Professional Documents
Culture Documents
THE MESTRUAL CYCLE Notes
Uploaded by
Germin Cesa0 ratings0% found this document useful (0 votes)
4 views3 pagesOriginal Title
THE-MESTRUAL-CYCLE-Notes
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
4 views3 pagesTHE MESTRUAL CYCLE Notes
Uploaded by
Germin CesaCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 3
THE MESTRUAL CYCLE postovulatory phase).
During these two
phases, the ovaries and the endometrium
each undergo their own set of changes,
The menstrual cycle refers to the regular which are separate but related. As a
changes in the activity of the ovaries and result, each phase of the menstrual cycle
the endometrium that make reproduction has two different names to describe these
possible. The endometrium is the layer of two different parallel processes. For the
tissue lining the inside of the uterus. This ovary, the two weeks leading up to
lining consists of a functional layer, which ovulation is called the ovarian follicular
is subject to hormonal changes and is phase, and this corresponds to the
shed during menstruation, and a thin menstrual and proliferative phases of the
basal layer which feeds the overlying endometrium. Similarly, the two weeks
function allayer. The menstrual cycle following ovulation is referred to as the
actually consists of two interconnected ovarian luteal phase, which also
and synchronized processes. The ovarian corresponds to the secretory phase of the
cycle, which centers on the development endometrium. So, let’s first focus on the
of the ovarian follicles and ovulation, and preovulatory period, starting with the
the uterine or endometrial cycle, which ovarian follicular phase. This phase starts
centers on the way in which the on the first day of menstruation and
functional endometrium thickens and represents weeks one and two of a four-
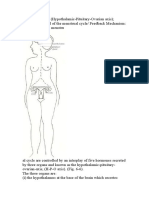
sheds in response to ovarian activity. week cycle. The whole menstrual cycle is
Menarche, which refers to the onset of controlled by the hypothalamus and the
the first menstrual period, usually occurs pituitary gland, which are like the
during early adolescence as part of masterminds of reproduction. The
puberty. Following menarche, the hypothalamus is a part of the brain that
menstrual cycle recurs on a monthly secretes gonadotropin-releasing
basis, pausing only during pregnancy, hormone, or GnRH, which causes the
until a person reaches menopause, when nearby anterior pituitary gland to release
her ovarian function declines and she follicle stimulating hormone, or FSH, and
stops having menstrual periods. The luteinizing hormone, or LH. Before
monthly menstrual cycle can vary in puberty, gonadotropin-releasing hormone
duration from 20 to 35 days, with an is released at a steady rate, but once
average of 28 days. Each menstrual cycle puberty hits, gonadotropin-releasing
begins on the first day of menstruation, hormone is released in pulses, sometimes
and this is referred to as day one of the more and sometimes less. The frequency
cycle. Ovulation, or the release of the and magnitude of the gonadotropin-
oocyte from the ovary, usually occurs 14 releasing hormone pulses determine how
days before the first day of menstruation much follicle stimulating hormone and
(i.e., 14 days before the next cycle luteinizing hormone will be produced by
begins). So, for an average 28-day the pituitary. These pituitary hormones
menstrual cycle, this means that there are control the maturation of the ovarian
usually 14 days leading up to ovulation follicles, each of which is initially made up
(i.e., the preovulatory phase) and 14 days of an immature sex cell, or primary
following ovulation (i.e., the oocyte, surrounded by layers of theca and
granulosa cells, the hormone-secreting whole lot of follicles stimulating hormone
cells of the ovary. Over the course of the and luteinizing hormone in response to
follicular phase, these oocyte-containing gonadotropin-releasing hormone. This
groups of cells, or follicles, grow and surge of follicle stimulating hormone and
compete for a chance at ovulation. During luteinizing hormone usually happens a
the first ten days, theca cells develop day or two before ovulation and is
receptors and bind luteinizing hormone, responsible for stimulating the rupture of
and in response secrete large amounts of the ovarian follicle and the release of the
the hormone androstenedione, an oocyte. You can think of it this way: for
androgen hormone. Similarly, granulosa most of the follicular phase, the pituitary
cells develop receptors and bind follicle saves its energy, then when it senses that
stimulating hormone, and in response the dominant follicle ready for release,
produce the enzyme aromatase. the pituitary uses all its energy to secrete
Aromatase converts androstenedione enough follicle stimulating hormone and
from the theca cells into 17β-estradiol, luteinizing hormone to induce ovulation.
which isa member of the estrogen family. While the ovary is busy preparing an egg
During days 10 through 14 of these for ovulation, the uterus, meanwhile, is
phases, granulosa cells also begin to preparing the endometrium for
develop luteinizing hormone receptors, in implantation and maintenance of
addition to the follicle stimulating pregnancy. This process begins with the
hormone receptors they already have. As menstrual phase, which is when the old
the follicles grow and estrogen is released endometrial lining, or functional layer,
into the bloodstream, increased estrogen from the previous cycle is shed and
levels act as a negative feedback signal, eliminated through the vagina, producing
telling the pituitary to secrete less follicle the bleeding pattern known as the
stimulating hormone. As a result of menstrual period. The menstrual phase
decreased follicle stimulating hormone lasts an average of five days and is
production, some of the developing followed by the proliferative phase,
follicles in the ovary will stop growing, during which high estrogen levels
regress and die off. The follicle that has stimulate thickening of the endometrium,
the most follicle stimulating hormone growth of endometrial glands, and
receptors, however, will continue to emergence of spiral arteries from the
grow, becoming the dominant follicle that basal layer to feed the growing functional
will eventually undergo ovulation. This endometrium. Rising estrogen levels also
dominant follicle continues to secrete help change the consistency of the
estrogen, and the rising estrogen levels cervical mucus, making it more hospitable
make the pituitary more responsive to to incoming sperm. The combined effects
the pulsatile action of gonadotropin- of this spike in estrogen on the uterus
releasing hormone from the and cervix help to optimize the chance of
hypothalamus. As blood estrogen levels fertilization, which is highest between day
start to steadily climb higher and higher, 11 and day 15 of an average 28-day cycle.
the estrogen from the dominant follicle Following ovulation, the remnant of the
now becomes a positive feedback signal – ovarian follicle becomes the corpus
that is, it makes the pituitary secrete a luteum, which is made up of luteinized
theca and granulosa cells, meaning that gradually degenerates into the
these cells have been exposed to the high nonfunctional corpus albicans. The corpus
luteinizing hormone levels that occur just albicans doesn’t make hormones, so
before ovulation. Luteinized theca cells estrogen and progesterone levels slowly
keep secreting androstenedione, and the decrease. When progesterone reaches its
luteinized granulosa cells keep converting lowest level, the spiral arteries collapse,
it to 17β-estradiol, as before. However, and the functional layer of the
luteinized granulosa cells also respond to endometrium prepares to shed through
the low luteinizing hormone menstruation. This shedding marks the
concentrations that are present after beginning of a new menstrual cycle and
ovulation by increasing the activity of another opportunity for fertilization. All
cholesterol side-chain cleavage enzyme, right, so as a quick recap - the menstrual
or P450scc for short. This enzyme cycle begins on the first day of
converts more cholesterol to menstruation. For an average 28-day
pregnenolone, a progesterone precursor. menstrual cycle, the changes which occur
So luteinized granulosa cells secrete more in the ovary during the first 14 days are
progesterone than estrogen during the called the follicular phase. Ovulation
luteal phase. Progesterone acts as a usually occurs at day 14, as a result of the
negative feedback signal on the pituitary, estrogen-induced surge in luteinizing
decreasing release of follicle stimulating hormone. The last 14 days of the cycle
hormone and luteinizing hormone. At the are the luteal phase, during which
same time, luteinized granulosa cells progesterone becomes the dominant
begin secreting inhibin, which similarly hormone. While the length of the
inhibits the pituitary gland from making follicular phase can vary, the luteal phase
follicle stimulating hormone. Both of almost always precedes the onset of
these processes result in a decline in menses by 14 days. The uterus also goes
estrogen levels, meaning that through its own set of changes. During
progesterone becomes the dominant the first 14 days of the cycle, the
hormone present during this phase of the endometrium goes through the menstrual
cycle. Together with the decreased level phase and the proliferative phase, and
of estrogen, the rising progesterone level during the last 14 days it goes through
signals that ovulation has occurred and the secretory phase.
helps make the endometrium receptive to
the implantation of a fertilized gamete.
Under the influence of progesterone, the
uterus enters into the secretory phase of
the endometrial cycle. During this time
spiral arteries continue to grow, and the
uterine glands begin to secrete more
mucus. After day 15 of the cycle, the
optimal window for fertilization begins to
close. The cervical mucus starts to thicken
and becomes less hospitable to the
sperm. Over time, the corpus luteum
You might also like
- T1-1 MS (IB Biology Topic 1 Question Bank Answer)Document27 pagesT1-1 MS (IB Biology Topic 1 Question Bank Answer)Kunakorn Kunthamas0% (2)
- The Halal Index - Pig-Based Pharmaceuticals Vol. 1 (SAMPLE)Document29 pagesThe Halal Index - Pig-Based Pharmaceuticals Vol. 1 (SAMPLE)Halal Media Malaysia100% (4)
- SCIENCE-10-Q3 WORKSHEET REVISED COPY-week-1-7Document46 pagesSCIENCE-10-Q3 WORKSHEET REVISED COPY-week-1-7Gian Evangelista67% (6)
- Moral VS Non Moral StandardsDocument20 pagesMoral VS Non Moral StandardsGermin CesaNo ratings yet
- Moral VS Non Moral StandardsDocument20 pagesMoral VS Non Moral StandardsGermin CesaNo ratings yet
- New Microsoft Office Word DocumentDocument16 pagesNew Microsoft Office Word DocumentDavid LeeNo ratings yet
- Placenta Previa Case StudyDocument59 pagesPlacenta Previa Case StudyKen KenNo ratings yet
- Reproductive System Practical ReportDocument10 pagesReproductive System Practical Reportrishabhvasisht03No ratings yet
- PDocument5 pagesPmedstudNo ratings yet
- ILA4Document7 pagesILA4Fadhlina OmarNo ratings yet
- The Menstrual Cycle Transkip-1Document4 pagesThe Menstrual Cycle Transkip-1selyNo ratings yet
- The Menstrual Cycle TranskipDocument5 pagesThe Menstrual Cycle Transkiplen lehangNo ratings yet
- And Luteinizing Hormone or LHDocument4 pagesAnd Luteinizing Hormone or LHSherrie Mae RoncalNo ratings yet
- TP Anglais FinalDocument7 pagesTP Anglais FinalGift NgongoNo ratings yet
- Female Reproductive SystemDocument3 pagesFemale Reproductive SystemJayricDepalobosNo ratings yet
- Menstrual CycleDocument24 pagesMenstrual Cyclemeez rameezNo ratings yet
- Ncma Sir VDocument3 pagesNcma Sir VMilca DavidNo ratings yet
- by Ems - Osmosis Notes: GinecoDocument4 pagesby Ems - Osmosis Notes: GinecoEmilly MeloNo ratings yet
- Menstrual Cycle HormonesDocument3 pagesMenstrual Cycle HormonesAine GrahamNo ratings yet
- Menstrual Cycle Stages and Hormone RegulationDocument6 pagesMenstrual Cycle Stages and Hormone RegulationNida RidzuanNo ratings yet
- HORMONAL CYCLE EXPLAINEDDocument20 pagesHORMONAL CYCLE EXPLAINEDGunaNo ratings yet
- Female Reproductive CycleDocument4 pagesFemale Reproductive CycleTRASH MAILNo ratings yet
- Haromonal Cycle Introduction-: HormoneDocument15 pagesHaromonal Cycle Introduction-: Hormonesuman guptaNo ratings yet
- Female HormoneDocument43 pagesFemale Hormoneامجد حسين جواد كاظمNo ratings yet
- MCN Cover To Cover ?Document247 pagesMCN Cover To Cover ?Elsid Nathaniel S. MartinNo ratings yet
- Hormonal Cycles: Ovarian CycleDocument5 pagesHormonal Cycles: Ovarian CycleashuNo ratings yet
- IntroDocument7 pagesIntroibrahim.21hm32No ratings yet
- Mesntrual CycleDocument3 pagesMesntrual CycleNabd NabdNo ratings yet
- Menstrual CycleDocument6 pagesMenstrual Cyclebuhari rabiuNo ratings yet
- 1642497170754_Family Health 1 - CopyDocument20 pages1642497170754_Family Health 1 - CopyGoogle MediaNo ratings yet
- Hormonal Cycles: Presented By: Miss. M.K.Kaku Nursing TutorDocument23 pagesHormonal Cycles: Presented By: Miss. M.K.Kaku Nursing TutorKaku ManishaNo ratings yet
- Topic-Menstural Cycle: Name-Divya Sharma Roll No-8 & Bharti Kotwal Roll No-7Document15 pagesTopic-Menstural Cycle: Name-Divya Sharma Roll No-8 & Bharti Kotwal Roll No-7chanderNo ratings yet
- Physiology of Female Reproductive System The Ovarian CycleDocument9 pagesPhysiology of Female Reproductive System The Ovarian CycleAmiraah MasriNo ratings yet
- The Menstrual Cycle by CK-12Document7 pagesThe Menstrual Cycle by CK-12woman in stemNo ratings yet
- Menstrual Cycle AutosavedDocument33 pagesMenstrual Cycle Autosavedნინო ღვინაძე100% (1)
- Menstrual Cycle Biology ProjectDocument4 pagesMenstrual Cycle Biology ProjectaddyNo ratings yet
- Ovarian and Menstrual CyclesDocument7 pagesOvarian and Menstrual CyclesMohamed FarahatNo ratings yet
- Menstrual CycleDocument41 pagesMenstrual CyclesharimileeratnamNo ratings yet
- ReproductionDocument6 pagesReproductionAbelle EnsuiNo ratings yet
- The Menstrual CycleDocument6 pagesThe Menstrual CycleiwennieNo ratings yet
- Menstrual CycleDocument6 pagesMenstrual CycleAthirah BidinNo ratings yet
- CycleDocument2 pagesCycleChinchay Guinto100% (1)
- The Menstrual Cycle PDFDocument6 pagesThe Menstrual Cycle PDFPerry Sin100% (1)
- Haromonal Cycle Introduction-: HormoneDocument10 pagesHaromonal Cycle Introduction-: Hormonesuman guptaNo ratings yet
- Notes MentrualDocument4 pagesNotes MentrualAngel JagongNo ratings yet
- Pregnancy Preparation: The Menstrual CycleDocument4 pagesPregnancy Preparation: The Menstrual CycleTobias GummNo ratings yet
- Biomed Womens HealthDocument16 pagesBiomed Womens HealthAndres CardenasNo ratings yet
- The Physiology of the Menstrual Cycle and FertilizationDocument3 pagesThe Physiology of the Menstrual Cycle and FertilizationAdri SinclaireNo ratings yet
- Mammalian Reproductive SystemDocument50 pagesMammalian Reproductive SystemLeena MuniandyNo ratings yet
- FOLLICULAR PHASE: (Ovarian Changes ..Cycle Days: Endocrine System NCLEXDocument52 pagesFOLLICULAR PHASE: (Ovarian Changes ..Cycle Days: Endocrine System NCLEXAsniah Hadjiadatu AbdullahNo ratings yet
- Fisiologia Sistema Genital Feminino (Resumo)Document3 pagesFisiologia Sistema Genital Feminino (Resumo)farmaciaNo ratings yet
- MCN Menstrual Cycle LatestDocument8 pagesMCN Menstrual Cycle LatestsophienNo ratings yet
- Normal Menstrual Cycle The ProcessDocument6 pagesNormal Menstrual Cycle The ProcessBrett StevensonNo ratings yet
- Producing Gametes and the Menstrual CycleDocument7 pagesProducing Gametes and the Menstrual CycleRichard GrayNo ratings yet
- Female Physiology 1Document2 pagesFemale Physiology 1JayricDepalobosNo ratings yet
- UntitledDocument8 pagesUntitledPJ Manuel SuerteNo ratings yet
- The Menstrual CycleDocument18 pagesThe Menstrual CycleSakshi Halve100% (1)
- Bio12 c10 10 7Document8 pagesBio12 c10 10 7Eric McMullenNo ratings yet
- Physiology of the menstrual cycle explainedDocument6 pagesPhysiology of the menstrual cycle explainedTeef SumayaNo ratings yet
- Coordinated Functions of The Reproductive, Endocrine And2Document27 pagesCoordinated Functions of The Reproductive, Endocrine And2Second BooksNo ratings yet
- Reproduction & Growth CycleDocument96 pagesReproduction & Growth Cyclebiologi88No ratings yet
- Physilogy of Menstrual CycleDocument13 pagesPhysilogy of Menstrual CycleVineet Kumar LalNo ratings yet
- Menstrual Cycle: An IntroductionDocument6 pagesMenstrual Cycle: An IntroductionAudrie Allyson GabalesNo ratings yet
- Physiology of OvulationDocument7 pagesPhysiology of OvulationAza Patullah ZaiNo ratings yet
- Menstrual CycleDocument8 pagesMenstrual CycleAlloiBialba100% (1)
- Female Repoductive CyclesDocument11 pagesFemale Repoductive CyclesbokkNo ratings yet
- Menstrual cycle, hormones, and female reproductive systemDocument3 pagesMenstrual cycle, hormones, and female reproductive systemKHRISTINE KAYE SALUDESNo ratings yet
- Physiology of Women Reproduction SystemDocument52 pagesPhysiology of Women Reproduction Systemram kumarNo ratings yet
- Hormone Reset Diet: Restore Your Metabolism, Sex Drive and Get Your Life Back, All While Losing 15lbsFrom EverandHormone Reset Diet: Restore Your Metabolism, Sex Drive and Get Your Life Back, All While Losing 15lbsNo ratings yet
- Bioethics Semifinals NotesDocument17 pagesBioethics Semifinals NotesGermin CesaNo ratings yet
- Trans 1 Medication Administration 1Document23 pagesTrans 1 Medication Administration 1Germin CesaNo ratings yet
- Drug Study - SampleDocument7 pagesDrug Study - SampleGermin CesaNo ratings yet
- PharmaDocument4 pagesPharmaGermin CesaNo ratings yet
- Assignment For Physical EducationDocument1 pageAssignment For Physical EducationGermin CesaNo ratings yet
- OrphenadrineDocument4 pagesOrphenadrineGermin CesaNo ratings yet
- ParacetamolDocument4 pagesParacetamolGermin CesaNo ratings yet
- 4.1 Bioethics and ResearchDocument58 pages4.1 Bioethics and ResearchGermin CesaNo ratings yet
- AmlodipineDocument4 pagesAmlodipineGermin CesaNo ratings yet
- KCL TabDocument3 pagesKCL TabGermin CesaNo ratings yet
- Nursing responsibilities for losartan administrationDocument6 pagesNursing responsibilities for losartan administrationGermin CesaNo ratings yet
- 4 PaDocument4 pages4 PaGermin CesaNo ratings yet
- Clinical Portrait Pertinent DataDocument9 pagesClinical Portrait Pertinent DataGermin CesaNo ratings yet
- 3 DPDocument2 pages3 DPGermin CesaNo ratings yet
- Cesa-BSN2G-Assignment 3 Reflection Paper (Elimination)Document1 pageCesa-BSN2G-Assignment 3 Reflection Paper (Elimination)Germin CesaNo ratings yet
- NCM 109 Orientation - PPTX 6Document63 pagesNCM 109 Orientation - PPTX 6Germin CesaNo ratings yet
- Fertilization To ComputationsDocument7 pagesFertilization To ComputationsGermin CesaNo ratings yet
- CHAPTER 16 Reproductive System PDFDocument172 pagesCHAPTER 16 Reproductive System PDFAl-waleed JulkanainNo ratings yet
- An Introspective Analysis: What It Means To Be Part of A SocietyDocument1 pageAn Introspective Analysis: What It Means To Be Part of A SocietyGermin CesaNo ratings yet
- Leopolds Contraction Tests - MaternalDocument6 pagesLeopolds Contraction Tests - MaternalGermin CesaNo ratings yet
- Gonads - Basic Functional Unit Female Reproductive Organ EXTERNAL (8 Kabuok) Mon Pubis/VineriesDocument8 pagesGonads - Basic Functional Unit Female Reproductive Organ EXTERNAL (8 Kabuok) Mon Pubis/VineriesGermin CesaNo ratings yet
- RLE LAB MidDocument425 pagesRLE LAB MidGermin CesaNo ratings yet
- MS GCS Cornual Ectopic PregnancyDocument57 pagesMS GCS Cornual Ectopic PregnancyCarelle Faith Serrano AsuncionNo ratings yet
- Reproduction: Helen Mason Senior Lecturer in Reproductive EndocrinologyDocument61 pagesReproduction: Helen Mason Senior Lecturer in Reproductive EndocrinologyronaldjacksonNo ratings yet
- Graphing Hormones LabDocument4 pagesGraphing Hormones LabSarahlynn CampbellNo ratings yet
- Worksheet. Menstrual Cycle.Document5 pagesWorksheet. Menstrual Cycle.Rigel Del CastilloNo ratings yet
- NEET Revision Test Answer KeyDocument11 pagesNEET Revision Test Answer KeykrishnaNo ratings yet
- Ovarian Cyst: ClassificationDocument31 pagesOvarian Cyst: ClassificationZozo Shadap100% (2)
- Endometrium by Shanojan ThiyagalingamDocument3 pagesEndometrium by Shanojan ThiyagalingamDr. Shanojan Thiyagalingam, FRCPC FACPNo ratings yet
- Anatomy Physiology of Female Reproductive SystemDocument96 pagesAnatomy Physiology of Female Reproductive SystemRabin BasnetNo ratings yet
- Q3 Science Reviewer - PopoDocument10 pagesQ3 Science Reviewer - PopoXY PLAYZNo ratings yet
- Module 12 - Human Reproduction Health PDFDocument137 pagesModule 12 - Human Reproduction Health PDFvarunNo ratings yet
- Material of Class Xii - BiologyDocument181 pagesMaterial of Class Xii - BiologyAravindhan RaviNo ratings yet
- MCN Finals NotesDocument287 pagesMCN Finals NotesbabyboyNo ratings yet
- Cervical Cancer Case PresDocument40 pagesCervical Cancer Case PresEna100% (1)
- 5grade 10 October QE 2018-2019Document21 pages5grade 10 October QE 2018-2019Lucille Gacutan AramburoNo ratings yet
- Human Reproduction: Type A: Multiple Choice QuestionsDocument7 pagesHuman Reproduction: Type A: Multiple Choice Questionsriya sharmaNo ratings yet
- Fisiologi HaidDocument3 pagesFisiologi HaidAndi Farid ANo ratings yet
- Dasar-Dasar Biomolekuler Reproduksi Wanita: Rahmatina B. HermanDocument29 pagesDasar-Dasar Biomolekuler Reproduksi Wanita: Rahmatina B. HermansilmiNo ratings yet
- Fogsi Position Statement On The Use of ProgestogensDocument9 pagesFogsi Position Statement On The Use of ProgestogensRaviraj TirukeNo ratings yet
- Care of The Mother and The Fetus During The Perinatal PeriodDocument22 pagesCare of The Mother and The Fetus During The Perinatal PeriodRoshin Tejero100% (1)
- Jaypee Gold Standard Mini Atlas Series® Embryology (2010) (PDF) (UnitedVRG)Document217 pagesJaypee Gold Standard Mini Atlas Series® Embryology (2010) (PDF) (UnitedVRG)reyod0% (1)
- Human Anatomy and PhysiologyDocument6 pagesHuman Anatomy and PhysiologyEduardo AnerdezNo ratings yet
- SOAL Masuk 2018Document142 pagesSOAL Masuk 2018Yoza FirdaozNo ratings yet
- Animal Reproduction - II MCQsDocument23 pagesAnimal Reproduction - II MCQsawaisNo ratings yet