Professional Documents
Culture Documents
Drugs For CHF and Arryhtmias
Uploaded by
Conrado Juisan Crisostomo0 ratings0% found this document useful (0 votes)
9 views5 pages1. Heart failure is a chronic condition where the heart cannot pump enough blood to meet the body's needs. It can be systolic, with reduced ejection fraction, or diastolic, with stiff heart muscles.
2. The body compensates for reduced cardiac output through increased sympathetic nervous system activity and activation of the renin-angiotensin-aldosterone system.
3. Natriuretic peptides counteract volume overload and adrenergic activation by stimulating sodium excretion and vasodilation.
Original Description:
DRUGS-FOR-CHF-AND-ARRYHTMIAS(1)
Original Title
DRUGS-FOR-CHF-AND-ARRYHTMIAS(1)
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. Heart failure is a chronic condition where the heart cannot pump enough blood to meet the body's needs. It can be systolic, with reduced ejection fraction, or diastolic, with stiff heart muscles.
2. The body compensates for reduced cardiac output through increased sympathetic nervous system activity and activation of the renin-angiotensin-aldosterone system.
3. Natriuretic peptides counteract volume overload and adrenergic activation by stimulating sodium excretion and vasodilation.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views5 pagesDrugs For CHF and Arryhtmias
Uploaded by
Conrado Juisan Crisostomo1. Heart failure is a chronic condition where the heart cannot pump enough blood to meet the body's needs. It can be systolic, with reduced ejection fraction, or diastolic, with stiff heart muscles.
2. The body compensates for reduced cardiac output through increased sympathetic nervous system activity and activation of the renin-angiotensin-aldosterone system.
3. Natriuretic peptides counteract volume overload and adrenergic activation by stimulating sodium excretion and vasodilation.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 5
DRUGS FOR CHF AND ARRYHTMIAS
What is heart failure? Manifestation of Heart Failure
- It is a chronic, progressive disorder in Systolic HF
which the heart muscle is unable to o Less blood pumped out of
pump enough blood to meet the body’s ventricles
needs o Ejection fraction <40%
- Decrease CO (Cardiac Output) o Weakened heart muscles
Frank-Starling Law Diastolic HF
- Increased filling of the ventricle results o Less blood fills the
in greater contraction forces and thus a ventricles
rise in the cardiac output o Ejection fraction – normal
o Stiff heart muscle
- In the presence of HF, in order to
counteract the effect of falling CO and
thus reduced perfusion to vital organs,
the body will try to compensate via two
tightly regulated mechanisms
- The first one involves the increase in
sympathetic nervous system activity
- Second major compensatory
mechanism, which involves activation of
the renin-angiotensin-aldosterone Electrophysiology of Normal Cardiac Rhythm
system - An electrophysiology (EP) study is a test
performed to assess your heart’s
Main role of natriuretic peptides is to counter electrical system or activity and is used
the effects of volume overload and adrenergic to diagnosis abnormal heartbeats or
activation by stimulation sodium and water arrhythmia
excretion, promoting myocardial relaxation, - The electrical impulse that triggers a
inhibiting cardiac hypertrophy and fibrosis, normal contraction originates at regular
suppressing sympathetic outflow & stimulating intervals in the sinoatrial (SA) node
vasodilation. usually at a frequency of 60-100 bpm
- Cardiac electrical activity is determined
by transmembrane potential-the
potential, or voltage the difference
between the intracellular and
extracellular environments. These
potential differences can only exist
because of the selectivity-permeable
cardiac cell membranes. This
membrane is composed of a lipid
bilayer which are situated specialized
proteins that form channels that allow
passage of certain ions at specific times
between the intra- and extracellular
spaces.
- The initiation of a heartbeat is governed
by automaticity
- The sinus node controls the heart rate
most of the time because its rate of
discharge is faster than the His cells
- The bundle of His is a heart muscle that
takes part in electrical conduction in the
heart. Purkinje fibers are branched
fibers that carry the electrical impulse ACTION POTENTIAL: Electrical stimulation
to the ventricles. created by a sequence of ion fluxes through
specialized channels in the membrane
(sarcolemma) of the cells responsible for
generating contractile force in the intact heart
that leads to cardiac contraction.
ACTION POTENTIAL IN CARDIOMYOCYTES
The action potential in typical
cardiomyocytes is composed of 5 phases (0-4),
beginning and ending with phase 4.
PHASE 0: DEPOLARIZATION
• An action potential triggered in a
neighboring cardiomyocyte or
pacemaker cell causes the TMP to rise
above −90 mV.
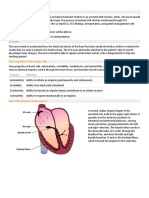
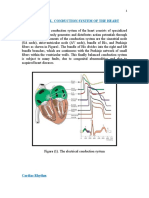
Schematic representation of the heart PHASE 1: EARLY REPOLARIZATION
and normal cardiac electrical activity • TMP is now slightly positive.
(intracellular recordings from areas • Some K+ channels open briefly and an
indicated and ECG). Sinoatrial (SA) node, outward flow of K+ returns the TMP to
atrioventricular (AV) node, and Purkinje approximately 0 mV.
cells display pacemaker activity (phase 4 PHASE 2: THE PLATEAU PHASE
depolarization). The ECG is the body surface • L-type Ca2+ channels are still open and
manifestation of the depolarization and there is a small, constant inward
repolarization waves of the heart. The P current of Ca2+. This becomes
wave is generated by atrial depolarization, significant in the excitation-contraction
the QRS by ventricular muscle coupling process described below.
depolarization, and the T wave by • K+ leaks out down its concentration
ventricular repolarization. Thus, the PR gradient through delayed rectifier K+
interval is a measure of conduction time channels.
from atrium to ventricle, and the QRS • These two countercurrents are
duration indicates the time required for all electrically balanced, and the TMP is
of the ventricular cells to be activated (ie, maintained at a plateau just below 0
the intraventricular conduction time). The mV throughout phase 2.
QT interval reflects the duration of the PHASE 3: REPOLARIZATION
ventricular action potential • Ca2+ channels are gradually inactivated.
• Transmembrane Potential (TMP) is the • Persistent outflow of K+, now exceeding
electrical potential difference (voltage) Ca2+ inflow, brings TMP back towards
between the inside and the outside of resting potential of −90 mV to prepare
a cell. When there is a net movement the cell for a new cycle of
of +ve ions into a cell, the TMP depolarization.
becomes more +ve, and when there is • Normal transmembrane ionic
a net movement of +ve ions out of a concentration gradients are restored by
cell, TMP becomes more –ve. returning Na+ and Ca2+ ions to the
extracellular environment, and K+ ions
to the cell interior. The pumps involved aspects: there is an abnormality in the
include the sarcolemma Na+-Ca2+ site of origin of the impulse, its rate or
exchanger, Ca2+-ATPase and Na+-K+- regularity, or its conduction.
ATPase. Specific Anti-arrhythmic Agents
PHASE 4: THE RESTING PHASE The most widely used scheme for the
• The resting potential in a cardiomyocyte classification of antiarrhythmic drug actions
is −90 mV due to a constant outward recognizes four classes:
leak of K+ through inward rectifier 1. Class 1 action is sodium channel
channels. blockade. Subclasses of this action
• Na+ and Ca2+ channels are closed at reflect effects on the action potential
resting TMP. duration (APD) and the kinetics of
• TMP approaches −70mV, the threshold sodium channel blockade. Drugs with
potential in cardiomyocytes, i.e. the class 1A action prolong the APD and
point at which enough fast Na+ dissociate from the channel with
channels have opened to generate a intermediate kinetics; drugs with class
self-sustaining inward Na+ current. 1B action shorten the APD in some
• The large Na+ current rapidly tissues of the heart and dissociate from
depolarizes the TMP to 0 mV and the channel with rapid kinetics; and
slightly above 0 mV for a transient drugs with class 1C action have minimal
period of time called the overshoot; fast effects on the APD and dissociate from
Na+ channels close (recall that fast Na+ the channel with slow kinetics.
channels are time-dependent). 2. Class 2 action is sympatholytic. Drugs
• L-type (“long-opening”) Ca2+ channels with this action reduce β-adrenergic
open when the TMP is greater than −40 activity in the heart.
mV and cause a small but steady influx 3. Class 3 action manifests as prolongation
of Ca2+ down its concentration of the APD. Most drugs with this action
gradient. block the rapid component of the
Mechanism of Arrhythmias delayed rectifier potassium current, IKr.
• Many factors can precipitate or 4. 4. Class 4 action is blockade of the
exacerbate arrhythmias: ischemia, cardiac calcium current. This action
hypoxia, acidosis or alkalosis, slows conduction in regions where the
electrolyte abnormalities, excessive action potential upstroke is calcium
catecholamine exposure, autonomic dependent, eg, the SA and AV nodes.
influences, drug toxicity (eg. digitalis or
antiarrhythmic drugs), overstretching of
cardiac fibers, and the presence of
scarred or otherwise diseased tissue.
However, all arrhythmias result from (1)
disturbances in impulse formation, (2)
disturbances in impulse conduction, or
(3) both.
• Arrhythmias consist of cardiac
depolarizations that deviate from the
above description in one or more
You might also like
- EKG/ECG Interpretation Made Easy: A Practical Approach to Passing the ECG/EKG Portion of NCLEXFrom EverandEKG/ECG Interpretation Made Easy: A Practical Approach to Passing the ECG/EKG Portion of NCLEXRating: 5 out of 5 stars5/5 (2)
- EKG/ECG Study GuideDocument13 pagesEKG/ECG Study GuideSherree HayesNo ratings yet
- A Simple Guide to the Heart beats, Related Diseases And Use in Disease DiagnosisFrom EverandA Simple Guide to the Heart beats, Related Diseases And Use in Disease DiagnosisRating: 5 out of 5 stars5/5 (1)
- Guyton Hall PHYSIOLOGY Chapter 9 PDFDocument8 pagesGuyton Hall PHYSIOLOGY Chapter 9 PDFOsman NazirNo ratings yet
- Basic ElectrophysiologyDocument46 pagesBasic Electrophysiologyiin setiyanaNo ratings yet
- CVS Physiology of HeartDocument74 pagesCVS Physiology of HeartHEMACHANDRAN G (RA1821002010077)100% (2)
- Information Security Risk Assessment The Qualitative Versus Quantitative DilemmaDocument6 pagesInformation Security Risk Assessment The Qualitative Versus Quantitative Dilemmamohammad.mamdooh9472No ratings yet
- Medical NotesDocument4 pagesMedical NotesRain CastillaNo ratings yet
- Perception and CoordinationDocument21 pagesPerception and Coordinationsimouny100% (28)
- Apch3.1 Problems-Equilibrium AnsDocument5 pagesApch3.1 Problems-Equilibrium AnsQueenQiNo ratings yet
- Healthy Lifestyle Essay ExampleDocument3 pagesHealthy Lifestyle Essay ExampleSabrina Azhar100% (1)
- Cardio NotesDocument15 pagesCardio NotesAngieNo ratings yet
- CV ED Sem 2 2020 2021Document43 pagesCV ED Sem 2 2020 2021Sarhan AliNo ratings yet
- 1 The Electrical Activity of The HeartDocument2 pages1 The Electrical Activity of The HeartRickertsNo ratings yet
- ELEC4810 Notes-3 PDFDocument82 pagesELEC4810 Notes-3 PDFKwan ChanNo ratings yet
- L2-Bioe345-EC Coupling - 2020 PresentedDocument12 pagesL2-Bioe345-EC Coupling - 2020 PresentedasdfghjklNo ratings yet
- Mechanisms of Cardiac Arrythmias: Conduction, or BothDocument5 pagesMechanisms of Cardiac Arrythmias: Conduction, or BothdeaNo ratings yet
- Cardiac Ion ChannelsDocument10 pagesCardiac Ion ChannelsPedro RodriguezNo ratings yet
- A1 Basic ECG Part1. Dr. Calibuso (Revised)Document6 pagesA1 Basic ECG Part1. Dr. Calibuso (Revised)Anne Lorraine BringasNo ratings yet
- Cardiac Function and Control: The HeartDocument12 pagesCardiac Function and Control: The HeartMiles HuiNo ratings yet
- Arrhythmia 2021-2022 Semester 1Document42 pagesArrhythmia 2021-2022 Semester 1Omar AlaamNo ratings yet
- VII-PHYSIOLOGY - Kaplan Medical USMLE Step 1 Lecture Notes 2021 (2021) (Arrastrado)Document1 pageVII-PHYSIOLOGY - Kaplan Medical USMLE Step 1 Lecture Notes 2021 (2021) (Arrastrado)Beto RendonNo ratings yet
- Wo 2Document10 pagesWo 2GabrielaNo ratings yet
- Cardiac Muscle: Dr. Kanimozhi Sadasivam, MD Associate Professor SRM Medical College & RC, ChennaiDocument57 pagesCardiac Muscle: Dr. Kanimozhi Sadasivam, MD Associate Professor SRM Medical College & RC, ChennaiShampa SenNo ratings yet
- Sistem Konduksi Jantung (Pembekalan) - DR PUT&DrHARDocument32 pagesSistem Konduksi Jantung (Pembekalan) - DR PUT&DrHARNur FarinahNo ratings yet
- Fisika BioelektrikDocument50 pagesFisika BioelektrikFachriza EffendiNo ratings yet
- CCN CardioDocument5 pagesCCN CardioSofia P. PanlilioNo ratings yet
- The Cardiovascular SystemDocument4 pagesThe Cardiovascular SystemSharie Mae MataumNo ratings yet
- N5 SampleDocument12 pagesN5 Sampleshaikhbakhtiyar3669No ratings yet
- Regulation of BPDocument17 pagesRegulation of BPLemon CatbaganNo ratings yet
- ECG and Einthoven's Triangle Flashcards - QuizletDocument5 pagesECG and Einthoven's Triangle Flashcards - QuizletMr. DybalaNo ratings yet
- Anti-Arrhythmic DrugsDocument15 pagesAnti-Arrhythmic DrugsYamin SanjuNo ratings yet
- Summary C19-20Document15 pagesSummary C19-20EleanorNo ratings yet
- Cardio PhysioDocument11 pagesCardio Physioanonymousperson4696No ratings yet
- Cardiac Muscles and Their PropertiesDocument19 pagesCardiac Muscles and Their PropertiesKiran DeviNo ratings yet
- Congestive Heart Failure: Pediatrics 2Document11 pagesCongestive Heart Failure: Pediatrics 2Rea Dominique CabanillaNo ratings yet
- Cardiovascular System - Electrical SystemDocument5 pagesCardiovascular System - Electrical SystemRashid DayaoNo ratings yet
- ElectrocardiogramDocument2 pagesElectrocardiogramonijinoNo ratings yet
- CARDIODocument15 pagesCARDIOArian Love YlmidoNo ratings yet
- HPP Lec Cvs2Document4 pagesHPP Lec Cvs2carlo baculiNo ratings yet
- Unit 8 Electricity IIDocument8 pagesUnit 8 Electricity II03152788No ratings yet
- Cardiovascular PhysiologyDocument15 pagesCardiovascular PhysiologyParker KapembwaNo ratings yet
- Cvs 1,2Document36 pagesCvs 1,2atefmoussaNo ratings yet
- Properties of Heart MusclesDocument11 pagesProperties of Heart MusclesSyedzulqurnainhussainshah ZulqurnainNo ratings yet
- Nervous System Part 1Document11 pagesNervous System Part 1Mariel AbatayoNo ratings yet
- HEART SimplifiedDocument94 pagesHEART Simplifiedcloud kumoishNo ratings yet
- Lecture 2 PDFDocument15 pagesLecture 2 PDFAya MuhannadNo ratings yet
- Lecture 4 Properties of Myocardium and Cardiac Cycle 2020-2021Document43 pagesLecture 4 Properties of Myocardium and Cardiac Cycle 2020-2021badarbhai222No ratings yet
- Special Conductive System of Heart: By: Azher SyedDocument14 pagesSpecial Conductive System of Heart: By: Azher SyedAzhersyedNo ratings yet
- Trans CardioDocument128 pagesTrans CardioWaiwit KritayakiranaNo ratings yet
- N5Document128 pagesN56qhx62pr42No ratings yet
- Sistema de Conduccion Karen Daniela VelascoDocument3 pagesSistema de Conduccion Karen Daniela Velascoapi-540316757No ratings yet
- Cardiac-Arrhythmia Cardiac-Arrhythmia: Pharma (Centro Escolar University) Pharma (Centro Escolar University)Document37 pagesCardiac-Arrhythmia Cardiac-Arrhythmia: Pharma (Centro Escolar University) Pharma (Centro Escolar University)Charles AbagonNo ratings yet
- Bioelectric Potentials: - Certain Cells of The Body Generates Their On Monitoring Signals - Excitable CellsDocument110 pagesBioelectric Potentials: - Certain Cells of The Body Generates Their On Monitoring Signals - Excitable CellsYadu KrishnanNo ratings yet
- Weekly Objectives PBL ThermoregulationDocument19 pagesWeekly Objectives PBL ThermoregulationKellyNo ratings yet
- CVS AnatomyDocument45 pagesCVS AnatomyAfk SystemNo ratings yet
- PHYSIO Cardiac Muscle and Heart As A PumpDocument5 pagesPHYSIO Cardiac Muscle and Heart As A PumpAyumi StarNo ratings yet
- 2 - Cardiac Electrical ActivityyytyyDocument31 pages2 - Cardiac Electrical ActivityyytyyTausif ChNo ratings yet
- 01 Res 32 2 215Document6 pages01 Res 32 2 215D.S.M.No ratings yet
- Clinical Electrocardiography and ECG Interpretation - ECG & ECHODocument15 pagesClinical Electrocardiography and ECG Interpretation - ECG & ECHORimaNo ratings yet
- الوحدة الثانيهDocument7 pagesالوحدة الثانيهHUAWEI HUAWEINo ratings yet
- Phase 2 Cardiac Muscle - 1Document30 pagesPhase 2 Cardiac Muscle - 1erenyorulmaz143No ratings yet
- Perdev NotesDocument7 pagesPerdev NotesConrado Juisan CrisostomoNo ratings yet
- BiologyDocument7 pagesBiologyConrado Juisan CrisostomoNo ratings yet
- Types of Social MediaDocument1 pageTypes of Social MediaConrado Juisan CrisostomoNo ratings yet
- Gen Bio 2 SpeciationDocument30 pagesGen Bio 2 SpeciationConrado Juisan CrisostomoNo ratings yet
- Gen Bio 2 PhylogenyDocument36 pagesGen Bio 2 PhylogenyConrado Juisan CrisostomoNo ratings yet
- Evolution and The Origin of EarthDocument3 pagesEvolution and The Origin of EarthConrado Juisan CrisostomoNo ratings yet
- Why Is Mental Health Important?Document1 pageWhy Is Mental Health Important?Conrado Juisan CrisostomoNo ratings yet
- Oversized Primary Pulley Regulator Valve Kit: Jatco/Nissan JF015E (RE0F11A)Document2 pagesOversized Primary Pulley Regulator Valve Kit: Jatco/Nissan JF015E (RE0F11A)marranNo ratings yet
- The Gazette of India: ExtraordinaryDocument72 pagesThe Gazette of India: ExtraordinaryRaaNo ratings yet
- City Laundry: Chart of Account Assets LiabilitiesDocument6 pagesCity Laundry: Chart of Account Assets LiabilitiesGina Calling DanaoNo ratings yet
- PN 2023 003746.fullDocument4 pagesPN 2023 003746.fullHenrique OliveiraNo ratings yet
- Phototransduction Occurs at The RetinaDocument13 pagesPhototransduction Occurs at The RetinaKathleen RussellNo ratings yet
- PRIYANKA S Thesis On Probiotic Shrikhand Very Importand PDFDocument230 pagesPRIYANKA S Thesis On Probiotic Shrikhand Very Importand PDFAshutosh MasihNo ratings yet
- DUPLEX 1500 - 11000 Multi-N Rooftop EN - 2018 - 03Document8 pagesDUPLEX 1500 - 11000 Multi-N Rooftop EN - 2018 - 03Constantin CilibiuNo ratings yet
- DROPSAFE PouchesDocument3 pagesDROPSAFE PouchesgustavoNo ratings yet
- ĐỀ THI VÀO 10 THANH HÓA 17Document5 pagesĐỀ THI VÀO 10 THANH HÓA 17Như KhánhNo ratings yet
- Zn-Al Tank Nozzels ScheduleDocument5 pagesZn-Al Tank Nozzels SchedulePravin BoteNo ratings yet
- Instructions For UseDocument16 pagesInstructions For UseMirkoNo ratings yet
- 5 Analyzing Consumer MarketsDocument38 pages5 Analyzing Consumer MarketsSoham ChatterjeeNo ratings yet
- Honeywell 4219 Install GuideDocument2 pagesHoneywell 4219 Install GuideAlarm Grid Home Security and Alarm MonitoringNo ratings yet
- Babylog vn500 PDFDocument284 pagesBabylog vn500 PDFEdgar CarreraNo ratings yet
- Psychological Hazards: How Can These Hazards Affect Workers' Psychological Health?Document2 pagesPsychological Hazards: How Can These Hazards Affect Workers' Psychological Health?Aries WillNo ratings yet
- 001 Eures-Leaflet AustriaDocument6 pages001 Eures-Leaflet AustriaAFIZ AVDIINo ratings yet
- L0810348 PDFDocument98 pagesL0810348 PDFhughstimsonNo ratings yet
- Check - List: 2) Circular No. RW/NH-III/P/66/76 Dated 11.05.1982Document1 pageCheck - List: 2) Circular No. RW/NH-III/P/66/76 Dated 11.05.1982mogijo11dffdfgdfgNo ratings yet
- 10 Science Life Processes Test 04Document1 page10 Science Life Processes Test 04asuhassNo ratings yet
- Chapter 14 - Bus. Combination Part 2Document16 pagesChapter 14 - Bus. Combination Part 2PutmehudgJasdNo ratings yet
- Seattle Coffee LRDocument4 pagesSeattle Coffee LRIan JaredNo ratings yet
- SANTECH - Componente Compresoare ACDocument64 pagesSANTECH - Componente Compresoare ACDominykas OrlovasNo ratings yet
- Intro To DownstreamprocessingDocument24 pagesIntro To DownstreamprocessingmluluNo ratings yet
- Radioactivity 6 QPDocument6 pagesRadioactivity 6 QPshookookie 101No ratings yet
- KPT AbstractDocument2 pagesKPT AbstractManan ParikhNo ratings yet
- Mud ArchitectureDocument13 pagesMud ArchitectureHarsha Madumali PadmasekaraNo ratings yet
- Company Profile Prodbtech PVT LTD PuneDocument3 pagesCompany Profile Prodbtech PVT LTD PuneAashish upadhyayNo ratings yet