Professional Documents
Culture Documents
Maternal Nursing: Anatomy and Physiology
Uploaded by
AmazingMind0 ratings0% found this document useful (0 votes)
0 views60 pagesThis document discusses human reproductive anatomy and physiology. It describes the development of reproductive organs from conception through puberty for both males and females. Key details include the roles of hormones like estrogen, progesterone, FSH and LH in sexual maturation and function. The structures and functions of the male and female reproductive systems are outlined, including the testes/ovaries, genitals and role in reproduction. Pubertal changes for both sexes are also summarized.
Original Description:
Original Title
Untitled
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses human reproductive anatomy and physiology. It describes the development of reproductive organs from conception through puberty for both males and females. Key details include the roles of hormones like estrogen, progesterone, FSH and LH in sexual maturation and function. The structures and functions of the male and female reproductive systems are outlined, including the testes/ovaries, genitals and role in reproduction. Pubertal changes for both sexes are also summarized.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
0 views60 pagesMaternal Nursing: Anatomy and Physiology
Uploaded by
AmazingMindThis document discusses human reproductive anatomy and physiology. It describes the development of reproductive organs from conception through puberty for both males and females. Key details include the roles of hormones like estrogen, progesterone, FSH and LH in sexual maturation and function. The structures and functions of the male and female reproductive systems are outlined, including the testes/ovaries, genitals and role in reproduction. Pubertal changes for both sexes are also summarized.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 60
Maternal Nursing
Anatomy and Physiology
Reproductive Development
Begins during intrauterine life
Full function is initiated at puberty
Hypothalamus – synthesis and releases GnRH
Anterior pituitary gland – release FSH and LH
FSH and LH – initiate production of androgen and
estrogen
Initiate visible signs of maturity – secondary sex
characteristic
Intrauterine Development
Sex – determined at the moment of conception
Gonad – body organ that produces sex cells
(testis-males, ovary-females)
Week 5 – primitive gonadal tissue is already
formed
Week 7 or 8 – differentiates into primitive testes
Testosterone formation begins
Mesonephric (wolffian) – develop into the male
reproductive organ
Week 10 – testosterone not present
Gonadal tissue differentiates into ovaries
Paramesonephric (mullerian) – develops into
female reproductive organs
Oocytes – cells that develop into eggs throughout
woman’s mature years
Already formed in ovaries
Week 12 – external genitals become visible
Testosterone secretion halted in utero –
chromosomal male born with female-
appearing genitalia
Testosterone during pregnancy –
chromosomal female born with male-
appearing genitalia
Pubertal Development
Secondary sex characteristics begin
Girls – develop earlier
Role of Androgen
Androgenic hormones
Responsible for muscular development,
physical growth, and increase in sebaceous
gland secretions
Males - adrenal cortex and testes
Females – adrenal cortex and ovaries
Testosterone in males:
Development of:
Testes, scrotum, penis, prostate and seminal
vesicles
Axillary and facial hair
Laryngeal enlargement accompanied by voice
change
Maturation of spermatozoa
Closure of growth in long bones
Testosterone in females:
Enlargement of the labia majora and clitoris
Formation of axillary and pubic hair
Adrenarche
Role of Estrogen
Triggered by FSH
Excreted by ovarian follicle
Estrone (E1), estradiol (E2), estriol (E3)
Influences the development of:
Uterus, fallopian tubes, vagina
Typical female fat distribution and hair patterns
Breast - trelarche
End to growth
Secondary Sex Characteristics
Girls
Order of changes:
1. Growth spurt
2. Increase in the transverse diameter of the pelvis
3. Breast development
4. Growth of pubic hair
5. Onset of menstruation
6. Growth of axillary hair
7. Vaginal secretions
Menarche – the first menstrual period
Ave. age – 12.5 years
9 – 17 years old
First year – irregular
Males
Production of spermatozoa does not begin
in intrauterine life
Produced in a continuous process
From puberty throughout life span
64 days - mature
Order of change:
1. Increase in weight
2. Growth of testes
3. Growth of face, axillary, pubic hair
4. Voice changes
5. Penile growth
6. Increase in height
7. Spermatogenesis
Anatomy and Physiology
The Reproductive System
Gynecology – study of the female
reproductive organs
Andrology – study of the male reproductive
organs
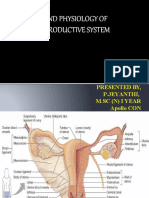
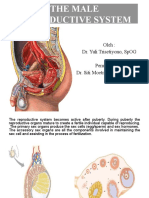
Male Reproductive System
External structures:
1. Scrotum
Support the testes and help regulate the
temperature of the skin
2. Testes
Leydig’s Cells – responsible for production of the
male hormone testosterone
Seminiferous tubules – produce spermatozoa
FSH – resposible for the release of androgen-
binding protein (ABP)
LH – responsible for the release of testosterone
One testis is slightly larger than the other
3. Penis
2 Corpus cavernosa
Corpus spongiosum
Penile artery – provides blood supply for the penis
Parasympathetic nerve – penile erection
Glans – bulging, sensitive ridge of tissue
Prepuce – retractable skin protecting the
glans
Circumsicion – removal of the prepuce
Internal structures:
1. Epididymis – approx 20 foot long
Conducts sperm from the testis to the vase
deferens
2. Vas deferens (ductus deferens)
Carries sperm from the epididymis to seminal
vesicles and the ejaculatory ducts
Spermatic cord – blood vessels and the vas
deferens
3. Seminal vesicle
Empty into the urethra by way of the
ejaculatory ducts
Produces a viscous portion of the semen
4. Ejaculatory ducts
Pass through the prostate gland and join the
seminal vesicles to the urethra
5. Prostate gland
Chestnut-sized gland that lies below the bladder
Secretes thin, alkaline fluid
6. Bulbourethral glands
Cowper’s gland
Secrete alkaline fluid
Semen – prostate gland (60%), seminal vesicles
(30%), epididymis (5%), bulbourethral glands
(5%)
7. Urethra
Approx 8 in (18 to 20cm)
Female Reproductive System
External Structures:
1. Mons veneris – protect the junction of the pubic
bone from trauma
2. Labia minora – abundant with sebaceous glands
3. Labia majora – protection for the external
genitalia and thedistal urethra and vagina
4. Vestibule – flattened surface inside the labia
Give rise to the urethra and the vagina
5. Clitoris – 1 to 2 cm rounded organ of
erectile tissue
Center of sexual arousal and orgasm
6. Prepuce – covers the clitoris
7. Skene’s gland (paraurethral glands) – one
on each side of the urethral meatus
8. Bartholin’s gland (vulvovaginal glands) –
located lateral to the distal vagina
Both glands – secretions help lubricate the
external vagina
Secretions with alkaline pH
9. Fourchette – ridge tissue formed by the
posterior joining of the two labia minora
and labia majora
Cut during childbirth
10. Perineal body – muscular area
11. Hymen – semicircle of tissue that
covers the opening of the vagina
Blood Supply
Pudendal artery and inferior rectus artery –
supply the external genitalia
Pudendal vein – venous return
Nerve Supply
Ilioinguinal and genitofemoral nerves (L1)
– anterior portion of the vulva
Pudendal nerve (S3) – posterior portions of
the vulva and vagina
Internal Structures:
1. Ovaries – produce, mature and discharge
ova
Produce estrogen and progesterone
Estrogen – prevent osteoporosis
Keep cholesterol levels reduced
Principal divisions:
A. Protective layer of epithelium
B. Cortex – filled with ovarian and graafian
follicles
C. Central medulla – contains nerves, blood
vessels, lymphatic tissue and some smooth
muscle tissue
2. Fallopian tubes – approx 10cm long
Convey the ovum from the ovaries to the
uterus
Provide a place for fertilization
Interstitial – lies within the uterine wall
1cm long
1mm in diameter
Isthmus – 2cm long
Portion that is cut and sealed in a tubal ligation
Ampulla – 5cm long
Fertilization takes place
Infundibulum – 2 cm long
Funnel-shaped
Rim is covered with fimbriae
Lining is composed of mucous membrane
and ciliated cells
Produces peristaltic movement
3. Uterus – hollow, muscular, pear-shaped
organ
8 years of age – increase in the size of the
uterus begins
17 years of age – reaches adult size
Functions:
Receive the ovum from the fallopian tube
Provide a place for implantation
Nourishment during fetal growth
Furnish protection to a growing fetus
Expel fetus from woman’s body
Divisions:
Body or corpus – uppermost part
Expands to contain the growing fetus
Cornua – upper aspects
Fundus – portion of the uterus between the
points of attachment of the fallopian tubes
Isthmus – short segment between the body
and cervix
Enlarges to accommodate the aid in
accommodating the growing fetus
Most commonly cut in CS
Cervix – lowest portion
Cervical canal – central cavity
Internal cervical os – opening of the canal
at the junction of the cervix and isthmus
External cervical os – distal opening to the
vagina
Uterine Layers
Endometrium – innermost, mucous
membrane
Basal layer – closest to the uterine wall
Not influenced by hormones
Glandular layer – influenced by estrogen
and progesterone
Grows and becomes thick
Shed as menstrual flow
Myometrium – middle one, muscle fibers
Constrict the tubal junctions
Holds the internal cervical os
Constrict blood vessels
Myomas, benign uterine tumors
Perimetrium – outer one, connective tissue
Add strength and support to the structure
Cervical Layer
Endocervix – mucous membrane
Secrete mucus
Estrogen peak – 700ml/day
Estrogen very low – few milliliters
Stratified squamous epithelium – similar to
the lining of the vagina
Important when obtaining a Papanicolaou
smear
Uterine Blood Supply
Uterine arteries – uterus
Ovarian artery – ovary
Joins the uterine artery
Uterine veins – empty into the internal iliac
veins
Uterine Nerve Supply
Supplied by efferent (motor) and afferent
(sensory) nerves
Efferent – T5 to T10
Afferent – T11 to T12
Epidural anesthesia
Uterine Supports
Posterior ligament – forms Douglas’ cul-de-
sac
Broad ligaments – cover the uterus front
and back and extend to the pelvic sides
Round ligaments – steady the uterus
4. Vagina – organ of intercourse
Convey sperm to the cervix
Birth canal
Anterior wall – 6-7 cm
Posterior wall – 8-9 cm
Fornices – recesses on all sides of the cervix
Anterior fornix – front
Posterior fornix – behind
Pooling of semen
Lateral fornix – sides
Rugae – folds
Bulbocavernosus – circular muscle at the
external opening of the vagina
Blood Supply - Vaginal artery
Nerve – sympathetic and parasympathetic at
S1 to S3 levels
Glycogen rich – broken down by
Doderlein’s bacillus
Breast
Ectodermic tissue
Estrogen – increase in size
Connective tissue and deposition of fat
Glandular tissue – undeveloped
Milk glands – 20 lobes
Acinar cells – produce milk
Lactiferous duct – reservoir for milk
Nipple – transmits sensations to the
posterior pituitary gland to release oxytocin
Oxytocin – constricts milk gland cells and
push milk forward
Areola – Montgomery’s tubercles
Blood supply – axillary, internal mammary
and intercostal arteries
Pelvis
Support and protect
Four united bones:
1. 2 Innominate bones
2. Coccyx
3. Sacrum
Innominate bones:
1. Ilium – iliac crest
2. Ischium
Ischial tuberosities
Ischial spines
3. Pubis – symphysis pubis
Sacrum – sacral prominence
Coccyx – 5 fused small bones
Divisions
False pelvis:
Superior half
Supports the uterus
Aids in directing the fetus into the true
pelvis
True pelvis:
Inferior half
Linea terminalis:
Imaginary line that divides the true and false
pelvis
Drawn from the sacral prominence to the superior
aspect of the symphysis pubis
Inlet - entrance to the true pelvis
Outlet – inferior portion of the pelvis
Pelvic cavity – space between the inlet and outlet
Curved
Slows and controls the speed of birth
Compresses the chest of the fetus
Midplane – level of the ischial spines
You might also like
- Obstetric Nursing Review (NLE)Document48 pagesObstetric Nursing Review (NLE)'jmark Francia100% (4)
- Obstetrics - Anatomy & PhysiologyDocument12 pagesObstetrics - Anatomy & PhysiologyDexter Lendio0% (1)
- Maternal Lectures EditedDocument77 pagesMaternal Lectures EditedSHEENA MAE DE LOS REYESNo ratings yet
- Gynecological Anatomy & PhysiologyDocument39 pagesGynecological Anatomy & Physiologynursereview100% (3)
- The Reproductive System: Alyssa Ashley R. DiegoDocument46 pagesThe Reproductive System: Alyssa Ashley R. DiegoteacherashleyNo ratings yet
- Structure and Function of The Reproductive SystemDocument83 pagesStructure and Function of The Reproductive SystemMagy Tabisaura GuzmanNo ratings yet
- The Reproductive SystemDocument68 pagesThe Reproductive SystemStef FieNo ratings yet
- Reproductive SystemDocument75 pagesReproductive SystemErnie SyarinaNo ratings yet
- Bio NotesDocument180 pagesBio NotesjyotibhalaNo ratings yet
- BIO 282 Male Reproductive SystemDocument46 pagesBIO 282 Male Reproductive SystemLira Pagara100% (1)
- The Reproductive SystemDocument42 pagesThe Reproductive SystemAries BautistaNo ratings yet
- Review of The Reproductive System 4Document44 pagesReview of The Reproductive System 4Shermaigne Ananayo BuyaNo ratings yet
- Reproductive System Notes - 2014-15 DraftDocument62 pagesReproductive System Notes - 2014-15 DraftMiguel MenendezNo ratings yet
- Reproductive Science 10Document22 pagesReproductive Science 10palicpicbea50No ratings yet
- Anatomy and Physiology of Female Reproductive SystemDocument67 pagesAnatomy and Physiology of Female Reproductive Systemannu panchalNo ratings yet
- CH 3Document8 pagesCH 3api-288494741No ratings yet
- Presented By, P.Jeyanthi, M.SC (N) I Year Apollo CONDocument67 pagesPresented By, P.Jeyanthi, M.SC (N) I Year Apollo CONPaul AndersonNo ratings yet
- The Reproductive Systems: Ms. Vernon Administrative and Clinical ProceduresDocument26 pagesThe Reproductive Systems: Ms. Vernon Administrative and Clinical ProceduresJustin MilliganNo ratings yet
- 4 Animal Reproduction and DevelopmentDocument26 pages4 Animal Reproduction and DevelopmentEGUIA, MARY SHENIETH M.No ratings yet
- Reproductive System - CompressedDocument109 pagesReproductive System - CompressedNoel Calvo Macarine100% (2)
- Physics Class 10 ICSEDocument5 pagesPhysics Class 10 ICSEmohammedumar7864521No ratings yet
- Reproductive Endocrine IntegumentaryDocument94 pagesReproductive Endocrine IntegumentaryMilyn Mae PalganNo ratings yet
- Human Reproduction UPDATEDDocument16 pagesHuman Reproduction UPDATEDCandy OpsadNo ratings yet
- HumanreproductionpptDocument59 pagesHumanreproductionpptsugi sivamNo ratings yet
- Reproductive SystemDocument33 pagesReproductive Systemjheannegabriellea.ylaganNo ratings yet
- Physiology - Ii Year BemsDocument10 pagesPhysiology - Ii Year BemsKumar M V ScNo ratings yet
- Maternal Health Nursing Part 1Document193 pagesMaternal Health Nursing Part 1Nacel CelesteNo ratings yet
- Assessment On The Reproductive System (Rusy Hepitriani)Document20 pagesAssessment On The Reproductive System (Rusy Hepitriani)Sri NadyaputriNo ratings yet
- Reproductive System ModuleDocument17 pagesReproductive System ModulePATRICIA KAYE RIONo ratings yet
- Human ReproductionDocument60 pagesHuman ReproductionOmiNo ratings yet
- Kuliah Sem4 2008-2Document16 pagesKuliah Sem4 2008-2cathencloxNo ratings yet
- 8.7.10 REPRODUCTION IN HUMANS My CS NotesDocument13 pages8.7.10 REPRODUCTION IN HUMANS My CS NotesAndre KachigambaNo ratings yet
- Reproductive SystemDocument7 pagesReproductive SystemRiaz siddiquiNo ratings yet
- 1a. Reproductive OrgansDocument60 pages1a. Reproductive OrgansJerrald Meyer L. BayaniNo ratings yet
- Human ReproductionDocument26 pagesHuman Reproductionbarunmahto001No ratings yet
- 1 TransDocument10 pages1 TranssenecabheNo ratings yet
- FemalereproductiveorganDocument57 pagesFemalereproductiveorganIwan MongayNo ratings yet
- Femalereproductiveorgan 150117083020 Conversion Gate01Document57 pagesFemalereproductiveorgan 150117083020 Conversion Gate01SARABIA, ARVIN JR.No ratings yet
- Screenshot 2022-03-28 at 10.17.47 PMDocument127 pagesScreenshot 2022-03-28 at 10.17.47 PMqdvvqvxn7gNo ratings yet
- SXSXDocument27 pagesSXSXJoevany E. BigorniaNo ratings yet
- Chapter 26 M&Freprod 2304Document55 pagesChapter 26 M&Freprod 2304sairahhannahNo ratings yet
- GE9 Module Lesson 3Document6 pagesGE9 Module Lesson 3agnesNo ratings yet
- Reproductive SystemDocument11 pagesReproductive Systemcasandra moranteNo ratings yet
- Male Reproductive SystemDocument71 pagesMale Reproductive Systemאילן גרינולדNo ratings yet
- Maternal and Child Nursing From Tina CompleteDocument51 pagesMaternal and Child Nursing From Tina CompleteArgee AlonsabeNo ratings yet
- Structure and Function of The Reproductive SystemDocument48 pagesStructure and Function of The Reproductive SystemJohnryl FranciscoNo ratings yet
- Anatomy - Physiology Lesson 16 Part 1 MALE REPRODUCTIVE SYSTEMDocument54 pagesAnatomy - Physiology Lesson 16 Part 1 MALE REPRODUCTIVE SYSTEMAubrey Princess F. CaceresNo ratings yet
- GENBIO REVIEWER - FinalsDocument6 pagesGENBIO REVIEWER - FinalsFiona CagolNo ratings yet
- P3 ReproductiveDocument24 pagesP3 ReproductiveZach DanielNo ratings yet
- Class 10 Biology 8.9.20Document11 pagesClass 10 Biology 8.9.20Shruti MahtoNo ratings yet
- Human Sexuality ConceptsDocument65 pagesHuman Sexuality ConceptsKrisRN01No ratings yet
- YL Anatomy of The Male Reproductive SystemDocument22 pagesYL Anatomy of The Male Reproductive SystemdrnyolNo ratings yet
- Rhsi, LSDocument56 pagesRhsi, LSMary AkellaNo ratings yet
- Science 3rd QuarterDocument22 pagesScience 3rd QuarterBethel AquinoNo ratings yet
- Bio InfoDocument5 pagesBio InfoSoham MultaniNo ratings yet
- Animal ReproductionDocument93 pagesAnimal ReproductionunattractiveyouNo ratings yet
- Animal Reproduction - Class PresentationDocument120 pagesAnimal Reproduction - Class PresentationRenz Dela Cruz ArellanoNo ratings yet
- Science Lesson 1 G5 1Document31 pagesScience Lesson 1 G5 1Sarah JumalonNo ratings yet
- 495Document2 pages495AmazingMindNo ratings yet
- 493Document2 pages493AmazingMindNo ratings yet
- 492Document2 pages492AmazingMindNo ratings yet
- 491Document2 pages491AmazingMindNo ratings yet
- 494Document2 pages494AmazingMindNo ratings yet
- Bible Bingo Calling CardsDocument8 pagesBible Bingo Calling CardsAmazingMindNo ratings yet
- 508Document2 pages508AmazingMindNo ratings yet
- How To Play The Undead Blocks Public Beta:: Step 1 - Create An NFT Compatible Crypto WalletDocument13 pagesHow To Play The Undead Blocks Public Beta:: Step 1 - Create An NFT Compatible Crypto WalletAmazingMindNo ratings yet
- UntitledDocument2 pagesUntitledAmazingMindNo ratings yet
- 506Document2 pages506AmazingMindNo ratings yet
- Application For LeaveDocument2 pagesApplication For LeaveAmazingMindNo ratings yet
- UntitledDocument2 pagesUntitledAmazingMindNo ratings yet
- Undead Blocks: Research ReportDocument13 pagesUndead Blocks: Research ReportAmazingMindNo ratings yet
- Research Report: FEBRUARY 14, 2022Document12 pagesResearch Report: FEBRUARY 14, 2022AmazingMindNo ratings yet
- 509Document2 pages509AmazingMindNo ratings yet
- Household Profiling Instructions Western Visayas 1Document4 pagesHousehold Profiling Instructions Western Visayas 1AmazingMindNo ratings yet
- Maternal Nursing: ComplicationsDocument57 pagesMaternal Nursing: ComplicationsAmazingMindNo ratings yet