Professional Documents
Culture Documents
24 Neuroconditions (FINAL)
Uploaded by
kath-kathOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
24 Neuroconditions (FINAL)
Uploaded by
kath-kathCopyright:
Available Formats
Neurological Conditions
Motor Systems
Pyramidal System
CST/CBT
Extrapyramidal System
All the other subcortical parts of brain that influence motor activity
BG (Lenticulostriate), Diencephalon, MB
Basal Ganglia
Corpus Striatum – motor system
Amygdala – limbic system
Claustrum – unknown
Corpus Striatum
Corpus Striatum
Caudate Nucleus Lentiform N
Striatum -> Putamen Globus Pallidus
Recurrent
Direct Pathway vs Indirect Pathway
Direct Pathway
→ → →
At rest: 𝐺𝑃𝐼 + 𝑆𝑁𝑝𝑟 𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠 𝑇ℎ𝑎𝑙𝑎𝑚𝑢𝑠
𝑑𝑜𝑒𝑠 𝑛𝑜𝑡 𝑠𝑡𝑖𝑚𝑢𝑙𝑎𝑡𝑒
𝐶𝑜𝑟𝑡𝑒𝑥
𝑐𝑎𝑢𝑠𝑒𝑠
𝑛𝑜 𝑚𝑜𝑣𝑒𝑚𝑒𝑛𝑡
→ →
During movement: 𝐺𝑃𝐼 + 𝑆𝑁𝑝𝑟 𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠 𝑇ℎ𝑎𝑙𝑎𝑚𝑢𝑠
𝑑𝑜𝑒𝑠 𝑛𝑜𝑡 𝑠𝑡𝑖𝑚𝑢𝑙𝑎𝑡𝑒
→ → → → →
𝐶𝑜𝑟𝑡𝑒𝑥 𝑆𝑁𝑃𝑐 𝐷𝑜𝑝𝑎𝑚𝑖𝑛𝑒 𝑆𝑡𝑟𝑖𝑎𝑡𝑢𝑚 𝐺𝑃𝐼 + 𝑆𝑁𝑝𝑟
𝑔𝑜𝑒𝑠 𝑡𝑜 𝑟𝑒𝑙𝑒𝑎𝑠𝑒𝑠 𝑠𝑡𝑖𝑚𝑢𝑙𝑎𝑡𝑒𝑠 𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠 𝑓𝑟𝑒𝑒𝑠
→ →
𝑇ℎ𝑎𝑙𝑎𝑚𝑢𝑠 𝐶𝑜𝑟𝑡𝑒𝑥 𝑚𝑜𝑣𝑒𝑚𝑒𝑛𝑡
𝑠𝑡𝑖𝑚𝑢𝑙𝑎𝑡𝑒 𝑐𝑎𝑢𝑠𝑒𝑠
Indirect Pathway
At rest: GPe ≠ subthalamus ≠ GPI ≠ Thalamus ≠ Cortex -> no mvmt of antagonist
→ → → →
During Movement: GPe 𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠 subthalamus
𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠
GPI
𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠
Thalamus
𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠
Cortex
→ → → → →
𝐶𝑜𝑟𝑡𝑒𝑥 𝑆𝑁𝑃𝑐 𝐷𝑜𝑝𝑎𝑚𝑖𝑛𝑒 𝑆𝑡𝑟𝑖𝑎𝑡𝑢𝑚 𝐺𝑃𝐸
𝑔𝑜𝑒𝑠 𝑡𝑜 𝑟𝑒𝑙𝑒𝑎𝑠𝑒𝑠 𝑠𝑡𝑖𝑚𝑢𝑙𝑎𝑡𝑒𝑠 𝑖𝑛ℎ𝑖𝑏𝑖𝑡𝑠 𝑓𝑟𝑒𝑒𝑠
→ → → →
𝑆𝑢𝑏𝑡ℎ𝑎𝑙𝑎𝑚𝑢𝑠 𝐺𝑃𝐼 𝑇ℎ𝑎𝑙𝑎𝑚𝑢𝑠 𝐶𝑜𝑟𝑡𝑒𝑥 𝑚𝑜𝑣𝑒𝑚𝑒𝑛𝑡
𝑠𝑡𝑖𝑚𝑢𝑙𝑎𝑡𝑒 𝑐𝑎𝑢𝑠𝑒𝑠 𝑠𝑡𝑖𝑚𝑢𝑙𝑎𝑡𝑒 𝑐𝑎𝑢𝑠𝑒𝑠
Neurotransmitter
In the Brain
o Inhibit: GABA
o Excitatory: Glutamate
Basal Ganglia
o Inhibit: DA
o Stimulate: Ach
o Primary Efferent Nucleus: GPI, SNPr
o Primary Afferent Nucleus: Striatum, Subthalamus
Parkinsonism (Hypokinetic)
A group of disorder with primary disturbances in the dopamine system of Basal Ganglia
o Primary PD – idiopathic – MC type of PD
o Secondary PD – with known etiology – LC type of PD
o Parkinson’s Plus – mimic PD
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
Primary PD
Idiopathic, Genetic
Gene: PINK1, PARK1, LRRK2
Paralysis Agitans, Shaking Palsy
Slowly progressive disorder of CNS with motor and non-motor symptoms
Progressive loss of dopaminergic cells that produces DA in the Substansia Nigra
Maybe 2° to hyperactivity of cholinergic cells in the striatum
MRI
o (+) Paleness
o (+) Lewy Bodies
Nonmotor > Motor Symptoms
o 30-60% of the Substansia Nigra should be damaged before seeing motor sx (Sullivan)
Dx Tool
o Apomorphine Test
If the px reacts = (+) PD
o 2 out of 4 cardinal signs
Epidemiology
o M>F
o 40-60 y/o
o Young Onset: 21-40 y/o
o Juvenile Onset: <21 y/o
Secondary PD (Etiology)
1. Post-infectious
a. Encephalitis Lethargica
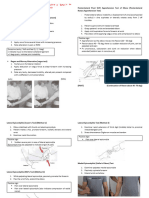
2. Post Traumatic PD:
a. 2° repetitive Microtrauma to brain
b. Common in boxers
c. Dementia Pugilistica aka Punch-Drunk Syndrome
3. Toxic PD
a. MC – Manganese
b. Pesticides
c. Cyanide
d. Carbon Disulfide
e. Ethanol
f. 1 Methyl-4Phenyl-1236-Tetrahydropyridine (MPTP)
4. Metabolic PD
a. Wilson’s Disease aka Hepatolenticular Degeneration
i. Buildup of Copper in the Brain
ii. Excess copper goes to
1. Eye: Kayser Fleischer Ring
2. BG: Lentiform Nucleus
3. Liver: becomes Large & Firm
5. Drug Induced PD
a. 2° Neuroleptic Drugs, Anti-depressant Drugs, Anti-HTN Drugs
Cardinal Signs
Tremor
Rigidity
Akinesia/Bradykinesia
Postural Instability – Advanced Stage
Tremor – Resting
o MC Symptom
o MC presenting Symptom
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
Signs
Hand – Mc pill-rolling tremor
o 3-5 Hz, 4-6 Hz, 4-7 Hz
FA – Pron-Sup
Jaw & Tongue
Postural Tremor
Legs
Action Tremor
Rigidity
Velocity independent resistance to passive movement
Proximal to distal
Leadpipe Cogwheel
Sustained resistance to passive jerky-ratchet like resistance
Uniform throughout 2° superimposed tremor
aka Plastic Rigidity aka Intermittent Rigidity
Manifestations
Akinesia – delayed initiation
Bradykinesia – slowness of movement (most disabling)
Hypokinesia – decrease in amplitude of movement
Hypomimia – Masked face
Bradyphrenia – slowness of thought
Micrographia – small handwriting
Postural Instability
o Last symptom to occur
o ↑ risk of fall
o Indicative of advanced stage PD
(+) Simian Posture
o Stopped forward
o Forward head – shadow pillow posture
o Protracted Sh
o Sh ADDIR
o Elbow Flexion
o Hip Flexion
o Knee Flexion
Striatal Hand
o FA Pro
o Wrist & MCP Flexion
o IP Extension
Striatal Foot
o DF
o Inv
o Big Toe Ext
Gait Difficulty
Shuffling Gait
o ↓ BOS
o ↓ Step & stride Length
o ↓ Velocity
Other Gait Patterns
Festination – small steps with ↑ speed
o Advanced Stage
o Displaced COG
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
Freezing of Gait
o Off State Phenomenon
Fear of Falling
o Cautious Gait
Others
Pain – MC Source of Limb rigidity
Postural Stress Syndrome
Restless Leg Syndrome
CN Affectation “1973”
o 3 – Gaze Palsy
o 7 – Facial Palsy
o 9 – (-) Gag Reflex
o 1 – Anosmia
Dysphagia
Sialorrhea – Drooling
Speech Problem
o Hypokinetic Dysarthria
Depression
Sleep Disorder
o Insomnia
o Excessive Daytime Sleeping
o REM – sleep behavior Disorder
Autonomic Dysfunction
o Erectile Dysfunction
o Constipation
o Urinary Incontinence (Nocturia)
o Excessive Sweating
o Seborrhea
o Orthostatic Hypotension
Prognosis
Positive
T remor
R igidity
F amily History
Negative
o Bradykinesia
o Akinesia
o Gait Difficulty
o Cognitive Impairment
o Postural Instability
o Late Age Onset
Modified Hoehn Yahr Scale
0 – No Disability
1 – Unilateral D/A
1.5 – Unilateral (+) Axial
2 – Bilateral without balance problem
2.5 – bilateral with recovery on pull test
3 – Bilateral with balance problem, unsteadiness, impaired righting reflex, px can live independently
4 – all s/sx are (+) and severe, standing and walking only possible with assistance, px is physical dependent
5 – confined to bed or w/c
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
Pharma
1. Dopamine Replacement
a. 1 hour before or after meal
b. Low Protein diet
c. Levodopa taken 1 hour after 1st dose
d. Levodopa + Carbidopa
i. Sinemet – Gold Standard
e. Tx for Bradykinesia & rigidity
f. Honeymoon Period: 7-8 years (time when DA is most effective)
g. Wearing Off State: meds not affective anymore
i. Adverse Effects
1. Visual Hallucination – MC
2. Peak Dose Dyskinesia
a. Face – Grimace
b. Limb - Choreoathetosis
3. Dystonia – end dose
a. MC – foot (clawing of toes)
4. End Dose Deterioration
5. On-Off Phenomenon
6. Akathisia – restlessness
7. Nocturia
8. Nausea
9. Dryness of Mouth
10. Mood/Personality/Sleep Disorder
11. Orthostatic Hypotension
2. Dopamine Agonist
a. ↑ the sensitivity of Dopamine Receptors
b. Examples
i. Bromocriptine
ii. Pramipexole
iii. Pergolide
iv. Ropinirole
v. Cabergolide
vi. Amantadine
vii. Apomorphine
3. Anticholinergic
a. Tx for tremor
b. eg. Trihexyphenidyl
4. MAO-Inhibitors
a. Mono Amine Oxidase
b. Eg. Rasagiline, Selegiline
Parkinson’s Plus Syndrome
1. Progressive Supranuclear Palsy
a. Gait Difficulty
b. Supranuclear Palsy
c. Difficulty in downward gaze – leads to Ophthalmoplegia
d. Onset – 5th decade of life
2. Corticobasal Ganglionic Degeneration
a. Asymmetric Akinetic Rigid Syndrome
b. Apraxia
c. Alien Hand Syndrome
3. Multisystem Atrophy
a. BG system – striatonigral degeneration
b. Autonomic System – Shy dragger syndrome
c. Cerebellar System – Olivopontocerebellar Atrophy
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
4. PD with Early Dementia
a. Alzheimer’s Disease
b. Diffuse – Cortico Lewy Bodies
c. Guamanian ALS
Hyperkinetic Movement Disorders
A. Athetosis
a. Globus Pallidus
b. Heubner
c. C/L
d. Proximal > Distal
e. Slow & Fluid
f. Slow writhing
g. Worm-like/snake-like
h. Inability to stop distal limb
B. Ballismus
a. Subthalamus
b. PCA
c. C/L
d. Proximal > Distal
i. Uni – Hemiballismus
ii. Bilat – Biballimus
e. Large amplitude
f. Wild/Violent
g. Wild Flinging
C. Chorea
a. Neostriatum
b. Lenticulostriate
c. C/L
d. Distal > Proximal
e. Brief, rapid, jerky, forceful, purposeless movement of distal limb
D. Dystonia
a. Putamen
b. Lenticulostriate
c. C/L
d. Abnormal repetitive twisting and torsional contraction of group of muscles that leads to abnormal
posture
e. Examples
i. Cervical Dystonia – MC
ii. Blepharospasm – sustained eye closure
iii. Oromandibular Dystonia – oral & facial muscle
iv. Meige Syndrome – combination of cervical + oromandibular dystonia
v. Writer’s Cramp Dystonia – task specific dystonia, common in writers, painful & tight forearm
muscle
Neostriatum
C horea
P utamen
D ystonia
G lobus Pallidus
A thetosis
S ubthalamus
H emiballismus
E. Tics
a. Repetitive Stereotypic Intermittent movement seen in head neck & trunk
b. Px is aware
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
F. Gilles Dela Tourette’s Syndrome
a. MC cause of inherited tics
b. M > F
c. < 21 y/o
d. OCD
e. Complex Tics
i. Vocal + Motor Tics
ii. Vocal – Profanity – Coprolalia
iii. Motor Tics – Ballistic – Copropraxia
f. > 1 year
G. Tardive Dyskinesia
a. 2° Long term use of drugs
i. eg. Peak dose dyskinesia
H. Stereotypy Methamphetamine
a. Head Nodding
b. Head Banging
c. Body Rocking
d. Purposeless, uniform, repetitive, voluntary movement of whole body area
I. Myoclonus
a. Brief, Sudden irregular, asynchronous, contraction of group of muscle
J. Myotonia
a. Delayed relaxation of muscle after contraction
K. Myokinia
a. Contraction of muscle fiber under skin with rippling like appearance
Multiple Sclerosis
General Information
Demyelinating Disease of CNS
Autoimmune Disease
o Segmental Demyelination
o Inflammation
o Gliosis
Charcot’s Triad – cardinal sign of MS
I ntention Tremor
N ystagmus
S canning Speech
Etiology: Idiopathic
Risk Factors
o F>M
o 20-40 y/o
o Geographical – Temperate
o Hereditary
o Smoking
o ↓ Vitamin D Level
o ↑ intake of dairy products
Medications
Immunomodulatory – Interferon B
B etaseron
E xtavia
A vonex
R ebif
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
Acute MS – Corticosteroids
Hallmark: plaques formation
P eriventricular White Matter
O ptic Nerve
B rainstem
C ortex
C erebellum
C ST
C ervical Spinal Cord (Posterior White Column) | (+) Lhermittes
4 Distinct Patterns
Type 1: cell mediated destruction of myelin sheath by T Cells
Type 2 (MC): cell mediated destruction of myelin sheath by T Cells & immunoglobulins
Type 3: Apoptosis of Oligodendrocytes
Type 4 (LC): Primary Degeneration of Oligodendrocytes
Clinical Types (Box 16.1 O’Sullivan)
Type I: Relapsing Remitting/Exacerbating-Remitting MS
o 85%/65%
o MC
o MS will last hours to days
o Periods between can last from months to years to decades
o Relapsing Remitting with complete remission
o Relapsing Remitting with incomplete remission (MC)
o Onset: sensory – paresthesia, optic neuritis
Type II: Secondary Progressive MS
o 1st Relapsing Remitting becomes Progressive
o Only 20% of relapsing remitting becomes progressive (2nd MC)
Type III: Primary Progressive
o 10%
o M>F
o Older Onset
o Motor Onset:
o In MRI: fewer lesions
Type IV: Progressive-Relapsing MS
o 5%
o Least Common
o Progressive Disease in the beginning but begins to have attacks later in the course
Benign vs Malignant MS
Benign Malignant/Marburg Disease
15 years of Stability rapid onset almost continual progressive disease that leads to significant disability or death
within short period of time
Kurtzke Expanded
Disability Scale = <3
7 Functional System
V isual System
P yramidal System
S ensory System
C erebellum
B rainstem
B owel/Bladder/Sexual
Mental
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
Visual System
o Optic Neuritis: inflammation of optic nerve with icepick like sensation behind eye and blurring or graying
of vision that leads to eye blindness.
o Visual Scotoma: presence of dark spots in the visual field
o Nystagmus
o Ophthalmoplegia
Pyramidal System
o UMNL
o Fatigue – most common, most disabling, most troubling, more pronounced in the afternoon
o Uthoff’s Phenomenon: anything that may increase body temperature will lead to pseudo-exacerbation
of symptom
Criteria
Reversible
<24 hrs
Sensory System
o Paresthesia: MC presenting symptom
o Pain: electric shock-like, burning
o Face Paroxysmal Pain Syndrome
Trigeminal Neuralgia
Tic Doloreux
o Limb
Paroxysmal limb pain
MC
LE > UE
Dysesthesia Limb
o Trunk
Painful band sensation around trunk
“MS Hug”
o Headache
MC Pain complaint
o Hyperpathia
Hypersensitivity to light stimulus
Cerebellum
o Ataxias: uncoordinated movement
Dysmetria
Dyssynergia
Dysdiadochokinesia
o Gait Ataxia – “Drunkenness”
o Intention Tremor
Brainstem
o CN 2, 5, 7, 8
o Speech Problem – “Controlling the Volume”
Bowel/Bladder/Sexual
o MC Bowel – Constipation
o MC Bladder – Detrusor Hyperreflexia
o Sexual
Female Male
Loss of Libido Loss of Libido
↓ Sensation ↓ sensation
Dryness of Vagina Difficulty ejaculation
Difficulty Reaching Orgasm Impotence
Mental
o Dementia
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
o Attention Deficit
o Memory Loss
Prognosis
Positive Negative
Female Male
<40, <35 <40, <35
Sensory Onset Motor Onset
One Symptom @ Onset Polysymptomatic
Relapsing Remitting Progressive
McDonald’s Criteria
Attacks Lesion
Attacks 2 2
1 2
Probable
2 1
Possible 1 1
Kurtzke Expanded Disability Scale
0 Normal
1 1 functional system
No disability, minimal signs in
1.5 2 functional system
2 1 functional system
Minimal Disability in
2.5 2 functional system
3 1 functional system
Moderate Disability in
3.5 2 functional system
4 500m
4.5 Fully Ambulatory without rest without 300m
5 assist 200m
5.5 100m
6 Intermittent Unilateral Assistance 100m
6.5 Constant Bilateral Assistance 20m
7 unable to walk beyond 5 meters
7.5 cannot take few more steps
8 can be out of bed much of the day
Bedbound
8.5 in bed much of the day
9 can eat, talk, swallow
Bedridden
9.5 cannot eat, talk, swallow
10 Death
TBI
Alteration of brain function 2° external force
Causes of TBI
Falls > MVA > Assaults > Others
o MVA – SCI
o The most common cause of Severe TBI – MVA
Types of TBI
Open Head – penetrating
Close Head – non-penetrating, MC
Pathophysiology
Primary Brain Injury
Diffuse Axonal Injury - 2° high velocity forces (acceleration-Deceleration-Angular Force)
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
o Distinguishing feature of TBI
o Responsible for initial LOC & Coma
o Common Sites: Corpus Callosum, Parasagittal white matter, Pons, Midbrain
Concussion
o Mild TBI
o Mild DAI
o 2° shaking of brain
o Alteration of Consciousness
Coma
If (-) Sleep/wake cycle
(-) arousal system
Requires (+) Ventilatory support
Can take from days to decades to wake up
GCS Score 3-8
Vegetative State
(+) sleep/wake cycle
(-) Awareness
(-) Ventilatory Support
(+) reflex smile/cry
Persistent Vegetative State: > 30 days/1 year (poor prognosis)
Minimally Conscious State
(+) minimal evidence of self & environmental awareness
Obtunded State
Often Sleeps
↓ interest
Delayed Reaction time
Stupor
Unresponsive state, but can be aroused briefly via vigorous repetitive sensory stimulus
Contusions
o Cortical bruises
o 2° low velocity forces
Coup – at the site of impact
Countercoup Injury – opposite site of impact
o Sites
Frontal (Inferior) – Behavioral
Temporal (Anterior) – Memory
o Behavioral Changes
Agitated – Excited
Aggressive – Violent
Apathy - ↓ Interest
Irritable – Moody
Impulsive – Quick
o Post Traumatic Amnesia
Length of time from the injury until the time in which px remembers ongoing events
Measured by
o Galveston Orientation & Amnesia Test (GOAT)
100 Questions
o Orientation Log Test
Secondary Brain Injury
1. ↑ ICP
a. Normal
i. 5-10 mmHg
ii. 4-15 mmHg
iii. <20 mmHg
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
b. >20 mmHg
i. (+) Nausea
ii. (+) Vomiting
iii. (+) Papilledema
iv. CN 2 Affectation
c. Medications
i. Diuretics
ii. Mannitol
d. Interventions
i. Elevate the head up to 30° from supine
2. Normal Pressure Hydrocephalus
a. Adult – Communication
b. ICP Flow “CLMTSFLMSA”
Ventriculomegaly
↓
Normal P°
↓
Triad
I ncontinence (Urinary)
G ait Ataxia
D ementia
3. Herniation
Uncal Central Tonsilar
C erebral Peduncle Paresis Midbrain-Pons: decerebrate Medulla Oblongata: alteration of
R AS Coma rigidity PR, RR, HR
O culomotor N. Gaze Palsy RAS – Coma Cerebellar Tonsils: neck pain
P CA Hemianopsia RAS – Coma
CN – 3, 7, 12
MC Involved Nerve in TBI – CN3
Scales
A. Modified Ashworth Scale
0 No ↑ in muscle tone
1 Catch followed release
1+ Catch followed min resistance / resistance is less than half of remaining ROM
2 More marked ↑ in muscle tone but the joint is easily moved
3 considerable ↑ muscle tone and passive movement is difficult
4 Affected parts is rigid flexion or extension
B. Tardieu Scale
0 no resistance through the passive movement
1 slight resistance without clear catch
2 slight resistance with clear catch
3 fatigable Clonus - <10sec
4 Non-fatigue Clonus – > 10sec
C. Classification of Severity of TBI
Mild Moderate Severe
L OC 0-30 minutes 30 min to 1 day > 1 day
P TA 0-1 day 1-7 day > 7 day
G CS 13-15 9-12 3-8
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
D. Glasgow Coma Scale (Gold Standard)
A. It has the highest reliability
Eyes
4 Spontaneous
3 to speech (command, request, directed to)
2 to pain (sternal rub, triceps/anterior FA pinch)
1 Closed
Motor
6 Follows Command
5 localized pain (pull therapist hand)
4 Withdraws to pain
3 Flexes to pain
2 Extends to pain
1 No response
Verbal
5 Oriented
4 Disoriented/confused
3 Inappropriate
2 Incomprehensible (moaning)
1 Silent
E. Glasgow Liège Scale
1 (+) Oculocardiac reflex Pressure in eye = bradycardia
2 (+) horizontal Oculocephalic Doll’s Eye Phenomenon
3 (+) Pupillary light reflex Accommodation Board Exam
4 (+) Vertical Oculocephalic Doll’s Eye Phenomenon
5 (+) Fronto Orbicular Reflex Glabellar Tap
F. Glasgow Outcome Scale – Extended
8 Upper completely
Good Recovery
7 Lower Return to previous lifestyle with some problems
6 Upper with modification
Moderate Disability
5 Lower Independence in ADLS but will not return to previous lifestyle
4 Upper Assistance 8hrs/day
Severe Disability
3 Lower Assistance 24hrs/day
2 Vegetative State
1 Dead
Gold Rank Intensive Review Baguio Batch 2017
Neuroconditions
G. Ranchos-Los Amigos
I No response Px is in deep sleep
Responses maybe physiologic body changes
Responses are limited & same
II Generalized Response
responses are not related to stimulus
stereotypic response
Responses are now related to stimulus
III Localized Response
May follow simple commands inconsistently
Px has bizarre behavior
IV Confused-Agitated Px is in heightened state of activity
Px has no short/long term memory
Confused-Inappropriate Px may follow simple commands fairly consistent
V
Confused Non-Agitated No learning is possible
Px has goal directed behavior
VI Confused-Appropriate Px may follow simple directions consistently
(+) Carryover of relearned tasks
Px has robot-like behavior
VII Automatic-Appropriate Judgement impaired
new learning at ↓ Rate
Environmental Awareness
VIII Purposeful-Appropriate Abstract reasoning
New learning without supervision
IX Purposeful-Appropriate with standby Assistance upon request
X Purposeful-Appropriate Modified Independence
Gold Rank Intensive Review Baguio Batch 2017
You might also like
- 19 Fractures (FINAL)Document7 pages19 Fractures (FINAL)kath-kathNo ratings yet
- 12 Sports Physiology (FINAL)Document6 pages12 Sports Physiology (FINAL)kath-kathNo ratings yet
- 8 Integumentary System (FINAL)Document11 pages8 Integumentary System (FINAL)kath-kathNo ratings yet
- 21 Prosthetics (FINAL)Document7 pages21 Prosthetics (FINAL)kath-kathNo ratings yet
- Initial Evaluation General InformationDocument8 pagesInitial Evaluation General InformationJoanna EdenNo ratings yet
- 26 Motor Neuron Diseases (FINAL)Document5 pages26 Motor Neuron Diseases (FINAL)kath-kathNo ratings yet
- Quiz IVDocument5 pagesQuiz IVErvin T MileNo ratings yet
- Cerebral Palsy Revalida FormatDocument10 pagesCerebral Palsy Revalida FormatChelsea CalanoNo ratings yet
- Group 2 - IeDocument14 pagesGroup 2 - IeGabriel RagasaNo ratings yet
- Elbow Special TestDocument4 pagesElbow Special TestEllaiza Astacaan100% (1)
- 3 Head, Neck, Back, and Spine ModuleDocument55 pages3 Head, Neck, Back, and Spine ModuleCoffee MorningsNo ratings yet
- Special TestsDocument31 pagesSpecial TestsKyle OrtegaNo ratings yet
- CAMP - Cervical Radic - ColladoDocument5 pagesCAMP - Cervical Radic - ColladoSergi Lee OrateNo ratings yet
- Myocardial Infarction MedBack RevisedDocument7 pagesMyocardial Infarction MedBack RevisedSteve ColbertNo ratings yet
- GaitDocument15 pagesGaitआशिष दादाNo ratings yet
- Prometric ReviewerDocument134 pagesPrometric ReviewerWilyam SerilNo ratings yet
- Lab Act 2 SensoryDocument5 pagesLab Act 2 SensoryZgama AbdulrahmanNo ratings yet
- Cardio Pulmonary Master Document Google DocsDocument186 pagesCardio Pulmonary Master Document Google DocsGokulakrishnan KrishnanNo ratings yet
- DystoniaDocument24 pagesDystoniaAyesha NasirNo ratings yet
- Siegelman Online Advantage 1.1Document35 pagesSiegelman Online Advantage 1.1Samantha AgustinNo ratings yet
- Hypothetical IE of Traumatic Brain Injury/TBIDocument10 pagesHypothetical IE of Traumatic Brain Injury/TBIMIKEE MEDRANONo ratings yet
- Special TestsDocument22 pagesSpecial TestsEsterGrefielNo ratings yet
- 7 MSCI ModuleDocument45 pages7 MSCI ModuleCoffee MorningsNo ratings yet
- THRDocument83 pagesTHRDanes PaguioNo ratings yet
- Interpretation: VS Are WNLDocument4 pagesInterpretation: VS Are WNLSteve ColbertNo ratings yet
- 2 Pulmonary System (FINAL)Document17 pages2 Pulmonary System (FINAL)kath-kathNo ratings yet
- REVIEW SONGS LyricsDocument10 pagesREVIEW SONGS LyricsClaNo ratings yet
- Rom MMT Trunk Study Sheet 1Document3 pagesRom MMT Trunk Study Sheet 1api-242889989No ratings yet
- Rehabilitation ProtocolDocument9 pagesRehabilitation ProtocolMukesh YadavNo ratings yet
- SEM1.GAG2 Adhesive CapsulitisDocument6 pagesSEM1.GAG2 Adhesive CapsulitisKatrina Vea CalaroNo ratings yet
- Orthopaedic AnatomyDocument1 pageOrthopaedic Anatomyintan rosliNo ratings yet
- Seminar On Upper Limb FractureDocument166 pagesSeminar On Upper Limb FractureArko dutta100% (1)
- 16 Upper Extremity (FINAL)Document30 pages16 Upper Extremity (FINAL)kath-kath100% (1)
- HEAD NECK BACK SPINE SPECIAL TESTS December 2022Document5 pagesHEAD NECK BACK SPINE SPECIAL TESTS December 2022Ted Lawrence CiscarNo ratings yet
- 17 Lower Extremity (FINAL)Document32 pages17 Lower Extremity (FINAL)kath-kath100% (1)
- College of Physical Therapy Sem2Document10 pagesCollege of Physical Therapy Sem2karen magallanesNo ratings yet
- Rembe EmeraldDocument7 pagesRembe EmeraldNinjaNo ratings yet
- Elbow Complex (Kinesiology)Document2 pagesElbow Complex (Kinesiology)Kimmybee Garcia50% (2)
- Red FlagsDocument2 pagesRed FlagsHeidiNo ratings yet
- Shoulder Peripheral Joint Mobilization No Joint Mobilization Indication Position of Patient Hand Placement Mobilization ForceDocument14 pagesShoulder Peripheral Joint Mobilization No Joint Mobilization Indication Position of Patient Hand Placement Mobilization ForceEdwinNo ratings yet
- Rehabilitation Protocol For Adhesive CapsulitisDocument2 pagesRehabilitation Protocol For Adhesive CapsulitisBartosz ZaczekNo ratings yet
- Special Test MidtermsDocument9 pagesSpecial Test MidtermsKinggy14No ratings yet
- Knee OsteoarthritisDocument7 pagesKnee OsteoarthritisSteve ColbertNo ratings yet
- Apk Mock Boards Practice Questions Set A No AnswerDocument26 pagesApk Mock Boards Practice Questions Set A No AnswerYuvienco DrecoNo ratings yet
- Clinical Examination of The Wrist PDFDocument11 pagesClinical Examination of The Wrist PDFAdosotoNo ratings yet
- Knee Special Test FinallllllDocument19 pagesKnee Special Test FinallllllElijah QuianoNo ratings yet
- .1 Arthritides-P1Document14 pages.1 Arthritides-P1ELIZABETH GRACE AMADORNo ratings yet
- Upper Extremity (Anatomy)Document17 pagesUpper Extremity (Anatomy)Margareth Christine CusoNo ratings yet
- Peripheral Nerve InjuriesDocument207 pagesPeripheral Nerve InjuriesAashka MahetaNo ratings yet
- GMSC Aug1999Document22 pagesGMSC Aug1999Eloisa Cellona100% (1)
- Special Tests For Elbow and ForearmDocument3 pagesSpecial Tests For Elbow and ForearmAllyza PenaNo ratings yet
- Clinical Orthopaedics: August 2011Document15 pagesClinical Orthopaedics: August 2011Tarun Singh SinghNo ratings yet
- 397.001 - Orthopedics) Rotator Cuff TearDocument11 pages397.001 - Orthopedics) Rotator Cuff Tearvkpremiyahoo.comNo ratings yet
- Ue MMTDocument5 pagesUe MMTKali AceñaNo ratings yet
- Cerebral PalsyDocument96 pagesCerebral PalsyRahini PaniNo ratings yet
- CB Medback - Mendez MercadoDocument9 pagesCB Medback - Mendez MercadoSteve ColbertNo ratings yet
- Refresher Course 2021 Mock Boards Name: - Batch NoDocument8 pagesRefresher Course 2021 Mock Boards Name: - Batch NoGabrielNo ratings yet
- PassThePCE - Ca Sample QuizDocument10 pagesPassThePCE - Ca Sample QuizNavpreet Kaur100% (1)
- IE Humeral Neck FractureDocument9 pagesIE Humeral Neck FractureEarll Justin N. DataNo ratings yet
- K17. Movement DisordersDocument5 pagesK17. Movement DisordersDesna Amanda DahliaNo ratings yet
- 26 Motor Neuron Diseases (FINAL)Document5 pages26 Motor Neuron Diseases (FINAL)kath-kathNo ratings yet
- 22 Assistive Devices (FINAL)Document9 pages22 Assistive Devices (FINAL)kath-kathNo ratings yet
- 16 Upper Extremity (FINAL)Document30 pages16 Upper Extremity (FINAL)kath-kath100% (1)
- 15 Head Neck Back Spine TMJ (Special Tests) (FINAL)Document8 pages15 Head Neck Back Spine TMJ (Special Tests) (FINAL)kath-kathNo ratings yet
- 17 Lower Extremity (FINAL)Document32 pages17 Lower Extremity (FINAL)kath-kath100% (1)
- 9 Digestive System (FINAL)Document6 pages9 Digestive System (FINAL)kath-kathNo ratings yet
- 4 Blood Physiology (FINAL)Document8 pages4 Blood Physiology (FINAL)kath-kathNo ratings yet
- 2 Pulmonary System (FINAL)Document17 pages2 Pulmonary System (FINAL)kath-kathNo ratings yet
- 5 Peripheral Vascular System (FINAL)Document4 pages5 Peripheral Vascular System (FINAL)kath-kathNo ratings yet
- Chapter 4 - Water PollutionDocument44 pagesChapter 4 - Water PollutionLuqman NHNo ratings yet
- TechdataDocument16 pagesTechdataapi-480442981No ratings yet
- Basilar Skull Fractures & DAIDocument17 pagesBasilar Skull Fractures & DAIIsabela OlgaNo ratings yet
- Exam Preparatory Manual, Paediatrics, Snehal Patel, 2eDocument2,737 pagesExam Preparatory Manual, Paediatrics, Snehal Patel, 2eklen100% (3)
- Case Management - B.R.Document109 pagesCase Management - B.R.Erika LlorenNo ratings yet
- Raz Lj50 Covidbirthday CLR DsDocument10 pagesRaz Lj50 Covidbirthday CLR DsRocío Bustos SaguaNo ratings yet
- Application To IndiaDocument7 pagesApplication To IndiaEdu OutsetNo ratings yet
- Epidemiology: Dr. Rajalekshmy.P.R Dept of Swasthavritta Avc, CbeDocument12 pagesEpidemiology: Dr. Rajalekshmy.P.R Dept of Swasthavritta Avc, CbeDr. Rajalekshmy P RNo ratings yet
- Damone Yankana Positive LetterDocument1 pageDamone Yankana Positive LetterLillian AwtNo ratings yet
- 1-Upper GI Malignancy (Moodle)Document31 pages1-Upper GI Malignancy (Moodle)Abdulrahman NanakaliNo ratings yet
- NMC High Risk ObjectivesDocument4 pagesNMC High Risk ObjectivesAwudu RuhainatNo ratings yet
- Malicdem v. Asia Bulk Transport Phils - G.R. No. 224753 (Case Digest)Document2 pagesMalicdem v. Asia Bulk Transport Phils - G.R. No. 224753 (Case Digest)Patrick DamasoNo ratings yet
- Unit 4 ReadingDocument4 pagesUnit 4 ReadingElvantNo ratings yet
- Acute Pancreatitis 2023Document25 pagesAcute Pancreatitis 2023raphael chidiebereNo ratings yet
- Largest Dengue Outbreak (2022) in Nepal: Original Article Nepal Med Coll J March 2023 25 (1) : 73-8Document6 pagesLargest Dengue Outbreak (2022) in Nepal: Original Article Nepal Med Coll J March 2023 25 (1) : 73-8hunzala shamirNo ratings yet
- SpeechDocument2 pagesSpeechAryan SinghNo ratings yet
- 01 Disorders and Diseases of The Human Reproductive SystemDocument7 pages01 Disorders and Diseases of The Human Reproductive SystemAlwaysSaugstNo ratings yet
- Movement Disorders - 2022 - Lange - Nomenclature of Genetic Movement Disorders Recommendations of The InternationalDocument38 pagesMovement Disorders - 2022 - Lange - Nomenclature of Genetic Movement Disorders Recommendations of The InternationalAgnes IacobNo ratings yet
- Recognizing, Diagnosing, and Treating Mitochondrial DiseaseDocument57 pagesRecognizing, Diagnosing, and Treating Mitochondrial DiseaseSnezana MihajlovicNo ratings yet
- Hiv Aidsawareness Weebly Com Argumentative Essay HTML PDFDocument2 pagesHiv Aidsawareness Weebly Com Argumentative Essay HTML PDFFritz Abraham SalinoNo ratings yet
- Psychopharma NotesDocument3 pagesPsychopharma Noteszh4hft6pnzNo ratings yet
- Tilembe Mayeso: 1. Concerning The Shoulder JointDocument3 pagesTilembe Mayeso: 1. Concerning The Shoulder JointmachesoNo ratings yet
- Full Download Test Bank For Diseases of The Human Body 6th Edition by Tamparo PDF Full ChapterDocument36 pagesFull Download Test Bank For Diseases of The Human Body 6th Edition by Tamparo PDF Full Chapterreportermaterw8s84n100% (16)
- Case Presentation-Neonatal SepsisDocument36 pagesCase Presentation-Neonatal SepsisDianne DawnNo ratings yet
- Transient Rise in Intact Parathyroid Hormone Concentration After Surgery For Parathyroid AdenomaDocument6 pagesTransient Rise in Intact Parathyroid Hormone Concentration After Surgery For Parathyroid Adenomaimran qaziNo ratings yet
- Human Organ Systems and Bio-Designs - 2: at Myintuition4865Document8 pagesHuman Organ Systems and Bio-Designs - 2: at Myintuition48651NC21IS038 POLATHALA MOUNIKANo ratings yet
- Primary Health CareDocument13 pagesPrimary Health CareJeanNo ratings yet
- Garcia Jomari A. BSN 2h Kawa-NcpDocument6 pagesGarcia Jomari A. BSN 2h Kawa-NcpRaid GarciaNo ratings yet
- Essay Research - Cognitive BiasDocument18 pagesEssay Research - Cognitive BiasMatreyi BhambiNo ratings yet
- Disseminated Intravascular Coagulation (DIC) During Pregnancy - Clinical Findings, Etiology, and Diagnosis - UpToDateDocument23 pagesDisseminated Intravascular Coagulation (DIC) During Pregnancy - Clinical Findings, Etiology, and Diagnosis - UpToDateCristinaCaprosNo ratings yet