Professional Documents
Culture Documents
Cartilage
Uploaded by
Abdi Asiis Omar Mohamed0 ratings0% found this document useful (0 votes)
62 views26 pagesHistology by dr abdiasis omar mohamed
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentHistology by dr abdiasis omar mohamed
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
62 views26 pagesCartilage
Uploaded by
Abdi Asiis Omar MohamedHistology by dr abdiasis omar mohamed
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 26
Cartilage
By dr Abdiasis Omar Mohamed
MBBS
Introduction
• Cartilage is a tough, durable form of supporting
connective tissue, characterized by an extracellular
matrix (ECM) with high concentrations of GAGs and
proteoglycans, interacting with collagen and elastic
fibers.
• Cartilage ECM has a firm consistency that allows the
tissue to bear mechanical stresses without permanent
distortion.
• In the respiratory tract, ears, and nose, cartilage forms
the framework supporting softer tissues.
• Because of its resiliency and smooth, lubricated
surface, cartilage provides cushioning and sliding
regions within skeletal joints and facilitates bone
movements.
• Cartilage also guides development and growth of
long bones, both before and after birth.
• Cartilage consists of cells called chondrocytes (Gr.
chondros, cartilage + kytos, cell) embedded in the
ECM which unlike connective tissue proper contains
no other cell types.
• Chondrocytes synthesize and maintain all ECM
components and are located in matrix cavities called
lacunae.
• The physical properties of cartilage depend on
electrostatic bonds between type II collagen fibrils,
hyaluronan, and the sulfated GAGs on densely
packed proteoglycans.
• All types of cartilage lack vascular supplies and
chondrocytes receive nutrients by diffusion from
capillaries in surrounding connective tissue (the
perichondrium).
• As might be expected of cells in an avascular tissue,
chondrocytes exhibit low metabolic activity. Cartilage
also lacks nerves.
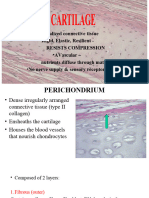
• The perichondrium is a sheath of dense connective
tissue that surrounds cartilage in most places, forming
an interface between the cartilage and the tissues
supported by the cartilage.
• The perichondrium harbors the blood supply serving
the cartilage and a small neural component.
• Articular cartilage, which covers the ends of bones in
movable joints and which erodes in the course of
arthritic degeneration, lacks perichondrium and is
sustained by the diffusion of oxygen and nutrients
from the synovial fluid.
Hyaline cartilage
• Hyaline (Gr. hyalos, glass) cartilage, the most
common of the three types, is homogeneous and
semitransparent in the fresh state.
• In adults hyaline cartilage is located in the articular
surfaces of movable joints, in the walls of larger
respiratory passages (nose, larynx, trachea, bronchi),
in the ventral ends of ribs, where they articulate with
the sternum, and in the epiphyseal plates of long
bones, where it makes possible longitudinal bone
growth.
• Matrix
• The dry weight of hyaline cartilage is nearly 40%
collagen embedded in a firm, hydrated gel of
proteoglycans and structural glycoproteins.
• Most of the collagen in hyaline cartilage is type II,
although small amounts of minor collagens are also
present.
• Aggrecan (250 kDa), with approximately 150 GAG
side chains of chondroitin sulfate and keratan sulfate,
is the most abundant proteoglycan of hyaline
cartilage.
• Another important component of cartilage matrix is
the structural multiadhesive glycoprotein
chondronectin.
• Chondrocytes
• Because cartilage matrix is avascular, chondrocytes
respire under low-oxygen tension. Hyaline cartilage
cells metabolize glucose mainly by anaerobic
glycolysis.
• Nutrients from the blood diffuse to all the
chondrocytes from the cartilage surface, with
movements of water and solutes in the cartilage
matrix promoted by intermittent tissue compression
and decompression during body movements.
• Chondrocyte synthesis of sulfated GAGs and
secretion of proteoglycans are accelerated by many
hormones and growth factors.
• A major regulator of hyaline cartilage growth is the
pituitary-derived protein called growth hormone or
somatotropin.
• This hormone acts indirectly, promoting the
endocrine release from the liver of insulin-like
growth factors, or somatomedins, which directly
stimulate the cells of hyaline cartilage
• Perichondrium
• Except in the articular cartilage of joints, all hyaline
cartilage is covered by a layer of dense connective
tissue, the perichondrium, which is essential for the
growth and maintenance of cartilage.
Elastic cartilage
• Elastic cartilage is essentially similar to hyaline
cartilage except that it contains an abundant network
of elastic fibers in addition to a meshwork of collagen
type II fibrils which give fresh elastic cartilage a
yellowish color.
• More flexible than hyaline cartilage, elastic cartilage
is found in the auricle of the ear, the walls of the
external auditory canals, the auditory (Eustachian)
tubes, the epiglottis, and the upper respiratory tract.
• Elastic cartilage in these locations includes a
perichondrium similar to that of most hyaline
cartilage.
• Throughout elastic cartilage the cells resemble those
of hyaline cartilage both physiologically and
structurally.
Fibrocartilage
• Fibrocartilage takes various forms in different
structures but is essentially a mingling of hyaline
cartilage and dense connective tissue.
• It is found in intervertebral discs, in attachments of
certain ligaments, and in the pubic symphysis—all
places where it serves as very tough, yet cushioning
support tissue for bone.
• Chondrocytes of fibrocartilage occur singly and often
in aligned isogenous aggregates, producing type II
collagen and other ECM components, although the
matrix around these chondrocytes is typically sparse.
• Intervertebral discs of the spinal column are
composed primarily of fibrocartilage and act as
lubricated cushions and shock absorbers preventing
damage to adjacent vertebrae from abrasive forces or
impacts.
Cartilage formation, growth, & repair
• All cartilage forms from embryonic mesenchyme in
the process of chondrogenesis.
• The first indication of cell differentiation is the
rounding up of the mesenchymal cells, which retract
their extensions, multiply rapidly, and become more
densely packed together.
• In general the terms “chondroblasts” and
“chondrocytes” respectively refer to the cartilage
cells during and after the period of rapid proliferation.
• During embryonic development, the cartilage
differentiation takes place primarily from the center
outward; therefore the more central cells have the
characteristics of chondrocytes, whereas the
peripheral cells are typical chondroblasts.
• The superficial mesenchyme develops as the
perichondrium.
• Once formed, the cartilage tissue enlarges both by
interstitial growth, involving mitotic division of
preexisting chondrocytes, and by appositional
growth, which involves chondroblast differentiation
from progenitor cells in the perichondrium.
• Except in young children, damaged cartilage
undergoes slow and often incomplete repair,
primarily dependent on cells in the perichondrium
which invade the injured area and produce new
cartilage.
• In damaged areas the perichondrium produces a scar
of dense connective tissue instead of forming new
cartilage.
• The poor capacity of cartilage for repair or
regeneration is due in part to its avascularity and low
metabolic rate.
THE END
You might also like
- Advanced farriery knowledge: A study guide and AWCF theory course companionFrom EverandAdvanced farriery knowledge: A study guide and AWCF theory course companionNo ratings yet
- مستند PDF 3Document24 pagesمستند PDF 3alshb7 gamesNo ratings yet
- JARINGAN TULANG RAWAN DAN FUNGSINYADocument20 pagesJARINGAN TULANG RAWAN DAN FUNGSINYAArtha CimutNo ratings yet
- Cartilage: Ethel Marie M. Mangada, RMTDocument34 pagesCartilage: Ethel Marie M. Mangada, RMTAesthetics MinNo ratings yet
- Cartilage: Histology Part 1: Module2, Unit 2Document30 pagesCartilage: Histology Part 1: Module2, Unit 2Obansa JohnNo ratings yet
- Cartilage and BoneDocument51 pagesCartilage and Bonet_225561332No ratings yet
- Tissue Biochemistry ChapterDocument25 pagesTissue Biochemistry ChapterMaria ArshadNo ratings yet
- Bones and CartilageDocument69 pagesBones and Cartilagesjs6r8wwv9No ratings yet
- Cartilage and BoneDocument58 pagesCartilage and BoneGer BengNo ratings yet
- Cartilage and Bone Structure and FunctionDocument8 pagesCartilage and Bone Structure and FunctionRehab OmerNo ratings yet
- Cartilage Tissue Types and Structure in 40 CharactersDocument2 pagesCartilage Tissue Types and Structure in 40 CharactersMuhammet Fatih CantepeNo ratings yet
- Bone and Cartilage Histology GuideDocument43 pagesBone and Cartilage Histology GuideMila AnriyaniNo ratings yet
- Cartilage (Structure & Types)Document26 pagesCartilage (Structure & Types)muhammadumarnawazsattiNo ratings yet
- 2 Cartilage and BoneDocument51 pages2 Cartilage and BoneJulia Anne RosalemNo ratings yet
- 1.2 Cartilage and BoneDocument27 pages1.2 Cartilage and BonePema GaleyNo ratings yet
- CartilageDocument32 pagesCartilageMajd HusseinNo ratings yet
- L10 Cartilage and BoneDocument43 pagesL10 Cartilage and BoneCarinaTingEeNo ratings yet
- Tissues: Dr. Tanveer Ahmed Khan Lecturer RLCPDocument65 pagesTissues: Dr. Tanveer Ahmed Khan Lecturer RLCPShafaqat Ghani Shafaqat GhaniNo ratings yet
- CartilageDocument33 pagesCartilageRahaf MajadlyNo ratings yet
- CartilageDocument20 pagesCartilageDoctora NourhanNo ratings yet
- CartilageDocument20 pagesCartilageNamra NoorNo ratings yet
- Chapter 7 (Cartilage)Document5 pagesChapter 7 (Cartilage)Jovilyn SilongaNo ratings yet
- DMS2 K3 (Kelas A) LECTURE CARTILAGE&BONE2020 PDFDocument67 pagesDMS2 K3 (Kelas A) LECTURE CARTILAGE&BONE2020 PDFdiqa aridaniNo ratings yet
- CARTILAGEDocument24 pagesCARTILAGEEdzeal Bruan JrNo ratings yet
- Tissue Anatomy and Physiology: The Four Main Tissue TypesDocument35 pagesTissue Anatomy and Physiology: The Four Main Tissue Typessnp88100% (1)
- CartilageDocument37 pagesCartilageFiraol DiribaNo ratings yet
- Lecture Cartilage and Bone 2009Document46 pagesLecture Cartilage and Bone 2009Danti Nelfa Riza100% (1)
- Cartilage and Bone: in Vivo, It Fills The Lacunae (Cavities) Where It ResidesDocument5 pagesCartilage and Bone: in Vivo, It Fills The Lacunae (Cavities) Where It ResidesSharon GabrielNo ratings yet
- Connective TissueDocument57 pagesConnective TissueSunil DhatwaliaNo ratings yet
- 1cartilage DR Amam PDFDocument49 pages1cartilage DR Amam PDFSarfraz Ahmad FaniNo ratings yet
- Histology of Musculoskeletal ModuleDocument9 pagesHistology of Musculoskeletal Moduledrahmed1028No ratings yet
- Proteoglycans, Whose Main Glycosaminoglycans Are Chondroitin-4-Sulfate and Chondroitin-6Document14 pagesProteoglycans, Whose Main Glycosaminoglycans Are Chondroitin-4-Sulfate and Chondroitin-6Joseph Enoch ElisanNo ratings yet
- HHDBI7 W FX Xe 35 R DNJHN 6 Xsadtz 5 PQ9 ZSNI6 SXZXWDocument26 pagesHHDBI7 W FX Xe 35 R DNJHN 6 Xsadtz 5 PQ9 ZSNI6 SXZXWleartaNo ratings yet
- Periodontal LigamentDocument56 pagesPeriodontal LigamentPurwana Nasir100% (2)
- Seminar On Cartilage and JointsDocument52 pagesSeminar On Cartilage and Jointskoyachew abateNo ratings yet
- HistoPath (Lect #4) TransDocument2 pagesHistoPath (Lect #4) TransSherlyn Giban InditaNo ratings yet
- Secret MineralizeDocument2 pagesSecret MineralizeMaricris CosmeNo ratings yet
- Cartilagedr 190528154146Document30 pagesCartilagedr 190528154146Dr.Aman SaxenaNo ratings yet
- CartilageDocument17 pagesCartilageasadullah2315No ratings yet
- CartilageDocument1 pageCartilageTarlan SharifiNo ratings yet
- Condylar CartilageDocument11 pagesCondylar CartilageMahesh kumarNo ratings yet
- Activity 3b - Specialized CT Cartilage and Bone TissuesDocument30 pagesActivity 3b - Specialized CT Cartilage and Bone TissuesRangel CuelloNo ratings yet
- Connective TissueDocument14 pagesConnective TissueDr NehaNo ratings yet
- CartilageDocument26 pagesCartilageMaxamed Faarax XaashiNo ratings yet
- Connective Tissue Cells and FunctionsDocument41 pagesConnective Tissue Cells and FunctionsAstrud LabradorNo ratings yet
- Screenshot 2022-10-09 at 1.39.31 AMDocument29 pagesScreenshot 2022-10-09 at 1.39.31 AMSeco AhmadNo ratings yet
- Histology Research Paper - CartilagesDocument5 pagesHistology Research Paper - CartilagesBasil AdeelNo ratings yet
- Bone and CartilageDocument56 pagesBone and CartilageGodwin ZengeniNo ratings yet
- Cartilage LectureDocument31 pagesCartilage LecturemalyaaNo ratings yet
- CartilageDocument3 pagesCartilageعلي المحترفNo ratings yet
- CartilageDocument15 pagesCartilagenyashamukamba15No ratings yet
- CartilageDocument12 pagesCartilageReycy Ruth Trivino100% (1)
- 1.2. Support and Movement SystemsDocument16 pages1.2. Support and Movement SystemssamiktshyagiriNo ratings yet
- Cartilage Structure and TypesDocument16 pagesCartilage Structure and TypesRSatriaSuryaCandraNo ratings yet
- BoneDocument26 pagesBoneAbdi Asiis Omar MohamedNo ratings yet
- 2.1 BM I Matrix ExtracelDocument48 pages2.1 BM I Matrix ExtracelDanti FadhilaNo ratings yet
- BSC Connective Tissues PDFDocument54 pagesBSC Connective Tissues PDFPuneeT Raj 470No ratings yet
- SkeletalSystem 2Document114 pagesSkeletalSystem 2LYRA GUEVARRANo ratings yet
- FRACTURESDocument85 pagesFRACTURESSteven OdhiamboNo ratings yet
- Histology SanadDocument31 pagesHistology SanadA-Naeem To'mah Al-sawaieNo ratings yet
- General Biology 2 ReviewerDocument1 pageGeneral Biology 2 ReviewerAlly OcbianNo ratings yet
- Exercise 2Document6 pagesExercise 2Gwyneth Marie DayaganNo ratings yet
- Sexual Reproduction in Flowering Plants DPP-01 Discussion Class NotesDocument4 pagesSexual Reproduction in Flowering Plants DPP-01 Discussion Class NotesTrendy TrendsNo ratings yet
- Biological Graphs QNS$M-SDocument53 pagesBiological Graphs QNS$M-Sbirgenenock47No ratings yet
- (Series in Positive Psychology.) Pluess, Michael - Genetics of Psychological Well-Being - The Role of Heritability and Genetics in Positive Psychology-Oxford UniveDocument317 pages(Series in Positive Psychology.) Pluess, Michael - Genetics of Psychological Well-Being - The Role of Heritability and Genetics in Positive Psychology-Oxford UniveLaura Quintero100% (1)
- Zoology 232 NotesDocument36 pagesZoology 232 NotesKevinNo ratings yet
- On The Origins of The MindDocument10 pagesOn The Origins of The MindScienceNo ratings yet
- MIDTERM EXAMINATION IN GEN BIO 1 Cell TheoryDocument4 pagesMIDTERM EXAMINATION IN GEN BIO 1 Cell TheoryIAN MAR VALENZUELA100% (1)
- Cambridge Assessment International Education: Biology 9700/21 May/June 2018Document14 pagesCambridge Assessment International Education: Biology 9700/21 May/June 2018Ali RanaNo ratings yet
- Eduqas A Level Biology Report s23Document26 pagesEduqas A Level Biology Report s23George Chan100% (1)
- Ebook Discover Biology 6Th Edition Singh Test Bank Full Chapter PDFDocument38 pagesEbook Discover Biology 6Th Edition Singh Test Bank Full Chapter PDFjamesreedycemzqadtp100% (10)
- Principles of Renal Physiology: Fifth EditionDocument15 pagesPrinciples of Renal Physiology: Fifth EditionAISHANo ratings yet
- DNA StructureDocument8 pagesDNA StructureKesithan AnandarashNo ratings yet
- Simpson 1951Document14 pagesSimpson 1951Luis Fernando ErazoNo ratings yet
- I Jsem 005461Document8 pagesI Jsem 005461Eloi Carlos GoveNo ratings yet
- Faculty of Earth Science: Bachelor of Applied Science (Natural Resource Science) With HonoursDocument17 pagesFaculty of Earth Science: Bachelor of Applied Science (Natural Resource Science) With HonoursNALINI MANIMARANNo ratings yet
- Ammann F1000 Evaluations 2013Document4 pagesAmmann F1000 Evaluations 2013Apo ghasan Al shargapiNo ratings yet
- Activity No. 7.Document3 pagesActivity No. 7.ALEXA JOIE CONCEPCION ARMONIANo ratings yet
- Year 1 Science Lesson Plan OverviewDocument9 pagesYear 1 Science Lesson Plan OverviewNur Ramadan JafflieNo ratings yet
- Joan's Module in Grade 10 Science (Fossils)Document10 pagesJoan's Module in Grade 10 Science (Fossils)Jenalyn NacasabugNo ratings yet
- Physioex Lab Report: Pre-Lab Quiz ResultsDocument5 pagesPhysioex Lab Report: Pre-Lab Quiz ResultsJoashan Vac100% (2)
- Sigma Xi, The Scientific Research SocietyDocument10 pagesSigma Xi, The Scientific Research SocietyDeive AlvesNo ratings yet
- Anatomy For Beginners - Movement WorksheetDocument4 pagesAnatomy For Beginners - Movement WorksheetJames DaurayNo ratings yet
- 9781003287056_12-1201Document256 pages9781003287056_12-1201Jinyoung ChoiNo ratings yet
- Short Story BMBPDocument9 pagesShort Story BMBPIntan DamayantiNo ratings yet
- CYANSmart Application Sheet for α-Amylase TestDocument60 pagesCYANSmart Application Sheet for α-Amylase TestMaria Alejandra Noguera Delgadillo100% (1)
- General Biology 1: Quarter 1, Week 1 - Module1: Postulates of The Cell TheoryDocument55 pagesGeneral Biology 1: Quarter 1, Week 1 - Module1: Postulates of The Cell TheoryCoulline DamoNo ratings yet
- Durian RAPD 3Document6 pagesDurian RAPD 3GiaHuyTrầnNo ratings yet
- Microprotein: (Pyrogallol Red Method)Document2 pagesMicroprotein: (Pyrogallol Red Method)Ranjit PathakNo ratings yet
- Habitat and Lifestyle: The Niche: What Makes An Organism Special?Document10 pagesHabitat and Lifestyle: The Niche: What Makes An Organism Special?Shiza RehmanNo ratings yet