Professional Documents
Culture Documents
RESPIRATORY PHYSIO REVIEW
Uploaded by
Meccanazaren Susvilla Bojorque0 ratings0% found this document useful (0 votes)
24 views8 pagesOriginal Title
Respiratory Physiology Review
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
24 views8 pagesRESPIRATORY PHYSIO REVIEW
Uploaded by
Meccanazaren Susvilla BojorqueCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 8
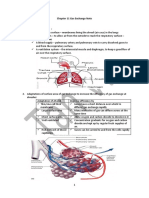
RESPIRATORY PHYSIOLOGY REVIEW Blood reservoir – The lung receives the venous blood to the respiratory muscles causing
to the respiratory muscles causing them to contract or
from the right ventricle. Due to the capacity of the relax.
Functions of the Respiratory System pulmonary circulation to receive blood, the lung acts
as a reservoir from which the left side of the heart The pneumotaxic center in the upper pons
The functions of the respiratory system are: functions to maintain rhythmic respirations. It
draws blood.
Oxygen supplier. The job of the respiratory system is stimulates the expiratory center, which then sends
to keep the body constantly supplied with oxygen. Filtering mechanism – The lung also constantly filters inhibitory signals to the inspiratory center. Inspiration
the air we breathe and removes trapped particles ends and expiration begins. Strong stimuli from the
Elimination. Elimination of carbon dioxide. through the mucocillary clearance mechanism and the pneumotaxic center result in shorter inspiration, and
lymphatic system. The lung also acts as a filtering mild stimuli results in a longer one. The apneustic
Gas exchange. The respiratory system organs
mechanism for blood by removing particles such gas center sends stimuli to the inspiratory center and
oversee the gas exchanges that occur between the
bubbles, small fibrin or blood clots, fat cells, prolongs inspiration. The pneumotaxic center usually
blood and the external environment.
aggregates of platelets or WBC, and other pieces of overrides the apneustic center. Impulses are
Passageway. Passageways that allow air to reach the cellular debris. transmitted from lung receptors, which are receptors
lungs. that respond to physical changes in the pulmonary
Metabolism – The lung produces some very important system, and chemoreceptors, which are receptors
Humidifier. Purify, humidify, and warm incoming air. chemicals that serve physiological regulatory that respond to changes in oxygen or carbon dioxide
functions such as vascular dilatation, blood clotting, concentrations, through the sympathetic and
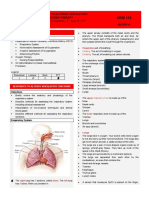
Respiratory Anatomy and Physiology lung structural stability and neurotransmitters. Some parasympathetic divisions of the ANS and the
Functionally the respiratory system consists of chemicals passing through the lungs are converted respiratory centers in the brain stem.
the conducting and respiratory zones, namely the into their more active form, such as angiotensin I,
upper and lower respiratory tract. The conducting produced by the kidneys, which is converted to Respiratory Volumes and Capacities
zones consist of the nasal cavities, pharynx, larynx angiotensin II, a potent vasoconstrictor
Tidal volume. Normal quiet breathing moves
and trachea. Control of respiration approximately 500 ml of air into and out of the lungs
The purpose of the conducting zones is to with each breath.
Breathing is usually involuntary but voluntary
filter, humidify, warm and allow the passage of air to breathing is necessary when the person is doing other Inspiratory reserve volume. The amount of air that can
the lower respiratory zones. The respiratory zones are activities such as walking, talking, singing, etc. In be taken in forcibly over the tidal volume is the
the site of gas exchange, containing the respiratory these cases homeostatic changes in ventilatory rate inspiratory reserve volume, which is normally between
bronchioles, alveolar ducts and alveoli. (Tortora & and volume are adjusted automatically by the nervous 2100 ml to 3200 ml.
Grabowski, 2000). system to maintain normal gas exchange
Expiratory reserve volume. The amount of air that can
In addition to the vital function of gas exchange, The lung is innervated by the autonomic be forcibly exhaled after a tidal expiration, the
the respiratory system fulfils the following nervous system (ANS). Fibers of the sympathetic expiratory reserve volume, is approximately 1200 ml.
functions division in the lung branch from the upper thoracic
and cervical ganglia of the spinal cord, while fibers of Residual volume. Even after the most strenuous
Acid base regulation – Through the process of expiration, about 1200 ml of air still remains in the
ventilation, the lung removes CO2 and regulates the the parasympathetic division travel in the vagus
nerve, which is important in the regulation of lungs and it cannot be voluntarily expelled; this is
pH of the body. Regulation of pH is accomplished by called residual volume, and it is important because it
removing volatile acid (ie acid converted into the ventilation.
allows gas exchange to go on continuously even
gaseous state; in this case, carbonic acid converted to The respiratory centers in the brain stem between breaths and helps to keep the alveoli
CO2). control involuntary ventilation by transmitting impulses inflated.
Vital capacity. The total amount of exchangeable air is Mechanical dead space – This is the Arterial blood gas measures the following parameters:
typically around 4800 ml in healthy young men, and contribution to the patient's dead space through the pH, PaO2, PaCO2. The ABG derives the base excess or
this respiratory capacity is the vital capacity, which is addition of respiratory circuit attachments, etc. deficit, HCO3 and SaO2.
the sum of the tidal volume, inspiratory reserve Measured Parameters:
volume, and the expiratory reserve volume. Physiologic / total dead space – This value
is the sum of anatomic and alveolar dead space. It 1. pH – this reflects the hydrogen ion
Dead space volume. Much of the air that enters the represents the total volume in the airways and alveoli concentration in the blood.
respiratory tract remains in the conducting zone not participating in gas exchange. 2. PaO2 – reflects the partial pressure of oxygen
passageways and never reaches the alveoli; this is in the arterial blood
called the dead space volume and during a normal LUNG MECHANICS
3. PaCO2 – reflects the partial pressure of
tidal breath, it amounts to about 150 ml. 1. Compliance carbon dioxide in the arterial blood
Functional volume. The functional volume, which is 2. Normally inspiration is an active process,
accomplished through the expansion of the Acid base imbalance assessment of ABG4
the air that actually reaches the respiratory zone and
contributes to gas exchange, is about 350 ml. lungs and the thorax. The ease with which the Buffers. The body will always try to maintain
lungs and thorax can be expanded, or homeostasis and restore the pH to normal. This
Spirometer. Respiratory capacities are measured with distended, is referred to as compliance. Total process is called compensation and is controlled by
a spirometer, wherein as a person breathes, the compliance therefore depends not only on the the use of buffers. Buffers are weak acids or bases
volumes of air exhaled can be read on an indicator, elasticity of the lung tissue, but also on that of that prevent sudden change in pH.
which shows the changes in air volume inside the the thoracic cage.
apparatus. Examples of buffer systems are:
LUNG MECHANICS: COMPLIANCE
DEAD SPACE VENTILATION - Phosphate Buffer System
Compliance is reduced by any factor that:
Dead space is the amount of gas that is involved in - Hb/OxyHb System - Hb releases O2 and attracts H
ventilation but does not take part in gas exchange. - Reduces the natural elasticity of the lungs, eg ions
(Not all the air in each breath is used for the exchange fibrosis, or interstitial edema.
of oxygen and carbon dioxide. About a third of every - Protein buffer system - Carboxyl (COO-H+) and
- Reduces the total number of functional alveoli, eg Amine (NH3-) groups.
resting breath is exhaled exactly as it came into the atelectasis or airway obstruction.
body.) - Bicarbonate - Carbonic Buffer System
- Increases the stiffness of the chest wall, eg splinting
There are four types of dead space: because of pain. Acidosis (pH < 7.35) is the abnormal increase in H ions
(acid) or loss of HCO3 (base).
Anatomic dead space – This refers to the - Decreases the stiffness of the chest wall, eg post-
amount of gas that fills the conducting passages of sternotomy, resulting in decreased FRC. Alkalosis (pH > 7.45) is the abnormal increase in HCO3
the airway and is not involved in gas exchange. In (base) or loss of H ions (acid).
most adults, this value is estimated at 2 mL/kg of body - Checks the ability of the thorax to increase in
volume, eg abdominal distension. Acidosis and alkalosis may be RESPIRATORY or
weight. For the normal sized adult, it is usually about
METABOLIC in nature:
150 mL. Therefore, if the normal tidal volume is 500
ARTERIAL BLOOD GASES
mL, only 350 mL of tidal volume is actually involved in 1. Conditions leading to Acidosis/Alkalosis
gas exchange as illustrated below. Measurements of arterial blood gases (ABGs) are involve a multitude of physiological processes
obtained to assess adequacy of oxygenation and such as:
Alveolar dead space – This is the amount of
ventilation, to evaluate acid-base status by measuring 2. Respiratory/renal dysfunction
gas filling the alveoli that does not contribute to gas
the respiratory and non-respiratory components, and 3. Disturbances of tissue oxygenation, circulation
exchange.
to monitor effectiveness of therapy. 4. Substance ingestion
5. Electrolyte loss/gain A protective mechanism within the pharyngeal cavity The lungs are also described in terms of their lobes.
prevents food or drink from entering the lower The lobes lie obliquely in the thoracic cavity. The right
NORMAL OXYGENATION PHYSIOLOGY REVIEW respiratory tract. The glottis is the opening into the lung has three lobes; the left lung has two lobes. The
Adequate oxygenation of the body depends on lower respiratory tract. The epiglottis is pendulous inferior lobes are the largest. Most of the inferior lobes
a healthy, intact respiratory system. tissue that covers the tracheal opening during lie in the posterior thoracic cavity. Each lung has a
The respiratory system obtains oxygen from swallowing or any time foreign matter contacts the pleural lining to aid respiration and separate it
the air and transports it into the alveoli, where glottis. The closure of the epiglottis is a reflexive
from the other lung. The pleural lining has two
oxygen diffuses into capillaries and is carried response. The lower respiratory tract is enclosed in
layers, and a minute amount of fluid between the
by the blood to all cells of the body. the musculoskeletal structures of the neck and
thoracic cavity. layers allows the structures to glide across one
The respiratory system also passes carbon another during respiration. The final portion of the
dioxide from the body. The trachea, which sits midline in the neck, is the lower respiratory system is the air sacs. The
The upper respiratory system is the inlet for air entrance for air into the lungs. During normal outcroppings of the air sacs are called alveoli. The
into the body. breathing, the muscular structures of the neck are alveoli are the portion of the lungs that fulfills the
The nose is the typical inlet. relaxed and the larynx easily rises and falls with each function of the respiratory system. Alveoli are not
The nose is divided into two nares, which are swallow. The chest wall effortlessly and symmetrically
directly connected to a specific bronchiole, but are
moist, pink, mucosa-lined passageways. rises and falls with each equally spaced breath.
interconnected to the terminal airways and to each
Nares warm, humidify, and filter air as it is Inspiration is half the rate of expiration. Eupnea
describes breathing within the expected respiratory other. This facilitates the filling of each alveoli with air.
breathed into the nose.
rates. Auscultation, listening to the body’s sounds with The sounds of air moving into and out of the
The upper respiratory tract has two protective a stethoscope, is an important diagnostic tool. When lobes at the alveolar level are soft and breezy,
mechanisms to prevent foreign matter from entering airways are clear and functioning, auscultation of the defined as vesicular.
the lower respiratory tract: sneezing and cilia. trachea will reveal a tubular sound of air movement,
as if produced through a tube. The alveoli have specialized cells that produce
Foreign matter that enters the nose irritates surfactant. Surfactant controls surface tension and
the nasal passages and induces sneezing. The trachea bifurcates (divides in two) into two keeps the alveoli from collapsing and sticking to
Sneezing is a reflexive action that clears the bronchi to access the right and left lungs the right themselves. Surfactant is produced only with
upper airway. This reflexive action is active bronchus is shorter and wider than the left. Each adequate oxygenation. Alveolar macrophages keep
even in the neonatal period. bronchus further divides into bronchioles that the alveoli region free of microbes and are swept
Cilia are microscopic fine hairs within the terminate in the alveoli sacs. These passageways for upward from the alveolar region by cilia in the
posterior portion of the nares that trap small
air dilate and contract. The trachea and larger bronchi airway passages. Macrophages are large cells of
particles of foreign matter to prevent their entry
are supported by C-shaped cartilage rings, as well as the immune system that remove waste and
into the lower respiratory tract. The cilia propel
foreign matter into the pharynx to be coughed by smooth muscle. The smaller bronchioles are harmful microorganisms from the alveoli and from
out or swallowed supported by smooth muscles only. Bronchioles other areas of the body. Mast The typical drive to
deliver air to the alveoli. These air passageways dilate breathe occurs due to hypercarbia, an increased
Breathing also happens through the mouth, which and contract as the autonomic nervous system level of carbon dioxide in the blood. Receptor sites
allows air to enter the respiratory system through regulates the smooth muscles supporting them. The within the medulla and pons are sensitive to carbon
the pharyngeal cavity. The respiratory system movement of air within the bronchial tree creates a dioxide levels in the blood. Elevated levels of carbon
shares this cavity with the gastrointestinal system,
mixture of sounds of air flowing through a tube and dioxide induce inhalation of air into the lungs.
providing passage for air during breathing and for
the breeziness of the open alveolar lung fields. This is Yawns and sighs are induced after periods of shallow
food or drink during swallowing.
termed bronchovesicular sound breathing or breath holding. Exhalation is a passive
response to relaxation of the muscles of
respiration. The typical breathing rate is regularly hypercarbia. Hypercarbia interferes with the body’s PHYSICAL ASSESSMENT TECHNIQUES
spaced, with inspiration half as long as expiration (I:E ability to respond appropriately to increased levels of
Physical assessment of the patient involves
= 1:2). Normal respiratory rates range from 30 to 60 carbon dioxide. When this happens, instead of
obtaining a history and the physical examination. With
breaths per minute in newborns to 10 to 20 breaths hypercarbia initiating the breathing response,
the frail elderly patient, the history may be a
per minute in an adult. Depth of normal inspiration is decreased levels of oxygen initiate the drive to
combination of admission information, answers from
about 500 mL of air with each breath. The expansion breathe. This is commonly seen in individuals
the next of kin, and comments from the patient. The
of the chest wall is observable, but is neither shallow with chronic obstructive pulmonary disease
assessment is divided into the data base and the
nor great. (COPD) resulting from prolonged cigarette
focused assessment. Prior to assessing any patient,
smoking because smoking is the primary cause of
Quality of breathing requires a patent airway, one that be sure that the procedure is explained to the patient
prolonged elevated levels of carbon dioxide.
is open and free of obstruction. Receptor sites in the and provision for privacy is assured.
aortic arch and carotid arteries monitor oxygen. These
receptors induce inspiration when oxygen levels fall
below normal. Stretch receptors within the lungs
control the volume of air inhaled with each breath.
During relaxed states, the lungs will fill to
approximately 0.5 L. Strenuous exercise results in
deeper breaths of increasing volume to meet the
oxygen demands of skeletal muscles. The ability of
the respiratory system to deliver oxygen to the blood
depends on an inflated and well-oxygenated alveolus
and an associated capillary with freely flowing blood
at an adequate blood pressure. The movement of
oxygen across the alveolar– capillary membrane
into a well-perfusing capillary is defined as the
ventilation-perfusion (V-Q) ratio. The concentration
levels of oxygen and carbon dioxide dictate the
movement of each gas across the alveolar–capillary
membrane.
Alterations and Manifestations Alterations in
oxygenation can be described in relation to changes
in breathing patterns, patency of airway, or
interference with gas exchange. Damage to the
supporting thoracic structure, either by injury or
disease, can interfere with effective respiration.
Irritation or inflammation of the respiratory mucosa
also affects the ability of the respiratory system to
obtain adequate oxygenation for the cells within the
body. The typical drive to breathe occurs due to
The physical examination portion of the Cardiovascular disease - a history of Congestive Chest pain - may be associated with cardiovascular
assessment requires the techniques of Heart Failure or disorders or musculoskeletal
inspection, palpation, percussion, and
auscultation.
Pulmonary Edema may in fact be the problem that is chest pain. The lungs do not have pain-
presented to you which would have symptoms of sensitive nerves. The pleura and
Inspection - is informed observation, or looking at your shortness of breath. tracheobronchial tree are sensitive to pain.
patient with a purpose. Adequate lighting is an Pleuritic pain usually hurts more during
Chest surgery - find out if patient has had any surgery
important tool for inspection. Inspection takes place deep breaths.
on the lungs.
during all components of the assessment from the
health history through the physical examination. Allergies - chronic allergies may predispose client t REVIEW OF SYSTEMS
other respiratory disorders. actual pulmonary problems
Palpation - all parts of the body can be palpated
including tissues, bones, muscles, glands, organs, PRESENT ILLNESS cardiovascular difficulties - differentiate if the
hair, and skin. When palpating, make sure that your shortness of breath is from
hands are warm. Try to get the patient to relax, since Progression of symptoms
tension can tighten muscles and alter the palpation Dyspnea or shortness of breath with chronic a cardiac or respiratory origin. Acute onset of
technique. One method for helping the patient to relax obstructive pulmonary disease (COPD) congestive heart failure is treated
is to have him/her take some slow deep breaths in differently than pneumonia or bronchitis.
and out of the mouth. This serves the purpose of usually progresses over a long period of time.
relaxing the muscles and helping the patient to focus neurological problems - since the stimulus for
An acute situation produces dyspnea at rest. Acute breathing is in the brain, the breathing
on something else. Palpation can be done with
onset of dyspnea or shortness
different parts of the hands for assessing different pattern you see could represent a neurological
qualities. of breath is important for assessing problem
Auscultation - involves listening with the ear or a pneumonia, pneumothorax, hemothorax, or
stethoscope. Try to keep the environment free of pulmonary embolism.
extraneous sounds. For example, turn the T.V. off Cough occurring daily over 2 or more years is Inspection
when auscultating. Essential to auscultation is a good indicative of chronic bronchitis. Respiratory Rate and Pattern - to observe your
stethoscope. The stethoscope should have short,
patient, make sure that he/she is at rest and unaware
thick, tubing and contain a bell and a diaphragm. Coughing is usually caused by irritants such
that you are observing the respirations.
as smoking.
Percussion - involves tapping one finger on top of the
Rate - normal respiratory rate is 12 to 20 / minute
finger of the other hand to determine sounds from Sputum production
underlying structures. Helpful to determine if there is eupnea - normal rate and rhythm
purulent sputum is associated with lung
air or consolidation. For the lungs, percussion is tachypnea - fast respiratory rate
abscess
performed at the location of the intercostals spaces. bradypnea - slow respiratory rate
viscous sputum associated with chronic
PAST HEALTH HISTORY obstructive pulmonary disease (COPD) Patterns
Blood tinged sputum can occur with
Respiratory System - ask if patient has had apnea - absence of breathing, may be periodic
tuberculosis, carcinoma, or pulmonary
pneumonia, asthma, bronchitis, emphysema,
embolism.
tuberculosis, and how often he/she gets colds.
hyperpnea - deeper respirations with normal Nasal flaring - seen in respiratory distress. shaped chest. You will notice that chest
rate excursion is decreased. Try this on a co-
Cheyne-Stokes - respirations gradually worker to determine normal chest excursion.
become faster and deeper than normal, than Tracheal deviation - the trachea is normally midline. Vocal or tactile fremitus - use the top portion of
slower with periods of apnea. When tracheal deviation occurs, it will shift to the side each palm and place on the back. For vocal
Biot's - faster and deeper respirations than of least resistance. fremitus have the patient say "99". Vibrations
normal, with abrupt pauses in between. Each will be transmitted from the tracheobronchial
breath has the same depth. May occur in pneumothorax - to affected side tree to your palms and fingers. Check for
spinal meningitis or other central nervous tension pneumothorax - unaffected side symmetry of vibrations. Fremitus will be more
system conditions. pleural effusion - unaffected side pronounced in the upper airways where there
Kussmaul's - faster and deeper respirations atelectasis - affected side is a greater amount of air flow. The level
without pauses. Can occur from renal failure or where you no longer feel vibration is the
Restlessness, anxiety, apprehension, headache, diaphragm.
metabolic acidosis (especially in diabetes with
confusion, disorientation, impaired judgment,
hyperglycemia). diminished or absent - pleural effusion,
hypotension, tachycardia, yawning,
Apneustic - prolonged gasping inspiration thickened pleura, or pneumothorax
followed by short inefficient expiration. Central cyanosis (on mouth and lips) are related to slightly increased - consolidation
Can occur from lesions in the brain's hypoxia (decreased oxygen in the blood).
Anterior Chest
respiratory center.
This hypoxia can result from COPD, pneumonia,
Tracheal position - normally trachea is midline.
central nervous system depression,
Gently place fingers in the space between the
Chest Wall Movements neuromuscular disorders, musculoskeletal sternum and the clavicle to determine position.
disorders, Adult Respiratory Distress Sternum and cartilages - palpate for
Asymmetrical - can occur with tension Syndrome (ARDS), or pulmonary edema. tenderness or deformity.
pneumothorax, a large pleural effusion, Drowsiness, tremors, confusion, generalized
consolidation, and atelectasis. Percussion
seizures, or headache are related to
Retractions - can be seen with bronchial hypercapnia (increased levels of carbon Overview - the lungs normally have a resonant or
plugging that may be seen in asthma or dioxide). This results from hypoventilation that hollow sound. To percuss place the middle finger on
COPD. can be seen in COPD or central nervous the surface of the chest and tap firmly with the middle
Use of accessory muscles - Increases work of system depression. finger of the other hand (mediate percussion). When
breathing common during an acute phase of percussing the lungs be sure to place your finger in
COPD. Palpation
the intercostal spaces and not on the ribs. Percuss in
Expiratory bulging of chest - this is an opposite Posterior Chest a side to side manner on the anterior and posterior
or paradoxical observation. Can be seen with chest walls.
flail chest. Chest Expansion - Place both hands on the
back with the thumbs pointed to the spine. Percussion Notes
General Signs and Symptoms
Have the patient take a deep breath. Watch for
Resonance - represents air-filled spaces. This
Pursed-lip breathing - seen with the COPD equal movement of your hands. This is called
is normal over the peripheral lung fields.
patient that needs to breath this way to get checking for bilateral chest excursion. In the
trapped air in the alveoli expelled. COPD patient, they tend to have a barrel
Hyperresonance (tympany) - drumlike sound Respiratory Tumors – Masses, cysts, or Emphysema
representing excess air in the space. Seen in tumors invading the lungs.
Vascular Lung Disease
pneumothorax or emphysema.
Some obstructive lung diseases are:
Dullness or flatness - represents fluid or solid Notable vascular lung diseases include:
tissue in area and will vary with patient's Emphysema
position if fluid is gravity dependent. Seen in Pulmonary edema
Bronchitis
emothorax, hydrothorax, empyema, or Pulmonary embolism
Asthma
pleuraleffusion. Pulmonary hypertension
Chronic obstructive pulmonary disease
Auscultation (COPD) Infectious Lung Disease
Bronchiectasis
Overview - auscultation is one of the most useful Infectious Lung Diseases are, as the name
Byssinosis
assessment techniques for evaluating changes in the suggests, typically caused by one of many infectious
Bronchiolitis
respiratory system. Breath sounds are produced by agents able to infect the mammalian respiratory
Asbestos
turbulent airflow through the airways. Crackles, system (for example the bacterium Streptococcus
rhonchi and wheezing are heard through auscultation. Notable restrictive lung diseases include: pneumonia).
Auscultation should be done in the same sequencing
Acute respiratory distress syndrome (ARDS) The clinical features and treatment options
as shown for palpation. Auscultation of the right
Asbestosis vary greatly between infectious lung disease sub-
middle lobe is accomplished by listening on the right
Fibrosis types as each type may be caused by a different
side in the midaxillary line. The diaphragm of the
infectious agent, with different pathogenesis and
stethoscope is used. When listening to lungs you will Hypersensitivity pneumonitis
virulence.
listen to a full inspiration and expiration at each Infant respiratory distress syndrome (IRDS)
location. Lung Cancer Features also vary between:
Mechanical diseases affecting pulmonary
Categorizing Lung Diseases Upper respiratory tract infection, including
musculature, including myasthenia gravis
strep throat and the common cold; and
Another method is to divide respiratory orders by Neurologic diseases affecting the ability of the
body to alter respiration rate, including spinal Lower respiratory tract infection, including
categories of:
cord injury pneumonia and pulmonary tuberculosis
Obstructive Lung Diseases – Increased airway Pleural effusion Respiratory neoplasms are most often malignant,
resistance.
Pleurisy although there are non-malignant neoplasms which
Restrictive Lung Diseases – Loss of airway
Sarcoidosis can affect lung tissue.
compliance.
Severe acute respiratory syndrome (SARS)
Parenchymal Lung Diseases – Destruction of Respiratory neoplasms include the following:
the air sacs or alveoli. Parenchymal Lung Disease
Mesothelioma
Vascular Lung Diseases – Affect the
pulmonary capillary blood vessels that impair
Notable parenchymal diseases include: Small cell lung cancer
the exchange of oxygen and carbon dioxide. Non-small cell lung cancer
COPD
Infectious Lung Diseases – Caused by Non-neoplastic respiratory tumors:
Sarcoidosis
bacteria invading the lungs. Tuberculosis cysts, other non-neoplastic
Pulmonary fibrosis
masses
Acute Respiratory by a variety of bacteria and viruses. Acute bronchitis gradually destroyed. Smoking is the leading cause of
can last from a few days to 10 emphysema. As it worsens,
Distress Syndrome
days. But the cough that comes with acute bronchitis emphysema turns the alveoli — into large, irregular
(ARDS)
may last for several weeks after pockets with gaping holes in their
A sudden failure of the respiratory system that occurs
the infection has gone Obstructive inner walls. This reduces the number of air sacs and
when fluid builds up in alveoli,
keeps some of the oxygen entering
Ventilation
resulting in destruction. In a short time, breathing
your lungs from reaching your bloodstream. In
becomes difficult, resulting in ❤
addition, the elastic fibers that hold open
hypoxemia. Most often occurs in critically ill persons. 1
the alveoli are slowly destroyed, so that they collapse
Severe shortness of breath — the
when exhaling preventing gas
main symptom of ARDS — usually develops within a
from leaving the lungs Obstructive
few hours to a few days after the
Parenchymal
original disease or trauma. ARDS is fatal in 25 to 40
percent of the people who develop Chronic obstructive pulmonary disease (COPD) refers Diffusion
to a group of lung diseases that
it. Restrictive
block airflow and make it increasingly difficult for to
Diffusion
breathe. Emphysema and chronic
bronchitis are the two main conditions that make up
COPD, but COPD can also refer to
damage caused by chronic asthmatic bronchitis.
Obstructive
Asthma is a chronic lung disease that inflames and
narrows the airways. Asthma causes Parenchymal
recurring periods of wheezing, chest tightness, Diffusion
shortness of breath, and coughing Obstructive
Ventilation
Emphysema is a condition that limits the flow of air
when breathing out. Emphysema
Bronchitis inflammation of the bronchial tubes, the occurs when the air sacs at the ends of your smallest
major airways into the lungs. It may be caused air passages (bronchioles) are
You might also like
- Pulmonary VentilationDocument24 pagesPulmonary VentilationAreeba KhanNo ratings yet
- Respiratory SystemDocument7 pagesRespiratory SystemNgenyi ChiarittaNo ratings yet
- ANATOMY OF THE RESPIRATORY SYSTEMzDocument12 pagesANATOMY OF THE RESPIRATORY SYSTEMzalthea jade villadongaNo ratings yet
- OXYGENATIONDocument8 pagesOXYGENATIONJo Marchianne Pigar0% (1)
- Gaseous Exchange in HumanDocument14 pagesGaseous Exchange in HumanIzzul Syahmi100% (1)
- The Respiratory SystemDocument21 pagesThe Respiratory SystemdeepakNo ratings yet
- Breathing and RespirationDocument30 pagesBreathing and Respirationhamzahazard527No ratings yet
- The Respiratory System: An OverviewDocument33 pagesThe Respiratory System: An OverviewCess Abad AgcongNo ratings yet
- Respiratory System PhysiologyDocument35 pagesRespiratory System PhysiologySherwan R Shal100% (2)
- Respiratory SystemDocument23 pagesRespiratory SystemsanathNo ratings yet
- Structural and Functional Organization of The Respiratory System. Stages of Respiration. Regulation of RespirationDocument39 pagesStructural and Functional Organization of The Respiratory System. Stages of Respiration. Regulation of RespirationMohammed Faizuddin siddiquiNo ratings yet
- Anaphy Lab ReviewerDocument12 pagesAnaphy Lab ReviewerCamille ParedesNo ratings yet
- Gas Exchange Notes ExplainedDocument6 pagesGas Exchange Notes ExplainedKai TongNo ratings yet
- Respiratory System - Week 3Document66 pagesRespiratory System - Week 3Reentsha EllyNo ratings yet
- Respiration Lecture NotesDocument7 pagesRespiration Lecture Notesamrutha mohandasNo ratings yet
- Chapter_13_Respiratory_System - CopyDocument4 pagesChapter_13_Respiratory_System - CopyfrommeyerjamesNo ratings yet
- A Level Gaseous Exchange Continued - 032759Document13 pagesA Level Gaseous Exchange Continued - 032759onyangaismail12No ratings yet
- Respiiiraatatoory SystemDocument78 pagesRespiiiraatatoory Systempriyanshuraj717No ratings yet
- Respiratory Physiology IDocument47 pagesRespiratory Physiology IDeea LobonțiuNo ratings yet
- Review of Respiratory PhysiologyDocument53 pagesReview of Respiratory PhysiologyMiftahul IfahNo ratings yet
- Respiratory System (Week 14)Document33 pagesRespiratory System (Week 14)Krisha Mabel TabijeNo ratings yet
- Respiratory SystemDocument192 pagesRespiratory SystemQuolette Constante100% (1)
- Functional Anatomy of The Respiratory SystemDocument3 pagesFunctional Anatomy of The Respiratory SystemRica Mae TingcoNo ratings yet
- 4 Alveolar Ventilation & Cough, Sneeze ReflexDocument47 pages4 Alveolar Ventilation & Cough, Sneeze ReflexNimra TariqNo ratings yet
- Nutrition and Diet TherapyDocument7 pagesNutrition and Diet TherapyNEIL NETTE S. REYNALDONo ratings yet
- Respiratory Physiology PostedDocument25 pagesRespiratory Physiology PostedYeni PuspitaNo ratings yet
- Chapter 15Document6 pagesChapter 15Holy HaeinNo ratings yet
- Respiratory System: Dr. Agung Kurniawan, MkesDocument31 pagesRespiratory System: Dr. Agung Kurniawan, MkesJojo BodhoNo ratings yet
- Respiratory system-3Document18 pagesRespiratory system-3samaranadotzulfiqarNo ratings yet
- Basic Respiratory Mechanics: Ventilation, Diffusion, and Gas ExchangeDocument36 pagesBasic Respiratory Mechanics: Ventilation, Diffusion, and Gas ExchangeRizqi Luqmanul HakimNo ratings yet
- Notes of Human Physiology Class 11Document9 pagesNotes of Human Physiology Class 11ADWAITH LALUNo ratings yet
- Johnson Jerry Alan Chinese Medical Qigong Therapy Vol 5-141-160Document20 pagesJohnson Jerry Alan Chinese Medical Qigong Therapy Vol 5-141-160toanbauNo ratings yet
- Oxygen InsufficiencyDocument16 pagesOxygen Insufficiencydeolzf100% (1)
- BREATHING & GASES EXCHANGEDocument7 pagesBREATHING & GASES EXCHANGEKankana Biswas100% (1)
- Introduction To Respiratory SystemDocument5 pagesIntroduction To Respiratory SystemDr Md Abedur RahmanNo ratings yet
- Breathing and Exchange of GasesDocument5 pagesBreathing and Exchange of Gaseslpc4944No ratings yet
- Dr. Fachrul Jamal, Span Kic: SMF Anestesiologi & Icu Fk-Unsyiah/Bpk Rsuza Banda AcehDocument62 pagesDr. Fachrul Jamal, Span Kic: SMF Anestesiologi & Icu Fk-Unsyiah/Bpk Rsuza Banda AcehSayed Saiful WajirNo ratings yet
- Regulation of RespirationDocument5 pagesRegulation of Respirationdanielfrontin2002No ratings yet
- Respiratory System 8Document32 pagesRespiratory System 8Naanmatha PuspanathanNo ratings yet
- WEEK 11 ANPH 111Document6 pagesWEEK 11 ANPH 111itsmearonsupanNo ratings yet
- Chapter 15Document6 pagesChapter 15Holy HaeinNo ratings yet
- Chapter 11 BioDocument18 pagesChapter 11 BioRylee LNo ratings yet
- Respiratory System Physiology PDFDocument121 pagesRespiratory System Physiology PDFVizhiNo ratings yet
- Referat Jason Respiratory PhysiologyDocument7 pagesReferat Jason Respiratory PhysiologyJason ChristopherNo ratings yet
- The Respiratory SystemDocument2 pagesThe Respiratory SystemRaluca MoldovanNo ratings yet
- Respiratory System Handout Explains Lung Functions & AnatomyDocument10 pagesRespiratory System Handout Explains Lung Functions & AnatomyMr. DummyNo ratings yet
- Physiology Linda Costanzo 6thDocument50 pagesPhysiology Linda Costanzo 6thMoonnime BlueNo ratings yet
- The respiratory system and how it worksDocument17 pagesThe respiratory system and how it worksangad singhNo ratings yet
- Normal Oxygen Transport: Susanne A ClarkDocument256 pagesNormal Oxygen Transport: Susanne A Clarkghoncheh0% (1)
- 118 Skills Lab-Week 1-Responses To Altered Ventilatory FunctionsDocument8 pages118 Skills Lab-Week 1-Responses To Altered Ventilatory FunctionsKeisha BartolataNo ratings yet
- Overview of The Resp System - PADocument27 pagesOverview of The Resp System - PAwajdjnbNo ratings yet
- 118 Skills Lab-Week 1-Responses To Altered Ventilatory FunctionsDocument8 pages118 Skills Lab-Week 1-Responses To Altered Ventilatory FunctionsKeisha BartolataNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemCraigNo ratings yet
- BIO 2701 Lecture Notes Exchange With The EnvironmentDocument11 pagesBIO 2701 Lecture Notes Exchange With The EnvironmentDorothy MayakaNo ratings yet
- Ila College of Health: Respiratory PhysiologyDocument29 pagesIla College of Health: Respiratory PhysiologyDaniel DendaNo ratings yet
- Self test 3Document6 pagesSelf test 3202310446No ratings yet
- Respiratory SystemDocument5 pagesRespiratory SystemPreeti ChouhanNo ratings yet
- Respiratory gymnastics (Translated): Purification - Health - Strength - EnergyFrom EverandRespiratory gymnastics (Translated): Purification - Health - Strength - EnergyNo ratings yet
- Lung Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandLung Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Theme 2: Family Prayer As A Space For Social SupportDocument1 pageTheme 2: Family Prayer As A Space For Social SupportMeccanazaren Susvilla BojorqueNo ratings yet
- Format CDX Guidelines 1Document7 pagesFormat CDX Guidelines 1Meccanazaren Susvilla BojorqueNo ratings yet
- Nursing Care Plan Profile: M.B (20 Yrs Old) Allergic RhinitisDocument1 pageNursing Care Plan Profile: M.B (20 Yrs Old) Allergic RhinitisMeccanazaren Susvilla Bojorque100% (1)
- The Child With Endocrine/Metabolic Dysfunction: Thyroid Gland DisordersDocument17 pagesThe Child With Endocrine/Metabolic Dysfunction: Thyroid Gland DisordersMeccanazaren Susvilla BojorqueNo ratings yet
- Grant ABS-CBN Franchise through People's InitiativeDocument10 pagesGrant ABS-CBN Franchise through People's InitiativeCorey LimNo ratings yet
- Ethical Issues in Community PracticeplainformatDocument14 pagesEthical Issues in Community PracticeplainformatMeccanazaren Susvilla BojorqueNo ratings yet
- Eb FormDocument2 pagesEb FormrhodzsulitNo ratings yet
- TURKEY Globalization Impact On HeritagesGROUP03Document10 pagesTURKEY Globalization Impact On HeritagesGROUP03Meccanazaren Susvilla BojorqueNo ratings yet
- Family Health Assessment ToolDocument7 pagesFamily Health Assessment ToolMeccanazaren Susvilla BojorqueNo ratings yet
- Family Health Assessment ToolDocument7 pagesFamily Health Assessment ToolMeccanazaren Susvilla BojorqueNo ratings yet
- Eb FormDocument2 pagesEb FormrhodzsulitNo ratings yet
- The Role of Technology MedicationsDocument10 pagesThe Role of Technology MedicationsMeccanazaren Susvilla BojorqueNo ratings yet
- Ethical Issues in Community PracticeplainformatDocument14 pagesEthical Issues in Community PracticeplainformatMeccanazaren Susvilla BojorqueNo ratings yet
- The Child With Endocrine/Metabolic Dysfunction: Thyroid Gland DisordersDocument17 pagesThe Child With Endocrine/Metabolic Dysfunction: Thyroid Gland DisordersMeccanazaren Susvilla BojorqueNo ratings yet
- NCM 14N - Critical Thinking - Group 2Document3 pagesNCM 14N - Critical Thinking - Group 2Meccanazaren Susvilla BojorqueNo ratings yet
- Pre-Assessment & Learning Activities - NCM 13N - CHN 2 - BojorqueDocument4 pagesPre-Assessment & Learning Activities - NCM 13N - CHN 2 - BojorqueMeccanazaren Susvilla BojorqueNo ratings yet
- Reflection: Group 2 - Bojorque - Eupeña - Joya - Lastimosa - Martin - Quinto - SR - Robles - Sakay - Samillano - VilarDocument4 pagesReflection: Group 2 - Bojorque - Eupeña - Joya - Lastimosa - Martin - Quinto - SR - Robles - Sakay - Samillano - VilarMeccanazaren Susvilla BojorqueNo ratings yet
- San Juan de Dios Educational Foundation, Inc.: 2772-2774 Roxas Boulevard, Pasay City 1300 PhilippinesDocument5 pagesSan Juan de Dios Educational Foundation, Inc.: 2772-2774 Roxas Boulevard, Pasay City 1300 PhilippinesMeccanazaren Susvilla BojorqueNo ratings yet
- The Role of Technology MedicationsDocument10 pagesThe Role of Technology MedicationsMeccanazaren Susvilla BojorqueNo ratings yet
- Excerpts From Customs of The TagalogsDocument7 pagesExcerpts From Customs of The TagalogsMeccanazaren Susvilla BojorqueNo ratings yet
- PA (Thorax Lungs Breast Axillae Heart)Document3 pagesPA (Thorax Lungs Breast Axillae Heart)Meccanazaren Susvilla BojorqueNo ratings yet
- 2017 Article 88Document14 pages2017 Article 88iskandarNo ratings yet
- Dr. S.K. Haldar's Lectures On Industrial Health For AFIH Students - Occu. Lung Dis Asbestosis Silicosis ByssinosisDocument26 pagesDr. S.K. Haldar's Lectures On Industrial Health For AFIH Students - Occu. Lung Dis Asbestosis Silicosis ByssinosisDr. Prakash Kulkarni100% (2)
- ASMPH Pulmo Histo Lab ImagesDocument58 pagesASMPH Pulmo Histo Lab ImagesKatNo ratings yet
- Therapeutic Strategies in CopdDocument378 pagesTherapeutic Strategies in Copdgermany23No ratings yet
- Respiratory System: Parts of The Upper Respiratory TractDocument2 pagesRespiratory System: Parts of The Upper Respiratory TractGRascia OnaNo ratings yet
- Substance Use and Abuse For Students 2018-2019Document50 pagesSubstance Use and Abuse For Students 2018-2019ZauraNo ratings yet
- Case Presentation: AsthmaDocument21 pagesCase Presentation: AsthmaCalingalan Hussin CaluangNo ratings yet
- 2 Respiratory TractDocument39 pages2 Respiratory TractnanxtoyahNo ratings yet
- Massage Therapies MT1 Cautions and ContraindicationsDocument21 pagesMassage Therapies MT1 Cautions and ContraindicationsRobertDochertyNo ratings yet
- Ibps Po-Xi Prelims Mt-94: Sreedhar'sDocument12 pagesIbps Po-Xi Prelims Mt-94: Sreedhar'sMaheshNo ratings yet
- Standardizing Asphyxia ClassificationDocument9 pagesStandardizing Asphyxia ClassificationCharin GressiliaNo ratings yet
- Health Lesson 1 Dangers of Cigarette SmokingDocument103 pagesHealth Lesson 1 Dangers of Cigarette SmokingKathleen Gail RagaNo ratings yet
- Monday Tuesday Wednesday Thursday Friday: I. ObjectivesDocument4 pagesMonday Tuesday Wednesday Thursday Friday: I. ObjectivesMary Joselyn BodionganNo ratings yet
- Pranvaha - Rahim FileDocument6 pagesPranvaha - Rahim FileRahimshaikhNo ratings yet
- Human Respiratory System: Gas Exchange ProcessDocument15 pagesHuman Respiratory System: Gas Exchange Processpraneeth satishNo ratings yet
- S3 Breathing SystemDocument18 pagesS3 Breathing System廖思明No ratings yet
- Dissection of The Amphibian Respiratory System and Mammalian Excretory SystemDocument6 pagesDissection of The Amphibian Respiratory System and Mammalian Excretory System门门No ratings yet
- Chest Physical Exam in Infants & ChildrenDocument14 pagesChest Physical Exam in Infants & ChildrenHuda KamalNo ratings yet
- Step Notes: RRC SampleDocument9 pagesStep Notes: RRC SampleRafia 0205No ratings yet
- Respiratory SystemDocument85 pagesRespiratory SystemWilson chumpukaNo ratings yet
- Science 9: Quarter 1 Respiratory SystemDocument23 pagesScience 9: Quarter 1 Respiratory Systemjelly marie flores0% (1)
- NCLEX Test Questions With RationaleDocument46 pagesNCLEX Test Questions With Rationaletetmetrangmail.com tet101486No ratings yet
- Upper and Lower Respiratory Disease (2003)Document552 pagesUpper and Lower Respiratory Disease (2003)Obreja Andreea Georgiana100% (1)
- Broncho Pneumonia 1Document28 pagesBroncho Pneumonia 1NocReyesNo ratings yet
- MED SURG OUTLINE Chapter 14 Care of Patients With Disorders of Upper Respiratory SystemDocument6 pagesMED SURG OUTLINE Chapter 14 Care of Patients With Disorders of Upper Respiratory SystemMichaela LemanNo ratings yet
- Anatomy and Physiology of Respiratory SystemDocument34 pagesAnatomy and Physiology of Respiratory SystemSamson SeiduNo ratings yet
- Concept Map Finished 2Document6 pagesConcept Map Finished 2api-352785497100% (1)
- Fire Safety in The HomeDocument46 pagesFire Safety in The Homemonch1998No ratings yet
- The Respiratory System: Lecture Presentation by Patty Bostwick-Taylor Florence-Darlington Technical CollegeDocument30 pagesThe Respiratory System: Lecture Presentation by Patty Bostwick-Taylor Florence-Darlington Technical CollegeFakultas Kedokteran UnhanNo ratings yet
- Fundamentos de Auscultacion Pulmonar NEJM PDFDocument8 pagesFundamentos de Auscultacion Pulmonar NEJM PDFMaría Fernanda RíosNo ratings yet