Professional Documents
Culture Documents
Cardiovascular Disorder
Uploaded by
gwyneth guintuOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Cardiovascular Disorder
Uploaded by
gwyneth guintuCopyright:
Available Formats
CARDIOVASCULAR DISORDER
OUTLINE
THE HEART
I Anatomy and Physiology of the Heart • A muscular pump that pushes blood into the arterial system
II Diagnostic Test and receives blood from the venous system.
III Assessment
• Location:
IV Disease of the Cardiovascular System
i. Coronary Artery Diseases o Thorax; between the lungs
i.i Angina Pectoris • Pointed apex directed toward left hip
i.ii Myocardial Infarction
ii. Congestive Heart Failure
o Size: about the size of your fist
iii. Heart Muscle Disease o Less than 1 lb.
iv. Inflammatory Disease of the Heart
v. Dysrhythmias
The Cardiovascular System
• A closed system of the heart and blood vessels
• The heart pumps blood
• Blood vessels allow blood to circulate to all parts of the
body
• Functions
o Circulation of blood
o Delivery of oxygen and other nutrients
o Removal of carbon dioxide and other products of
cellular metabolism
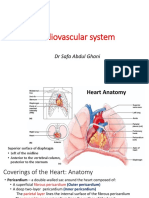
THE HEART COVERINGS
• Pericardium – a thin membrane (fibroelastic sac)
composed of 2 layers that separate the heart from
surrounding structures.
o Visceral pericardium - next to heart
o Parietal pericardium - outside layer
• Serous fluid fills the space between the layers of
pericardium
THE HEART WALL
• Three layers:
• Epicardium
o Outside layer, continuous with the visceral
pericardium
o Connective tissue layer- support, protect and give
structure
• Myocardium
o Middle layer, mostly cardiac muscle
• Organs of the Cardiovascular System
• Endocardium
o Heart
o Inner layer
o Blood Vessels
• Endothelium – thin membrane that lines inside of the heart
▪ Arteries
and blood vessels
- Arterioles THE HEART CHAMBERS
- Capillaries • Right and left side act as separate pumps
▪ Veins • Four chambers:
- Venules o Atria
- Receiving chambers
Michaella Canlas, 3BSN 1
CARDIOVASCULAR DISORDERS
▪ Right Atrium
▪ Left Atrium
• Ventricles THE HEART CONDUCTION SYSTEM
- Discharging chambers • Special tissue sets the pace.
▪ Right Ventricle o Sinoatrial node (right atrium)- “Pacemaker”
▪ Left Ventricle o Atrioventricular node (junction of R & L atria and
ventricles)
THE HEART VALVES
o Atrioventricular bundle (Bundle of His)
• Allow blood to flow in only one direction
o Bundle branches (right and left)
• Four valves
• Atrioventricular valves – between atria and ventricles o Purkinje fibers
o Bicuspid (mitral) valve - (left)
o Tricuspid valve - (right)
• Semilunar valves - between ventricle and artery
o Pulmonary semilunar valve
o Aortic semilunar valve
• Valves open as blood is pumped through
• Held in place by chordae tendineae (“heart strings”)
• Close to prevent backflow.
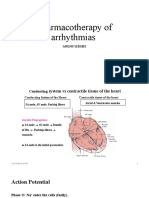
• SINO ATRIAL NODE (SA)
o Initiates the cardiac impulse which spreads across the
atria and into AV node
• ATRIOVENTRICULAR (AV) NODE
o Delays the impulse from the atria while the ventricles
fill
• BUNDLE OF HIS
Functions of ATRIOVENTRICULAR VALVES o RIGHT BUNDLE BRANCH: transmit impulses down
• Permit the unidirectional flow of blood from specific atrium the right side of the interventricular septum toward the
to specific ventricle during ventricular diastole. right ventricular myocardium
o LEFT BUNDLE BRANCH: divided into anterior and
• Prevent reflux flow during ventricular systole
posterior; transmit impulses to the left side of the heart
• The valve leaflets open during ventricular diastole and close
• PURKINJE FIBERS
during ventricular systole
o Transmit impulses to the ventricles and provide for
• The first heart sound (S1, "lub") is due to the closing AV
depolarization after ventricular contraction
valves and associated blood turbulence.
ELECTROCARDIOGRAMS (EKG/ECG)
Functions of SEMI LUNAR VALVES
• Three formations
• Permit unidirectional flow of blood from specific ventricle to
o P wave: impulse
arterial vessel during ventricular systole
across atria
• prevent reflux blood flow during ventricular diastole o QRS complex:
• Valves open when ventricles contract and close during spread of impulse
ventricular diastole down septum,
• The second heart sound (S2, "dup") occurs when the around ventricles
semilunar (aortic and pulmonary) valves close. in Purkinje fibers
• S2 is normally split because the aortic valve closes slightly o T wave: end of
earlier than the pulmonary valve. electrical activity in
ventricles
Michaella M. Canlas 3BSN 2
CARDIOVASCULAR DISORDERS
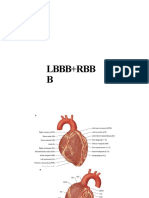
THE HEART AND THE GREAT BLOOD VESSELS • Exercise
• Aorta --Leaves the left ventricle • Decreased blood volume
o The main trunk of the systemic arteries, carrying blood • Decreased heart rate
from the left side of the heart to the arteries of all limbs o Parasympathetic Nervous System
and organs. ▪ High blood pressure or high blood volume
• Pulmonary artery-- Leaves the right ventricle ▪ Decreased venous return
o carries blood to lungs ▪ In congestive heart failure, the heart is worn out and
• Vena cava (Superior and Inferior) -- Enter the right atrium pumps weakly
• Pulmonary veins (four) -- Enter left atrium ▪ Digitalis works to provide slow, steady but
THE CARDIAC CYCLE ▪ Stronger beat
• Atria contract simultaneously • Non-invasive test that produces a graphic record of the
• Atria relax, then ventricles contract electrical activity of the heart
• Systole = contraction • HOLTER MONITOR
• Diastole = relaxation o Portable recorder provides continuous recording of
ECG for up to 24 hours
Filling of Heart Chambers –
EXERCISE ECG (STRESS TEST)
the Cardiac Cycle
• Stress test may show heart disease when resting ECG does
not
ECHOCARDIOGRAM
• Noninvasive recording of the cardiac structures using
ultrasound
• TYPES
o Resting Surface Echocardiogram
o Transesophageal Echocardiogram
NURSING RESPONSIBILITIES
• Resting Surface Echocardiogram
o No food/drinks restriction
o Ask the patient to remain still
• Transesophageal Echocardiogram
o No food/drinks 4-6 hours before the procedure
THE CARDIAC OUTPUT o Assess for any GI problems
• Cardiac Output (CO) is the amount of blood the heart o Assess for risk for aspiration
pumps from each ventricle per minute. It is usually o VS are monitored during and after the procedure
expressed in litres per minute (L/min). o Eating and drinking may be resumed after gag reflex
• Stroke volume -The amount of blood pumped by the heart returned
per cardiac cycle. It is measured in ml/beat. CARDIAC CATHETERIZATION OR
• Normal range of SV is 50-100ml ANGIOGRAPHY
• CO = HR x SV • Invasive, but often definitive test for diagnosis of cardiac
• CO = 75 beats/min x 70 ml/beat disease
• CO = 5250 ml/min • Visualization of the heart and its structures
• Normal CO = 4-8L/min • PURPOSE
o To evaluate blockage of coronary arteries
• Entire blood supply passes through body once per minute.
o To evaluate functions of heart valves and other
• CO varies with demands of the body.
structures
• Stroke volume usually remains relatively constant o To assess coronary circulation and over all heart
• Starling’s law of the heart – the more that the cardiac function
muscle is stretched, the stronger the contraction NURSING RESPONSIBILITIES
• Changing heart rate is the most common way to change
• Informed consent
cardiac output
REGULATION OF HEART RATE • Assess for allergies, baseline data
• Increased heart rate: • No food/drinks prior to procedure
o Sympathetic nervous system – preparing the body for: • Remove all metal objects/jewelry
o Crisis • A hot, flushing sensation is expected.
o Low blood pressure • Ask patient to hold his/her breath as the dye travels to heart
• Hormones and lungs
o Epinephrine • Monitor Cardiac rhythm
o Thyroxine • Assess for bleeding after the procedure
Michaella M. Canlas 3BSN 3
CARDIOVASCULAR DISORDERS
• Check peripheral pulses; keep affected extremity immobile o Heart sounds
o S1
ASSESSMENT o S2
SUBJECTIVE DATA o S3-associated with ventricular problems
HEALTH HISTORY o S4- associated with atrial contractions
• Presenting Problem • Murmurs – auditory vibrations that varies in loudness,
• Nonspecific symptoms may include pitch and duration of sound (harsh, blowing, hissing,
o Fatigue musical)
o Cough
o headache
o syncope
o Dizziness
o anorexia
o Shortness of breath
o Palpitations
o Weight loss/gain
o Difficulty sleeping
• Specific signs and symptoms
o chest pain
o dyspnea (shortness of breath)
o orthopnea / paroxysmal nocturnal dyspnea
o palpitations: precipitating factors
o edema
o cyanosis
LIFESTYLE
• occupation,
• hobbies, RISK FACTORS
• financial status, • Non-modifiable
• stressors, exercise, o Age
• smoking, o Race
• living conditions o Gender
Use of medications Modifiable Risk Factors
• over the counter drugs, o HYPERLIPIDEMIA
o Cholesterol - ≤ 200mg/dl
• contraceptives,
▪ LDL - ≤ 100mg/dl
• cardiac drugs
Personality profile ▪ HDL - > 60 mg/dl
o Triglycerides - ≤ 150 mg/dl
• Type A,
• HYPERTENSION
• manic-depressive,
o Causes shearing force injury to the arterial wall
• anxieties
o Enhances lipid infiltration and calcium accumulation
Nutrition
• dietary habits,
• cholesterol,
• salt intake,
• alcohol consumption
Past medical history
Family history
OBJECTIVE DATA
• Inspection
o Color
o Posture
o Breathing Pattern
o Sores/Ulceration
• Palpation/Inspection
o Apical Pulse
o Pulsation-extremities
• Auscultation
• CIGARETTE SMOKING
Michaella M. Canlas 3BSN 4
CARDIOVASCULAR DISORDERS
o Increases the risk of dying from CAD by 200 to 400 ANGINA PECTORIS
percent and is proportional to the number of cigarettes • transient, paroxysmal chest pain produced by insufficient
smoked per day. blood flow to the myocardium resulting in myocardial
o The irritant effects of cigarette promotes ischemia
atherosclerotic changes • Types:
• Diabetes Mellitus o Stable angina
o Promotes atherogenesis
o Unstable angina
• Physical Inactivity Stable Angina
• Obesity
• Other risk factors • Most common form. Chronic stenosing coronary
atherosclerosis, reaching a critical level, leaving the heart
vulnerable to increased demand.
o Low daily fruit and vegetable intake • Typically relieved by rest or a vasodilator
o Alcohol consumption • Pattern here is the pain occurs with progressively
o Psychosocial index - chronically stressful life, social increasing frequency and tends to be more prolonged
isolation, anxiety and depression • Associated with disruption of the atherosclerotic plaque,
NON-MODIFIABLE FACTORS with superimposed thrombosis, embolisation or spasm.
• Age: Simply getting old is a risk factor for cardiovascular • Predictor of Myocardial Infarction
disease; risk of stroke doubles every decade after age 55. Unstable Angina
• Gender: Men are at greater risk of heart disease than a pre- • Unstable angina is when symptoms of chest pressure,
menopausal woman. But once past the menopause, a shortness of breath occur for the first time, or have been
woman’s risk is similar to a man’s. Risk of stroke is similar happening for less that two weeks
for men and women. • can happen anytime like taking a nap or having a cup of
• Ethnicity: People with African or Asian ancestry are at coffee.
higher risks of developing cardiovascular disease than • may feel different than the pain or discomfort of stable
other racial groups. angina.
CARDIAC DISORDER • is more painful or severe and lasts longer than stable
angina—more than a few minutes.
CORONARY ARTERY DISEASE (CAD) • may not go away with rest or use of angina medication.
• refers to a variety of pathology that cause narrowing or Precipitating Factors
obstruction of the coronary arteries, resulting in decreased
• physical exertion - sexual activity
blood supply to the myocardium
• strong emotions
• major causative factor: Atherosclerosis
• cigarette smoking
• bet 30-50 y.o., men>women
• consumption of a heavy meal
• may manifest as angina pectoris or MI
PATHOPHYSIOLOGY • extremely cold weather
Assessment findings
• Injury to endothelial lining
• Pain: substernal
• Allows entry of lipids
• palpitations, tachycardia, dyspnea, diaphoresis
• LDL particles recruit monocytes and stimulate the release
of inflammatory mediators Diagnostic tests:
• Monocytes act as macrophages • 12- lead ECG - ST segment depression/T-wave inversion
• Ingest LDL in large quantities during chest pain
• Engorged lipid laden macrophages (foam cells) • Holter monitor
• Formed to a fatty streak • Stress ECG/Echocardiogram
• progress to fibrous plaques • Pharmacologic stress test
• Increase in size • Nuclear scans – injection of radioactive agent following an
exercise or stress test; repeated after 24 hours
• Artery may become occluded
• Coronary angiography
MANAGEMENT GOALS
• To improve quality of life by decreasing episodes of angina
and ischemia.
o Relieve acute pain and restore coronary blood flow
o Prevent further attack
• To increase quantity of life by preventing progression to MI
and death
PHARMACOLOGIC MANAGEMENT
• Drugs that decrease the workload of the heart and increase
myocardial perfusion
o Nitrates – increases blood flow and oxygen to the
myocardium
Michaella M. Canlas 3BSN 5
CARDIOVASCULAR DISORDERS
o Isosorbide Dinitrate (ISORDIL, SORBITRATE) o 1st 20 min critical
▪ Nitrogylcerin o 48 hrs inflammation begins to subside
▪ Nitroglycerin Ointment (NITRO-BID, NITROL) o 7th day necrosis area replaced by fibrous tissue
▪ Nitroglycerin Trandermal (NITRO-DUR; o 6-8 weeks scar forms
TRANSDERM-NITRO)
o Beta blockers – decreases the force of myocardial
contraction and slows the heart rate
• Beta blockers – decreases the force of myocardial
contraction and slows the heart rate
• acebutolol, atenolol, betaxolol, bisoprolol, metoprolol,
nadolol, nebivolol, pindolol, propranolol, and timolol
• Calcium channel blockers - blocks influx of calcium and
causes vasodilation; decreasing force of myocardial
contraction and slows the heart rate
o Amlodipine (NORVASC)
o Nefidipine (PROCARDIA)
o Verapamil (CALAN, ISOPTIN)
• Drugs that prevent MI and death
o Aspirin – inhibits platelet aggregation
o ACE inhibitors – Angiotensin-converting enzyme
(ACE) inhibitor ASSESSMENT FINDINGS
o promote endothelial vasodilation; reduce myocardial
• Pain same as in angina, crushing, viselike with sudden
oxygen demand
onset;
o Ex: Captopril,Enalapril, Ramipril, Quinapril, Lisinopril
• nausea/vomiting, dyspnea
o Statins – lower lipid levels, lower inflammatory
• skin: cool, clammy, ashen
markers, stabilize atherosclerotic plaques.
▪ atorvastatin (Lipitor) • elevated temperature
▪ fluvastatin (Lescol) • initial increase in BP and pulse, with gradual drop in
BP
▪ lovastatin (Mevacor, Altocor)
• Restlessness
▪ pravastatin (Pravachol)
Diagnostic tests
▪ pitavastatin (Livalo)
▪ simvastatin (Zocor) • ECG
▪ rosuvastatin (Crestor) • Serum Cardiac Markers – released into blood from necrotic
PATIENT AND FAMILY TEACHING heart muscles after an ischemic event
o Creatine Kinase (CK) MB
• Medications
o Troponin – highly specific indicators of cardiac
• Risk factors modifications damage
• Compliance to treatment • Echocardiography
MYOCARDIAL INFARCTION Management
• General information:
• Rest, oxygen therapy, morphine
o death of myocardial cells
• Anticoagulant
o formation of necrosis (tissue destruction)
• Drugs
PATHOPHYSIOLOGY
• Cardiac rehabilitation
• Coronary artery completely obstructed
• Prognosis depends on site/size of infarct, presence of
o Prolonged ischemia and cell death of myocardium collateral circulation, time elapsed before treatment
• Most common cause is atherosclerosis with thrombus • Mortality rate in 1st year
• 3 ways it may develop o 30-40% due to complications, recurrences
o Thrombus obstruct artery PERCUTANEOUS CORONARY INTERVENTION
o Vasospasm due to partial occlusion
• Advantages
o Embolus blocks small branch of coronary artery
o Low mortality and morbidity
• Majority involve anterior wall of the left ventricle
o Minimal discomfort
o Size and location of infarction determine severity of
o Short hospital stay
damage.
• Function of myocardium contraction and conduction quickly o Short recovery time
lost o Early return to work
o Oxygen supplies depleted DIAGNOSTIC PROCEDURE
o 1st 20 minutes critical – irreversible injury occurs within Percutaneous transluminal coronary
20-40 minutes angioplasty (PTCA)
• Time Line • General information:
Michaella M. Canlas 3BSN 6
CARDIOVASCULAR DISORDERS
o PTCA can be performed in various clients with
single vessel CAD.
o Aim: revascularize the myocardium
▪ decrease angina – increase survival
o a balloon tipped catheter is inserted into the stenotic,
diseased coronary artery.
DIRECTIONAL CORONARY ATHERECTOMY
• Reduces coronary stenosis by excising and removing
atheromatous plaque.
• Nursing interventions: preoperative
o Informed consent
o NPO 8-12 hours prior
o Reassure availability of pain medications
• Nursing interventions: post-operative
o Maintain patent airway
INTRACORONARY STENTS o Promote lung re-expansion
o Monitor cardiac status
• To reduce restenosis and abrupt closure of coronary
vessels resulting from complications of coronary o Maintain fluid and electrolyte balance
angioplasty. o Maintain adequate cerebral circulation
• PRE OP o provide pain relief
o Antiplatelet medication o Provide client teaching and discharge planning
o Calcium blockers concerning:
o Blood typing and cross matching a) Limitation with progressive increase in
activities
o Informed consent
▪ avoid driving for 4-6 weeks
• Post OP
▪ avoid sitting behind an airbag when riding a vehicle
o Monitoring for changes in vital signs/ECG
▪ avoid sitting on the front seat of the car
o Monitor for puncture site
▪ avoid taking a hot water bath
o Distal circulation evaluation
▪ sexual activity may be resumed once the patient can
• DISCHARGE TEACHING climb 2 flights of stairs without chest pain
o Compliance to antiplatelet therapy in long term b) Modify lifestyle
CABG- Coronary artery bypass grafting
• General information:
o A procedure to bypass a blocked section of coronary CONGESTIVE HEART FAILURE
artery and to deliver oxygen to the heart • Cardiac decompensation
o surgery of choice for clients with severe CAD • Cardiac insufficiency
o Procedure requires use of extracorporeal circulation. • Ventricular failure
GENERAL INFORMATION
• Inability of the heart to pump an adequate supply of
blood to meet the metabolic needs of the body
• can be acute or chronic
• Results from
o Problem in heart itself
o Increased demands placed on heart
o Combination of both
• One side usually fails first
ETIOLOGY
Michaella M. Canlas 3BSN 7
CARDIOVASCULAR DISORDERS
• Causes of failure on affected side: • Caused by:
o Infarction that impairs pumping ability or efficiency of o left ventricular damage (MI, CAD)
conduction system o hypertension, aortic valve disease
o Valve defects • Assessment findings:
o Congenital heart defects o shortness of breath/dyspnea
o Coronary artery disease o orthopnea
• Increased demands on heart cause failure o palpitations
o Depends on ventricle most adversely affected o cough, hemoptysis
o Ex: Hypertension increases diastolic bp o fatigue, weakness, syncope
▪ Requires L ventricle to contract more forcibly to open o heart murmurs, extra heart sound
aortic valve o lung crackles
o Ex: Pulmonary disease
• Diagnostic tests:
▪ Damages lung capillaries, increases pulmonary
o ECG, echocardiography, chest x-ray (cardiomegaly,
resistance
pleural effusion)
▪ Increase work load to R ventricle
o stress test
PATHOPHYSIOLOGY
o ABG
• 1st compensation mechanism to maintain CO RIGHT SIDED HEART FAILURE
o Often aggravates instead of assists • Weakened RV is unable to pump blood into the pulmonary
o Decreased flow to systemic circulation causes; system
▪ Kidney increase renin, aldosterone secretion • Caused by:
▪ Vasoconstriction (increase afterload) and increased o Left Sided heart failure
blood volume (increased preload) = increased work o RV Infacrtion
load for heart o Atherosclerotic heart disease
• SNS increases heart function and peripheral resistance o COPD, pulmonic stenosis
• Dilatation of heart chambers, myocardium, hypertrophies o Pulmonary embolism
• 2nd effect when heart cannot maintain pumping capability: • Assessment findings:
o Decrease in CO or SV o peripheral edema - ankle
▪ “forward effect” – refers to the problems of o enlarged liver/hepatomegaly
inadequate perfusion/tissue hypoxia – weakness, o weight gain
restlessness, mental confusion o jugular vein distention
▪ “backward effect” – refers to venous congestion o increased CVP
arising from damming of blood behind the failing o ascites
chamber • Diagnostic tests:
o ECG, echocardiography, chest x-ray, ABG
MANAGEMENT
• Improve ventricular pump performance
o supplemental oxygen
o digitalis (Digoxin, Lanoxin) –
▪ Has positive inotropic effect(increases the force of
contraction)leading to better tissue perfusion
▪ Has diuretic effect
▪ Has negative chronotropic effect – decreases heart
rate (do not give if HR is less than 60/minute)
▪ Has cumulative effect – can cause toxicity as
manifested by abdominal cramps nausea and
vomiting, headache, bradycardia, flickering flashes of
light.
• Reduce workload of the heart
o vasodilators – to reduce afterload
o Diuretics – to reduce preload
o Positioning – semi-Fowler’s to reduce pulmonary
TYPES congestion
• Reduce stress and risk of injury
• Left Sided heart failure
• Collaborative management –
• Right sided heart failure
o Dietary management – low sodium (2-3gms/day),
LEFT SIDED HEART FAILURE o Avoid excessive fluid intake
• Left ventricular damage causes blood to back up through • Afterload describes the resistance that the heart has to
the left atrium and into the pulmonary veins. overcome, during every beat, to send blood into the aorta.
These resistive forces include vasoactivity and blood
viscosity.
Michaella M. Canlas 3BSN 8
CARDIOVASCULAR DISORDERS
• Preload: CLINICAL MANIFESTATION
o Preload occurs during diastole. It is the combination of • Shortness of breath
pulmonary blood filling the atria and the stretching of
• Dependent edema
myocardial fibers. Preload is regulated by the variability
in intravascular volume. • Chest pain, palpitations
• Lightheadedness, fatigue
PLANNING AND IMPLEMENTATION
HEART MUSCLE DISEASES • Minimizing symptoms
CARDIOMYOPATHY • Emotional/psychological support
• a problem with the physical shape of the muscle • Lifestyle modification
• Origin is unknown • Pharmacologic management: ACEIs, Diuretics,
• heart muscle is unable to function correctly resulting to an Anticoagulants, Betablockers, Anti arrhythmics,
impaired cardiac output and increased workload of the INFLAMMATION DYSFUNCTION (carditis)
heart. ENDOCARDITIS
• Four types of Cardiomyopathy:
DILATED CARDIOMYOPATHY • GENERAL INFORMATION
• Dilated heart chamber resulting to a decreased ability of the • Inflammation of the heart’s inner lining
heart to pump strongly and forcefully.
• caused by bacterial infection:
HYPERTROPHIC CARDIOMYOPATHY
• Precipitating factors: medical procedure
• Increase in the size and thickness of the heart muscle
resulting to a decrease blood volume in the heart’s
chambers.
ARRHYTHMOGENIC RIGHT Ventricular
CARDIOMYOPATHY
• The heart muscle is replaced by fibrous scar and fatty tissue
leading to alteration in the heart’s ability to effectively pump.
RESTRICTIVE CARDIOMYOPATHY
• The ventricular muscle walls become stiff, but not
necessarily thickened resulting to ineffective myocardial
contraction.
ASSESSMENT FINDINGS
• Vague signs and symptoms of infection
• murmurs
• Janeway lesions
• Roth’s spots
Michaella M. Canlas 3BSN 9
CARDIOVASCULAR DISORDERS
• petechiae - – are pinpoint round spots that appear on the PERICARDITIS
skin as a result of bleeding • General Info:
• fingertips may become enlarged, clubbing of nails o An inflammation of the visceral and parietal
• Janeway lesions – are non-tender, small erythematous or pericardium
haemorrhagic macular or nodular lesions on the palms or o caused by bacterial, viral, or fungal infection;
soles only a few millimeters in diameter that are indicative trauma
of infective endocarditis
• Assessment
o chest pain
o fever, dyspnea and abdominal pain
o Beck’s triad - signs of low arterial blood pressure,
distended neck veins, and distant, muffled heart
sounds.
CARDIAC TAMPONADE
• BECKS TRIAD
o Distant Heart Sounds
o Distended jugular veins
o Decreased arterial pressure
• Roth’s spots – are retinal hemorrhages with white or pale
centers composed of coagulated fibrinogens. DIAGNOSTICS
• Blood culture
• Imaging studies
• NURSING DIAGNOSIS
MANAGEMENT
• Prevent systemic infection
• Eradication of microorganism
• Reduce cardiac workload
• Assess complications (HF, embolism, increased infection)
• Pharmacology
• Surgery if necessary
MYOCARDITIS
• General Info: an acute or chronic inflammation of the
myocardium as a result of systemic infection, radiation, or
toxic agents
o cause dilation of the heart and degeneration of the
muscle fibers
• Assessment:
o fever, dyspnea, palpitations, chest discomfort
o heart murmurs
CARDIAC TAMPONADE
• Life-threatening complication caused by accumulation of
fluid in the pericardium.
• Compresses the heart and restrict blood flow in and out of
the ventricles.
• Assessment:
o Hypotension, tachycardia, jugular vein distention,
cyanosis of lips and nails, dyspnea, muffled heart
sound, diaphoresis
• Management: Pericardiocentesis – fluid or air is
aspirated from the pericardial space
Michaella M. Canlas 3BSN 10
CARDIOVASCULAR DISORDERS
SINUS BRADYCARDIA
• A heart rate <60bpm
• Caused by:
o pain
o increased intra cranial pressure
o hypothermia
o drugs
• symptoms: decreased cardiac output, decreased
• LOC, syncope, hypotension
Arrhythmia
• (also called dysrhythmia)
• A disturbance or irregularity in the electrical system of the
heart
• An irregular or abnormal heartbeat. ATRIAL FLUTTER
• may be benign or life threatening • a very rapid and regular atrial rhythm.
• Arrhythmias can be caused by:
• caused by: anxiety, caffeine, alcohol intake, thyrotoxicosis
o Coronary artery disease
• manifested by: fluttering sensation in the chest or throat,
o High blood pressure decreased LOC, hypotension, decreased urinary output,
o Changes in the heart muscle (cardiomyopathy) cool and clammy skin
o Valve disorders
o Electrolyte imbalances in the blood, such as sodium or
potassium
o Injury from a heart attack
o The healing process after heart surgery
o Other medical conditions
DYSRHYTHMIAS
• Types accdg to sites:
SUPRAVENTRICULAR RHYTHMS (QRS remains
normal)
SINUS TACHYCARDIA
o A heart rate of over 100.
o can be caused by anxiety, pain, fever, hypoxia,
hyperthyroidism, caffeine and drugs
ATRIAL FIBRILLATION
• characterized by disorganized atrial activity
• manifestations
o irregular pulses of variable strength, hypotension,
shortness of breath, fatigue and angina
Michaella M. Canlas 3BSN 11
CARDIOVASCULAR DISORDERS
VENTRICULAR DYSRHYTHMIAS (wide,bizarre, QRS
complex)
PREMATURE VENTRICULAR CONTRACTIONS
• occur before the next expected beat of the normal rhythm
• triggered by: anxiety, stress, tobacco, alcohol, caffeine.
VENTRICULAR FIBRILLATION
• extremely rapid, chaotic ventricular depolarization that
causes the ventricles to quiver and stop contracting.
• Unconscious
o Unresponsive
o No breathing
o Looks terribly sick and discolored
• triggered by: MI or angina
VENTRICULAR TACHYCARDIA
• three or more consecutive PVCs. rate is greater than
100bpm, rhythm is usually regular.
• Caused by: MI, angina
• Manifested by: fluttering in the chest, palpitations, and brief
shortness of breath
• Sustained VT is a medical emergency
ATRIOVENTRICULAR CONDUCTION BLOCKS
FIRST-DEGREE AV BLOCK
• benign conduction delay that poses no immediate threat
and requires no treatment
• characterized by prolonged PR interval
• caused by: MI, digitalis therapy, chronic heart disease
Michaella M. Canlas 3BSN 12
CARDIOVASCULAR DISORDERS
COLLABORATIVE CARE
• DIAGNOSTIC TESTS
• CARDIAC MONITORING
o Continuous cardiac monitoring
o Portable cardiac monitoring
CARDIOVERSION
• a procedure in which an electric current is used to reset the
heart's rhythm back to its regular pattern (normal sinus
rhythm).
• The low-voltage electric current enters the body through
metal paddles or patches applied to the chest wall.
• Cardioversion is used:
o To stop atrial fibrillation that has not stopped on its
own or after a trial of antiarrhythmic medicines has
failed.
o As an emergency procedure to correct
Supraventricular tachycardia that is causing low
blood pressure, chest pain, or heart failure.
Automatic Implantable Cardioverter
Defibrillator (AICD)
• A sophisticated electronic device used primarily to treat
ventricular tachycardia and ventricular fibrillation — two life-
threatening abnormal heart rhythms.
• The ICD constantly monitors the heart rhythm and
automatically delivers an electric shock to convert the
rhythm back into a normal rhythm
• Types:
o Antitachycardia pacing,
SECOND-DEGREE AV BLOCK o Cardioversion, Defibrillation, Antibradycardia pacing
• some atrial impulses are totally blocked in the AV node. Ventricular fibrillation
• Mobitz I – characterized by a repeating pattern in which PR • Defibrillation -countershock)– is the delivery of an
intervals become progressively longer electrical current to the heart through the use of a
defibrillator.
PACEMAKER
• A device that sends small electrical impulses to the heart
muscle to maintain a normal heart rate.
o Used to treat AV blocks.
o Can be permanent or temporary
• The pacemaker has a pulse generator (which houses a
battery and a tiny computer) and leads (wires) that send
impulses from the pulse generator to the heart muscle, as
well as sense the heart’s electrical activity.
THIRD-DEGREE AV BLOCK
MEDICATIONS
• Occurs when the atrial impulses are completely blocked at • ANTIARRHYTHMIC: These drugs either suppress the
the AV node and not conducted to the ventricles. abnormal firing of pacemaker tissue or depress the
• Caused by: acute MI, electrolyte imbalances transmission of impulses in tissues that either conduct too
• Manifested by: decreased C.O., light-headedness, rapidly or participate in reentry.
confusion, syncope • EXAMPLES:
• May be life-threatening o Amiodarone (Cordarone, Pacerone)
o Bepridil Hydrochloride (Vascor)
o Disopyramide (Norpace)
o Lidocaine (Xylocaine)
o Procainamide (Procan, Procanbid)
o Propranolol (Inderal
o Atropine, Epinephrine
Michaella M. Canlas 3BSN 13
CARDIOVASCULAR DISORDERS
• Anticoagulants (blood thinners) work by making it harder
for the blood to clot, or coagulate.
• They aren't designed to dissolve existing blood clots. They
prevent new clots from forming or existing clots from getting
larger.
• Anticoagulants are also given to certain people at risk for
forming blood clots, such as those with artificial heart valves
or who have atrial fibrillation.
• Warfarin is one of the most commonly-prescribed
anticoagulant drugs
• Aspirin – has an antiplatelet effect
Lifestyle changes
• Stop smoking
• Limit intake of alcohol.
• Limit or stop using caffeine.
• Avoid using stimulants. Beware of stimulants used in cough
and cold medications and herbal or nutritional supplements.
• Learn to recognize symptoms
• Avoid certain activities that causes irregular heart rhythm.
Nursing Care
• Evaluate the patient’s ECG regularly for arrhythmia and
assess hemodynamic parameters.
• Document arrhythmias and notify the physician immediately
• Assess the patient’s LOC, pulse and respiratory rates and
hemodynamic parameters when life-threatening arrhythmia
occur. Monitor ECG continuously and be prepared to initiate
CPR
• Administer oxygen to help improve myocardial oxygen
supply
• Administer analgesics as appropriate and help patient
decrease anxiety
• Assess the patient for predisposing factors such as fluid and
electrolyte imbalance, signs of drug toxicity
• Administer medications as ordered, monitor for adverse
effects and monitor vital signs, laboratory studies,
hemodynamic parameters
• Prepare to assist with or perform cardioversion or
defibrillation if indicated
• If drug toxicity is suspected, report to the physician
immediately.
•
Michaella M. Canlas 3BSN 14
You might also like
- AP Chapter 16BDocument35 pagesAP Chapter 16BJay Patel100% (1)
- Cardiovascular DiseaseDocument22 pagesCardiovascular DiseaseSunday JamesNo ratings yet
- CVS Examination EditedDocument134 pagesCVS Examination EditedThilak JayalathNo ratings yet
- Decrease All Properties of Cardiac Muscle: - H.R - C.O.P Essential For Normal Development of Nervous SystemDocument1 pageDecrease All Properties of Cardiac Muscle: - H.R - C.O.P Essential For Normal Development of Nervous Systemahmed K.Abd el SaterNo ratings yet
- Principles of Managent of Hypovolemic Shock in ADocument43 pagesPrinciples of Managent of Hypovolemic Shock in Aasi basseyNo ratings yet
- Cardiovascular SytemDocument56 pagesCardiovascular SytemlindapramusintaNo ratings yet
- Anatomy of Larynx Lecture 7Document21 pagesAnatomy of Larynx Lecture 7sallykamareddine100% (1)
- Blood CirculationDocument8 pagesBlood CirculationnorafidaishakNo ratings yet
- Module 4 - Cardiac EmergencyDocument30 pagesModule 4 - Cardiac EmergencyElaine AntonetteNo ratings yet
- Bundle Branch BlockDocument37 pagesBundle Branch BlocksyukronchalimNo ratings yet
- Circulatory System HandoutDocument4 pagesCirculatory System HandoutshearmureighNo ratings yet
- Cardiovascular System ReviewDocument9 pagesCardiovascular System ReviewsenjicsNo ratings yet
- Right Bundle Branch BlockDocument13 pagesRight Bundle Branch BlockKweenie QueenieNo ratings yet
- Body Fluids and Fluid CompartmentsDocument7 pagesBody Fluids and Fluid CompartmentsAditya Shrivastava100% (1)
- Musculoskeletal System: Dr. Dipti RamaniDocument30 pagesMusculoskeletal System: Dr. Dipti Ramaniaarti HingeNo ratings yet
- HEENT Cheat SheetDocument22 pagesHEENT Cheat SheetKatrina FeriNo ratings yet
- Anticoagulants ParamedDocument20 pagesAnticoagulants ParamedManikanta GupthaNo ratings yet
- Body Organization Worksheet: InstructionsDocument18 pagesBody Organization Worksheet: InstructionsAngelina AbellanaNo ratings yet
- Lesson 1 Urinary SystemDocument7 pagesLesson 1 Urinary SystemJulio De GuzmanNo ratings yet
- Complete Guide To ECGDocument78 pagesComplete Guide To ECGAnas YahyaNo ratings yet
- History Taking and Physical Examination of Cardiovascular System-The EssentialsDocument72 pagesHistory Taking and Physical Examination of Cardiovascular System-The EssentialsReena Joanella TimbreNo ratings yet
- Blood Pressure RegulationDocument35 pagesBlood Pressure Regulationبراءة أحمد السلاماتNo ratings yet
- Physio MCQDocument31 pagesPhysio MCQanaeshkl80% (15)
- Pharmacotherapy of ArrythmiasDocument68 pagesPharmacotherapy of ArrythmiasABREHAM BUKULONo ratings yet
- Management Lethal ArrhythmiaDocument42 pagesManagement Lethal ArrhythmiaNovi CahyaNo ratings yet
- ROSELA, ERLAINE MARIE BSN 1F Heart-LabDocument4 pagesROSELA, ERLAINE MARIE BSN 1F Heart-LabPado100% (1)
- Circulatory System Packet BDocument5 pagesCirculatory System Packet BLouise SalvadorNo ratings yet
- Congestive Heart FailureDocument86 pagesCongestive Heart FailureNabeel ShahzadNo ratings yet
- Congestive Heart FailureDocument118 pagesCongestive Heart Failureunagracia100% (6)
- Unit 1 New Syllabus NotesDocument69 pagesUnit 1 New Syllabus Notesmalak sherif100% (1)
- CHAPTER 3 GcsDocument14 pagesCHAPTER 3 GcsNurse NotesNo ratings yet
- ICP Head InjuryDocument57 pagesICP Head InjuryWengel RedkissNo ratings yet
- Case 1 - Sickle Cell Disease - PPSXDocument44 pagesCase 1 - Sickle Cell Disease - PPSXNICHOLAS KAUMBA100% (1)
- IABP Learning PackageDocument35 pagesIABP Learning PackageVerghese George100% (1)
- Composition and Function of Blood ComponentsDocument17 pagesComposition and Function of Blood ComponentsPrakash Kumar Nayak100% (1)
- Cardiovascular System TransesDocument8 pagesCardiovascular System Transesadrielvamos28No ratings yet
- Blood and Cardiovascular System TransesDocument12 pagesBlood and Cardiovascular System Transeskuroko senpaiNo ratings yet
- 1 Cardiovascular SystemDocument37 pages1 Cardiovascular SystemEldevincey Macabata100% (1)
- 6 Renal PhysiologyDocument37 pages6 Renal PhysiologyD TekNo ratings yet
- PulseDocument13 pagesPulseArdi EroNo ratings yet
- Physiology 3Document28 pagesPhysiology 3Chuan RuiNo ratings yet
- Proliferation Phase: Corpus AlbicansDocument18 pagesProliferation Phase: Corpus AlbicansJOHN CARL GOMEZNo ratings yet
- ELECTROCARDIOGRAM by Aldrin Jayson AlmadenDocument23 pagesELECTROCARDIOGRAM by Aldrin Jayson AlmadenItsMe AJNo ratings yet
- TONGUE SeminarDocument82 pagesTONGUE SeminarArun MamachanNo ratings yet
- Arteries and Veins Mind MapDocument7 pagesArteries and Veins Mind MapNo Name100% (1)
- Anatomy GI TractDocument54 pagesAnatomy GI TractSaran DNo ratings yet
- The Cardiac Cycle: Chapter 19Document62 pagesThe Cardiac Cycle: Chapter 19BishwambherNo ratings yet
- Fluids and ElectrolytesDocument69 pagesFluids and ElectrolytesHarold DiasanaNo ratings yet
- Frank-Starling LawDocument5 pagesFrank-Starling LawNTA UGC-NETNo ratings yet
- Emergency Room Medicine - 4th EdDocument32 pagesEmergency Room Medicine - 4th EdRaees ParmarNo ratings yet
- Disorders of The Circulatory System Table-AnswersDocument2 pagesDisorders of The Circulatory System Table-Answersapi-281108263No ratings yet
- Heart FailureDocument44 pagesHeart FailureHarold DiasanaNo ratings yet
- Action Potential of Cardiac MusclesDocument16 pagesAction Potential of Cardiac Muscleswaqas_xsNo ratings yet
- Electrocardiogram: What Is An ECG?Document8 pagesElectrocardiogram: What Is An ECG?Ali dhyaa100% (1)
- Fetal CirculationDocument5 pagesFetal CirculationJaime PorscheNo ratings yet
- Cardiac Cycle: Mechanical Event and Their Electrical and Clinical CorrelationDocument28 pagesCardiac Cycle: Mechanical Event and Their Electrical and Clinical Correlationhawas muhammed100% (1)
- Chest Pain Chest Pain: Focused History Focused Physical ExamDocument1 pageChest Pain Chest Pain: Focused History Focused Physical ExamdocNo ratings yet
- Chapter 15 - Cardiovascular SystemDocument89 pagesChapter 15 - Cardiovascular SystemOliver Namyalo100% (1)
- Ch.2 Histology NotesDocument12 pagesCh.2 Histology NotesStephanie M. Lazo100% (1)
- Cardiovascular SystemDocument58 pagesCardiovascular Systemsultan khabeebNo ratings yet
- Review of Cardiovascular SystemDocument20 pagesReview of Cardiovascular SystemVăn ĐứcNo ratings yet
- Anaesthesia and Atrial FibrillationDocument15 pagesAnaesthesia and Atrial FibrillationNaresh Dhawan100% (1)
- Diabetes Mellitus - Nursing CareDocument51 pagesDiabetes Mellitus - Nursing CareJoice DasNo ratings yet
- Clinical HYPERTENSION LecDocument44 pagesClinical HYPERTENSION LecFarwaNo ratings yet
- Electrolytes (3607)Document11 pagesElectrolytes (3607)JennNo ratings yet
- Anatomy 1Document13 pagesAnatomy 1jekeri bekeriNo ratings yet
- Cardiovascular SystemDocument5 pagesCardiovascular Systemy30ny30nNo ratings yet
- Hemodynamics of Cardiac Arrest: Michael. P. Frenneaux and Stig SteenDocument22 pagesHemodynamics of Cardiac Arrest: Michael. P. Frenneaux and Stig SteenJai BabuNo ratings yet
- Cardiovascular System (Seeley)Document110 pagesCardiovascular System (Seeley)Reniella HidalgoNo ratings yet
- Biology: Pearson Edexcel International Advanced LevelDocument28 pagesBiology: Pearson Edexcel International Advanced Level윤소리No ratings yet
- Circulation and Gas Exchange: For Campbell Biology, Ninth EditionDocument116 pagesCirculation and Gas Exchange: For Campbell Biology, Ninth EditionMahnoor AnjumNo ratings yet
- Cardiovascular Physiology 0 Anesthetic ImportanceDocument100 pagesCardiovascular Physiology 0 Anesthetic ImportanceSurya SuryaNo ratings yet
- Biology HSSC 1 Paper IDocument12 pagesBiology HSSC 1 Paper Ikirshnadembra44No ratings yet
- Intra Aortic Balloon CounterpulsationDocument39 pagesIntra Aortic Balloon Counterpulsationmerin sunilNo ratings yet
- The Cardiovascular System: The Heart: © 2012 Pearson Education, IncDocument51 pagesThe Cardiovascular System: The Heart: © 2012 Pearson Education, IncLeilaNo ratings yet
- Etextbook PDF For Huszars Ecg and 12 Lead Interpretation 5th EditionDocument61 pagesEtextbook PDF For Huszars Ecg and 12 Lead Interpretation 5th Editioneve.sampson314100% (42)
- June 2014 (IAL) MS - Unit 1 Edexcel Biology A-LevelDocument22 pagesJune 2014 (IAL) MS - Unit 1 Edexcel Biology A-LevelCheung PhilaNo ratings yet
- Cardiac Asthma - Causes, Symptoms, Diagnosis and Treatment - Tips Curing DiseaseDocument5 pagesCardiac Asthma - Causes, Symptoms, Diagnosis and Treatment - Tips Curing DiseaseBharat JamodNo ratings yet
- CH 13 ActivityDocument4 pagesCH 13 Activityash vldnbrNo ratings yet
- Normal ValuesDocument2 pagesNormal ValuesRese AlvarezNo ratings yet
- Unit 7Document228 pagesUnit 7ShekharNo ratings yet
- Cardiovascular System ConditionsDocument4 pagesCardiovascular System ConditionsNinjaNo ratings yet
- Acute Medicine Surgery - 2020 - KamedaDocument13 pagesAcute Medicine Surgery - 2020 - KamedapaquitoNo ratings yet
- 22323-Article Text-71358-1-10-20190228 PDFDocument4 pages22323-Article Text-71358-1-10-20190228 PDFErna MiraniNo ratings yet
- LP AdhfDocument20 pagesLP AdhfsudiNo ratings yet
- PH32 Exp-9qfrDocument2 pagesPH32 Exp-9qfrMello DiaxNo ratings yet
- AQA A-Level Biology The Cardiac CycleDocument7 pagesAQA A-Level Biology The Cardiac CycleMina BeeNo ratings yet
- Test Bank For Health Psychology 3rd Canadian EditionDocument38 pagesTest Bank For Health Psychology 3rd Canadian EditionCarrie Stavis100% (36)
- Cape Biology Unit 2 2017 p1Document13 pagesCape Biology Unit 2 2017 p1Amarah MohammedNo ratings yet