Professional Documents
Culture Documents
Male Reproductive Histology
Uploaded by
Carmela MarianoCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Male Reproductive Histology
Uploaded by
Carmela MarianoCopyright:
Available Formats
MICRO ANATOMY
HISTOLOGY OF MALE REPRODUCTIVE SYSTEM (2ND SEMESTER) | (DR. PERALDO) | (01-07-20)
OUTLINE III. SEMINIFEROUS TUBULES
I. MALE REPRODUCTIVE SYSTEM
II. TESTES
• Convoluted tubules lined with a complex stratified
III. SEMINIFEROUS TUBULES
IV. SERTOLI CELLS epithelium
V. GENITAL DUCTS • Terminates in short segments, known as straight tubules
VI. PENIS or tubuli recti to the rete testis.
VII. MEDICAL APPLICATION About 10-20 efferent ductules connect the rete testis to
VIII. APPENDICES the head of the epididymis.
Each seminiferous tubule is lined with a complex
specialized stratified epithelium called germinal or
spermatogenic epithelium.
Spermatogenic epithelium consists of:
o Sertoli Cells
o Spermatogenic Lineage
I. MALE REPRODUCTIVE SYSTEM
• Male reproductive system consists of the
o Testes
o Genital ducts:
▪ INTRATESTICULAR: tubuli recti, rete
testes, ductuli efferentes
▪ EXCRETORY: ductus epididymis, ductus
(vas) deferens, ejaculatory duct, urethra
o Accessory Glands: seminal vesicles, prostate,
bulbourethral gland and Penis.
• Testes produce sperm but also contain endocrine cells
such as TESTOSTERONE. Testosterone is important for
spermatogenesis and sexual differentiation.
• Genital ducts and accessory glands produce secretions
required for sperm activity and contract to propel
spermatozoa.
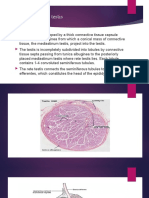
II. TESTES LAYERS
• Male gonads, paired organs lying in the scrotal sac 1. Tunic of fibrous connective tissue - consists of
• Responsible for production of male gametes, several layers of fibroblasts
spermatozoa and secretion of male sex hormones 2. Basal lamina - adhering to it are flattened cells,
• Surrounded by thick capsule of collagenous connective myoid cells
tissue, the tunica albuginea 3. Germinal epithelium – consists of two types of cells:
• Suspended in the scrotum and carries serous sac, the sertoli cells and cells that constitute the spermatogenic
tunica vaginalis derived from the investing layer of lineage
peritoneum
• Divided by collagenous septa into about 250 testicular The Germinal or Seminiferous Epithelium
lobules each with one to four highly convoluted tubes, the
seminiferous tubules
Develop retroperitoneally in the dorsal wall of the
embryonic abdominal cavity.
Permissive temperature of about 34 Celsius is maintained
in the scrotal sac. Each testicular artery is surrounded by
pampiniform venous plexus containing cooler blood from
testis, which draw heat from arterial blood by
countercurrent heat exchange system.
Contraction or relaxation of Dartos Muscle move the
testes away from or closer to the body.
MICRO ANATOMY CRUCILLO 1 of 7
MICRO ANATOMY
HISTOLOGY OF MALE REPRODUCTIVE SYSTEM (2ND SEMESTER) | (DR. PERALDO) | (01-07-20)
IV. SERTOLI CELLS
• Tall “columnar” epithelial cells that nourish the
spermatogenic cells.
• Rest on the basement, cytoplasm extends to the lumen
of the tubules.
• Fills the narrow spaces between the spermatogenic
series.
• Elongated pyramidal cells with oval nucleus with
numerous unfoldings and prominent nucleolus. B. Primary Spermatocytes
• Cytoplasm: contains abundant SER, some RER, well • Spherical cells with Euchromatic nuclei
developed golgi complex, numerous mitochondria and • Recognized by their copious cytoplasm and large nuclei
lysosomes. containing coarse clumps or thin threads of chromatin
• Adjacent cells bound together by occluding junction • IN EM, dividing cells can be seen
forming the blood testis barrier that prevents • Enters 1st meiotic division
autoimmune attacks against the unique spermatogenic • Largest cells of the series and are characterized by
cells. presence of chromosomes in various stages of the coiling
process within their nuclei.
C. Secondary Spermatocytes
• less commonly seen in sections of the testes
• Short-lived cells, remain in the interphase very briefly
and quickly enters the second meiotic division
D. Spermatids
• Cells that result from the division of the secondary
spermatocytes
• Undergo long maturation process known as
spermiogenesis
• Small size cells, nuclei with areas of condensed
chromatin and less granular cytoplasm
Spermiogenesis
• Final phase of Sperm Production
• No cell division occurs here
FUNCTIONS OF SERTOLI CELLS • Complex process of differentiation that includes:
1. Support, protection and nutritional regulation of the 1. Formation of acrosome
developing spermatozoa 2. Condensation and elongation of the nucleus
2. Phagocytosis – thru action of lysosomes 3. Development of the flagellum
3. Secretion – fluid used for sperm transport, ABP 4. Loss of the much of the cytoplasm
(Androgen Binding Protein), converts testosterone to • End result: formation of spermatozoon
estradiol, and inhibin
4. Production of the anti-mullerian hormone or Mullerian 4 Phases of Spermiogenesis accdg to Junqueira:
Inhibiting Substance 1. Golgi Phase
I. Cause regression of the embryonic Mullerian 2. Cap Phase
duct or regression of manifestation of female 3. Acrosome Phase
reproductive organs. 4. Maturation Phase
E. Spermatozoa
Cells of the Spermatogenic Series • Extremely elongated cell (about 65 um long)
A. Spermatogonia (germ cells) • Main components: head, neck, and tail
• Found in basal layer
• Of two types: stem cells (Type A spermatogonia)
spermatogonia committed to meiosis (Type B
spermatogonia)
MICRO ANATOMY CRUCILLO 2 of 7
MICRO ANATOMY
HISTOLOGY OF MALE REPRODUCTIVE SYSTEM (2ND SEMESTER) | (DR. PERALDO) | (01-07-20)
INTERSTITIAL TISSUE
• Space between seminiferous tubules
• Filled with accumulations of connective tissue, nerves,
blood and lymphatic vessels
LEYDIG CELLS or INTERSTITIAL CELLS
• Principal cell type
• Rounded or polygonal in shape with central nucleus
and an eosinophilic cytoplasm rich in small lipid
droplets
• Occur simply or in clumps embedded in the rich
plexus of blood and lymph capillaries
• Produce the male hormone TESTOSTERONE
V. GENITAL DUCTS
INTRATESTICULAR GENITAL DUCTS
All of which carry spermatozoa and liquid from the
seminiferous tubules to the duct of the epididymis.
1. Tubuli Recti
• Aka Straight tubules
• Recognized by gradual loss of spermatogenic cells
• Initial segment contains only Sertoli cell, then main
segments consisting of cuboidal epithelium
supported by dense CT.
• Empty into rete testes
MAIN COMPONENTS OF SPERMATOZOON 2. Rete Testes
1. Head • Contained within the mediastinum, thickening of
• Basic structural feature, consists primarily by condensed tunica albuginea
nuclear chromatin • Highly anastomotic channels lined with cuboidal
• Flattened, pear-shaped epithelium with surface microvilli and a single
• Anterior two thirds of nuclear, surrounded by acrosomal flagellum
cap-flattened membrane-bound vesicle containing
glycoproteins and hydrolytic enzymes principally
hyaluronidase
2. Neck
• Very short segment connecting the head with tail
• Contains vestiges of centrioles, that give rise to axoneme
of the flagellum, surrounded by several condensed
fibrous rings
3. Tail – divided into middle piece, principal piece and
end piece
a. Middle piece - proximal part, thickened portion
containing aggregates of mitochondria
- consists of flagellar axonemes surrounded
by fibrous CT around longitudinally 3. Ductuli Efferent
b. Principal piece – constitute most of the tail length • Convoluted ducts that connect rete testes and
c. End piece – short tapering portion of the tail containing epididymis
axoneme only • Lined by single layer of alternating tall columnar
• Both principal piece and end piece are ciliated and short columnar non ciliated
responsible for flagellar motion via interaction • Surrounded by a single circularly arranged smooth
among microtubules, ATP and dynein muscle
MICRO ANATOMY CRUCILLO 3 of 7
MICRO ANATOMY
HISTOLOGY OF MALE REPRODUCTIVE SYSTEM (2ND SEMESTER) | (DR. PERALDO) | (01-07-20)
2. Ductus deferens
• Thick-walled, muscular tube consisting of inner and
outer longitudinal layers separated by a circular layer
of smooth muscle
• Lined by pseudostratified columnar epithelium with
stereocilia
• Forms part of the spermatic cord
• Has a distal dilated portion called ampulla that
receives duct draining the seminal vesicle forming
the short ejaculatory duct
EXCRETORY GENITAL DUCTS
1. Epididymis
• Single, highly coiled tube with surrounding
connective tissue and blood vessels
• Tube of smooth muscle lined by pseudostratified
columnar epithelium with stereocilia
• Function: accumulation, storage, and maturation of
spermatozoa
Important changes in the sperm while passing through
epididymis include:
o Competence for independent forward motility
o Maturation of the acrosome
o Biochemical and organizational changes within
the cell membrane 3. Ejaculatory duct
• Segment entering the prostate
• Ductus deferens + duct of seminal vesicle
4. Urethra
• Prostatic urethrae: lined by transitional epithelium
receives the ductus deferens
• Penile urethrae: lined by stratified or pseudo
stratified columnar epithelium
ACCESSORY GLANDS
1. Seminal Vesicle
• Consists of 2 highly tortous tubes, each is a complex
of glandular diverticulum of associated ductus
deferens
• Viscide, yellow secretion
• Has folded mucosa lined with pseudostratified
columnar epithelium rich in secretory granules
• Secretion: alkaline fluid containing spermatozoa-
activating substances such as fructose, inositol,
citrate and several proteins and Vitamin C (about
half of the total volume of seminal fluid = 70%
volume)
• Lamina propria: rich in elastic fibers and surrounded
by thin layer of smooth muscle, supplied by
sympathetic nervous system.
MICRO ANATOMY CRUCILLO 4 of 7
MICRO ANATOMY
HISTOLOGY OF MALE REPRODUCTIVE SYSTEM (2ND SEMESTER) | (DR. PERALDO) | (01-07-20)
• Epithelium: psedostratified columnar or cuboidal
with basally located nuclei and poorly stained
cytoplasm
• Secretory product: thin and milky rich in citric acid
and hydrolytic enzymes which makes up about half
of the seminal fluid volume
3 Groups of Glands
1. Main prostatic glands – constitute the bulk of the
organ, occupy the peripheral 2/3 and drain via long
ducts
2. Submucosal glands – occupy the inner third of the
gland drain via short ducts into urethral sinuses
3. Mucosal glands – innermost group of glands very
small, not usually visible to in low magnification;
open directly into the urethra over its whole surface
3. Bulbourethral glands (Cowper’s glands)
• Located proximal to the membranous portion of
urethra
• Tubuloalveolar glands lined with mucus secreting
simple cuboidal epithelium
• Secreted mucus is clear and acts as a lubricant
VI. PENIS
• Consist mainly of 3 cylindrical masses of erectile
tissues: corpora cavernosa and corpus spongiosum
• Covered by resistant layer of dense connective tissue
2. Prostate • Epithelium: penile urethra is lined with pseudo
• Large gland which surrounds the bladder neck and stratified columnar but becomes stratified
the first part of the urethra squamous in the glans penis
• Tubulo alveolar glands whose ducts empty into • Glands of Littre: found through out the length of the
prostatic urethra urethra
• Invested by fibro elastic capsule from which • Arterial supply: internal pudendal arteries
incomplete septa extend in toward the central
stroma dividing the glands into poorly defined
lobules
Three Major Zones:
o Transition Zone – 5% of prostate volume,
superior portion of urethra and contains
periurethral mucosal glands.
o Central Zone – 25%
o Peripheral Zone – 70%, contains prostate’s main
glands with longer ducts.
VII. MEDICAL APPLICATIONS
1. HYDROCELE – excessive accumulation of serous fluid in
one or both sides of the scrotal sac; most common cause
of scrotal swelling.
2. CRYPTORCHIDISM - failure of one or both testes to
descend from the abdomen
MICRO ANATOMY CRUCILLO 5 of 7
MICRO ANATOMY
HISTOLOGY OF MALE REPRODUCTIVE SYSTEM (2ND SEMESTER) | (DR. PERALDO) | (01-07-20)
3. TESTICULAR CANCER – involves GERM CELL TUMOR only
appear after puberty and more likely to develop in men
with untreated cryptorchidism.
4. OLIGOSPERMIA - decreased semen quality, major cause
of male infertility.
5. ORCHITIS - inflammation of the testis produced by
infective agents and occur secondarily to UTI or STP such
as Chlamydia or Neisseria gonorrhea.
6. PROSTATE PROBLEMS:
a. CHRONIC PROSTATITIS
b. NODULAR HYPERPLASIA OR BENIGN PROSTATIC
HYPERTROPHY
c. PROSTATE CANCER – usually in PERIPHERAL
ZONE.
7. ERECTILE DYSFUNCTION OR IMPOTENCE – results from
diabetes, anxiety, vascular disease, or nerve damaging
during prostatectomy.
VIII. APPENDICES
MICRO ANATOMY CRUCILLO 6 of 7
MICRO ANATOMY
HISTOLOGY OF MALE REPRODUCTIVE SYSTEM (2ND SEMESTER) | (DR. PERALDO) | (01-07-20)
REFERENCES:
Dr. Peraldo’s PPT Lecture
Junqueira’s Basic Histology
MICRO ANATOMY CRUCILLO 7 of 7
You might also like
- Malereproductive (Author T.globa)Document40 pagesMalereproductive (Author T.globa)Cristina caimac100% (1)
- Male Reproduction System - Histology LectureDocument28 pagesMale Reproduction System - Histology LectureAstri Novia RizqiNo ratings yet
- Structure of The TestisDocument24 pagesStructure of The TestisBassam MohamedNo ratings yet
- Micro - Male Repro (Sec A) PDFDocument5 pagesMicro - Male Repro (Sec A) PDFKaren ValdezNo ratings yet
- Gonad & GametogenesisDocument40 pagesGonad & GametogenesisAnggita DaniellaNo ratings yet
- Summary Notes - Topic 3 Edexcel (A) Biology A-Level PDFDocument8 pagesSummary Notes - Topic 3 Edexcel (A) Biology A-Level PDFmohammedNo ratings yet
- Male Reproductive OrganDocument43 pagesMale Reproductive OrganIsrahia CopiocoNo ratings yet
- Histology of The Testicle Spermatogenesis TZsDocument21 pagesHistology of The Testicle Spermatogenesis TZsYogita BhansaliNo ratings yet
- Gametogenesis and Spermatogenesis ExplainedDocument23 pagesGametogenesis and Spermatogenesis ExplainedhusshamNo ratings yet
- NCM 101 Assessing Male GenitaliaDocument13 pagesNCM 101 Assessing Male GenitaliaKIM KALIBAYNo ratings yet
- 7 Reproductive and Hormonal Functions of The MaleDocument78 pages7 Reproductive and Hormonal Functions of The MaleClarissa CletNo ratings yet
- Male Reproductive System OverviewDocument14 pagesMale Reproductive System OverviewJasmine KaurNo ratings yet
- 13 - Male Reproductive SystemDocument60 pages13 - Male Reproductive SystemWai Kwong ChiuNo ratings yet
- Spermatogenesis Group 4Document20 pagesSpermatogenesis Group 4sugarxglossNo ratings yet
- Chap 15&16Document27 pagesChap 15&16Janine AlintanaNo ratings yet
- Histology of Male Reproductive System: DR G M Kibria UPNM-2 24.4.13Document29 pagesHistology of Male Reproductive System: DR G M Kibria UPNM-2 24.4.13AaronMaroonFiveNo ratings yet
- MRS LabDocument6 pagesMRS Lab2012000600No ratings yet
- Colorful Handwritten About Me Blank Education PresentationDocument27 pagesColorful Handwritten About Me Blank Education PresentationDevone Claire Bolanos GonzalesNo ratings yet
- Voice of The GenomeDocument8 pagesVoice of The GenomehtbfdgNo ratings yet
- Histologymalegenitaltract FinalDocument11 pagesHistologymalegenitaltract FinaljohnllenalcantaraNo ratings yet
- Male Histology Trans-Batch 2023Document11 pagesMale Histology Trans-Batch 2023Hanako Sasaki AranillaNo ratings yet
- EMBRYOLOGY: Gametogenesis, Fertilization in Details.Document46 pagesEMBRYOLOGY: Gametogenesis, Fertilization in Details.Mercy AdeolaNo ratings yet
- Ana Histo MaleDocument4 pagesAna Histo MaleCarlito RiveraNo ratings yet
- Reproductive SystemDocument7 pagesReproductive SystemshaniaericaNo ratings yet
- Spermatogenesis: Feriha Ercan, Ph.D. Dept. Histology and EmbryologyDocument41 pagesSpermatogenesis: Feriha Ercan, Ph.D. Dept. Histology and EmbryologyErdem AltunNo ratings yet
- Devl Biol-SpermatogenesisDocument9 pagesDevl Biol-SpermatogenesisSuresh DavuluriNo ratings yet
- Lecture Notes Module - 3 - Male Reproductive Anatomy and PhysiologyDocument8 pagesLecture Notes Module - 3 - Male Reproductive Anatomy and PhysiologyMariaImranNo ratings yet
- Spermatogenesis Group 3 PresentationDocument10 pagesSpermatogenesis Group 3 Presentationmarkmuiruri581No ratings yet
- Gametogenesis p1 PDFDocument13 pagesGametogenesis p1 PDFLiane LomioNo ratings yet
- Histology Department Medical Faculty Bandung Islamic UniversityDocument51 pagesHistology Department Medical Faculty Bandung Islamic UniversityRizal AuliaNo ratings yet
- Anatomy 2nd-U-6 Reproductive SystemDocument134 pagesAnatomy 2nd-U-6 Reproductive Systemsinte beyuNo ratings yet
- Fk-Umi: Dr. Kamajaya, MSC, SpandDocument68 pagesFk-Umi: Dr. Kamajaya, MSC, SpanddebiNo ratings yet
- MCN Lec M1L3B ReviewerDocument6 pagesMCN Lec M1L3B ReviewerEmily BernatNo ratings yet
- Lecture #3: Theme: Epithelial TissuesDocument45 pagesLecture #3: Theme: Epithelial TissuesKhurshidbuyamayumNo ratings yet
- Endorepro1.5 111210 DR Ika Histo Repro MaleDocument52 pagesEndorepro1.5 111210 DR Ika Histo Repro MalemahardikaNo ratings yet
- Human Anatomy and Physiology Chapter 12: Reproductive SystemsDocument17 pagesHuman Anatomy and Physiology Chapter 12: Reproductive SystemsHannah DiñosoNo ratings yet
- Jawahar Navodaya Vidyalaya, Bolangir Biology Assingment Guided by - Swastitapa Kar Prepared by - Sujata Goud Class - Xii Section-A Roll No. - 16Document19 pagesJawahar Navodaya Vidyalaya, Bolangir Biology Assingment Guided by - Swastitapa Kar Prepared by - Sujata Goud Class - Xii Section-A Roll No. - 16preetamgoud225No ratings yet
- Embryology ReviewerDocument6 pagesEmbryology ReviewerrexartoozNo ratings yet
- Cell Structure FunctionsDocument4 pagesCell Structure FunctionsGian Carlo MadriagaNo ratings yet
- MicroPara 03 - Prokaryotic CellsDocument23 pagesMicroPara 03 - Prokaryotic CellsJianne CaloNo ratings yet
- 4.1 - Tissue Level of OrganizationDocument94 pages4.1 - Tissue Level of OrganizationEmman ImbuidoNo ratings yet
- Cells & TissuesDocument17 pagesCells & TissuesClaraNo ratings yet
- Case+11+-+Histophysiology+of+Male+Reproductive+System 2023Document22 pagesCase+11+-+Histophysiology+of+Male+Reproductive+System 2023ZolwethuNo ratings yet
- Sertoli Cell Cell Testes Germ Cells SertoliDocument3 pagesSertoli Cell Cell Testes Germ Cells Sertolihur-azmi-1154No ratings yet
- Gametogenesis: Formation of Eggs and SpermDocument21 pagesGametogenesis: Formation of Eggs and Spermmadhu dwivediNo ratings yet
- Cell Structure: A Guide to the OrganellesDocument11 pagesCell Structure: A Guide to the OrganellesAli MahmoudNo ratings yet
- Male Reproductive SystemDocument46 pagesMale Reproductive Systemencouragemthethwa3No ratings yet
- Male SubfertilityDocument41 pagesMale SubfertilityIshaThapaNo ratings yet
- Spermatogenesis PPTDocument42 pagesSpermatogenesis PPTInsatiable CleeNo ratings yet
- NCERT Biology Cell Organelle Functions Key PointsDocument19 pagesNCERT Biology Cell Organelle Functions Key PointsHarsh YadavNo ratings yet
- Embryo Lab Exercise 1Document7 pagesEmbryo Lab Exercise 1Karmina Santos100% (1)
- BB 101 Help Session PDFDocument124 pagesBB 101 Help Session PDFNaren RahulNo ratings yet
- CGEN - 100 - #2-Parts of A CellDocument2 pagesCGEN - 100 - #2-Parts of A CellEricka MasakayanNo ratings yet
- Department of Morphology: Penza State University Medical InstituteDocument18 pagesDepartment of Morphology: Penza State University Medical InstituteunnatiNo ratings yet
- Epithelial Tissue ClassificationDocument46 pagesEpithelial Tissue ClassificationFady FadyNo ratings yet
- As Level BiologyDocument18 pagesAs Level BiologyAasiya SultanaNo ratings yet
- 4 Regeneration RepairDocument65 pages4 Regeneration RepairMustafa YılmazNo ratings yet
- Male Reproductive SystemDocument92 pagesMale Reproductive SystemYunandhika RizkiNo ratings yet
- Reproductive System Reviewer - BAYLONDocument16 pagesReproductive System Reviewer - BAYLONElijah Joaquin Payumo BaylonNo ratings yet
- 1 1a Mtc Bch Catabolism of the Carbon Skeletons of Amino AcidsDocument16 pages1 1a Mtc Bch Catabolism of the Carbon Skeletons of Amino AcidsCarmela MarianoNo ratings yet
- 1.1 Renal Physiology 1Document8 pages1.1 Renal Physiology 1Carmela MarianoNo ratings yet
- Lecture 01 Pediatric Endocrinology Dr. CuaDocument21 pagesLecture 01 Pediatric Endocrinology Dr. CuaCarmela MarianoNo ratings yet
- 4 O2 and CO2 TransportDocument9 pages4 O2 and CO2 TransportCarmela MarianoNo ratings yet
- BRS Anatomy - Intro Flashcards by Grace Caldwell - BrainscapeDocument10 pagesBRS Anatomy - Intro Flashcards by Grace Caldwell - BrainscapeCarmela MarianoNo ratings yet
- BRS Anatomy - Thorax Flashcards by Grace Caldwell - BrainscapeDocument45 pagesBRS Anatomy - Thorax Flashcards by Grace Caldwell - BrainscapeCarmela MarianoNo ratings yet
- Reference RangesDocument2 pagesReference RangesCarmela MarianoNo ratings yet
- BRS Anatomy - Back & Spine Flashcards by Grace Caldwell - BrainscapeDocument29 pagesBRS Anatomy - Back & Spine Flashcards by Grace Caldwell - BrainscapeCarmela MarianoNo ratings yet
- Venous Drainage of The CNS - Cerebrum - TeachMeAnatomyDocument4 pagesVenous Drainage of The CNS - Cerebrum - TeachMeAnatomyCarmela MarianoNo ratings yet
- Arterial Supply To The Brain - Carotid - Vertebral - TeachMeAnatomyDocument5 pagesArterial Supply To The Brain - Carotid - Vertebral - TeachMeAnatomyCarmela MarianoNo ratings yet
- 2Y1S - MIDTERM - Gram Pos and Neg - MycobacteriumDocument9 pages2Y1S - MIDTERM - Gram Pos and Neg - MycobacteriumCarmela MarianoNo ratings yet
- HannaDocument3 pagesHannaMagda FrutasNo ratings yet
- Maternal AnatomyDocument27 pagesMaternal AnatomyGio BalisiNo ratings yet
- Menstrual CycleDocument18 pagesMenstrual CycleKim RamosNo ratings yet
- Crochet VaginaDocument12 pagesCrochet VaginaGabrielaCuadraditoUróborosSerendipia57% (7)
- How To Stretch Penis LigamentsDocument2 pagesHow To Stretch Penis LigamentsJayson Jonson AraojoNo ratings yet
- Science 10: Prepared By: Jergen A. Romulo Sst-IiiDocument8 pagesScience 10: Prepared By: Jergen A. Romulo Sst-IiiRona May EsperanzateNo ratings yet
- Lee Jenkins - Female Orgasm Black BookDocument120 pagesLee Jenkins - Female Orgasm Black Bookstenacom82% (11)
- Stages of the Estrous Cycle in Domestic AnimalsDocument3 pagesStages of the Estrous Cycle in Domestic AnimalsYounas marri100% (1)
- DocumentDocument2 pagesDocumentЭрвин ЗайцевNo ratings yet
- Tristan TaorminoDocument252 pagesTristan Taorminomaquis870% (1)
- 4 The Female and Male External Genitalia DiyaDocument48 pages4 The Female and Male External Genitalia DiyaOmotosho DavidNo ratings yet
- Structure and Function of the OvaryDocument4 pagesStructure and Function of the OvaryJay PaulNo ratings yet
- Male Multiple Orgasms Are Possible PDFDocument2 pagesMale Multiple Orgasms Are Possible PDFfeowfeow0% (1)
- 12th Biology Lab ManualDocument4 pages12th Biology Lab ManualVasudha GudiNo ratings yet
- The Menstrual CycleDocument18 pagesThe Menstrual CycleSakshi Halve100% (1)
- Human Reproductive SystemDocument5 pagesHuman Reproductive SystemSubatomoNo ratings yet
- Ovarian Cyst FinalDocument26 pagesOvarian Cyst FinalReicy Aquino SacularNo ratings yet
- Anatomy and Physiology of the Reproductive SystemDocument93 pagesAnatomy and Physiology of the Reproductive SystemMelizza Fajardo BañanoNo ratings yet
- Science 10 Quarter 3 Module 1Document14 pagesScience 10 Quarter 3 Module 1Zahra Alexä DavidsonNo ratings yet
- Male Reproductive System Structures and FunctionsDocument31 pagesMale Reproductive System Structures and FunctionsnamitaNo ratings yet
- Fenton Growth Chart Boy v1Document2 pagesFenton Growth Chart Boy v1nurhapsari20100% (3)
- Chap 31 HWDocument12 pagesChap 31 HWizabelaNo ratings yet
- Involved in The Female and Male Reproductive Systems. (A10Lt-Iiib-34)Document15 pagesInvolved in The Female and Male Reproductive Systems. (A10Lt-Iiib-34)Nerie FakihNo ratings yet
- Jurnal Analisi MeyDocument8 pagesJurnal Analisi MeyMey Aulia UrrohmahNo ratings yet
- Male Genitals and Inguinal AreaDocument20 pagesMale Genitals and Inguinal Areamalyn1218100% (1)
- Histology of Female Reproductive System: Dr. Rajesh Ranjan Assistant Professor Deptt. of Veterinary Anatomy C.V.SC., RewaDocument26 pagesHistology of Female Reproductive System: Dr. Rajesh Ranjan Assistant Professor Deptt. of Veterinary Anatomy C.V.SC., RewaDiahNo ratings yet
- The Forever Man: The Definitive Guide To Male Stamina: The Ins and Outs of Holding Back: Mastering "Injaculation"Document7 pagesThe Forever Man: The Definitive Guide To Male Stamina: The Ins and Outs of Holding Back: Mastering "Injaculation"jake0% (2)
- The Repoductive SystemDocument6 pagesThe Repoductive SystemIsabel CajamarcaNo ratings yet
- Activity On The Menstrual CycleDocument3 pagesActivity On The Menstrual CycleElaine BaratitaNo ratings yet
- Module 1.1 Reproductive SystemDocument12 pagesModule 1.1 Reproductive SystemPrincess Dela CruzNo ratings yet