Professional Documents
Culture Documents
21 Prosthetics (FINAL)
Uploaded by
kath-kathCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
21 Prosthetics (FINAL)
Uploaded by
kath-kathCopyright:
Available Formats
Prosthetics
Replacement to lost body part
MC Amputation
Congenital Acquired
UE (L) Terminal Trans radial (R) Transradial d/t Trauma -> PVD
LE Absence of Fibula (Tibial Bowing) Transtibial (BKA) – PVD -> Trauma
Pre-Prosthetic Considerations
Considerations UE BK AK
Size 3-4” 5-7” >10”
Posterior
Middle Middle
Flap Burges
Fishmouth Fishmouth
(Gastrocs)
Any
Shape Cy Co
Best: Cy
Skin 100% Sensation, dry, pliable
Nerves Retracted (cutting nerve under tension); prevent neuroma formation
Bones Rounded: check for bony overgrowth (pedia)
Muscles Stabilized, MMT 4-5/5, (-) Contractures
Blood Vessels (-) edema, (-) hematoma
You know the size of all your stumps
its 3-4, 5-7, gree-eat than 10!
How ‘bout the flast, that cover up,
‘upper above middle yan, below burgess naman
Song Any ang shape pag kay UE but
“You don’t know Your the best is cylindrica-al!
Beautiful”
SKIN has 100 sensation, dry and pliable
NERVES are retracted, bones rounded, check for overgrowth
MUSCLE are stabilized, Gr 4-5 walang tikop
BLOOD VESSELS No-o-o edema o buong dugo-o-o; bawal may dugong buo!
Cy: cylindrical; Co: conical
Choke Syndrome: brownish-yellow skin d/t tight bandaging
Muscle Procedures
1. Myodesis – muscle connected to bone
2. Tenodesis – most physiologic; tendon connected to bone
3. Myoplasty – muscle connected to muscle
4. Myofascial Closure – muscle connected to fascia
Typically all is done together
UE Prosthesis
Gold Rank Intensive Review Baguio Batch 2017
Prosthetics
Components
1. Terminal Device – hand
2. Wrist Unit – handles the wrist movements
3. Control Devices – make terminal device move
4. Elbow unit
5. Socket – cradle of the stump
6. Suspension – connects prosthesis to the rest of the body part
I. Terminal Device
Hand or hook
PBEQ: “What is the MC prehension of your Terminal Device? A – 3 Jaw Chuck
a. Passive Cosmetic/Hands
b. Electric Powered (Batteries motor units)
c. Body powered (contraction of a muscle) usually deltoids
d. Cable Driven – obsolete
PBEQ: “What is the most common and most functional terminal device?” A. Voluntary OFening
Most Physiologic: Closing
II. Wrist Unit
Function:
o A quick disconnect
o Friction control: used for a more controlled movement
o Spring Assisted: ↑ flexion & extension of the wrist
III. Control Devices
Makes terminal devices move
o Bowden: 1 casing
o Fair Lead: 2 casings (More complex)
IV. Elbow Unit
5-135° elbow flexion
a. Mechanical: hinged-type
b. Electric Powered
c. Myoelectric (contractions)
o Digital: (+) on/off controls
o Proportional: ↑ contraction = ↑ speed of movement
V. Socket
a. Standard: fitted to size
b. Müenster: very short Below Elbow Amp.
c. 3-Walled Socket: preferred for infants; provides very low pressure; inner, middle, outer walls
VI. Suspension
Suction: most effective
o Uses (-) atmospheric P°; preferred for younger
o One-way valve
Figure of 8: Most common
Figure of 9: One strap connected to bowden device
Condylar: encloses humeral condyles; ↑ stability
Lanyard: cord socket-outer socket
Pediatric Readiness
UE: 3 – 6 mos.
LE: 8 – 10 mos.
Active T.D: 2 y.o
Active E.U: 2 – 3 y.o
Gold Rank Intensive Review Baguio Batch 2017
Prosthetics
Functional Hand: 3 y.o
Active KJ: 3 – 4 y.o
Awwh!!!!
Pediatric Check-Out
UE LE
0-5 y/o Annually
5-12 y/o at 18 months Bi-annully
12-21 y/o every 3-4 years
Normal Lifespan: 3 y/o (depends on wear and tear)
Golden Period of Prosthetic Fitting: 1 mo or 30 days
Lower Extremity Prosthesis
I. Below Knee
1A. Foot Ankle Assembly: Non-Articulated
1. (-) mechanical ankle joint
2. FAA connected to shank
3. Lighter & quieter
4. Active
5. Simpler Designs
6. Keel: weight supporting structure inside the prosthetic foot
Types of Non-Articulated FAA
1. SACH (Solid Ankle Cushion Heel)
a. Most Common
b. Cushion Heel: absorbs shock
i. Stiff: DF --> Knee flexion
ii. Soft: PF --> Knee extension
c. Toe Break: MTP Joints
2. SAFE (Stationary Attachment Flexible Endoskeleton)
a. SA: rigid bolt blod
b. FE: movable keel
c. Modified SAFE: SAFE Lite (lighter)
3. STEN (Stored Energy)
a. Has 3 pieces of wooden keel and 2 pieces of rubber plugs
b. Heavier than SACH
4. Quantum: spring module (keel)
a.
5. Seattle: “C-shaped” Delrin Keel
a. Seattle – “C”
b. Acts like a cantilever
c. Modified: Seattle Lite
6. Carbon Copy II
a. Has 2 carbon plates
b. Long (Walk)
c. Short (Run)
d. Light Weight
7. Flex-Walk
a. Foot made of Carbon Graphite
8. Flex-Foot
a. Same with flex walk
b. Foot continues to be the shaft
Non-Articulated FAA Codes
Heavy: SAFE STreet in SEATTLE are heavy (SAFE, STEN, SEATTLE)
Lightweight: CAR QUo WALK FOOT kaya lightweight (Carbon Copy II, Quantum, Flex Walk, Flex Foot)
Gold Rank Intensive Review Baguio Batch 2017
Prosthetics
M-L Motion: SACH SAFE CARBON QUd WALK M-L Motion (SACH, SAFE, Carbon Copy II, Quantum, Flex Walk)
1B. Foot Ankle Assembly: Articulated
1. (+) Mechanical Ankle Joint
2. Px with sit-stand transfer difficulty
3. Heavier & noisy
4. Complex in Design
Parts
1. Axis
a. Single: DF (5), PF (15) inherent stability
b. Multi: DF, PF, Inv, Ev, slight rot
c. Polycentric: Sports
II. Shank
a. Exoskeletal – normal leg, hollow inside; aka Crustacean type
b. Endoskeletal – aka central support, modular, pylon; More common
III. Socket
1. Patellar Tendon Bearing (PTB)
a. Most Common
b. PBEQ: Pressure Sensitive vs Pressure Tolerant
Pressure Sensitive Pressure Tolerant
AT PT
Depressions Built-ups/Bulges
provide relief
No Redness
2. Hard (Thermoplastic)
a. Given to px with Heavy Perspiration
b. Px must have good/mature tissue covering
3. ISNY (Icelandish Swedish New York)
a. Good Ventilation
b. Thin to dissipate heat
c. Translucent (plastic)
IV. Suspension
1. Cuff: Most Common
2. SC (Supra-Condylar)
a. Encloses femoral condyles
b. Better Stability
c. High Med & Lat Walls
d. More Cosmetic
3. SC-SP (Supracondylar-Suprapatellar) Suspension
a. High Med.Lat.Ant. Walls
b. Greater stability
c. Very Short Below Knee Amp.
II. Above Knee
Energy Expenditure
1 below: 10-40%
2 below: 41%
1 Above: 65%
1 Above, 1 below: 75%
2 above: 110%
Crutches: 60%
Gold Rank Intensive Review Baguio Batch 2017
Prosthetics
W/C: 9%
I. Knee Assembly
a. Axis
a. Single: F, E
b. Multi/Polycentric: F, E, IR, ER
i. (+) Screwhome mechanism
ii. For Sports/active px
b. Friction
a. Constant
i. Sliding
ii. Friction remains constant all throughout gait
iii. ↑ speed
b. Variable
i. Sliding
ii. ↑ friction during acceleration and deceleration
iii. Prevents terminal swing impact
c. Fluid Control
i. More expensive; provides cadence dependent motion
ii. Pneumatic: air
iii. Hydraulic: oil
c. Extension Aid/Extension Stop
a. Extension Aid: aids knee extension, for px with weak quads
b. Extension Stop/Bumper/Resistance: for px with G. Recurvatum
d. Locking Mechanism
a. Manual
b. Weight Activated:
i. Locks at 20°-30° extension
ii. Elderly
e. Socket
a. Quadrilateral Sockets
i. Has wider Medial-Lateral structure
ii. Weight bearing: ischial Tuberosity
iii. Walls
1. Posterior Wall (WB Part)
a. G.Max rests on Posterior Wall
2. Anterior and Lateral Walls are higher 2.5-3” higher
3. Medial Wall accommodates for the adductor muscles
4. Lateral Wall prepositioned in adduction to give greater leverage for the Abductors: 7°
iv. Stability (Elderly)
v. Most Commonly Used
b. Ischial Containment
i. WB: Ascending ischio-pubic ramus
ii. For Mobility
iii. For young/athletic
f. Suspension
a. Suction
i. MC
ii. Difficult to wear
iii. Painful for elderly
b. Partial Suction with Auxiliary Suspension
c. Silesian Bandage
i. Provides rotatory control
d. Pelvic Bandage/Corset
i. Last Option
ii. Very unstable
Gold Rank Intensive Review Baguio Batch 2017
Prosthetics
iii. (+) Heavy perspiration
iv. Can promote atrophy
v. Heavy in weight
Below Knee Gait Deviation
1. HS --> FF --> MS
A. Increased Knee Flexion
a. Increased DF
b. Excessively STIFF Cushion Heel
c. Increase Anterior Displacement of Socket
d. Flexion Contracture: 20° + 15-20° = 35-40°
B. Decreased Knee Flexion
a. Increased PF
b. Soft Cushion Heel
c. Increase Posterior Socket
d. Quadriceps Weakness: eccentric contraction
e. Anterodistal discomfort
f. Habit: knees kept in extension
2. MS Only
A. Lateral Thrusting Position
a. ↑ Medial Displacement of Foot
b. Abd Socket
3. HO --> TO
A. Early Flexion (weight nearer toe break)
a. ↑ Anterior Socket
b. ↑ Posterior Toe Break
c. ↑ DF
d. ↑ Soft DF Bumper
B. Late Flexion
a. ↑ posterior socket
b. ↑ anterior toe break
c. ↑ PF
d. ↑ Hard DF Bumper
Above Knee Gait Deviation
1. Lateral Trunk Bending (Trendelenburg)
a. Weak Hip Abd
b. Abd Contracture
c. Abd Socket
d. ↓ support for Lateral Wall
e. Pain discomfort
f. Short Prosthesis
2. Wide Walking Base/Abducted Gait
a. Pain on crotch area
b. Contracted hip abductors
c. Prosthesis too long
d. Shank aligned in VALGUS
e. Socket is abducted
f. Insecurity
3. Circumduction
a. Insecurity/fear
b. ↑ friction/↑ tight extensor aid
c. ↓ suspension
d. Too small socket
e. ↑ PF
Gold Rank Intensive Review Baguio Batch 2017
Prosthetics
f. Long prosthesis
4. Vaulting
a. ↓ friction (↑mov’t)
b. Long prosthesis + all of circumduction
5. Swing Phase Whips
a. At & just after TO
b. Heel
i. Medial: Knee ER
ii. Lateral: Knee IR
c. Causes
i. Improper alignment (Knee)
ii. Weak/Flabby Muscle (Suction)
iii. Too Small Socket
6. Foot Rotation @ HS
a. Too stiff cushion Heel
b. ER (lateral)
7. Foot Slap
a. PF Stop, Too soft
8. Uneven Heel Rise
a. ↑/Excessive
i. ↓ friction
ii. ↓ tension (Extension aid)
iii. Forceful hip flexion
b. ↓ Heel Rise
i. ↑ friction
ii. Too tight (extension aid)
iii. Insecure
iv. Manual lock
9. Terminal Impact
a. Causes
i. ↓ friction at terminal unit
ii. Too tight
iii. Fear of buckling
iv. Absent extension bumper
10. Uneven Step Length
a. Pain/insecurity
b. Hip flexion contracture
c. ↓ friction
11. Exaggerated Lordosis
a. Hip flexion contracture
b. ↓ socket flexion (initial flexion: 5°)
c. ↓support for anterior wall
d. Weak hip extensors
e. Weak abdominal mm
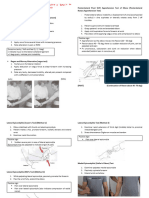
Below Knee Pressure Sensitive Areas
Anterior Tibia
Anterior Tibial Crest
Fibular Head & neck
Peroneal N.
Above Knee Pressure Sensitive Areas (All other areas not listed are tolerant areas)
Pubic Symphysis
Perineal A.
Distolateral end of the femur
Gold Rank Intensive Review Baguio Batch 2017
You might also like
- 19 Fractures (FINAL)Document7 pages19 Fractures (FINAL)kath-kathNo ratings yet
- 12 Sports Physiology (FINAL)Document6 pages12 Sports Physiology (FINAL)kath-kathNo ratings yet
- GaitDocument15 pagesGaitआशिष दादाNo ratings yet
- 24 Neuroconditions (FINAL)Document14 pages24 Neuroconditions (FINAL)kath-kathNo ratings yet
- Rehabilitation ProtocolDocument9 pagesRehabilitation ProtocolMukesh YadavNo ratings yet
- Motor Neuron Disease GuideDocument5 pagesMotor Neuron Disease Guidekath-kathNo ratings yet
- DystoniaDocument24 pagesDystoniaAyesha NasirNo ratings yet
- Elbow Special TestDocument4 pagesElbow Special TestEllaiza Astacaan100% (1)
- Elbow biomechanics overviewDocument7 pagesElbow biomechanics overviewsanavoraNo ratings yet
- 12 - Rehabilitation After Fractures of - 2018 - Clinical Orthopaedic Rehabilitat PDFDocument7 pages12 - Rehabilitation After Fractures of - 2018 - Clinical Orthopaedic Rehabilitat PDFTolo CantallopsNo ratings yet
- Fractures of Spine and Pelvis2007Document70 pagesFractures of Spine and Pelvis2007api-19916399No ratings yet
- Special TestsDocument31 pagesSpecial TestsKyle OrtegaNo ratings yet
- PT Evaluation Reveals Sensory LossDocument5 pagesPT Evaluation Reveals Sensory LossZgama AbdulrahmanNo ratings yet
- SHOULDER INSTABILITY ManagDocument18 pagesSHOULDER INSTABILITY ManagFarhan JustisiaNo ratings yet
- 8 Integumentary System (FINAL)Document11 pages8 Integumentary System (FINAL)kath-kathNo ratings yet
- Radial Head FractureDocument40 pagesRadial Head FractureammarNo ratings yet
- Lower Extremity Anatomy ReviewDocument32 pagesLower Extremity Anatomy Reviewkath-kath100% (1)
- Prometric ReviewerDocument134 pagesPrometric ReviewerWilyam SerilNo ratings yet
- Group 2 - IeDocument14 pagesGroup 2 - IeGabriel RagasaNo ratings yet
- 2 Pulmonary System (FINAL)Document17 pages2 Pulmonary System (FINAL)kath-kathNo ratings yet
- Special TestsDocument22 pagesSpecial TestsEsterGrefielNo ratings yet
- Spine AnatomyDocument7 pagesSpine AnatomydoctoryyyNo ratings yet
- Case History TakingDocument30 pagesCase History TakingShabeel Pn100% (1)
- Ayesha UroojDocument43 pagesAyesha Uroojpasha100% (1)
- PIVDDocument18 pagesPIVDAayushi SrivastavaNo ratings yet
- The Hip JointDocument6 pagesThe Hip JointSiva ShanmugamNo ratings yet
- Upper Extremity FracturesDocument80 pagesUpper Extremity FracturesSidan EmozieNo ratings yet
- Quiz IVDocument5 pagesQuiz IVErvin T MileNo ratings yet
- Physio Exam 27917 QueDocument23 pagesPhysio Exam 27917 QueDeepa SeiraNo ratings yet
- Modul Hip Disarticulation ProstheticsDocument67 pagesModul Hip Disarticulation ProstheticsCapt KidsNo ratings yet
- Hip Examination Bone SchoolDocument63 pagesHip Examination Bone SchoolKhan Go Pang ShahidNo ratings yet
- Spinal Column and Pelvis PalpationDocument14 pagesSpinal Column and Pelvis PalpationMa Rhodalyn Mae AtienzaNo ratings yet
- Knee Biomechanics: Andrew CrosbyDocument32 pagesKnee Biomechanics: Andrew CrosbyBhanu Pratap PangteyNo ratings yet
- Damage Control Orthopaedics in Spinal Trauma JAAOSDocument12 pagesDamage Control Orthopaedics in Spinal Trauma JAAOSAzmi FarhadiNo ratings yet
- Cerebral Palsy Revalida FormatDocument10 pagesCerebral Palsy Revalida FormatChelsea CalanoNo ratings yet
- Norkin, C. C., & White, D. J. (2009) - Measurement of Joint Motion: A Guide To Goniometry. Philadelphia: F.A. Davis. jdcptrp2019Document12 pagesNorkin, C. C., & White, D. J. (2009) - Measurement of Joint Motion: A Guide To Goniometry. Philadelphia: F.A. Davis. jdcptrp2019Anne SerneoNo ratings yet
- KMC Dept of Orthopaedics Floor Reaction OrthosisDocument5 pagesKMC Dept of Orthopaedics Floor Reaction OrthosischinmayghaisasNo ratings yet
- Pediatric OrthopedicsDocument28 pagesPediatric OrthopedicsEdwin OkonNo ratings yet
- GAIT 2 - Clinical Gait Analysis - HandoutDocument32 pagesGAIT 2 - Clinical Gait Analysis - Handoutj100% (1)
- Hip Joint: 5 December 2016 Anatomy Lecture By: DR Anita RaniDocument38 pagesHip Joint: 5 December 2016 Anatomy Lecture By: DR Anita RaniDr'Dinesh MishraNo ratings yet
- Shoulder Peripheral Joint Mobilization No Joint Mobilization Indication Position of Patient Hand Placement Mobilization ForceDocument14 pagesShoulder Peripheral Joint Mobilization No Joint Mobilization Indication Position of Patient Hand Placement Mobilization ForceEdwinNo ratings yet
- Seminar On Upper Limb FractureDocument166 pagesSeminar On Upper Limb FractureArko dutta100% (1)
- Adolescent Idiopathic ScoliosisDocument29 pagesAdolescent Idiopathic ScoliosisfenskaNo ratings yet
- Principles of Tendon Transfer in The Hand and ForearmDocument9 pagesPrinciples of Tendon Transfer in The Hand and Forearm'Ema Surya PertiwiNo ratings yet
- Gait by SRSDocument109 pagesGait by SRSSreeraj S RNo ratings yet
- Harrison TablesDocument163 pagesHarrison TablesPratikNo ratings yet
- Prosthetic GaitDocument33 pagesProsthetic GaitDibyendu DuttaNo ratings yet
- Anatomy #2 Vertebral Column-1Document49 pagesAnatomy #2 Vertebral Column-1ffNo ratings yet
- P&O Elementary MathematicsDocument22 pagesP&O Elementary MathematicsrrutayisireNo ratings yet
- Rembe EmeraldDocument7 pagesRembe EmeraldNinjaNo ratings yet
- Clinical Biomechanics of Gait: OutlineDocument7 pagesClinical Biomechanics of Gait: Outlinechacho1971100% (1)
- 3 Head, Neck, Back, and Spine ModuleDocument55 pages3 Head, Neck, Back, and Spine ModuleCoffee MorningsNo ratings yet
- Biomechanics of The ElbowDocument16 pagesBiomechanics of The ElbowAsmaa Ahmad SharawyNo ratings yet
- Connective TissueDocument14 pagesConnective TissueDr NehaNo ratings yet
- Acumed® Clavicle PlatingDocument68 pagesAcumed® Clavicle Platingthomsoon01No ratings yet
- Lower Limb Evaluation Format Lower Limb Fracture Assesstment FormDocument12 pagesLower Limb Evaluation Format Lower Limb Fracture Assesstment FormsridharNo ratings yet
- 4 ScoliosisDocument8 pages4 ScoliosisApril IsidroNo ratings yet
- Floor Reaction OrthosisDocument22 pagesFloor Reaction Orthosischinmayghaisas50% (2)
- Splinting Techniques: by Madhumitha M, Aruna G, Abi P, Sakthivelayudham G, Sujidha R, Srivignesh MDocument99 pagesSplinting Techniques: by Madhumitha M, Aruna G, Abi P, Sakthivelayudham G, Sujidha R, Srivignesh MSakthivelayudhamganesanNo ratings yet
- Anatomy and Physiology-A ReviewDocument38 pagesAnatomy and Physiology-A Reviewjava_biscocho1229100% (4)
- Motor Neuron Disease GuideDocument5 pagesMotor Neuron Disease Guidekath-kathNo ratings yet
- 22 Assistive Devices (FINAL)Document9 pages22 Assistive Devices (FINAL)kath-kathNo ratings yet
- Kinesiology of the Shoulder ComplexDocument30 pagesKinesiology of the Shoulder Complexkath-kath100% (1)
- Lower Extremity Anatomy ReviewDocument32 pagesLower Extremity Anatomy Reviewkath-kath100% (1)
- 15 Head Neck Back Spine TMJ (Special Tests) (FINAL)Document8 pages15 Head Neck Back Spine TMJ (Special Tests) (FINAL)kath-kathNo ratings yet
- 9 Digestive System (FINAL)Document6 pages9 Digestive System (FINAL)kath-kathNo ratings yet
- 4 Blood Physiology (FINAL)Document8 pages4 Blood Physiology (FINAL)kath-kathNo ratings yet
- 8 Integumentary System (FINAL)Document11 pages8 Integumentary System (FINAL)kath-kathNo ratings yet
- 2 Pulmonary System (FINAL)Document17 pages2 Pulmonary System (FINAL)kath-kathNo ratings yet
- Peripheral Vascular System Functions and DiseasesDocument4 pagesPeripheral Vascular System Functions and Diseaseskath-kathNo ratings yet
- TR Rolling Contact Fatigue Comprehensive Review FinalDocument132 pagesTR Rolling Contact Fatigue Comprehensive Review FinalHenkNo ratings yet
- Brain Death Testing Protocol (Rev220605) PDFDocument2 pagesBrain Death Testing Protocol (Rev220605) PDFRei Irinco100% (1)
- Motor Vehicle Insurance: Class NotesDocument3 pagesMotor Vehicle Insurance: Class Notesgoyal_divya18No ratings yet
- Complications During Intrahospital Transport of Critically Ill Patients: Focus On Risk Identification and PreventionDocument9 pagesComplications During Intrahospital Transport of Critically Ill Patients: Focus On Risk Identification and PreventionYuanita M.No ratings yet
- Splinting The FingersDocument17 pagesSplinting The FingersValentinaRestrepoNo ratings yet
- Importance of Physiotherapy in HaemophiliaDocument48 pagesImportance of Physiotherapy in HaemophiliaPhysioVolunteers100% (3)
- Arthritis: by DR Samra Tahseen Registrar, Radiology LNHDocument86 pagesArthritis: by DR Samra Tahseen Registrar, Radiology LNHAngelic khanNo ratings yet
- Massage Intake FormDocument2 pagesMassage Intake Formapi-253959832No ratings yet
- Chap 16Document125 pagesChap 16BaneeIshaqueK100% (1)
- Human Anatomy. The Human Muscles.Document70 pagesHuman Anatomy. The Human Muscles.Stefania Ungureanu100% (1)
- Knee ExaminationDocument5 pagesKnee ExaminationQandeelNo ratings yet
- Abrasion and Laceration Wound CareDocument5 pagesAbrasion and Laceration Wound CareEtriNo ratings yet
- Chcdis002 - 345Document3 pagesChcdis002 - 345priyashvi kNo ratings yet
- A Chance To Life by MeotjinDocument574 pagesA Chance To Life by MeotjinNiel A.100% (1)
- Lower Limb Orthosis: Dr. Sumit Raghav, PT Assistant Professor Jyotirao Subharti College of PhysiotherapyDocument56 pagesLower Limb Orthosis: Dr. Sumit Raghav, PT Assistant Professor Jyotirao Subharti College of PhysiotherapyKavya Mittal100% (2)
- Reviewer in Mapeh 9Document5 pagesReviewer in Mapeh 9Jaydee DecastroNo ratings yet
- Itachi's Future Wife - Stopping SuccessDocument142 pagesItachi's Future Wife - Stopping Successeileenmaree100% (1)
- Kno Sys 9865Document57 pagesKno Sys 9865Tatiana BorisenkoNo ratings yet
- Chapter 9 Kitchen Safety and Sanitation: 9.1 Hand WashingDocument9 pagesChapter 9 Kitchen Safety and Sanitation: 9.1 Hand WashingCaleb HeNo ratings yet
- Spleen MCQDocument22 pagesSpleen MCQShriyansh Chahar0% (1)
- Nursing Care Plan for Patient with Impaired Physical MobilityDocument4 pagesNursing Care Plan for Patient with Impaired Physical Mobilityssairej06100% (3)
- Heinemann English Wordbuilder-Posture & MovementDocument3 pagesHeinemann English Wordbuilder-Posture & MovementKarolinaNo ratings yet
- 1.) Senit Vs PeopleDocument2 pages1.) Senit Vs PeopleAreeya ManalastasNo ratings yet
- CST GX Promo BookDocument8 pagesCST GX Promo BookaikiguyNo ratings yet
- Soal OrthopediDocument3 pagesSoal OrthopediPoppy GhufraniNo ratings yet
- Hazard Profile-Rebar ActivityDocument12 pagesHazard Profile-Rebar ActivityRoshin99No ratings yet
- Ergonomics at Work: Reference PosturesDocument2 pagesErgonomics at Work: Reference PosturesJohn WNo ratings yet
- (Gallagher Girls 5.5 - Heist Society 2.5) Carter, Ally - Double CrossedDocument104 pages(Gallagher Girls 5.5 - Heist Society 2.5) Carter, Ally - Double CrossedMARÍA PAZ MONTERONo ratings yet
- Mandibulasr Truma ManagementDocument18 pagesMandibulasr Truma Managementjoal510No ratings yet
- Tensegrity CompendiumDocument13 pagesTensegrity Compendiumannoyingspore100% (1)