Professional Documents
Culture Documents
RP 1 PDF
Uploaded by
Obsa Abrahim0 ratings0% found this document useful (0 votes)
8 views9 pagesOriginal Title
Rp_1_pdf
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
8 views9 pagesRP 1 PDF
Uploaded by
Obsa AbrahimCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 9
Lecture Outline
• Basics of the Respiratory System
– Functions & functional anatomy
• Gas Laws
Respiratory Physiology • Ventilation
• Diffusion & Solubility
• Gas Exchange
– Lungs
– Tissues
• Gas Transport in Blood
• Regulation of Ventilation & Impacts on
– Gas levels, pH
Basics of the Respiratory System Basics of the Respiratory System
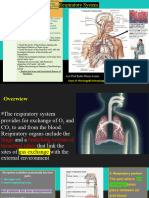
General Functions Respiration
• Exchange of gases • What is respiration?
• Directionality depends on gradients! – Respiration = the series of exchanges that leads to
the uptake of oxygen by the cells, and the release of
– Atmosphere to blood carbon dioxide to the lungs
Step 1 = ventilation
– Blood to tissues – Inspiration & expiration
• Regulation of pH Step 2 = exchange between alveoli (lungs) and pulmonary
capillaries (blood)
– Dependent on rate of CO2 release – Referred to as External Respiration
Step 3 = transport of gases in blood
• Protection Step 4 = exchange between blood and cells
– Referred to as Internal Respiration
• Vocalization – Cellular respiration = use of oxygen in ATP
• Synthesis synthesis
1
Schematic View of Respiration
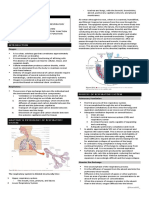
Basics of the Respiratory System
Functional Anatomy
• What structural aspects must be considered in the
process of respiration?
External Respiration – The conduction portion
– The exchange portion
– The structures involved with
ventilation
• Skeletal & musculature
• Pleural membranes
• Neural pathways
• All divided into
– Upper respiratory tract
• Entrance to larynx
– Lower respiratory tract
Internal Respiration • Larynx to alveoli (trachea
to lungs)
Basics of the Respiratory System Basics of the Respiratory System
Functional Anatomy Functional Anatomy
• Bones, Muscles & Membranes • Function of these Bones, Muscles & Membranes
– Create and transmit a pressure gradient
• Relying on
– the attachments of the
muscles to the ribs
(and overlying tissues)
– The attachment of the
diaphragm to the base
of the lungs and associated
pleural membranes
– The cohesion of the parietal
pleural membrane to the
visceral pleural membrane
– Expansion & recoil of the lung
and therefore alveoli with the
movement of the overlying
structures
2
Basics of the Respiratory System Basics of the Respiratory System
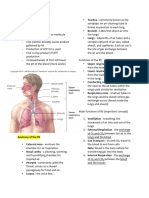
Functional Anatomy Functional Anatomy
• Pleural Membrane Detail • The Respiratory Tree
– Cohesion between parietal and visceral layers – connecting the external environment to the
is due to serous fluid in the pleural cavity exchange portion of the lungs
• Fluid (30 ml of fluid) creates an attraction between
the two sheets of membrane – similar to the vascular component
• As the parietal membrane expands due to – larger airway = higher flow & velocity
expansion of the thoracic cavity it “pulls” the • small cross-sectional area
visceral membrane with it
– And then pulls the underlying structures which expand as – smaller airway = lower flow & velocity
well
• large cross-sectional area
• Disruption of the integrity of the pleural membrane
will result in a rapid equalization of pressure and
loss of ventilation function = collapsed lung or
pneumothorax
Basics of the Respiratory System
Functional Anatomy
• The Respiratory Tree
– Upper respiratory tract is for all intensive purposes a single large
conductive tube
– The lower respiratory tract starts after the larynx and divides
again and again…and again to eventually get to the smallest
regions which form the exchange membranes
• Trachea
• Primary bronchi
• Secondary bronchi
conductive portion
• Tertiary bronchi
• Bronchioles
• Terminal bronchioles
• Respiratory bronchioles with
start of alveoli outpouches
exchange portion
• Alveolar ducts with outpouchings
of alveoli
3
Basics of the Respiratory System
Functional Anatomy
• What is the function of the upper
respiratory tract? Raises
incoming air to
– Warm 37 Celsius Forms
mucociliary
– Humidify Raises escalator
incoming air to
– Filter 100% humidity
– Vocalize
Basics of the Respiratory System Basics of the Respiratory System
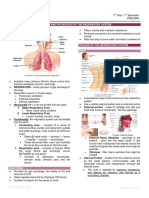
Functional Anatomy Functional Anatomy
• What is the function of the lower respiratory • Characteristics of exchange membrane
tract? – High volume of blood through huge capillary
– Exchange of gases …. Due to network results in
• Huge surface area = 1x105 m2 of type I alveolar cells (simple
squamous epithelium) • Fast circulation through lungs
• Associated network of pulmonary capillaries – Pulmonary circulation = 5L/min through lungs….
– 80-90% of the space between alveoli is filled with blood in – Systemic circulation = 5L/min through entire body!
pulmonary capillary networks • Blood pressure is low…
• Exchange distance is approx 1 um from alveoli to blood! – Means
– Protection » Filtration is not a main theme here, we do not want a
• Free alveolar macrophages (dust cells) net loss of fluid into the lungs as rapidly as the
• Surfactant produced by type II alveolar cells (septal cells) systemic tissues
» Any excess fluid is still returned via lymphatic system
4
Basics of the Respiratory System Respiratory Physiology
Functional Anatomy Gas Laws
• Sum-up of functional anatomy • Basic Atmospheric conditions
– Pressure is typically measured in mm Hg
– Ventilation? – Atmospheric pressure is 760 mm Hg
– Atmospheric components
– Exchange? • Nitrogen = 78% of our atmosphere
– Vocalization? • Oxygen = 21% of our atmosphere
• Carbon Dioxide = .033% of our atmosphere
– Protection? • Water vapor, krypton, argon, …. Make up the rest
• A few laws to remember
– Dalton’s law
– Fick’s Laws of Diffusion
– Boyle’s Law
– Ideal Gas Law
Respiratory Physiology Respiratory Physiology
Gas Laws Gas Laws
• Dalton’s Law • Fick’s Laws of Diffusion
– Law of Partial Pressures
• “each gas in a mixture of gases will exert a pressure
– Things that affect rates of diffusion
independent of other gases present” • Distance to diffuse 3
Or
• Gradient sizes
• The total pressure of a mixture of gases is equal to the sum
of the individual gas pressures. • Diffusing molecule sizes 3
– What does this mean in practical application? • Temperature 3
• If we know the total atmospheric pressure (760 mm Hg) and
the relative abundances of gases (% of gases) – What is constant & therefore out of our realm
– We can calculate individual gas effects! of concern? 3
– Patm x % of gas in atmosphere = Partial pressure of any
atmospheric gas • So it all comes down to partial pressure gradients
» PO2 = 760mmHg x 21% (.21) = 160 mm Hg of gases… determined by Dalton’s Law!
• Now that we know the partial pressures we know the
gradients that will drive diffusion!
5
Respiratory Physiology Respiratory Physiology
Gas Laws Gas Laws
• How does Boyle’s Law work in us?
• Boyle’s Law – As the thoracic cavity (container) expands the volume must up
– Describes the relationship between pressure and pressure goes down
• If it goes below 760 mm Hg what happens?
and volume – As the thoracic cavity shrinks the volume must go down and
pressure goes up
• “the pressure and volume of a gas in a system are • If it goes above 760 mm Hg what happens
inversely related”
• P1V1 = P2V2
Respiratory Physiology Ventilation
Gas Laws
• Ideal Gas law • Terminology
– Inspiration = the movement of air into the respiratory tracts
– The pressure and volume of a container of (upper & lower)
gas is directly related to the temperature of – Expiration = movement of air out of the respiratory tracts
– Respiratory cycle is one inspiration followed by an expiration
the gas and the number of molecules in the • Cause of Inspiration?
container – Biological answer
• Contraction of the inspiratory muscles causes an increase in the
– PV = nRT thoracic cavity size, thus allowing air to enter the respiratory tract
• n = moles of gas – Physics answer
• T = absolute temp • As the volume in the thoracic cavity increases (due to inspiratory
muscle action) the pressure within the respiratory tract drops below
• R = universal gas constant @ 8.3145 J/mol K atmospheric pressure, creating a pressure gradient which causes
molecular movement to favor moving into the respiratory tract
– Do we care? – Cause of Expiration?
6
Ventilation Ventilation
Besides the
diaphragm (only
creates about
60-75% of the
volume change)
what are the
muscles of
inspiration &
expiration?
What is the relationship
between alveolar pressure
and intrapleural pressure and
the volume of air moved?
Ventilation Ventilation
• What are the different respiratory
patterns?
– Quiet breathing (relaxed)
– Forced inspirations & expirations
• Respiratory volumes follow these
respiratory patterns…
7
Ventilation Ventilation
• Inspiration • Expiration
– Occurs as alveolar pressure drops below atmospheric – Occurs as alveolar pressure elevates above
pressure atmospheric pressure due to a shrinking
• For convenience atmospheric pressure = 0 mm Hg thoracic cage
– A (-) value then indicates pressure below atmospheric P
• At time 2-4 seconds
– A (+) value indicates pressure above atmospheric P
– Inspiratory muscles relax, elastic tissue of corresponding
• At the start of inspiration (time = 0), structures initiates a recoil back to resting state
– atmospheric pressure = alveolar pressure – This decreases volume and correspondingly increases
» No net movement of gases! alveolar pressure to 1 mm Hg
• At time 0 to 2 seconds » This is above atmospheric pressure, causing…?
– Expansion of thoracic cage and corresponding pleural • At time 4 seconds
membranes and lung tissue causes alveolar pressure to drop to
– Atmospheric pressure once again equals alveolar
-1 mm Hg
pressure and there is no net movement
– Air enters the lungs down the partial pressure gradient
Ventilation Ventilation
• Both inspiration and expiration can be • Things to consider
modified – surfactant effect
– Forced or active inspiration
– airway diameter
– Forced or active expiration
– Minute volume respiration (ventilation rate times tidal
– The larger and quicker the expansion of the volume) & anatomical dead space
thoracic cavity, the larger the gradient and • Leading to a more accurate idea of alveolar ventilation rates
• The faster air moves down its pressure gradient
– Changes in ventilation patterns
8
Ventilation Ventilation
• Surfactant is produced by the septal cells
– Disrupts the surface tension & cohesion of water molecules
– Impact? Airway
• prevents alveoli from sticking together during expiration
diameter &
other factors
that affect
airway
resistance?
Ventilation Next Time…
The relationship between minute volume (total pulmonary ventilation)
and alveolar ventilation & the subsequent “mixing” of air
• Diffusion and Solubility
– Gas composition in the alveoli
• Gas exchange
• Gas transport in blood
• Regulation of pulmonary function
9
You might also like
- Anatomy and PhysiologyDocument49 pagesAnatomy and PhysiologyRainier CalisaganNo ratings yet
- Respiratory PhysiologyDocument37 pagesRespiratory PhysiologyGuillermo Sasso Pacheco100% (1)
- Respiratory Physiology Part 1, Revised 2020Document48 pagesRespiratory Physiology Part 1, Revised 2020Allan Q Venus100% (1)
- Thorax McqsDocument23 pagesThorax McqsBassamSheryanNo ratings yet
- Medical Surgical Nursing Module 11Document26 pagesMedical Surgical Nursing Module 11weissNo ratings yet
- Thorax Practice Exam QuestionsDocument19 pagesThorax Practice Exam QuestionsAlejandra Dávalos TeranNo ratings yet
- I. Review of Respiratory System A.ppt 2Document115 pagesI. Review of Respiratory System A.ppt 2arielleortuosteNo ratings yet
- Pleur EvacDocument20 pagesPleur Evacmina zayNo ratings yet
- Test Bank For Essentials of Anatomy Physiology 2nd Edition Kenneth Saladin Robin McfarlandDocument31 pagesTest Bank For Essentials of Anatomy Physiology 2nd Edition Kenneth Saladin Robin McfarlandAntonio Demetro100% (28)
- Pcap C CaseDocument81 pagesPcap C CaseAyaBasilio70% (10)
- Respiratory System ReviewerDocument7 pagesRespiratory System ReviewerVictoria Ellex TiomicoNo ratings yet
- Thorax & LungsDocument14 pagesThorax & LungsRed MontemayorNo ratings yet
- MC 1B 11 Respiratory System DisordersDocument9 pagesMC 1B 11 Respiratory System DisordersjambyNo ratings yet
- Functions of The Respiratory SystemDocument10 pagesFunctions of The Respiratory Systemadelina.jianu9991No ratings yet
- The Respiratory SystemDocument22 pagesThe Respiratory System5130022035 ARINA DINANANo ratings yet
- Respiratory Systm1-2 BileşikDocument55 pagesRespiratory Systm1-2 BileşikDeniz asmazNo ratings yet
- The Respiratory Structures and Breathing Mechanisms in Humans and AnimalsDocument5 pagesThe Respiratory Structures and Breathing Mechanisms in Humans and AnimalsireneNo ratings yet
- Nurs 13 Week 2Document20 pagesNurs 13 Week 2cheskalyka.asiloNo ratings yet
- (Ofi) Respiratory SystemDocument12 pages(Ofi) Respiratory SystemPimpamNo ratings yet
- 02 Pulmonary Physiol 27-02-10Document8 pages02 Pulmonary Physiol 27-02-10angealityNo ratings yet
- Gen BioDocument15 pagesGen BioCAMILLE JELLA ALZOLANo ratings yet
- Respiarotry SystemDocument4 pagesRespiarotry SystemrueNo ratings yet
- NCM103j OXYGENATIONDocument4 pagesNCM103j OXYGENATIONTamara RomuarNo ratings yet
- 1 Mechanics of Breathing PDFDocument38 pages1 Mechanics of Breathing PDFEkrem VarlikNo ratings yet
- Chapter 11 Gas Exchange in Humans 23-24Document127 pagesChapter 11 Gas Exchange in Humans 23-24Huraiza AsifNo ratings yet
- 3 Explanation - Respiratory System Presentation - Interactive W Integrated Digital INBs MDocument19 pages3 Explanation - Respiratory System Presentation - Interactive W Integrated Digital INBs MDennis OgavarNo ratings yet
- Respiration and Gas ExchangeDocument25 pagesRespiration and Gas ExchangeTyrsonNo ratings yet
- CH 23 Respiration F 2017 SRMDocument153 pagesCH 23 Respiration F 2017 SRMJuliaNo ratings yet
- Form 4 Revision QuizDocument80 pagesForm 4 Revision QuizEnvira LeeNo ratings yet
- Anatomy Final pt.2Document8 pagesAnatomy Final pt.2Gladys Mae S. BañesNo ratings yet
- Respiratory PhysiologyDocument39 pagesRespiratory Physiologytesfamichael mengistuNo ratings yet
- 1.airway, Airflow, Ventilation and DiffusionDocument64 pages1.airway, Airflow, Ventilation and DiffusionEbin EbenezerNo ratings yet
- Circulatory SystemDocument30 pagesCirculatory SystemScheherazade CNo ratings yet
- Respiratory and Circulatory SystemDocument35 pagesRespiratory and Circulatory SystemScheherazade CNo ratings yet
- 04 OxygenationDocument4 pages04 Oxygenationbunso padillaNo ratings yet
- Respiratory System 1Document29 pagesRespiratory System 1John SmithNo ratings yet
- 3.1 Oxygenation Orpeza Cezar 1 7Document8 pages3.1 Oxygenation Orpeza Cezar 1 7Mika Marielle TrincheraNo ratings yet
- Physiology Of: RespirationDocument51 pagesPhysiology Of: RespirationDr. R. PeriasamyNo ratings yet
- Gas Exchange in Humans: 7.1 Human Breathing SystemDocument10 pagesGas Exchange in Humans: 7.1 Human Breathing Systemka klklklNo ratings yet
- Module 5-Respiratory SystemDocument64 pagesModule 5-Respiratory SystemBorja MelanieNo ratings yet
- RT 105 Prefinal NotesDocument24 pagesRT 105 Prefinal NotesLouiseNo ratings yet
- Respiratory KeypointsDocument11 pagesRespiratory KeypointsShahina ShayneNo ratings yet
- Dissection of The Amphibian Respiratory System and Mammalian Excretory SystemDocument6 pagesDissection of The Amphibian Respiratory System and Mammalian Excretory System门门No ratings yet
- The Respiratory SystemDocument53 pagesThe Respiratory SystemShaila AliNo ratings yet
- (BIOLOGY) Human Respiratory SystemDocument7 pages(BIOLOGY) Human Respiratory SystemHAJIRA RAMLANNo ratings yet
- Lab 11 Respiration Mammalian PhysiologyDocument61 pagesLab 11 Respiration Mammalian PhysiologyCedric KanyindaNo ratings yet
- Anatomy and Physiology of The Respiratory SystemDocument14 pagesAnatomy and Physiology of The Respiratory SystemAmore BuenafeNo ratings yet
- 16 Respiratory System 2022Document67 pages16 Respiratory System 2022Yiannis AlatsathianosNo ratings yet
- Drugs Acting On The Respiratory System Respiratory System: Lung ComplianceDocument9 pagesDrugs Acting On The Respiratory System Respiratory System: Lung ComplianceAdiel CalsaNo ratings yet
- Bio CH8 F4 Studywithadmin PDFDocument16 pagesBio CH8 F4 Studywithadmin PDFMUHAMMAD FAREEZ HAIKAL MOHD SHAIFUDDINNo ratings yet
- Resource Guide: Principles of CapnographyDocument70 pagesResource Guide: Principles of CapnographyJohn Paul PunzalanNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemChelsie NicoleNo ratings yet
- Assessment of The Thorax and LungsDocument9 pagesAssessment of The Thorax and LungsJasmin MolanoNo ratings yet
- 1st-quarter-PART 1 DLLDocument35 pages1st-quarter-PART 1 DLLCatherineNo ratings yet
- 11J Caybot Jashjovian Task11Document19 pages11J Caybot Jashjovian Task11JASH JOVIAN CAYBOTNo ratings yet
- Funda Lec 1ST Week OxygenationDocument8 pagesFunda Lec 1ST Week OxygenationBasty BautistaNo ratings yet
- Respiratory Physiology First EpisodesDocument26 pagesRespiratory Physiology First EpisodesjunaidukabirnabadeNo ratings yet
- 04 Respiration 2022 - AnswersDocument10 pages04 Respiration 2022 - Answersria khanNo ratings yet
- 3 Explanation - Respiratory System Presentation - Standard VersionDocument13 pages3 Explanation - Respiratory System Presentation - Standard VersionVictoria LowmanNo ratings yet
- Fisio RespirasiDocument114 pagesFisio Respirasigrace liwantoNo ratings yet
- Overview of The Resp System - PADocument27 pagesOverview of The Resp System - PAwajdjnbNo ratings yet
- Respiratory PhysiologyDocument55 pagesRespiratory PhysiologyANDRES GUARDIA CAYONo ratings yet
- Self Test 3Document6 pagesSelf Test 3202310446No ratings yet
- Respiratorio Con TextoDocument119 pagesRespiratorio Con TextoLMN214No ratings yet
- Ncma 113Document4 pagesNcma 113Wonie booNo ratings yet
- Respiratory System PPT (Biology)Document8 pagesRespiratory System PPT (Biology)Maxxdlc 16No ratings yet
- BBMS2004 L13 Respiratory System - Thoracic Cavity and Respiration 2022Document26 pagesBBMS2004 L13 Respiratory System - Thoracic Cavity and Respiration 2022JinyoungNo ratings yet
- PTB Grand Case Pres Group A 1Document46 pagesPTB Grand Case Pres Group A 1Community BNo ratings yet
- 1st Week Lecture - Cells, Tissues, Glands and MembranesDocument35 pages1st Week Lecture - Cells, Tissues, Glands and MembranesWaleed AhmadNo ratings yet
- Pulmonary Function I: Biopac Student Lab Lesson 12Document4 pagesPulmonary Function I: Biopac Student Lab Lesson 12komangNo ratings yet
- #1 Points 2 Kool Medic PDFDocument137 pages#1 Points 2 Kool Medic PDFSyed Ali Raza NaqviNo ratings yet
- Anatomy and Physiology of The Respiratory SystemDocument14 pagesAnatomy and Physiology of The Respiratory SystemAmore BuenafeNo ratings yet
- A.respiratory HistoryDocument3 pagesA.respiratory HistoryEl SpinnerNo ratings yet
- Case Study Tension Pneumothorax BSN 4 2 1Document57 pagesCase Study Tension Pneumothorax BSN 4 2 1aaron tabernaNo ratings yet
- ANAPHY111Document60 pagesANAPHY111Gerlyn MortegaNo ratings yet
- Chapter 1: Introduction To Anatomy and Physiology NotesDocument6 pagesChapter 1: Introduction To Anatomy and Physiology Notesapi-305436791No ratings yet
- Respiratory System HandoutDocument11 pagesRespiratory System HandoutJohn Carlo SantiagoNo ratings yet
- 1-Mechanism and Regulation of Respiration ModifiedDocument10 pages1-Mechanism and Regulation of Respiration Modifiedخالد القرشيNo ratings yet
- Human Anatomy and PhysiologyDocument37 pagesHuman Anatomy and Physiology813 cafeNo ratings yet
- Thoracic Surgery: Cervical, Thoracic and Abdominal ApproachesDocument1,068 pagesThoracic Surgery: Cervical, Thoracic and Abdominal ApproachesAlexandru GibuNo ratings yet
- PneumothoraxDocument11 pagesPneumothoraxmrinmayee deshmukhNo ratings yet
- Fundamentals of Financial Management Concise 7th Edition Brigham Test BankDocument25 pagesFundamentals of Financial Management Concise 7th Edition Brigham Test BankMalloryHartmanmkgqd100% (63)
- English Homework 4Document2 pagesEnglish Homework 4Teodora TanaseNo ratings yet
- 2005 10 24 Review AnswersDocument30 pages2005 10 24 Review Answersaip1000No ratings yet
- Incomplete Border Sign - Print Friendly - STATdxDocument2 pagesIncomplete Border Sign - Print Friendly - STATdxmihaelaNo ratings yet
- Thorax and Lungs Jarvis-Chap 18Document94 pagesThorax and Lungs Jarvis-Chap 18guy3280100% (6)
- Praktikum 1 Patologi ThoraxDocument61 pagesPraktikum 1 Patologi ThoraxFarizky DwitiaNo ratings yet
- 1st Prof MBBS Supplementary 10 Years CompilationDocument67 pages1st Prof MBBS Supplementary 10 Years CompilationDebasis PramanikNo ratings yet