
○ Tertiary intention
■ Delayed wound closure; no sutures placed or sutures have degraded
■ Granulation developing in two opposing areas
● Requires packing
■ Large, wide, deep scars
○ Dressings
■ Moisture-retentive dressings
● Hydrocolloids, hydrogels, alginates
● Keep the wound bed moist and promote healing
■ Occlusive dressings
● Foam, gauze
● To cover topical medications
■ Autolytic debridement
● Use of collagenase (an enzyme that breaks down necrotic tissue)
over the affected area only, not on the intact skin surrounding the
wound bed
■ Negative pressure therapy
Disclaimer: This study guide is intended for educational purposes only.
● Involves applying a special foam and using a vacuum device that
creates a constant negative air pressure around the wound
● To drain excess fluid and promotes healing
○ Drains
■ Penrose drain
● flat and flexible open tube that drains by gravity
● Not suture in place; a safety pin is attached to the tube to prevent
migration backwards into the wound
■ JP drain & Hemovac
● Closed drainage system by vacuum pressure
● JP can contain up to 50 ml and Hemovac up to 500 ml
Skin cancers
● Types
○ Basal cell carcinoma (BCC)
■ Epidermal tumor
■ Most common and has a good prognosis if treated early
■ Common on the head, neck, and arms
○ Squamous cell carcinoma (SCC)
■ Epidermal tumor
■ Can become invasive and can spread to lymph nodes
○ Malignant melanoma
■ Highly malignant and metastatic
■ Risk factors: genetic predisposition, sun exposure, moles
○ Kaposi’s sarcoma
■ A cancer of the vasculature and forms purplish-reddish skin lesions
■ In those who are immunosuppressed
■ Common on the nose tip, eyelid, oropharynx, penis, thigh, sole of the foot
● Risk factors: sun/UV light exposure, older male, smoking, lighter skin color, blue or green
eyes, blonde or red hair
Other skin disorders
● Psoriasis and eczema
○ Both are incurable skin conditions that cause red, inflamed skin
○ Both are NOT infectious
○ Psoriasis
■ Red, itchy plaques, loose silvery-colored scales
■ Common in scalp, elbows, palms, knees, soles, pitting/depression in nail
○ Eczema
■ Red, peeling/cracked areas, small blisters, scaly with no dead skin
■ Intense itching
■ Can be in any body parts
○ Patient education
■ Good hygiene/skin care, keep skin moist
■ Avoid harsh soaps/detergents, environmental irritants
Disclaimer: This study guide is intended for educational purposes only.
■ Stress management
● Cellulitis
○ An acute bacterial invasion of the skin and subcutaneous tissue
○ S/S: warmth, redness, edema, tenderness, drainage, low grade fever,
leukocytosis
○ Culture & sensitivity: culture of the area diagnoses the pathogen and sensitivity
verifies the susceptibility of the pathogen to specific antibiotics
○ Monitor blood sugar in diabetic patients (due to impaired wound healing)
○ IV or PO antibiotics, topical treatment
○ Warm, moist compress, extremity elevation
● Herpes
○ Herpes Simplex (HSV-1, HSV-2)
■ Occurs around the mouth or genital area
■ Spreads via oral to oral, oral to genital contact, and sexual contact
■ Is not curable and is contagious no matter symptomatic or not
■ S/S begin 3-7 days after contact
■ Tenderness, pain, tingling and burning happens before vesicles appear
■ Treatment: antiviral, skin hygiene and care, avoid secondary infection
○ Herpes Zoster (Shingles)
■ Reactivation of shingles and remains contagious until the rash crusted
over
■ Risk factors: immunocompromised, age > 50
■ Eruption of small, red blisters with severe pain, burning, or pruritis
■ Common on the trunk and buttocks; but does NOT cross the body’s
midline
■ Treatment: antiviral, topical steroids, pain control
Disclaimer: This study guide is intended for educational purposes only.
Theories in Nursing
Maslow’s Hierarchy of Needs
● Physiological needs and safety must be satisfied before individuals can attend to higher
psychological needs
● Always address physiological needs before psychological (unless the question is
specifically asking for psychological interventions)
● First level: Physiological needs
○ Air, water, food, shelter, sleep, clothing, reproduction
● Second level: Safety needs
○ Personal security, employment, resources, health, property
● Third level: Love and belonging
○ Friendship, intimacy, family, sense of connection
● Fourth level: Esteem
○ Respect, self-esteem, status, recognition, strength, freedom
● Fifth level: Self-actualization
○ Desire to become the most that one can be
Kubler-Ross Stages of Grief
● Denial: avoidance, confusion, shock/fear
● Anger: frustration, irritability, anxiety
● Bargaining: struggle to find meaning, to help others, to tell your own story
● Depression: helplessness, hostility, avoidance
● Acceptance: exploring opportunities, introducing new plans, moving forward
Types of grief
● Anticipatory grief
○ A grief reaction that occurs in anticipation of an impending loss
○ About 25% of patients with incurable cancer experience anticipatory grief
○ More likely to occur among individuals with dependent relationships, limited
external social support, lower levels of education, undergoing a spiritual crisis
● Normal or common grief
○ Are marked by gradual movement toward an acceptance of the loss
○ Occur in 50%-85% of persons after they experienced a loss
● Difference between grief and depression
○ In grief, painful feelings come in waves, lessen in intensity and frequency over
time, and are often intermixed with positive memories of the deceased; in
depression, mood and ideation are constantly negative.
○ In grief, the prevailing effect is one of emptiness; in major depression, it is a long,
sustained, depressed mood and an inability to expect pleasure or happiness.
○ In grief, self-esteem is usually preserved; in major depression, feelings of
worthlessness and self-loathing are common.
○ In grief, while symptoms such as suicidal ideation can occur, they are generally
focused on the deceased, such as a wish to join the deceased in death or
feelings of guilt toward certain gaps or failures in the relationship with the
Disclaimer: This study guide is intended for educational purposes only.
deceased. In major depression, suicidal ideation is more likely directed at self
only.
● Complicated grief: a lack of normal mourning or an extended mourning period that does
not lessen in intensity with time
Kurt Lewin Change Management Model: Unfreeze, Change, Freeze
● Stage I: Unfreezing
○ Recognizes that change is necessary and overcomes the strains of individual
resistance
● Stage II: Change (or transition)
○ Process of change in feeling, behavior, thoughts
○ Occurs as changes are being made
○ Hardest
● Stage III: Freezing (Refreezing)
○ Establishing stability once the changes have been made
○ The changes are accepted and become the new norm
Patricia Benner: From Novice to Expert
● Describes 5 levels of nursing experience
○ Novice
○ Advanced beginner
○ Competent
○ Proficient
○ Experience
Patient Education
● Learning needs: the gap between what someone knows and what someone wants or
needs to know
○ Identify the learner
○ Choose the right setting/environment
○ Collect data about the learner: determining the characteristic needs of the target
audience
○ Collect data from the learner: allowing the patient and/or family to identify what is
important to learn and what resources are available
○ Involve members of the healthcare team
○ Prioritize needs: Maslow’s hierarchy of needs
○ Determine availability of educational resources
○ Assess demands of the organization: being knowledgeable of the standards of
performance of the microsystem
○ Take time-management issues into account
● Key principles of adult learning
○ Adults want to know why they should learn; “what is in it for me?”
○ Adults need to be seen and treated as being capable of taking the responsibility
to learn
Disclaimer: This study guide is intended for educational purposes only.
○ Adults bring experience to learning
○ Adults are ready to learn when the need arises. The desire to learn usually
coincides with the transition from one developmental stage to another is related
to developmental task, such as career planning, acquiring job competencies,
improving job performance
○ Adults are task oriented
Disclaimer: This study guide is intended for educational purposes only.
Test Taking Tips
Focus on the following while studying
● keywords/phrases that are bolded throughout this study guide
● Lifestyle modification for diseases/conditions (for example, diet change for diabetes,
fluid/Na restriction for CHF)
● Patient education on side effects of medications, precautions, what to look out for
● Focus on the symptoms and interventions/treatments
○ Know the most common symptoms or symptoms that are specific to the disease
○ Consider the less invasive and less expensive intervention first
■ For ex, choose medications first before surgery
● Nursing process
○ Assessment, analysis, plan, intervention, evaluation
○ Follow the orders of the nursing process (unless the question specially asks for
one aspect; “how does the nurse evaluate the patient’s understanding of taking
this medication?”)
How to approach the questions?
● Read the directions carefully
● Identify words that help you understand what the question is asking
○ Is it asking for an assessment?
■ Then you can rule out answers with interventions
○ Words related to time
■ Preop vs postop, during, after, first, initially, early vs late side effect
○ Specific keywords
■ NOT, LEAST, EXCEPT, MOST
● Think of possible answers before reading the answer choices
● Do not read into the question
How to approach answer choices?
● Keep in mind that the correct answers will be “textbook” and evidence based
○ Do not make assumptions based on your experience or facility protocols
○ For the test, you have all the resources/supplies available
● Modest words are more likely true: sometimes, often, many, few, generally
● Avoid answers with absolute words: always, never, only, must, completely
● Prioritize
○ Airway
○ Circulation
○ Maslow’s hierarchy of needs (physiological needs and safety before
psychological needs)
● When in doubt
○ Keep your first answer choice (unless you have a strong reason not to)
○ Pick lengthy or highly specific answers
○ When an answer choice has two parts, both of them need to be correct
Disclaimer: This study guide is intended for educational purposes only.
You might also like
- Immediate Life Support for healthcare Practitioners: A Step-By-Step GuideFrom EverandImmediate Life Support for healthcare Practitioners: A Step-By-Step GuideNo ratings yet
- EKG | ECG Interpretation. Everything You Need to Know about 12-Lead ECG/EKG InterpretationFrom EverandEKG | ECG Interpretation. Everything You Need to Know about 12-Lead ECG/EKG InterpretationRating: 3 out of 5 stars3/5 (1)
- KNES320 NotesDocument55 pagesKNES320 NotesOlamide GNo ratings yet
- RT 105 Finals NotesDocument24 pagesRT 105 Finals NotesLouiseNo ratings yet
- 12 Drugs Acting On The Cardiovascular SystemDocument7 pages12 Drugs Acting On The Cardiovascular SystemJAN CAMILLE LENONNo ratings yet
- CARDIOVASCULARDocument9 pagesCARDIOVASCULARcsfcfssfNo ratings yet
- 12 Drugs Acting On The Cardiovascular SystemDocument5 pages12 Drugs Acting On The Cardiovascular SystemJAN CAMILLE LENONNo ratings yet
- Cardiovascular SystemDocument11 pagesCardiovascular SystemJanet Floreno VillasanaNo ratings yet
- Cvs 253Document253 pagesCvs 253CHALIE MEQUNo ratings yet
- Heart FailureDocument21 pagesHeart FailureJazzy Kathlene Dumable0% (1)
- Tara's Anatomy and Physiology - Aehlert ECGs Made EasyDocument16 pagesTara's Anatomy and Physiology - Aehlert ECGs Made EasyTara McNeillNo ratings yet
- Learning Material - Introduction To Cardiovascular DrugsDocument12 pagesLearning Material - Introduction To Cardiovascular DrugskristiannedenNo ratings yet
- Critical Care and Small Bowel ObstructionDocument16 pagesCritical Care and Small Bowel Obstructionsofea zamriNo ratings yet
- 07 Heart Pathology (Part 1 and 2)Document13 pages07 Heart Pathology (Part 1 and 2)carlgangcaNo ratings yet
- Anatomy 3 MidtermDocument17 pagesAnatomy 3 MidtermCourtney FlaniganNo ratings yet
- Wk6-AF&Arrhythmia 2021Document49 pagesWk6-AF&Arrhythmia 2021Khashayar MastooriNo ratings yet
- Medsurg 3 Exam 1Document55 pagesMedsurg 3 Exam 1Melissa Blanco100% (1)
- CVS & HypertensionDocument92 pagesCVS & HypertensionNimesh ModiNo ratings yet
- Viva Emergencies & EthicsDocument93 pagesViva Emergencies & EthicsPei Xing KwekNo ratings yet
- Structure of The Heart TransesDocument6 pagesStructure of The Heart TransesReign SaplacoNo ratings yet
- Cardiovascular AssessmentsreviewDocument34 pagesCardiovascular AssessmentsreviewLydia Lopz MsnrncdNo ratings yet
- Cardio Renal MedicationsDocument14 pagesCardio Renal MedicationsHarly E. DeniegaNo ratings yet
- Med Surg MidtermDocument17 pagesMed Surg Midtermjhan grabierNo ratings yet
- Cardiovascular System: Dr. Dipti VasaniDocument52 pagesCardiovascular System: Dr. Dipti Vasaniaarti HingeNo ratings yet
- Critical CareDocument25 pagesCritical Carejassen karylle IbanezNo ratings yet
- Seeley's Essentials of Anatomy & Physiology Chapter 12 Seeley's Essentials of Anatomy & Physiology Chapter 12Document11 pagesSeeley's Essentials of Anatomy & Physiology Chapter 12 Seeley's Essentials of Anatomy & Physiology Chapter 12Aysha AishaNo ratings yet
- Cardiovascular 1Document7 pagesCardiovascular 1simonedarling100% (2)
- Cardio NclexDocument40 pagesCardio NclexGabrielle WashingtonNo ratings yet
- Cardio-Vascular ExaminationDocument43 pagesCardio-Vascular ExaminationDimas FrasesaNo ratings yet
- CA - Adult Health Nursing PDFDocument55 pagesCA - Adult Health Nursing PDFMarvin Heramis RyanNo ratings yet
- Blood PressureDocument57 pagesBlood PressureMatende husseinNo ratings yet
- CardiologyDocument44 pagesCardiologyJim XieNo ratings yet
- Cardiology & Ekgs: Archer Nclex ReviewDocument59 pagesCardiology & Ekgs: Archer Nclex Reviewdaphne farleyNo ratings yet
- HLTAAP002 CardiovascularDocument56 pagesHLTAAP002 CardiovascularJesse SimonNo ratings yet
- Cardiovascular SystemDocument51 pagesCardiovascular SystemClarice AsenjoNo ratings yet
- Ventricel Septal DefectDocument38 pagesVentricel Septal DefectzaipullahNo ratings yet
- Basics of Cath LabDocument121 pagesBasics of Cath LabizalxrayNo ratings yet
- Cardiac 1 Conduction Disorders I 6Document28 pagesCardiac 1 Conduction Disorders I 6nkurian1No ratings yet
- Cardio N41Document13 pagesCardio N41ashafernandesssNo ratings yet
- LA Cardiac Arythmia - 0Document61 pagesLA Cardiac Arythmia - 0Karthik SNo ratings yet
- Lab 5 Cardiovascular Examination, ECG and BPDocument43 pagesLab 5 Cardiovascular Examination, ECG and BP202310446No ratings yet
- EKG Reading Basics - Inservice Summer 2016Document39 pagesEKG Reading Basics - Inservice Summer 2016Anonymous 5kykKe2QLWNo ratings yet
- Cardiovascular Physiology Pre-Lab LectureDocument33 pagesCardiovascular Physiology Pre-Lab LecturenayoonNo ratings yet
- Notes On Ciculatory SystemDocument7 pagesNotes On Ciculatory SystemAmr KhalilNo ratings yet
- Cardiovascular Physiology & Urine Formation: Biology 25 A. SantiagoDocument39 pagesCardiovascular Physiology & Urine Formation: Biology 25 A. Santiagoapi-3826751No ratings yet
- Crat - Cardio PulmoDocument11 pagesCrat - Cardio PulmoJULIANE MAE BALANGNo ratings yet
- Cardiovascular SystemDocument20 pagesCardiovascular SystemFisco DessereiNo ratings yet
- Cardiac Physiology Circulatory System: BIOL212 11/8Document96 pagesCardiac Physiology Circulatory System: BIOL212 11/8mary ann aquinoNo ratings yet
- Heart & Neck Vessels Assessment: Kousar Perveen Assistant Professor The University of LahoreDocument43 pagesHeart & Neck Vessels Assessment: Kousar Perveen Assistant Professor The University of LahoreChenii RoyNo ratings yet
- Chapter 2 - CardiovascularDocument74 pagesChapter 2 - CardiovascularNoriani ZakariaNo ratings yet
- Responses To Altered Oxygenation, Cardiac and Tissue - Anatomy To AssessmentDocument254 pagesResponses To Altered Oxygenation, Cardiac and Tissue - Anatomy To Assessmentlouradel100% (1)
- 10 Medical Surgical Nursing Intensive Review PDFDocument68 pages10 Medical Surgical Nursing Intensive Review PDFShanine Alexia CordovezNo ratings yet
- Cardiology: DR Isaak M Osman MBCHB, Mmed Int. Medicine/Cardiology 10 Sept 2019Document19 pagesCardiology: DR Isaak M Osman MBCHB, Mmed Int. Medicine/Cardiology 10 Sept 2019Imraan MohaNo ratings yet
- Valvular Heart DiseaseDocument43 pagesValvular Heart Diseaseurmila prajapatiNo ratings yet
- Spiro Me TryDocument24 pagesSpiro Me TryVanissa Taehyung KimNo ratings yet
- Heart Failure: Andi Wahjono Adi, MD, FIHADocument46 pagesHeart Failure: Andi Wahjono Adi, MD, FIHAYuanita WahyuningsihNo ratings yet
- Cardiovascular Examination:: General InspectionDocument6 pagesCardiovascular Examination:: General InspectionPhysician AssociateNo ratings yet
- Cardiovascular ExaminationDocument54 pagesCardiovascular ExaminationsankethNo ratings yet
- Physiology 09Document36 pagesPhysiology 09Sumeyya Binte BockthierNo ratings yet
- EKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!From EverandEKG and ECG Interpretation: Learn EKG Interpretation, Rhythms, and Arrhythmia Fast!No ratings yet
- Aids & Cancer Disease Hindu MantraDocument3 pagesAids & Cancer Disease Hindu MantralalagopegapangamdassNo ratings yet
- AACPDM Guidelines For Sialorrhea in Children With Cerebral PalsyDocument4 pagesAACPDM Guidelines For Sialorrhea in Children With Cerebral PalsyDr.Shridhar joshi100% (1)
- Acute Respiratory Distress Syndrome by Mr. Ashish RoyDocument45 pagesAcute Respiratory Distress Syndrome by Mr. Ashish RoySyedzulqurnainhussainshah ZulqurnainNo ratings yet
- Sign, Sypmtoms and Tretment of PosioningDocument18 pagesSign, Sypmtoms and Tretment of PosioningmaryamNo ratings yet
- Bu Erger 'S Disea Se OR Thromboan Gitis Obliter An S (TAO) : DR Bhupendra Chouhan Assistant ProfessorDocument19 pagesBu Erger 'S Disea Se OR Thromboan Gitis Obliter An S (TAO) : DR Bhupendra Chouhan Assistant ProfessorAnupam MantriNo ratings yet
- Epidermolysis Bullosa in Animals A ReviewDocument13 pagesEpidermolysis Bullosa in Animals A Reviewalejandro sotoNo ratings yet
- Vedanta Ias General ScienceDocument24 pagesVedanta Ias General ScienceChinmay JenaNo ratings yet
- A CASE PRESENTATION ON CELLULITIS by RuqiyaDocument16 pagesA CASE PRESENTATION ON CELLULITIS by RuqiyaSafoora Rafeeq50% (2)
- Definitions: The Social Determinants of Health. SummaryDocument4 pagesDefinitions: The Social Determinants of Health. SummaryS VaibhavNo ratings yet
- Table Atrial FlagellatesDocument4 pagesTable Atrial FlagellatesNinaRicaR.RamosNo ratings yet
- Suicide Attempts in First-Episode PsychosisDocument6 pagesSuicide Attempts in First-Episode PsychosisAdam García BuenoNo ratings yet
- MCQs On Esophagus and ThyroidDocument2 pagesMCQs On Esophagus and ThyroidvaegmundigNo ratings yet
- Triprolidine: What Is in This LeafletDocument6 pagesTriprolidine: What Is in This LeafletDara PuspitaNo ratings yet
- Too Much Water Too Little Water Class 4 Notes CBSE EVS Chapter 18 (PDF)Document4 pagesToo Much Water Too Little Water Class 4 Notes CBSE EVS Chapter 18 (PDF)ANJALI 4856100% (1)
- Genital Herpes: Aarthi (2012)Document36 pagesGenital Herpes: Aarthi (2012)Aiman TymerNo ratings yet
- Delirium Using The 4AT AssessmentDocument10 pagesDelirium Using The 4AT AssessmentAna KmaidNo ratings yet
- Practical Bacteriology Laboratory Manual: Prepared byDocument37 pagesPractical Bacteriology Laboratory Manual: Prepared bysalamon2tNo ratings yet
- Case Study of AnemiaDocument3 pagesCase Study of AnemiaAmina Tariq100% (1)
- On Farm BiosecurityDocument26 pagesOn Farm BiosecurityAvskilt MazidNo ratings yet
- Nursing Responsibilities During Radiation TherapyDocument59 pagesNursing Responsibilities During Radiation TherapyJhe Victoriano91% (22)
- A Nationwide Population-Based Study On The Incidence of Parapharyngeal and Retropharyngeal Abscess-A 10-Year StudyDocument7 pagesA Nationwide Population-Based Study On The Incidence of Parapharyngeal and Retropharyngeal Abscess-A 10-Year StudyfayzaNo ratings yet
- Acute Upper Airway Obstruction in Children: Paediatric Anaesthesia Tutorial 368Document9 pagesAcute Upper Airway Obstruction in Children: Paediatric Anaesthesia Tutorial 368Fireka JuniantikaNo ratings yet
- Prepared By, Gayathri R 2 Yr MSC (N) UconDocument41 pagesPrepared By, Gayathri R 2 Yr MSC (N) UconGayathri RNo ratings yet
- Free Somatics: Reawakening The Minds Control of Movement, Flexibility, and Health PDFDocument6 pagesFree Somatics: Reawakening The Minds Control of Movement, Flexibility, and Health PDFRajesh S VNo ratings yet
- Homoeopathy BookletDocument66 pagesHomoeopathy BookletNafisa AhmadNo ratings yet
- Introduction To VirologyDocument30 pagesIntroduction To VirologyAkshaya MistryNo ratings yet
- Chapter 1 ParasitologyDocument47 pagesChapter 1 ParasitologyYvn C.No ratings yet
- Maestro2003 InglesDocument16 pagesMaestro2003 Inglesmarta alejandre rodriguezNo ratings yet
- Diuretics: Chris Hague, PHDDocument29 pagesDiuretics: Chris Hague, PHDranachamanNo ratings yet
- Measures and Effective Methods of Treatment Against Ichthyobodosis (Costiosis) Disease of FishDocument4 pagesMeasures and Effective Methods of Treatment Against Ichthyobodosis (Costiosis) Disease of FishAcademic JournalNo ratings yet