Professional Documents
Culture Documents
Sodium, Magnesium) : Patella (Makes Quads MM Group FNX
Sodium, Magnesium) : Patella (Makes Quads MM Group FNX
Uploaded by
ALFONSO JAMORA III0 ratings0% found this document useful (0 votes)
17 views4 pagesBone is a living tissue that undergoes constant remodeling through the actions of osteoblasts, osteoclasts, and osteocytes. It has both organic and inorganic components that provide strength and flexibility. There are two main types of bone - cortical bone which is dense and strong, and cancellous bone which is lighter and aids in shock absorption. Fractures heal through the inflammatory, repair, and remodeling phases as the body forms callus and remodels the bone. Successful healing depends on factors like the injury characteristics, patient health, bone type, treatment, and presence of infection or other tissue issues. Smoking significantly impairs healing by reducing blood flow.
Original Description:
Bone Physiology
Original Title
Bone physiology et repair
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentBone is a living tissue that undergoes constant remodeling through the actions of osteoblasts, osteoclasts, and osteocytes. It has both organic and inorganic components that provide strength and flexibility. There are two main types of bone - cortical bone which is dense and strong, and cancellous bone which is lighter and aids in shock absorption. Fractures heal through the inflammatory, repair, and remodeling phases as the body forms callus and remodels the bone. Successful healing depends on factors like the injury characteristics, patient health, bone type, treatment, and presence of infection or other tissue issues. Smoking significantly impairs healing by reducing blood flow.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
17 views4 pagesSodium, Magnesium) : Patella (Makes Quads MM Group FNX
Sodium, Magnesium) : Patella (Makes Quads MM Group FNX
Uploaded by
ALFONSO JAMORA IIIBone is a living tissue that undergoes constant remodeling through the actions of osteoblasts, osteoclasts, and osteocytes. It has both organic and inorganic components that provide strength and flexibility. There are two main types of bone - cortical bone which is dense and strong, and cancellous bone which is lighter and aids in shock absorption. Fractures heal through the inflammatory, repair, and remodeling phases as the body forms callus and remodels the bone. Successful healing depends on factors like the injury characteristics, patient health, bone type, treatment, and presence of infection or other tissue issues. Smoking significantly impairs healing by reducing blood flow.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 4
MIDTERM: REHAB102- MSK (e.g.
Rapid healing in hand compared to the
distal ankle d/t inc blood supply in the hand)
PART I: (eg. Same as pt who smoke, since smoke
BONE PHYSIOLOGY AND REPAIR constricts and impedes blood supply)
- “Bone is a living tissue, goes in the process - Major sources:
of bone turnover” Nutrient artery system
- 10 years to replace the skeletal components Metaphyseal-epiphyseal system
- Rigid connective tissue; has a tensile Periosteal system
strength of a cast iron but 3x lighter and 10x
more flexible and elastic *Periosteum
- extra cellular rigidity (calcium - soft tissue that surrounds the bone
hydroxyapatite), flexibility (collagen fibers) - rich in blood supply
- contains osteoblasts
Function of Bones:
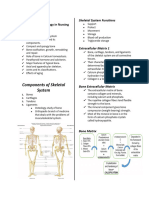
1. Mineral homeostasis BONE TYPES
- (storage of for calcium, phosphorous, 1. Lamellar Bone/ Mature, Normal Bone
sodium, magnesium) Cortical/ Compact Bone (80%)
2. House the hematopoietic (blood-forming) - Strong bone
elements - Slow turnover rate (slower
3. Mechanical Support healing)
4.Determines the attributes of size and - High elasticity
shape - Higher resistance to torsion et
bending
Components: Cancellous/ Trabecular/
Cellular elements (2%) Spongy Bone (20%)
Matrix (98%) - Not as strong
ORGANIC MATRIX - Good for shock absorption
(collagen) - Higher cells; higher turnover rate
INORGANIC MATRIX (rapid healing)
(calcium hydroxyapatite) 2. Woven Bone/ Immature, may be
pathologic bone
Cellular Elements:
OSTEOBLAST BONE CLASSIFICATION BY SHAPE:
- Bone-forming cells a) Long bone (most common)
- Very active during growth or bone b) Short bone
repair c) Flat bone (skull, sternum, pelvis)
OSTEOCYTES d) Irregular bone
- Semi-retired or inactive bone cells e) Sesamoid bone (unsual, embedded
- Bone-maintaining cells. Makes up in a tendon, improves biomechanics
90% of all cellular elements in bone through improving lever arm, biggest
OSTEOCLASTS patella (makes quads mm group fnx better
- Opposite of osteoblast as a knee extensor.
- Breaks down bone (bone remodeling, or
when the body needs extra calcium) *Long bone
- 2 parts; diaphysis et metaphysis
MATRIX: - Diaphysis (body or shaft); abundant in
ORGANIC COMPONENTS (40%) Coritcal bones
Collagen (Type I) - Metaphysis (distally or proximally then
Proteoglycans widens up) (transition zone); Combination of
Noncollagenous matrix protein Cortical and Cancellous bone
INORGANIC COMPONENTS (60%) - Epiphysis end part; abundant in Cancellous
Calcium hydroxyapatite bone
Osteocalcium phosphate
TISSUE SURROUNDING THE BONE:
CIRCULATION 1) BONE MARROW
- Receives 5% to 10% of total cardiac output - Source of progenitor cells
- Major determinant of fracture healing Red marrow - creates the RBC
Palmerola, Duke P. BSPT III GOODMAN CLUSTER A
Yellow marrow - fat and PART 2:
inactive cells FRACTURE REPAIR OR HEALING
2) PERIOSTEUM - “In any living tissue, once it’s injured,
- Connective tissue membrane that covers the body automatically repairs it, same for all
bone soft tissues”
More thicker et highly
developed in children STAGES OF FRACTURE HEALING
Contains cells that are capable I. INFLAMMATION/
of becoming osteoblasts (to INFLAMMATORY PHASE
form bone) - Not always bad, first stage of healing
- 10% of time
- Inflammatory phase, presence of
(Hematoma; which carries protein that
will enhance healing)
BONE FORMATION - *Periosteum (important source of
Types of Bone Formation: Ostroprogenetor cells; cells for healing)
1. Endochondral Bone Formation/ II. REPAIR/ REPARATIVE PHASE
Mineralization - 40 % of time
Primary callus forms within 2
2. Intramembranous Ossification weeks:
- Bridging (soft) callus (little collagen
and calcium hydroxic apatite, soft or
geline phase)
- Woven (hard) callus (hardens due to
calcium deposition)
- Medullary callus
Amount of callus formation
varies with the method of treatment.
III. HEALING/ REMODELING PHASE
- 70% of time
- Begins during the middle of Repair
phase and continues long after the
fracture has healed
- Remodeling allows the bone to
assume its normal configuration and
shape based on its stresses (Wolff’s
Law).
*Osteoclasts starts to remove the
callus, then the bone follows the
pressure applied to it; once the bone
is fixed the body tries to remodel the
bone so that it can adopt to different
stresses
PART 3:
FAILURE IN FRACTURE HEALING
Delayed Union
- The bone did not heal in the
normal amount of time
Malunion
- Complete fracture healing but
the alignment is not optimal
Non-union
- No union; failure of bone
healing
- has 2 types:
HYPERTROPHIC AND ATROPHIC
- Hypertrophic nonunion: Bone
Palmerola, Duke P. BSPT III GOODMAN CLUSTER A
itself has an ability to heal, but - Disorders in parathyroid hormone
because of gross motion, it did not Nicotine
unite. (+) Callus - Very common
- Atrophic nonunion: Impaired bone - Always ask the pt, check for second and
healing (seen in areas like distal tibia, third-hand smoke
smoking pt’s due to constriction) or
infection that limits healing. (-) Callus TISSUE VARIABLE
1. Bone type
VARIABLES IN BONE HEALING: 2. Bone necrosis
1. Injury Variables 3. Bone disease
2. Patient Variables 4. Infection
3. Tissue Variables
4. Treatment Variables BONE TYPE
- What heals better, Cortical bone or
Injury Variables Cancellous bone ? *Cancellous Bone
-”How severe the injury was ?”
- “Where is the injury ?” BONE NECROSIS
Patient Variables - Part of the bone dies
- “Does pt has diabetes ?” - In severe injuries: Bone are hit and
- co-morbidity factors shattered on impact, stripped blood
- (+) smoker supply then dies.
Tissue Variables Bone Disease
- The tissue itself - Vit D deficiency or rickets
Treatment Variables - Osteogenesis imperfecta
- Tx done to the pt Infection
- very common
INJURY VARIABLES: - often associated with atrophic nonunion
1. Open fractures
2. Severity of injury TISSUE VARIABLE
3. Intra-articular fractures 1. Apposition of fracture fragments
4. Segmental fractures 2. Loading and Micromotion
5. Soft-tissue interposition 3. Fracture stabilization
6. Damage to blood supply
Loading and Micromotion
Open fractures - “Micromotion a little bit of motion
- Complicated soft injury since it is open measured via micrometers, very very little
to the environment; high rate of infection motions in the fracture is actually good”
Severity of injury - “Loading a little bit of stress on the
- Serious injury: Periostium layer is stripped fracture is also good”
off, severe lost of blood supply which will - Excessive load plus macromotion, the
result to poor healing. healing process will result not in bone
Intra-articular fractures formation but fibrous tissue formation that
- Fx within joint can lead to pseudogout joint.
- Poor healing due to the synovial fluid that Fracture Stabilization
prevents hematoma formation - Important to stabilize the fracture and
limit macromotion
PATIENT VARABLES - External Fixator or Antenna is used to
1. Age immobilize the fracture until bone heals
2. Nutrition
3. Systemic Hormones METHODS OF PROMOTING
4. Nicotine FRACTURE HEALING:
Good fixation/ immobilization
Age Bone grafting
- Chances for recovery; young>old Bone transport
Nutrition Electrical Fields (Galvanic Currents)
- Well nourished to supply healing Ultrasound
Systemic Hormones
Palmerola, Duke P. BSPT III GOODMAN CLUSTER A
Good fixation/ immobilization
- Stable but not too stable to restrict
micromotion
- Fracture ends must be compressed:
load
Bone grafting
- getting a piece of bone from own body or
a cadaver
Bone transport
Electrical Fields
- Galvanic current: DC currents, put near
the fracture to stimulate healing
Ultrasound
- US creates vibration
Palmerola, Duke P. BSPT III GOODMAN CLUSTER A
You might also like
- Experimental PsychologyDocument70 pagesExperimental PsychologyAmisha MakwanaNo ratings yet
- Bone Healing ProcessDocument21 pagesBone Healing ProcessWing YenNo ratings yet
- Skeletal SystemDocument14 pagesSkeletal SystemCharlize PalmaNo ratings yet
- 1998 - Copper and Zinc in Inflammatory and Degenerative DiseasesDocument198 pages1998 - Copper and Zinc in Inflammatory and Degenerative DiseasesvmarinelliNo ratings yet
- Skeletal and Muscular System - FinalDocument30 pagesSkeletal and Muscular System - Finalastraia celesteNo ratings yet
- Progressive Calisthenics - The 20-Minute Dream Body With Bodyweight Exercises (Calisthenics) (PDFDrive)Document171 pagesProgressive Calisthenics - The 20-Minute Dream Body With Bodyweight Exercises (Calisthenics) (PDFDrive)Erisson S. Dos SantosNo ratings yet
- Skeletal System Functions of The Skeletal System: Human Anatomy & Physiology Kylie Jan C. SilvaDocument15 pagesSkeletal System Functions of The Skeletal System: Human Anatomy & Physiology Kylie Jan C. SilvaKert trocioNo ratings yet
- 31 Plant Hormones-SDocument6 pages31 Plant Hormones-SLeo Ding0% (1)
- Bone HealingDocument5 pagesBone HealingFadliArifNo ratings yet
- Hema FC Part 2 1Document10 pagesHema FC Part 2 1Lynther Myle ArizoNo ratings yet
- Lecture 2 BoneDocument22 pagesLecture 2 BoneiamkpvemuriNo ratings yet
- ANAPHY Lec Session #5 - SAS (Agdana, Nicole Ken)Document9 pagesANAPHY Lec Session #5 - SAS (Agdana, Nicole Ken)Nicole Ken AgdanaNo ratings yet
- Protein Metabolism Questions W - Answers (Biochemistry) (Bio 024)Document3 pagesProtein Metabolism Questions W - Answers (Biochemistry) (Bio 024)Vienna GilmoreNo ratings yet
- Introduction To Pschy - StudocDocument18 pagesIntroduction To Pschy - Studocarvie montemayorNo ratings yet
- ORTHO-Bone Physiology and Repair (Dr. Gerochi)Document4 pagesORTHO-Bone Physiology and Repair (Dr. Gerochi)Monique BorresNo ratings yet
- Skeletal System NotesDocument5 pagesSkeletal System NotesNina IlaganNo ratings yet
- 1.2 Musculoskeletal Disorders PDFDocument10 pages1.2 Musculoskeletal Disorders PDFDiana CalderonNo ratings yet
- Skeletal SystemDocument7 pagesSkeletal Systemopingaangelamae.opingaNo ratings yet
- Skeletal SystemDocument8 pagesSkeletal SystemNo RefundNo ratings yet
- MC I Modular Reviewer Skeletal SystemDocument21 pagesMC I Modular Reviewer Skeletal SystemSteiner LimNo ratings yet
- Skeletal SystemDocument6 pagesSkeletal SystemMikhaella GwenckyNo ratings yet
- AnaPhy Unit 3 Notes ReviewerDocument12 pagesAnaPhy Unit 3 Notes Reviewer쥬얼이No ratings yet
- MS LectureDocument5 pagesMS LectureHershetNo ratings yet
- Chapter 8-BonesDocument1 pageChapter 8-BonesLynNo ratings yet
- Skeletal 6Document28 pagesSkeletal 6BSN-2F Neutral Axis SiazonNo ratings yet
- 6 SkeletalDocument14 pages6 SkeletalprincessstephNo ratings yet
- The Skeletal SystemDocument7 pagesThe Skeletal SystemKathleenJoyGalAlmasinNo ratings yet
- Medsurg 1.0 - GeneralitiesDocument5 pagesMedsurg 1.0 - GeneralitiesDK'S PATATANo ratings yet
- Skeletal SystemDocument14 pagesSkeletal SystemCharlize PalmaNo ratings yet
- Biological Science ReviewsDocument7 pagesBiological Science ReviewsAlibabaNo ratings yet
- C6-Skeletal SystemDocument5 pagesC6-Skeletal SystemLorrine MagramoNo ratings yet
- Skeletal System Chapter 6Document14 pagesSkeletal System Chapter 6Merry Grace CandoNo ratings yet
- Skeletal System LectureDocument28 pagesSkeletal System LectureLittle CloudNo ratings yet
- Skeletal SystemDocument123 pagesSkeletal SystemZekiah MagsayoNo ratings yet
- CHAPTER 6 ANAPHY TransesDocument13 pagesCHAPTER 6 ANAPHY TransesHoly HaeinNo ratings yet
- Teaching Series BoneDocument26 pagesTeaching Series BoneNAND KUMARNo ratings yet
- C5 Skeletal NotesDocument10 pagesC5 Skeletal NotesJocelyn AlunanNo ratings yet
- Table of ContentDocument52 pagesTable of ContentJasvir SinghNo ratings yet
- HAP ReviewerDocument35 pagesHAP Reviewerjennie's gfNo ratings yet
- MODULE 4 Skeletal SystemDocument16 pagesMODULE 4 Skeletal SystemKate Andrea PanizalesNo ratings yet
- WEEK 6-Skeletal SystemDocument15 pagesWEEK 6-Skeletal SystemG a i l R i c h w e l lNo ratings yet
- Tereos - Structure of PresentationDocument72 pagesTereos - Structure of PresentationSumitNo ratings yet
- Skeletal System TransesDocument11 pagesSkeletal System Transesadrielvamos28No ratings yet
- 6 Skeletal SystemDocument8 pages6 Skeletal SystemmargaretNo ratings yet
- 4.2.2. Bone TissueDocument7 pages4.2.2. Bone Tissuealexandra4wineNo ratings yet
- Classifications of Bones: Gross AnatomyDocument6 pagesClassifications of Bones: Gross AnatomyArchie CabacheteNo ratings yet
- Skeletal System Bone and JointsDocument18 pagesSkeletal System Bone and JointsShahina ShayneNo ratings yet
- Bone Tissue and The Skeletal System: (Hyaline) CartilageDocument3 pagesBone Tissue and The Skeletal System: (Hyaline) CartilageMae CanlasNo ratings yet
- Me 471-Bio-Engineering / Bio-Medical Topics: Bone: Prepared ByDocument20 pagesMe 471-Bio-Engineering / Bio-Medical Topics: Bone: Prepared ByehteshamalhanifNo ratings yet
- 09lect Bone Summary2017Document3 pages09lect Bone Summary2017Dan ChoiNo ratings yet
- HistoPath (Lect #5) TransDocument5 pagesHistoPath (Lect #5) TransSherlyn Giban InditaNo ratings yet
- Skeletal System ReviewerDocument19 pagesSkeletal System ReviewerChloe Mikaela MonsantoNo ratings yet
- Skeletal SystemDocument40 pagesSkeletal System119286kinNo ratings yet
- Normal Structure of Bone & Biology of Fracture Healing: Dr. Aashish ChaudhryDocument22 pagesNormal Structure of Bone & Biology of Fracture Healing: Dr. Aashish ChaudhryPankaj VatsaNo ratings yet
- Ringkasan Salter - Chapter 2Document7 pagesRingkasan Salter - Chapter 2Herlangga Fadhillah AkbarNo ratings yet
- Bone Physiology DR NzauDocument84 pagesBone Physiology DR NzauNzau MuangeNo ratings yet
- PhysioDocument14 pagesPhysioEllysa Endrina BatiancilaNo ratings yet
- The Skeletal SystemDocument10 pagesThe Skeletal SystemBeah Marie AlisosoNo ratings yet
- Bones As A Living Dynamic TissueDocument13 pagesBones As A Living Dynamic TissueSanish Basnet100% (1)
- 06 KnightDocument5 pages06 Knightcristina ArraisNo ratings yet
- Musculoskeletal Disorders in ChildrenDocument8 pagesMusculoskeletal Disorders in ChildrenshainakyllebarbonNo ratings yet
- The Skeletal SystemDocument3 pagesThe Skeletal SystemMiguel GumatayNo ratings yet
- 6 PATHO 3b Part 1 - Musculoskeletal IIA - Dr. Dy-LedesmaDocument12 pages6 PATHO 3b Part 1 - Musculoskeletal IIA - Dr. Dy-LedesmaBanana BananaNo ratings yet
- Salter Bab 1-2Document30 pagesSalter Bab 1-2elizabeth angelinaNo ratings yet
- BONEDocument36 pagesBONEdrharmainaNo ratings yet
- Healing of Tooth Extraction Socket: Dr. Pankaj Datta Dr. Shilpa Khullar Dr. Mittal ADocument3 pagesHealing of Tooth Extraction Socket: Dr. Pankaj Datta Dr. Shilpa Khullar Dr. Mittal AwatidinaNo ratings yet
- Biological Nitrogen Fixation: Its Mechanism and Role of Boron in Nitrogen FixationDocument5 pagesBiological Nitrogen Fixation: Its Mechanism and Role of Boron in Nitrogen FixationZorinawmi KhiangteNo ratings yet
- Dekkers, 1995, F. J. J. Buytendijk's Concept of An Anthropological PhysiologyDocument26 pagesDekkers, 1995, F. J. J. Buytendijk's Concept of An Anthropological PhysiologyFilip JarošNo ratings yet
- Key To The Review Question of Absorption by Roots: A. Multiple ChoiceDocument7 pagesKey To The Review Question of Absorption by Roots: A. Multiple ChoiceKriticaNo ratings yet
- PHD Ifergan Ilan 031810245Document141 pagesPHD Ifergan Ilan 031810245api-19799287No ratings yet
- 1.-Introduction To Zoology-HandoutsDocument25 pages1.-Introduction To Zoology-HandoutsKyrby CabalquintoNo ratings yet
- Accuracy in Judgment (AFSHEEN ZEHRA)Document11 pagesAccuracy in Judgment (AFSHEEN ZEHRA)Afsheen Zehra100% (2)
- Digestion ResonanceDocument52 pagesDigestion ResonanceEkta ManglaniNo ratings yet
- Bio 2 Icse 10Document5 pagesBio 2 Icse 10neelam luktukeNo ratings yet
- Daftar Pustaka: Disease. Williams & Wilkins, BaltimoreDocument7 pagesDaftar Pustaka: Disease. Williams & Wilkins, BaltimoreHelda SeptivanyNo ratings yet
- Download pdf The Language Of Medicine 11Th Edition Davi Ellen Chabner ebook full chapterDocument53 pagesDownload pdf The Language Of Medicine 11Th Edition Davi Ellen Chabner ebook full chaptersara.gleim919No ratings yet
- Latihan Kelas9Document12 pagesLatihan Kelas9Afrijal DahrinNo ratings yet
- Chapter 5Document55 pagesChapter 5naynes.ariannenicoleNo ratings yet
- Gettingto Know Plants BookDocument14 pagesGettingto Know Plants BookSOMEONE OUT Of your knowledgeNo ratings yet
- Animal Cell Coloring RevisedDocument2 pagesAnimal Cell Coloring RevisedjosieA_123No ratings yet
- Francisco, Ma. Theresa Q. 1bsn-Ui (Session 19-Lec)Document5 pagesFrancisco, Ma. Theresa Q. 1bsn-Ui (Session 19-Lec)DANICA JEAN PRIANES100% (1)
- Biomedical Engineering Vocabulary Revision ExercisesDocument5 pagesBiomedical Engineering Vocabulary Revision ExercisesKasia ManżukNo ratings yet
- Animal KingdomDocument5 pagesAnimal KingdomArthav KumarNo ratings yet
- Blood Grouping 12thDocument17 pagesBlood Grouping 12thPranjal SharmaNo ratings yet
- Notes For Chapter 4Document15 pagesNotes For Chapter 4joeNo ratings yet
- 01 Introduction To HistologyDocument60 pages01 Introduction To HistologyMartha Orendu Oche AttahNo ratings yet
- Hepatic Critical Care: EditorsDocument312 pagesHepatic Critical Care: EditorsAhmed HegazyNo ratings yet
- General Biology 2122 Week 1-10Document7 pagesGeneral Biology 2122 Week 1-10Piei CornerNo ratings yet
- 296 2020 Article 4636Document12 pages296 2020 Article 4636thiago_eliseuNo ratings yet