Professional Documents
Culture Documents
Care of Patients With Problems in Oxygenation
Uploaded by
Fatima Ivan CenizaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Care of Patients With Problems in Oxygenation
Uploaded by
Fatima Ivan CenizaCopyright:
Available Formats
Care of Patients with Problems in
Oxygenation
Monday, 4 September 2023 1:11 pm
The Concept of Oxygenation Assessment
Oxygenation – mechanisms that facilitate or impair the body’s ability to supply oxygen to cells. 1. History
2. Physical Assessment
Respiration – an act of inhaling and exhaling air to transport oxygen to alveoli. 3. Inspection
So oxygen may be exchanged for carbon dioxide 4. Palpation
Carbon dioxide expelled from the body 5. Auscultation
6. Percussion
Ventilation – actual exchange of oxygen & carbon dioxide.
Pediatric Considerations
Breathing – contributes to vital oxygenation • Mouth & nose – generally, all structures are smaller and more easily obstructed than in adults.
• Pharynx – Infants’ and children’s tongues take up proportionally more space in the mouth than adults’.
Adequate oxygenation depends on a healthy & intact respiratory system. • Trachea – (windpipe)
• Infants and children have narrower tracheas that are obstructed more easily by swelling.
Steps in Oxygenation • Trachea is softer and more flexible in infants and children.
• Cricoid cartilage – like other cartilage in the infant and child, the cricoid cartilage is less developed and less rigid. It is the narrowest
• Ventilation – the process of moving gases into and out of the lungs. part of the infant’s or child’s airway.
• Diaphragm – chest wall is softer, and infants and children tend to depend more heavily on the diaphragm for breathing.
• Perfusion – the ability of the cardiovascular system to pump oxygenated blood to the
tissues and return deoxygenated blood to the lungs. Respiratory Rates
Infant: 30 - 60
• Diffusion – exchange of respiratory gases in the alveoli and capillaries. Child: 20 - 30
Adult: 12 - 20
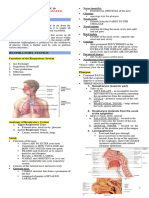
What are the primary functions of the respiratory system?
Assessment
✓ Inspection
✓ Back & front
✓ Chest symmetry
✓ Tracheal deviation
✓ Skin & nail beds color
✓ Clubbing fingers
✓ RR & pattern
✓ Using accessory muscles
✓ Nasal flaring
✓ Purses of the lips during breathing
Primary Functions
Palpation Percussion
• Delivers oxygen to the bloodstream and removes excess carbon dioxide from the body.
✓ Emphysema Determine the presence of
• Gas exchange (O2 & CO2).
✓ Pain air, fluid, or mass
• Sound production & resonation
✓ Tenderness
• Protection (from dust and microbes entering the body through mucus production, cilia, and
✓ Symmetry
coughing).
✓ Warmth & dryness
Remember that we need the cardiovascular system to work intimately with the respiratory
system because the cardiovascular system helps us transport these gases (O2 & CO2).
Auscultation
✓ Air entry
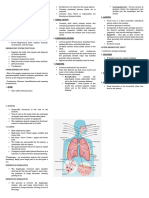
Airways & Lungs
✓ Breath sounds
✓ Compare side to side
• Upper respiratory tract
✓ Quality of pitch
• Lower respiratory tract
• Two lungs are part of the lower airway & share space in the thoracic cavity with
the heart & great vessels, trachea, esophagus & bronchi.
Assessing Lung Sounds
Upper Respiratory Tract
✓ To auscultate lung sounds, use the diaphragm of your stethoscope.
There are three normal breath sounds
▪ ¤ Bronchial breath sounds
▪ ¤ Bronchovesicular breath sounds
▪ ¤ Vesicular breath sounds
Auscultation Landmarks
Auscultating the lungs is comprised of three parts:
Landmarking correctly
Being able to identify which lobe is being auscultated and
The interpretation of adventitious sounds
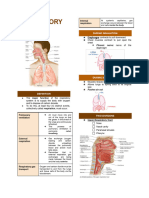
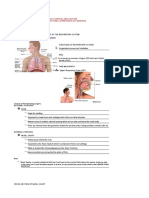
Upper Respiratory Tract
❖ Nasal cavity
✓ Covered with mucous membrane which produces fluid for moistening
✓ Contains blood vessels for warming
✓ Hairs to filter the air. –
✓ Smell odor (olfactory nerve)
Function of the sinuses ???
Lighten the skull & voice
Bronchial Breath Sounds
Loud, harsh, & high-pitched
Heard over the trachea, bronchi
(between clavicles & mid-sternum),
and over the main bronchus
Bronchovesicular Breath Sounds
Blowing sounds
Moderate intensity & pitch
Heard over large airways, on either side of the sternum,
at the sternal angle, and between scapulae
Vesicular Breath Sounds
✓ Larynx Soft breezy quality
Vocal cords (pitch, volume, resonance) Low pitched
Glottis & Epiglottis Heard over the peripheral lung area
✓ Glottis Heard best at the base of the lungs
(space between the vocal cord)
✓ Epiglottis Adventitious Breath Sounds
(cartilage that keeps the food & 1. Crackles
liquid out of the respiratory tract) * Popping, crackling, bubbling, & moist sounds.
Humidifying, Filtering & warming * Heard on inspiration
Lung Problem:
Pneumonia
Pulmonary edema
Pulmonary fibrosis
2. Rhonchi
* Rumbling sound
Quick Notes Page 1
Lung Problem:
Pneumonia
Pulmonary edema
Pulmonary fibrosis
2. Rhonchi
* Rumbling sound
Trachea * Heard on expiration
✓ C-shaped rings of cartilage ?? Lung Problem:
✓ To keep the trachea open & allow esophagus Pneumonia
to expand during swallowing Emphysema
✓ Humidifying, Filtering & warming Bronchitis
✓ Cough reflex (vagus nerve) Bronchiectasis
✓ Mucociliary escalator
(Push mucus & particles upwards 3. Wheezes
towards the larynx, cough, sneeze, * High-pitched musical sound
or blow). * Heard during both inspiration & expiration
* Louder on expiration
Lung Problem:
Emphysema
Asthma
Foreign bodies
Upper Respiratory Infection 4. Pleural Friction Rub
These infections affect your sinuses and throat. * Dry, grating sound, leather on leather
▫ Common cold * Heard on both inspiration & expiration
acute illness of the upper respiratory tract caused * Created when the visceral and parietal pleurae become inflamed and roughened
by a virus (rhinovirus). * The inflamed membranes will stick together.
S/sx: runny nose, nasal congestion, itchy throat, watery eyes, & headache. Lung Problem:
Pleurisy
▫ Epiglottitis Pneumonia
inflammation and swelling of your epiglottis caused by Pleural infarct
bacterial infection.
S/sx: pain when swallowing, severe sore throat, & Diagnostic Tests
difficulty breathing. • Chest Xray (CXR)
Four D’s Produce images of the heart, lungs, blood vessels, airways & the bones of the chest and spine.
a).Dysphagia – difficulty swallowing CXR detects and reveals:
b).Dysphonia –hoarseness or an abnormal voice * Heart-related lung problems
c).Drooling – saliva flows out in the * Collapsed lung
mouth involuntarily * Pneumonia
d).Distress – difficulty breathing or lack of oxygen * Emphysema
* Fractures
Epiglottitis is a medical emergency as the swelling blocks airflow into * Usually taken after full inspiration (deep breath)
the lungs. * Lungs are best visualized when they are well aerated
▫ Laryngitis (acute or chronic)
inflammation of your voice box (larynx) from overuse, irritation, or infection.
S/sx: hoarseness, sore throat, dry throat, & dry cough. • Arterial Blood Gases (ABG’s)
Sinusitis (sinus infection) * ABG is a blood test that requires a sample from an artery
Acute Sinusitis – spaces inside your nose (sinuses) become in your body to measure the levels of O2 & CO2 in the blood
inflamed & swollen, interfere with drainage, & cause mucus to Fatima Ivan Ceniza at 5 Sep 2023 8:21 am
buildup. * Check the balance of acids & bases in your blood,
S/sx: runny nose, postnasal drainage, headache, pain, and known as the pH balance
pressure around your forehead, & headache.
▫ Pharyngitis (sore throat)
S/sx: throat pain, runny nose, nasal congestion, & swollen lymph
nodes. It is caused by bacterial or viral infection, tonsillitis, &
allergies. • Incentive Spirometry
* Helps promote lung expansion after prolonged bed rest or surgery
* Requires patient to take a deep breath and
Lower Respiratory Tract hold it for several seconds
Lung * Performing Incentive Spirometry:
✓ Bronchial & alveolar structures ✓ Increases lung volume
✓ Right & left lobes ✓ Boosts alveolar inflation
✓ Right lung – larger with (3) lobes ✓ Promotes venous return, which helps prevent atelectasis
✓ Left lung – smaller with (2) lobes & pneumonia
Why is the right lung bigger than the left lung?
• Peak Flow
• Pulse Oximetry
Pleura (Serous Membrane) * A non-invasive method of continuously monitoring the oxygen saturation of hemoglobin.
✓ Visceral pleura covers the lung * It does not replace ABG measurement;
✓ Parietal pleura lines the thoracic cavity & contains it is an effective tool for monitoring subtle oxygen saturation changes.
nerve endings
✓ Pleural fluids between the two layers of the
pleura
✓ Lubricate the thorax and lungs
✓ Allow layers to slide smoothly over each other as
the chest expands & contracts (inspiration &
expiration). • Magnetic Resonance Imaging (MRI)
* MRI uses magnetic field & radio frequency signals instead
of a narrow beam x-ray.
* Yield a much more detailed diagnostic image than CT scans.
* Evaluate inflammatory activity in interstitial lung disease,
acute pulmonary embolism, & chronic thrombolytic
pulmonary hypertension.
• Fluoroscopic Studies
* Assist with invasive procedures like chest needle or
trans-bronchial biopsy to identify lesions.
* Study the movement of the chest wall, mediastinum,
heart & diaphragm, to detect diaphragm paralysis, &
to locate lung masses
• Lung Function Test
• Bronchoscopy
Bronchi & Bronchioles
* Direct inspection & examination of the larynx, trachea,
Bronchi (Sing. Bronchus): & bronchi using either flexible or rigid fiberoptic bronchoscope
Each bronchus leads into a lung and branches into * Examine tissues or collect secretions
smaller and smaller bronchioles, resembling an inverted * Determine the location & extent of the pathologic process &
tree. to obtain a tissue sample for diagnosis.
Bronchioles * Determine if a tumor can be resected surgically or diagnose
▫ Fine tubes that allow passage of air. bleeding sites
▫ Epithelium of bronchioles is covered with cilia and
mucus to trap and remove dust and other particles. • Lung Biopsy
▫ Bronchioles end in tiny air sacs called alveoli • Sputum studies
Alveoli • Cultures
Type I cells
□ Alveolar wall (the barrier between air & the
Quick Notes Page 2
▫ Fine tubes that allow passage of air. bleeding sites
▫ Epithelium of bronchioles is covered with cilia and
mucus to trap and remove dust and other particles. • Lung Biopsy
▫ Bronchioles end in tiny air sacs called alveoli • Sputum studies
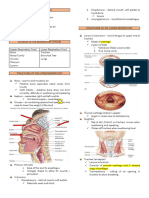
Alveoli • Cultures
Type I cells
□ Alveolar wall (the barrier between air & the • Computed Tomography (CT)
alveolar surface) * Lungs are scanned in successive layers by a
□ Gas exchange (O2 & CO2) narrow-beam x-ray.
Type II cells * Produce & provide a cross-sectional view of the chest.
□ Surfactant * Distinguish fine tissue density.
□ Lipid-type substance that coats the alveoli
Type III cells
□ Alveolar macrophages (defense mechanism)
SOME FACTS
Alveoli: functional units of the lungs where O2 is • Fluoroscopic Studies
exchanged * Assist with invasive procedures like chest needle
The wall of the alveoli are only 1 cell thick or trans-bronchial biopsy to identify lesions.
Surfactant lines the alveoli walls and helps keep alveoli * Study the movement of the chest wall, mediastinum,
from collapsing * heart & diaphragm, to detect diaphragm paralysis, & to
60-80square meters in the lungs for gas exchange locate lung masses.
Alveoli are grouped in clusters.
A network of capillaries surrounds each alveolus.
Gas Exchange
Gas exchange takes place in the alveoli. • Pulmonary Angiography
Oxygen diffuses into the blood. * Investigate thrombo-embolic disease of the lungs,
Carbon dioxide in the blood diffuses into the alveolus e.g., pulmonary emboli & congenital abnormalities of the
pulmonary vascular tree.
* Rapid injection of a radiopaque agent for radiographic study of the
pulmonary vessels.
Why are we talking about pulmonary surfactant?
Synthesized by type II cellular cells
Reduces surface tension (prevents alveolar collapse during expiration) • Thoracentesis
Prevents bacterial invasion * Aspiration of fluid & air from the pleural space.
Cleans alveoli surface * Diagnostic or therapeutic reasons.
* Removal of fluids & air (rare)from the pleural cavity.
Surface Tension * Aspiration of pleural fluid for analysis, pleural biopsy
Liquid molecules line the alveolar walls and attract each other & instillation of medication into the pleural space.
This attractive force is called surface tension
These attractive forces MUST BE overcome to expand lung
SURFACTANT reduces surface tension
Lower Respiratory Diseases
▪ Asthma
- breathing is impaired by constriction of bronchi and bronchioles. Inflammation
of the lining of the bronchial airways.
▪ Causes: precipitated by inhalation of allergens (e.g., pollen & cats), pollutants,
infection, or emotional stress.
▪ Cells that line the bronchi release chemicals that cause inflammation when
they are stimulated by irritants or allergens.
▪ S/sx: SOB, wheezing, chest tightness, & pallor
▪ Bronchitis
- inflammation of the mucous membranes of the bronchi.
S/sx: cough, fever, chest or back pain, & fatigue.
Causes: smoking, pollution, & bacterial or viral infections.
▪ Pneumonia
- acute lung tissue inflammation with alveoli consolidation commonly impairs
gas exchange.
Causes: Bacterial, fungal, or viral infections.
S/sx: dyspnea, high fever, chills, headache, severe cough, & chest pain & rusty
colored sputum.
▪ Emphysema
- permanent and irreversible destruction of
alveolar walls, resulting in loss of lung elasticity & gas exchange surface.
Air that is normally exchanged becomes trapped in the alveoli.
Unable to exhale, lungs become distended & muscles suffer from lack of O2,
becoming less elastic.
S/sx: SOB, chronic cough, weakness, drowsy, & barrel shaped chest.
Causes: Smoking, pollution, old age, & infections.
If fresh gas is not delivered to the alveoli
and blood is not delivered to the alveolar
capillaries, or if the alveolar surface is
Factors Affecting Ventilation damaged, oxygenation or CO2 elimination
may be impaired
▪ Compliance
What is lung compliance?
* lungs’ ability to stretch
* lungs’ ability to expand
Elastance
ability of a structure to return to its resting
position after being stretched
Elastic recoil
magnitude of the force to return to its resting
position
Decreased compliance occurs if the lungs and
the thorax are stiff.
How do lungs adapt and why?
Compliance of the lungs occurs due to elastic forces.
A. Elastic forces of the lung tissue itself
B. Elastic forces of the fluid that lines the inside walls of alveoli and
other lung air passage
Quick Notes Page 3
other lung air passage
A B
Elastin + Collagen Fibres Is provided by the substance
called surfactant that is present
inside walls of the alveoli.
What would influence elastance and elastic recoil?
• Disease
• Pulmonary Fibrosis
• Aging
• Emphysema (COPD)
• Obesity
• Pneumothorax
What is resistance?
* force opposes flow from one point to another (opposition of the flow of gases)
* dynamic force - involved only during movement
* Primary factors that determine resistance are:
* Size and radius (or diameter) of the airway
* Flow rate
* Secretions/water in the airway system
Could having a tracheostomy affect resistance?
* Flow into and out of the lungs will be adversely affected by obstructed airways
* Airways get smaller & shorter during exhalation = greater resistance
Causes of Increased Resistance
• Small endotracheal tube
• Bronchospasm
• Mucosal edema
• Airway obstruction (mucus, tumor, or a foreign body)
• Secretions
Quick Notes Page 4
You might also like
- Respiratory SystemDocument5 pagesRespiratory SystemGlen DaleNo ratings yet
- Gas ExchangeDocument7 pagesGas ExchangefaithdanielleyNo ratings yet
- Respiratory System Clips 1-5Document1 pageRespiratory System Clips 1-5api-552227798No ratings yet
- Cat Vs Dog Anatomy Anatomical DifferencesDocument2 pagesCat Vs Dog Anatomy Anatomical DifferencesAlliNo ratings yet
- Introduction To Terminology and Body Organization Study GuideDocument9 pagesIntroduction To Terminology and Body Organization Study GuideNgọc QuỳnhNo ratings yet
- Form 4 Revision QuizDocument80 pagesForm 4 Revision QuizEnvira LeeNo ratings yet
- The Respiratory SystemDocument63 pagesThe Respiratory Systembreanna coyneNo ratings yet
- Gen Physiology - Transes 9Document3 pagesGen Physiology - Transes 9karmylle andradeNo ratings yet
- 3 Explanation - Respiratory System Presentation - Interactive W Integrated Digital INBs MDocument19 pages3 Explanation - Respiratory System Presentation - Interactive W Integrated Digital INBs MDennis OgavarNo ratings yet
- Anaphy-Respiratory HandoutDocument7 pagesAnaphy-Respiratory HandoutAEGEL DARO TORRALBANo ratings yet
- Happ Finals Week 14Document8 pagesHapp Finals Week 14angelaggabao0No ratings yet
- Science - The Human BodyDocument31 pagesScience - The Human BodyHarshil PatelNo ratings yet
- Case Scenerio PneumoniaDocument8 pagesCase Scenerio PneumoniaEllen AngelNo ratings yet
- Thorax and LungsDocument2 pagesThorax and LungsHNo ratings yet
- Gas Exchange in HumansDocument17 pagesGas Exchange in HumansrituNo ratings yet
- 1 PDFsam KSSM 2019 DP DLP BIOLOGY FORM 4 PART 2-7Document1 page1 PDFsam KSSM 2019 DP DLP BIOLOGY FORM 4 PART 2-7deathangel88 GtNo ratings yet
- Thorax & LungsDocument14 pagesThorax & LungsRed MontemayorNo ratings yet
- In Consortium With N. Bacalso Ave. Cor Panganiban ST., 6000 Cebu City, Cebu, Philippines Tel. Nos. (032) 316-5128/ (032) 4186105 Email AddressDocument5 pagesIn Consortium With N. Bacalso Ave. Cor Panganiban ST., 6000 Cebu City, Cebu, Philippines Tel. Nos. (032) 316-5128/ (032) 4186105 Email AddressCarl Jayson LeysonNo ratings yet
- Science Topical RevisionDocument195 pagesScience Topical RevisionCharles NjithiNo ratings yet
- Complete Breathing and Exchange of GasesDocument20 pagesComplete Breathing and Exchange of GasesANo ratings yet
- How Does Respiration Work?: Key WordsDocument2 pagesHow Does Respiration Work?: Key WordstoñiNo ratings yet
- Anatomy RespirationDocument29 pagesAnatomy RespirationPatricia Rosabelle RoñoNo ratings yet
- Rle 070722Document14 pagesRle 070722kyla arachelleNo ratings yet
- Respiratory System HandoutDocument11 pagesRespiratory System HandoutJohn Carlo SantiagoNo ratings yet
- The Respiratory Structures and Breathing Mechanisms in Humans and AnimalsDocument5 pagesThe Respiratory Structures and Breathing Mechanisms in Humans and AnimalsireneNo ratings yet
- Human Gas ExchangeDocument9 pagesHuman Gas ExchangeVeer RamloghunNo ratings yet
- Gas Exchange in HumansDocument29 pagesGas Exchange in HumansLizzy AnthonyNo ratings yet
- Clinical Examination Sheet (General Examination)Document3 pagesClinical Examination Sheet (General Examination)Yara WaelNo ratings yet
- RP 1 PDFDocument9 pagesRP 1 PDFObsa AbrahimNo ratings yet
- Anaphy - MOD 1 (Finals)Document6 pagesAnaphy - MOD 1 (Finals)smzw4r78sqNo ratings yet
- 8Cb Gas Exchange (Part 1)Document19 pages8Cb Gas Exchange (Part 1)maryamNo ratings yet
- Respiratory SystemDocument2 pagesRespiratory Systemlim.angelyne0126No ratings yet
- (Unit 6) m.02 Physiology of The Nose and Paranasal SinusesDocument6 pages(Unit 6) m.02 Physiology of The Nose and Paranasal Sinusesjustme12345mNo ratings yet
- Review On Respiratory SystemDocument4 pagesReview On Respiratory Systemsecondacvalo123No ratings yet
- Anatomical and Physiological Differences Between Children and AdultsDocument13 pagesAnatomical and Physiological Differences Between Children and AdultsShubham KathareNo ratings yet
- Sci Grade 5 NotesDocument44 pagesSci Grade 5 NotesDennis MutukuNo ratings yet
- Chapter 11 Gas Exchange in Humans 23-24Document127 pagesChapter 11 Gas Exchange in Humans 23-24Huraiza AsifNo ratings yet
- Anatomy and Physiology of The Respiratory SystemDocument14 pagesAnatomy and Physiology of The Respiratory SystemAmore BuenafeNo ratings yet
- General Biology (Reviewer B5) (Page 36-49)Document14 pagesGeneral Biology (Reviewer B5) (Page 36-49)Daniela Mae NuescaNo ratings yet
- Medical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationDocument44 pagesMedical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationYman Gio BumanglagNo ratings yet
- NCM 1234 - Thorax and LungsDocument150 pagesNCM 1234 - Thorax and LungsXerxes DejitoNo ratings yet
- Medical Surgical Nursing Module 19Document4 pagesMedical Surgical Nursing Module 19weissNo ratings yet
- 2.3a CELLS ARE GROUPED INTO TISSUESDocument6 pages2.3a CELLS ARE GROUPED INTO TISSUES2023820042No ratings yet
- Bio CH8 F4 Studywithadmin PDFDocument16 pagesBio CH8 F4 Studywithadmin PDFMUHAMMAD FAREEZ HAIKAL MOHD SHAIFUDDINNo ratings yet
- Assessing The Thorax and LungsDocument100 pagesAssessing The Thorax and LungsAiren LianNo ratings yet
- Respiratory SystemDocument99 pagesRespiratory SystemNelson Louie III RicerraNo ratings yet
- Newborn Assessment Format (Pedia Ward Assessment Tool)Document5 pagesNewborn Assessment Format (Pedia Ward Assessment Tool)R GhNo ratings yet
- Pedia Prof - OamilDocument147 pagesPedia Prof - OamilOne Click Online ShopNo ratings yet
- ScP018 BiologyDocument1 pageScP018 BiologyORBeducationNo ratings yet
- Nayli Bio SBP 2019 EseiDocument5 pagesNayli Bio SBP 2019 EseiEqis AlfiesyaNo ratings yet
- Respiratory SystemDocument2 pagesRespiratory SystemjuliamaesimbreNo ratings yet
- The Respiratory SystemDocument22 pagesThe Respiratory System5130022035 ARINA DINANANo ratings yet
- Respiratory SystemDocument31 pagesRespiratory SystemMarian ReyesNo ratings yet
- 2g Gas Exchange HumansDocument33 pages2g Gas Exchange HumansAnto DefinaNo ratings yet
- Respiratory SystemDocument5 pagesRespiratory Systemden mNo ratings yet
- Lecture 6 - Respiratory DisordersDocument7 pagesLecture 6 - Respiratory DisordersMaikaylaNo ratings yet
- NCP - Ineffective Airway ClearanceDocument2 pagesNCP - Ineffective Airway Clearancelarapatricia1215No ratings yet
- 45 Mins or Less to Memorize, Pronounce and Understand Medical Terms. The Best and Most Effective Way to Build Your Medical Vocabulary Quickly!From Everand45 Mins or Less to Memorize, Pronounce and Understand Medical Terms. The Best and Most Effective Way to Build Your Medical Vocabulary Quickly!Rating: 2 out of 5 stars2/5 (2)
- Summary of Breath: The New Science of a Lost Art: A Guide to James Nestor’s BookFrom EverandSummary of Breath: The New Science of a Lost Art: A Guide to James Nestor’s BookNo ratings yet
- Chapters 6 10Document50 pagesChapters 6 10Fatima Ivan CenizaNo ratings yet
- Chest LandmarksDocument22 pagesChest LandmarksFatima Ivan CenizaNo ratings yet
- Common Acupressure Points and Its IndicationDocument10 pagesCommon Acupressure Points and Its IndicationFatima Ivan CenizaNo ratings yet
- First Principle and Types of PremisesDocument4 pagesFirst Principle and Types of PremisesFatima Ivan CenizaNo ratings yet
- Local Theorist.Document46 pagesLocal Theorist.Fatima Ivan Ceniza100% (2)
- Rhythmic Gymnastics: Physical EducationDocument7 pagesRhythmic Gymnastics: Physical EducationFatima Ivan CenizaNo ratings yet
- Bacterial MeningitisDocument11 pagesBacterial MeningitisFatima Ivan CenizaNo ratings yet
- R&W PPT 1Document43 pagesR&W PPT 1Fatima Ivan CenizaNo ratings yet
- Ball Exercise History: Group-1Document8 pagesBall Exercise History: Group-1Fatima Ivan CenizaNo ratings yet
- Protein Analysis: Electrophoresis, Blotting, and ImmunodetectionDocument24 pagesProtein Analysis: Electrophoresis, Blotting, and ImmunodetectionFatima Ivan CenizaNo ratings yet
- Chapter 21 Second Homecoming and The Liga Filipina - CenizaDocument17 pagesChapter 21 Second Homecoming and The Liga Filipina - CenizaFatima Ivan Ceniza0% (1)
- Script FinalDocument29 pagesScript FinalFatima Ivan CenizaNo ratings yet
- Spies May Be Gathering Encrypted Data To Crack With Future Quantum ComputerDocument1 pageSpies May Be Gathering Encrypted Data To Crack With Future Quantum ComputerHÀ ĐỖ VIẾTNo ratings yet
- Week 1 Macro (DDR)Document49 pagesWeek 1 Macro (DDR)Stevie Sean100% (1)
- 32 Forms of God GaneshaDocument16 pages32 Forms of God Ganeshasudhakarpk2011100% (2)
- Bhagavatam English Chapter 10bDocument22 pagesBhagavatam English Chapter 10bsrimatsimhasaneshwarNo ratings yet
- Lay Planning TypesDocument1 pageLay Planning TypesGaurav Shakya100% (1)
- Cyanocobalamin Injection Clinical Pharmacology Drug MonographDocument36 pagesCyanocobalamin Injection Clinical Pharmacology Drug MonographLaureyNo ratings yet
- Ericsson Private 5G Solution BriefDocument5 pagesEricsson Private 5G Solution BriefTanesan WyotNo ratings yet
- Branch & Category Wise Opening & Closing Rank of JEE (Main) 2019Document46 pagesBranch & Category Wise Opening & Closing Rank of JEE (Main) 2019soni dwivediNo ratings yet
- Peter Brandt InterviewDocument38 pagesPeter Brandt InterviewNishant P Kalaskar100% (1)
- Test Iii Cultural Social and Political OrganizationDocument2 pagesTest Iii Cultural Social and Political OrganizationTin NatayNo ratings yet
- Adolescents and Career DevelopmentDocument10 pagesAdolescents and Career DevelopmentMasrijah MasirNo ratings yet
- Differentiating Language Difference and Language Disorder - Information For Teachers Working With English Language Learners in The Schools PDFDocument23 pagesDifferentiating Language Difference and Language Disorder - Information For Teachers Working With English Language Learners in The Schools PDFIqra HassanNo ratings yet
- Ashfaque Ahmed-The SAP Materials Management Handbook-Auerbach Publications, CRC Press (2014)Document36 pagesAshfaque Ahmed-The SAP Materials Management Handbook-Auerbach Publications, CRC Press (2014)surajnayak77No ratings yet
- The Names of Allah and Their ReflectionsDocument98 pagesThe Names of Allah and Their ReflectionsSuleyman HldNo ratings yet
- 陳v Endometrial Cancer 2Document48 pages陳v Endometrial Cancer 201范芷紜No ratings yet
- Web Programming: GET / HTTP/1.1 ..Document16 pagesWeb Programming: GET / HTTP/1.1 ..Alecu IlieNo ratings yet
- Data Abstraction and Problem Solving With C Walls and Mirrors 6th Edition Carrano Solutions ManualDocument36 pagesData Abstraction and Problem Solving With C Walls and Mirrors 6th Edition Carrano Solutions Manualallocaturnonylgvtt100% (12)
- Compal Confidential: Ziwb2/Ziwb3/Ziwe1 DIS M/B Schematics DocumentDocument56 pagesCompal Confidential: Ziwb2/Ziwb3/Ziwe1 DIS M/B Schematics DocumentSuhpreetNo ratings yet
- CN Blue Love Rigt Lyrics (Romanized)Document3 pagesCN Blue Love Rigt Lyrics (Romanized)Dhika Halet NinridarNo ratings yet
- A B&C - List of Residents - VKRWA 12Document10 pagesA B&C - List of Residents - VKRWA 12blr.visheshNo ratings yet
- Action Research in Araling PanlipunanDocument3 pagesAction Research in Araling PanlipunanLotisBlanca94% (17)
- British Airways Culture and StructureDocument29 pagesBritish Airways Culture and Structure陆奕敏No ratings yet
- GTAG-14 Edited With Ad 05-20-20101 PDFDocument32 pagesGTAG-14 Edited With Ad 05-20-20101 PDFpiornelNo ratings yet
- MINDSET 1 EXERCISES TEST 1 Pendientes 1º Bach VOCABULARY AND GRAMMARDocument7 pagesMINDSET 1 EXERCISES TEST 1 Pendientes 1º Bach VOCABULARY AND GRAMMARanaNo ratings yet
- Safe Motherhood Ao2016-0035 Quality Antenatal Care PDFDocument9 pagesSafe Motherhood Ao2016-0035 Quality Antenatal Care PDFGa B B OrlonganNo ratings yet
- Reforms of Parvez MusharifDocument8 pagesReforms of Parvez MusharifTalha AslamNo ratings yet
- Kimberly Jimenez Resume 10Document2 pagesKimberly Jimenez Resume 10kimberlymjNo ratings yet
- Ninja 5e v1 5Document8 pagesNinja 5e v1 5Jeferson Moreira100% (2)
- Arabian Choice General Trading Co. LLCDocument1 pageArabian Choice General Trading Co. LLCjaanNo ratings yet