Professional Documents
Culture Documents
Endocrine System
Uploaded by
Roeisa Salinas0 ratings0% found this document useful (0 votes)
28 views7 pagesAnatomy and Physiology - Endocrine System transes by Roeisa Salinas
Original Title
ENDOCRINE SYSTEM
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAnatomy and Physiology - Endocrine System transes by Roeisa Salinas
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
28 views7 pagesEndocrine System
Uploaded by
Roeisa SalinasAnatomy and Physiology - Endocrine System transes by Roeisa Salinas
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 7
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
ENDOCRINE SYSTEM Gross Anatomy & Basic Function of Endocrine
Glands
Functional Anatomy of the Endocrine Glands
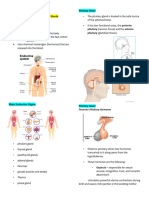
PITUITARY GLAND (hypophysis)
• 2nd major control system of body
• Coordinate and integrate body activities • in the sella turcica of sphenoid bone
• Hormone = Greek “to arouse” • 2 lobes: Adenohypophysis (APG) &
• Target Organs – respond to particular hormone Neurohypophysis (PPG) + infundibulum
• Cells have nuclei, mitochondria, ER, Golgi
bodies, secretory vesicles
4 main chemical groups that act as hormones:
1. Protein & glycoprotein molecules – insulin, GH,
PTH
2. Small peptide molecules – vasopressin, prods of
enteroendocrine cells
3. AA derivatives – thyroxine, adrenaline/epi,
noradrenaline/nore
4. Steroids from cholesterol – adrenal cortical
hormones, ovarian/testicular hormones
• Endocrine function – anterior P.G., thyroid,
adrenals, parathyroids
• Endo & Exocrine function – pancreas and Anterior Pituitary Gland (Adenohypophysis)
gonads • Epithelial upgrowth from roof of primitive oral
• Both gland types are derived from epithelium cavity – Rathke’s pouch (R’sP)
• Endocrine glands (EnG) – release hormones in • Contain a cleft/group of cyst-like spaces w/c
ECF/blood represent vestigial lumen of R’sP
• Exocrine glands (ExG) – release at body • Remnant of R’sP divides major part of APG from
surface/ducts thin zone of tissue, between APG & PPG – pars
intermedia
• Extension surrounds the neural stalk – pars
tuberalis
Posterior Pituitary Gland (Neurohypophysis/pars
nervosa)
• Downgrowth of nervous tissue from
hypothalamus, joined by pituitary stalk –
infundibulum
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
1. Oxytocin – produced in paraventricular nuclei,
“swift birth”
2. Antidiuretic hormone (ADH) –
vasopressin/arginine vasopressin, in supraoptic
nuclei; conserve water in distal convoluted tubules
of kidneys & collecting tubules reabsorb water by
sodium
PINEAL GLAND
• Small cone-shaped gland in rood of 3rd ventricle
• Major endo product is melatonin – diurnal
cycle/sleep-wake cycle
Anterior Pituitary Hormones: • Melatonin - peaks at night/lowest at noon; effect
on reprod. system that prevents precocious
• Target organ is another endoc. gland; secrete sexual maturation; changing level may affect
hormone in response to stimulation biological rhythms: body temp, sleep, appetite
• “master gland” – controls activity of many other
THYROID GLAND
endoc. Gland
1. Gonadotropins – regulate gamete production & • 2 lobes joined by a central mass – isthmus
hormonal activity (ovaries/testes) • Located in throat, inferior to larynx
• Epithelial downgrowth from fetal tongue
o Follicle-stimulating hormone (FSH) • C cells are from ultimobranchial element of 4th
o Luteinizing hormone (LH) branchial pouch
2. Adrenocorticotropic hormone (ACTH) – • Also part of normal brain development
endocrine activity of adrenal cortex • Cretinism – like dwarfism + affected brain,
3. Thyroid-stimulating hormone (TSH) – influence absence of thyroxine
growth and activity of thyroid gland 1. Thyroid hormone (TH) – 2 active hormones,
2 hormones not directly involved in EnG regulation: control rate of body metabolism and cellular
oxidation
4. Growth Hormone (GH) – determine body size,
growth of muscle/long bones o T4 (thyroxine/tetraiodothyronine)
o T3 (triiodothyronine) – more active
5. Prolactin (PRL) – milk production by breasts
2. Calcitonin – released in response to high blood
• Ventral hypothalamic hormones control Ca level
production/secretion of tropic hormones, GH,
PARATHYROID GLANDS
PRL
• Hypothalamic hormones reach cells of APG via • Embedded on posterior surface of thyroid gland
hypophyseal portal system (2nd image) • 2 small oval glands on each lobe
Posterior Pituitary Hormones: • Secrete parathyroid hormone (PTH) – most
important regulator of calcium balance of blood
• Not an EnG, does not synthesize hormones • Stimulate kidneys to convert vit D to active D3
• Storage area for 2 neurohormones transported form (Calcitriol)
to it via axons of neurons in paraventricular &
supraoptic nuclei of hypothalamus THYMUS
• Cell body (producer, in hypothalamus), • Bilobed gland in superior thorax, posterior to
infundibulum (long axon), herring bodies sternum, anterior to heart/lungs
(ends of PPG, storage of secretory vesicles) • Visible in infant, begins to thin at puberty, almost
invisible at old age
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
• Produces families of hormones: thymulin, THE GONADS
thymosin, thymopoietin
• Ovaries – paired, almond-sized organs in pelvic
• Involved in maturation of T lymphocytes/T cells cavity, produce female sex cells (ova); EnG and
and immune response ExG functions only begin at puberty; 2 steroid
• Act locally as paracrines (affect nearby cells) hormone groups
ADRENAL (SUPRARENAL) GLANDS 1. Estrogens
• At the top of kidneys - development of secondary sex charac.: maturation
• Triangle, “kidney party hats” of reprod. system and development of the breasts
• Adrenal medulla develops from neural crest - act w/ progesterone to bring cyclic changes of the
tissue uterine lining – menstrual cycle
• Directly controlled by SNS - prepare mammary gland for lactation
• Adrenal medulla – act w/ SNS, fight-or-flight
2. Progesterone
response
- uterine musculature in quiescent state
1. Epinephrine – 80%
- Helps prepare breast tissue for lactation
2. Norepinephrine – 20%
• Testes – paired oval suspended in pouchlike sac
• Adrenal cortex – 3 major groups of steroid (scrotum) outside pelvic cavity; produce male
hormones (corticosteroids) sex cells (sperm); EnG and ExG begin at
1. Mineralocorticoids (aldosterone) – zona puberty
glomerulosa, regulate water and electrolyte balance 1. Testosterone – maturation of reprod. system,
in ECFs by Na ion reabsorption in kidney tubules male secondary charac, sexual drive/libido
2. Glucocorticoids (cortisol (hydrocortisone),
cortisone, corticosterone) – z. fasciculata, resist
Microscopic Anatomy of Endocrine Glands
long-term stressors by increasing blood glucose
levels Anterior Pituitary Gland
3. Gonadocorticoids (sex hormones) – z. 2 main cells population based on color:
reticularis, androgens (male), estrogens (female) • Chromophils – w/ color
PANCREAS o Basophils – Violet/blue
o Acidophils – orange
• Partially behind stomach in abdomen
Note: Eosinophils - pink
• EnG and ExG functions
• Chromophobes – w/o color
• Produce digestive enzymes, insulin, glucagon
• Pancreatic islets/islets of Langerhans secrete
the hormones
1. Insulin – decrease blood sugar levels, accelerate
transport of glucose in body cells (oxidized for
energy/converted to glycogen or fat for storage);
from alpha cells
2. Glucagon – increase blood sugar level,
stimulates liver to break down glycogen stores to
glucose, synthesize glucose by gluconeogenesis, Other cells involved in secretion:
release glucose to blood; from beta cells
• Somatotrophs – GH secretion, 50%
• Mammotrophs – lactotrophs, PRL, 20%
• Corticotrophs – secrete ACTH, 20%
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
• Thyrotrophs – TSH (thyrotrophin), 5% Thyroid Gland
• Gonadotrophs – FSH and LSH, 5% • Follicles – spherical sacs w/ pink-stained
Pars intermedia material (colloid); stored T3 & T4 attached to
protein colloidal material stored in follicles as
• Derived embryologically from R’Sp
thyroglobulin; formed by simple
• Basophilic cells lying in irreg clusters between
cuboidal/squamous epithelial cells that
APG and PPG
synthesize products
• Contain small cystic spaces filled with
eosinophilic material
• Contain secretory granules like corticotrops
• Produce alpha-MSH from POMC at low levels
• Inactive – thyroid epithelial cells are simple
flat/cuboidal cells
• Active – tall and columnar
• Scalloped pale edge of colloid is where the
colloid has been removed from follicle lumen
(bitten off to release stored hormones)
Posterior Pituitary Gland
• Non-myelinated axons of specialized neurons
(neurosecretory activity)
• Cell bodies are in supraoptic (ADH) &
paraventricular nuclei (oxytocin) of
hypothalamus
• Hormones are passed down to axons in
neurosecretory granules, accumulate in
• Parafollicular or C cells – 2nd type of endoc cell
distended terminations of axons where contact
w/ neuroendocrine cells structure; found as
w/ capillaries happen – Herring bodies
scattered cells in the follicle lining/small clumps
• Pituicytes – specialized highly branched glial
in interstices between follicles; secrete
cells, supports axons
calcitonin
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
Parathyroid Glands - aldosterone secretion is independent of ACTH
control
2 major cell types:
• Chief cells – small w/ round central nuclei and
pale eosinophilic/clear cytoplasm; secrete and
synthesize PTH
• Oxyphil cells – occur in nodules; copious
eosinophilic cytoplasm seen packed with
mitochondria
2. Zona fasciculata – middle and broadest of the
cortical zones; w/ narrow columns and cords of cells,
1 cell thick, separated by fine strands of collagen and
wide-bore capillaries; abundant cytoplasm and pale
staining due to many lipid droplets; abundant
mitochondria and smooth ER
Adrenal (Suprarenal) glands - secretes glucocorticoid hormones (cortisol) w/
• Small, flat endoc glands closely applied to upper many metabolic effects:
pole of each kidney o Raise blood glucose level, increase cellular
2 types with diff functions and origin: synthesis of glycogen
• Adrenal cortex – similar embryological origin to o Increase rate of CHON breakdown and rate
gonads; secrets various steroid hormones; of liberation of lipid from tissue stores
adrenal steroids divided to 3:
o Mineralocorticoids – z.g. - cortisol secretion is controlled by hypothalamus
o Glucocorticoids – z.f. via APG tropic hormone ACTH
o Sex hormones – z.r.
Adrenal glands layers: 3 zonas + top & bottom layer
• Capsule
• Zona glomerulosa (z.g.)
• Zona fasciculata (z.f.)
• Zona reticularis (z.r.)
• Adrenal medulla
3. Zona reticularis – thin, innermost layer, lies next
1. Zona glomerulosa - cells arranged in irreg ovoid
to adrenal medulla; irreg network of branching cords
clusters separated by delicate fibrous trabeculae;
and clusters of glandular cells separated by wide
round nuclei, less cytoplasm than cells in z.f.;
diameter capillaries; cells are smaller than z.f. w/
cytoplasm with many smooth ER and mitochondria
less cytoplasm but darker staining because of fewer
w/ scanty lipid droplets
lipid droplets
- secretes mineralocorticoid hormones
(aldosterone) controlled by the RA system - brown lipofuscin pigment is seen, secretes small
- aldosterone acts directly on renal tubules to quantities of androgens and glucocorticoids
increase Na and water retention
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
2. Glucagon – metabolic effects that oppose insulin
Other cells present in the islets:
• Somatostatin – released by delta cells
• Vasoactive intestinal peptide (VIP)
• Pancreatic polypeptide (PP)
Enterochromaffin (EC) Cells:
• Motilin
• 5-hydroxytryptamine (5-HT, serotonin)
• Substance P
• Adrenal medulla – similar origin to SNS, highly
specialized add-on of this system; secretes • Islet of Langerhans – groups of up to 3000
catecholamine hormones under control of secretory cells supported by a fine collagenous
preganglionic neurons of SNS: network w/ fenestrated (tiny openings/pores)
o Adrenaline (epinephrine) capillary; delicate capsule surrounds each islet;
o Noradrenaline (norepinephrine) cells are small w/pale-stained granular
- clusters of cells w/ granular, faintly basophilic cytoplasm
cytoplasm, w/ many capillaries in their fine
supporting stroma
- acute physical and psychological stresses
initiate the release of these hormones
- released catecholamines act on adrenergic
receptors: heart/BVs, bronchioles, visceral
muscle, skeletal muscle
- adrenaline also has potent metabolic effects
(glycogenolysis)
- Insulin-producing beta cells over 60%
distributed in islet
- Glucagon-producing alpha cells about
25% arranged around periphery
Pineal Gland
2 main cell types:
• Pinealocytes (pineal chief cells) – highly
modified neurons in clusters and cords
surrounded by fenestrated capillaries; round
nuclei w/ prominent nucleoli and granular
Endocrine Pancreas cytoplasm; cytoplasmic granules w/ melatonin
and precursor 5-HT
• embryonic epithelium of the pancreatic ducts
• Neuroglial cells – like astrocytes of CNS;
consists of both exocrine and endocrine cells
dispersed between clusters of pinealocytes and
• during development, endocrine cells migrate in association w/ capillaries
from duct system and aggregate around
capillaries = isolated clusters of cells – islets of
Langerhans
• main secretory products:
1. Insulin – promotes uptake of glucose by most
cells (liver, skeletal muscle, adipose tissue)
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
You might also like
- Endocrine SystemDocument20 pagesEndocrine SystemSheena Pasion100% (2)
- Notes in Science LT 10 - Endocrine SystemDocument3 pagesNotes in Science LT 10 - Endocrine SystemAlven ReyNo ratings yet
- 4 Day Workout SplitDocument4 pages4 Day Workout SplitChristopher AlNo ratings yet
- A Simple Guide to The Pineal Gland (The Third Eye) And Its FunctionFrom EverandA Simple Guide to The Pineal Gland (The Third Eye) And Its FunctionRating: 5 out of 5 stars5/5 (1)
- Endocrine SystemDocument7 pagesEndocrine SystemMikaella Viador100% (2)
- The Endocrine System: Presented By: 5th Group Feby Amalia Hardianty Suryana Syuaib Andi Nurul Virninda Debby Trisia SariDocument24 pagesThe Endocrine System: Presented By: 5th Group Feby Amalia Hardianty Suryana Syuaib Andi Nurul Virninda Debby Trisia SariAndi Nurhidayah100% (1)
- Kapalabhati Pranayama or Breath of FireDocument6 pagesKapalabhati Pranayama or Breath of Firemsayee100% (1)
- Head To Toe Assessment (Elder)Document2 pagesHead To Toe Assessment (Elder)ZnarfNo ratings yet
- BSc. MEDICAL IMAGING TECHNOLOGY - 2019 PDFDocument91 pagesBSc. MEDICAL IMAGING TECHNOLOGY - 2019 PDFMujahid Pasha0% (1)
- Chapter 2 - General Characteristics of The SpineDocument50 pagesChapter 2 - General Characteristics of The SpineveronicalovirgenNo ratings yet
- Somatic Nervous SystemDocument4 pagesSomatic Nervous SystemGuenNo ratings yet
- Anaphy LecDocument5 pagesAnaphy Lecmelbertconag1973No ratings yet
- AnaPhy Lec - Endocrine SystemDocument2 pagesAnaPhy Lec - Endocrine SystemReigh DakotaNo ratings yet
- 22 Chemical Co-OrdinationDocument47 pages22 Chemical Co-OrdinationRachna JaiswalNo ratings yet
- Script For Midterm VRDocument5 pagesScript For Midterm VRDanica MerinNo ratings yet
- Endocrine System Animal ScienceDocument15 pagesEndocrine System Animal ScienceJairus LampanoNo ratings yet
- 22. Chemical Co Ordination and Integration_434dea34 f494 4704 a8c9 6876397e324eDocument53 pages22. Chemical Co Ordination and Integration_434dea34 f494 4704 a8c9 6876397e324epcgurukotari9No ratings yet
- Genbio2 ReviewerDocument4 pagesGenbio2 ReviewerLovely QuezonNo ratings yet
- Quick Study Guide To The Endocrine SystemDocument11 pagesQuick Study Guide To The Endocrine SystemMc Luis Glen AserdanoNo ratings yet
- Endocrine Glands - 1st - ChapterDocument12 pagesEndocrine Glands - 1st - Chaptervarun kumarNo ratings yet
- Endocrine System NotesDocument8 pagesEndocrine System NotesShiela Mae SagayoNo ratings yet
- Endokrinologi Reproduksi: Bayu Kurniawan, DRDocument48 pagesEndokrinologi Reproduksi: Bayu Kurniawan, DRdocbay100% (1)
- Animal Hormones PDFDocument11 pagesAnimal Hormones PDFAin HusnaNo ratings yet
- ANATOMY Endocrine TranscribedDocument9 pagesANATOMY Endocrine TranscribedYanyan PanesNo ratings yet
- EndocrineDocument49 pagesEndocrineHerbert DelacruzNo ratings yet
- Endocrine System (Zoology)Document3 pagesEndocrine System (Zoology)Cheska de GuzmanNo ratings yet
- Endocrine SystemDocument43 pagesEndocrine SystemnandaNo ratings yet
- Chemical Coordination and IntegrationDocument3 pagesChemical Coordination and Integrationakhil01ajNo ratings yet
- Reproduction & Endocrinology 1: Hypothalamus and PituitaryDocument41 pagesReproduction & Endocrinology 1: Hypothalamus and PituitaryabdulNo ratings yet
- Endocrine Glands and Their FunctionsDocument31 pagesEndocrine Glands and Their FunctionsAfrina Asmi MINo ratings yet
- Endocrine SystemDocument7 pagesEndocrine SystemClyde CapapasNo ratings yet
- Physio 1Document6 pagesPhysio 1amjadNo ratings yet
- Endocrine System Hormone ControlDocument4 pagesEndocrine System Hormone Controlden mNo ratings yet
- The Endocrine Glands and The Nervous SystemDocument5 pagesThe Endocrine Glands and The Nervous SystemLyanna MormontNo ratings yet
- Endocrine System NotesDocument23 pagesEndocrine System NoteslacyNo ratings yet
- OhohohDocument34 pagesOhohohuriNo ratings yet
- Topic 3 THE ENDOCRINE SYSTEMDocument41 pagesTopic 3 THE ENDOCRINE SYSTEMIreneNo ratings yet
- Chemical Coordination & Integration PowernotesDocument3 pagesChemical Coordination & Integration PowernotesSushmit SrivastavaNo ratings yet
- Endocrine System Chemical MessengersDocument14 pagesEndocrine System Chemical MessengersElaine Victoria ElizanNo ratings yet
- Endorine SystemDocument4 pagesEndorine SystemMichaela Shianne E. MatituNo ratings yet
- The Endocrine System: Properties: Mechanisms of Hormone ActionDocument5 pagesThe Endocrine System: Properties: Mechanisms of Hormone ActionaudreyNo ratings yet
- PNKND Les 0 V 9 VWR60 B RCNDocument4 pagesPNKND Les 0 V 9 VWR60 B RCNaadeshthite476No ratings yet
- EndocrineDocument5 pagesEndocrineShem DelolaNo ratings yet
- Module 5Document9 pagesModule 5CamilleCalmaLenonNo ratings yet
- Endocrine Histology NotesDocument5 pagesEndocrine Histology NotesJulie TranNo ratings yet
- Unit 8: Endocrine System: Hormones Because Lipids Fear Water That's WhyDocument7 pagesUnit 8: Endocrine System: Hormones Because Lipids Fear Water That's WhyFaoloPanganNo ratings yet
- Endocrine System NotesDocument6 pagesEndocrine System Noteshannah pelonia100% (1)
- Endocrine SystemDocument4 pagesEndocrine SystemJames CastroNo ratings yet
- Endo ReviewerDocument5 pagesEndo ReviewerZIAN LABADIANo ratings yet
- Science: Endocrine & Nervous SystemDocument5 pagesScience: Endocrine & Nervous SystemLUISE DANIELLA DELOS REYES DOLOTALLASNo ratings yet
- Endocrine System Hormones and GlandsDocument6 pagesEndocrine System Hormones and GlandsFrancine Dominique CollantesNo ratings yet
- Endocrine System Reviewer LecDocument3 pagesEndocrine System Reviewer LecNOELLE LAURAINNE TANZONo ratings yet
- Endocrine NotesDocument1 pageEndocrine NotesShivraj singh RajputNo ratings yet
- The Role of Hormones in the Endocrine SystemDocument4 pagesThe Role of Hormones in the Endocrine SystemAshly Santhosh KNo ratings yet
- Endo AnaphysioDocument9 pagesEndo AnaphysioShelley Jade MenorNo ratings yet
- Human physiology lecture on endocrine system coordinationDocument12 pagesHuman physiology lecture on endocrine system coordinationPoorva NaikNo ratings yet
- Estrutura e Função Do Sistema Hipófise-HipotálamoDocument49 pagesEstrutura e Função Do Sistema Hipófise-HipotálamoMicheli CastroNo ratings yet
- Endocrine System TransesDocument5 pagesEndocrine System Transesadrielvamos28No ratings yet
- The endocrine system and its major glandsDocument5 pagesThe endocrine system and its major glandskatNo ratings yet
- Hypothlamic-Pituitary Physiology: Mona Abou Chebl MD. METABOLISM-2017 Lectures 1-2 March 20 2018Document197 pagesHypothlamic-Pituitary Physiology: Mona Abou Chebl MD. METABOLISM-2017 Lectures 1-2 March 20 2018rachid09No ratings yet
- 10-17-2019 Neuroendocrinology in Mental Health An UpdateDocument44 pages10-17-2019 Neuroendocrinology in Mental Health An UpdatehelalNo ratings yet
- Pharma SF 1Document19 pagesPharma SF 1John MajanNo ratings yet
- Endocrine SystemDocument13 pagesEndocrine SystemAlliyah SalindoNo ratings yet
- 3. Endocrine PhysiologyDocument7 pages3. Endocrine PhysiologyLomongo ChristianNo ratings yet
- Endocrine System Group 9Document77 pagesEndocrine System Group 9Jei SanNo ratings yet
- English For Medicine: Anthropometric Ma'Am Yuniasih Taihutu S.Ssi, Msi BiomedDocument3 pagesEnglish For Medicine: Anthropometric Ma'Am Yuniasih Taihutu S.Ssi, Msi BiomedGabriela Elisabeth TasidjawaNo ratings yet
- WFE Vs McKenzieDocument5 pagesWFE Vs McKenzieRennyRay0% (1)
- Skin Fold TestDocument5 pagesSkin Fold TestMiljana VujanovicNo ratings yet
- Caries Patterns in Primary Dentition in 3-To 5-Year-Old Children. Medellín, ColombiaDocument10 pagesCaries Patterns in Primary Dentition in 3-To 5-Year-Old Children. Medellín, ColombiaLuis Gonzaga Lopez BNo ratings yet
- 2002 Qualitative Clinical Evaluation of Scapular Dysfunction, A Reliability StudyDocument7 pages2002 Qualitative Clinical Evaluation of Scapular Dysfunction, A Reliability StudyIsrael Matías Chandia RamírezNo ratings yet
- Luke Vetti - NBPME Part 1 - LEA - Anterior Hip + Gluteal Muscles 1Document3 pagesLuke Vetti - NBPME Part 1 - LEA - Anterior Hip + Gluteal Muscles 1Tyler Lawrence CoyeNo ratings yet
- Sample RUDocument25 pagesSample RUmaria riza lagromaNo ratings yet
- Hip Knee Ankle Foot OrthosisDocument44 pagesHip Knee Ankle Foot OrthosisGulzar Ahmad100% (1)
- Ms Word Notes - Template (May 2022)Document4 pagesMs Word Notes - Template (May 2022)Jaycee Anne AregloNo ratings yet
- Posture Pro posts on posture, performance and posturologyDocument15 pagesPosture Pro posts on posture, performance and posturologyVlad PadinaNo ratings yet
- Embryology of HeartDocument6 pagesEmbryology of HeartWidelmark FarrelNo ratings yet
- Dutton Chapter 24 The Temporomandibular JointDocument47 pagesDutton Chapter 24 The Temporomandibular JointdralismNo ratings yet
- Coordination & Response QuestionDocument18 pagesCoordination & Response QuestionTeddy BooNo ratings yet
- Lumbosacral PlexusDocument3 pagesLumbosacral Plexusgehaoi4No ratings yet
- Development of OcclusionDocument49 pagesDevelopment of OcclusionSardarni Ramandeep KaurNo ratings yet
- Mcdonald 2011Document6 pagesMcdonald 2011sinem yıldırımNo ratings yet
- Anatomy Chapter 12 The Spinal Cord and The Spinal NerveDocument36 pagesAnatomy Chapter 12 The Spinal Cord and The Spinal NerveLagunamedical PharmacyNo ratings yet
- CKD Case AnalysisDocument25 pagesCKD Case Analysisしゃいな ふかみNo ratings yet
- Large Animal Internal DiseasesDocument4 pagesLarge Animal Internal Diseasesiin AgustinaNo ratings yet
- G&DDocument20 pagesG&Dahead1234No ratings yet
- NPB 101 Lecture Notes 1Document4 pagesNPB 101 Lecture Notes 1Harika NanduriNo ratings yet
- Pulmonary Vascular Anatomy & Anatomical Variants: Asha Kandathil, Murthy ChamarthyDocument7 pagesPulmonary Vascular Anatomy & Anatomical Variants: Asha Kandathil, Murthy ChamarthyFauzan Mahfuzh MashudiNo ratings yet
- Brodmann Area 13Document2 pagesBrodmann Area 13descataNo ratings yet
- Adolescence: 1. Change in HeightDocument15 pagesAdolescence: 1. Change in HeightVijay KumarNo ratings yet
- Anatomy Head and NeckDocument25 pagesAnatomy Head and NeckMARISOL GALLEGO DUQUENo ratings yet