Professional Documents
Culture Documents
MUSCULAR SYSTEM MIDTERMS
Uploaded by
KIM EUNHA0 ratings0% found this document useful (0 votes)
18 views14 pagesOriginal Title
ANAPHYSIO LEC (midterms)
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
18 views14 pagesMUSCULAR SYSTEM MIDTERMS
Uploaded by
KIM EUNHACopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 14
ANAPHYSIO LECTURE o Motor neurons- specialized nerve cells
MIDTERMS responsible for stimulating skeletal
MUSCULAR SYSTEM muscle contraction.
Histology and Physiology Skeletal Muscle Fiber Anatomy
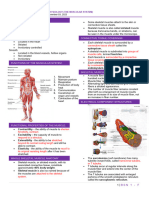
Functions of the Muscular System o Long, cylindrical cells, each with several
Types of Muscle Tissue nuclei located near the plasma
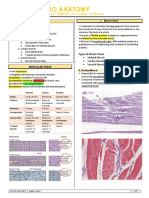
o Skeletal Muscle- Most abundant and membrane.
most studied type o Length: 1mm to 4 cm from 10
o Smooth Muscle- most widely micrometers to 100 in diameter
distributed type of muscle in the body. Muscle Fiber Development
o Cardiac Muscle- found only in the o Myoblasts- muscle fibers develop from
heart, and its contractions provide the less mature, multinucleated cells
major force for moving blood through o Hypertrophy- enlargement of muscles
the circulatory system. in children and adults results from an
Major Functions increase in the size of each muscle fiber,
o Movement of the body not from a substantial increase in the
o Maintenance of posture number of muscle fibers. Similarly,
o Respiration hypertrophy
o Production of Body Heat Sarcolemma- plasma membrane of a muscle
o Communication fiber
External lamina- deeper & thinner; delicate CT
o Constriction of organs and vessels
layers located outside sarcolemma.
o Contraction of the heart
Endomysium-second layer also consists mostly
4 Major functional properties
of reticular fibers, but it is a much thicker layer.
o Contractility- the ability of muscle to
T tubules/transverse tubules- many tubelike
shorten forcefully, or contract
invaginations of the sarcolemma.
o Excitability- the capacity of muscle to
sarcoplasmic reticulum- highly organized
respond to an electrical stimulus.
smooth endoplasmic reticulum,
o Extensibility- means a muscle can be
sarcoplasm- the cytoplasm of a muscle fiber
stretched beyond its normal resting
myofibrils- The sarcoplasm also contains
length and still be able to contracts.
numerous bundles A myofibril contains two
o Elasticity- the ability of muscle to spring
kinds of long, thin protein filaments of protein
back to its original resting length after it filaments
has been stretched. o myofilaments- A myofibril contains two
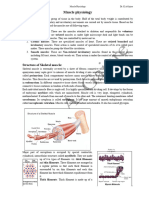
Whole Skeletal Muscle Anatomy kinds of long, thin protein filaments
Connective Tissue Coverings Actin myofilaments(thin)- are
o Fascicles- a muscle is composed of linear polymers of globular
numerous visible bundles. actin (G-actin) subunits and
o Perimysium- Connective tissue layer occur as microfilaments in the
that surrounds each fasciculus. cytoskeleton and as thin
o Epimysium- The entire muscle is filaments, which are part of the
surrounded by a layer of dense irregular contractile apparatus, in muscle
collagenous connective tissue (DICCT) and non-muscle cells
o Fascia- is a general term for sheets of Myosin myofilaments(thick)-
DICCT within the body. filament composed of either
o Muscular fascia- located superficial to multiple myosin or actin
the epimysium and separates individual proteins that slide over each
muscles or groups of muscles. other to generate tension.
Nerves and Blood Vessels Actin and Myosin Myofilament
Synapse – cell-to-cell junction bet. a nerve cell and
Sarcomeres- The actin and myosin another nerve cell/effector cell
Motor unit – a single motor neuron and all the skeletal
myofilaments are arranged into highly ordered muscle fibers it innervates
units Presynaptic terminal – enlarged axon terminal
- the basic structural and functional unit of Synaptic cleft – the space bet. the presynaptic terminal
skeletal; the smallest portion that is capable and the muscle fiber membrane
Postsynaptic membrane – the muscle fiber membrane
of contracting. Synaptic vesicles – presynaptic terminal that contains
- Z disks- separate one sarcomere from the small vesicles
next; a filamentous network of proteins; Acetylcholine (ACh) – neurotransmitter contained in
forms the attachment of actin the vesicles; a molecule released by a presynaptic nerve
cell that stimulates/inhibits a postsynaptic cell
myofilaments. Acetylcholinesterase – an enzyme that rapidly breaks
- I band/isotropic bands- light staining down the synaptic cleft bet. the neuron and the muscle
bands; extends to the ends of the myosin fiber
Muscle Contraction
filaments; consists only of action
Sliding filament model – sliding of actin myofilaments
myofilaments past myosin myofilaments during contraction
- A band- dark staining in the center of each Cross-bridges – myosin heads attach to the myosin
sarcomere; extends the length of the attachment sites on the actin myofilaments
Muscle Twitch, Summation, Tetanus, Recruitment
myosin myofilaments within a sarcomere.
Muscle Twitch – contraction of a muscle fiber in
- H zone – actin and myosin filaments do not reponse to a stimulus
overlap and only myosin myofilaments are 1. Lag/Latent Phase – time bet. the application of a
present stimulus and the beginning of contraction
2. Contraction Phase – time during which the
- M line – in the middle of H zone; consists of
muscle contract
filaments that attach to the center of the 3. Relaxation Phase – time during which the
myosin myofilaments: holds it in place. muscle relaxes
- Titin- one of the largest proteins, consisting Summation – the force of contraction of an individual
muscle fiber is increased by rapidly stimulating them
of a single chain of amino acids- it attaches
Tetanus – convulsive tension; a sustained contraction
to Z disks and extends along myosin that occurs when the frequency of stimulus is so rapid
myofilaments to the M line that no relaxation occurs
Excitability of Muscle Fibers O Caused by Ca+ build up in the myofibrils
Resting membrane potential – cell membranes have a Recruitment – the no. of muscle fibers contraction is
negative charge on the inside relative to a positive increased by the increasing no. of motor units stimulated
charge outside; occurs bcos there is an uneven + muscle contracts with more force
distribution of ions Stimulus frequency – no. of times a motor neuron is
1. Concentration of K+ inside the cell CM > stimulated per second
outside the CM Energy Requirement for Muscle Contraction
2. Concentration of Na+ outside the CM > inside Aerobic Respiration – requires O2; breaks down glucose
the CM to produce ATP, CO2, H2O
Different types of Ion Channels Anaerobic respiration – doesn’t require O2; breaks
O Nongated/Leak channels – always open down glucose to yield ATP and lactic acid
O Chemically gated channels – closed until a Creatine phosphate – high-energy molecule that can be
chemical binds them and stimulates them to stored in muscle fibers
open Fatigue
Depolarization – the inside of the CM membrane comes § A state of reduced work capacity
more positive than the outside of the cell; Na+ ions Muscular Fatigue – when muscle fibers use ATP faster
move into cells than they are produced; when the effectiveness of Ca+ to
Repolarization – the change back to the resting stimulate actin + myosin is reduced
membrane potential; K+ ions moves out of cells Physiological contracture – muscles may become
Action Potentials – the rapid depolarization and incapable of either contracting or relaxing
repolarization of the CM; results in muscle Psychological fatigue – involves the CNS; an individual
contraction perceives that continued muscle contraction is
Motor neurons – specialized nerve cells that stimulate impossible
muscles to contract Type of Muscle Contractions
Neuromuscular junction – a branch that forms a Isometric contractions – equal distance; length of the
junction with a muscle fiber muscle does not change; the amount of tension increases
during the contraction process
Isotonic contraction – equal tension; the amount of (sternum), cleido (clavicle), mastoid (mastoid
tension produced by the muscle is constant during process), brachio (arm), radialis (radius)
contraction; length of the muscle decreases
O Cocentric contractions – isotonic; muscle 3. Accdg. To Number of Origin – biceps (2),
tension increases as the muscle shortens triceps, quadriceps
O Eccentric contractions – isotonic; tension is 4. Accdg. To Function – flexor (flexion)
maintained in a muscle; the opposing resistance 5. Accdg. To Size – maximus (largest), minimus
causes the muscle to lengthen
Muscle Tone (smallest), vastus (large)
§ Constant tension produced by body muscles 6. Accdg. To Shape – deltoid (triangle), orbicularis
over long periods of time (circular)
§ Responsible for keeping the back and legs 7. Orientation of Fasciculi – rectus (straight)
straight, the head in an upright position, and the
abdomen from bulging I. Muscles of the Head and Neck
Slow-Twitch and Fast-Twitch Fibers Facial Expression
Classification of Muscle Fiber Occipitofrontalis – raises the eyebrows
1. Slow Twitch – contains type I myosin; contracts Orbicularis oculi – encircle the eyes, tightly close the
slowly and resistant to fatigue respiration
2. Fast Twitch eyelids, and causes crow’s feet wrinkles
a. Type IIa – intermediate speed; more Orbicularis oris – encircles the mouth
fatigue resistant than type IIb Buccinator – kissing muscles; pucker the mouth; flattens
b. Type IIb – contract 10x faster than type I
the cheeks I whistling/blowing
Myglobin – stores oxygen temporarily
Hypertrophy – enlarging of muscle fibers Zygomaticus – elevate the upper lip and corner of the
Satellite cells – undifferentiated cells just below the mouth
endomysium Levator labile superioris – sneering; elevates one side
Smooth and Cardiac Muscle
of
Autorhythmicity – resulting periodic spontaneous
contraction of smooth muscle. the upper lip
Intercalated disks – specialized structures that facilitate Depressor anguli oris – frowning & pouting; depresses
action potential conduction bet. cells the corner of the mouth
Skeletal Muscle Anatomy Mastification (for chewing)
General Principles Temporalis – fan-shaped muscle
Tendon – muscle connected to a bone Masseter – seen & felt on the side of the head
Aponeuroses – broad, sheet like tendons Pterygoid (paired) – protraction, excursion, elevation of
Retinaculum – a band of CT that holds down the mandible
tendons at each wrist and ankle Tongue and Swallowing Muscles
Origin – head; most stationary end of the muscle Intrinsic muscles – located within the tongue and
Insertion – end of the muscle attached to the bone change its shape
undergoing the greatest movement Extrinsic muscles – attached to and move the tongue
Belly – part of the muscle bet. the origin & the insertion Hyoid muscles – hold the hyoid bone; elevate the larynx
Agonist – muscle that accomplishes a certain Pharyngeal elevators – elevate the pharynx
movement Pharyngeal constrictors – constrict the pharynx from
Antagonist – muscle acting in opposition to an agonist superior to inferior (forcing food into the esophagus);
Synergists – a group of muscles working together to also open the auditory tube
produce a movement Neck Muscles
Prime Mover – muscle that plays the major role in Sternocleidomastoid – prime mover of the lateral
accomplishing desired movement muscle group; rotates the head; flexes the neck or
Fixators – muscles that hold one bone in place relative extends the head; prayer muscle
to Torticollis – wryneck; injury to the sternocleidomastoid
the body Deep neck muscles – flexes/extends head and neck
Nomenclature Trapezius – extends and laterally flexes neck
1. Accdg. To Location – temporalis, frontalis, II. Trunk Muscles
pectoralis, brachialis Muscles Moving the Vertebral Column
2. Accdg. To Origin and Insertion – sterno Erector spinae – responsible for keeping the back
straight and the body erect Rotator cuff muscles – attached the humerus to the
Deep back muscles – responsible for several scapula and forms a cuff/cap over the proximal
movements humerus
of the vertebral column Deltoid – attaches the humerus to the scapula and
External intercostal – elevate the ribs during inspiration clavicle; major abductor of the upper limb
Internal intercostal – contract during forced expiration, Forearm Movements
depressing the ribs Triceps brachii – primary extensor of the elbow
Diaphragm – major movement produced in the thorax Biceps brachii & brachialis – primary flexors of the
during quiet breathing elbow
Scalenes – inspiration and rib elevation Brachioradialis – posterior forearm muscle; helps flex
Abdominal Wall Muscles the elbow
Linea alba – tendinous area of the abdominal wall that Supination and Pronation
consists of white connective tissue Supinator – supination of the forearm or turning the
Rectus abdominis – located on each side of the linea flexed forearm so that the palm is up
alba Pronator – pronation, turning other forearm so that the
Tendinous intersections – causes the abdominal wall of palm is down
a lean, well-muscled person to appear segmented. Wrist and Finger Movements
External/Internal abdominal oblique & Transversus Retinaculum – fibrous connective tissue that covers the
abdominis – flex and rotate the vertebral column or flexor & extensor tendons and holds them in place
compress the abdominal contents around the wrist
Pelvic Floor and Perineal Muscles Flexor carpi – flex the wrist
Pelvic Floor – pelvic diaphragm Extensor carpi – extend the wrist
Levator ani – muscle that forms the pelvic floor Flexor digitorum – flexor of the digits/fingers
Perineum – associated with the male/female Extensor digitorum – extension of the fingers
reproductive structures Intrinsic hand muscles – 19 muscles located within the
Perineum bulbospongiosus – constricts the urethra; hand
erects the penis, clitoris Interossei – responsible for abduction and adduction of
Perineum ischiocavernosus – compresses the base of the fingers
penis/clitoris Tennis elbow – inflammation and pain due to forceful,
Perineum external anal sphincter – keeps the orifice of repeated contraction of the wrist extensor muscles
the anal canal closed Palmus longus – tightens palm skin
III. Upper Limb Muscles IV. Lower Limb Muscles
Scapular Movements Thigh Movements
§ Attach the scapula to the thorax and move the Iliopsoas – flexes the hip
scapula Tensor fasciae latae – helps steady the femur on the
§ Acts as fixators to hold the scapula firmly in tibi.
position when the muscle of the arm contract when a person is standing
§ Move the scapula into different positions Gluteus maximus – extends the hip; adducts and
v Trapezius laterally rotates the thigh; contributes most of the mass
v Levator scapulae Gluteus medius – extends the hop when the thigh is
v Rhomboids flexed at a 45O angle; common site for injections in the
v Serratus anterior buttocks (sciatic nerve lies deep to the g. maximus)
v Pectoralis minor Leg Movements
Arm Movements Quadriceps femoris – primary extensors of the knee
Pectoralis major – adducts the arm and flexes the Sartorius – tailor’s muscle; longest muscle in the body;
shoulder; extend the shoulder from a flexed position flexes the hip and knee; rotates the thigh laterally for
Latissimus dorsi – swimmer’s muscle; medially rotates sitting cross legged
and adducts the arm and powerfully extends the Hamstring muscles – flexing the knee
shoulder Adductor muscles – adducting the thigh
Ankle and Toe Movements 1. Ventilation
Gastrocnemius & Soleus – form the bulge of the calf 2. External respiration
Calcaneal tendon – Achilles tendon; flexors and are 3. Gas transport
involved in plantar flexion of the foot 4. Internal respiration
Fibularis muscles – primary everters of the foot; aid in FUNCTIONS
plantar flexion 1. Regulation of blood pH
Intrinsic foot muscles – flex, extend, abduct, and adduct 2. Production of chemical mediators
the toes 3. Voce production-Air moving past the vocal folds
Extensor digitorum longus – extends 4 lateral toes, makes sound and speech possible.
everts foot. 4. Olfaction- The sensation of smell occurs when
Extensor halluces longus – extends great toe; inverts airborne molecules are drawn into the nasal
foot cavity
Tibialis anterior – inverts foot 5. Protection-The respiratory system provides
Fibularis tertius – everts foot protection against some microorganisms by
Flexor digitorum longus – flexes 4 lateral toes, inverts preventing them from entering the body and
foot removing them from respiratory surfaces.
Flexor halluces longus – flexes great toe, inverts foot
7 Structures
Tibialis posterior – inverts foot
Fibularis brevis – everts foot External nose
Fibularis longus – everts foot Nasal cavity
Effects of Aging on Skeletal Muscle Pharynx (throat)
§ Decreased muscle mass Larynx (voice box)
§ Slower reaction time Trachea (windpipe)
§ Reduced stamina Bronchi (branches of trachea)
§ Increased recovery time Lungs
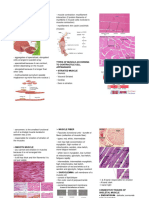
Types of Muscular Tissue Anatomy
I. Skeletal (striated voluntary) UPPER RESPIRATORY TRACT
§ Large, long, cylindrical cells - External nose, nasal cavity, pharynx
§ Multinucleated LOWER RESPIRATORY TRACT
§ Attached to bones - Larynx, trachea, bronchi, lungs
§ Responsible for body movement Conducting Zone- exclusively for air movement and
II. Cardiac (striated involuntary) extends from the nose to the bronchioles.
§ Cylindrical cells NOSE
§ Branched and connected to one another by - Consists of the external nose and nasal cavity
intercalated disks EXTERNAL NOSE – visible structure that forms a
§ Single nucleated prominent feature of the face.
§ Found in the heart NARES (nostrils) – external openings of the nose
§ Pumps the blood CHOANAE – openings into the pharynx; posterior
III. Smooth (nonstriated involuntary) structures
§ End tapered cells Vestibule -The vestibule is lined with stratified
§ Single nucleated squamous epithelium, which is continuous with the
§ Found in hollow organs: stomach, intestine; stratified squamous epithelium of the skin
skin, eyes HARD PALATE – floor of the nasal cavity; separates the
§ Regulates size of organs, forces fluid through nasal and oral cavity
tubes, controls the amount of light entering the NASAL CAVITY –open chamber inside the nose where
eye, produces ‘goose bumps’ air first enters the respiratory system. extends from the
nares to the choanae
RESPIRATORY SYSTEM NASAL SEPTUM – a partition dividing the nasal cavity
Complete exchange of o2 and co2 into right and left parts
DEVIATED NASAL SEPTUM – occurs when the septum to the hyoid bone
bulges to one side - Has 3 unpaired cartilages and 6 paired cartilages
CONCHAE – three prominent bony ridges on the lateral UNPAIRED (3):
walls on each side of the nasal cavity; increase the 1. THYROID CARTILAGE – Adam’s apple; largest
surface area of the nasal cavity and cause air to churn cartilage
MEATUS- tunnels where air passes through 2. CRICOID CARTILAGE – most inferior, forms the
PARANASAL SINUSES – air-filled spaces within bone base of the larynx
NASOLACRIMAL DUCTS – carry tears from the eyes 3. EPIGLOTTIS – 3rd unpaired cartilage; consist of
SNEEZE REFLEX – dislodges foreign substances from elastic cartilage; is attached to the thyroid cartilage and
the nasal cavity. projects superiorly as a free flap toward the tongue
Functions of nasal cavity PAIRED (6): they form an attachment site for the vocal
1. Serves as a passageway for air. folds
2. Cleans the air 1. CUNEIFORM CARTILAGE (wedge)– Top; contained in
3. Humidifies and warms the air. a mucous membrane anterior to the corniculate
cartilages
4. Contains the olfactory epithelium.
2. CORNICULATE CARTILAGE (horn)– Middle; attached
5. Helps determine voice sound.
to the superior tips of the arytenoid cartilages.
PHARYNX 3. ARYTENOID CARTILAGE (ladle) – Bottom; the
- Common passageway for both the respiratory and posterior, superior border of the cricoid cartilage
digestive systems. receives air from the nasal cavity and 2 PAIRS OF LGAMENTS
receives air, food, and drink from the oral cavity VESTIBULAR FOLDS – false vocal cords; superior
THREE REGIONS: mucous membrane.
1. NASOPHARYNX – superior part; contains openings on VOCAL FOLDS/CORDS – true vocal cords; inferior
each side from the auditory tubes that are continuous mucous membrane
with the middle ear. GLOTTIS-The combination of the vocal folds and the
a. SOFT PALATE – an incomplete muscle and opening between them
connective tissue partition separating the LARYNGITIS – inflammation of the mucous
nasopharynx from the oropharynx epith. of the vocal folds
b. UVULA – posterior extension of the soft palate
c. PHARYNGEAL TONSIL – helps defend the
body against infection
2. OROPHARYNX – extends from the uvula to the
Epiglottis; air, food, and drink all pass through the TRACHEA(Windpipe)
oropharynx. - Membranous tube attached to the larynx
a. PALATINE TONSILS – located in the lateral - Consists of CT and smooth muscle; Reinforced with 15-
walls near the border of the oral cavity and the 20 C-shaped pieces of hyaline cartilage
oropharynx TRACHEALIS MUCLE- an elastic ligamentous membrane
b. LINGUAL TONSIL – located on the surface of and bundles of smooth muscle
the posterior part of the tongue C-SHAPED CARTILAGES – form the anterior and
FAUCES- the narrow passage from the mouth to the lateral sides of the trachea; protect the trachea and
pharynx between the soft palate and the base of the maintain an open passageway for air
tongue. COUGH REFLEX – dislodges foreign substances
3. LARYNGOPHARYNX – passes posterior to the from the trachea
larynx and extends from the tip of the epiglottis to SMOKER’S COUGH – results from constant
the esophagus; lined with stratified squamous epith. irritation and inflammation of the respiratory
and ciliated columnar epith. passages by cigarette smoke
LARYNX (Voice box) BRONCHI
- Passageway for air between the pharynx and trachea - The trachea divides into the left and right main
- held in place by membranes and/or muscles superior bronchi or primary bronchi, each of which connects to a
lung - Consists of 6 LAYERS:
CARINA- tracheal cartilage separating the openings into 1. Thin layer of fluid lining the alveolus
the main bronchi forms a ridge 2. Alveolar epithelium – composed of simple squamous
LEFT MAIN BRONCHUS – more horizontal because it epithelium
is displaced by the heard 3. Basement membrane of the alveolar epith.
RIGHT MAIN BRONCHUS – where foreign objects 4. Thin interstitial space
that enter the trachea usually lodge; more vertical. 5. Basement membrane of the capillary endothelium
LUNGS 6. Capillary endothelium – simple squamous epith.
- tracheal cartilage separating the openings into the PLEURAL CAVITIES
main bronchi forms a ridge - surround the lungs and provide protection against
- Principal organs of respiration friction
RIGHT LUNG – has 3 lobes (superior, middle, PLEURA – serous membrane lining the pleural cavity
inferior) • PARIETAL PLEURA – lines the walls of the
LEFT LUNG – has 2 lobes (superior, inferior) thorax, diaphragm and mediastinum
- The lobes of the lungs are separated by deep, • VISCERAL PLEURA – covers the surface of the
prominent fissures on the lung surface. lung
- Each lobe is divided into Bronchopulmonary segments PLEURAL FLUID – acts as a lubricant and helps hold
separated from one another by CT septa. the pleural membranes together
- The main bronchi branch many times to form the LYMPHATIC SUPPLY
TRACHEOBRONCHIAL TREE. SUPERFICIAL LYMPHATIC VESSELS – are deep to
MAIN BRONCHI the visceral pleura; they drain lymph from the
o LOBAR BRONCHI – Secondary bronchi superficial lung tissue and the visceral pleura
SEGMENTAL BRONCHI – DEEP LYMPHATIC VESSELS – follow the bronchi;
Tertiary bronchi they drain lymph from the bronchi and associated CTs.
BRONCHIOLES VENTILATION AND RESP. VOLUMES
TERMINAL BRONCHIOLES VENTILATION (breathing) – the process of moving air
RESPIRATORY BRONCHIOLES into and out of the lungs.
ALVEOLI – small, air- 2 PHASES:
filled chambers where 1. INSPIRATION – inhalation; movement of air into
the air and the blood the lungs
come into close contact 2. EXPIRATION – exhalation; movement of air out of
with each other. the lungs
CHANGING THORACIC VOLUME
ALVEOLAR DUCTS –
MUSCLES OF INSPIRATION – include the diaphragm
long, branching
and the muscles that elevate the ribs and sternum, such
hallways with many
as the external intercostals
open doorways
• DIAPHRAGM – a large dome of skeletal
ALVEOLAR SACS-
muscle that separates the thoracic cavity from
chambers connected to
abdominal cavity
two or more alveoli
MUSCLES OF EXPIRATION – internal intercostals;
BRONCHODILATION- occurs when the smooth muscle depress the ribs and sternum.
relaxes, making the bronchiole diameter larger PRESSURE CHANGES AND AIRFLOW
BRONCHOCONSTRICTION- occurs when the smooth Two physical principles that govern the airflow:
muscle contracts, making the bronchiole diameter 1. Changes in volume result in changes in pressure.
smaller. 2. Air flows from an area of higher pressure to an area
RESPIRATORY MEMBRANE OF THE LUNGS – of lower pressure
where gas exchange between the air and blood takes - During INSPIRATION, air flows into the alveoli
place because atmospheric pressure is greater than the
- It is very thin to facilitate the diffusion of gases alveolar pressure.
- During EXPIRATION, air flows out of the alveoli 3. VITAL CAPACITY – IRV + TV + ERV
because alveolar pressure is greater than atmospheric O It is the maximum volume of air that a person can
pressure. expel from the resp. tract after maximum
LUNG RECOIL inspiration (4600mL)
- The tendency for an expanded lung to decrease in size. 4. TOTAL LUNG CAPACITY – IRV + ERV + TV +RV
- When thoracic volume and lung volume decrease O Also equal to the VC + RV (5800mL)
during quiet expiration. GAS EXCHANGE
- Two factors keep the lungs from collapsing: - Gas exchange bet. air and blood occurs in the
SURFACTANT and PLEURAL PRESSURE. respiratory membrane
SURFACTANT – reduces the surface tension of the DEAD SPACE – the parts of the resp. passageways
fluid lining the alveoli (surface acting agent). where gas exchange bet. air and blood does not occur.
PLEURAL PRESSURE – lower than alveolar pressure, RESPIRATORY MEMBRANE THICKNESS
which causes the alveoli to expand. - Increases in the thickness of the respiratory
CHANGING ALVEOLAR VOLUME membrane
- Increasing thoracic volume results in decreased result in decreased gas exchange.
pleural pressure, increased alveolar volume, decreased SURFACE AREA
alveolar pressure, and air movement into the lungs - Small decreases in surface area adversely affect gas
(inspiration). exchange during strenuous exercise. When the surface
- Decreasing thoracic volume results in increased area is decreased to 1/3 or 1/4 of normal, gas exchange
pleural pressure, decreased alveolar volume, increased is restricted under resting conditions.
alveolar pressure, and air movement out of the lungs PARTIAL PRESSURE
(expiration). - is the pressure exerted by a specific gas in a mixture of
RESPIRATORY VOLUMES & CAPACITIES gases, such as air.
SPIROMETRY – is the process of measuring volumes of DIFFUSION OF GASES IN THE LUNGS
air that move into and out of the respiratory system. - O2 diffuses from a higher partial pressure in the
SPIROMETER – device that measures the resp. volumes alveoli
RESPIRATORY VOLUMES – are measures of the to a lower pp in the pulmonary capillaries.
amount of air movement during different portions of - CO2 diffuses from a higher partial pressure in the
ventilation pulmonary capillaries to a lower pp in the alveoli.
RESPIRATORY CAPACITIES – are sums of two or DIFFUSION OF GASES IN THE TISSUES
more respiratory volumes - O2 diffuses from a higher pp in the tissue capillaries to
RESPIRATORY VOLUMES: a lower pp in the tissue spaces.
1. TIDAL VOLUME – air inspired or expired with each - CO2 diffuses from a higher pp in the tissues to a lower
breath (at rest, quiet breathing = 500mL) pp in the tissue capillaries.
2. INSPIRATORY RESERVE VOLUME – air that can GAS TRANSPORT IN THE BLOOD
be inspired forcefully beyond the resting TV OXYGEN TRANSPORT
(3000mL) OXYHEMOGLOBIN – hemoglobin with oxygen bound
3. EXPIRATORY RESERVE VOLUME – air that can be to its heme groups
expired forcefully (1100mL) MORE OXYGEN IS RELEASED FROM
4. RESIDUAL VOLUME – air still remaining in the HEMOGLOBIN IF (FOUR FACTORS):
respiratory passages and lungs after maximum 1. Partial pressure for O2 is low
expiration (1200mL) 2. Partial pressure for CO2 is high
RESPIRATORY CAPACITIES: 3. pH is low
1. FUNCTIONAL RESIDUAL CAPACITY – ERV + RV 4. Temperature is high
O Amount of air remaining in the lungs at the end of CO2 TRANSPORT AND BLOOD pH
a normal expiration (2300mL) CARBONIC ANHYDRASE – enzyme that promotes the
2. INSPIRATORY CAPACITY – TV + IRV uptake of CO2 by RBCs
O Amount of air a person can inspire maximally after - As CO2 levels increase, blood pH decreases (becomes
a normal expiration (3500mL) more acidic)
- As CO2 levels decrease, blood pH increases (becomes RESPIRATORY ADAPTATIONS TO EXERCISE
more basic) - Training results in increased minute volume at
RHYTHMIC BREATHING maximal exercise because of increased TV and
RESPIRATORY AREAS IN THE BRAINSTEM respiratory rate.
MEDULLARY RESPIRATORY CENTER – establishes EFFECTS OF AGING ON THE RESP. SYSTEM
rhythmic breathing 1. VC and Maximum min. ventilation decrease
O DORSAL RESPIRATORY GROUPS (2) – primarily 2. RV and dead space increase
responsible for stimulating contraction of the 3. Increase in resting TV compensates for increased
diaphragm. dead space, loss of alveolar walls, and thickening of
O VENTRAL RESPIRATORY GROUPS (2) – primarily alveolar walls
responsible for stimulating the external and internal 4. The ability to remove mucus from respiratory
intercostal, and abdominal muscles. passageways decrease with age.
o PRE-BOTZINGER COMPLEX – establish the
basic rhythm of breathing DIGESTIVE SYSTEM
PONTINE RESPIRATORY GROUP – is a collection of FUNCTIONS (IDEA)
neurons in the pons. 1. Ingestion of food.
- It plays a role in switching between inspiration and 2. Digestion of food.
expiration. 3. Elimination of wastes.
GENERATION OF RHYTHMIC BREATHING 4. Absorption of nutrients.
- involves the integration of stimuli that start and stop ANATOMY AND HISTOLOGY
inspiration Digestive Tract / Gastrointestinal Tract
1. Starting inspiration § Oral cavity, pharynx, esophagus, stomach, small
2. Increasing inspiration intestine, large intestine, anus
3. Stopping inspiration Four Tunics
NERVOUS CONTROL OF BREATHING 1. Mucosa
HIGHER BRAIN CENTERS – allow voluntary control § Innermost tunic
of breathing. § Consists of mucous epithelium, lamina propria
HERING-BREUER REFLEX – supports rhythmic (loose CT), muscularis mucosae (thins SM layer)
respiratory movements by limiting the extent of § Mouth, esophagus, anus; resists abrasion
inspiration § Stomach, intestine; absorbs and secrets
TOUCH, THERMAL, PAIN RECEPTORS – can 2. Submucosa
stimulate breathing. § Thick layer of loose CT, consists of nerves, blood
CHEMICAL CONTROL OF BREATHING vessels, small glands
HYPERCAPNIA – a greater than normal amount of CO2 § Plexus – extensive network of nerve cell
in the blood processes (innervated by the autonomic nerves)
CARBON DIOXIDE – major chemical regulator of 3. Muscularis
breathing § Consists of circular SM (inner), longitudinal SM
CHEMORECEPTORS (in medulla oblongata) – (outer)
respond to changes in blood pH § Enteric nervous system – composed of the
CHEMORECEPTORS (in carotid and aortic bodies) – nerve plexuses of the submucosa and
respond to changes in blood O2. muscularis; controls movement and secretion
HYPOXIA – a condition when blood O2 declines to a within the tract
low level 4. Serosa
EFFECT OF EXERCISE ON BREATHING § Outermost layer
1. Breathing increases abruptly § Consists of the peritoneum (smooth epithelial
2. Breathing increases gradually layer + underlying CT)
ANAEROBIC THRESHOLD – the highest level of § Adventitia – connective tissue; regions of the DT
exercise that can be performed without causing a not covered by the peritoneum
significant change in blood pH Peritoneum
1. Visceral Peritoneum / Serosa – serous b. Cusps
membrane that covers the organs c. Neck
2. Parietal Peritoneum – serous membrance that d. Root
covers the wall of the abdominal cavity Pulp cavity – center of the tooth; contains blood vessels
Mesenteries – CT sheets that hold the abdominal cavity nerves, and pulp (connective tissue)
organs in place Dentin – bonelike tissue that surrounds the pulp cavity
a. Lesser omentum – connects the lesser curvature Enamel – extremely hard, acellular substance that
of the stomack to the liver and diaphragm covers
b. Greater omentum – connects the greater the dentin of the tooth drown
curvature of the stomach to the transverse colon Cementum – covers the surface of the dentin in the
and posterior body wall root; anchors the tooth in the jaw.
v Omental bursa – a long, double fold of Alveoli (along the alveolar process of mandible x
mesentery that extends inferiorly from maxillae) – where the teeth are rooted
the stomach before looping back to the Gingiva – dense fibrous CT and most stratified
transverse colon to create a squamous epithelium that covers the alveolar processes
cavity/pocket Periodontal ligaments – CT fibers that extend from the
v Mesentery proper – attaches the small alveolar walls that hold the teeth in place
intestine to the posterior abdominal wall Dental caries / Tooth decay – result of the breakdown
Retroperitoneal – abdominal organs that have no of
mesenteries; duodenum, pancreas, ascending + enamel by acids produced by bacteria on tooth surface
descending colon, rectum, kidneys, adrenal glands, Periodontal disease – inflammation x degeneration of
urinary bladder the periodontal ligaments, gingiva, alveolar bone
ORAL CAVITY, PHARYNX, AND ESOPHAGUS Palate and Tonsils
Anatomy of Oral Cavity Palate – roof of the oral cavity; prevents food from
§ Bounded by the lips and cheeks ++ contains the passing into the nasal cavity during chewing and
teeth and tongue swallowing
Lips – muscular structures formed by the orbicularis a. Hard palate – anterior part that contains bone
oris muscle b. Soft palate – posterior portion that consists of
Cheeks – buccinators muscles flatten the cheeks against skeletal muscle _ CT
teeth v Uvula – grape-like; posterior extension of the
Mastification – begins the process of mechanical soft palate
digestion Tonsils – protect against pathogens from entering the
Tongue – plays a major role in the process of nose and mouth
swallowing; major sensory organ for taste; one of the Salivary Glands
major organs of speech § Produce saliva (serous + mucous fluids)
v Frenulum – thin fold of tissue inferior to the 3 Pairs of SG
tongue 1. Parotid glands – largest; serous glands located
Teeth anterior to each ear
§ 32 teeth in normal adult mouth 2. Submandibular glands – produce more serous
§ Located in the mandible and maxillae than mucous secretions
1. Incisor – to cut 3. Sublingual glands – smallest; produce
2. Canine – to tear primarily mucous secretions
3. Premolars Mumps – inflammation of the parotid gland caused by
4. Molars viral infection
5. Wisdom teeth – third molars Saliva
Permanent teeth – secondary teeth § Helps keep the oral cavity moist
Primary teeth – deciduous teeth; milk or baby teeth § Contains enzymes that begin the process of
Parts digestion
a. Crown Salivary amylase – a digestive enzyme that breaks the
covalent bonds bet. glucose molecules (starch) and Outer longitudinal, middle circular, and inner obique
other layer – produce a churning action in the stomach
polysaccharides; enhances the sweet taste of food Rugae – large folds where the submucosa and mucosa
Lysozyme – enzyme that has weak antibacterial action are thrown into when the stomach is empty
Mastification Gastric pits – openings for the gastric glands; formed by
§ Breaks large food particles into many small ones simple columnar epithelium
§ Increases the efficiency of digestion Epithelial cells of the Stomach
Pharynx 1. Surface mucous cells – inner surface of stomach
§ Throat & lining the gastric pits; coats and protects the
§ Connects the mouth with the esophagus stomach lining
§ Oropharynx + laryngopharynx – transmit food 2. Mucous neck cells – produce mucus
§ Contains pharyngeal constrictor muscles 3. Parietal cells – produce hydrochloric acid &
Esophagus intrinsic factor
§ Muscular tube that ransports food from the 4. Endocrine cells – produce regulatory chemicals
pharynx to the stomach 5. Chief cells – produce pepsinogen (precursor of
§ Esophageal sphincters – regulate the movement the protein digesting enzyme pepsin)
of food into and out of the esophagus Secretions of the Stomach
§ Cardiac sphincter – lower ES Chyme – semifluid mixture (food + stomach secretions)
Swallowing / Deglutition 1. Hydrochloric acid kills microorganisms and
1. Voluntary Phase activates pepsin
§ Bolus (mass of food) us formed in the mouth 2. Pepsin breaks covalent bond of proteins to form
§ Bolus is pushed by the tongue forcing in into the smaller peptide chains.
oropharynx 3. Mucus lubricates and protects epithelial cells
2. Pharyngeal Phase from the damaging effect of acidic chime +
§ A reflex initiated when a bolus of food pepsin
stimulates receptors in the oropharynx 4. Intrinsic factor binds with vit. B12 (DNA
§ Epiglottis – tipped posteriorly to cover the synthesis and RBC prod.) and makes it more
larynx readily absorbed in the small intestine
3. Esophageal Phase Regulation of Stomach Secretions
§ Responsible for moving food form the pharynx 1. Cephalic phase – stomach secretions are
to the stomach initiated by the sight, smell, taste, or thought of
§ Peristaltic waves – muscular contractions of the food
esophagus 2. Gastric phase – partially digested proteins and
STOMACH distention of the stomach promote secretion
§ Functions primarily as a storage and mixing O Gastrin – hormone that enters the
chamber for ingested food circulation and is carried back to the
Anatomy stomach
Gastroesophageal opening – opening from the 3. Intestinal phase – acidic chime in the
esophagus ino the stomach duodenum stimulates neuronal reflexes and the
Cardiac region – region of t around the secretion of hormones that inhibit gastric
gastroesophageal opening; near the heart secretions by negative feedback loops
Fundus – most superior part of the stomach O Secretin – hormone that inhibits gastric
Body – largest part of the stomach secretions; released from the duodenum
v Greater curvature in response to low pH
v Lesser curvature O Cholecystokinin – major inhibitor of
Pyloric opening – opening from the stomach into the gastric motility; released from the
small intestine duodenum initiated by fatty acids and
Pyloric sphincter – thick ring of smooth muscle peptides
Pyloric region – region near the pyloric opening Movement in the Stomach
§ Increased motility = increases emptying 1. Peptidases – break peptide bonds in proteins to
§ Distention of stomach = increases gastric form amino acids
motility 2. Disaccharidases – break down disaccharides
A. Mixing waves – thoroughly mix ingested food (maltose) into monosaccharides (glucose)
with stomach secretions to form chime Movement of the Small Intestine
O Fluid part of chime – pushed toward A. Peristaltic contractions – proceed along the
the pyloric sphincter length of the intestine for variable distances;
O Solid center – moves back toward the causes the chime to move along the small
body of the stomach intestine
B. Peristaltic waves – force the chime toward and B. Segmental contractions – propagate for shot
through the pyloric sphincter distances; mix intestinal contents
SMALL INTESTINE LIVER AND PANCREAS
§ Major site of digestion and absorption of food Anatomy of Liver
§ Major function is the absorption of nutrients Major Lobes
Anatomy 1. Right lobe
1. Duodenum – 12 in. long 2. Left lobe
2. Jejunum – 2.5 m long; makes up 2/5 Falciform ligament – CT septum that separates the right
3. Ileum – 3.5 m long; makes up 3/5 and left lobe of the liver.
Common bile duct (liver) and pancreatic duct Smaller Lobes
(pancreas) – join and empty into the duodenum 1. Caudate lobe
Increased surface area 2. Quadrate lobe
1. Circular folds – formed by mucosa and Porta – gate through which blood vessels, ducts, and
submucosa that run perpendicular to the long nerves enter and exit the liver
axis of the digestive tract Sources of Blood in the Liver
2. Villi – formed by tiny, fingerlike projections of 1. Hepatic artery – takes oxygen-rich blood to the
the mucosa liver; supplies liver with oxygen
3. Microvilli – numerous cytoplasmic extensions 2. Hepatic portal vein – oxygen-poor blood but
on the surface of the villi rich in nutrients
Lacteal – lymphatic capillary Hepatic veins – where blood exits the liver and empty
Simple Columnar Epithelium into the inferior vena cava
1. Absorptive cells – have microvilli, produce Portal Triads
digestive enzymes, absorb digested food 1. Hepatic artery
2. Goblet cells – produce a protective mucus 2. Hepatic portal vein
3. Granular cells – help protect the intestinal 3. Hepatic duct
epithelium from bacteria Hepatic cords – located bet. the center and margins of
4. Endocrine cells – produce regulatory hormones each lobule
Intestinal glands – epithelial cells produced within Hepatocytes – platelike groups that form the hepatic
tubular galnds of mucosa cords
Duodenal glands – mucous glands in the submucosa of Hepatic sinusoids – blood channels that separates the
the duodenum hepatic cords from one another
Peyer patches – clusters of lymphatic nodules along the Central vein – where mixed blood flows toward the
digestive tract center of each lobule
Ileocecal junction – where the ileum connects to the Bile canaliculus – a cleftlike lumen bet. the cells of each
large intestine hepatic cord
Ileocecal sphincter – ring of smooth muscle Common hepatic duct – right + left hepatic ducts
Ileocecal valve – allow intestinal contents to move from Common bile duct – common hepatic duct + cystic duct
the ileum to the large intestine; but not in opposite Gallbladder – stores and concentrates bile
direction Duodenal papilla – where the common bile duct joind
Secretions of the Small Intestine the pancreatic duct and opens into the duodenum
Functions of the Liver termination of sigmoid colon & ends at the anal
1. Digestion canal
2. Excretion Anal Canal
3. Nutrient storage § Begins at the inferior end of the rectum and ends
4. Nutrient conversion at the anus (external digestive tract opening)
5. Detoxification of harmful chemicals Internal anal sphincter – smooth muscle layer at
6. Synthesis of new molecules superior end
Bile – dilutes and neutralizes stomach acid; dramatically External anal sphincter – skeletal muscle at inferior end
increases the efficiency of fat digestion and absorption; Hemorrhoids – enlarged or inflamed rectal or
stimulated by secretin hemorrhoidal, veins that supply the anal canal; may
Bile salts – emulsify fats cause pain, itching, bleeding around anus
Bilirubin – bile pigment that results from the Functions of Large Intestine
breakdown of hemoglobin 1. Feces production
Anatomy of Pancreas 2. Water absorption
1. Head – near the midline of the body MAVM.
2. Tail – extends to the left Feces – converted chyme
Pancreatic islet / Islets of Langerhans – endocrine part; Defecation – elimination of feces from the colon
produce insulin and glucagon Mass movements – strong contractions in the large
Compound acinar gland – exocrine part parts
Acini – produce digestive enymes of the colon; propel the colon contents a considerable
Pancreatic duct – formed by larger ducts from clusters distance towards the anys
of acini Defecation reflex – local (weak contractions) +
Functions of the Pancreas parasympathetic (strong contractions) reflexes
Major Proteolytic enzymes – continue protein digestion DIGESTION, ABSORPTION, AND TRANSPORT
that began in the stomach Digestion – breakdown of food to molecules tha are
1. Trypsin small enough to be absorbed into the circulation
2. Chymotrypsin a. Mechanical digestion – breaks large good
3. Carboxypeptidase particles into smaller ones
Pancreatic amylase – continues polysaccharide b. Chemical digestion – breaking of covalent
digestion chemical bonds in organic molecules by
that began in the oral cavity digestive enzymes
Lipase – lipid-digesting enzyme Absorption – begin in stomach; lipid-soluble molecules
Nucleases – enzymes that degrade DNA and RNA to diffuse through the stomach epithelium into the
their component nucleotides circulation
LARGE INTESTINE Transport – requires carrier molecules and includes
Anatomy facilitated diffusion, cotransport, and active transport
Cecum Carbohydrates
§ Proximal end of the large intestine § Consist primarily of starches, cellulose, sucrose
Appendix – 9 cm tube attached to the cecum (table sugar), small amounts of fructose (fruit
Colon sugar), and lactose (milk sugar)
1. Ascending colon Polysaccharides – large carbohydrates that consist of
2. Transverse colon many sugars linked by chemical bonds
3. Descending colon Salivary amylase – begins the digestion of
4. Sigmoid colon carbohydrates in the mouth
Crypts – straight, tubular glands in the mucosal lining of Pancreatic amylase – continues digestion of
the colon carbohydrates
Teniae coli – three bands Disaccharides – two sugars; broken down
Rectum polysaccharide
§ Straight, muscular tube that begins at the Disaccharidase – group of enzymes that break the
disaccharides to monosaccharides
Monosaccharides – single sugars; glucose, galactose,
and fructose
Lipids
§ Molecules which are insoluble or slightly
soluble in water
Triglycerides – most common type of lipid; 3 fatty acids
bound to glycerol
Saturated – fatty acids have only single bonds
Unsaturated – fatty acids have one or more double
bonds
Emulsification – large lipid droplets are transformed
into much smaller droplets
Lipase – secreted by pancreas; digests lipid molecules
Micelles – aggregated bile salts around small droplets of
digested lipids
Chylomicrons – packaged lipid-protein complexes
(lipoproteins)
Chyle – lymph containing late amounts of absorbed
lipid
Proteins
§ Chains of amino acids
Pepsin – enzyme secreted by stomach that breaks down
proteins
Polypeptides – shorter amino acid chains
Trypsin, Chymotrypsin, Carboxypeptidase – enzymes
produced by pancreas that continue the digestive
process
Peptidases – small peptides
Water and Minerals
§ Approximately 9 L of water enters the digestive
tract
§ Approximately 2 L from food & drink &
remaining 7 liters is from digestive secretions
You might also like
- Anaphyio (1st Sem Midterms)Document24 pagesAnaphyio (1st Sem Midterms)KIM EUNHANo ratings yet
- HAPP Week VII XDocument32 pagesHAPP Week VII Xxuxi dulNo ratings yet
- Muscular SystemDocument10 pagesMuscular SystemKYLA LORENZ BALUMANo ratings yet
- Muscular System ReviewerDocument3 pagesMuscular System ReviewerRea BrangueloNo ratings yet
- AnaPhy Lesson 6 Muscular SYstemDocument7 pagesAnaPhy Lesson 6 Muscular SYstemLM KishimotoNo ratings yet
- Muscular System Lecture 1DDocument7 pagesMuscular System Lecture 1DShane PascualNo ratings yet
- Muscle Tissue NotesDocument11 pagesMuscle Tissue NotesAubrey Unique EvangelistaNo ratings yet
- Muscular System FunctionsDocument17 pagesMuscular System FunctionsNicoleVideñaNo ratings yet
- Muscular SystemDocument6 pagesMuscular SystemTricia Mae LlerenaNo ratings yet
- Chapter 10: Muscle Tissue: VoluntaryDocument13 pagesChapter 10: Muscle Tissue: VoluntaryClyde BaltazarNo ratings yet
- Muscular System and Muscle ContractionDocument5 pagesMuscular System and Muscle ContractionPhilline ReyesNo ratings yet
- Chapter 7 - Muscular SystemDocument29 pagesChapter 7 - Muscular SystemlNo ratings yet
- The Muscle Tissue ReviewerDocument5 pagesThe Muscle Tissue ReviewerSasukeNo ratings yet
- The Muscular SystemDocument4 pagesThe Muscular SystemMazon, Dinah Melisse P.No ratings yet
- Functional Anatomy - ContentDocument14 pagesFunctional Anatomy - ContentxanaduNo ratings yet
- Muscles Part1 DoxDocument13 pagesMuscles Part1 DoxjeffdelacruzNo ratings yet
- Topic 5 Genhisto NotesDocument6 pagesTopic 5 Genhisto NotesShiina MashiroNo ratings yet
- Muscular system overviewDocument2 pagesMuscular system overviewSachdev KingNo ratings yet
- Muscular System Functions and StructureDocument5 pagesMuscular System Functions and StructureMayet BautistaNo ratings yet
- Muscular System - Part 1 (BSN - 1F)Document5 pagesMuscular System - Part 1 (BSN - 1F)yulo.jhoselleanne.bsnNo ratings yet
- Anaphy Notes MidtermDocument10 pagesAnaphy Notes MidtermAndrea SaldivarNo ratings yet
- Chapter 10Document5 pagesChapter 10Nona PeriarceNo ratings yet
- The Muscular SystemDocument9 pagesThe Muscular SystemKeiffer Ann LopezNo ratings yet
- Muscul Arsystem: Skeletal MuscleDocument5 pagesMuscul Arsystem: Skeletal MuscleGracia Dela CruzNo ratings yet
- Histo 1.9 Muscle TissueDocument7 pagesHisto 1.9 Muscle TissueMonesa Christy VillanuevaNo ratings yet
- Muscular and Nervous SystemDocument13 pagesMuscular and Nervous SystemDionne EllaNo ratings yet
- Muscular System - Part 1 (BSN - 1F)Document5 pagesMuscular System - Part 1 (BSN - 1F)yulo.jhoselleanne.bsnNo ratings yet
- 589bc774 Df1d 47c6 Bc97 b5fd73030ca6Muscle PhysiologyDocument3 pages589bc774 Df1d 47c6 Bc97 b5fd73030ca6Muscle PhysiologyMalti SharmaNo ratings yet
- ANAPHY - Muscular SystemDocument11 pagesANAPHY - Muscular SystemSoleil RiegoNo ratings yet
- Muscular SystemDocument8 pagesMuscular SystemChristine Joanne CelendroNo ratings yet
- Muscle TissueDocument5 pagesMuscle TissueSheena PasionNo ratings yet
- 7 Muscular SystemDocument11 pages7 Muscular SystemmargaretNo ratings yet
- Chapter 7: Muscular System: SarcomeresDocument11 pagesChapter 7: Muscular System: SarcomeresPrecious Faith RodriguezNo ratings yet
- 6.0 Muscular SystemDocument76 pages6.0 Muscular System[R2A] Khadijah AzlanNo ratings yet
- 11J - Caybot - Jash Jovian - Task10Document11 pages11J - Caybot - Jash Jovian - Task10JASH JOVIAN CAYBOTNo ratings yet
- Week 7 - Muscular SystemDocument12 pagesWeek 7 - Muscular SystemG a i l R i c h w e l lNo ratings yet
- Célula Muscular, Macro y MicrobiologicoDocument11 pagesCélula Muscular, Macro y MicrobiologicoimanolNo ratings yet
- Muscularsyste M: Balisado Marylei Ann ADocument5 pagesMuscularsyste M: Balisado Marylei Ann ASeanLian SeliNo ratings yet
- Muscularsyst EM: Actin and Myosin MyofilamentsDocument16 pagesMuscularsyst EM: Actin and Myosin MyofilamentsCatherine Joy delos SantosNo ratings yet
- 7-muscleDocument3 pages7-muscleprincessstephNo ratings yet
- Muscular SystemDocument13 pagesMuscular SystemavilajrjimuelNo ratings yet
- Physiology of Skeletal Muscle and Muscle FibreDocument7 pagesPhysiology of Skeletal Muscle and Muscle FibreNoor-E-Khadiza ShamaNo ratings yet
- ANAPHY LAB W5.5 ReviewerDocument5 pagesANAPHY LAB W5.5 Reviewerangelmalang41No ratings yet
- Reviewer - Muscular SystemDocument11 pagesReviewer - Muscular SystemIvy Jan OcateNo ratings yet
- Lab Muscle Tissue EditinggDocument12 pagesLab Muscle Tissue EditinggLyn YmiNo ratings yet
- Histology of Muscle: Lecturer Anatomy DepartmentDocument19 pagesHistology of Muscle: Lecturer Anatomy DepartmentSUMAN GHOSHNo ratings yet
- Midterm Reviewer - Google DocsDocument61 pagesMidterm Reviewer - Google Docscpagente01No ratings yet
- The Muscular SystemDocument9 pagesThe Muscular SystemKathleenJoyGalAlmasinNo ratings yet
- Muscular SystemDocument20 pagesMuscular Systempriya garciaNo ratings yet
- Types of MusclesDocument8 pagesTypes of MusclesJoan Vito CruzNo ratings yet
- Muscular SystemDocument3 pagesMuscular SystemJanica Pauline DaydayNo ratings yet
- Histo MuscleDocument11 pagesHisto MuscleaikaNo ratings yet
- mascularDocument39 pagesmascularAive BelistaNo ratings yet
- Muscular System ReviewerDocument21 pagesMuscular System ReviewerChloe Mikaela MonsantoNo ratings yet
- Eme 1Document20 pagesEme 1Tara LingatingNo ratings yet
- 7.1 Muscular SystemDocument8 pages7.1 Muscular SystemEly FructuosoNo ratings yet
- Human Histology (Lecture) Lesson 6: Muscle Tissue (Anatomy & Physiology)Document4 pagesHuman Histology (Lecture) Lesson 6: Muscle Tissue (Anatomy & Physiology)AJ MERCADONo ratings yet
- Muscle A&P: Structure, Types, Sensory Feedback & ContractionDocument23 pagesMuscle A&P: Structure, Types, Sensory Feedback & ContractionjhnnolanNo ratings yet
- CHAPTER 7 ANAPHY TransesDocument17 pagesCHAPTER 7 ANAPHY TransesHoly HaeinNo ratings yet
- TFN NotesDocument3 pagesTFN NotesKIM EUNHANo ratings yet
- Uts RebyuwerDocument14 pagesUts RebyuwerKIM EUNHANo ratings yet
- Osup TTDocument23 pagesOsup TTKIM EUNHANo ratings yet
- Introduction to Anatomy and PhysiologyDocument6 pagesIntroduction to Anatomy and PhysiologyKIM EUNHANo ratings yet
- Anaphy Chapter 1Document5 pagesAnaphy Chapter 1Hans De GuzmanNo ratings yet
- Internal II BEEE QPDocument1 pageInternal II BEEE QPsivaNo ratings yet
- Pneumatic System and Basic Valve UsedDocument401 pagesPneumatic System and Basic Valve Usedtarang srivasNo ratings yet
- Development of Automatic Mini Fan with PIR SensorDocument8 pagesDevelopment of Automatic Mini Fan with PIR SensorToheebdareNo ratings yet
- ACS Appl. Energy Mater. 5 (2022) 367-379 PDFDocument13 pagesACS Appl. Energy Mater. 5 (2022) 367-379 PDFEdgar QuintanillaNo ratings yet
- Mind Map AvalanchesDocument3 pagesMind Map AvalanchescgmaliaNo ratings yet
- Detection Dogs Allow For Systematic Non-Invasive Collection of DNA Samples From Eurasian LynxDocument5 pagesDetection Dogs Allow For Systematic Non-Invasive Collection of DNA Samples From Eurasian Lynxsusey madelit apaza mamaniNo ratings yet
- Subway's Fresh Look: CEO Suzanne Greco Is Taking The Company To A Whole New Level With The Fresh Forward RebrandDocument9 pagesSubway's Fresh Look: CEO Suzanne Greco Is Taking The Company To A Whole New Level With The Fresh Forward RebrandTanvir KhanNo ratings yet
- Implant Dentistry - The Most Promising Discipline of Dentistry PDFDocument488 pagesImplant Dentistry - The Most Promising Discipline of Dentistry PDFnaresh sharmaNo ratings yet
- High Efficiency 2.45 GHZ Low Power Hybrid Junction Rectifier For RF Energy HarvestingDocument4 pagesHigh Efficiency 2.45 GHZ Low Power Hybrid Junction Rectifier For RF Energy HarvestingPrakash SunnyNo ratings yet
- Graphing linear functions and writing equations in standard formDocument15 pagesGraphing linear functions and writing equations in standard formnmarjonoNo ratings yet
- Amulets Talismans and CharmsDocument3 pagesAmulets Talismans and CharmsreikiladyNo ratings yet
- Budget-of-Work-General Biology 1Document2 pagesBudget-of-Work-General Biology 1joei ArqueroNo ratings yet
- Plant Coordination and ControlDocument13 pagesPlant Coordination and ControlMarilyn GumeyiNo ratings yet
- Fluosilic Acid MsdsDocument5 pagesFluosilic Acid MsdsVuglaShemmanNo ratings yet
- Monthly HSE report summaryDocument5 pagesMonthly HSE report summaryNiraNo ratings yet
- Ball Pen Canvas Painting Exhibition MumbaiDocument19 pagesBall Pen Canvas Painting Exhibition Mumbaiapi-25885725No ratings yet
- S6000-Operation-Manual SkyliftDocument50 pagesS6000-Operation-Manual SkyliftSetiawan Tuhu basukiNo ratings yet
- Factors Effecting PerformanceDocument47 pagesFactors Effecting Performancebembie83No ratings yet
- Jazz Band LiteratureDocument4 pagesJazz Band LiteratureJohnny LaounNo ratings yet
- Realtime Physics: Active Learning Labs Transforming The Introductory LaboratoryDocument14 pagesRealtime Physics: Active Learning Labs Transforming The Introductory LaboratorysaleemNo ratings yet
- UTHM Construction Safety Group AssignmentDocument19 pagesUTHM Construction Safety Group AssignmentWan Muhammad Faiz Bin Mohd RoslanNo ratings yet
- 42183878Document264 pages42183878Sakthirama VadiveluNo ratings yet
- Hydroelectric and Pumped Storage, Tidal, WaveDocument62 pagesHydroelectric and Pumped Storage, Tidal, WavePrince AbrahamNo ratings yet
- To 1 SMPN 210 JKT Tahun 2016-2017Document11 pagesTo 1 SMPN 210 JKT Tahun 2016-2017Sugeng Supoyo Pawit DigdotriratnaNo ratings yet
- CIA Patho 1Document23 pagesCIA Patho 1Suhas H GNo ratings yet
- Banaba Tea Aids Weight LossDocument5 pagesBanaba Tea Aids Weight LossAveriAlonzoNo ratings yet
- Variac MFG Business Plan Annexure - 1Document6 pagesVariac MFG Business Plan Annexure - 1Manav MatetiNo ratings yet
- Me6404 Te Even QBDocument32 pagesMe6404 Te Even QBBala NarayanasamyNo ratings yet
- OL Lect 9 Seismic Acquisition NewDocument106 pagesOL Lect 9 Seismic Acquisition NewMohammad BilalNo ratings yet
- DR Vatsal Patel AhmedabadDocument30 pagesDR Vatsal Patel AhmedabadSayali PhansekarNo ratings yet
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- The Ancestor's Tale: A Pilgrimage to the Dawn of EvolutionFrom EverandThe Ancestor's Tale: A Pilgrimage to the Dawn of EvolutionRating: 4 out of 5 stars4/5 (811)
- The Molecule of More: How a Single Chemical in Your Brain Drives Love, Sex, and Creativity--and Will Determine the Fate of the Human RaceFrom EverandThe Molecule of More: How a Single Chemical in Your Brain Drives Love, Sex, and Creativity--and Will Determine the Fate of the Human RaceRating: 4.5 out of 5 stars4.5/5 (515)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Tales from Both Sides of the Brain: A Life in NeuroscienceFrom EverandTales from Both Sides of the Brain: A Life in NeuroscienceRating: 3 out of 5 stars3/5 (18)
- 10% Human: How Your Body's Microbes Hold the Key to Health and HappinessFrom Everand10% Human: How Your Body's Microbes Hold the Key to Health and HappinessRating: 4 out of 5 stars4/5 (33)
- A Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsFrom EverandA Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsRating: 4.5 out of 5 stars4.5/5 (4)
- All That Remains: A Renowned Forensic Scientist on Death, Mortality, and Solving CrimesFrom EverandAll That Remains: A Renowned Forensic Scientist on Death, Mortality, and Solving CrimesRating: 4.5 out of 5 stars4.5/5 (397)
- The Other Side of Normal: How Biology Is Providing the Clues to Unlock the Secrets of Normal and Abnormal BehaviorFrom EverandThe Other Side of Normal: How Biology Is Providing the Clues to Unlock the Secrets of Normal and Abnormal BehaviorNo ratings yet
- Buddha's Brain: The Practical Neuroscience of Happiness, Love & WisdomFrom EverandBuddha's Brain: The Practical Neuroscience of Happiness, Love & WisdomRating: 4 out of 5 stars4/5 (215)
- Why We Sleep: Unlocking the Power of Sleep and DreamsFrom EverandWhy We Sleep: Unlocking the Power of Sleep and DreamsRating: 4.5 out of 5 stars4.5/5 (2083)
- Who's in Charge?: Free Will and the Science of the BrainFrom EverandWho's in Charge?: Free Will and the Science of the BrainRating: 4 out of 5 stars4/5 (65)
- Undeniable: How Biology Confirms Our Intuition That Life Is DesignedFrom EverandUndeniable: How Biology Confirms Our Intuition That Life Is DesignedRating: 4 out of 5 stars4/5 (11)
- Wayfinding: The Science and Mystery of How Humans Navigate the WorldFrom EverandWayfinding: The Science and Mystery of How Humans Navigate the WorldRating: 4.5 out of 5 stars4.5/5 (18)
- Gut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)From EverandGut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)Rating: 4 out of 5 stars4/5 (378)
- Inside of a Dog: What Dogs See, Smell, and KnowFrom EverandInside of a Dog: What Dogs See, Smell, and KnowRating: 4 out of 5 stars4/5 (390)
- The Invention of Tomorrow: A Natural History of ForesightFrom EverandThe Invention of Tomorrow: A Natural History of ForesightRating: 4.5 out of 5 stars4.5/5 (5)
- Crypt: Life, Death and Disease in the Middle Ages and BeyondFrom EverandCrypt: Life, Death and Disease in the Middle Ages and BeyondRating: 4 out of 5 stars4/5 (4)
- The Lives of Bees: The Untold Story of the Honey Bee in the WildFrom EverandThe Lives of Bees: The Untold Story of the Honey Bee in the WildRating: 4.5 out of 5 stars4.5/5 (44)
- Good Without God: What a Billion Nonreligious People Do BelieveFrom EverandGood Without God: What a Billion Nonreligious People Do BelieveRating: 4 out of 5 stars4/5 (66)
- The Consciousness Instinct: Unraveling the Mystery of How the Brain Makes the MindFrom EverandThe Consciousness Instinct: Unraveling the Mystery of How the Brain Makes the MindRating: 4.5 out of 5 stars4.5/5 (93)
- Human: The Science Behind What Makes Your Brain UniqueFrom EverandHuman: The Science Behind What Makes Your Brain UniqueRating: 3.5 out of 5 stars3.5/5 (38)
- A Series of Fortunate Events: Chance and the Making of the Planet, Life, and YouFrom EverandA Series of Fortunate Events: Chance and the Making of the Planet, Life, and YouRating: 4.5 out of 5 stars4.5/5 (62)