Professional Documents
Culture Documents
SGD4 - Isaac
Uploaded by
isaac.daryl15820 ratings0% found this document useful (0 votes)
4 views16 pagesThis document describes medications used to treat asthma, including their mechanisms of action and side effects. It discusses short-acting beta-2 agonists (SABA) which are first-line treatment for acute asthma attacks. It also discusses long-acting beta-2 agonists (LABA) which can be used for nocturnal asthma. Inhaled corticosteroids are the primary treatment to prevent asthma exacerbations. Leukotriene receptor antagonists also play a role, particularly for wheezy infants/toddlers. The document explains the mechanisms of these drug classes in reducing airway inflammation and smooth muscle constriction. Potential side effects for each class are also outlined.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document describes medications used to treat asthma, including their mechanisms of action and side effects. It discusses short-acting beta-2 agonists (SABA) which are first-line treatment for acute asthma attacks. It also discusses long-acting beta-2 agonists (LABA) which can be used for nocturnal asthma. Inhaled corticosteroids are the primary treatment to prevent asthma exacerbations. Leukotriene receptor antagonists also play a role, particularly for wheezy infants/toddlers. The document explains the mechanisms of these drug classes in reducing airway inflammation and smooth muscle constriction. Potential side effects for each class are also outlined.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
4 views16 pagesSGD4 - Isaac
Uploaded by
isaac.daryl1582This document describes medications used to treat asthma, including their mechanisms of action and side effects. It discusses short-acting beta-2 agonists (SABA) which are first-line treatment for acute asthma attacks. It also discusses long-acting beta-2 agonists (LABA) which can be used for nocturnal asthma. Inhaled corticosteroids are the primary treatment to prevent asthma exacerbations. Leukotriene receptor antagonists also play a role, particularly for wheezy infants/toddlers. The document explains the mechanisms of these drug classes in reducing airway inflammation and smooth muscle constriction. Potential side effects for each class are also outlined.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 16
SGD4 - Isaac
LO7 – Describe the medications used in asthma treatment including
their pharmacological properties and side effects.
SABA and LABA
Short acting ß-2 agonists (SABA)
First-line treatment for acute asthma; bronchodilators of choice.
Administered rapidly after a quick history, physical examination, and
vital examination are done.
MDI SABA delivered via spacer (loaded one puff at a time and given
separately) has the same efficacy as nebulized SABA.
Parenteral/subcutaneous route SABA should be given in children with
moderate to severe/life-threatening acute exacerbations.
Long-acting ß-2 agonists (LABA)
E.g. salmeterol, formoterol
Treatment option for nocturnal asthma (instability/suboptimal
treatment) which are often controlled by appropriate doses of ICS.
When symptoms remain troublesome, adding LABA can relieve
symptoms and lessen the morning dip in lung function.
Mode of action
Mode of action Both SABA and LABA fall under the class of bronchodilators.
They mimic the actions of naturally occurring catecholamines to activate
adrenergic receptors to produce parasympathetic and sympathetic
physiological responses.
They mimic the actions of naturally occurring catecholamines to activate
adrenergic receptors to produce parasympathetic and sympathetic
physiological responses.
Beta-2 agonists act as ligands to adrenergic receptors with increased
selectivity towards beta-2 adrenergic receptors.
Activation of the beta-2 adrenergic receptor initiates a transmembrane signal
cascade, which involves G protein and adenylyl cyclase.
Mode of action
Adenylyl cyclase increases intracellular cAMP via the hydrolysis of
ATP, which serves to activate cAMP-dependent protein kinase A (PKA).
PKA acts to phosphorylate Gq-coupled receptors leading to a cascade
of intracellular signals, which reduces intracellular Ca2+ or decrease
the sensitivity of Ca2+.
The change in Ca2+ results in the inhibition of myosin light chain
phosphorylation, subsequently preventing airway smooth muscle
contraction (underlying mechanism behind beta-2 agonist; promotes
bronchodilatory effects)
Side effects
Potential side effects include:
Tremors
Tachycardia
Palpitations
Nervous tension
Headache
Muscle cramp
These side effects are seen more often during initial exposure
(improve and disappear completely after a few days/few weeks of
use)
Corticosteroids
Systemic corticosteroids
Essential in treatment of acute exacerbation to hasten recovery and
should be given early.
Administered via oral or IV route (parenteral route is indicated in
children who are vomiting/unable to tolerate orally or children with
moderate to severe/life-threatening acute exacerbations).
Inhaled corticosteroids
Treatment of choice in preventing asthma exacerbation in patients
with persistent asthma.
Regular use of ICS reduces the frequency of asthma symptoms,
bronchial hyper-responsiveness, risk of serious exacerbation, and
improves the quality of life.
Mode of action
Corticosteroids diffuse across the cell membrane and bind to
glucocorticoid receptors (GR) in the cytoplasm.
Activated GRs rapidly translocate to the nucleus where they produce
their molecular effects.
A pair of GRs (GR homodimer) bind to glucocorticoid response
elements (GRE) in the promoter region of steroid-responsive genes
and switches on the gene transcription for genes encoding β2-
adrenergic receptors and the anti-inflammatory proteins secretory
leukoprotease inhibitor and mitogen-activated protein kinase
phosphatase-1 (MKP-1) which inhibits MAP kinase pathways.
Side effects of inhaled corticosteroids
Local adverse effects include:
Dysphonia
Oral candidiasis
Reflex cough
Bronchospasm
These adverse effects are less common with low-dose compared to
high-dose inhaled corticosteroids, and are also mitigated by spacer
use when taking the medication via metered-dose inhalers
Leukotriene Receptor Antagonist (LTRA)
Leukotriene Receptor Antagonist (LTRA)
LTRAs are of definite role in management of wheezy infants and
toddler and moderate to severe chronic asthma.
Most commonly used in pediatrics is cysteinyl leukotriene
antagonists: Montelukast, Zafirlukast.
Mode of action
Leukotrienes are synthesized from arachidonic acid by the action of 5-
lipoxygenase in many inflammatory cells in the airways.
Cysteinyl leukotrienes (LTC4, LTD4, and LTE4) have amino acid moiety
and bind to cysteinyl leukotriene receptors (CysLT1 and CysLT2).
Bronchoconstriction, vascular permeability, eosinophil recruitment,
and chronic inflammation are mediated through the G protein-
coupled activation of cysteinyl leukotriene receptors.
Montelukast and zafirlukast are antagonists to cysteinyl leukotriene
CysLT1 receptors but not CysLT2 receptors.
Side effects
Side effects of leukotriene receptor antagonists may include the
following:
Headache
Gastrointestinal disorders
Pharyngitis
Fatigue
Upper respiratory tract infection
Cutaneous rash
Reversible alterations in levels of serum transaminase
You might also like
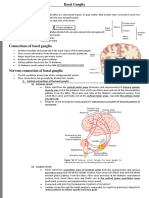
- Basal GangliaDocument6 pagesBasal Ganglia381a53c99bNo ratings yet
- Pharmacology of Drugs Used in Bronchial Asthma & COPDDocument84 pagesPharmacology of Drugs Used in Bronchial Asthma & COPDdfngjlnNo ratings yet
- Robert Plutchik (Auth.), Manfred Clynes, Jaak Panksepp (Eds.) - Emotions and Psychopathology-Springer US (1988)Document336 pagesRobert Plutchik (Auth.), Manfred Clynes, Jaak Panksepp (Eds.) - Emotions and Psychopathology-Springer US (1988)Lalón Gitud De Onda100% (1)
- NSAIDsDocument12 pagesNSAIDsjelly100% (1)
- Tocolytics & EcobolicsDocument25 pagesTocolytics & Ecobolicssaad0% (1)
- 2&3-Pharmacology of Drugs Used in Bronchial Asthma & COPDDocument58 pages2&3-Pharmacology of Drugs Used in Bronchial Asthma & COPDKishan SethNo ratings yet
- Carnivorous Plants - Physiology, Ecology, and Evolution 2018 - OUP OxfordDocument563 pagesCarnivorous Plants - Physiology, Ecology, and Evolution 2018 - OUP Oxfordfernando LEISNo ratings yet
- Physical Development of Infants and ToddlersDocument30 pagesPhysical Development of Infants and ToddlersDiana Garcia SaclutiNo ratings yet
- Athma, COPD and Cough AgentsDocument71 pagesAthma, COPD and Cough AgentsBriana NdayisabaNo ratings yet
- Anti Inflammatory DrugsDocument90 pagesAnti Inflammatory Drugsdrnasim2008817160% (5)
- Nsaids 190204194047Document40 pagesNsaids 190204194047Harini Bala100% (1)
- Bronchial AsthmaDocument43 pagesBronchial AsthmaAmar BimavarapuNo ratings yet
- Biosynthesis of CarbohydratesDocument31 pagesBiosynthesis of CarbohydratesDaniella Pasilbas Sabac100% (2)
- Cambridge o Level Biology Revision GuideDocument10 pagesCambridge o Level Biology Revision GuideAmmar RizwanNo ratings yet
- AsthmaDocument42 pagesAsthma7w2b96qznkNo ratings yet
- Antiasthma and Cough MedicineDocument47 pagesAntiasthma and Cough MedicineYordanos EshetuNo ratings yet
- Systemic Effects of Histamine and SerotoninDocument5 pagesSystemic Effects of Histamine and SerotoninibrahimNo ratings yet
- Respiratory PharmacologyDocument34 pagesRespiratory PharmacologyHirpâsà MămoNo ratings yet
- Respiratory SystemDocument27 pagesRespiratory SystemSowndariyaNo ratings yet
- Drug StudyDocument4 pagesDrug StudyMäc LäntinNo ratings yet
- Asthma and RenalDocument9 pagesAsthma and RenalHlaSoe WinNo ratings yet
- Year 1 Drug List CompleteDocument39 pagesYear 1 Drug List Completefarcry2ismNo ratings yet
- Drugs For Treatment of Bronchial Asthma: DR Sanjay Junior Resident Department of Pharmacology Ims-BhuDocument19 pagesDrugs For Treatment of Bronchial Asthma: DR Sanjay Junior Resident Department of Pharmacology Ims-BhuBisweswar OjhaNo ratings yet
- Autacoids, Respiratory Diseases Drug Treatment 2023Document38 pagesAutacoids, Respiratory Diseases Drug Treatment 2023adetola adetayoNo ratings yet
- Modul Muskuloskeletal - NSAIDs 2017Document56 pagesModul Muskuloskeletal - NSAIDs 2017khairunnisanurainiNo ratings yet
- Anti-Asthmatics: Dr. Sadia Shahid PGT-Pharmacology IimcDocument30 pagesAnti-Asthmatics: Dr. Sadia Shahid PGT-Pharmacology IimcWafaa AbdullahNo ratings yet
- Antiasthmatic DrugsDocument36 pagesAntiasthmatic DrugsJannah ZahraaNo ratings yet
- Obat Golongan KortikosteroidDocument43 pagesObat Golongan KortikosteroidFitri Andriani IbrahimNo ratings yet
- Analgesics Non OpioidDocument6 pagesAnalgesics Non Opioidhlouis8No ratings yet
- Cardiovascular Pharmacology PDFDocument20 pagesCardiovascular Pharmacology PDFMelanie PrinceNo ratings yet
- 3 Analgesic Anitpyretic InfamDocument10 pages3 Analgesic Anitpyretic InfamAnonymous dRAu54No ratings yet
- Management of AsthmaDocument20 pagesManagement of Asthmazaidiarisha52No ratings yet
- 4 - Chapter - Respiratory SystemDocument25 pages4 - Chapter - Respiratory SystemleonNo ratings yet
- AsthmaDocument8 pagesAsthmaAbdul WahidNo ratings yet
- Asthma MedicationDocument2 pagesAsthma MedicationAlexandra AlexaNo ratings yet
- Phama Exam.Document14 pagesPhama Exam.muwonge benonNo ratings yet
- Anti Asthamatic DrugsDocument28 pagesAnti Asthamatic DrugsGOPALNo ratings yet
- NSAIDs, DMARDs & Antigout1Document69 pagesNSAIDs, DMARDs & Antigout1Melissa SalayogNo ratings yet
- Pharmacotherapy of Bronchial AsthmaDocument7 pagesPharmacotherapy of Bronchial AsthmaAhmedshaker21100% (2)
- Drugs Acting On Respiratory System of AnimalsDocument8 pagesDrugs Acting On Respiratory System of AnimalsSunil100% (4)
- Anti Asthmatic DrugsDocument8 pagesAnti Asthmatic DrugsNavjot BrarNo ratings yet
- Journal Reading AsthmaDocument12 pagesJournal Reading AsthmaMuhammad Ihsan AuliaNo ratings yet
- Cology 3 Unit 1Document28 pagesCology 3 Unit 1imrujlaskar111No ratings yet
- Farmakologi Analgetik NSAID (Dr. Atina)Document56 pagesFarmakologi Analgetik NSAID (Dr. Atina)RidhaNo ratings yet
- Asma Felino TratamientoDocument7 pagesAsma Felino TratamientoRenzo Alessandro Pacherres NietoNo ratings yet
- Pharmacotherapy of Asthma-1Document6 pagesPharmacotherapy of Asthma-1AmjaSaudNo ratings yet
- (13384139 - Acta Medica Martiniana) Bronchial Asthma - Current Trends in TreatmentDocument9 pages(13384139 - Acta Medica Martiniana) Bronchial Asthma - Current Trends in TreatmentteuuuuNo ratings yet
- Anti - TB DrugsupdatedDocument35 pagesAnti - TB DrugsupdatedgNo ratings yet
- Drugs in Treatment of Bronchial AsthmaDocument46 pagesDrugs in Treatment of Bronchial AsthmaNikita JangraNo ratings yet
- Drugs Acting On The Pulmonary System 1: Dr. Dita Hasni, M.BiomedDocument50 pagesDrugs Acting On The Pulmonary System 1: Dr. Dita Hasni, M.BiomedYeny ElfiyantiNo ratings yet
- BRONCHIAL ATHMA 2014 Final 2nd y Medicine (M)Document26 pagesBRONCHIAL ATHMA 2014 Final 2nd y Medicine (M)Ahmedshaker21No ratings yet
- Respiratory Tract PharmacologyDocument68 pagesRespiratory Tract PharmacologyRohaan SharmaNo ratings yet
- Pharmacology of The Respiratory SystemDocument39 pagesPharmacology of The Respiratory Systemaleah morenoNo ratings yet
- Hospital Pharmacy Training AssignmentDocument24 pagesHospital Pharmacy Training AssignmentSathish SatzzNo ratings yet
- Pharmacological Management of FeverDocument6 pagesPharmacological Management of FeverNabillaMerdikaPutriKusumaNo ratings yet
- Outpatient Management of Chronic Asthma in 2020: Clinical UpdateDocument2 pagesOutpatient Management of Chronic Asthma in 2020: Clinical UpdateCarla CANo ratings yet
- Pharmacology of AntiepilepticDocument36 pagesPharmacology of AntiepilepticManWol JangNo ratings yet
- NSAIDS 3, 4 SummaryDocument29 pagesNSAIDS 3, 4 SummaryAhmed ExaminationNo ratings yet
- Bronchial Asthma 2.0Document15 pagesBronchial Asthma 2.0Bisweswar OjhaNo ratings yet
- Null 1Document60 pagesNull 1tbuyinza21apNo ratings yet
- (OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Document16 pages(OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Yavuz DanisNo ratings yet
- Saba Hanif Presentation...Document19 pagesSaba Hanif Presentation...Saba KhanNo ratings yet
- Anticonvulsant Part2Document35 pagesAnticonvulsant Part2Rameez ShamounNo ratings yet
- Drugs in ObstetricsDocument95 pagesDrugs in ObstetricsPriya jNo ratings yet
- Fast Facts: Ottimizzazione del trattamento delle fluttuazioni motorie nella malattia di ParkinsonFrom EverandFast Facts: Ottimizzazione del trattamento delle fluttuazioni motorie nella malattia di ParkinsonNo ratings yet
- ANA101 Respiratory System DR GIEDocument44 pagesANA101 Respiratory System DR GIEMarian Kyla MarianoNo ratings yet
- Biology Full Sylabus TestDocument18 pagesBiology Full Sylabus TestgouthamskNo ratings yet
- ABC of Antithrombotic Therapy (True H) 1st Edition 2003Document73 pagesABC of Antithrombotic Therapy (True H) 1st Edition 2003Dr Abdul SattarNo ratings yet
- BM6504U4LS06 Respiration Rate MeasurementsDocument34 pagesBM6504U4LS06 Respiration Rate MeasurementsPrasidha PrabhuNo ratings yet
- GI Polyps DR OdzeDocument30 pagesGI Polyps DR OdzeJuliana Do CoutoNo ratings yet
- L1 Is Introduction To Immunity and The Immune SystemDocument4 pagesL1 Is Introduction To Immunity and The Immune SystemErickson MoragaNo ratings yet
- Science 10 Third Quarter Exam Final Answer OrigDocument4 pagesScience 10 Third Quarter Exam Final Answer Origbernadette delgadoNo ratings yet
- Embryology ReviewerDocument52 pagesEmbryology ReviewerAngela Nicole ManasNo ratings yet
- Braintome PDFDocument49 pagesBraintome PDFPamGarcíaNo ratings yet
- Endocrine System: A & P-Ii Unit VDocument25 pagesEndocrine System: A & P-Ii Unit VAsad KHANNo ratings yet
- GARATA - Week 1 - GB1 - Activity 3 - WorksheetDocument4 pagesGARATA - Week 1 - GB1 - Activity 3 - WorksheetKaren May GarataNo ratings yet
- Activity 7 ConnectorsDocument3 pagesActivity 7 ConnectorsDeniss ArenivasNo ratings yet
- Plant LeavesDocument11 pagesPlant LeavesAndreaaAAaa TagleNo ratings yet
- Muscle Fiber Type Transitions With Exercise Training: Shifting PerspectivesDocument11 pagesMuscle Fiber Type Transitions With Exercise Training: Shifting PerspectivesEnzoNo ratings yet
- Energy Medicine Techniques For Natural Eye and Vision SupportDocument3 pagesEnergy Medicine Techniques For Natural Eye and Vision Supportealzueta4712No ratings yet
- Cambridge IGCSE: BIOLOGY 0610/43Document20 pagesCambridge IGCSE: BIOLOGY 0610/43Rino DoctNo ratings yet
- Answer To Exam Practice CHP 5 PDFDocument5 pagesAnswer To Exam Practice CHP 5 PDF[4D06] CHAU PAK YU [4D06] 周柏宇No ratings yet
- The Cardiovascular System AssignmentDocument6 pagesThe Cardiovascular System AssignmentFarheen AmerNo ratings yet
- Physiology of Labor PDFDocument68 pagesPhysiology of Labor PDFAJ MendozaNo ratings yet
- SR Elite (Set - 2), SR Aiims S60 & Neet MPL Neet Module Test - 3 Paper (01-04-2024)Document26 pagesSR Elite (Set - 2), SR Aiims S60 & Neet MPL Neet Module Test - 3 Paper (01-04-2024)prabha bandaruNo ratings yet
- Dopamine Receptor Subtypes, Physiology and Pharmacology - New Ligands and Concepts in SchizophreniaDocument17 pagesDopamine Receptor Subtypes, Physiology and Pharmacology - New Ligands and Concepts in SchizophreniaolivukovicNo ratings yet
- CHAPTER 14 Cabin Atmosphere Control PDFDocument47 pagesCHAPTER 14 Cabin Atmosphere Control PDFchris laskyNo ratings yet
- Soleus - PhysiopediaDocument6 pagesSoleus - PhysiopediaVahid AtaeiNo ratings yet
- The Importance of The Process of Metabolism On The BodyDocument5 pagesThe Importance of The Process of Metabolism On The BodyCentral Asian StudiesNo ratings yet