Professional Documents
Culture Documents
Renal Diseases
Uploaded by
Jolan Fernando Herce0 ratings0% found this document useful (0 votes)
3 views4 pagesAUBF-Lecture
Original Title
renal-diseases
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAUBF-Lecture
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
3 views4 pagesRenal Diseases
Uploaded by
Jolan Fernando HerceAUBF-Lecture
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 4
ANALYSIS OF URINE Herce, Jolan
AND BODY FLUIDS BSMT-3B
RENAL DISEASES
INTRODUCTION Goodpasture Syndrome
Three classifications: • Attachment of a cytotoxic antibody formed during viral
1. Glomerular respiratory infections to glomerular and alveolar
2. Tubular basement membranes
3. Interstitial Clinical course: Hemoptysis and dyspnea followed by
hematuria
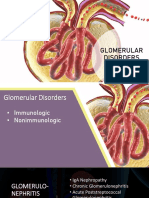
GLOMERULAR DISORDERS Urinalysis findings:
• result from immunologic disorders throughout the • Macroscopic hematuria
body including the kidney • Proteinuria
Immune complexes: result of immunologic reactions and • RBC casts
increased serum immunoglobulins Other tests:
Nonimmunologic causes of glomerular damage include • Antiglomerular basement membrane antibody
the following:
• Exposure to chemicals and toxins that also affect the Granulomatosis With Polyangiitis
tubules • Antineutrophilic cytoplasmic autoantibody (ANCA)
• Disruption of the electrical membrane charges as binds to neutrophils in vascular walls, producing damage
occurs in nephrotic syndrome (NS) to small vessels in the lungs and glomerulus
• Deposition of amyloid material from systemic disorders Clinical course: Pulmonary symptoms, including
that may involve chronic inflammation and acute-phase hemoptysis, develop first, followed by renal involvement
reactants and possible progression to end-stage renal failure
• Thickening of the basement membrane associated Urinalysis findings:
with diabetic nephropathy • Macroscopic hematuria
• Proteinuria
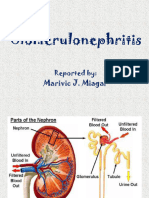
GLOMERULONEPHRITIS • RBC casts
• a sterile, inflammatory process that affects the Other tests:
glomerulus and is associated with the finding of • Antineutrophilic peripheral or cytoplasmic antibody
blood, protein, and casts in the urine
Henoch-Schönlein Purpura
Acute Poststreptococcal Glomerulonephritis • Occurs primarily in children after viral respiratory
Symptoms: infections; a decrease in platelets disrupts vascular
• fever, edema, fatigue, nausea, hypertension integrity
Course of infection: nephrogenic strains of streptococci Clinical course: Initial appearance of purpura followed
form immune complexes with their corresponding by blood in sputum and stools and eventual renal
circulating antibodies and become deposited on the involvement
glomerular membranes Urinalysis findings:
Urinalysis findings: • Macroscopic hematuria
• hematuria • Proteinuria
• proteinuria • RBC casts
• oliguria Other tests:
• RBC, hyaline and granular casts • Stool occult blood
• dysmorphic RBCs
• white blood cells (WBCs) Membranous Glomerulonephritis
Other tests: • Thickening of the glomerular membrane after IgG
• Anti–group A streptococcal enzyme tests immune complex deposition associated with systemic
disorders
Rapidly Progressive (Crescentic) Glomerulonephritis Clinical course: Slow progression to nephrotic syndrome
• more serious form of acute glomerular disease or possible remission
• Deposition of immune complexes from systemic Urinalysis findings:
immune disorders on the glomerular membrane • Microscopic hematuria
Urinalysis findings: • Proteinuria
• macroscopic hematuria Other tests:
Other tests: • Stool occult blood
• Blood urea nitrogen • Hepatitis B surface antigen
• Creatinine • Fluorescent treponemal antibody-absorption test (FTA-
• eGFR ABS)
TRANSCRIBED BY: JOLAN HERCE BSMT-3B
ANALYSIS OF URINE Herce, Jolan
AND BODY FLUIDS BSMT-3B
Membranoproliferative Glomerulonephritis Minimal Change Disease
• Cellular proliferation affecting the capillary walls or the • Disruption of the podocytes occurring primarily in
glomerular basement membrane, possibly immune children after allergic reactions and immunizations;
mediated dysfunction of T-cell immunity
Clinical course: Slow progression to chronic Clinical course: Frequent complete remission after
glomerulonephritis (CGN) or nephrotic syndrome (NS) corticosteroid treatment
Urinalysis findings: Urinalysis findings:
• Hematuria • Heavy proteinuria
• Proteinuria • Transient hematuria
Other tests: • Fat droplets
• Serum complement levels Other tests:
• Serum albumin
Chronic Glomerulonephritis • Cholesterol
• Marked decrease in renal function resulting from • Triglycerides
glomerular damage precipitated by other renal disorders
Clinical course: Noticeable decrease in renal function Focal Segmental Glomerulosclerosis
progressing to renal failure • Disruption of podocytes in certain areas of glomeruli
Urinalysis findings: associated with heroin and analgesic abuse and with HIV
• Hematuria and hepatitis viruses
• Proteinuria Clinical course: May resemble nephrotic syndrome (NS)
• Glucosuria or minimal change disease (MCD)
• Cellular and granular casts Urinalysis findings:
• Waxy and broad casts • Proteinuria
Other tests: • Microscopic hematuria
• BUN • Macroscopic or microscopic
• Serum creatinine • hematuria
• eGFR Other tests:
• Electrolytes • Drugs of abuse
• HIV tests
Immunoglobulin A Nephropathy
• Deposition of IgA on the glomerular membrane TUBULAR DISORDERS
resulting from increased levels of serum IgA • Disorders affecting the renal tubules include
Clinical course: Recurrent macroscopic hematuria after those in which tubular function is disrupted as a
exercise with slow progression to chronic result of actual damage to the tubules, as well
glomerulonephritis (CGN) as those in which a metabolic or hereditary
Urinalysis findings: disorder affects the intricate functions of the
• Macroscopic or microscopic hematuria tubules.
Other tests:
• Serum IgA Acute tubular necrosis (ATN)
• Damage to renal tubular cells caused by ischemia or
Nephrotic Syndrome toxic agents
• Disruption of the shield of negativity and damage to Clinical course: Acute onset of renal dysfunction usually
the tightly fitting podocyte barrier, resulting in massive loss resolved when underlying cause is corrected
of protein and lipid Urinalysis findings:
Clinical course: Acute onset after systemic shock • Microscopic hematuria
Urinalysis findings: • Proteinuria
• Heavy proteinuria • Renal tubular epithelial (RTE) cells
• Microscopic hematuria • RTE cell casts
• Renal tubular cells • Hyaline, granular, waxy, broad casts
• Oval fat bodies Other tests:
• Fat droplets • Hemoglobin
• Fatty and waxy casts • Hematocrit
Other tests: • Cardiac enzymes
• Serum albumin
• Cholesterol
• Triglycerides
TRANSCRIBED BY: JOLAN HERCE BSMT-3B
ANALYSIS OF URINE Herce, Jolan
AND BODY FLUIDS BSMT-3B
Fanconi syndrome Nephrogenic Diabetes Insipidus
• Inherited in association with cystinosis and Hartnup • Inherited defect of tubular response to ADH or
disease or acquired through exposure to toxic agents acquired from medications
Clinical course: Generalized defect in renal tubular Clinical course: Requires supportive therapy to prevent
reabsorption requiring supportive therapy dehydration
Urinalysis findings: Urinalysis findings:
• Glucosuria • Low specific gravity
• Possible cystine crystals • polyuria
Other tests: Other tests:
• Serum and urine electrolytes • ADH testing
• Amino acid chromatography
Renal Glycosuria
Alport Syndrome • Inherited autosomal recessive trait
• Genetic disorder showing lamellated and thinning Clinical course: Benign disorder
glomerular basement membrane Urinalysis findings:
Clinical course: Slow progression to nephrotic syndrome • Glucosuria
(NS) and end-stage renal disease Other tests:
Urinalysis findings: • Blood glucose
• Heavy proteinuria
• Microscopic hematuria INTERSTITIAL DISORDERS
• Renal tubular cells • disorders affecting the interstitium also affect
• Oval fat bodies the tubules, resulting in the condition commonly
• Fat droplets called tubulointerstitial disease
• Fatty and waxy casts
• Microalbuminuria Urinary Tract Infection
Other tests: • Ascending bacterial infection of the bladder
• Genetic testing Clinical course: Acute onset of urinary frequency and
burning; resolved with antibiotics
Uromodulin-Associated Kidney Disease Urinalysis findings:
• Inherited defect in the production of normal • Leukocyturia
uromodulin by the renal tubules and increased uric acid • Bacteriuria
causing gout • Microscopic
Clinical course: Continual monitoring of renal function • hematuria
for progression to renal failure and possible kidney • Mild proteinuria
transplantation • Increased pH
Urinalysis findings: Other tests:
• RTE cells • Urine culture
• Hematuria
• Proteinuria Acute Pyelonephritis
• Glucosuria • Infection of the renal tubules and interstitium related to
• Cellular and granular casts interference of urine flow to the bladder, reflux of urine
• Waxy and broad casts from the bladder, and untreated cystitis
Other tests: Clinical course: Acute onset of urinary frequency,
• Serum uric acid burning, and lower back pain; resolved with antibiotics
Urinalysis findings:
Diabetic Nephropathy • Leukocyturia
• most common cause of ESRD • Bacteriuria
•increased proliferation of mesangial cells and • WBC casts
increased deposition of cellular and noncellular material • Bacterial casts
within the glomerular matrix, resulting in accumulation of • Microscopic
solid substances around the capillary tufts • hematuria
• This glomerular damage is believed to be associated • Proteinuria
with deposition of glycosylated proteins resulting from Other tests:
poorly controlled levels of blood glucose. • Urine culture
• The vascular structure of the glomerulus also develops
sclerosis.
TRANSCRIBED BY: JOLAN HERCE BSMT-3B
ANALYSIS OF URINE Herce, Jolan
AND BODY FLUIDS BSMT-3B
Chronic Pyelonephritis CAUSES OF ACUTE RENAL FAILURE
• Inherited autosomal recessive trait Prerenal
Clinical course: Benign disorder • Decreased blood pressure/cardiac output
Urinalysis findings: • Hemorrhage
• Leukocyturia • Burns
• Bacteriuria • Surgery
• WBC casts • Septicemia
• Bacterial casts Renal
• Granular, waxy, • Acute glomerulonephritis (AGN)
• broad casts • Acute tubular necrosis (ATN)
• Hematuria • Acute pyelonephritis
• Proteinuria • Acute interstitial nephritis (AIN)
Other tests: Postrenal
• Urine culture • Renal calculi
• BUN • Tumors
• Creatinine
• eGFR
RENAL LITHIASIS
Acute Interstitial Nephritis Renal calculi (kidney stones): may form in the calyces
• Allergic inflammation of the renal interstitium in and pelvis of the kidney, ureters, and bladder
response to certain medication Lithiasis: calculi vary in size from barely visible to large,
Clinical course: staghorn calculi resembling the shape of the renal pelvis
Acute onset of renal dysfunction often accompanied by and smooth, round bladder stones with diameters of 2 or
a skin rash more inches
Resolves after discontinuation of medication and 1. Small calculi - may be passed in the urine,
treatment with corticosteroids subjecting the patient to severe pain radiating
Urinalysis findings: from the lower back to the legs
• Hematuria 2. Larger stones - cannot be passed and may not
• Proteinuria be detected until patients develop symptoms of
• Leukocyturia urinary obstruction
• WBC casts Lithotripsy: a procedure using high-energy shock waves,
Other tests: can be used to break stones located in the upper urinary
• Urine tract into pieces that then can be passed in the urine
• eosinophils Calcium oxalate or Calcium phosphate: Approx. 75% of
• BUN the renal calculi are composed of these stones and are
• Creatinine associated with metabolic calcium and phosphate
• eGFR disorders and, occasionally, diet
Magnesium ammonium phosphate: often are
RENAL FAILURE accompanied by urinary infections involving urea-
exists in both acute and chronic forms splitting bacteria
The progression to ESRD is characterized as follows: Uric acid: may be associated with increased intake of
• Marked decrease in the glomerular filtration rate (less foods with high purine content and with uromodulin-
than 25 mL/min) associated kidney disease
• Steadily rising serum BUN and creatinine values Cystine: seen in conjunction with hereditary disorders of
(azotemia) cystine metabolism
• Electrolyte imbalance
• Lack of renal concentrating ability, producing an
isosthenuric urine
• Proteinuria
• Renal glycosuria
• Abundance of granular, waxy, and broad casts, often
referred to as a telescoped urine sediment
TRANSCRIBED BY: JOLAN HERCE BSMT-3B
You might also like
- NEPHROLOGYDocument15 pagesNEPHROLOGYDiana Jean100% (1)
- PSGNDocument23 pagesPSGNalpha mae beltranNo ratings yet
- A Toxic Triangle of Destructive Leadership at Bristol Royal InfirmaryDocument19 pagesA Toxic Triangle of Destructive Leadership at Bristol Royal InfirmaryJesicca DeviyantiNo ratings yet
- UntitledDocument340 pagesUntitledAlistair KohNo ratings yet
- NAC Protocol PrintableDocument21 pagesNAC Protocol Printablemaadyyy123100% (1)
- HKDSE Biology Part 3 Health & DiseasesDocument17 pagesHKDSE Biology Part 3 Health & DiseasesTSZ YAN CHEUNGNo ratings yet
- Chronic Kidney Disease DR Moses KazevuDocument29 pagesChronic Kidney Disease DR Moses KazevuMoses Jr KazevuNo ratings yet
- 5.nephritic SyndromeDocument64 pages5.nephritic Syndromeyeni100% (1)
- Clinical Microscopy ReviewerDocument31 pagesClinical Microscopy ReviewerbokbokbokNo ratings yet
- Clinical LaboratoriesDocument24 pagesClinical Laboratoriespdamodar200788% (8)
- Case 2Document4 pagesCase 2Kim Ruiz100% (1)
- Transfusion Medicine and Hemostasis: Clinical and Laboratory AspectsFrom EverandTransfusion Medicine and Hemostasis: Clinical and Laboratory AspectsRating: 4 out of 5 stars4/5 (9)
- Case Study OutlineDocument3 pagesCase Study OutlineExcel MarieNo ratings yet
- Attention Deficit Hyperactivity DisorderDocument8 pagesAttention Deficit Hyperactivity DisorderShinjiNo ratings yet
- Sindroma Nefrotik Vs NefritikDocument23 pagesSindroma Nefrotik Vs NefritikBetha456100% (1)
- Sindroma Nefrotik Vs NefritikDocument23 pagesSindroma Nefrotik Vs NefritiksiayuNo ratings yet
- Sindroma Nefrotik Vs NefritikDocument23 pagesSindroma Nefrotik Vs NefritikBobby Fildian Siswanto100% (3)
- Practical Hemostasis and ThrombosisFrom EverandPractical Hemostasis and ThrombosisNigel S. KeyNo ratings yet
- Sindroma Nefrotik Vs NefritikDocument22 pagesSindroma Nefrotik Vs NefritikAyueka EkaNo ratings yet
- MTAUBFLec M5 AssignmentDocument8 pagesMTAUBFLec M5 AssignmentPaul Richard G. CalmaNo ratings yet
- Glomerular Disorders: CATALUÑA, Hanz Nikko GDocument15 pagesGlomerular Disorders: CATALUÑA, Hanz Nikko GHanz Nikko CatalunaNo ratings yet
- Renal DisordersDocument28 pagesRenal DisordersChristine CalumaNo ratings yet
- Glomerulonefrita Acuta Poststreptococica (GNAPS) - Engleza 2 (User-PC - S Conflicted Copy 2013-04-29) - 1Document37 pagesGlomerulonefrita Acuta Poststreptococica (GNAPS) - Engleza 2 (User-PC - S Conflicted Copy 2013-04-29) - 1Ashley PaulNo ratings yet
- Aubf RenaallllllllDocument7 pagesAubf RenaallllllllMarienel PingolNo ratings yet
- The Urinary System: Dr. Khan, MD, MCPS, DTCD PA 5402 T/W/RDocument35 pagesThe Urinary System: Dr. Khan, MD, MCPS, DTCD PA 5402 T/W/RCrystal Lynn Keener SciariniNo ratings yet
- Glomerulonephritis: Marivic J. MiagarDocument28 pagesGlomerulonephritis: Marivic J. MiagarMarivic DianoNo ratings yet
- AUBF Lec - Renal DiseasesDocument6 pagesAUBF Lec - Renal Diseasescdsteenkamp18No ratings yet
- Seminar Acute Poststreptococcal GlomerulonephritisDocument33 pagesSeminar Acute Poststreptococcal GlomerulonephritisHakimah K. SuhaimiNo ratings yet
- Glomerular Disorders - GlomerulonephrtisDocument56 pagesGlomerular Disorders - GlomerulonephrtisValerie Suge-MichiekaNo ratings yet
- WSU Renal ReviewDocument100 pagesWSU Renal ReviewLeticia BornsteinNo ratings yet
- AUBF Lec Week#8 Renal DiseasesDocument10 pagesAUBF Lec Week#8 Renal DiseasesLexaNatalieConcepcionJuntadoNo ratings yet
- Renal DiseasesDocument50 pagesRenal DiseasesjvbapialNo ratings yet
- Acute Nephrotic SyndromeDocument1 pageAcute Nephrotic SyndromeXarius FidelNo ratings yet
- AUBF FinalsDocument62 pagesAUBF FinalsAlthea Jam Grezshyl GaloNo ratings yet
- Quality Assessment, Renal Disease & Urine ScreeningDocument15 pagesQuality Assessment, Renal Disease & Urine ScreeningAnya IgnacioNo ratings yet
- Hematology: Monoclonal Gammapathies-Multiple Myeloma Lymphoma Hodgkin and Non HodgjknDocument29 pagesHematology: Monoclonal Gammapathies-Multiple Myeloma Lymphoma Hodgkin and Non HodgjknBelu DanielaNo ratings yet
- Analysis of Urine and Body Fluids w8Document3 pagesAnalysis of Urine and Body Fluids w8Cheska ReyesNo ratings yet
- GlomerulonephritisDocument28 pagesGlomerulonephritisqayyum consultantfpscNo ratings yet
- Glo Me Rulo NefritisDocument58 pagesGlo Me Rulo NefritisFany SholehaNo ratings yet
- Basic Laboratory 2010Document11 pagesBasic Laboratory 2010AnastasiafynnNo ratings yet
- Approach To The Patient With Renal Disease: Dr. Silvia SpânuDocument25 pagesApproach To The Patient With Renal Disease: Dr. Silvia SpânuSergiuNo ratings yet
- Chapter 8 - Renal DiseaseDocument7 pagesChapter 8 - Renal DiseaseCha GuingabNo ratings yet
- Nephrotic Syndrome: By: Yeni Ayu Prihastuti Moderator: DR. Dr. Hani Susianti, SP - PK (K)Document42 pagesNephrotic Syndrome: By: Yeni Ayu Prihastuti Moderator: DR. Dr. Hani Susianti, SP - PK (K)yeniNo ratings yet
- AUBF Group 1 Chapter 8Document12 pagesAUBF Group 1 Chapter 8Gerald John PazNo ratings yet
- Sindroma Nefrotik Vs NefritikDocument23 pagesSindroma Nefrotik Vs NefritikUswatun Aortatika KhasanahNo ratings yet
- Midterm Chapter7Document43 pagesMidterm Chapter7Frances FranciscoNo ratings yet
- Cerebrospinal Fluid Serous and Synovial Transfusion Cerebrospinal FluidDocument12 pagesCerebrospinal Fluid Serous and Synovial Transfusion Cerebrospinal FluidZllison Mae Teodoro MangabatNo ratings yet
- NephritisDocument21 pagesNephritisruchika100% (1)
- Glomerulonephritis PresentationDocument23 pagesGlomerulonephritis Presentationjacksonyu1234No ratings yet
- Proteinuria &Document38 pagesProteinuria &Agustinus BethaNo ratings yet
- 7.2. Hemolytic AnemiaDocument29 pages7.2. Hemolytic AnemiaMichellyTjoaNo ratings yet
- Atypical Renal Presentation in Severe LeptospirosisDocument3 pagesAtypical Renal Presentation in Severe LeptospirosisADINo ratings yet
- Case Presentation Febrile Neutropenia NizarDocument25 pagesCase Presentation Febrile Neutropenia NizarNizar IJNo ratings yet
- Glomerulonephritis: Prof DR DR Haerani Rasyid, Mkes, SPPD, KGH, SPGK Tim Ginjal Hipertensi Unhas 2019Document68 pagesGlomerulonephritis: Prof DR DR Haerani Rasyid, Mkes, SPPD, KGH, SPGK Tim Ginjal Hipertensi Unhas 2019uzan100% (1)
- Nephritic Syndrome: Pyuza, MDDocument41 pagesNephritic Syndrome: Pyuza, MDawadh mbaroukNo ratings yet
- Nephrotic Syndrom WardDocument49 pagesNephrotic Syndrom WardHelene AlawamiNo ratings yet
- Abnormal Composition of UrineDocument77 pagesAbnormal Composition of Urineangela marie abadillaNo ratings yet
- Nephrotic SyndDocument21 pagesNephrotic Synd238439904No ratings yet
- L20 - Glomerular DiseasesDocument34 pagesL20 - Glomerular Diseasesabdideba6No ratings yet
- Renal DiseaseDocument5 pagesRenal DiseasefeajhanineladagaNo ratings yet
- Renal Disease 2023Document9 pagesRenal Disease 2023MaeNo ratings yet
- 7 Renal Disease StudentDocument34 pages7 Renal Disease Studentrbm121415chyNo ratings yet
- Human Tumours Secreting Catecholamines: Clinical and Physiopathological Study of the PheochromocytomasFrom EverandHuman Tumours Secreting Catecholamines: Clinical and Physiopathological Study of the PheochromocytomasRating: 5 out of 5 stars5/5 (1)
- Inflammatory Diseases of Blood VesselsFrom EverandInflammatory Diseases of Blood VesselsGary S. HoffmanNo ratings yet
- Homework 1 Herce Bsmt2bDocument1 pageHomework 1 Herce Bsmt2bJolan Fernando HerceNo ratings yet
- APznzab7n0tTt9B3o6nrEulLujxEm FmBRigdivDocument2 pagesAPznzab7n0tTt9B3o6nrEulLujxEm FmBRigdivJolan Fernando HerceNo ratings yet
- Biochem Herce Bsmt2bDocument3 pagesBiochem Herce Bsmt2bJolan Fernando HerceNo ratings yet
- Biochemistry Herce Bsmt2bDocument1 pageBiochemistry Herce Bsmt2bJolan Fernando HerceNo ratings yet
- Background of The ProjectDocument2 pagesBackground of The ProjectJolan Fernando HerceNo ratings yet
- Assessment QuestionnaireDocument3 pagesAssessment QuestionnaireJolan Fernando HerceNo ratings yet
- 20 Amino Acids Herce Bsmt2bDocument2 pages20 Amino Acids Herce Bsmt2bJolan Fernando HerceNo ratings yet
- SEATWORK1Document2 pagesSEATWORK1Jolan Fernando HerceNo ratings yet
- Activity 1 Herce Bsmt1bDocument1 pageActivity 1 Herce Bsmt1bJolan Fernando HerceNo ratings yet
- Activity On Endocrinology HERCE BSMT1BDocument1 pageActivity On Endocrinology HERCE BSMT1BJolan Fernando HerceNo ratings yet
- Letter of Two Students For InterviewDocument1 pageLetter of Two Students For InterviewJolan Fernando HerceNo ratings yet
- Cytogen FnalsDocument17 pagesCytogen FnalsJolan Fernando HerceNo ratings yet
- ACFrOgBSxI6Havvmnh9Te1qpS qBO9uYA HesicDocument6 pagesACFrOgBSxI6Havvmnh9Te1qpS qBO9uYA HesicJolan Fernando HerceNo ratings yet
- Biostat and Epi Transes SophomoresDocument60 pagesBiostat and Epi Transes SophomoresJolan Fernando HerceNo ratings yet
- Practical Test-Balancing and Types of Chemical RXNDocument1 pagePractical Test-Balancing and Types of Chemical RXNJolan Fernando HerceNo ratings yet
- Group Learning ActivityDocument3 pagesGroup Learning ActivityJolan Fernando HerceNo ratings yet
- Script For StepsDocument5 pagesScript For StepsJolan Fernando HerceNo ratings yet
- Medical Quackery and Folk MedicinesDocument2 pagesMedical Quackery and Folk MedicinesJolan Fernando HerceNo ratings yet
- Steps in Foodborne OutbreakDocument2 pagesSteps in Foodborne OutbreakJolan Fernando HerceNo ratings yet
- Activity Lab Sheet 4Document5 pagesActivity Lab Sheet 4Jolan Fernando HerceNo ratings yet
- Covid19 Pandemic - HerceDocument6 pagesCovid19 Pandemic - HerceJolan Fernando HerceNo ratings yet
- Cytogen ReviewerDocument6 pagesCytogen ReviewerJolan Fernando HerceNo ratings yet
- QajjquoisiDocument41 pagesQajjquoisiJolan Fernando HerceNo ratings yet
- Activity 8 - HERCE - BSMT1BDocument3 pagesActivity 8 - HERCE - BSMT1BJolan Fernando HerceNo ratings yet
- SGL 3 (Haematinics)Document32 pagesSGL 3 (Haematinics)raman mahmudNo ratings yet
- Adult Assessment ToolDocument4 pagesAdult Assessment ToolRiss CalmaNo ratings yet
- Swine FluDocument32 pagesSwine FluSajan Varghese100% (1)
- 3 - Harada Mori TechniqueDocument2 pages3 - Harada Mori TechniqueHONEYLYNNE DELA TORRENo ratings yet
- Carpal TunnelDocument1 pageCarpal TunnelKadek Rudita YasaNo ratings yet
- Lecture NotesDocument61 pagesLecture NotesTom Anthony Tonguia100% (1)
- The Navarro Urine TestDocument3 pagesThe Navarro Urine TestSalvator2000100% (2)
- CK-MB Isoenzyme: Immunoinhibition MethodDocument2 pagesCK-MB Isoenzyme: Immunoinhibition MethodFariz KasyidiNo ratings yet
- Cardiogenic Shock: BY Dr. M L Patel MD Associate Professor Deptt. of MedicineDocument19 pagesCardiogenic Shock: BY Dr. M L Patel MD Associate Professor Deptt. of MedicineDurgesh PushkarNo ratings yet
- Challenges of Mass Casualty Management at A RegionDocument5 pagesChallenges of Mass Casualty Management at A RegionEbuwa AmadasunNo ratings yet
- 1 s2.0 S2173572723000693 MainDocument11 pages1 s2.0 S2173572723000693 MainGabriela PachecoNo ratings yet
- Bloodcomponents: Anti-A and Anti-B Titers in Pooled Group O Platelets Are Comparable To Apheresis PlateletsDocument8 pagesBloodcomponents: Anti-A and Anti-B Titers in Pooled Group O Platelets Are Comparable To Apheresis Plateletsmy accountNo ratings yet
- Cellulitis - Acute - NICE CKS PDFDocument40 pagesCellulitis - Acute - NICE CKS PDFDinu IuliaNo ratings yet
- Reey8t.b. OsteomyelitisDocument52 pagesReey8t.b. Osteomyelitiskuku93No ratings yet
- Cisplatin As An Anti Cancer DrugDocument10 pagesCisplatin As An Anti Cancer DrugMahima KamraNo ratings yet
- Paediatric DKA Integrated Care Pathway For CportalDocument39 pagesPaediatric DKA Integrated Care Pathway For Cportalteresita vargasNo ratings yet
- Drug Study PharmacologyDocument3 pagesDrug Study PharmacologyZyrene RiveraNo ratings yet
- Clinical Group Study Case 1Document8 pagesClinical Group Study Case 1Olivia JagroopNo ratings yet
- Blood Pressure 911Document7 pagesBlood Pressure 911Judith J. LaneNo ratings yet
- Dampak Perkembangan Teknologi Terhadap AnakDocument23 pagesDampak Perkembangan Teknologi Terhadap Anakyeyen fitriaNo ratings yet
- Exam 1 Outline Notes - Docx NewDocument4 pagesExam 1 Outline Notes - Docx NewHeather MoralesNo ratings yet
- DAFTAR PUSTAKA P Rosea PDFDocument2 pagesDAFTAR PUSTAKA P Rosea PDFClara KumororiniNo ratings yet
- In Service Exam For Breast DR Paul BalisiDocument11 pagesIn Service Exam For Breast DR Paul BalisiAmiel Francisco ReyesNo ratings yet