Professional Documents
Culture Documents
Connective Tissue Matrix
Uploaded by
aimi Batrisyia0 ratings0% found this document useful (0 votes)
19 views32 pagesOriginal Title
3. Connective Tissue Yr1
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
19 views32 pagesConnective Tissue Matrix
Uploaded by
aimi BatrisyiaCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 32
Prepared by
Dr. Belqees A. Allaw
2021
Introduction
vConnective tissue is the tissue
that connects, separates and
supports all other types of
tissues in the body.
vit consists of cells surrounded by
a compartment of fluid called the
extracellular matrix (ECM).
Introduction
• Based on the cells present and the ECM
structure, we differ two types of
connective tissue:
1- Connective tissue proper divided into:
A- loose connective tissues
B- dense connective tissues
2- Specialised connective tissue: reticular,
blood, bone, cartilage and adipose tissues.
Cells and fibers of connective tissue
The three components of
connective tissue are
A- cells
• fibroblasts, macrophages,
lymphocytes and mast cells,
adipocytes, chondrocytes and
osteocytes.
B- Ground substance
C- Fibers. extracellular
matrix (ECM)
Cells of connective tissue
v fibroblasts are the most common cells of
connective tissue. Typically only the oval
nuclei are visible.
v function:
• synthesizes the extracellular matrix and
collagen.
• plays a critical role in wound healing.
v Macrophages are specialised cells involved in
the detection, phagocytosis and destruction
of bacteria and other harmful organisms.
Cells of connective tissue
vMast cells: are round/oval cells that
contain granules that are
metachromatic because of their
glycosaminoglycan content;
Mast cells
v Lymphocytes: are the most common
connective tissue leukocyte. They have Lymphocytes
a small amount of slightly basophilic
cytoplasm and a large darkly stained
nucleus because of condensed
chromatin.
Cells and fibers of connective tissue
• Ground substance is a viscous gel made of
water, proteoglycans (proteins that are
heavily glycosylated), glycoproteins and
glycosaminoglycans (long chain of sugar
molecules)
• These make the ground substance viscous
and bind high amounts of water which
allows:
1- hydration.
2- diffusion of nutrients.
3- nourishing of the tissue.
fibres of connective tissue
There are three types of protein fibers:
1- Collagen fibers
• predominantly made of collagen type I
(resistance to tension).
• These are the most abundant protein
fiber type, providing varying degrees of
strength and rigidity to tissues.
• Found in scar tissue, skin, tendons,
artery walls, and bones.
fibres of connective tissue
2- Reticular fibers
• consist of collagen type III
(structural maintenance in
expansible organs),
• they are thin delicate fibers that
form a fine meshwork (reticulin) in
organs such as the:
• spleen.
• Kidneys.
• Lymph nodes.
fibers of connective tissue
3- Elastic fibers (yellow fibres)
are made from the protein elastin, giving
stretching and bending properties to tissues.
vThey are mostly found within the walls of
• Large blood vessels.
• Elastic Cartilages e.g: (outer ear, Eustachian tube
and epiglottis).
• Periodontal ligaments (surrounding root of tooth)
• Lungs
• skin
Connective tissue proper
1- loose CT:
• Much ground substance
• Chief cells are the fibroblasts & immune system
cells.
• Main fibers is collagen fibers sparsely distributed
within the ECM.
• moderate amounts of reticular and elastic fibers
are present as well.
Function: support microvasculature, nerves and
immune defense cells.
Examples:
Lamina propria under epithelial lining of digestive &
respiratory tracts.
Connective tissue proper
2- Dense irregular CT:
• Little ground substance
• Few cells (mostly fibroblasts)
• Much collagen fibers in randomly arranged
fibers.
Function: forming a three-dimensional network
resistant to distension in all directions
Examples:
submucosa of the digestive tract.
fibrous capsules of joints.
lymph nodes.
some types of fascia.
Connective tissue proper
3- Dense regular CT:
• Completely filled with parallel bundles of
collagen fibers.
• Few fibroblasts.
Function:
provide strong connections within
musculoskeletal system; strong resistance to
force.
Examples:
Ligaments, tendons (Ligaments connect one
bone to another, while tendons connect muscle
to bone)
Specialized connective tissue
1- Reticular connective tissue
• produced by modified fibroblasts called reticular
cells.
• fibers arranged in an interlaced network similar to
dense irregular CT (the difference is reticular fibers are
thinner, compose a more delicate mesh, with reticular cells
remaining bonded to the fibers)
• Examples:
1- red bone marrow.
2- lymph nodes.
3- the spleen.
Specialized connective tissue
2- Cartilage
is the avascular connective tissue that
connects bones at joints & comprises walls of
upper respiratory airways and external ear.
• It is surrounded by perichondrium:
A- a layer of dense connective tissue.
B- rich in blood vessels.
• Chief cells :chondrocytes, occupied into
cavities within the ECM called lacunae.
• The ECM is vast, rich in water bound to
glycosaminoglycans which makes cartilage
flexible in various degrees but resilient to
mechanical stress.
Types of the cartilages
1- Hyaline cartilage
• most represented type.
• Rich in collagen II molecules
(resistance to pressure),
it is found on:
üthe articular surface of joints
üin the walls of the upper
respiratory airways.
ümedial ends of the ribs.
Types of the cartilages
2- Elastic cartilage
has many elastic fibers.
It is found in the
üwalls of the external ear.
üepiglottis
üCuneiform cartilage in the larynx.
Types of the cartilages
3- Fibrocartilage
has many collagen I molecules
(resistance to tension).
It comprises articular discs, such as:
üIntervertebral discs
üpubic symphysis.
üknee menisci.
Specialized connective tissue
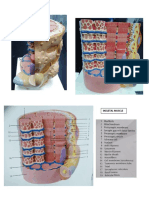
3- Bone
it is a strong, flexible and semi-rigid supporting
tissue. It can withstand compression forces.
• Support - bones make up a structural
framework for the body, and provide
attachment sites for muscles.
• Protection - protection of internal organs - i.e.
brain, heart and lungs,
• Assisting movement.
• Mineral homeostasis - the bone is a store for
calcium and phosphorus
• Blood cell production - takes place in the bone
marrow.
Specialized connective tissue
It Composed of:
A- Cells - osteoclasts and osteocytes.
B- ECM which made up of:
1- an organic matrix (30%).
2- collagen fibres mostly type I (90%).
3- 25% of bone is water.
4- Almost 70% of bone is made up of bone mineral called
hydroxyapatite.
• The EC bone matrix is arranged in circular layers
called lamellae.
• central canal (Haversian canal) which serve for the
passage of neurovascular that supplies the bone and
house the cells.
Specialized connective tissue
• Bone ECM is produced and maintained by several
cells:
1- osteoblasts: actively produce the bone matrix. In
non active stage known as osteocytes.
2- osteoclasts: which are responsible for bone
resorption; rare cells with only 2-3 cells seen per 1
mm3 of bone. Osteoclasts have a " ruffled border"
and are multinucleated.
• The balance of bone formation and resorption is
controlled by a mix of hormones and
biochemicals.
e.g: The loss of estrogen in post-menopausal
women is associated with rapid bone resorption
and loss of bone density and therefore puts this
population at highest risk for osteoporosis.
Specialized connective tissue
4- Blood
is the specialized connective tissue within
the circulatory system that transports blood
cells and dissolved substances throughout
the body via blood vessels.
ECM: known as blood plasma (It consists of
water and solutes (proteins, electrolytes,
nutrients, gases, hormones and waste
products).
Specialized connective tissue
The blood cells:
1- erythrocytes(red blood cells).
2- leukocytes (white blood cells).
3- Thrombocytes (platelets).
These cells produced in the bone
marrow in the process
of hematopoiesis.
Specialized connective tissue
4- Adipose tissue
is the energy-storing connective tissue.
It consists of:
1- adipocytes (fat cells) are large cells specialized
in storage of neutral fats.
Consequently the cell appears as a thin rim of
cytoplasm surrounding the vacuole of dissolved
lipid.
The nucleus is eccentric and flattened.
2- small amount of ECM made of only a few
collagen fibers that keep the cells together.
Depending on how the lipids are distributed
within the cell; there are white and brown
adipose tissues.
Specialized connective tissue
A- brown adipose tissue:
• each cell contains multiple fat drops,
surrounding the centrally positioned
nucleus.
• found in babies which serves for
thermogenesis (heat production).
Specialized connective tissue
B- White adipose tissue
• predominant found in adults.
• Functions:
1- plays a critical role in whole body
energy homeostasis.
2- It stores excess energy in form of
triglycerides.
3- releases fatty acids via lipolysis for
usage by other organs (endocrine organs)
Specialized connective tissue
• White adipose tissue distributes into:
1-Visceral fats surround and support the body
organs, such as eyeballs.
2- Parietal fats are aggregations embedded in the
connective tissue proper of the skin, typically in
the abdominal, back and thigh regions.
Specialized connective tissue
5- Embryonic connective tissue
found in the early embryos and umbilical cord.
Chief cells are mesenchymal cells.
It is divided into:
A- mesenchyme (in embryos).
B- mucoid connective tissue (umbilical cord).
Specialized connective tissue
ØMesenchyme connective tissue
• originates from mesoderm, one of the three
germinative layers in embryos.
• It matures into other types of connective
tissues: muscles, vessels, mesothelium and the
urogenital system.
• mesenchymal cells are dispersed within ECM
filled mainly with reticular fibers.
Specialized connective tissue
ØMucoid connective tissue
found in the umbilical cord.
Its mesenchymal cells are loosely
distributed within a collagen rich ECM
called Wharton’s jelly.
Clinical importance
• Some cells in mesenchyme are multipotent stem
cells potentially useful in regenerative medicine
after grafting to replace damaged tissue in certain
patients.
• Mesenchyme like cells remain present in some
adults CTs including:
1- tooth pulp.
2- some adipose tissue.
You might also like
- Vitamin What The Vitamin Does Significant Food Sources B1 (Thiamin)Document4 pagesVitamin What The Vitamin Does Significant Food Sources B1 (Thiamin)Safi BroNo ratings yet
- 4 - TissueDocument13 pages4 - TissueGel Austin PascuaNo ratings yet
- Skeletal Anatomy NotesDocument7 pagesSkeletal Anatomy NotesalchriwNo ratings yet
- Anatomy 1.02 Axial SkeletonDocument8 pagesAnatomy 1.02 Axial SkeletonMark AbrazaldoNo ratings yet
- Im Dude HandoutDocument1 pageIm Dude Handoutapi-535001113No ratings yet
- The Impact of Vitamin D Pathway Genetic Variation and Circulating 25-Hydroxyvitamin D On Cancer Outcome. Systematic Review and Meta-AnalysisDocument19 pagesThe Impact of Vitamin D Pathway Genetic Variation and Circulating 25-Hydroxyvitamin D On Cancer Outcome. Systematic Review and Meta-AnalysisDaniel AriasNo ratings yet
- MODUL HEMATOLOGIE AND BIOCHEMISTRY TESTSDocument2 pagesMODUL HEMATOLOGIE AND BIOCHEMISTRY TESTSOana PaduraruNo ratings yet
- NextGen Practice Management Accounts and Patient Records Guide Version 5.8Document100 pagesNextGen Practice Management Accounts and Patient Records Guide Version 5.8dikivNo ratings yet
- Fused Deposition Modeling (FDM) Technology: Z Resolution - Layer ThicknessDocument11 pagesFused Deposition Modeling (FDM) Technology: Z Resolution - Layer ThicknessFaizanwajidNo ratings yet
- 16.classification of JointsDocument19 pages16.classification of JointsdenekeNo ratings yet
- Ospe ParasitologyDocument19 pagesOspe Parasitologyaimi Batrisyia100% (1)
- Health Assessment: Focus on Abnormal FindingsDocument2 pagesHealth Assessment: Focus on Abnormal FindingsDanna TanNo ratings yet
- Speech 30 SyllabusDocument7 pagesSpeech 30 SyllabusHaruki AkemiNo ratings yet
- AAP Module 9 SupplementDocument20 pagesAAP Module 9 Supplementmaryelle conejarNo ratings yet
- B Vitamins 1Document1 pageB Vitamins 1api-245692797No ratings yet
- Skeletal and Muscular System - FinalDocument30 pagesSkeletal and Muscular System - Finalastraia celesteNo ratings yet
- Joints TransesDocument19 pagesJoints TransesskidamarinkNo ratings yet
- Imaging of UroradiologyDocument32 pagesImaging of UroradiologyAdib Ul IslamNo ratings yet
- Higher Education Module ProgramDocument2 pagesHigher Education Module ProgramWen Jie LauNo ratings yet
- Timer Temporary Immersion Bio-Reactor (Basic DIY Diagram)Document1 pageTimer Temporary Immersion Bio-Reactor (Basic DIY Diagram)potadoNo ratings yet
- Cell Fucking MembraneDocument12 pagesCell Fucking MembraneColeen ParejaNo ratings yet
- Muscle Chart Upper ExtremityDocument3 pagesMuscle Chart Upper Extremitykep1313100% (1)
- All About Skull PDFDocument28 pagesAll About Skull PDFJoel SeradNo ratings yet
- TissuesDocument42 pagesTissuesJeevitha VanithaNo ratings yet
- Bacteria Nutrition, Growth and CultureDocument40 pagesBacteria Nutrition, Growth and Cultureaimi BatrisyiaNo ratings yet
- Community Psychology Rudkin PDFDocument2 pagesCommunity Psychology Rudkin PDFLance0% (2)
- English For Business: Level 1Document24 pagesEnglish For Business: Level 1anonymous9196806No ratings yet
- Well Construction Journal - May/June 2014Document28 pagesWell Construction Journal - May/June 2014Venture PublishingNo ratings yet
- Hand Soap CDCDocument2 pagesHand Soap CDCswesty100% (1)
- Process Analyzer Sampling System TrainingDocument3 pagesProcess Analyzer Sampling System TrainingPhilNo ratings yet
- CONNECTIVE TISSUE LEC WEEK 4Document5 pagesCONNECTIVE TISSUE LEC WEEK 4Abigrael TangcoNo ratings yet
- General Medicine Diagnostic Points PDFDocument14 pagesGeneral Medicine Diagnostic Points PDF1031 Muhammad zaryabNo ratings yet
- Professional Self-ImprovementDocument19 pagesProfessional Self-ImprovementBenedict AguilarNo ratings yet
- Anatomy of Vertebral ColumnDocument59 pagesAnatomy of Vertebral ColumnRivan DwiutomoNo ratings yet
- Anatomy and Physiology Reviewer: 4 Types of TissuesDocument9 pagesAnatomy and Physiology Reviewer: 4 Types of TissuesBaylon, MarkNo ratings yet
- Connective Tissue by Dr. Gironella PDFDocument3 pagesConnective Tissue by Dr. Gironella PDFFatima RadeenaNo ratings yet
- 3D Printer InformationDocument16 pages3D Printer Informationmahesh mulikNo ratings yet
- Chapter 6. HistologyDocument22 pagesChapter 6. Histologymaryelle conejarNo ratings yet
- Blood/plasma/serum Tests Patient's Value Normal Values UnitsDocument2 pagesBlood/plasma/serum Tests Patient's Value Normal Values UnitsDragos Rosca100% (1)
- Anatomy & Physiology With Pathophysiology Lecture (Midterms)Document4 pagesAnatomy & Physiology With Pathophysiology Lecture (Midterms)Millen ArenasNo ratings yet
- Study Guide 1Document3 pagesStudy Guide 1msmickey24No ratings yet
- Tissue CTDocument1 pageTissue CTAditi MishraNo ratings yet
- SKIN STRUCTURE &FUNCTION Lec 1Document40 pagesSKIN STRUCTURE &FUNCTION Lec 1Sadia SohailNo ratings yet
- Biochem Nutrition TransDocument7 pagesBiochem Nutrition TransCyril Dayne Marie BaldeNo ratings yet
- NDI SDK DocumentationDocument53 pagesNDI SDK DocumentationПравда За НародNo ratings yet
- AACN Procedure For High-Acuity, Progressive, and Critical Care 2017Document11 pagesAACN Procedure For High-Acuity, Progressive, and Critical Care 2017Cathy BellNo ratings yet
- S. Y. B.Sc. Botany CBCS Pattern Practical (Semester IV Paper III) 2020-2021 BO 243: Practical Based On BO 241 & BO 242Document36 pagesS. Y. B.Sc. Botany CBCS Pattern Practical (Semester IV Paper III) 2020-2021 BO 243: Practical Based On BO 241 & BO 242Pallavi JadhavNo ratings yet
- 1A Non ChordataDocument62 pages1A Non ChordataDeepak ThakurNo ratings yet
- Standard of Care - NotesDocument25 pagesStandard of Care - NotesIso ShizhengNo ratings yet
- Corneum and Is Directly Exposed To TheDocument3 pagesCorneum and Is Directly Exposed To Theydnic alykPNo ratings yet
- WT - Anatomy of Flowering PlantsDocument71 pagesWT - Anatomy of Flowering PlantsRenu100% (1)
- Natural Selection PracticalDocument3 pagesNatural Selection Practicalapi-664238572No ratings yet
- Natural Product As AntiviralDocument30 pagesNatural Product As AntiviralMayuriNo ratings yet
- Smart Helmet Wiper Automatically Cleans VisorDocument4 pagesSmart Helmet Wiper Automatically Cleans VisorBhavana DornalaNo ratings yet
- CELLDocument45 pagesCELLKimberly Clarisse VegaNo ratings yet
- Cell Structure & OrganisationDocument62 pagesCell Structure & OrganisationSUNDARI SIVASANKARNo ratings yet
- The Cell in Its Environment SummaryDocument1 pageThe Cell in Its Environment Summaryapi-292648627100% (1)
- Thermoelectric Generator for Home EnergyDocument6 pagesThermoelectric Generator for Home EnergyRommel J. OlorazaNo ratings yet
- 雅思口语 900 句话题速查Document40 pages雅思口语 900 句话题速查LingYan LyuNo ratings yet
- CVBD Easy-To-digest No 2 CoinfectionDocument8 pagesCVBD Easy-To-digest No 2 Coinfectionsnooty.eli.gamedogsNo ratings yet
- Biology AML NMAT ReviewerDocument15 pagesBiology AML NMAT ReviewerJocelyn Mae CabreraNo ratings yet
- AnaPhy Cells and TissueDocument17 pagesAnaPhy Cells and TissueVernice LopezNo ratings yet
- Cell Cycle Guide 2Document3 pagesCell Cycle Guide 2api-318387471No ratings yet
- Panic (Critical) Values 06-14-2021 0Document2 pagesPanic (Critical) Values 06-14-2021 0JorgeNo ratings yet
- Food Matters Food Additives To AvoidDocument1 pageFood Matters Food Additives To AvoidPopescu Bogdan ConstantinNo ratings yet
- 4.1 Connective Tissue - SMDocument52 pages4.1 Connective Tissue - SMManjunathNo ratings yet
- التشريح والفسلجة نظريDocument16 pagesالتشريح والفسلجة نظريem2200139No ratings yet
- Single Verb Agreement Exercise (Aimi Batrisyia Ali - MBBS0321299)Document7 pagesSingle Verb Agreement Exercise (Aimi Batrisyia Ali - MBBS0321299)aimi BatrisyiaNo ratings yet
- (Challenges of Online Learning) AIMI BATRISYIA BT ALI-MBBS0321299Document2 pages(Challenges of Online Learning) AIMI BATRISYIA BT ALI-MBBS0321299aimi BatrisyiaNo ratings yet
- Muscle TissueDocument31 pagesMuscle Tissueaimi BatrisyiaNo ratings yet
- Types of Sentences in Writing (AIMI BATRISYIA BT ALI-MBBS0321299)Document2 pagesTypes of Sentences in Writing (AIMI BATRISYIA BT ALI-MBBS0321299)aimi BatrisyiaNo ratings yet
- Ospe HistologyDocument17 pagesOspe Histologyaimi BatrisyiaNo ratings yet
- Histology Nervous TissueDocument27 pagesHistology Nervous Tissueaimi BatrisyiaNo ratings yet
- Effect of Acid Attacks (Aimi Batrisyia BT Ali-Mbbs0321299)Document1 pageEffect of Acid Attacks (Aimi Batrisyia BT Ali-Mbbs0321299)aimi BatrisyiaNo ratings yet
- Lab 4Document12 pagesLab 4yemurai shureNo ratings yet
- Introduction & Cell Morphology 1Document55 pagesIntroduction & Cell Morphology 1aimi BatrisyiaNo ratings yet
- The Human Anatomy Guide: Skeletal, Muscular & Nervous SystemsDocument16 pagesThe Human Anatomy Guide: Skeletal, Muscular & Nervous Systemsaimi BatrisyiaNo ratings yet
- 4 PharmacodynamicsDocument21 pages4 Pharmacodynamicsaimi BatrisyiaNo ratings yet
- Culture MethodsDocument26 pagesCulture Methodsdrunken monkeyNo ratings yet
- Epithelial TissueDocument26 pagesEpithelial Tissueaimi BatrisyiaNo ratings yet
- Cranial Nerves - AllDocument96 pagesCranial Nerves - Allaimi BatrisyiaNo ratings yet
- Bacterial Genetics: I. II. Mutations Iii. Transfer of Dna Between Cells IV. RecombinationDocument23 pagesBacterial Genetics: I. II. Mutations Iii. Transfer of Dna Between Cells IV. Recombinationaimi BatrisyiaNo ratings yet
- 6-PATHOGENICITY AND HOST DEFENSES (Autosaved)Document56 pages6-PATHOGENICITY AND HOST DEFENSES (Autosaved)aimi BatrisyiaNo ratings yet
- 4 Pharmacokinetics 3Document19 pages4 Pharmacokinetics 3aimi BatrisyiaNo ratings yet
- 2-Bacterial Classification and Normal FloraDocument26 pages2-Bacterial Classification and Normal Floraaimi BatrisyiaNo ratings yet
- Pharmacology overview and history of the fieldDocument17 pagesPharmacology overview and history of the fieldaimi BatrisyiaNo ratings yet
- 3 Routes of Administration of DrugsDocument20 pages3 Routes of Administration of Drugsaimi BatrisyiaNo ratings yet
- 1-Introduction To MicrobologyDocument17 pages1-Introduction To Microbologyaimi BatrisyiaNo ratings yet
- Bacterial Genetics: I. II. Mutations Iii. Transfer of Dna Between Cells IV. RecombinationDocument23 pagesBacterial Genetics: I. II. Mutations Iii. Transfer of Dna Between Cells IV. Recombinationaimi BatrisyiaNo ratings yet
- 3 Pharmacokinetics 2Document15 pages3 Pharmacokinetics 2aimi BatrisyiaNo ratings yet
- Exercise (One Sentence Each Rule) Aimi Batrisyia-MBBS0321299Document1 pageExercise (One Sentence Each Rule) Aimi Batrisyia-MBBS0321299aimi BatrisyiaNo ratings yet
- Embryonic Period 4-8weekDocument25 pagesEmbryonic Period 4-8weekaimi BatrisyiaNo ratings yet
- Embryology of 2nd WeekDocument25 pagesEmbryology of 2nd Weekaimi BatrisyiaNo ratings yet
- 2 Pharmacokinetics 1Document20 pages2 Pharmacokinetics 1aimi BatrisyiaNo ratings yet
- New Pricelist Iclean Zone 1 HK PDFDocument3 pagesNew Pricelist Iclean Zone 1 HK PDFegierpeNo ratings yet
- Ficha María y Beatriz 14Document16 pagesFicha María y Beatriz 14Alex8mRNo ratings yet
- Horno Industrial HC1 v1.1Document30 pagesHorno Industrial HC1 v1.1Cristian urielNo ratings yet
- PaliLossy PDFDocument408 pagesPaliLossy PDFtemp100% (2)
- Chapter 4Document4 pagesChapter 4juncatalanNo ratings yet
- A Memory of SolferinoDocument44 pagesA Memory of SolferinoTuan Ahmad Aminro NasrinNo ratings yet
- Individual and Market Demand: Chapter OutlineDocument57 pagesIndividual and Market Demand: Chapter OutlineAbdullahiNo ratings yet
- 2309 The Memory Tree BookDash FKBDocument19 pages2309 The Memory Tree BookDash FKBuyhgjhNo ratings yet
- Claim and Counter Claim Signal WordsDocument21 pagesClaim and Counter Claim Signal WordsYra MatiasNo ratings yet
- Registered Architects 2019 Grade 1Document3 pagesRegistered Architects 2019 Grade 1santosh bharathy100% (1)
- Effect of Smell in Space PerceptionDocument8 pagesEffect of Smell in Space PerceptionApoorva KalraNo ratings yet
- Azure FaDocument4 pagesAzure Faanurag pattanayakNo ratings yet
- Middle School English Planning GuideDocument8 pagesMiddle School English Planning GuideVictoria GutierrezNo ratings yet
- Pike County Sheriff Forms Major Crimes Task Force For Unsolved MurdersDocument2 pagesPike County Sheriff Forms Major Crimes Task Force For Unsolved MurdersAndy Burgoon100% (1)
- About The Rosary of Our LadyDocument2 pagesAbout The Rosary of Our LadyINONG235No ratings yet
- Computerized Scholarship Monitoring SystemDocument11 pagesComputerized Scholarship Monitoring SystemCharles VegasNo ratings yet
- Ethnonationalism and Liberal DemocracyDocument66 pagesEthnonationalism and Liberal DemocracyLaw&CrimeNo ratings yet
- Vegetable Salad RecipesDocument11 pagesVegetable Salad RecipesPraneet NagdevNo ratings yet
- WEG-WEMOB-totem-10008242920-guia-de-instalacao-ptDocument2 pagesWEG-WEMOB-totem-10008242920-guia-de-instalacao-ptalexcampos172No ratings yet
- Group 1 RRLSDocument4 pagesGroup 1 RRLScyrusarckreibagoNo ratings yet
- Demise of Blockbuster - A Case Study ReviewDocument13 pagesDemise of Blockbuster - A Case Study ReviewYash MudliarNo ratings yet
- GaDocument101 pagesGaSugan GeeNo ratings yet
- OSHA3871Document3 pagesOSHA3871SHANE ANGEL BORBENo ratings yet
- F. Rizal Trip To MadridDocument2 pagesF. Rizal Trip To MadridAdrian MarananNo ratings yet
- 4 Bedroom HouseDocument1 page4 Bedroom Housepatrick chegeNo ratings yet