Professional Documents
Culture Documents
Principles of Medical Technology Practice 1
Uploaded by
Jose Villareal0 ratings0% found this document useful (0 votes)
12 views6 pagesOriginal Title
422253817-PRINCIPLES-OF-MEDICAL-TECHNOLOGY-PRACTICE-1-docx.docx
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
12 views6 pagesPrinciples of Medical Technology Practice 1
Uploaded by
Jose VillarealCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 6
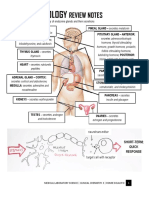
PRINCIPLES OF MEDICAL TECHNOLOGY It is a facility that performs chemical and microscopic
PRACTICE 1 examinations of various body fluids (e.g. blood
tissues).
OVERVIEW OF THE MEDICAL Inside the Clinical Laboratory
TECHNOLOGY/MEDICAL LABORATORY - Pathologist
SCIENCE PROFESSION - Medical Technologist
- Medical Technician
OUTLINE
Historical Perspective
Medical Technology/Medical Laboratory Science Practices Medical Technologist acts as…
Medical Technology Education MEDICAL DETECTIVES
LEARNING OUTCOMES
Trace the history of Medical Technology Globally and in the
Philippines.
Roles of Medical Technologist
Enumerate the scope of Medical Technology Practices. Observe, identify, and analyze organisms
Discuss the scope of medical technology curriculum and different job
opportunities. and cells causing infection and disease.
Perform blood tests.
MEDICAL TECHNOLOGY Measure substance in blood and other body
is also known as: fluids.
Clinical Laboratory Science Operate complex apparatus, instruments and
Medical Laboratory Science machines.
Use standards and controls to improve
What is Medical Technology (according to) ? reliability of results.
Work under pressure with accuracy and
Ruth Heinemann precision.
-is the application of natural, physical and biological Adhere to high ethical standards of
sciences to the performance of laboratory procedures performance.
which aid in the diagnosis and treatment of disease.
HISTORY OF MEDICAL TECHNOLOGY
Anne Fagelson GLOBAL AND LOCAL
-is the branch of medicine concerned with the
performance of laboratory determinations and EARLY BEGINNINGS
analyses used in the diagnosis and treatment of the
disease and maintenance of health. 400 B.C.
- Hippocrates (Father of Medicine) described
Walters the “four humors” in man; BLOOD,
-is the health profession concerned with performing PHLEGM, YELLOW BILE and BLACK
laboratory analyses in view of obtaining information BILE
necessary in the diagnosis and treatment of disease - Urine was regarded as composite of these
as well as in the maintenance of good health. humors.
RA 5527 (The Philippine Medical Technology Act 600 B.C.
of 1969) - Hindu physicians recorded the sweet taste of
-is an auxiliary branch of laboratory medicine which diabetic urine as well as polyuria in diabetes.
deals with the examination of tissues, secretion and
excretion of human body and body fluids by various 1500 B.C.
chemical, microscopic, bacteriologic and other - Vivian Herrick identified Taenia and
medical laboratory procedures of technic which will Ascaris.
aid the physician in the diagnosis strictly and - “Ebers Papyrus” was discovered.
treatment of disease and in the promotion of health in - “Ebers Papyrus” – the oldest preserved
general. Egyptian compilation of medical texts.
What is common among them? 1632
- Performing laboratory procedures - Anton Van Leeuwenhoek invented the
(samples) compound microscope.
- Analysis (results) - He was the first to describe the red blood
- Diagnosis and treatment (disease) cells, protozoa, and to classify bacteria
according to shape.
CLINICAL LABORATORY
1628-1694 - Automated equipment.
- Marcelo Malphigi (Founder of Pathology) - Quality control programs.
- Greatest of the early microscopists.
- Contributed to Embryology and Anatomy. IN THE PHILIPPINES
1847 Jan. 9, 1945
- Rudolph Virchow - First Clinical Laboratory in Phil. at
- Founder of the “Archives of Pathology” in Quiricada St., Sta. Cruz, Manila ws
Berlin. established and is known as Public Health
Laboratory.
1848
- Herman Fehling Oct. 1, 1945
- Performed the first quantitative test for - Dr. Pio de Roda and Dr. Mariano Icasiano
urine sugar. reopened Manila Public Health Laboratory.
15th Century 1947
- Discovery of dyes (aniline dyes) made - Dr. Pio de Roda and Dr. Prudencia Sta.
possible the staining and study of Ana offered a training for highschool and
microorganisms such as bacteria. paramedical graduates.
IN THE UNITED STATES 1954
- 6-month laboratory training was offered.
1878 - Formal education of Medical Technology
- Dr. William H. Welch began.
- Established a laboratory at Bellevue Hospital
Medical College. HISTORY OF MEDICAL TECHNOLOGY
- Became the first professor of Pathology at EDUCATION IN THE PHILIPPINES
John Hopkins University (1885).
MRS. WILLA HILGERT HEDRICK
1896 Founder of Medical Technology Education in the
- Dr. William Osler opened the first clinical Philippines
laboratory at John Hopkins Hospital.
- William Pepper Laboratory was also 1954
opened at the University of Pennsylvania. - Philippine Union College of Baesa
- First to offer BS Medtech.
1908 - Dr. Jesse Umali was its first graduate after 2
- Dr. James C. Todd wrote “A Manual of years.
Clinical Diagnosis” which became the
standard reference for laboratories. 1957-1959
- Dr. Antonio Gabriel and Dr. Gustavo
1921 Reyes of UST offered MT as an elective to
- Denver Society of Clinical Pathologists was pharmacy students. Due to its popularity, it
organized. was decided to be offered as a course.
- American Board of Pathology was
organized in 1936. 1960
- CEU offered MT course
World War I - First batch graduated in 1962.
- Produced a great demand for technicians.
- University of Minessota is one of the first 1662-1662
schools to establish trainings for workers in - Dr. Horacio Ylagan and Dr. Serafin
1922 and first to offer degree program in Juliano applied for the offering of BSMT
1923. courses in FEU which was approved in 1662.
- First batch graduated in 1663.
World War II
- “Closed system” of blood collection was U.P – offers the same course but the degree is
adopted. conferred to as B.S. Public Health.
- Advanced instrumentation.
Professional Organizations of Medical Technology
in the Philippines: Program Curriculum
-The Philippine Association of Schools of Medical The Course shall be at least four years, including a 12-
-Technology and Public Health, Inc. (PASMETH) month long internship in accredited laboratories and
The Philippine Association of Medical Technologists shall include the following subjects:
(PAMET) GENERAL EDUCATION
CORE COURSES
MEDICAL TECHNOLOGY EDUCATION IN PROFESSIONAL COURSES
THE PHILIPPINES
Scope of Licensure Examination
Nature of the Field of Study The given examination covers the following subjects
Program course shall be called as: with its specific percentage:
-Bachelor of Science in Medical Technology or Clinical Chemistry 20%
-Bachelor of Science in Medical Laboratory Science Microbiology and Parasitology 20%
- It is a four year program consisting of a one Hematology 20%
year internship with rotational duties in Blood Banking and Serology 20%
different sections during the 4th level in a Clinical Microscopy 10%
CHED-accredited training laboratory. Histopathologic Techniques and MT Laws10%
- A licensure examination is given to all
applicants for registration as Medical
Technologist. Employment Opportunities of Medical Technology
Graduates
Program Goals
The program aims for the graduates to: Medical technologist (generalist/specialist)
- Develop knowledge, skills, professional Clinical laboratory supervisors
attitude and values in the performance of Chief medical technologist
laboratory procedures. Laboratory owners
- Acquire critical thinking skills. Sales and public relations representative
- Engage in research and community-related Educational representatives (company/health
activities. program)
- Participate in activities promoting the
Researcher (industrial/medical)
profession and engage in the life-long
Teachers/Instructors (secondary/tertiary
learning undertakings.
levels)
- Develop collaborative and leadership
qualities. Employment abroad
Expected Performance Outcomes of Graduates (Medical Technologist Specialist, Phlebotomist,
The graduates must be able to: Industrial/Medical Researcher, Medical Doctors,
- Demonstrate technical competence in the Medical Sales Representatives)
performance of clinical laboratory tests.
- Demonstrate analytical and critical thinking
skills in the workplace.
- Engage in the proper collection, analysis
and projection of health information.
- Demonstrate inter-personal skills, leadership
qualities and ethical practice of the
profession.
- Apply research skills in relevance to areas to
areas of Medical Technology/Laboratory
Science practice.
- Participate in community oriented activities.
- Engage in life-ling learning activities.
- Demonstrate effective teaching and
communication skills.
C. Based on Institutional Character
1. Institution-based
2. Freestanding
UNIT 2 D. Based on Service Capability
CLINICAL LABORATORY 1. General Clinic Laboratory
2. Special Laboratory
OUTLINE
General overview
General Clinical Laboratory
Classification of medical laboratories a. Primary Category
Organization of the laboratory 1. Routine hematology (CBC)
Laboratory Sections
Information flow in the clinical laboratory 2. Qualitative platelet determination
Three phases of the laboratory testing 3. Routine urinalysis and fecalysis
Laboratory policies
4. Blood typing – for hospital-based
LEARNING OUTCOMES
Identify and differentiate the classification of clinical laboratory settings.
b. Secondary Category
Construct an organizational chart/architectural plan. 1. Routine clinical chemistry
Explain the roles, functions and services offered by the different sections 2. Quantitative platelet determination
of the laboratories.
Justify and explain various information on a laboratory requisition. 3. Cross matching
Identify the different phases of laboratory testing. 4. Gram staining
5. KOH staining for fungal disease
CLINICAL LABORATORY c. Tertiary Category
Facility 1. All secondary lab services
Specimens (whole blood, serum, plasma, 2. Special chemistry (Cardiac markers)
urine, stool, etc.) from the human body 3. Special hematology (coagulation tests)
Collected, processed, examined or analyzed 4. Immunology/Serology (HIV, hepa profile,
Prevention, diagnosis, and treatment tumor markers)
5. Microbiology – culture of sensitivity
CLASSIFICATION OF CLINICAL d. Limited Service Capability
LABORATORY Special Clinical Laboratory
DEPARTMENT OF HEALTH a. Assisted reproduction technology laboratory
Administrative Order no. 20017-0027
b. Molecular and cellular technology
c. Molecular pathology, Forensic pathology, and
A. Based on ownership
Anatomic laboratory
1. Government
2. Private
E. National Reference Laboratory
1. Confirmatory testing
B. Based on Function
2. Surveillance
1. Clinical Pathology
3. Resolution of conflicting results
2. Anatomical Pathology
4. Training and research
Clinical Pathology:
5. Evaluation of diagnostic kits and reagents
1. Clinical Chemistry
2. Hematology
F. Satellite Testing Sites
3. Microbiology
Testing site owned by a licensed laboratory
4. Clinical Microscopy
but situated in a location some distance from
5. Immunology
the main laboratory.
6. Molecular Biology
7. Immunohematology
G. Mobile Clinical Laboratories
8. Cytogenetics
9. Endocrinology Laboratory testing unit
10. Toxicology Moves form one testing site to another testing
11. Therapeutic drug monitoring site
Anatomical Pathology: Has a temporary testing location
1. Surgical Pathology Shall have a base laboratory
2. Immunohistopathology Permitted to collect specimen only
3. Cytology Operate within a 100-km radius from its main
4. Autopsy lab
5. Forensic Pathology
6. Molecular Pathology ORGANIZATION OF THE LABORATORY
…….
LABORATORY REPORTS
to transmit test results
Reference rangers
Date and time of the specimen collection
LABORATORY SECTIONS Name, address of the laboratory
Name and identification number of patient
A. SPECIMEN PROCESSING Source of specimen
B. HEMATOLOGY SECTION Date and time the report was generated
C. COAGULATION SECTION
D. CLINICAL MICROSCOPY THREE PHASES OF LABORATORY TESTING
E. PARASITOLOGY
F. CLINICAL CHEMISTRY A. PREANALYTICAL PHASE
G. CLINICAL MICROBIOLOGY occurs first in the laboratory process
H. IMMUNOLOGY/SEROLOGY SECTION Patient preparation
SEROLOGY TESTS Paper work and data entry
Pregnancy test – detects B-HCG Specimen collection, processing, storage,
Dengue Test and transportation
HbsAg – for hepatits Responsible Personnel
Bacterial Agglutination test ***Phlebotomist, laboratory technician
a. Widal test –typhoid fever
b. Weil-Felix – nonspecific test for B. PREANALYTICAL PHASE
typhus fever Considered the “actual” laboratory testing or
I. IMMUNOHEMATOLOGY/BLOOD the diagnostic procedures, processes and
BANK products
J. HISTOPATHOLOGY/ Proper instrument maintenance
CYTOPATHOLOGY Reagent supplies
Quality control
Why is Laboratory Testing Performed? Responsible Personnel
1. To assign a diagnosis ***Medical Technologist or Medical Lab
**confirm clinical diagnosis Scientist
**to establish an appropriate plan of action Ensure accuracy, precision, reliability of
2. Prevention by early detection of diseases the test procedure
through screening tests. Validates the following:
3. Ongoing assessment of the patient’s progress Test reagents/kits
and treatment. Testing process
Training of the lab personnel
INFORMATION FLOW IN THE CLINICAL performing the test
LABORATORY
C. POST-ANALYTIC PHASE
Laboratory requisition Includes the following:
A form used by physician to document the Review and analysis of results
tests that are to be performed on patients. Recording and reporting of test results
Contains the following Storage and disposal of specimen
Patient’s demographic data, name data, Releasing of results
address, birth data Responsible Personnel
Test selection – should be marked clearly ***Medical Technologist, Section
Date and time of collection Supervisor, Chief Medical Technologist,
Identification of the person who performed office clerk or staff
the collection, name of ordering physician
Additional comments LABORATORY POLICIES
Laboratory Directory
Stability of the specimen A. Laboratory hour and emergency work
Minimum volume Definite working hours
Test schedule Outside regular working hours organize a
Specimen processing system for testing urgent specimens.
Method
B. Range of tests to be performed and those to be
referred to higher level
Range of tests to be performed
1. The number of staff available
2. The availability of material resources
3. The types of health institutions
(hospital or health center)
Referral of specimens (when
necessary)
Example specimens for HIV detection
and water samples for bacteriological
analysis.
C. Collection of laboratory specimen
1. The specimen containers should be clearly
labeled with the patient’s name, identification
number, date of collection and time of
collection
2. A fully completed, request form should
accompany each specimen with the detail
mentioned above.
D. Workload capacity of a laboratory
- Should match to the number of staff
- Their level of training
- Size of the laboratory
- The availability of laboratory facilities
You might also like
- Clinical Chemistry 3: EndocrinologyDocument21 pagesClinical Chemistry 3: EndocrinologyRomie Solacito100% (3)
- Healing Lyme: Natural Healing of Lyme Borreliosis and The Coinfections Chlamydia and Spotted Fever Rickettsiosis, 2nd Edition - Stephen Harrod BuhnerDocument5 pagesHealing Lyme: Natural Healing of Lyme Borreliosis and The Coinfections Chlamydia and Spotted Fever Rickettsiosis, 2nd Edition - Stephen Harrod Buhnerxyrokuwu0% (6)
- Grafting and BuddingDocument21 pagesGrafting and BuddingAmyza ZamriNo ratings yet
- Medical Laboratory Science Review Harr Robert R.Document28 pagesMedical Laboratory Science Review Harr Robert R.Arriel A. Aranggo50% (2)
- Ereviewer. Mtlaws. Prelims and Midterms PDFDocument8 pagesEreviewer. Mtlaws. Prelims and Midterms PDFCatlyn RivalNo ratings yet
- Daily Lesson LogDocument18 pagesDaily Lesson LogApple SamoyNo ratings yet
- Pathogens of The Female Reproductive System - Leah NechamkinDocument1 pagePathogens of The Female Reproductive System - Leah NechamkinMicroposterNo ratings yet
- Medtech Law's and BioethicsDocument24 pagesMedtech Law's and BioethicsDayledaniel Sorveto100% (5)
- PMLS 1 1ST Semester Prelim NotesDocument8 pagesPMLS 1 1ST Semester Prelim NotesLol lolNo ratings yet
- 6 Belizario Et Al Medical Parasitology in The Philippines 3rd Ed PDFDocument530 pages6 Belizario Et Al Medical Parasitology in The Philippines 3rd Ed PDFElma Gonzales100% (9)
- Clinical Chemistry ReviewerDocument4 pagesClinical Chemistry ReviewerJudith Dayag Dorado100% (1)
- PMLS2 Understanding Phlebotomy ReviewerDocument5 pagesPMLS2 Understanding Phlebotomy ReviewerShane G.No ratings yet
- West Philippine Sea DisputeDocument9 pagesWest Philippine Sea DisputeEm-em CantosNo ratings yet
- Sagrada Orden vs. NACOCO ObliconDocument1 pageSagrada Orden vs. NACOCO ObliconEm-em Cantos100% (2)
- Principles of Medical Laboratory Science Practice 1Document30 pagesPrinciples of Medical Laboratory Science Practice 1JACOB AQUINTEYNo ratings yet
- Nucleotide BiosynthesisDocument25 pagesNucleotide BiosynthesisinigoNo ratings yet
- Ra 1517 & Ra7719Document5 pagesRa 1517 & Ra7719fniegas172No ratings yet
- MT Laws Reviewer MidtermsDocument6 pagesMT Laws Reviewer MidtermsKyaru Fuentes100% (1)
- Nri1201 Hiv Poster PDFDocument1 pageNri1201 Hiv Poster PDFalfredoibc100% (1)
- Medical Technology Laws PDFDocument153 pagesMedical Technology Laws PDFKami TazuNo ratings yet
- Pmls Transes Prelims 1Document5 pagesPmls Transes Prelims 1Kimberly Jean OkitNo ratings yet
- Biological Macromolecules Lab ReportDocument7 pagesBiological Macromolecules Lab Reportapi-31452059289% (9)
- Markell and Voges Medical Parasitology 9th EdDocument487 pagesMarkell and Voges Medical Parasitology 9th EdJudith P83% (12)
- PMLS 2 ReviewerDocument8 pagesPMLS 2 ReviewerNepoy Beltran Entendez100% (3)
- Pmls Topic 1Document6 pagesPmls Topic 1Marie Abluyon75% (4)
- Medtechbmlslawsbioethicsintro 160915135141Document19 pagesMedtechbmlslawsbioethicsintro 160915135141Kristine Marie PateñoNo ratings yet
- Histopathologic TechniquesDocument9 pagesHistopathologic TechniquesKate Alyssa Caton100% (11)
- The Medical Technology ProfessionDocument9 pagesThe Medical Technology ProfessionHeumice ClomeraNo ratings yet
- Clinical Laboratory Law RA. 4688Document26 pagesClinical Laboratory Law RA. 4688Dayledaniel Sorveto67% (3)
- History of Medical Technology ProfessionDocument5 pagesHistory of Medical Technology ProfessionJunnie Lastimosa33% (6)
- PMLS2 EsentialsDocument38 pagesPMLS2 EsentialsKen Novero100% (1)
- Introduction To MLS 1Document11 pagesIntroduction To MLS 1Thea sam penafloridaNo ratings yet
- MUST To KNOW in Immunology and SerologyDocument18 pagesMUST To KNOW in Immunology and SerologyRona Salando50% (2)
- PAMET Presidents, MedTech Prayer, Code of EthicsDocument3 pagesPAMET Presidents, MedTech Prayer, Code of EthicsEllaine Milar67% (3)
- Unit 4.0 Nature of The Clinical LaboratoryDocument15 pagesUnit 4.0 Nature of The Clinical LaboratoryJean Carmelette Balallo100% (1)
- Pmls ReviewerDocument9 pagesPmls ReviewerKat Ronolo100% (3)
- 2 History of Medtech ProfessionDocument2 pages2 History of Medtech Professionxiejie22590No ratings yet
- PMLS Midterm ReviewerDocument41 pagesPMLS Midterm ReviewerGwen YosheenNo ratings yet
- Pmls 1 - Lesson 1 - Overview and History of MTDocument3 pagesPmls 1 - Lesson 1 - Overview and History of MTHans De Guzman0% (1)
- Principles of Medical Laboratory ScienceDocument6 pagesPrinciples of Medical Laboratory ScienceKatrina VelosoNo ratings yet
- SONEDCO Workers Free Labor Union v. URCDocument2 pagesSONEDCO Workers Free Labor Union v. URCEm-em CantosNo ratings yet
- Trans Principles of Medical Laboratory 1Document66 pagesTrans Principles of Medical Laboratory 1Ella IrabonNo ratings yet
- Principles of Medical Laboratory Science 1Document6 pagesPrinciples of Medical Laboratory Science 1Sharon Daliva100% (3)
- PASMETH Through The YearsDocument5 pagesPASMETH Through The YearsJohn Terrence M. Romero40% (5)
- Pmls 1 Lec Lesson 9Document32 pagesPmls 1 Lec Lesson 9Red Aj Malayas0% (1)
- Syllabus in Community and Public Health For Medical Laboratory ScienceDocument4 pagesSyllabus in Community and Public Health For Medical Laboratory ScienceIrish De Vera100% (2)
- MTLB Week 1 and 2Document86 pagesMTLB Week 1 and 2Josh Buenafe Macapallag100% (1)
- Principles of Medical Technology Practice 1 Midterm TranseesDocument19 pagesPrinciples of Medical Technology Practice 1 Midterm TranseesSean Rafael LedesmaNo ratings yet
- PNCC Skyway Corp. vs. SOLE (Feb 6, 2017)Document3 pagesPNCC Skyway Corp. vs. SOLE (Feb 6, 2017)Em-em CantosNo ratings yet
- Medtech Laws and EthicsDocument14 pagesMedtech Laws and EthicsDreyden Halo0% (1)
- PMLS Reviewer For Midterms PDFDocument14 pagesPMLS Reviewer For Midterms PDFJerica Mae GabitoNo ratings yet
- PMLS 1 Lesson 8 Nature of Clinical LabDocument200 pagesPMLS 1 Lesson 8 Nature of Clinical Labangelica fayeNo ratings yet
- Handouts MTLB 4688 The Clinical Lab LawDocument6 pagesHandouts MTLB 4688 The Clinical Lab LawFait Hee100% (1)
- Defining The Practice of The Medical Technology PDFDocument6 pagesDefining The Practice of The Medical Technology PDFNicole Reyes100% (1)
- History of Medical Technology in The PhilippinesDocument52 pagesHistory of Medical Technology in The PhilippinesRalph Alday0% (1)
- Pmls ReviewerDocument11 pagesPmls ReviewerAnn Caluma100% (1)
- Alcantara & Sons v. CADocument3 pagesAlcantara & Sons v. CAEm-em CantosNo ratings yet
- Philippine Scout Veterans Security v. SecretaryDocument3 pagesPhilippine Scout Veterans Security v. SecretaryEm-em CantosNo ratings yet
- Gemudian v. Naess Shipping Phils. Inc. and Royal DragonDocument4 pagesGemudian v. Naess Shipping Phils. Inc. and Royal DragonEm-em CantosNo ratings yet
- (Laboratory Animal Pocket Reference Series) Villano, Jason - Sharp, Patrick E - The Laboratory rat-CRC Press (2013)Document382 pages(Laboratory Animal Pocket Reference Series) Villano, Jason - Sharp, Patrick E - The Laboratory rat-CRC Press (2013)Charles santos da costa100% (1)
- Medtech HistoryDocument8 pagesMedtech HistoryMandy A. Delfin78% (9)
- Medical Technology Philippine Medical Technology Act OF 1969Document4 pagesMedical Technology Philippine Medical Technology Act OF 1969John-Karl JimenezNo ratings yet
- History of Medical Technology PDFDocument19 pagesHistory of Medical Technology PDFKat De Lara71% (7)
- #1 Glasswares: A. Plain Test TubesDocument3 pages#1 Glasswares: A. Plain Test Tubessansastark100% (3)
- MTLBDocument3 pagesMTLBDanNo ratings yet
- Molbio Lab W3Document2 pagesMolbio Lab W3KYLELA PANGILINAN100% (2)
- Principles of Medical Laboratory Science PracticeDocument14 pagesPrinciples of Medical Laboratory Science PracticeJanna EchavezNo ratings yet
- Pmls MidtermsDocument6 pagesPmls MidtermsChristine LumactayNo ratings yet
- PMLS .Docx 1Document9 pagesPMLS .Docx 1ain't your saintessNo ratings yet
- Overview of The Medical Technology/Medical Laboratory Science ProfessionDocument7 pagesOverview of The Medical Technology/Medical Laboratory Science ProfessionMikay.No ratings yet
- PMLS Lesson 1Document8 pagesPMLS Lesson 1seaynNo ratings yet
- Chapter 1Document9 pagesChapter 1Rica Mae ApallaNo ratings yet
- MTLB211 Week 2 LEC ReviewerDocument7 pagesMTLB211 Week 2 LEC ReviewerMONICA VILLANUEVANo ratings yet
- Medtech Laws and Bioethics MTE 114Document3 pagesMedtech Laws and Bioethics MTE 114Lowin NavarroNo ratings yet
- Principles of Medical Laboratory Science 1Document15 pagesPrinciples of Medical Laboratory Science 1Julianne Marie LacsentoNo ratings yet
- MTLB Week 2Document9 pagesMTLB Week 2FelicityNo ratings yet
- SGV Train LawDocument149 pagesSGV Train LawEm-em CantosNo ratings yet
- Bravo v. Urios CollegeDocument4 pagesBravo v. Urios CollegeEm-em CantosNo ratings yet
- Move-In SetDocument8 pagesMove-In SetEm-em CantosNo ratings yet
- AC No. 99-634 June 10, 2002 DOMINADOR P. BURBE, Complainant, ATTY. ALBERTO C. MAGULTA, Respondent. Panganiban, J.Document48 pagesAC No. 99-634 June 10, 2002 DOMINADOR P. BURBE, Complainant, ATTY. ALBERTO C. MAGULTA, Respondent. Panganiban, J.Em-em CantosNo ratings yet
- San Miguel Corp. Supervisors and Exempt Union v. LaguesmaDocument4 pagesSan Miguel Corp. Supervisors and Exempt Union v. LaguesmaEm-em CantosNo ratings yet
- G.R. No. L-15824 May 30, 1961 RICARDO M. GUTIERREZ, Petitioner, HON. ARSENIO SANTOS, ETC. ET AL., RespondentsDocument49 pagesG.R. No. L-15824 May 30, 1961 RICARDO M. GUTIERREZ, Petitioner, HON. ARSENIO SANTOS, ETC. ET AL., RespondentsEm-em CantosNo ratings yet
- Week 2Document36 pagesWeek 2Em-em CantosNo ratings yet
- Complementarity of Man and WomanDocument4 pagesComplementarity of Man and WomanEm-em CantosNo ratings yet
- PH Visual Arts-ASCIVDocument6 pagesPH Visual Arts-ASCIVEm-em CantosNo ratings yet
- Indonesia: Name of The CountryDocument26 pagesIndonesia: Name of The CountryEm-em CantosNo ratings yet
- The Jewelry - SummaryDocument11 pagesThe Jewelry - SummaryEm-em CantosNo ratings yet
- Cambodia: Executive SummaryDocument9 pagesCambodia: Executive SummaryEm-em CantosNo ratings yet
- Breastcancer Predisposition Syndromes: Deborah Hemel,, Susan M. DomchekDocument16 pagesBreastcancer Predisposition Syndromes: Deborah Hemel,, Susan M. DomchekPietro PeraldoNo ratings yet
- PresentationDocument7 pagesPresentationfatima zafarNo ratings yet
- Systematics Based On Evolutionary Relationships: Taxonomy/Cladistics and PhylogenyDocument3 pagesSystematics Based On Evolutionary Relationships: Taxonomy/Cladistics and PhylogenyPatricia PascualNo ratings yet
- Grade 12 Second Term Test Unit 4Document23 pagesGrade 12 Second Term Test Unit 4Asha justin josephNo ratings yet
- BABY BOOM (BBM) : A Candidate Transcription Factor Gene in Plant BiotechnologyDocument12 pagesBABY BOOM (BBM) : A Candidate Transcription Factor Gene in Plant BiotechnologyMalik NADA-ABINo ratings yet
- Anti-Hiv Drug Discovery PDFDocument18 pagesAnti-Hiv Drug Discovery PDFMandapati JanakiramNo ratings yet
- BDNF With Fasting and ExerciseDocument4 pagesBDNF With Fasting and ExerciseanirudhjayNo ratings yet
- 2008 - Ehninger, Kempermann - Neurogenesis in The Adult HippocampusDocument8 pages2008 - Ehninger, Kempermann - Neurogenesis in The Adult HippocampusNityananda PortelladaNo ratings yet
- Lewis Book ChapterDocument24 pagesLewis Book ChapterHarjotBrar100% (1)
- Ez-Pcr Mycoplasma Test Kit: Instructions For UseDocument2 pagesEz-Pcr Mycoplasma Test Kit: Instructions For Usenauval mangantjoNo ratings yet
- Concept MapDocument1 pageConcept Mapapi-249598813No ratings yet
- Science - Unit 2 ExaminationDocument7 pagesScience - Unit 2 ExaminationAkhssnnajaNo ratings yet
- Non-Mendelian GeneticsDocument31 pagesNon-Mendelian GeneticsrogermaximoffNo ratings yet
- Lecture 4 - 15 End Replication and Genetic Code - Transcription PDFDocument78 pagesLecture 4 - 15 End Replication and Genetic Code - Transcription PDFFafa MusNo ratings yet
- 03 The Miracle of The Human BrainDocument6 pages03 The Miracle of The Human BrainAbhijeet SavantNo ratings yet
- Dna-Structure-And-Replication L v47 320 s1Document7 pagesDna-Structure-And-Replication L v47 320 s1api-302502919No ratings yet
- Protein Crystallization DissertationDocument4 pagesProtein Crystallization DissertationWriteMyBiologyPaperCanada100% (1)
- Gene Therapy: Submitted To: Mrs. Annalie Solamo Bejoc Submitted By: Sibi, Emmanuel John S. Bsme-P4Document10 pagesGene Therapy: Submitted To: Mrs. Annalie Solamo Bejoc Submitted By: Sibi, Emmanuel John S. Bsme-P4Emman WuzNo ratings yet
- MangosteenDocument2 pagesMangosteenHening Tirta KusumawardaniNo ratings yet
- ArticuloDocument7 pagesArticuloCarlosGuevaraPáezNo ratings yet
- Agriculture and Nanotechnology Pre and Post TestDocument6 pagesAgriculture and Nanotechnology Pre and Post Testapi-288531740No ratings yet