Professional Documents
Culture Documents
Adverse Blood Reaction and HDN
Uploaded by
Adeniran Charles0 ratings0% found this document useful (0 votes)
14 views34 pagesOriginal Title
Adverse Blood reaction and HDN
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
14 views34 pagesAdverse Blood Reaction and HDN
Uploaded by
Adeniran CharlesCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 34
COMPLICATIONS AND DISEASES
ASSOCIATED WITH BLOOD
TRANSFUSION
Dr OT Ojo
Introduction
• Blood transfusion is a life saving procedure but
potentially hazardous.
• In spite of measures designed to remove adverse
effects of blood transfusion, complications remain a
source of concern.
• The type and frequency of complication however
depend on the amount of care exercised in the
preparation for, and the supervision of the
transfusion procedure.
• Blood transfusion should be considered only when
there is no alternative means of treatment.
Complications of transfusion
Immediate Delayed
• Immunological • Immunological
Febrile non haemolytic transfusion
reactions Haemolytic transfusion
Haemolytic transfusion reaction reaction
Allergic reaction Post transfusion purpura
Anaphylaxis
Transfusion-associated lung injury
GVHD
• Non immunological • Non immunological
Circulatory overload Transfusion of infectious
Bacterial contamination of donor
blood unit
agents
Air embolism Iron overload
FNHTR
• Due to reaction of alloantibodies in the recipient against
transfused leucocyte antigen.
• Also due to release of cytokines from leucocytes in the
stored blood.
• Common in previously sensitized individual- previous
transfusion or pregnancy.
• Present with fever, occasional chills, rigors, headache.
• Occur within 30-60mins of transfusion.
• R/O HTR and bacterial contamination of donor unit.
• Management- Stop transfusion, give antipyretics/
antihistamine, slow speed of transfusion.
• Prevention- Leucocyte-depleted packed cells.
HTR
• Haemolytic complication results from premature
destruction of donor cells as a result of immune
antibodies in the recipient.
• Classification- immediate (acute) haemolytic and
delayed haemolytic.
• Immediate: Often result from ABO
incompatibility mediated by by IgM or
sometimes IgG Anti-A or Anti-B.
Usually due to Clerical error- incorrect
identification of recipient and incorrect labelling
of sample bottle or filling of request form
HTR…
• Pathogenesis:
Antibodies in patient plasma bind to donor
red cells→ full complement activation (C5-
C9)→ Acute intravascular haemolysis.
C3a & C5a cause vasodilation →hypotension,
ARF.
Release of procoagulant from destroyed RBC
→activation of coagulation →DIC
HTR…
• Clinical features:
Occurs within mins of starting transfusion
Heat or pain at the infusion site, loin or low back
pain, chest tightness, breathlessness, throbbing
headache, nausea/ vomiting, Pyrexia, rigor,
Hypotension and vascular collapse.
Others include Haemoglobinuria, DIC, Acute renal
failure with Oliguria, and death.
Anaesthetized patient- hypotension, DIC
Management
• Stop blood transfusion
• restore blood volume and blood pressure.
• Investigate
Investigations
• Confirm that recipient identity is the same as that on compatibility
label and donor unit
• Repeat grouping on pre-and post-transfusion sample of recipient ,
as well as donor sample.
• Repeat the crossmatch on donor cell against recipient pre and
post-transfusion sample.
• DAT on post-transfusion sample
• Check plasma for haemoglobinaemia (pink colouration)
• urine for Haemogloninuria
• LFT - ↑ unconjugated bilirubin
• Test for DIC- PLT, PT/APTT, FDPs
• E/u/Cr
• Bacteria contamination-
black/ purple discolouration of RC with evidence of haemolysis
Blood culture
Delayed HTR
• Due to secondary response in a patient
already previously sensitized to antigens
present on recently transfused red cells.
• It occurs within 5 to 10 days.
• Cf- Anaemia and jaundice
• Usually caused by Rh (anti-c) and Kidd (anti-
JK).
• DAT is +ve
Post-transfusion purpura
• This is characterised by a sudden onset of severe
thrombocytopaenia 7 -10 days post-transfusion.
• It follows a history of previous transfusion or
pregnancy and is far commoner in women.
• It is due to Anti-HPA -1a, both transfused and
recipient PLT are destroyed.
• Usu. self-limiting.
• Otherwise, Immunoglobulin or plasma exchange
may be needed.
Anaphylactic reaction
• It is caused by Anti-IgA in an IgA deficient person.
• Prior sensitization or without stimulation
• Anti-IgA-IgA complex activate complement → C3a &C5a
generation.
• Features :
Nausea, abdominal cramps, vomitting, diarrhoea,
hypotension, breathlessness, facial edema
Shock may occur rarely and can be potentially fatal.
• Stop transfusion immediately.
• Treat with antihistamine, hydrocortisone, adrenaline.
Allergic Reactions
• Due to reaction between plasma proteins and
IgE antibodies in recipient’s plasma→release
of histamine.
• Cf- Urticaria, rash and pruritus.
• Treatment-antihistamine & hydrocortisone
Transfusion-related acute lung Injury
(TRALI)
• Leucoagglutinins from donor+ leucocytes in
recipient= leucocyte aggregate, lodgement in
pulmonary microcirculation causes increase in
vascular permeability.
• Cf- fever, chills, respiratory distress, dry cough
• CXR- Diffuse pulmonary infiltrate
• Donors usu. Multiparous women.
• Treatment-supportive
Graft-versus-host disease(GvHD)
• occurs when live lymphocyte are transfused to
an immunocompromised patient.
• Cf-fever, skin rash, vomiting, diarrhoea,
hepatitis, pancytopaenia.
• Prevention- Irradiation of blood.
• NON-IMMUNOLOGICAL
COMPLICATIONS
Transfusion of infectious agents
• These include Hepatitis B virus (HBV), Hepatitis C
virus (HCV), Human Immunodeficiency virus
(HIV), Cytomegalovirus (CMV), Filaria, Syphilis,
toxoplasma and Malaria.
• Reaction to bacteria and or its pyrogen:
This is rare because of sterilization of fluid and
disposable equipment.
Can present with circulatory collapse.
Prevention is by the use of aseptic techniques in
blood donation, and the storage of blood at a
temperature of 2-80C.
Circulation Overload
• Due to rapid transfusion of large volumes of
blood without equivalent blood loss.
• Can also occur after transfusion of small amt
of blood to a patient with abnormal cardiac or
renal function.
• Treatment: Prop up in bed,O2, diuretic
• Prevention: give packed cells
use diuretics.
• Thrombophlebitis: This is due to indwelling
venous canula.
• Air embolism: This has been eliminated by the
use of plastic bags and a closed system.
• Post-transfusion iron overload occurs in
multiply transfused individuals.
Complication of massive blood
transfusion
• Replacement of a patient’s total blood volume
with stored blood within 24hrs.
Dilution of Platelets, Reduction of coagulation
factors, especially factors Va and VIIIa
Hypocalcaemia and Hyperkaleamia –
Acidosis
Hypothermia causing cardiac irregularities
•HAEMOLYTIC
DISEASE OF THE
NEWBORN (HDN)
Introduction
• It is a disease in which there is destruction of
RBCs of the fetus or newborn by maternal
alloantibodies against paternal antigens on the
child’s RBCs.
• Maternal antibodies is stimulated due to blood
group incompatibility between mother and fetus.
• Causal Red cell antigens-Rh-D, Rh-c, kell, A and B.
• Rh-D, Rh-c, kell- can cause severe HDN while ABO
incompatibility cause mild disease.
• Others- Duffy, Kidd
•Rh HDN
Introduction
• RhD negative mother pregnant with RhD +ve
baby.
• RhD +ve fetal RBC cross into maternal
circulation at parturition/ 3rd trimester and
sensitize the mother to produce anti-D.
• Sensitization could also be due to
Amniocentesis, External cephalic version,
threatened abortion, and chorion villus
sampling or trauma to placenta.
Pathogenesis
• Fetomaternal haemorrhage→10 Immune response
with production of IgM abs in the 1st pregnancy, baby
is not affected
• FMH in 2nd pregnancy→ 20 Immune response with
production of IgG abs which cross placenta to coat
fetal RhD +ve RBC.
• IgG coated fetal RBCs are destroyed in the spleen→
anaemia →erythroid hyperplasia in the BM
→extramedulary erythropoesis in the spleen and
liver.
• uncojugated bilirubin in fetus cross into maternal
circulation and metabolised
• ↑uncojugated bilirubin in neonate due to
immaturity of glucoronyl transferase, this may cross
the BBB and damage basal ganglia → kernicterus.
Clinical features
• Variable
• Mild anaemia & jaundice
• Kernicterus-neurological deficit resulting in
deafness, mental retardation, spasticity, and
epilepsy
• Still birth (Hydop fetalis)-severe anaemia,
hepatosplenomegaly, ascitis and anarsarca
Laboratory investigations
ANC:
• mother
History of sensitization
Blood group-ABO and Rh
Antibody screening, identification, titer
• Blood group of the father
• Fetal
Amniocentesis- assess conc. of bilirubin done between
28-32wks GA, but if bad obstetric Hx done 10wks prior
to the date of previous fetal or neonatal death.
Laboratory investigations…
Indicated when maternal anti-D titer is 1:32, rising anti-D
titer on ff up visit, bad obstetric hx (previously severely
affected offspring).
Liley’s chart- Zone 1 (low), II (middle), III (high)
Zone III indicate severely affected fetus with imminent
death: GA<34wks- intrauterine transfusion, GA >34wks-
delivery
Zone II- repeat and do as in I
Zone I-proceed to term
• Cordocentesis- estimate Hb and bilirubin, blood group,
DAT
• Velocimetry of fetal middle cerebral artery by doppler
USS- ↑vel correlate with fetal anaemia (IUFT)
Laboratory investigations…
• Newborn
Blood group
PBF- numerous NRBCs (erythroblastosis),
polychromasia
DAT-+ve
Hb and bilirubin conc.-do urgent EBT if Hb<
12g/dL or unconjugated bilirubin> 5mg/dL
• Maternal post delivery-Betke-Kleihauer test/ flow
cytometry for FMH vol. estimation
Rh HDN
Blood film from a baby with Rh HDN due to anti-D showing
polychromasia and large numbers of NRCs, but relatively few
spherocytes.
Treatment
• Fetus- IUFT or delivery depending on fetal
lung maturity
• Neonate-
EBT if bilirubin is rising rapidly
Phototherapy
Albumin infusion
Prevention of Rh isoimmunisation
• During antenatal- anti-D IgG given to RhD-ve mother
with potentially sensitizing episode, 250iu given
before 20wks GA and 500iu thereafter.
• Post delivery-
administer anti-D IgG to RhD –ve mother within 72hrs
of delivery of Rh D +ve neonate.
Dose-500iu of anti-D IgG to neutralize 4mls of fetal
red cell.
Increase anti-D dose if there is FMH> 4mls, at 125iu/
mL of FMH > 4mL
ABO HDN
• Commoner than Rh HDN.
• Usually mild
• Usually cause by immune IgG abs in group O
mothers carry group A or B fetus.
• Ist pregnancy may be affected.
• DAT may be –ve or weakly +ve.
• PBF- spherocytosis, polychromasia
• Treatment-phototherapy, EBT in severe
hyperbilirubinaemia.
ABO HDN
Blood film from a neonate with ABO HDN due to anti-A,
showing very large numbers of spherocytes,
polychromasia and no nucleated red cells.
You might also like
- DTC Codes Mercedes CPC4 EnglishDocument24 pagesDTC Codes Mercedes CPC4 Englishjonny david martinez perez100% (1)
- Transfusion Reaction and Coombs Test: Moderator:-Dr Sanjay Agrwal Presenter: - DR Pratima Singh PG Jr-1Document33 pagesTransfusion Reaction and Coombs Test: Moderator:-Dr Sanjay Agrwal Presenter: - DR Pratima Singh PG Jr-1UmikaguptaNo ratings yet
- Introduction to S.G. Iron Casting IndustryDocument30 pagesIntroduction to S.G. Iron Casting Industryavnishchauhan8_46499100% (1)
- Approach and Management of Bleeding NeonateDocument49 pagesApproach and Management of Bleeding NeonateG VenkateshNo ratings yet
- Legalism QuotesDocument14 pagesLegalism QuotesfruittinglesNo ratings yet
- Abo Typing Discrepancies: Rene Jesus Alfredo R. Dinglasan, RMTDocument14 pagesAbo Typing Discrepancies: Rene Jesus Alfredo R. Dinglasan, RMTdirenjan100% (1)
- 7 Adverse Reactions to TransfusionDocument11 pages7 Adverse Reactions to TransfusiondrkamalakarNo ratings yet
- Pediatric Transfusion Risks and GuidelinesDocument57 pagesPediatric Transfusion Risks and GuidelinesDR.RAJESWARI SUBRAMANIYANNo ratings yet
- Transfusion Reaction - DRGSPDocument42 pagesTransfusion Reaction - DRGSPGaurav PawarNo ratings yet
- Blood Transfusion Reactions: Life Saving Yet Life ThreateningDocument52 pagesBlood Transfusion Reactions: Life Saving Yet Life Threateninganam farzand100% (2)
- Adverse Reactions To Blood Transfusion1Document38 pagesAdverse Reactions To Blood Transfusion1Abby Liew100% (1)
- Blood TransfusionDocument55 pagesBlood Transfusionanand7504100% (2)
- Transfusion Medicine and Hemostasis: Clinical and Laboratory AspectsFrom EverandTransfusion Medicine and Hemostasis: Clinical and Laboratory AspectsRating: 4 out of 5 stars4/5 (9)
- Vdocuments - MX Setting Procedure Evs HMF Tech Procedure Evs 11 16pdf Setting ProcedureDocument37 pagesVdocuments - MX Setting Procedure Evs HMF Tech Procedure Evs 11 16pdf Setting ProcedureKrum Kashavarov100% (1)
- Complications of Blood TransfusionDocument18 pagesComplications of Blood TransfusionIqra ghafoorNo ratings yet
- Adverse Blood Reaction and HDNDocument34 pagesAdverse Blood Reaction and HDNAdeniran CharlesNo ratings yet
- HPB Adverse Transfusion ReactionDocument26 pagesHPB Adverse Transfusion ReactionFransiscus RivaldyNo ratings yet
- Blood Transfusion and Its ComplicationsDocument31 pagesBlood Transfusion and Its ComplicationsSaima Hasnain MinhasNo ratings yet
- 5 Transfusion ReactionsDocument20 pages5 Transfusion ReactionsDeladem EmmanuelNo ratings yet
- Blood ProductsDocument70 pagesBlood Productsjadhamade339No ratings yet
- A-Gvhd M.saeedDocument20 pagesA-Gvhd M.saeedaymenNo ratings yet
- Blood Transfusion ReactionsDocument8 pagesBlood Transfusion ReactionsStephanie AngelaNo ratings yet
- Transfusion Medicine by Dr. Sharad JohriDocument54 pagesTransfusion Medicine by Dr. Sharad JohriShashwat JohriNo ratings yet
- Lecture On Blood Groups, Transfusion, RH Incompatibility by Dr. RoomiDocument41 pagesLecture On Blood Groups, Transfusion, RH Incompatibility by Dr. RoomiMudassar Roomi100% (1)
- Blood Transfusion Reaction 3032018Document33 pagesBlood Transfusion Reaction 3032018Kelly YeowNo ratings yet
- Division of Blood Transfusion Services: Ministry of Health and Family WelfareDocument46 pagesDivision of Blood Transfusion Services: Ministry of Health and Family WelfareKirandragonNo ratings yet
- Hematology Transfusion ReactionDocument69 pagesHematology Transfusion ReactionSharmin Nahar NabilaNo ratings yet
- Blood Transfusion Complications & Management (40Document30 pagesBlood Transfusion Complications & Management (40kushalNo ratings yet
- Serious Hazards of Transfusion: DR Kenneth S Charles MB - Bs (Uwi), FRCP (Uk), Frcpath (Uk) Senior Lecturer in HaematologyDocument65 pagesSerious Hazards of Transfusion: DR Kenneth S Charles MB - Bs (Uwi), FRCP (Uk), Frcpath (Uk) Senior Lecturer in HaematologySuneil R AlsNo ratings yet
- 5 Transfusion ReactionsDocument34 pages5 Transfusion ReactionsFuentes, Jade Andrey R. BSMT 2-ANo ratings yet
- Unit - 5 Blood Banking HaematologyDocument82 pagesUnit - 5 Blood Banking HaematologySumit PandyaNo ratings yet
- Session 8Document6 pagesSession 8madcalNo ratings yet
- ICU Blood Transfusion & Electrolytes DisturbanceDocument26 pagesICU Blood Transfusion & Electrolytes Disturbancef6080683No ratings yet
- Adverse Effects: Blood TransfusionDocument43 pagesAdverse Effects: Blood TransfusionDumindu PereraNo ratings yet
- Blood Transfusion Basic Concepts Blood Transfusion inDocument103 pagesBlood Transfusion Basic Concepts Blood Transfusion iniahmad9No ratings yet
- Blood Transfusion Notes..Document9 pagesBlood Transfusion Notes..queenethNo ratings yet
- Adverse Effects of TransfusionDocument5 pagesAdverse Effects of Transfusionlubna aloshibiNo ratings yet
- Adverse Effects of TransfusionDocument5 pagesAdverse Effects of Transfusionlubna aloshibiNo ratings yet
- Adverse Effects of Plasma TherapyDocument80 pagesAdverse Effects of Plasma TherapyShaiji ShahidNo ratings yet
- Transfusion Medicine: DR Abdullah AnsariDocument53 pagesTransfusion Medicine: DR Abdullah AnsariFabsNo ratings yet
- ITP LectureDocument20 pagesITP LectureReza MajidiNo ratings yet
- Blood Transfusion Reactions: Dr. Madhuvan GuptaDocument42 pagesBlood Transfusion Reactions: Dr. Madhuvan GuptaDr. Madhuvan GuptaNo ratings yet
- Blood Transfusion 2Document12 pagesBlood Transfusion 2Helene AlawamiNo ratings yet
- Hemolytic Disease of the Fetus and Newborn (HDFNDocument46 pagesHemolytic Disease of the Fetus and Newborn (HDFNK.M.S. ChathunikaNo ratings yet
- Research questions on blood typing procedures and hemolytic disease of the newborn (HDNDocument3 pagesResearch questions on blood typing procedures and hemolytic disease of the newborn (HDNBrielleNo ratings yet
- Blood Transfusion AlexDocument33 pagesBlood Transfusion AlexaymenNo ratings yet
- Adverse Effects of Blood TransfusionDocument3 pagesAdverse Effects of Blood Transfusionay254No ratings yet
- Blood Transfusion Blood Grouping and Cross MatchingDocument46 pagesBlood Transfusion Blood Grouping and Cross MatchingHa LeemNo ratings yet
- TransfusionDocument48 pagesTransfusionSandy LavedaNo ratings yet
- Essential principles and complications of blood transfusionDocument27 pagesEssential principles and complications of blood transfusionisuhuNo ratings yet
- Adverse Reactions to Transfusion ChapterDocument6 pagesAdverse Reactions to Transfusion ChapterAdina TîrnoveanuNo ratings yet
- Red Cell AlloimmunizationDocument30 pagesRed Cell AlloimmunizationjarssooNo ratings yet
- Transfusion of Blood and Red CellsDocument34 pagesTransfusion of Blood and Red CellsAdams Westlifer SophianoNo ratings yet
- Blood Transfusion ProblemsDocument52 pagesBlood Transfusion ProblemsAulia RahmanNo ratings yet
- 11a. Blood TransfusionDocument28 pages11a. Blood TransfusionMuwanga faizoNo ratings yet
- Surgery Slide 6 - Blood TransfusionsDocument54 pagesSurgery Slide 6 - Blood TransfusionsEman NazzalNo ratings yet
- Local Media4202655613631600684Document6 pagesLocal Media4202655613631600684Haniya KhanNo ratings yet
- Blood Transfusion Guide for Immediate ReactionsDocument8 pagesBlood Transfusion Guide for Immediate ReactionsJohann OrtizNo ratings yet
- Complications of Blood TransfusionsDocument4 pagesComplications of Blood TransfusionsZain Hadi100% (1)
- RJDocument2 pagesRJRj King AstreroNo ratings yet
- Blood Products Indications and Complications GuideDocument40 pagesBlood Products Indications and Complications GuideAzizah AsmarNo ratings yet
- 6.blood Transfusion, Hemostasis & Coagulation DisordersDocument42 pages6.blood Transfusion, Hemostasis & Coagulation DisordersEyouel TadesseNo ratings yet
- Complications of Blood TransfusionDocument15 pagesComplications of Blood TransfusionAdeniran CharlesNo ratings yet
- Cardiovascular Pathology GuideDocument33 pagesCardiovascular Pathology GuideAdeniran CharlesNo ratings yet
- 2020-2021 Practical and Tutorial ScheduleDocument5 pages2020-2021 Practical and Tutorial ScheduleAdeniran CharlesNo ratings yet
- Anxiolytic and Hypnotic Drugs 2Document44 pagesAnxiolytic and Hypnotic Drugs 2Adeniran CharlesNo ratings yet
- Acute Renal Failure: Dr. Sami Abdo RadmanDocument23 pagesAcute Renal Failure: Dr. Sami Abdo RadmanAdeniran CharlesNo ratings yet
- Protein synthesis inhibitor: Tetracyclines inhibit protein synthesisDocument113 pagesProtein synthesis inhibitor: Tetracyclines inhibit protein synthesisAdeniran CharlesNo ratings yet
- The Drawing WebsiteDocument99 pagesThe Drawing WebsiteAdeniran CharlesNo ratings yet
- Cell wall inhibitors cell wall dysfunction mechanismsDocument99 pagesCell wall inhibitors cell wall dysfunction mechanismsAdeniran CharlesNo ratings yet
- Principles of HIV TreatmentDocument67 pagesPrinciples of HIV TreatmentAdeniran CharlesNo ratings yet
- Burkitt's Lymphoma BbcockDocument27 pagesBurkitt's Lymphoma BbcockAdeniran CharlesNo ratings yet
- HAEMATOLOGIC MANIFESTATIONS OF SYSTEMIC DISEASESDocument38 pagesHAEMATOLOGIC MANIFESTATIONS OF SYSTEMIC DISEASESAdeniran CharlesNo ratings yet
- Neuromuscular Pharmacology 305-1Document43 pagesNeuromuscular Pharmacology 305-1Adeniran CharlesNo ratings yet
- Clinical Blood TransfusionDocument13 pagesClinical Blood TransfusionAdeniran CharlesNo ratings yet
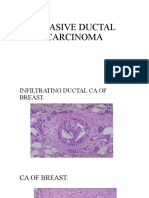
- Invasive Ductal CarcinomaDocument3 pagesInvasive Ductal CarcinomaAdeniran CharlesNo ratings yet
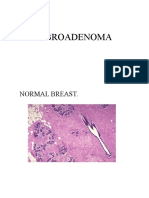
- Fi Bro AdenomaDocument4 pagesFi Bro AdenomaAdeniran CharlesNo ratings yet
- ENGLISH CONTENT UNIT 4 2022 5tos.Document9 pagesENGLISH CONTENT UNIT 4 2022 5tos.Dylan QuiñónezNo ratings yet
- 4 A CompiledDocument167 pages4 A CompiledArjun MiddhaNo ratings yet
- LPC Licensure Process HandbookDocument14 pagesLPC Licensure Process HandbookMac PatelNo ratings yet
- Vergara, Valerie G. Drug Study (Ma'Am Dean)Document3 pagesVergara, Valerie G. Drug Study (Ma'Am Dean)Valerie VergaraNo ratings yet
- Probability Concepts and Random Variable - SMTA1402: Unit - IDocument105 pagesProbability Concepts and Random Variable - SMTA1402: Unit - IVigneshwar SNo ratings yet
- Instruction Manual: Shimadzu Analytical BalanceDocument169 pagesInstruction Manual: Shimadzu Analytical BalanceChanthar SoeNo ratings yet
- 14 Ways To Acquire KnowledgeDocument4 pages14 Ways To Acquire KnowledgeRenato MiguelNo ratings yet
- Excerpts From The Way of The Samurai (Shīdo) : Primary Source Document With Questions (DBQS)Document2 pagesExcerpts From The Way of The Samurai (Shīdo) : Primary Source Document With Questions (DBQS)Valeria MontalvaNo ratings yet
- Timbering Week 5Document22 pagesTimbering Week 5FikaduKitessa0% (1)
- Individualized Learning Program Project Evaluation FormDocument3 pagesIndividualized Learning Program Project Evaluation Formakbisoi1No ratings yet
- SEO-Optimized Title for Document on English Exam QuestionsDocument4 pagesSEO-Optimized Title for Document on English Exam Questionsminh buiNo ratings yet
- AWS Architecture Icons Deck For Light BG 20190729 LegacyDocument111 pagesAWS Architecture Icons Deck For Light BG 20190729 LegacyHenson ChinNo ratings yet
- Power Over Ethernet - Wikipedia, The Free EncyclopediaDocument7 pagesPower Over Ethernet - Wikipedia, The Free EncyclopediaManitNo ratings yet
- Set 177Document599 pagesSet 177adilfarooq25No ratings yet
- Rulings On Healing and RukiyaDocument324 pagesRulings On Healing and RukiyatheproboxerNo ratings yet
- The Role of Human Resource Costs To Achieve Competitive Advantage in The Jordanian Commercial BanksDocument10 pagesThe Role of Human Resource Costs To Achieve Competitive Advantage in The Jordanian Commercial BanksGizachewNo ratings yet
- Unit 5 - Lesson 1 - Understanding Hypothesis TestingDocument31 pagesUnit 5 - Lesson 1 - Understanding Hypothesis TestingJasper A. SANTIAGONo ratings yet
- The Bourne Identity ReviewDocument3 pagesThe Bourne Identity ReviewBoldizsár Zeyk AnnaNo ratings yet
- Ricoh Aficio SP c830dn-c831dn AP-p3 (m124-m125) FSMDocument1,064 pagesRicoh Aficio SP c830dn-c831dn AP-p3 (m124-m125) FSMDương Minh Phụng100% (1)
- Logging Levels in Log4j - Tutorialspoint ExamplesDocument3 pagesLogging Levels in Log4j - Tutorialspoint ExamplesJai PannuNo ratings yet
- Arm Cortex InstructionsDocument14 pagesArm Cortex InstructionsHamsini ShreenivasNo ratings yet
- Structural Stainless Steel Designing With Stainless Steel: Ing. Maarten FortanDocument153 pagesStructural Stainless Steel Designing With Stainless Steel: Ing. Maarten FortanJohn Philip Neri BesedillasNo ratings yet
- Last Lesson: How Did Franz Feelings About M Hamel and School Change ?Document4 pagesLast Lesson: How Did Franz Feelings About M Hamel and School Change ?RitikaNo ratings yet
- ZISCO Installs World LongestDocument11 pagesZISCO Installs World LongestJoshua GrahitaNo ratings yet
- Muhammad Farrukh QAMAR - Assessment 2 Student Practical Demonstration of Tasks AURAMA006 V2Document19 pagesMuhammad Farrukh QAMAR - Assessment 2 Student Practical Demonstration of Tasks AURAMA006 V2Rana Muhammad Ashfaq Khan0% (1)
- Set 1Document24 pagesSet 1TutorTutorNo ratings yet