Professional Documents
Culture Documents
Sullivan 2015
Uploaded by
Karoline Pascoal Ilidio PeruchiCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Sullivan 2015
Uploaded by
Karoline Pascoal Ilidio PeruchiCopyright:
Available Formats
584923
research-article2015
SCVXXX10.1177/1089253215584923Seminars in Cardiothoracic and Vascular AnesthesiaSullivan et al
Review
Seminars in Cardiothoracic and
Insertion and Management of Temporary
Vascular Anesthesia
1–11
© The Author(s) 2015
Pacemakers Reprints and permissions:
sagepub.com/journalsPermissions.nav
DOI: 10.1177/1089253215584923
scv.sagepub.com
Breandan Lawrence Sullivan1, Karsten Bartels2, and Natalie Hamilton2
Abstract
Temporary pacemakers are used in a variety of critical care settings. These life-saving devices are reviewed in 2 major
categories in this review: first, the insertion and management of epicardial pacemakers after and during cardiac surgery;
and second, the insertion of transvenous temporary pacemakers for the emergent treatment of bradyarrhythmias.
Temporary epicardial pacemakers are used routinely in patients recovering from cardiac surgery. Borrowing from
advances in cardiac resynchronization therapy there are many theoretical and untested benefits to pacing the postoperative
cardiac surgery patient. Temporary transvenous pacing is traditionally an emergency procedure to stabilize patients
suffering from hemodynamically unstable bradyarrhythmia. We review the traditional and expanding use of transvenous
pacemakers inside and outside the operating room.
Keywords
temporary epicardial pacemaker, temporary transvenous pacemaker, cardiothoracic anesthesia, perioperative, critical
care
Introduction surgery to override the intrinsic rate of the patient in an
attempt to increase cardiac output. Additional consider-
Temporary pacemakers in the emergency room, intensive ations driving advance this practice are the following: (a)
care unit (ICU), or in the operating room can provide clini- atrial pacing may decrease the incidence of atrial fibrilla-
cians with the ability to alter the electromechanical conduc- tion,2 (b) inotropic medications increase myocardial oxy-
tance of the heart. In this review article, we will discuss the gen consumption and may increase mortality after cardiac
indications, options for placement, and strategies to manip- surgery,3 and (c) the left ventricle is less compliant after
ulate temporary pacemakers to optimize hemodynamics. cardiopulmonary bypass and cardiac output may be more
dependent on heart rate.4
Epicardial Pacemakers
Indications Heart Block
In the United States, temporary epicardial pacemaker leads The use of an epicardial pacemaker for the treatment of
are often placed prior to weaning from cardiopulmonary transient heart block represents one of its most obvious
bypass. Temporary leads are often placed secondary to the and beneficial indications. While transient heart block
surgeon’s preference. In this context, the majority of pac- requiring pacing usually gets better, some patients will
ing wires are placed for backup emergency pacing capabil- become permanently dependent on pacemakers. After cor-
ity rather than due to a clear assessment of the actual need onary artery bypass grafting (CABG), permanent pacing
for temporary pacing. The vast majorities of pacing wires may be required in up to 4% of patients, while after aortic
are placed for backup emergency pacing capability. In or tricuspid valve replacement up to 24% of patients will
many instances, temporary leads are not used in the peri- require permanent pacing.5
operative postoperative period.
1
University of Colorado Denver, CO, USA
2
Bradyarrhythmias University of Colorado, Aurora, CO, USA
Corresponding Author:
Sinus bradycardia, first degree atrioventricular (AV) block, Breandan Lawrence Sullivan, University of Colorado Denver, Mail Stop
and atrial flutter after cardiac surgery can be treated with B113, 12401 East 17th Avenue, Room 727, Denver, CO 80238, USA.
atrial pacing.1 Some centers use atrial pacing after cardiac Email: breandan.sullivan@ucdenver.edu
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
2 Seminars in Cardiothoracic and Vascular Anesthesia
RA-RV pacing not only decreased mean arterial blood pres-
sure (MAP) and cardiac output (CO), when compared to
sinus rhythm, but also increased left ventricular dyssyn-
chrony and decreased cardiac output when compared to
RA-BiV pacing.11
This finding is indirectly supported by electrophysiologic
studies focused on permanent pacing. For example, Tse and
colleagues compared pacing at the right ventricular outflow
tract to pacing the right ventricular apex in patients with
complete heart block. Here, apically paced patients devel-
oped more myocardial perfusion defects and a worsening in
left ventricular ejection fraction over time.12 Furthermore,
when biventricular leads are placed in heart failure patients
with abnormal conduction systems there is symptomatic
improvement of their heart failure, reverse remodeling of the
left ventricle, and in certain populations even mortality
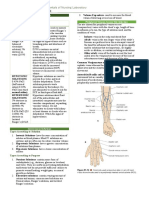
Figure 1. Epicardial lead placement: (A) Atrial lead placed improvement.13 However, it is important to point out that the
at right atrial appendage; (B) Right ventricular lead placed on goals of care in the immediate postoperative period after car-
diaphragmatic surface of right ventricle (not visible); (C) Leads diac surgery represent a very different population as com-
exiting the skin for attachment to external pacing generator. pared to patients presenting electively for placement of a
permanent pacemaker/defibrillator. In a trial examining pro-
phylactic implantation of defibrillators in CABG patients
Supraventricular Tachyarrhythmias with left ventricular dysfunction and evidence of risk factors
The incidence of atrial fibrillation after CABG has ranged for sudden cardiac death, there was no survival improvement
from 15% to 40% and from 37% to 50% after valve sur- 5 years after implantation.14 As the authors of this article
gery and can be as high as 60% in combined valve and point out, solid evidence supported by randomized trials that
CABG surgery.6,7 Diagnosis of atrial fibrillation can some- suggest a survival benefit of a particular perioperative pacing
times be difficult especially postoperatively in patients approach after cardiac surgery is lacking at this time.
with a widened QRS. By using existing epicardial pace-
maker leads, diagnosis of the arrhythmia can be greatly Mimicking the Natural Electrical Vector of the
improved.8 The atrial leads can be hooked up to a standard
electrocardiogram (EKG) machine and a separate atrial
Heart
EKG can be recorded. This can greatly assist in interpreta- Mimicking the natural conduction system of the heart may
tion of complex arrhythmias.9 be beneficial in certain patient populations and tradition-
ally placed epicardial RA-RV pacemaker leads can be
disadvantageous:
Approaches to Insertion (Surgical Placement)
There are theoretical benefits to placing epicardial pace- 1. Post–cardiac surgery septal dyssynchrony.
maker leads in positions that mimic the natural conduction Paradoxical septal motion is defined as movement
pathway in the heart. However, epicardial pacemaker leads of the interventricular septum toward the right ven-
are traditionally placed on the right atrial appendage (atrial tricle with normal myocardial thickening. This
lead) and at the diaphragmatic surface of the right ventricle process can result in decrease myocardial perfor-
(ventricular lead; Figure 1). Both these positions are ante- mance, worsening mitral regurgitation, and may be
riorly located and are chosen to facilitate placement of the misinterpreted as septal ischemia. Paradoxical sep-
wires. Unfortunately, placing the electrodes in these posi- tal motion is also seen in patients with left bundle
tions does not mimic the intrinsic electrical conduction of branch blocks.15 Traditionally, epicardial pace-
the heart and in certain circumstances can have deleterious maker leads are placed on the anterior surface of
effects on mean arterial blood pressure, cardiac output, and the right ventricle. When the right ventricular lead
possibly on coronary blood flow.10 is activated this will cause a left bundle branch
Approaches aimed at mimicking the natural conduction block leading to delayed activation and contraction
system of the heart, via pacemaker lead configuration, may of the left ventricle. Hence, this iatrogenic left bun-
improve postoperative hemodynamics. When right atrial to dle branch block can cause regional wall motion
right ventricular pacing (RA-RV) was compared to right abnormalities and enhance septal dyssynchrony
atrial biventricular (RA-BiV) pacing in post-CABG patients, after cardiac surgery.
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
Sullivan et al 3
2. Low ejection fraction with intrinsic conduction lead to pathologic ventricular remodeling.22
delay. For patients with chronic heart failure with However, CRT itself, when leads are not optimally
prolonged QRS (duration greater than 120 ms), placed, can enhance mechanical dyssynchrony,
cardiac resynchronization therapy (CRT) has sig- that can lead to a decrease in ventricular filling
nificant benefits. The Cardiac Resynchronization- time, increase in mitral regurgitation, and decrease
Heart Failure (CARE-HF) Study showed a 36% overall cardiac performance.23 These consider-
decrease in all-cause mortality in patients with ations beg the question of whether inappropriate
depressed ejection fraction and prolonged QRS pacing after cardiac surgery leads to electrical and
with CRT when compared to optimal medical ther- mechanical disturbances that in consequence could
apy alone.13 This landmark trial led to the European lead to worse outcomes after cardiac surgery?
and North American Guidelines being changed to Future research should address if enhanced CRT
include CRT for all patients with New York Heart techniques could play a role to improve outcomes.
Association class III and IV heart failure with pro-
longed QRS.16 Interestingly, the benefits of CRT Intraoperative Management of Temporary
seem to be highly dependent on location of lead
placement. Pacing the left ventricle in a nonopti-
Pacing
mal site is associated with worse outcomes as it can Prior to committing a patient to postoperative pacing, it is
lead to pathologic remodeling of the heart.17-19 critical to determine what the patient’s underlying rhythm
Whether these findings using permanent pacemak- is. It is important to do this in a safe manner. Weaning from
ers can ever be translated to postoperative cardiac cardiopulmonary bypass, decannulation, hemostasis, and
surgery patients is unclear at this time. Could chest closure can cause electromechanical interference
placement of epicardial leads in patients with low with the epicardial pacemaker leads. The patient’s rhythm
ejection fraction or patients with advanced heart can also be in a state of flux, and it is important for the
failure prevent early hormonally induced patho- anesthesiologists to understand how to safely manage the
logic ventricular remodeling? While results from temporary pacemaker in the operating room and in the
nonoperative patient populations should be consid- ICU. The underlying heart rhythm should be frequently
ered with great caution, studying the effects of reassessed to help determine when the pacemaker is no
perioperative pacing approaches that mimic the longer needed.
natural conduction pathways in at-risk patients
clearly deserves more effort.
Weaning From Cardiopulmonary Bypass
3. Myocardial stunning. After cardiopulmonary
bypass there can be significant myocardial stun- Shortly after the surgeon places the epicardial leads, they
ning. Myocardial stunning is caused by ineffectual should be tested for their functionality, sensitivity, and
cardioplegia, ischemia-reperfusion injury, inade- pacing threshold. The sensitivity of the electrodes is
quate revascularization, or ongoing ischemia. Fluid defined as the ability of the pacemaker to detect myocar-
status optimization, inotropic medications, pacing, dial voltage. If the pacemaker has an extremely high sensi-
and mechanical support are all treatment options tivity, it will not be able to detect any electrical activity in
used to support patients while their myocardial the heart. This potentially dangerous mode is known as the
stunning improves. Inotropic support has been asynchronous mode. The range of the epicardial pacemak-
linked to increased mortality in propensity matched er’s sensitivity is 0.4 mV to 10 mV for the right atrium and
retrospective trials.3,20 Mechanical support is 0.8 mV to 20 mV for the right ventricle. New wires in good
fraught with complications and is usually used as position can detect very low voltages and are able to inter-
an extreme last measure. However, while pacing pret whether to pace or not, whereas poorly placed older
seems like a potentially benign intervention that wires will not be able to sense lower voltages. An easy way
can increase cardiac output, pacing in the setting of to check the patients pacing threshold is to turn the pace-
myocardial stunning, however, may not be a benign maker into a mode where the patient’s heart rate will
intervention. While the duration of pacing required inhibit the actions of the pacemaker (DDD, AAI, VVI).
and the exact mechanism responsible are unclear, While you are watching the sensing indicator on the pace-
chronic pacing is known to cause regional wall maker box decrease the sensitivity of the pacemaker until
motion abnormalities and may even impair coro- the pacemaker will no longer sense the electrical activity
nary blood flow.21 The development of CRT was of the heart. This will reveal the patient’s underlying
based on the theory that pathologic electrical con- rhythm. Next, increase the sensitivity of the pacemaker.
duction (prolonged PR intervals, increase in QRS Eventually a minimum voltage will be reached where the
duration) can induce cellular modifications that pacemaker will sense every P-wave or possibly every
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
4 Seminars in Cardiothoracic and Vascular Anesthesia
attempted first. If the patient has heart block with a slow
ventricular rate then the patient should be AV- or V-paced
for weaning from cardiopulmonary bypass, decannulation,
and hemostasis. Electrocautery will cause electrical inter-
ference with the pacemaker, leading it to inhibit its pacing
action unless it is programed to an asynchronous mode.
Failure to recognize electrical inhibition will lead to the
patient having long pauses when electrocautery is used.
If the patient is dependent on pacing to maintain ade-
quate hemodynamics, then the pacemaker should be turned
to an asynchronous mode. Asynchronous pacing can put
the patient at risk for R on T phenomenon, and therefore
places the patient at risk for torsades de pointes.
The patient with an underlying rhythm should be paced
in the following hierarchy of pacing: no pacing if sinus
rhythm with adequate rate present, atrial pacing, atrial-ven-
tricular pacing, ventricular pacing. When these pacing strat-
egies have been studied in patients after cardiac surgery that
have intact conduction systems, there is significant hemody-
Figure 2. (Left) Cardiotronic pacing generator. (Right) namic perturbations that the patient experiences as they
Medtronic pacing generator. Each has controls to adjust rate, descend down the hierarchy of pacing.11
atrial and ventricular output and sensitivity, mode, and other
fine-tuning features.
Arrival to the Intensive Care Unit
QRS. This minimal voltage is the pacing or sensing thresh- Once the patient arrives in the ICU, a key part of the transition
old of the epicardial wires in that particular position on the of care to the ICU team is communication about the patient’s
heart. The technical manual for the Medtronic 5388 model rhythm and the hemodynamic goals of the immediate postop-
dual-chamber pacemaker, which is the most common tem- erative care. If the patient is hemodynamically stable, the
porary pacemaker used in the United States, recommends underlying rhythm should be investigated. At this point the
setting the sensitivity to 2× the pacing or sensing threshold patient should be switched out of their asynchronous pacing
(Figure 2). This will prevent inadvertently turning the and put in a demand mode. This will greatly decrease the risk
pacemaker into an asynchronous pacemaker. to the patient of having an iatrogenic R on T.
The pacemaker leads need to be tested for their output or To test the underlying rhythm, the patient should be
capture threshold. This is the current at which the pace- placed in a demand-pacing mode and their heart rate should
maker will produce a depolarization. Once the epicardial be slowly turned down. The ICU physician should pay
leads are connected in the surgical field, the patient’s heart close attention to the patient’s hemodynamics while the
rate should be increased higher than the native rate; the tech- patient’s rate is turned down. The pacemaker can be set to a
nical manual recommends 10 beats per minute higher than demand mode once the patient’s underlying rhythm
their intrinsic rate. Start with the current at the maximum emerges. At this time, the ICU physician needs to decide
settings on the pacemaker (20 mA for the atrial lead and 25 what the optimal pacing mode and rate is, given the patient’s
mA for the ventricular leads on the Medtronic 538824) and hemodynamics. The authors of this review strongly dis-
slowly turn down the current until capture is lost. This cur- courage the practice of unplugging the pacemaker wires
rent, where capture is lost, is the stimulation threshold. The from the pacemaker box in a paced patient to investigate
technical manual recommends setting the current at 2 to 3 their underlying rhythm and the practice of turning down
times the stimulation threshold. The pacemaker will default the current rapidly to investigate the patient’s underlying
to a stimulation threshold of 10 mA. On the ventricular lead rhythm. We believe that this practice can put the patient at
an initial stimulation threshold above 5 mA should be fur- risk for an R on T and that this practice may not allow the
ther investigated, while a stimulation threshold of 2 mA on patient’s intrinsic pacemaker to initiate pacing.25
the atrial leads should be further investigated. All the con-
nections should be investigated and the surgeons should Continuous Management of Temporary
make sure that the leads are optimally attached.
Epicardial Pacemaker Wires
The next important step is to determine how the patient
can be successfully and safely paced given the presence or Patients that require temporary epicardial pacing to main-
absence of conduction delays. Atrial pacing should be tain normal hemodynamics should be monitored in the
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
Sullivan et al 5
ICU with continuous telemetry until they have an underly- and use can be compromised by pain and ineffective ven-
ing rhythm that provides them with appropriate hemody- tricular capture. Esophageal electrodes can be placed into
namic stability. The patients that are being paced for the esophagus and/or stomach under light sedation for
reasons besides complete heart block do not necessarily both atrial and ventricular pacing with improved capture
need to be housed in the ICU. These indications include over transcutaneous pacing, but are rarely used today.32
atrial fibrillation prophylaxis and atrial pacing for
improved cardiac output. Patients after cardiac surgery can
Indications
experience multiple temporary rhythm disturbances, with
peak incidences of atrial fibrillation and atrial flutter on The indications for temporary pacing can be generally
postoperative days 2 and 3.26,27 If the patient is dependent qualified as emergent or elective. Management of symp-
on their temporary epicardial wires secondary to complete tomatic bradycardia is well established and should be
heart block this may be a transient phenomenon. Once the managed according to the published standards by the
epicardial leads are no longer needed, they can be removed American Heart Association guidelines for cardiopulmo-
at the bedside. It is highly variable among surgeons and nary resuscitation and emergency cardiovascular care
ICU physicians when the wires are removed. If the leads (Figure 3).33
are needed, then the patient may need to be evaluated by a
cardiologist for placement of a permanent pacemaker. For
practical purposes, it should be kept in mind that the longer
Emergent
the epicardial leads are in place and used the higher the Emergent pacing is most commonly performed for brady-
threshold for capture can become. arrhythmias. The underlying mechanisms are the follow-
ing: (a) primary abnormality of cardiac automaticity and/
or conduction (idiopathic); (b) unintended side effect of
Complications therapeutic levels of cardio-active drugs (beta-blockers,
The presence or use of are the source of rare but serious calcium channel blockers, digitalis); (c) bradycardia
complications: inappropriate sensing leading to an R on T caused by conduction defect secondary to acute myocar-
phenomenon, incomplete removal leading to a retained dial infarction; (d) failure of previously implanted pace-
foreign body, and bleeding leading to tamponade follow- maker device; (e) toxicity or overdose of cardioactive
ing removal.28 In a prospective observational study of drugs; (f) severe electrolyte abnormalities.34 The goal of
patients undergoing CABG, there were 3 patient character- initial management is stabilization by increasing the ven-
istics that predicted the need for temporary postoperative tricular rate using both pharmacological and nonpharma-
pacing: history of arrhythmias, pacing required to come cological interventions, while identifying and treating a
off cardiopulmonary bypass, and diabetes mellitus.29 cause. Prior to transvenous pacing chronotropic medica-
tions like dopamine, epinephrine, isoproterenol, and atro-
pine can be tried (Figure 2). Transcutaneous pacing is an
Temporary Transvenous Pacemakers alternative and can be used in an emergent setting; how-
ever, most patients require sedation to tolerate transcutane-
Introduction ous pacing. These drugs and transcutaneous pacing may
Temporary transvenous pacing (TTvP) has been performed temporize a patient’s condition until transvenous pacing
for 60 years to provide temporary ventricular rate support can be initiated either temporarily or via permanent pace-
and thus cardiac output, in patients suffering from severe maker placed by a qualified consultant. TTvP may be
or clinically significant episodes of bradycardia or high- appropriate as a temporizing measure before permanent
grade heart block and asystole from multiple causes pacemaker placement or as a bridge to resolution of revers-
including acute myocardial infarction. This can be a life- ible causes like drug toxicity or in septic patients who are
saving procedure, and temporary pacemakers have become otherwise contraindicated for PPM placement. There is
more common procedures in emergency departments and evidence that delaying definitive treatment greater than 24
ICUs.30 Advances in temporary pacing have allowed the hours is dangerous, and as soon as a patient can be stabi-
use of transcutaneous, esophageal, epicardial, as well as lized with temporary measures an expert should be con-
percutaneous transvenous (endocardial) electrodes. All sulted for evaluation for a permanent pacemaker35 (see
require an external pulse generator that attaches to the Table 1).36
electrodes, allowing for the adjustment of pacing output,
pacing rate, pacing mode, and sensitivity to intrinsic activity.31 Elective
Transcutaneous pacing uses adhesive electrode pads
applied directly to the chest in anteroposterior or antero- TTvP is generally utilized in the perioperative period dur-
apical configurations. Transvenous pacemaker insertion ing a surgical or other procedural intervention. If a
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
6 Seminars in Cardiothoracic and Vascular Anesthesia
Figure 3. American Heart Association adult bradycardia algorithm.
Table 1. Emergent Indications for Temporary Transvenous procedure is likely to cause hemodynamically significant
Pacing36. bradycardia, temporary pacing has been used to prevent
Bradyarrhythmias not associated with acute myocardial this dangerous situation. For example, TTvP has been used
infarction with success in carotid body tumor excision and manipula-
Symptomatic sinus node dysfunction tion after preoperative embolization of carotid body tumors
Sinus arrest where carotid sinus hypersensitivity has been found.37
Sinus bradycardia Temporary transvenous pacing has also been used for
Mobitz type II 2nd degree AV block more precise deployment of aortic endografts, percutane-
3rd degree AV block ous aortic valve replacement, and balloon valvuloplasty
Tachydysrhythmias requiring overdrive pacing refractory to
using rapid ventricular pacing. Controlled hypotension is
medical therapy
Failure of permanent pacemaker critical to the precise placement of these thoracic aorta
Bradyarrhythmias associated with acute myocardial infarction endografts, particularly, as many aneurysms and dissec-
Symptomatic sinus node dysfunction tions arise near the left subclavian artery. Inappropriately
Mobitz type II 2nd degree AV block positioned grafts may compromise the cerebral circulation
3rd degree AV block or predispose the patient to postdeployment endoleaks.
New right, left, alternating bundle branch block, or Pulsatile aortic blood flow can exert a force moving the
bifascicular block stent distally. Rapid right ventricular pacing at 130 to 200
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
Sullivan et al 7
beats per minute will reduce mean arterial pressure to 40 to
60 mm Hg via loss of AV synchrony and reduction of ven-
tricular filling time, decreasing left ventricular preload,
stroke volume, and cardiac output. Rapid pacing is a safe,
effective, and predictable method of inducing brief con-
trolled hypotension with rapid onset and offset. Pacing is
also titratable to desired systemic blood pressure by merely
adjusting the rate. Brief controlled hypotension can also be
accomplished with pharmacological methods.38 These
require dose titration and are relatively slower in onset and
offset than pacing. In one study, rapid right ventricular
pacing was compared to sodium nitroprusside administra-
tion (3 µg/kg/min) and 0.5 mg/kg adenosine bolus. Rapid
pacing produced the most pronounced (desirable) hypo-
tension, shortest duration, quickest recovery to baseline
blood pressure, shortened overall procedure time, and
more precise positioning without a difference in postpro-
cedural neurologic function.39
Another indication for rapid pacing involves transcuta-
neous aortic valve replacement (TAVR). Transvenous pac-
ing leads are advanced via percutaneous access from the
groin to the right ventricle. Under fluoroscopic guidance a
guidewire is advanced into the left ventricle, and rapid
pacing of 150 to 200 beats per minute is initiated to mini-
mize left ventricular outflow prior to balloon valvuloplasty
of the stenotic aortic valve is performed. The balloon is
removed, and the valve itself is advanced over the guide-
wire and positioned within the native valve annulus (Figure
4). Rapid pacing is again initiated and the valve is expanded
Figure 4. Control room monitor during transcatheter aortic
with TEE and/or fluoroscopic guidance.40 Transapical valve replacement (TAVR) using temporary transvenous rapid
TAVR is performed using a left anterolateral minithora- ventricular pacing. (Top) Initiation of rapid ventricular pacing.
cotomy with a sheath advanced through a ventriculostomy The rate is set to 180 beats/min to decrease systolic flow
made in the left ventricular apex. Femoral venous access is across the aortic valve and establish controlled hypotension for
established in a similar fashion to the transfemoral balloon valvuloplasty and valve deployment. (Bottom) End of
approach for rapid pacing during balloon valvuloplasty rapid pacing with quick recovery of systemic blood pressure.
and valve deployment. In addition, less rapid ventricular
pacing can be used to titrate blood pressure to surgeon this reason, it is recommended by the manufacturer
preference during closure of the ventriculostomy site. (Medtronic, Inc, Minneapolis, MN) to place TTvP elec-
TAVR with the Medtronic CoreValve (Medtronic, Inc, trodes and continue them for at least 24 hours postproce-
Minneapolis, MN) is currently only approved for trans- dure. In the case of high-grade AV block or severe
femoral deployment. The CoreValve differs from the bradycardia, a permanent pacemaker should be implanted
Edwards-Sapien valve in its construction using a self- according to the guidelines of the Heart Rhythm Society.43
expanding Nitinol frame. Rapid ventricular pacing is not
required for deployment, merely titration of systemic
Approaches to TTvP
blood pressure through pacing to a systolic blood pressure
of 100 mm Hg. The frame continues to expand slightly Each major venous access site has advantages and disad-
postimplantation and has a higher incidence (5.7% t o vantages, and the optimal site is controversial. Goals of
50%) of permanent pacemaker implantation than the site selection should consider ease and speed of placement,
Edwards-Sapien valve (4% to 12%).41 In another study, the a high success rate, low incidence of complications, and
CoreValve prosthesis was associated with a 33.3% inci- avoidance of pacemaker lead misdirection, as malposition
dence of postprocedural permanent pacing.42 This is impairs satisfactory capture.44 Sites include internal and
thought to be due to its length, as contact between the self- external jugular, subclavian, brachial, and femoral veins
expanding Nitinol stent and the subaortic conduction path- and is often dictated by the experience and comfort of the
way being unavoidable during valve deployment.41 For individual performing the procedure. Consideration should
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
8 Seminars in Cardiothoracic and Vascular Anesthesia
be given to the anticipated length of time the pacemaker is atrium, through the tricuspid valve to the right ventricular
needed. For example, while femoral access can be per- apex. A properly placed lead should be seen in the ante-
formed with ease, it can be more difficult to advance the rior–inferior aspect of the cardiac shadow, usually slightly
electrodes to the right ventricle, limits patient mobility, has left of the thoracic spine in the routine anterior–posterior
a higher risk of venous thromboembolism, and offers the direction. This may be difficult to distinguish from place-
least stable wire position. Need for PPM should also be ment in the coronary sinus without lateral X-ray, which
considered, as the left and right subclavian veins are most will show a more posterior position, while one in the apex
often used.31 Choice of site should also include the patient’s will point toward the apex a few centimeters behind the
coagulation status during the procedure and the need for sternum.46
anticoagulation afterwards. The most recent review of
access points for temporary pacing from 1973 to 2004
Blind Technique
states that the right internal jugular is the preferred route.
It is likely safest for inexperienced operators, provides the To perform the blind procedure an EKG monitor is attached
most direct route to the right ventricle, and is associated to the patient, and the catheter electrodes are connected
with the lowest rate of loss of ventricular capture.45 One directly to the pacing generator. The electrode is inserted
small study favored right supraclavicular access to the and the generator turned on. If a balloon is present on the
subclavian/innominate vein with a 94.1% first time suc- electrode tip, it can be inflated once through the sheath to
cess rate (100% overall).44 There are no more recent stud- help direct the lead. The generator is set to a rate signifi-
ies comparing access points. cantly greater than the patient’s existing rate, output to
maximal current, and sensitivity to the lowest level. As the
catheter is advanced, pacemaker spikes will be seen on the
Technique EKG monitor, and when the catheter enters the right ven-
Equipment needed to insert TTvP includes an introducer tricle and makes contact with the ventricular wall, a left
sheath, pacing catheter, and external pacing generator. In bundle branch pattern (eg, wide QRS complex) will be
addition, fluoroscopy should be available and the patient seen after every pacemaker spike indicating capture. The
attached to an EKG monitor. Commercial kits are available balloon can then be deflated and the electrode catheter
containing necessary supplies and adapters to attach to the secured in place.36
external pacing generator and the EKG lead. The catheters
are approximately 100 cm in length and come in both flex-
EKG-Guided Technique
ible and rigid varieties with and without a balloon tip. The
external pacing generator delivers electrical current in mil- This technique utilizes the generator’s sensing function to
liamperes (mA), through the pacing catheter. The rate con- monitor the transit of the catheter as it nears the right ven-
trol dial selects the pacing rate. The output control dial tricle by interpreting the different waveforms that appear
regulates the current from 0.1 to 20 mA. This determines the as the catheter advances. The negative electrode of the
ability to capture the heart. The sensitivity control estab- catheter is attached to the V (precordial) lead of the EKG
lishes a threshold required to suppress the pacemaker from monitor, while the rest of the leads are attached to the
firing. Decreasing the sensitivity will lead to asynchronous patient in the usual fashion. The magnitude and polarity of
or fixed rate pacing at the set rate, regardless of the patient’s the waveforms change as the catheter moves through the
own underlying rhythm, and this is uniform among pace- heart. A detailed description with images of the various
makers and has already been discussed above in reference to waveforms is described in Harrigan et al.36 Once the cath-
epicardial pacemaker leads. Increasing the sensitivity and eter is in position at the right ventricular apex, it should be
modifying the rate will lead to demand (synchronous) pac- disconnected from the EKG monitor and attached the pac-
ing, where the pacemaker senses the patient’s underlying ing generator. The settings should be set as with the blind
ventricular rate and will not fire unless the patient’s underly- technique to asynchronous mode, and a left bundle branch
ing rate drops below the rate set on the generator.36 pattern should be seen after every pacer spike on the EKG
monitor, indicating capture. If capture does not occur, the
lead needs to be repositioned.36
Fluoroscopic Technique
The availability of portable fluoroscopy can simplify the Verification of Placement, Function, and
procedure and likely increases the success of increasing
the success of placement. After a venous sheath is placed
Optimization
and secured, multiple methods have been described to Chest radiography should be used to confirm placement in
position the lead appropriately in the right ventricular the right ventricular apex as described above and to rule
apex. The lead is advanced through the vein to the right out pneumothorax if internal jugular or subclavian access
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
Sullivan et al 9
is used. A 12-lead EKG can further verify placement with lead can perforate the atrial or ventricular septum as well
a left bundle branch-like pattern. Pacing (output) and sens- as the ventricular free wall resulting in cardiac tamponade.
ing thresholds should be tested after capture has been dem- The lead can become looped or entrapped, damaging the
onstrated. To determine the pacing threshold (minimum tricuspid apparatus. It can also be misplaced in the atrium
current needed to obtain capture), the rate is set to at least or coronary sinus.
10 beats/min faster than the patient’s native rate, or
between 60 and 80 if there is no underlying rhythm.
Electrical Performance of the Lead
Reduce the output slowly until capture is lost, and repeat
the measurement. Then set the output to 2 to 2.5 times the Failure to capture or sense are common complications
threshold current. Ideal threshold is <1 mA and therefore a occurring in 37% to 43% of cases.36 Pacing thresholds can
pacing output of 2 to 3 mA. Reposition the catheter if the change based on the patient’s underlying pathology as well
threshold is above 5 to 6 mA. The sensing threshold only as drug therapy used.31 If pacing suddenly fails, one should
needs to be tested if the patient has an underlying rhythm check the connections to the generator and the generator
to be sensed, and if the pacemaker will be used in demand batteries. If pacing spikes are seen without capture,
mode. Set the rate to 10 beats/min below the patient’s increase the output and consider repositioning or replace-
intrinsic rate and increase the sensitivity to the highest ment of the lead. The lead could become dislodged or
value. The generator should now indicate a flashing light migrate with or without patient movement and require
for each sensed beat, and not pace. Decrease the sensitivity repositioning or replacement. Undersensing and oversens-
slowly until the pacer captures, and this setting defines the ing may require lead reposition or changes to the sensitiv-
sensing threshold. Lower the sensitivity a bit further to ity of the pulse generator.
adequately sense the underlying rhythm.36
Conclusion
Postprocedural Care Temporary epicardial and temporary transvenous pace-
It is imperative that any patient with TTvP be on continu- makers provide clinicians with valuable diagnostic and
ous telemetry monitoring and cared for by staff familiar therapeutic tools to patients after cardiac surgery and suf-
with pacemaker operation. Daily EKG and chest X-ray fering from bradyarrhythmias. While the exact technique
should be considered. Daily maintenance requires daily and utilization of epicardial pacemaker wires remains a
checks for pacing thresholds, inspection of the skin site for topic of debate and research, their use can be extremely
infection with dressing changes per hospital protocol, beneficial in the postoperative recovery of patients.
integrity of the connections, and status of the external gen- Temporary transvenous pacing can be a life-saving proce-
erator battery. The underlying rhythm should be assessed dure for those with unstable bradyarrhythmias unrespon-
and recorded as well.31 In the absence of contraindications, sive to medical therapy. Future research in positioning and
it seems reasonable to consider anticoagulation with hepa- pacing technique of epicardial pacemakers may improve
rin, at least when the femoral route is used due to its higher patient outcomes who present for high-risk cardiac
rate of deep venous thrombosis.10 surgery.
Declaration of Conflicting Interests
Complications
The author(s) declared no potential conflicts of interest with
The multiple phases of the procedure and the duration the respect to the research, authorship, and/or publication of this
catheter is in place are the major categories for complica- article.
tions. In addition to complications from central venous
access, further complications arise from passing the pace- Funding
maker wire into the heart. Not surprisingly, complication The author(s) received no financial support for the research,
rates are affected by the experience of the physician per- authorship, and/or publication of this article.
forming the procedure. Complication rates vary depending
on author, as each seems to use different definitions, and References
occurs in 10% to 60%.30,45
1. De Belder MA, Malik M, Ward DE, Camm AJ. Pacing
modalities for tachycardia termination. Pacing Clin
Mechanical Effects of the Lead Electrophysiol. 1990;13:231-248.
2. Crystal E, Garfinkle MS, Connolly SS, Ginger TT, Sleik K,
The lead itself can cause other problems separate from the Yusuf SS. Interventions for preventing post-operative atrial
obvious risks of central venous access. Arrhythmias again fibrillation in patients undergoing heart surgery. Cochrane
can occur as the lead passes into the right ventricle. The Database Syst Rev. 2004;(4):CD003611.
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
10 Seminars in Cardiothoracic and Vascular Anesthesia
3. Nielsen DV, Hansen MK, Johnsen SP, Hansen M, Hindsholm therapy (MADIT-CRT) trial. Circulation. 2011;123:
K, Jakobsen CJ. Health outcomes with and without use of ino- 1159-1166.
tropic therapy in cardiac surgery: results of a propensity score- 18. Ypenburg C, van Bommel RJ, Delgado V, et al. Optimal left
matched analysis. Anesthesiology. 2014;120:1098-1108. ventricular lead position predicts reverse remodeling and
4. Wallace A, Lam HW, Nose PS, Bellows W, Mangano DT. survival after cardiac resynchronization therapy. J Am Coll
Changes in systolic and diastolic ventricular function with Cardiol. 2008;52:1402-1409.
cold cardioplegic arrest in man. The Multicenter Study of 19. Becker M, Altiok E, Ocklenburg C, et al. Analysis of LV
Perioperative Ischemia (McSPI) Research Group. J Card lead position in cardiac resynchronization therapy using
Surg. 1994;9(3 suppl):497-502. different imaging modalities. JACC Cardiovasc Imaging.
5. Jaeger FJ, Trohman RG, Brener S, Loop F. Permanent pac- 2010;3:472-481.
ing following repeat cardiac valve surgery. Am J Cardiol. 20. Fellahi JL, Parienti JJ, Hanouz JL, Plaud B, Riou B, Ouattara
1994;74:505-507. A. Perioperative use of dobutamine in cardiac surgery and
6. Maisel WH, Rawn JD, Stevenson WG. Atrial fibrillation adverse cardiac outcome: propensity-adjusted analyses.
after cardiac surgery. Ann Intern Med. 2001;135:1061-1073. Anesthesiology. 2008;108:979-987.
7. Creswell LL, Schuessler RB, Rosenbloom M, Cox JL. 21. Skalidis EI, Kochiadakis GE, Koukouraki SI, et al.
Hazards of postoperative atrial arrhythmias. Ann Thorac Myocardial perfusion in patients with permanent ventricu-
Surg. 1993;56:539-549. lar pacing and normal coronary arteries. J Am Coll Cardiol.
8. McRae ME, Chan A, Imperial-Perez F. Cardiac surgical 2001;37:124-129.
nurses’ use of atrial electrograms to improve diagnosis of 22. Spragg DD, Leclercq C, Loghmani M, et al. Regional altera-
arrhythmia. Am J Crit Care. 2010;19:124-133. tions in protein expression in the dyssynchronous failing
9. Yabek SM, Akl BF, Berman W Jr, Neal JF, Dillon T. Use of heart. Circulation. 2003;108:929-932.
atrial epicardial electrodes to diagnose and treat postopera- 23. Leclercq C, Kass DA. Retiming the failing heart: principles
tive arrhythmias in children. Am J Cardiol. 1980;46:285-289. and current clinical status of cardiac resynchronization. J Am
10. Garcia-Bengochea JB, Fernandez AL, Calvelo DS, Escudero Coll Cardiol. 2002;39:194-201.
JA, Gude F, Juanatey JR. Temporary epicardial left ventric- 24.
Medtronic. Model 5388. Dual chamber temporary
ular and biventricular pacing improves cardiac output after pacemaker(technicalmanual). http://www.clinicalguide-
cardiopulmonary bypass. J Cardiothorac Surg. 2012;7:113. lines.scot.nhs.uk/PICU%20HDU%20guidelines/YOR-
11. Cannesson M, Farhat F, Scarlata M, Cassar E, Lehot JJ. The PICU-026%20Pacing%20Aug%202011.pdf/.
impact of atrio-biventricular pacing on hemodynamics and 25. Chemello D, Subramanian A, Kumaraswamy N. Cardiac
left ventricular dyssynchrony compared with atrio-right ven- arrest caused by undersensing of a temporary epicardial
tricular pacing alone in the postoperative period after cardiac pacemaker. Can J Cardiol. 2010;26:e13-e14.
surgery. J Cardiothorac Vasc Anesth. 2009;23:306-311. 26. Zaman AG, Archbold RA, Helft G, Paul EA, Curzen NP,
12. Tse HF, Yu C, Wong KK, et al. Functional abnormalities Mills PG. Atrial fibrillation after coronary artery bypass sur-
in patients with permanent right ventricular pacing: the gery: a model for preoperative risk stratification. Circulation.
effect of sites of electrical stimulation. J Am Coll Cardiol. 2000;101:1403-1408.
2002;40:1451-1458. 27. Aranki SF, Shaw DP, Adams DH, et al. Predictors of atrial
13. Cleland JG, Daubert JC, Erdmann E, et al. The effect of car- fibrillation after coronary artery surgery. Current trends and
diac resynchronization on morbidity and mortality in heart impact on hospital resources. Circulation. 1996;94:390-397.
failure. N Engl J Med. 2005;352:1539-1549. 28. Gal Th J, Chaet MS, Novitzky D. Laceration of a saphenous
14. Bigger JT Jr. Prophylactic use of implanted cardiac defi- vein graft by an epicardial pacemaker wire. J Cardiovasc
brillators in patients at high risk for ventricular arrhythmias Surg. 1998;39:221-222.
after coronary-artery bypass graft surgery. Coronary Artery 29. Bethea BT, Salazar JD, Grega MA, et al. Determining
Bypass Graft (CABG) Patch Trial Investigators. N Engl J the utility of temporary pacing wires after coronary artery
Med. 1997;337:1569-1575. bypass surgery. Ann Thorac Surg. 2005;79:104-107.
15. Reynolds HR, Tunick PA, Grossi EA, Dilmanian H, Colvin 30. Munoz Bono J, Prieto Palomino MA, Macias Guarasa I, et
SB, Kronzon I. Paradoxical septal motion after cardiac sur- al. Efficacy and safety of non-permanent transvenous pace-
gery: a review of 3,292 cases. Clin Cardiol. 2007;30:621-623. maker implantation in an intensive care unit. Med Intensiva.
16. Dickstein K, Vardas PE, Auricchio A, et al. 2010 Focused 2011;35:410-416.
update of ESC Guidelines on device therapy in heart fail- 31.
Gammage MD. Temporary cardiac pacing. Heart.
ure: an update of the 2008 ESC Guidelines for the diagnosis 2000;83:715-720.
and treatment of acute and chronic heart failure and the 2007 32. McEneaney DJ, Cochrane DJ, Anderson JA, Adgey AA. A
ESC Guidelines for cardiac and resynchronization therapy. gastroesophageal electrode for atrial and ventricular pacing.
Developed with the special contribution of the Heart Failure Pacing Clin Electrophysiol. 1997;20:1815-1825.
Association and the European Heart Rhythm Association. 33. Neumar RW, Otto CW, Link MS, et al. Part 8: adult
Eur J Heart Fail. 2010;12:1143-1153. advanced cardiovascular life support: 2010 American Heart
17. Singh JP, Klein HU, Huang DT, et al. Left ventricular lead Association Guidelines for Cardiopulmonary Resuscitation
position and clinical outcome in the multicenter automatic and Emergency Cardiovascular Care. Circulation.
defibrillator implantation trial-cardiac resynchronization 2010;122(18 suppl 3):S729-S767.
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
Sullivan et al 11
34. Sodeck GH, Domanovits H, Meron G, et al. Compromising 40. Heinze H, Sier H, Schafer U, Heringlake M. Percutaneous
bradycardia: management in the emergency department. aortic valve replacement: overview and suggestions for
Resuscitation. 2007;73:96-102. anesthestic management. J Clin Anesth. 2010;22:373-378.
35. Risgaard B, Elming H, Jensen GV, Johansen JB, Toft
41. Schroeter T, Linke A, Haensig M, et al. Predictors of per-
JC. Waiting for a pacemaker: is it dangerous? Europace. manent pacemaker implantation after Medtronic CoreValve
2012;14:975-980. bioprosthesis implantation. Europace. 2012;14:1759-1763.
36. Harrigan RA, Chan TC, Moonblatt S, Vilke GM, Ufberg 42. Khawaja MZ, Rajani R, Cook A, et al. Permanent pace-
JW. Temporary transvenous pacemaker placement in the maker insertion after CoreValve transcatheter aortic valve
emergency department. J Emerg Med. 2007;32:105-111. implantation: incidence and contributing factors (the UK
37. Bauer AM, Smith RB, Thorell WE. Implications of carotid CoreValve Collaborative). Circulation. 2011;123:951-960.
sinus hypersensitivity following preoperative embolization 43. Epstein AE, Dimarco JP, Ellenbogen KA, et al. ACC/AHA/
of a carotid body tumor. An indication for prophylactic intra- HRS 2008 guidelines for device-based therapy of cardiac
operative cardiac pacing. JAMA Otolaryngol Head Neck rhythm abnormalities: executive summary. Heart Rhythm.
Surg. 2014;140:459-463. 2008;5:934-955.
38. Pornratanarangsi S, Webster MW, Alison P, Nand P. Rapid 44. Laczika K, Thalhammer F, Locker G, et al. Safe and effi-
ventricular pacing to lower blood pressure during endo- cient emergency transvenous ventricular pacing via the right
graft deployment in the thoracic aorta. Ann Thorac Surg. supraclavicular route. Anesth Analg. 2000;90:784-789.
2006;81(5):e21-23. 45. McCann P. A review of temporary cardiac pacing wires.
39. Nienaber CA, Kische S, Rehders TC, et al. Rapid pacing for Indian Pacing Electrophysiol J. 2007;7:40-49.
better placing: comparison of techniques for precise deploy-
46. Ezeugwu CO, Oluwole BO, Leibowitz AB, Benjamin E.
ment of endografts in the thoracic aorta. J Endovasc Ther. Chest X-ray and electrocardiographic abnormality after per-
2007;14:506-512. manent pacemaker insertion. Am J Cardiol. 1994;73:618-619.
Downloaded from scv.sagepub.com at UNIV OF CHICAGO LIBRARY on July 4, 2015
You might also like
- ACLS Advanced Cardiovascular Life Support Provider Manual 2023From EverandACLS Advanced Cardiovascular Life Support Provider Manual 2023No ratings yet
- Anesthetic Management For Cardiopulmonary BypassDocument16 pagesAnesthetic Management For Cardiopulmonary BypassAhmet PinarbasiNo ratings yet
- ExpertConsensus ResuscitationAfterCardiacSurgery PDFDocument16 pagesExpertConsensus ResuscitationAfterCardiacSurgery PDFJuan Guillermo BuitragoNo ratings yet
- Overdrive PacingDocument24 pagesOverdrive PacingWilliam Perero RodríguezNo ratings yet
- 1 s2.0 S0736467906006445 PDFDocument7 pages1 s2.0 S0736467906006445 PDFDiego Fernando Escobar GarciaNo ratings yet
- 4 Arterial, Central Venous, and Pulmonary Artery CathetersDocument12 pages4 Arterial, Central Venous, and Pulmonary Artery CathetersToujours ÁmeNo ratings yet
- Manejo Perioperatorio de MarcapasosDocument6 pagesManejo Perioperatorio de MarcapasosPao Sofía MoralesNo ratings yet
- Webb 2015 Management of Intra Aortic Balloon PumpsDocument16 pagesWebb 2015 Management of Intra Aortic Balloon PumpsAjiNo ratings yet
- Nursing Management of Patients Requiring Acute Mechanical Circulatory Support DevicesDocument11 pagesNursing Management of Patients Requiring Acute Mechanical Circulatory Support DevicesJaide AdderleyNo ratings yet
- Cardiac Arrest BritishDocument18 pagesCardiac Arrest Britishalejandro montesNo ratings yet
- Advances in Interventional Cardiology: Percutaneous Mechanical Circulatory Support Devices in Cardiogenic ShockDocument11 pagesAdvances in Interventional Cardiology: Percutaneous Mechanical Circulatory Support Devices in Cardiogenic ShockjoannaNo ratings yet
- Chapter 80Document7 pagesChapter 80annisarachmaNo ratings yet
- Pulmonary Atresia With An Intact Ventricular Septum: Preoperative Physiology, Imaging, and ManagementDocument12 pagesPulmonary Atresia With An Intact Ventricular Septum: Preoperative Physiology, Imaging, and ManagementGusti Ayu Radhitia OctaviaNo ratings yet
- Adjunctive Therapies For Ventricular Arrhythmia ManagementDocument10 pagesAdjunctive Therapies For Ventricular Arrhythmia ManagementsaikrishnaNo ratings yet
- Coronary Artery Bypass Graft SurgeryDocument8 pagesCoronary Artery Bypass Graft SurgeryJatin SinghNo ratings yet
- Cardiopulmonary Transplantation An Anaesthesia ReDocument7 pagesCardiopulmonary Transplantation An Anaesthesia ReAlia SandoQaNo ratings yet
- Echo HitsDocument3 pagesEcho HitsHany ElbarougyNo ratings yet
- Cardiac Electrical Assistive DevicesDocument14 pagesCardiac Electrical Assistive DevicesaprnworldNo ratings yet
- Journal of Cardiac Surgery - 2021 - Datt - Vasoplegic Syndrome After Cardiovascular Surgery A Review of PathophysiologyDocument12 pagesJournal of Cardiac Surgery - 2021 - Datt - Vasoplegic Syndrome After Cardiovascular Surgery A Review of Pathophysiologyjcr87No ratings yet
- Right Approach To VTDocument7 pagesRight Approach To VTNicole BabcockNo ratings yet
- Preliminary Experience With Cangrelor For Endovascular Treatment ofDocument9 pagesPreliminary Experience With Cangrelor For Endovascular Treatment ofPedro VillamorNo ratings yet
- Temporary Mechanical Circulatory Support Devices - Practical Considerations For All StakeholdersDocument15 pagesTemporary Mechanical Circulatory Support Devices - Practical Considerations For All StakeholdersGustavo TeixeiraNo ratings yet
- ArritmiasDocument12 pagesArritmiasJorgeNo ratings yet
- A Case Report On Middle Cerebral Artery Aneurysm.44Document5 pagesA Case Report On Middle Cerebral Artery Aneurysm.44SuNil AdhiKariNo ratings yet
- Pulmonary Atresia With An Intact Ventricular Septum: Preoperative Physiology, Imaging, and ManagementDocument11 pagesPulmonary Atresia With An Intact Ventricular Septum: Preoperative Physiology, Imaging, and ManagementAkilaNo ratings yet
- Principles of Cardiac Anaesthesia: Learning ObjectivesDocument5 pagesPrinciples of Cardiac Anaesthesia: Learning ObjectivesFitri AmaliahNo ratings yet
- AnnCardAnaesth19 Maret 2017 12Document10 pagesAnnCardAnaesth19 Maret 2017 12Henny Apriani ARNo ratings yet
- Periprocedural Anticoagulation Guidelines - UKDocument14 pagesPeriprocedural Anticoagulation Guidelines - UKjoshNo ratings yet
- Mics 7Document10 pagesMics 7Ramya ENo ratings yet
- Day 3 - APPEC 2021Document413 pagesDay 3 - APPEC 2021GaurieNo ratings yet
- Postoperative Critical Care of The Adult Cardiac16Document21 pagesPostoperative Critical Care of The Adult Cardiac16Mauricio P�rez Mac�asNo ratings yet
- 1 s2.0 S0735109720344909 MainDocument13 pages1 s2.0 S0735109720344909 MainIndira Ulfa DunandNo ratings yet
- ECOC FUNCION VENTRICULARfunctionDocument8 pagesECOC FUNCION VENTRICULARfunctionsueNo ratings yet
- 2022 The Intensive Care Management of Acute Ischaemic StrokeDocument9 pages2022 The Intensive Care Management of Acute Ischaemic StrokeOmar Alejandro Agudelo ZuluagaNo ratings yet
- Approach To Ventricular ArrhythmiasDocument18 pagesApproach To Ventricular ArrhythmiasDavid CruzNo ratings yet
- Emergency Cardiac Surgery in DOACsDocument3 pagesEmergency Cardiac Surgery in DOACsAlexander JosethangNo ratings yet
- Arrhythmias 2° To HyperkalaemiaDocument11 pagesArrhythmias 2° To Hyperkalaemiamarwanelsaeed1981No ratings yet
- Pharmacological Treatment of ArrhytmiaDocument6 pagesPharmacological Treatment of ArrhytmiaLućia-Simona Perić ExOalđeNo ratings yet
- Anaesthetic Management of Patients With Cardiac Pacemakers and Defibrillators For Noncardiac SurgeryDocument12 pagesAnaesthetic Management of Patients With Cardiac Pacemakers and Defibrillators For Noncardiac SurgeryzaheerNo ratings yet
- Beyond The Guidelines - An Approach To Cardiac Arrest in The Emergency Department - EMOttawaDocument12 pagesBeyond The Guidelines - An Approach To Cardiac Arrest in The Emergency Department - EMOttawaMohamed Saeed El KhayatNo ratings yet
- Eco in Cardiac Sugrery Anesthesic 1-s2.0-S1053077020305875-MainDocument11 pagesEco in Cardiac Sugrery Anesthesic 1-s2.0-S1053077020305875-MainCésar Marriaga ZárateNo ratings yet
- Type of PacemakerDocument26 pagesType of PacemakerMohammad AlmuhaiminNo ratings yet
- Electrical Storm 2020Document13 pagesElectrical Storm 2020Aníbal José Arroyo RodríguezNo ratings yet
- Anesthesia For Endovascular Therapy For Acute IschemicDocument36 pagesAnesthesia For Endovascular Therapy For Acute IschemicPietro DamoNo ratings yet
- Cardiac Surgery NotesDocument28 pagesCardiac Surgery Notessaranya amuNo ratings yet
- 2015 Manejo Postquirurgico Del Paciente Con Cirugia Cardiaca Parte IIDocument20 pages2015 Manejo Postquirurgico Del Paciente Con Cirugia Cardiaca Parte IIAdiel OjedaNo ratings yet
- Krish GoyalDocument10 pagesKrish GoyalAnanya ShrimankarNo ratings yet
- Antiarrhythmic Drugs and Anaesthesia 2Document9 pagesAntiarrhythmic Drugs and Anaesthesia 2CamiloRadaNo ratings yet
- HSR1 04 NaderDocument7 pagesHSR1 04 Naderserena7205No ratings yet
- Doc-20240131-Wa0 240131 224409Document6 pagesDoc-20240131-Wa0 240131 22440922alhumidi2020No ratings yet
- Diagnostic Angiography SOPDocument2 pagesDiagnostic Angiography SOPQuality Assurance DepartmentNo ratings yet
- 0-00009Document28 pages0-00009Agastya DesaiNo ratings yet
- European J of Heart Fail - 2017 - OstadalDocument4 pagesEuropean J of Heart Fail - 2017 - OstadalGustavo TeixeiraNo ratings yet
- Critical Care Volume Issue 2018 (Doi 10.1097/MCC.0000000000000516) Jozwiak, Mathieu Monnet, Xavier Teboul, Jean-Louis - Less or More Hemodynamic Monitoring in Critically Ill PaDocument7 pagesCritical Care Volume Issue 2018 (Doi 10.1097/MCC.0000000000000516) Jozwiak, Mathieu Monnet, Xavier Teboul, Jean-Louis - Less or More Hemodynamic Monitoring in Critically Ill PaShovie Thalia MirandaNo ratings yet
- Part IX: Vascular Surgery: Renal and Spinal Cord ProtectionDocument1 pagePart IX: Vascular Surgery: Renal and Spinal Cord ProtectioncesaliapNo ratings yet
- CVC Partner 1Document40 pagesCVC Partner 1stefani83No ratings yet
- NCMA113 - Finals LABORATORY Part 2Document9 pagesNCMA113 - Finals LABORATORY Part 2KYLE MITZIE SENGCONo ratings yet
- Dynamic Myocardial Perfusion (MOICT0133EA)Document13 pagesDynamic Myocardial Perfusion (MOICT0133EA)hectorjara131596No ratings yet
- 2.1. Pharmacological Therapeutics. 2.2. Basic Cardiac Life Support (BCLS) and Advanced Cardiac Life Support (ACLS) in Neonates and ChildDocument3 pages2.1. Pharmacological Therapeutics. 2.2. Basic Cardiac Life Support (BCLS) and Advanced Cardiac Life Support (ACLS) in Neonates and Childclint xavier odangoNo ratings yet
- Journal of Arrhythmia - 2018 - Alasti - Pacemaker Mediated ArrhythmiasDocument8 pagesJournal of Arrhythmia - 2018 - Alasti - Pacemaker Mediated ArrhythmiasVaishnavi YacheNo ratings yet
- The Orbit: D.Hanan Darif 2016Document16 pagesThe Orbit: D.Hanan Darif 2016henry cazeNo ratings yet
- Pico PaperDocument9 pagesPico Paperapi-251822043No ratings yet
- J of Clinical Hypertension - 2019 - Ishiyama - Constipation Induced Pressor Effects As Triggers For Cardiovascular EventsDocument5 pagesJ of Clinical Hypertension - 2019 - Ishiyama - Constipation Induced Pressor Effects As Triggers For Cardiovascular Eventskahar ahmadNo ratings yet
- Henry Dionio, Petitioner, V. Trans-Global Maritime AgencyDocument2 pagesHenry Dionio, Petitioner, V. Trans-Global Maritime AgencyDYbieNo ratings yet
- Icpc Heart ScreeningDocument2 pagesIcpc Heart ScreeningMahmoud TitilayoNo ratings yet
- Transport Test V1 2016Document11 pagesTransport Test V1 2016Indraneel BhattacharjeeNo ratings yet
- The Heart Shadow in The MediatinumDocument7 pagesThe Heart Shadow in The MediatinumRolando Reyna100% (1)
- AQ FamilyMedicine 06Document12 pagesAQ FamilyMedicine 06Eduardo OrtizNo ratings yet
- AEBA QUESTIONS-WPS OfficeDocument2 pagesAEBA QUESTIONS-WPS OfficeMarj Castor LisondraNo ratings yet
- ECIM 2024 Scientific ProgrammeDocument39 pagesECIM 2024 Scientific ProgrammeFenix RenaceNo ratings yet
- Drug Study AzathioprineDocument3 pagesDrug Study AzathioprineBunnie AlphaNo ratings yet
- Case Study - Urinary SystemDocument4 pagesCase Study - Urinary SystemVanessa PalomaNo ratings yet
- Lect 10 - Opioids and LADocument40 pagesLect 10 - Opioids and LARaneem ShiferNo ratings yet
- LESSON PLAN HypertensionDocument9 pagesLESSON PLAN HypertensionARUN JOSE (08156864174)85% (39)
- MCQs and Cases in MedicineDocument14 pagesMCQs and Cases in Medicineyoune6No ratings yet
- The Strawberry Tongue: What, How and WhereDocument6 pagesThe Strawberry Tongue: What, How and WhereVasishta NadellaNo ratings yet
- Curriculum VitaeDocument12 pagesCurriculum VitaeHannah AlmacenNo ratings yet
- Jurnal R2 YerlizaDocument15 pagesJurnal R2 YerlizaYerliza AgrichaNo ratings yet
- Health Assessment PortfolioDocument25 pagesHealth Assessment PortfolioGEN ERIGBUAGASNo ratings yet
- Alvarez Duran Priscilla Jacqueline: ExercisesDocument1 pageAlvarez Duran Priscilla Jacqueline: ExercisesPRISCILLA JACQUELINE ALVAREZ DURANNo ratings yet
- Carcinosinum: Materia MedicaDocument7 pagesCarcinosinum: Materia Medicas.s.r.k.m. gupta100% (1)
- Obs Muhs LaqsDocument66 pagesObs Muhs Laqs2n72wdwv45No ratings yet
- Cystic Fibrosis PDFDocument22 pagesCystic Fibrosis PDFAbdelrahman AlshatnawiNo ratings yet
- Nurs 106 Final OutcomesDocument11 pagesNurs 106 Final OutcomesJulia ThindNo ratings yet
- Abarelix: Drugbank Id Name Weight Structure Categories Therapeutic IndicationDocument19 pagesAbarelix: Drugbank Id Name Weight Structure Categories Therapeutic IndicationVinay KumarNo ratings yet
- EdemaDocument5 pagesEdemaaldwinngNo ratings yet
- CPR Awareness TrainingDocument5 pagesCPR Awareness TrainingSayed SallamNo ratings yet
- Patient FinalDocument51 pagesPatient FinalCharmmaine Yu-AcmanNo ratings yet
- Neurocritical Care in The General Intensive Care UnitDocument17 pagesNeurocritical Care in The General Intensive Care UnitdanielNo ratings yet
- Francisco, Ma. Theresa Q. 1bsn-Ui (Session 19-Lec)Document5 pagesFrancisco, Ma. Theresa Q. 1bsn-Ui (Session 19-Lec)DANICA JEAN PRIANES100% (1)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Rating: 3 out of 5 stars3/5 (1)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (2)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (29)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (81)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 4 out of 5 stars4/5 (4)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (5)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (45)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- Summary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedRating: 4 out of 5 stars4/5 (61)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesFrom EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesRating: 4.5 out of 5 stars4.5/5 (1412)
- How to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingFrom EverandHow to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingRating: 1 out of 5 stars1/5 (1)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (59)