Professional Documents
Culture Documents
Lung Lab Discussion
Uploaded by
api-632682404Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Lung Lab Discussion
Uploaded by
api-632682404Copyright:
Available Formats
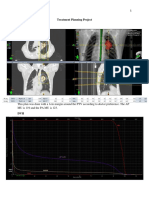
Lung tumors are especially intricate when deciding on beam energy.
Patient
separation can be exceedingly large within the chest, but tissue density creates issues
beyond that. According to Khan, the effects of tissue inhomogeneities for points that are
within inhomogeneous tissue are mainly related to changes in electron fluence.1 This is
seen within the treatment planning systems when you load dose into a plan treating a
tumor of the chest. Thus, isodose distribution in the lungs is controlled by the density of
the lung tissue as well as depth for a specific energy.1 Lung tissue is considered
inhomogeneous as its electron density is so different than that of soft tissue or a water
equivalent phantom. This is very technical language, but it boils down to the fact that
change in density of the lung tissue alters the isodose lines with respect to the energies
selected.2 Interestingly enough, the alteration of dose from lower energy beams and
higher energies is unique.2
There was a study published in the International Journal of Radiation Research
in 2020, regarding the alterations of dose distribution from lung density. The main
takeaways from this article are the unique effects that field size, density, and energy
have on dose distribution in the lung. Within the lower density tissue of the lung, the
PDD increases for low energy beams.2 Immediately beyond the lung tissue there is a
loss of expected PDD in soft tissue. It works almost like a second build up region within
the patient. Khan mentions that areas beyond inhomogeneity are primarily affected by
attenuation of the primary beam.1
However, for very small fields or higher beam energies there is another issue for
treating through the lung. When the beam energy is higher or field size is smaller, there
is more scatter traveling outside of the field and the beam becomes less sharp.1 The
loss of lateral scatter contributing dose means a reduction in PDD within the lung. This
is contradictory to the phenomenon experienced from lower energies and larger fields in
the lung tissue. This would mean less dose to the outer portions of the tumor volumes
when using higher energies or smaller field sizes. At my clinical site our physicians who
frequently treat lung cancer prefer 6MV beams for all fields that traverse large areas of
lung tissue. If you were to use higher energy beams, you may need a bigger margin on
the volume to provide adequate coverage.
I have included a link to the research article representing the change in PDD with field
size and tissue density that helped me to better understand this subject. The figures are
on page 5.
http://ijrr.com/article-1-3093-en.pdf
1. Gibbons, Khan. The Physics of Radiation Therapy. 6th ed. Philadelphia:
Wolters Kluwer; 2020.
2. Zabihzadeh M, Ghahremani Z, Hoseini S, Shahbazian H, Hoseini
Ghahfarokhi M. Effect of lung inhomogeneity on dose distribution during
radiotherapy of patients with lung cancer. Int J Radiat Res 2020; 18 (3)
:579-586
You might also like
- Radiation Hormesis and the Linear-No-Threshold AssumptionFrom EverandRadiation Hormesis and the Linear-No-Threshold AssumptionNo ratings yet
- Treatment Planning ProjectDocument7 pagesTreatment Planning Projectapi-631250296No ratings yet
- Michals Treatment Planning ProjectDocument10 pagesMichals Treatment Planning Projectapi-480222490No ratings yet
- TreatmentplanninglabDocument11 pagesTreatmentplanninglabapi-644802109No ratings yet
- Treatment PlanningDocument9 pagesTreatment Planningapi-426094285No ratings yet
- Treatment Planning PaperDocument15 pagesTreatment Planning Paperapi-632827798No ratings yet
- TxplanningprojectDocument9 pagesTxplanningprojectapi-432489466No ratings yet
- Module 6 DiscussionDocument2 pagesModule 6 Discussionapi-691667702No ratings yet
- Tissue Heterogeneity PaperDocument8 pagesTissue Heterogeneity Paperapi-213038536No ratings yet
- TX Planning PaperDocument15 pagesTX Planning Paperapi-633087057No ratings yet
- Paper UpdateDocument8 pagesPaper Updateapi-630484455No ratings yet
- Heterogeneity Correction Paper PDF WeeblyDocument16 pagesHeterogeneity Correction Paper PDF Weeblyapi-630263039No ratings yet
- Treatment Planning PaperDocument6 pagesTreatment Planning Paperapi-632526087No ratings yet
- Treatment Planning Project PaperDocument12 pagesTreatment Planning Project Paperapi-332574751No ratings yet
- HeterogeneityDocument8 pagesHeterogeneityapi-635186395No ratings yet
- Heterogenity Paper 1Document7 pagesHeterogenity Paper 1api-309296181No ratings yet
- TPC Paper AllisonwrightDocument9 pagesTPC Paper Allisonwrightapi-632741700No ratings yet
- Treatment Planning Paper 3Document12 pagesTreatment Planning Paper 3api-642376263No ratings yet
- Treatment Planning Paper Raver 4 1Document8 pagesTreatment Planning Paper Raver 4 1api-635923017No ratings yet
- TP HeterogeneityDocument10 pagesTP Heterogeneityapi-529438966No ratings yet
- Rod 1 FinalDocument1 pageRod 1 Finalapi-280366843No ratings yet
- Treatment Planning PaperDocument8 pagesTreatment Planning Paperapi-598487146No ratings yet
- Dos 523 - Treatment Planning LabDocument10 pagesDos 523 - Treatment Planning Labapi-645531105No ratings yet
- Heterogeneity Versus Homogeneity in Treatment PlanningDocument8 pagesHeterogeneity Versus Homogeneity in Treatment Planningapi-632493717No ratings yet
- Treatment Planning PaperDocument10 pagesTreatment Planning Paperapi-632529930No ratings yet
- Treatment Planning PaperDocument13 pagesTreatment Planning Paperapi-569210408No ratings yet
- Treatment Planning Project PDFDocument10 pagesTreatment Planning Project PDFapi-692385376No ratings yet
- Lung Cancer Plan With and Without Heterogeneity CorrectionDocument11 pagesLung Cancer Plan With and Without Heterogeneity Correctionapi-264047496No ratings yet
- Treatment Planning ProjectDocument12 pagesTreatment Planning Projectapi-523912641No ratings yet
- Treatment Planning Heterogeneity Vs Homogeneity Lung ProjectDocument13 pagesTreatment Planning Heterogeneity Vs Homogeneity Lung Projectapi-299138743No ratings yet
- Heterogeneity and Lung TreatmentsDocument8 pagesHeterogeneity and Lung Treatmentsapi-691277740No ratings yet
- Treatment Planning PaperDocument10 pagesTreatment Planning Paperapi-633057533No ratings yet
- Treatment Planning Final Copy 1Document13 pagesTreatment Planning Final Copy 1api-373572658No ratings yet
- Heterogeneity Corrections For Lung Treatment PlanningDocument11 pagesHeterogeneity Corrections For Lung Treatment Planningapi-543077883No ratings yet
- Energy Deposition AuDocument10 pagesEnergy Deposition AuIin Tirta SunartaNo ratings yet
- Thesis RadiotherapyDocument6 pagesThesis Radiotherapylakeishajonesjackson100% (2)
- GapsDocument6 pagesGapsapi-432489466No ratings yet
- Treatment Planning ProjectDocument11 pagesTreatment Planning Projectapi-484763634No ratings yet
- Treatment Planning PaperDocument14 pagesTreatment Planning Paperapi-631272802No ratings yet
- E Winn LungDocument12 pagesE Winn Lungapi-574567198No ratings yet
- TxplanningpaperDocument10 pagesTxplanningpaperapi-530717893No ratings yet
- Treatment Planning Project Guide Heterogeneity Correction 1 2Document9 pagesTreatment Planning Project Guide Heterogeneity Correction 1 2api-645453685No ratings yet
- Compare and Contrast PaperDocument4 pagesCompare and Contrast Paperapi-542965039No ratings yet
- Group 5 FinalDocument11 pagesGroup 5 Finalapi-404851310No ratings yet
- Staceysong Treatmentplanninglab 2023spring 1Document8 pagesStaceysong Treatmentplanninglab 2023spring 1api-634067897No ratings yet
- 4T3 Radiation TherapyDocument43 pages4T3 Radiation TherapydanaNo ratings yet
- Treatment Planning Project BmeyerDocument7 pagesTreatment Planning Project Bmeyerapi-350437453No ratings yet
- Research ProposalfinalDocument4 pagesResearch Proposalfinalapi-280366843No ratings yet
- Ultrasound TherapyDocument5 pagesUltrasound TherapyWin ErwinNo ratings yet
- Radiation Oncology A Physicists Eye ViewDocument332 pagesRadiation Oncology A Physicists Eye Viewquyen2012100% (1)
- Wael TP ProjectDocument15 pagesWael TP Projectapi-267335639No ratings yet
- Walt-low-Energy Laser Therapy As Quantum MedicineDocument4 pagesWalt-low-Energy Laser Therapy As Quantum Medicinemuitasorte9No ratings yet
- Iacobo TxplanningpaperDocument11 pagesIacobo Txplanningpaperapi-524151719No ratings yet
- Prone Position in Acute Respiratory Distress Syndrome:: Rationale, Indications and LimitsDocument34 pagesProne Position in Acute Respiratory Distress Syndrome:: Rationale, Indications and LimitsZaLvin Al FaresNo ratings yet
- Treatment Planning Project 4Document11 pagesTreatment Planning Project 4api-282901112No ratings yet
- TT115Document19 pagesTT115arexixNo ratings yet
- HSCI 540 Homework 11 Alternatives, Combination, and ImmunotherapyDocument7 pagesHSCI 540 Homework 11 Alternatives, Combination, and Immunotherapyমারুফ হাসানNo ratings yet
- Law of Bergonie and TribondeauDocument7 pagesLaw of Bergonie and TribondeauRuelyn AcedoNo ratings yet
- Principles of Radiation OncologyDocument21 pagesPrinciples of Radiation Oncologydinu_maria95No ratings yet
- 4 Radiobiology of Brachytherapy and The Dose-Rate EffectDocument27 pages4 Radiobiology of Brachytherapy and The Dose-Rate EffectDiana MitreaNo ratings yet
- Service Learning Project Part 3Document2 pagesService Learning Project Part 3api-632682404No ratings yet
- Outline 4Document8 pagesOutline 4api-630263039No ratings yet
- Larynx ProknowDocument1 pageLarynx Proknowapi-632682404No ratings yet
- Larynx ProknowDocument1 pageLarynx Proknowapi-632682404No ratings yet
- Group 1 Capstone Submission 6 10Document12 pagesGroup 1 Capstone Submission 6 10api-632682404No ratings yet
- LTCW Breast Write UpDocument21 pagesLTCW Breast Write Upapi-632682404No ratings yet
- Practice Problems Weeks 3-5Document3 pagesPractice Problems Weeks 3-5api-333668576No ratings yet
- Eval 2 SpringDocument3 pagesEval 2 Springapi-632682404No ratings yet
- RPD NewDocument4 pagesRPD Newapi-632682404No ratings yet
- Service Learning Journal SpringDocument1 pageService Learning Journal Springapi-632682404No ratings yet
- 1st Affective Eval 2Document3 pages1st Affective Eval 2api-632682404No ratings yet
- Eval 3 SpringDocument3 pagesEval 3 Springapi-632682404No ratings yet
- Sim TX CompetencyDocument2 pagesSim TX Competencyapi-632682404No ratings yet
- Lung Lab InstructionsDocument2 pagesLung Lab Instructionsapi-484763634No ratings yet
- Pelvis Lab DocumentDocument3 pagesPelvis Lab Documentapi-632682404No ratings yet
- ChiasmDocument1 pageChiasmapi-632682404No ratings yet
- Phase I Rod NewDocument4 pagesPhase I Rod Newapi-632682404No ratings yet
- Co Essay 1Document15 pagesCo Essay 1api-632682404No ratings yet
- Phase II Rod NewDocument4 pagesPhase II Rod Newapi-632682404No ratings yet
- Radiation Safety Essay Ryan MonagoDocument5 pagesRadiation Safety Essay Ryan Monagoapi-632682404No ratings yet
- Ryan Monago Resume 2022 2Document1 pageRyan Monago Resume 2022 2api-632682404No ratings yet
- (Main Manuscript) Clinical Practice Guidelines For The Screening, Diagnosis, Treatment and Prevention of Neonatal SepsisDocument69 pages(Main Manuscript) Clinical Practice Guidelines For The Screening, Diagnosis, Treatment and Prevention of Neonatal Sepsiskaydee.arNo ratings yet
- BEd GuidelinesDocument84 pagesBEd GuidelinesshindochaNo ratings yet
- Fibromyalgia: Invisible Pain (Body Image and Depression)Document8 pagesFibromyalgia: Invisible Pain (Body Image and Depression)4gen_3No ratings yet
- KER48201059583796394Document3 pagesKER48201059583796394fahad fahadNo ratings yet
- Novilyn C. Pataray BSN - Ii Pharyngitis: St. Paul College of Ilocos SurDocument1 pageNovilyn C. Pataray BSN - Ii Pharyngitis: St. Paul College of Ilocos SurCharina AubreyNo ratings yet
- Unit 2Document15 pagesUnit 2StudentNo ratings yet
- NCP For Dizziness and HeadacheDocument4 pagesNCP For Dizziness and Headachekarthi karthi100% (1)
- Danone Case PreparationDocument7 pagesDanone Case PreparationXiuNo ratings yet
- Health and Safety Environmental ManagementakistanDocument40 pagesHealth and Safety Environmental ManagementakistanAminullah01No ratings yet
- PDEV Notes For Periodical ExamDocument7 pagesPDEV Notes For Periodical ExamErjie GerasmioNo ratings yet
- Freezing in ParkinsonDocument14 pagesFreezing in ParkinsonGermaine Sperberg DuhartNo ratings yet
- Clinical Practice Guidelines and ProtocolsDocument4 pagesClinical Practice Guidelines and ProtocolsMahmoud NaggarNo ratings yet
- Bowel PreparationDocument20 pagesBowel Preparationrosybash100% (1)
- "Natural Amphetamine" Khat: A Cultural Tradition or A Drug of Abuse?Document21 pages"Natural Amphetamine" Khat: A Cultural Tradition or A Drug of Abuse?Eliana TorresNo ratings yet
- Definition of GriefDocument16 pagesDefinition of GriefNaveen Eldose100% (1)
- Essential GCP by Prof David Hutchinson 2017Document78 pagesEssential GCP by Prof David Hutchinson 2017Luis Marcas VilaNo ratings yet
- K102 Referencing FAQs 21JDocument5 pagesK102 Referencing FAQs 21JpaulNo ratings yet
- Pazoki Et Al. 2022 - Efficacy and Safety of Saffron As Adjunctive Therapy in Adults With ADHDDocument7 pagesPazoki Et Al. 2022 - Efficacy and Safety of Saffron As Adjunctive Therapy in Adults With ADHDLaura DecockNo ratings yet
- The Re-Emergence of Tuberculosis 2Document4 pagesThe Re-Emergence of Tuberculosis 2Navid Ali AskariNo ratings yet
- GREEN Manual - 2021Document157 pagesGREEN Manual - 2021Bon Ber Amad Orofeo100% (2)
- 1.2 Patient Care Coordinator DepartmentDocument16 pages1.2 Patient Care Coordinator DepartmentIurii IuriiNo ratings yet
- Mei Penyakit UmumDocument1 pageMei Penyakit Umumghaniangga11No ratings yet
- Healthcare Analytical Testing ServicesDocument34 pagesHealthcare Analytical Testing ServicesAaryan AgrahariNo ratings yet
- Addiction Counsellors Guide To Working With Alcohol and Drug UsersDocument193 pagesAddiction Counsellors Guide To Working With Alcohol and Drug Usersxiejie22590100% (1)
- RLE Evaluation FormDocument2 pagesRLE Evaluation Formtwothumbs100% (1)
- Sophie Young Eportfolio Pds 2022Document2 pagesSophie Young Eportfolio Pds 2022api-609422028No ratings yet
- TLE 7 Health and Safety in The KItchenDocument32 pagesTLE 7 Health and Safety in The KItchenChristine Mabelle AlmojuelaNo ratings yet
- Autism Spectrum OET-Reading-14Document25 pagesAutism Spectrum OET-Reading-14Aravind JosephNo ratings yet
- The Concepts and Principles of Equity and HealthDocument18 pagesThe Concepts and Principles of Equity and HealthPaulo César López BarrientosNo ratings yet
- Dark Matter and the Dinosaurs: The Astounding Interconnectedness of the UniverseFrom EverandDark Matter and the Dinosaurs: The Astounding Interconnectedness of the UniverseRating: 3.5 out of 5 stars3.5/5 (69)
- Quantum Spirituality: Science, Gnostic Mysticism, and Connecting with Source ConsciousnessFrom EverandQuantum Spirituality: Science, Gnostic Mysticism, and Connecting with Source ConsciousnessRating: 4 out of 5 stars4/5 (6)
- A Brief History of Time: From the Big Bang to Black HolesFrom EverandA Brief History of Time: From the Big Bang to Black HolesRating: 4 out of 5 stars4/5 (2193)
- A Beginner's Guide to Constructing the Universe: The Mathematical Archetypes of Nature, Art, and ScienceFrom EverandA Beginner's Guide to Constructing the Universe: The Mathematical Archetypes of Nature, Art, and ScienceRating: 4 out of 5 stars4/5 (51)
- Summary and Interpretation of Reality TransurfingFrom EverandSummary and Interpretation of Reality TransurfingRating: 5 out of 5 stars5/5 (5)
- Knocking on Heaven's Door: How Physics and Scientific Thinking Illuminate the Universe and the Modern WorldFrom EverandKnocking on Heaven's Door: How Physics and Scientific Thinking Illuminate the Universe and the Modern WorldRating: 3.5 out of 5 stars3.5/5 (64)
- Midnight in Chernobyl: The Story of the World's Greatest Nuclear DisasterFrom EverandMidnight in Chernobyl: The Story of the World's Greatest Nuclear DisasterRating: 4.5 out of 5 stars4.5/5 (409)
- Giza: The Tesla Connection: Acoustical Science and the Harvesting of Clean EnergyFrom EverandGiza: The Tesla Connection: Acoustical Science and the Harvesting of Clean EnergyNo ratings yet
- Packing for Mars: The Curious Science of Life in the VoidFrom EverandPacking for Mars: The Curious Science of Life in the VoidRating: 4 out of 5 stars4/5 (1395)
- The Simulated Multiverse: An MIT Computer Scientist Explores Parallel Universes, The Simulation Hypothesis, Quantum Computing and the Mandela EffectFrom EverandThe Simulated Multiverse: An MIT Computer Scientist Explores Parallel Universes, The Simulation Hypothesis, Quantum Computing and the Mandela EffectRating: 4.5 out of 5 stars4.5/5 (20)
- Black Holes: The Key to Understanding the UniverseFrom EverandBlack Holes: The Key to Understanding the UniverseRating: 4.5 out of 5 stars4.5/5 (13)
- Quantum Physics: What Everyone Needs to KnowFrom EverandQuantum Physics: What Everyone Needs to KnowRating: 4.5 out of 5 stars4.5/5 (49)
- The Tao of Physics: An Exploration of the Parallels between Modern Physics and Eastern MysticismFrom EverandThe Tao of Physics: An Exploration of the Parallels between Modern Physics and Eastern MysticismRating: 4 out of 5 stars4/5 (500)
- The Beginning of Infinity: Explanations That Transform the WorldFrom EverandThe Beginning of Infinity: Explanations That Transform the WorldRating: 5 out of 5 stars5/5 (60)
- Strange Angel: The Otherworldly Life of Rocket Scientist John Whiteside ParsonsFrom EverandStrange Angel: The Otherworldly Life of Rocket Scientist John Whiteside ParsonsRating: 4 out of 5 stars4/5 (94)
- Too Big for a Single Mind: How the Greatest Generation of Physicists Uncovered the Quantum WorldFrom EverandToo Big for a Single Mind: How the Greatest Generation of Physicists Uncovered the Quantum WorldRating: 4.5 out of 5 stars4.5/5 (8)
- The Physics of God: How the Deepest Theories of Science Explain Religion and How the Deepest Truths of Religion Explain ScienceFrom EverandThe Physics of God: How the Deepest Theories of Science Explain Religion and How the Deepest Truths of Religion Explain ScienceRating: 4.5 out of 5 stars4.5/5 (23)
- Chernobyl 01:23:40: The Incredible True Story of the World's Worst Nuclear DisasterFrom EverandChernobyl 01:23:40: The Incredible True Story of the World's Worst Nuclear DisasterRating: 4 out of 5 stars4/5 (264)
- Lost in Math: How Beauty Leads Physics AstrayFrom EverandLost in Math: How Beauty Leads Physics AstrayRating: 4.5 out of 5 stars4.5/5 (125)
- The Sounds of Life: How Digital Technology Is Bringing Us Closer to the Worlds of Animals and PlantsFrom EverandThe Sounds of Life: How Digital Technology Is Bringing Us Closer to the Worlds of Animals and PlantsRating: 5 out of 5 stars5/5 (5)
- Bedeviled: A Shadow History of Demons in ScienceFrom EverandBedeviled: A Shadow History of Demons in ScienceRating: 5 out of 5 stars5/5 (5)
- The Reality Revolution: The Mind-Blowing Movement to Hack Your RealityFrom EverandThe Reality Revolution: The Mind-Blowing Movement to Hack Your RealityRating: 4.5 out of 5 stars4.5/5 (19)